Abstract
The optic nerve sheath diameter (ONSD) is considered as an indirect marker for intracranial pressure (ICP). However, the optimal cut-off value for an abnormal ONSD indicating elevated ICP and its associated factors have been unclear. Thus, we investigated normative values for the ONSD using ultrasonography and investigate the potential factors affecting it. We prospectively recruited healthy volunteers between September 2016 and March 2017. A total of 585 individuals were included, in which the mean ONSD was 4.11 mm [95% confidence interval (CI), 4.09–4.14 mm]. Although ONSD was correlated with sex (p = 0.015), height (p = 0.003), and eyeball transverse diameter (ETD) (p < 0.001) in simple linear regression analyses, multiple linear regression analysis revealed that only ETD was independently associated with ONSD (p < 0.001). Accordingly, we further established a normative value for the ONSD/ETD ratio and its associated factors. The mean ONSD/ETD ratio was 0.18 (95% CI, 0.18–0.18), but the ONSD/ETD ratio was not correlated with sex, height, weight, body mass index, and head circumference. Our findings suggest that the ONSD had a strong correlation with ETD, and ONSD/ETD ratio might provide more reliable data than ONSD itself as a marker of ICP.
Similar content being viewed by others
Introduction
Elevated intracranial pressure (ICP) is a potentially devastating condition resulting from various neurological and non-neurological disorders1. Rapid detection of elevated ICP and subsequent management are important because it is associated with poor prognosis2,3. The golden standard for estimating ICP includes invasive methods such as intraventricular catheterization and intraparenchymal probes4. However, such procedures are not routinely performed because of the absence of neurosurgeons or intensive care units and the risk of complications including hemorrhage and infection. In addition, they are contraindicated in patients with thrombocythemia or coagulopathy5,6. Accordingly, the importance of non-invasive methods for ICP measurement has increased.
The optic nerve sheath diameter (ONSD) is considered as an indirect marker for ICP estimation7. Measurement of ONSD by ultrasonography is a rapid and easily accessible bedside test. Furthermore, growing evidence has shown that this procedure has high reproducibility and low intra- and inter-observer variability8,9. Given that computed tomography (CT) or magnetic resonance imaging is time consuming and requires patient transfer, ultrasonographic measurement of ONSD may be a good choice for the detection of elevated ICP in clinical settings and research. However, despite its usefulness and popularity, the optimal cut-off value for an abnormal ONSD indicating elevated ICP has been unclear, because most studies on ONSD measurement included only a small number of healthy individuals. Furthermore, although previous studies investigated demographic and physiological factors associated with ONSD, the results have been inconsistent or inconclusive. A clear understanding of the normal range for ONSD and its associated factors is crucial to interpret the measurement as a marker of ICP.
Therefore, the main aims of the current study were to establish normative values for ONSD using ultrasonography in a large number of healthy Korean adults and investigate potential factors affecting this parameter.
Materials and Methods
Study Population
We prospectively recruited healthy volunteers who visited the Republic of Korea Air Force Education And Training Command for physical examination required to become a soldier between September 2016 and March 2017. All volunteers were limited to young healthy adults aged 18–30 years, given the nature of the military organization. We excluded individuals with a history of neurological disorders. Written informed consent was obtained from all participants before enrollment. The study protocol was approved by the Institutional Review Board of the Armed Forces Medical Command (Seongnam, Korea) and followed to the principles of the Declaration of Helsinki.
The following data were recorded for each subject: age, sex, height, weight, and head circumference. The head circumference was measured by a single investigator (R.K., a board-certified neurologist) using a nonstretchable tape around the widest possible occipitofrontal circumference. The body mass index (BMI) was calculated as the weight in kilograms divided by the height in meters squared.
