Abstract
Previous studies have demonstrated an association between high body mass index (BMI) and acute myeloid leukemias (AML), particularly acute promyelocytic leukemia (APL). However, the effect of obesity and overweight on the incidence of AML is not supported by all studies, and the relationship between obesity and prognosis of AML and APL has not been established. Thus, we conducted a meta-analysis to determine the role of BMI on the risk and clinical outcome of AML, including APL. Twenty-six eligible studies enrolling 12,971 AML (including 866 APL) patients were retrieved and analyzed. Overweight and obesity was associated with an increased incidence of AML (relative risk [RR], 1.23; 95% confidence interval [CI], 1.12–1.35; P < 0.001). High BMI did not significantly affect overall survival (OS) (hazard ratio [HR], 0.97; 95% CI, 0.92–1.03; P = 0.323) or disease-free survival (HR, 0.98; 95% CI, 0.88–1.10; P = 0.755) in patients with non-APL AML. By contrast, APL patients with high BMI had shorter OS (HR, 1.77; 95% CI, 1.26–2.48; P = 0.001) and a higher risk of differentiation syndrome (HR, 1.53; 95% CI, 1.03–2.27, P = 0.04). Overall, our findings suggest that patients with overweight or obesity have a higher incidence of AML, and high BMI is a predictor of adverse clinical outcomes in APL.
Similar content being viewed by others
Introduction
The prevalence of obesity has been increasing worldwide over the past decades. According to World Health Organization (WHO), overweight and obesity are defined by a body mass index (BMI) of 25–29.9 kg/m2 and ≥30 kg/m2, respectively. Currently, the proportion of overweight or obesity in adults has increased to approximately 40% worldwide1. It has been reported that overweight or obesity is associated with over 20 types of cancer, such as cancers of the breast, colon, uterus, gallbladder, and cervix, as well as leukemia2,3.
Leukemia is a clonal hematopoietic disorder characterized by the aggressive proliferation of immature hematopoietic progenitor cells arrested at an early stage of differentiation. Acute myeloid leukemia (AML) is one of the most common myeloid malignancies in adults4. Although much effort has been devoted to studying this disease, the etiology and pathophysiology of AML are still poorly understood and the outcome remains unsatisfactory. Epidemiologic observations have suggested that obesity is a risk factor for AML5,6,7. However, obesity did not affect risk for AML in several studies8,9,10, and Wong et al. even reported that obesity is protective against AML11. Overweight may have a similar effect on the incidence of AML, although this relationship is less certain6,8,12. The most recent meta-analysis on this topic was performed in 2012 and suggested that obesity, but not overweight, increases incidence of AML7. However, the number of patients with AML was limited because this meta-analysis included all types of leukemia and only included five studies on AML. Since 2012, five new studies, including two large multinational survey programs, have been published5,6,10,12,13. Thus, including these new studies in an updated analysis is needed to comprehensively evaluate the association between BMI and risk for AML.
In addition to the incidence of AML, the association between high BMI and the prognosis of AML is unclear due to the lack of a meta-analysis, although several studies have investigated this issue14,15,16. Reports on the prognostic value of obesity for AML are somewhat inconsistent. Several studies have found that obesity adversely affects the clinical outcome of AML17 whereas others have failed to confirm such an association15,18,19.
Notably, several studies have shown that the percentage of obese patients with acute promyelocytic leukemia (APL), a unique subtype of AML, is higher than that observed in patients with non-APL AML15,20,21. APL generally carries the PML/RARα fusion protein linking the retinoic acid receptor alpha gene (RARα) on chromosome 17 with the PML gene on chromosome 15. Historically, APL was one of the most fatal forms of acute leukemia but currently has a cure rate of approximately 80–85% with the introduction of all-trans retinoic acid (ATRA) and arsenic trioxide (ATO)15,22. Emerging studies have demonstrated that obesity has adverse effects on the treatment outcome of APL15,23. However, to our knowledge, a quantitative analysis that evaluates this association with APL is not available.
With the aim of evaluating the prognostic value of obesity in patients with AML (including APL), we conducted the first comprehensive meta-analysis to clarify the potential association between AML, particularly APL, with overweight and obesity as defined by BMI. Another objective of our study was to investigate the association between obesity and the incidence of AML.