Ultrasound Measurement
Ultrasonic examination was performed by an experienced investigator (D.H.K., a board-certified radiologist) using a GE Logiq P6 scanner (General Electrics Medical Systems, Milwaukee, WI, USA) with a 11–3 MHz linear transducer. The subjects were examined in a supine position with the head elevated at 20–30°. They were instructed to keep their eyes shut in a mid-position of the bulb and suppress any eye movement. A thick layer of conductive ultrasound gel was applied over the closed upper eyelid. The probe was placed gently on the gel in the temporal area of the eyelid to prevent pressure from being exerted on the eye.
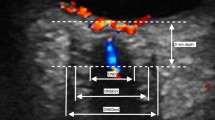
ONSD and the eyeball transverse diameter (ETD) were measured for each eye in the horizontal plane (Fig. 1). ONSD was defined as the distance between the external borders of the hyperechoic area 3 mm posterior to the point where the optic nerve entered the globe, using an electronic caliper along the axis perpendicular to the retina. ETD (retina to retina) was defined as the maximal transverse diameter of the eyeball obtained by scanning from the superior to the inferior side. To minimize intraobserver variability, each measurement was performed three times and the mean value was derived. Before the enrollment of participants, a training session with 15 healthy volunteers who were not included in this study was held to familiarize the examiner with the ultrasonic measurement of ONSD and ETD.
Statistical Analysis
Continuous variables are presented as medians and interquartile ranges (IQRs) or means ± standard deviations (SDs), while categorical variables are reported as frequencies and percentages. Continuous variables were compared using paired t-tests. We used a series of simple linear regression models to identify demographic and physiological factors associated with ONSD. Potential factors of interest were selected a priori on the basis of previous literature; these included sex, height, weight, BMI, head circumference, and ETD. The factors that survived simple linear regression analyses were then evaluated using multiple linear regression models. A two-tailed p-value of <0.05 was considered statistically significant. All statistical analyses were performed with IBM SPSS version 18 (IBM Software Inc.).
Results
In total, 585 healthy volunteers were included in this study. The mean age was 21.4 ± 1.9 years, and 508 (90.4%) subjects were men. The mean height, weight, BMI, and head circumference of the individuals were 171.1 ± 6.8 cm, 68.5 ± 11.6 kg, 22.8 ± 3.1 kg/m2, and 57.6 ± 1.7 cm, respectively.
ONSD and ETD values are detailed in Table 1. ONSD ranged from 3.30 mm to 5.20 mm, and 95% subjects exhibited a mean ONSD in the range of 4.09 mm to 4.14 mm. The median ONSD was 4.10 mm (IQR, 3.85–4.35 mm). There was no significant difference in ONSD between the right and left eyes (p = 0.510). The median and mean ETD were 22.85 mm (IQR, 22.25–23.45 mm) and 22.91 ± 0.93 mm, respectively.
The results of regression analyses are summarized in Table 2. Simple linear regression analyses showed that ONSD was correlated with sex (p = 0.015), height (p = 0.003), and ETD (p < 0.001). After adjustment for potential confounders between these factors, only ETD was found to be independently associated with ONSD (p < 0.001). Accordingly, we further analyzed normative values for the ONSD/ETD ratio and its associated factors including sex, height, weight, BMI, and head circumference. The ONSD/ETD ratio ranged from 0.14 to 0.23, and 95% subjects exhibited a mean ONSD/ETD ratio of 0.18. There was no significant difference in the ONSD/ETD ratio between the right and left eyes (p = 0.329). Simple linear regression analyses showed that the ONSD/ETD ratio was not correlated with sex (p = 0.140), height (p = 0.505), weight (p = 0.826), BMI (p = 0.516), and head circumference (p = 0.387).
Discussion
In the present study, we assessed normative values for ONSD and its associated factors using ultrasonography in 585 healthy Korean adults. The mean [95% confidence interval (CI)] values for ONSD, ETD, and the ONSD/ETD ratio were 4.11 ± 0.35 mm (4.09–4.14 mm), 22.91 ± 0.93 mm (22.83–22.98 mm), and 0.18 ± 0.02 (0.18–0.18), respectively, and ONSD was associated with ETD, but not with sex, height, weight, BMI, and head circumference. To our knowledge, the present study included the largest number of healthy volunteers among all studies evaluating ONSD using ultrasonography. Therefore, we believe that our findings regarding the normal range for ONSD and its associated factors are reliable.
The mean ultrasonographic ONSD in the current study was 4.11 mm (range, 3.3–5.2 mm); this value is close to that reported by Lee et al.10, who reported a mean CT-based ONSD of 4.1 mm (range, 2.9–5.3 mm) in the Korean population. The normal range for ultrasonographic ONSD in healthy volunteers has been reported in many other countries (Table 3)8,9,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29. Despite the diversity in the results of these studies, the ONSD measurements in this study were within the normal range of previously reported values. In addition, the upper normal ONSD limit (5.2 mm) and the upper bound of the 95% CI (4.14 mm) for the mean ONSD value corroborated with the optimal cut-off value for the identification of elevated ICP suggested by previous studies where the lowest bound of ONSD values was ≥5.2 mm in patients with elevated ICP30,31,32,33,34,35,36. Although some authors insist that ONSD is influenced by ethnicity, we could not find obvious differences between Korea and other countries13,14,16,35,37.
There was a strong correlation between ONSD and ETD in the present study, and this finding is supported by a previous study evaluating CT-based ONSD38. Several studies have assessed the relationship between sex and ONSD, although the results have been inconsistent (Table 3)8,11,13,14,24,27. We found an association between sex and ONSD in our simple regression analyses but not in our multiple regression analyses including ETD. This finding strongly suggests that sex is not associated with ONSD, and ETD is a confounding factor for their relationship. Weight was not associated with ONSD in the current study, which is consistent with the results of previous studies (Table 3)13,27. On the other hand, Wang et al.14 reported that ONSD was associated with BMI in a study of 230 healthy individuals; however, no significant association was found between the two variables in our larger-scale study.
To the best of our knowledge, the present study is the first to establish a normal value for the ONSD/ETD ratio using ultrasonography. Our derived ratio is very similar to the CT-based ratio of 0.19 derived by Vaiman and Beckerman et al.38, who also found that the ONSD/ETD ratio was significantly higher in patients with intracerebral hemorrhage than in healthy individuals and exhibited a reasonably good correlation with invasive ICP values39,40. The ultrasonographic ONSD/ETD ratio may be a better marker of elevated ICP compared with ONSD alone for several reasons. First, there was a strong correlation between ONSD and ETD. Second, the standard deviation between the normative and pathological values for ONSD was overlapping. Finally, the ONSD/ETD ratio was independent of demographic factors such as sex, height, weight, and BMI. Further trials are warranted to validate this parameter in patients with elevated ICP.
There have been technical issues associated with ultrasonographic measurement of the ONSD. Although some authors have suggested that B-mode ultrasound scan is less accurate in evaluating ONSD owing to blooming effect41,42,43,44,45, we used this mode in the current study because in standardized A-mode scan, it is difficult to choose a distance behind the globe in order to consistently measure the nerve7. Moreover, B-mode scan is easier to use compared to the A-mode scan and can be used even for patients with a reduced level of cooperation. For these reasons, B-mode scan is more commonly used in the emergency room and intensive care unit7,46. The other technical issue is that measurement of the ONSD using B-mode scan may be more accurate in lateral gaze position (abduction) given the poor lateral resolution47. However, these eye movements can be performed only in well-coordinated individuals. Unfortunately, patients with suspected elevated ICP are either unconscious or poorly coordinated in many cases. In addition, Lagreze et al.48 reported no significant difference between the results of the straight and lateral gaze tests with B-mode ultrasound in healthy subjects. Thus, we measured the ONSD in the straight gaze position.