Methods
BMI calculation and classification
BMI was calculated by dividing weight in kilograms by the square of height in meters (weight [kg]/height [m2]). According to the criteria from the World Health Organization, BMI was categorized as underweight (<18.5 kg/m2), normal (18.5–25 kg/m2), overweight (25–29.9 kg/m2), and obese (≥30 kg/m2). Most of the studies used 25 and 30 kg/m2 as the thresholds for overweight and obesity, respectively. Studies that did not meet these criteria11,13,24 were eligible for analysis of the association based on high BMI but were excluded from the overweight and obese subgroup analysis. Lin et al. used body weight (BW) ≥130% ideal body weight (IBW) as the criteria to define obesity25.
Literature search
A literature search (last search updated to Dec. 4, 2016) was conducted in PubMed, EMBASE, Web of Science and the Cochrane Library for articles assessing the effect of overweight and obesity on the incidence and clinical outcome of AML using the keywords as follows: (obesity OR overweight OR body mass OR BMI OR body weight OR anthropometric) AND leukemia. References lists from the retrieved studies were also examined. The results were limited to peer-reviewed English language studies.
Eligibility criteria
The studies were considered eligible if they reported the effect of overweight and obesity on the incidence or clinical outcome of patients with AML and provided sufficient data to determine an estimate of relative risk (RR) or hazard ratio (HR) and a 95% confidence interval (CI). Odd ratios (OR) were converted to RRs using methods reported by Zhang et al.26. When the patient populations overlapped between studies, only the most recent or most complete publication was included to avoid duplications.
Data extraction and quality assessment
The data extracted for our meta-analysis included the first author’s name, year of publication, country, number of patients analyzed, enrollment period, source of the cohort, adjustments, and other relevant data stratified by BMI. Quality assessment of eligible papers was conducted according to the Newcastle-Ottawa Scale (NOS)7. The NOS score includes an assessment of subject selection (four points), comparability of groups (two points), and exposure or clinical outcome (three points). The maximum score is 9 and the scores of eligible papers included in our meta-analysis is ranged from 5 to 9 (Supplementary Table S1).
Statistical analysis
RR or HR from each article was extracted directly from the original reports or calculated using the method reported by Tierney et al.27. The potential heterogeneity across studies was evaluated using the Cochran’s Q-test and expressed using the I2 index. The pooled results for RR and HR were calculated by the fixed-effects model (I2 ≤ 50%) or the random-effects model (I2 > 50%). Publication bias was evaluated by the funnel plot and Egger’s and Begg’s tests. The effect of publication bias on the pooled findings was evaluated by trim-and-fill analyses. The stability of the pooled findings was confirmed by one-way sensitivity and subgroup analyses. All statistical analyses were conducted using STATA version 11.0.
Results
Identification of relevant studies
A total of 7,475 studies were retrieved from the preliminary literature search (PubMed:2,362, EMBASE:2,302, Web of Science:2,636, and the Cochrane library:175), and an additional two studies were identified from a review of citations. 173 potential relevant publications were retrieved for detailed evaluation. Of these publications, 111 articles were excluded after reading the title and abstract because they were irrelevant to our meta-analysis, or because they were mechanistic studies, case reports, conference abstracts, or reviews. An additional 38 publications were then excluded because they were irrelevant to AML, provided no data for further analysis, or were duplicate publications or reviews. Finally, 26 studies were included in our meta-analysis (Fig. 1, Table 1), including 12 papers about relative risk (RR) with 6,724 AML patients5,6,8,9,10,11,12,13,28,29,30,31, 11 papers regarding AML survival with 5,505 non-APL AML patients and 538 APL patients14,15,16,17,18,19,24,25,32,33,34, and three papers on the subject of differentiation syndrome in APL (after excluding duplicate publications32,35,36) with 243 patients23,37,38.