This study has some limitations. Ultrasonographic measurements were obtained by a single experienced board-certified radiologist; therefore, interobserver variability was not evaluated in this study. However, each measurement was obtained three times to minimize errors and bias. In addition, all volunteers were limited to young healthy adults; therefore, the generalizability of our findings to populations of all ages is limited. However, many previous studies have reported that ONSD is not associated with age, and some authors have suggested that ONSD remains more or less constant during the life of an individual8,11,13,14,24,27. Accordingly, this limitation is not likely to be significant.
In conclusion, we found that the mean ONSD and the ONSD/ETD ratio determined using ultrasonography in healthy Korean adults were 4.11 mm (95% CI, 4.09–4.14 mm; IQR, 3.85–4.35 mm) and 0.18 (95% CI, 0.18–0.18; IQR, 0.17–0.19), respectively. ONSD exhibited a strong correlation with ETD, but not with sex, height, weight, BMI, and head circumference. Our findings suggest that the ONSD/ETD ratio measured using ultrasonography may be a more accurate and helpful marker of elevated ICP compared with ONSD alone, which is further investigated in the future study.
Disclosure Statement
Dr. D.H. Kim reports no disclosures relevant to the manuscript. Dr. J.S. Jun reports no disclosures relevant to the manuscript. Dr. R. Kim reports no disclosures relevant to the manuscript.
References
Dunn, L. T. Raised intracranial pressure. J Neurol Neurosurg Psychiatry 73, 23–27 (2002).
Juul, N., Morris, G. F., Marshall, S. B. & Marshall, L. F. Intracranial hypertension and cerebral perfusion pressure: influence on neurological deterioration and outcome in severe head injury. The Executive Committee of the International Selfotel Trial. J Neurosurg 92, 1–6 (2000).
Balestreri, M. et al. Impact of intracranial pressure and cerebral perfusion pressure on severe disability and mortality after head injury. Neurocrit Care 4, 8–13 (2006).
Raboel, P. H., Bartek, J. Jr., Andresen, M., Bellander, B. M. & Romner, B. Intracranial Pressure Monitoring: Invasive versus Non-Invasive Methods-A Review. Crit Care Res Pract 2012, 950393 (2012).
Czosnyka, M. & Pickard, J. D. Monitoring and interpretation of intracranial pressure. J Neurol Neurosurg Psychiatry 75, 813–821 (2004).
Kristiansson, H. et al. Measuring elevated intracranial pressure through noninvasive methods: a review of the literature. J Neurosurg Anesthesiol 25, 372–385 (2013).
Newman, W. D., Hollman, A. S., Dutton, G. N. & Carachi, R. Measurement of optic nerve sheath diameter by ultrasound: a means of detecting acute raised intracranial pressure in hydrocephalus. Br J Ophthalmol 86, 1109–1113 (2002).
Bauerle, J., Lochner, P., Kaps, M. & Nedelmann, M. Intra- and interobsever reliability of sonographic assessment of the optic nerve sheath diameter in healthy adults. J Neuroimaging 22, 42–45 (2012).
Lochner, P. et al. Intra- and interobserver reliability of transorbital sonographic assessment of the optic nerve sheath diameter and optic nerve diameter in healthy adults. J Ultrasound 19, 41–45 (2016).
Lee, J. S. et al. Normative measurements of Korean orbital structures revealed by computerized tomography. Acta Ophthalmol Scand 79, 197–200 (2001).
Maude, R. R. et al. Transorbital sonographic evaluation of normal optic nerve sheath diameter in healthy volunteers in Bangladesh. PLoS One 8, e81013 (2013).
Shirodkar, C. G. et al. Optic nerve sheath diameter as a marker for evaluation and prognostication of intracranial pressure in Indian patients: An observational study. Indian J Crit Care Med 18, 728–734 (2014).
Chen, H., Ding, G. S., Zhao, Y. C., Yu, R. G. & Zhou, J. X. Ultrasound measurement of optic nerve diameter and optic nerve sheath diameter in healthy Chinese adults. BMC Neurol 15, 106 (2015).
Wang, L. et al. Ultrasonographic Evaluation of Optic Nerve Sheath Diameter among Healthy Chinese Adults. Ultrasound Med Biol 42, 683–688 (2016).
Karami, M., Shirazinejad, S., Shaygannejad, V. & Shirazinejad, Z. Transocular Doppler and optic nerve sheath diameter monitoring to detect intracranial hypertension. Adv Biomed Res 4, 231 (2015).
Rehman, H., Khan, M. S., Nafees, M., Rehman, A. U. & Habib, A. Optic Nerve Sheath Diameter on Sonography in Idiopathic Intracranial Hypertension Versus Normal. J Coll Physicians Surg Pak 26, 758–760 (2016).
Ballantyne, S. A., O’Neill, G., Hamilton, R. & Hollman, A. S. Observer variation in the sonographic measurement of optic nerve sheath diameter in normal adults. Eur J Ultrasound 15, 145–149 (2002).
Romagnuolo, L., Tayal, V., Tomaszewski, C., Saunders, T. & Norton, H. J. Optic nerve sheath diameter does not change with patient position. Am J Emerg Med 23, 686–688 (2005).
Blehar, D. J., Gaspari, R. J., Montoya, A. & Calderon, R. Correlation of visual axis and coronal axis measurements of the optic nerve sheath diameter. J Ultrasound Med 27, 407–411 (2008).
Shah, S., Kimberly, H., Marill, K. & Noble, V. E. Ultrasound techniques to measure the optic nerve sheath: is a specialized probe necessary? Med Sci Monit 15, MT63–68 (2009).
Skoloudik, D. et al. Distal enlargement of the optic nerve sheath in the hyperacute stage of intracerebral haemorrhage. Br J Ophthalmol 95, 217–221 (2011).
Bauerle, J. et al. Reproducibility and accuracy of optic nerve sheath diameter assessment using ultrasound compared to magnetic resonance imaging. BMC Neurol 13, 187 (2013).
Strapazzon, G. et al. Factors associated with optic nerve sheath diameter during exposure to hypobaric hypoxia. Neurology 82, 1914–1918 (2014).
Lochner, P. et al. Transorbital sonography in acute optic neuritis: a case-control study. AJNR Am J Neuroradiol 35, 2371–2375 (2014).
Amini, R., Stolz, L. A., Patanwala, A. E. & Adhikari, S. Coronal Axis Measurement of the Optic Nerve Sheath Diameter Using a Linear Transducer. J Ultrasound Med 34, 1607–1612 (2015).
Lefferts, W. K., Hughes, W. E. & Heffernan, K. S. Effect of acute high-intensity resistance exercise on optic nerve sheath diameter and ophthalmic artery blood flow pulsatility. J Hum Hypertens 29, 744–748 (2015).
Goeres, P., Zeiler, F. A., Unger, B., Karakitsos, D. & Gillman, L. M. Ultrasound assessment of optic nerve sheath diameter in healthy volunteers. J Crit Care 31, 168–171 (2016).
Zeiler, F. A. et al. A unique method for estimating the reliability learning curve of optic nerve sheath diameter ultrasound measurement. Crit Ultrasound J 8, 9 (2016).
Dinsmore, M., Han, J. S., Fisher, J. A., Chan, V. W. & Venkatraghavan, L. Effects of acute controlled changes in end-tidal carbon dioxide on the diameter of the optic nerve sheath: a transorbital ultrasonographic study in healthy volunteers. Anaesthesia 72, 618–623 (2017).
Soldatos, T. et al. Optic nerve sonography in the diagnostic evaluation of adult brain injury. Crit Care 12, R67 (2008).
Geeraerts, T. et al. Ultrasonography of the optic nerve sheath may be useful for detecting raised intracranial pressure after severe brain injury. Intensive Care Med 33, 1704–1711 (2007).