Relationship between high BMI and incidence of AML
AML is one of the most common myeloid malignancies in adults. To explore the association between BMI and the incidence of AML, we analyzed 12 studies that reported on incidence estimates for AML according to BMI (Table 1). All ORs were transformed into RRs before pooled analysis. The pooled RR indicated that high BMI was associated with increased risk for AML (RR, 1.23; 95% CI, 1.12–1.35; P < 0.001; I2 = 66.0%; random effects; Fig. 2A). Although no significant publication bias was identified by Begg’s and Egger’s tests (PBegg = 0.227; PEgger = 0.156), the funnel plot suggested the possibility of missing studies (Supplementary Fig. S1A). After performing a trim-and-fill analysis (Supplementary Fig. S1B), we found that six studies might be missing. When these potentially missing studies were added to the analysis, the adjusted RR would be 1.14 (95% CI, 1.04–1.26, P = 0.008).
We further divided the patients into overweight and obesity subgroups. As shown in Fig. 2B and C, both overweight and obesity were associated with higher incidence of AML (for overweight, RR, 1.10; 95% CI, 1.03–1.17; P = 0.007; I2 = 43.1%; fixed effects; and for obesity, RR, 1.41; 95% CI, 1.24–1.61; P < 0.001; I2 = 66.5%; random effects). One-way sensitivity analysis further confirmed the stability of our results (Supplementary Fig. S1C).
Relationship between high BMI and clinical outcome of AML
Next, we investigated the prognostic value of BMI for clinical outcomes of AML. Because treatment strategy and prognosis of APL and non-APL are significantly different, we analyzed their clinical outcomes separately.
No association between high BMI and clinical outcome of non-APL AML
Nine studies were included in the survival estimates for BMI in non-APL AML (Table 1). Our data suggested that high BMI did not significantly affect the survival of non-APL AML patients (HR, 0.97; 95% CI, 0.92–1.03; P = 0.323; I2 = 42.1%, fixed effects, Fig. 3A). No significant publication bias was identified by Begg’s and Egger’s tests (PBegg = 0.434; PEgger = 0.25). Although the funnel plot showed asymmetry (Supplementary Fig. S2A), no missing study were identified by the trim-and-fill analysis (Supplementary Fig. S2B).
The effects of high BMI on the overall survival of non-APL AML patients. (A) Meta-analysis of the overall survival (OS) of AML according to BMI with the fixed-effects model. (B) Estimates of OS in overweight AML individuals with the random-effects model. (C) Estimates of OS in obese AML individuals with fixed-effects model.
We divided these patients into overweight and obese subgroups. Similarly, neither overweight nor obesity affected OS of patients with non-APL AML relative to patients of normal weight (for overweight, HR, 0.86; 95% CI, 0.70–1.05; P = 0.14; I2 = 59.5%; random effects; and for obesity, HR, 0.99; 95% CI, 0.93–1.07; P = 0.281; I2 = 32.9%; fixed effects; Fig. 3B,C). One-way sensitivity analysis further confirmed the stability of our pooled findings (Supplementary Fig. S2C).
The HRs for disease free survival (DFS) were available in three studies about non-APL AML (Table 1). The results indicated that high BMI at diagnosis did not affect DFS of non-APL AML (HR, 0.98; 95% CI, 0.88–1.10; fixed effects, Fig. 4). The heterogeneity among studies was absent (P = 0.765; I2 = 0%). Specifically with respect to obesity, there was still no association between obesity and DFS (HR, 1.00; 95% CI, 0.88–1.14; P = 0.951; I2 = 0%; fixed effects, Fig. 4).
Significant association between high BMI and clinical outcome of APL
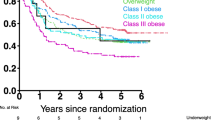
APL is a unique subtype of AML. Surprisingly, we found that among patients with APL, those with high BMI had a shorter duration of OS than those with low BMI after pooling three relevant studies (HR, 1.77; 95% CI, 1.26–2.48; P = 0.001; I2 = 0%; fixed effects; Fig. 5A)15,24,32. Moreover, high BMI in patients with APL was associated with an increased risk of developing differentiation syndrome, a severe complication of chemotherapy, (HR, 1.86; 95% CI, 1.23–2.82; P = 0.003; I2 = 38.9%; fixed effects; Fig. 5B), according to three related studies23,37,38. The DFS data of APL was available in only one publication, which demonstrated that obese patients have worse DFS (HR, 1.53; 95% CI, 1.03–2.27, p = 0.04)15.
Discussion
Increasing evidence has demonstrated that obesity is correlated to the incidence and clinical outcome of AML5,6,7,29,39. In our meta-analysis, we systematically collected related literature and analyzed the association between obesity and AML, including APL. First, we observed that both overweight and obesity increased the risk for AML. This is an important update since previous studies showed no correlation between overweight and incidence of AML7,39,40. Second, our study was the first to evaluate the relationship between obesity and the clinical outcomes (OS and DFS) of AML using a meta-analytical methodology. We found that obesity had no effect on the OS or DFS of non-APL AML, whereas overweight or obese patients with APL had a poorer OS and a higher risk of developing differentiation syndrome. Overall, obesity was closely related to AML, especially APL.
Exploring the association between obesity and AML is important for drug development and the battle against AMLs. However, mechanistic studies investigating the adverse association between obesity and AML are still in the early stages. Recently, epigenome-wide association studies identified that BMI is associated with widespread changes in DNA methylation41. In fact, fatty acid binding protein 4 (FABP4)/IL-6/STAT3/DNA methyltransferase 1 (DNMT1) have been shown to link obesity to the growth of AML cells42. Li et al. demonstrated that the obesity-associated gene FTO is highly expressed in AML with the MLL-fusion gene, thereby promoting leukemogenesis and inhibiting ATRA-induced cell differentiation43. Moreover, studies have shown that leukemia stem cells with a high expression of CD36 (fatty acid transporter) are prone to be chemoresistance44, and CD36+ patients with AML have a poorer leukemia-free survival45.
Apart from the mechanisms illustrated above, the function of obesity in contributing to leukemogenesis requires more research. Adipose tissue is a complex and active endocrine organ and can secrete various bioactive adipokines, hormones, inflammatory factors, angiogenesis factors, and free fatty acids. These secretory factors have been shown to participate in production and progression of tumors46,47, suggesting they may also contribute to the leukemogenesis of AML. Furthermore, as adipocytes are one of the most abundant cell types in blood-producing bone marrow48, direct cell-to-cell interaction cannot be disregarded, as Tabe et al. have demonstrated that the direct cell-to-cell interaction between adipocytes and APL cells is required for adipocyte-induced anti-apoptotic effect49. Also, it should be noted that obese individuals have unique pharmacokinetics compared to normal-weight controls. Reduced efficacy of chemotherapy drugs in overweight and obese patients, probably as a result of altered liver enzyme function, is a likely and often underestimated event related to cancer mortality46. It is also unclear whether the increased incidence and adverse outcome of obese patients with leukemia are associated to complications from obesity-related co-morbidities and a chronic inflammatory state or to obesity itself. In addition, microbiota can modulate the response to cancer therapy and susceptibility to toxic side effects, and obesity-induced gut microbial metabolites alterations may influence the clinical outcomes of AML patients47.
When evaluating the prognosis of patients with AML, the treatment strategies and patient’s characteristics should also be factors to consider, including gender, age, chromosome karyotype, genetic changes, and ECOG. In our meta-analysis, multivariate analysis was conducted to avoid the interference of confounding factors in most studies (Table 1 and Supplementary Table S2). Another important issue is that the dosing strategies may be different for the obese AML patients in different studies. For this, Percival et al. summarized several retrospective analyses and concluded that dosing according to body surface area based on ideal body weight (cap) or actual body weight (not cap) have similar complete remission rates, toxicity, and overall survival in obese patients with AML50.
Our finding that obesity has no effect on the OS of adult patients with AML was somewhat surprising, particularly because a high BMI is associated with poorer OS in pediatric patients with AML51. This discrepancy may be due to the physiological and metabolic differences between children and adults. However, we did find that obesity was associated with poorer OS in adult patients with APL. Actually, Tabe et al. showed that the leptin receptor is highly expressed on APL cells, and co-culturing of mesenchymal stem cell-derived adipocytes with APL cells significantly reduced ATRA and doxorubicin-induced apoptosis of APL cells49. More mechanistic studies are required to investigate the association between obesity and APL.
Our meta-analysis may carry inherent limitations within the published literature. First, there is risk for publication, ecological, and racial bias. Second, although the survival data included was primarily obtained through multivariable analyses considering the most influential confounder, some confounders may have still been ignored. Third, BMI is inappropriate for evaluating adiposity in individuals at extreme heights or older ages. Moreover, self-reported height and weight in some studies may be inaccurate and thus result in classification errors. Obese individuals vary in their distribution of visceral and subcutaneous fat. Since the function and metabolism between the two types are different, individuals who have the same BMI may respond differently to risk factors and cancer drugs due to variance in fat distributions. Finally, the research on APL is relatively limited because its incidence is lower than in other subtypes of AML. Further studies should be conducted to sufficiently address these issues.
In conclusion, both overweight and obesity were associated with increased risk of AML, with obesity producing more palpable effects. However, obesity does not significantly affect the OS and DFS of non-APL AML. APL patients are, more obese, on average, than those with other forms of AML, and obesity is an adverse prognostic factor for clinical outcome in APL (demonstrated by reduced OS and the increased incidence of differentiation syndrome). Thus, APL is more specifically associated with obesity.
Evaluating the underlying mechanisms responsible for their relationship is necessary to develop the novel therapeutic approaches for AML. Also, given that high BMI increases the incidence of AML, controlling body weight may be considered for obese individuals. In addition, for obese APL patients, more attention should be given to possible ATRA-associated complications during induction therapy.
References
Trends in adult body-mass index in 200 countries from 1975 to 2014: a pooled analysis of 1698 population-based measurement studies with 19.2 million participants. LANCET 387, 1377 (2016).
Hefetz-Sela, S. & Scherer, P. E. Adipocytes: impact on tumor growth and potential sites for therapeutic intervention. Pharmacol Ther 138, 197 (2013).
Bhaskaran, K. et al. Body-mass index and risk of 22 specific cancers: a population-based cohort study of 5.24 million UK adults. LANCET 384, 755 (2014).
Estey, E. & Dohner, H. Acute myeloid leukaemia. LANCET 368, 1894 (2006).
Poynter, J. N. et al. Obesity over the life course and risk of acute myeloid leukemia and myelodysplastic syndromes. Cancer Epidemiol 40, 134 (2016).
Murphy, F. et al. Body size in relation to incidence of subtypes of haematological malignancy in the prospective Million Women Study. Brit J Cancer 108, 2390 (2013).
Castillo, J. J. et al. Obesity but not overweight increases the incidence and mortality of leukemia in adults: A meta-analysis of prospective cohort studies. Leukemia Res 36, 868 (2012).
Söderberg, K. C. et al. Overweight, obesity and risk of haematological malignancies: A cohort study of Swedish and Finnish twins. Eur J Cancer 45, 1232 (2009).
Engeland, A., Tretli, S., Hansen, S. & Bjorge, T. Height and Body Mass Index and Risk of Lymphohematopoietic Malignancies in Two Million Norwegian Men and Women. Am J Epidemiol 165, 44 (2006).
Nagel, G. et al. Metabolic factors and blood cancers among 578,000 adults in the metabolic syndrome and cancer project (Me-Can). Ann Hematol 91, 1519 (2012).
Wong, O., Harris, F., Yiying, W. & Hua, F. A hospital-based case-control study of acute myeloid leukemia in Shanghai: Analysis of personal characteristics, lifestyle and environmental risk factors by subtypes of the WHO classification. Regul Toxicol Pharm 55, 340 (2009).
Strom, S. S., Oum, R., Elhor Gbito, K. Y., Garcia-Manero, G. & Yamamura, Y. De novo acute myeloid leukemia risk factors. Cancer-Am Cancer Soc 118, 4589 (2012).
Saberi Hosnijeh, F. et al. Anthropometric characteristics and risk of lymphoid and myeloid leukemia in the European Prospective Investigation into Cancer and Nutrition (EPIC). Cancer Cause Control 24, 427 (2013).
Medeiros, B. C., Othus, M., Estey, E. H., Fang, M. & Appelbaum, F. R. Impact of body-mass index on the outcome of adult patients with acute myeloid leukemia. Haematologica 97, 1401 (2012).
Castillo, J. J. et al. Relationship between obesity and clinical outcome in adults with acute myeloid leukemia: A pooled analysis from four CALGB (alliance) clinical trials. Am J Hematol 91, 199 (2016).
Tavitian, S. et al. Impact of obesity in favorable-risk AML patients receiving intensive chemotherapy. Am J Hematol 91, 193 (2016).
Finn, L. et al. Epidemiology of adult acute myeloid leukemia: Impact of exposures on clinical phenotypes and outcomes after therapy. Cancer Epidemiol 39, 1084 (2015).
Brunner, A. M. et al. Association between baseline body mass index and overall survival among patients over age 60 with acute myeloid leukemia. Am J Hematol 88, 642 (2013).
Wenzell, C. M. et al. Outcomes in obese and overweight acute myeloid leukemia patients receiving chemotherapy dosed according to actual body weight. Am J Hematol 88, 906 (2013).
Estey, E. et al. Association between increased body mass index and a diagnosis of acute promyelocytic leukemia in patients with acute myeloid leukemia. Leukemia 11, 1661 (1997).
Tedesco, J., Qualtieri, J., Head, D., Savani, B. N. & Reddy, N. High Prevalence of Obesity in Acute Promyelocytic Leukemia (APL): Implications for Differentiating Agents in APL and Metabolic Syndrome. Ther Adv Hematol 2, 141 (2011).
Coombs, C. C., Tavakkoli, M. & Tallman, M. S. Acute promyelocytic leukemia: where did we start, where are we now, and the future. Blood Cancer J 5, e304 (2015).
Breccia, M. et al. Increased BMI correlates with higher risk of disease relapse and differentiation syndrome in patients with acute promyelocytic leukemia treated with the AIDA protocols. Blood 119, 49 (2012).
Wang, Y. et al. Long-term follow-up of homoharringtonine plus all-trans retinoic acid-based induction and consolidation therapy in newly diagnosed acute promyelocytic leukemia. Int J Hematol 101, 279 (2015).
Lin, A., Othus, M., McQuary, A., Chi, M. & Estey, E. Influence of obesity on efficacy and toxicity of induction chemotherapy in patients with newly diagnosed acute myeloid leukemia. Leukemia Lymphoma 54, 541 (2012).
Zhang, J. & Yu, K. F. What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. Jama 280, 1690 (1998).
Tierney, J. F., Stewart, L. A., Ghersi, D., Burdett, S. & Sydes, M. R. Practical methods for incorporating summary time-to-event data into meta-analysis. Trials 8, 16 (2007).
Kasim, K., Levallois, P., Abdous, B., Auger, P. & Johnson, K. C. Lifestyle factors and the risk of adult leukemia in Canada. Cancer Cause Control 16, 489 (2005).
Ross, J. A., Parker, E., Blair, C. K., Cerhan, J. R. & Folsom, A. R. Body mass index and risk of leukemia in older women. Cancer Epidemiol Biomarkers Prev 13, 1810 (2004).
Samanic, C., Chow, W., Gridley, G., Jarvholm, B. & Fraumeni, J. F. Relation of body mass index to cancer risk in 362,552 Swedish men. Cancer Cause Control 17, 901 (2006).
Samanic, C. et al. Obesity and cancer risk among white and black United States veterans. Cancer Causes Control 15, 35 (2004).
Jeddi, R. et al. Treatment of acute promyelocytic leukemia with PETHEMA LPA 99 protocol: a Tunisian single center experience. Hematology 15, 204 (2010).
Kempf, E. et al. Prognosis of body mass index and chemotherapy dose capping in acute myeloid leukaemia. Leukemia Res 38, 1425 (2014).
Lee, H. J. et al. Is obesity a prognostic factor for acute myeloid leukemia outcome? Ann Hematol 91, 359 (2012).
Jeddi, R. et al. Predictive factors of all-trans-retinoic acid related complications during induction therapy for acute promyelocytic leukemia. Hematology 13, 142 (2008).
Jeddi, R. et al. Treatment of Acute Promyelocytic Leukemia with AIDA Based Regimen. Update of a Tunisian Single Center Study. Mediterr J Hematol Infect Dis 3, e2011033 (2011).
Jeddi, R. et al. High body mass index is an independent predictor of differentiation syndrome in patients with acute promyelocytic leukemia. Leukemia Res 34, 545 (2010).
Leblebjian, H. et al. Predictive factors for all-trans retinoic acid-related differentiation syndrome in patients with acute promyelocytic leukemia. Leukemia Res 37, 747 (2013).
Lichtman, M. A. Obesity and the Risk for a Hematological Malignancy: Leukemia, Lymphoma, or Myeloma. The Oncologist 15, 1083 (2010).
Larsson, S. C. & Wolk, A. Overweight and obesity and incidence of leukemia: A meta-analysis of cohort studies. Int J Cancer 122, 1418 (2008).
Wahl, S. et al. Epigenome-wide association study of body mass index, and the adverse outcomes of adiposity. Nature (2016).
Yan, F. et al. Fatty acid-binding protein FABP4 mechanistically links obesity with aggressive AML by enhancing aberrant DNA methylation in AML cells. Leukemia (2016).
Li, Z. et al. FTO Plays an Oncogenic Role in Acute Myeloid Leukemia as a N6-Methyladenosine RNA Demethylase. Cancer Cell (2016).
Ye, H. et al. Leukemic Stem Cells Evade Chemotherapy by Metabolic Adaptation to an Adipose Tissue Niche. Cell Stem Cell 19, 23 (2016).
Perea, G. et al. Adverse prognostic impact of CD36 and CD2 expression in adult de novo acute myeloid leukemia patients. Leuk Res 29, 1109 (2005).
Mazzarella, L. Why does obesity promote cancer? Epidemiology, biology, and open questions. Ecancermedicalscience 9, 554 (2015).
Tahergorabi, Z., Khazaei, M., Moodi, M. & Chamani, E. From obesity to cancer: a review on proposed mechanisms. Cell Biochem Funct 34, 533 (2016).
Scheller, E. L., Cawthorn, W. P., Burr, A. A., Horowitz, M. C. & MacDougald, O. A. Marrow Adipose Tissue: Trimming the Fat. Trends Endocrinol Metab 27, 392 (2016).
Tabe, Y. PML-RAR is associated with leptin-receptor induction: the role of mesenchymal stem cell-derived adipocytes in APL cell survival. Blood 103, 1815 (2004).
Percival, M. M. & Medeiros, B. C. Chemotherapy dose in obese AML patients: To cap or not to cap? Leukemia Res 39, 30 (2015).
Orgel, E. et al. Association of body mass index and survival in pediatric leukemia: a meta-analysis. Am J Clin Nutr 103, 808 (2016).
Acknowledgements
This work was supported in part by National Natural Science Foundation Grants of China (81530003), the National Key Research and Development Program of China (2016YFC0902800), Shanghai Leading Talent Projects (2015008) and the Academic Leader Program of Shanghai Science and Technology Committee (2015137).
Author information
Authors and Affiliations
Contributions
S.F.L. and K.K.W. designed the study, S.F.L. and L.C. searched and screened the studies, S.F.L., Y.L.M. and X.F.M. extracted and analyzed the data, F.Y.D., W.J., H.M.Z. and J.M.L. performed statistical analysis, S.F.L. and K.K.W. wrote the manuscript, all the authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Li, S., Chen, L., Jin, W. et al. Influence of body mass index on incidence and prognosis of acute myeloid leukemia and acute promyelocytic leukemia: A meta-analysis. Sci Rep 7, 17998 (2017). https://doi.org/10.1038/s41598-017-18278-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-18278-x
This article is cited by
-
Global, regional, and national burden of acute myeloid leukemia, 1990–2021: a systematic analysis for the global burden of disease study 2021
Biomarker Research (2024)
-
Association between class III obesity and overall survival in previously untreated younger patients with acute myeloid leukemia enrolled on SWOG S1203
Leukemia (2024)
-
Obesity and Leukemia: Biological Mechanisms, Perspectives, and Challenges
Current Obesity Reports (2023)
-
Regional and national burden of leukemia and its attributable burden to risk factors in 21 countries and territories of North Africa and Middle East, 1990–2019: results from the GBD study 2019
Journal of Cancer Research and Clinical Oncology (2023)
-
Obesity-induced galectin-9 is a therapeutic target in B-cell acute lymphoblastic leukemia
Nature Communications (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.