Geeraerts, T., Merceron, S., Benhamou, D., Vigue, B. & Duranteau, J. Non-invasive assessment of intracranial pressure using ocular sonography in neurocritical care patients. Intensive Care Med 34, 2062–2067 (2008).
Moretti, R. & Pizzi, B. Optic nerve ultrasound for detection of intracranial hypertension in intracranial hemorrhage patients: confirmation of previous findings in a different patient population. J Neurosurg Anesthesiol 21, 16–20 (2009).
Moretti, R., Pizzi, B., Cassini, F. & Vivaldi, N. Reliability of optic nerve ultrasound for the evaluation of patients with spontaneous intracranial hemorrhage. Neurocrit Care 11, 406–410 (2009).
Lee, S. U. et al. Optic nerve sheath diameter threshold by ocular ultrasonography for detection of increased intracranial pressure in Korean adult patients with brain lesions. Medicine (Baltimore) 95, e5061 (2016).
Amini, A. et al. Use of the sonographic diameter of optic nerve sheath to estimate intracranial pressure. Am J Emerg Med 31, 236–239 (2013).
Wang, L. et al. Optimal optic nerve sheath diameter threshold for the identification of elevated opening pressure on lumbar puncture in a Chinese population. PLoS One 10, e0117939 (2015).
Vaiman, M., Gottlieb, P. & Bekerman, I. Quantitative relations between the eyeball, the optic nerve, and the optic canal important for intracranial pressure monitoring. Head Face Med 10, 32 (2014).
Vaiman, M., Sigal, T., Kimiagar, I. & Bekerman, I. Intracranial Pressure Assessment in Traumatic Head Injury with Hemorrhage Via Optic Nerve Sheath Diameter. J Neurotrauma 33, 2147–2153 (2016).
Vaiman, M., Sigal, T., Kimiagar, I. & Bekerman, I. Noninvasive assessment of the intracranial pressure in non-traumatic intracranial hemorrhage. J Clin Neurosci 34, 177–181 (2016).
De Bernardo, M. & Rosa, N. Clarification on Using Ultrasonography to Detect Intracranial Pressure. JAMA Ophthalmol 135, 1004–1005 (2017).
Rosa, N. & De Bernardo, M. Ultrasound assessment of optic nerve sheath diameter in healthy volunteers. J Crit Care 40, 279 (2017).
Iaconetta, G., De Bernardo, M. & Rosa, N. Coronal Axis Measurement of the Optic Nerve Sheath Diameter. J Ultrasound Med 36, 1073 (2017).
Tenuta, M., De Bernardo, M. & Rosa, N. Comments on “Neuromuscular Ultrasonography of Cranial Nerves”. J Clin Neurol 13, 212–213 (2017).
Rosa, N. & De Bernardo, M. Measurement of the Optic Nerve in a Resource-Limited Setting. J Neurosci Rural Pract 8, 310–311 (2017).
Caffery, T. S. & Musso, M. W. Questions regarding the utility of the 30-degree test in measuring optic nerve sheath diameters in ED patients. Am J Emerg Med 33, 595–596 (2015).
Moosajee, M., Restori, M., Acheson, J. & Dahlmann-Noor, A. The cost-effectiveness of different strategies to evaluate optic disk drusen in children. J Aapos 19, 392–393 (2015).
Lagreze, W. A. et al. Morphometry of the retrobulbar human optic nerve: comparison between conventional sonography and ultrafast magnetic resonance sequences. Invest Ophthalmol Vis Sci 48, 1913–1917 (2007).
Acknowledgements
This work was supported by the Korean Military Medical Research Project funded by the ROK Ministry of National Defense (ROK-MND-2017-KMMRP-001).
Author information
Authors and Affiliations
Contributions
Dr. D.H. Kim designed the research, acquired and analyzed the data and drafted the manuscript. Dr. J.S. Jun made critical revisions to the manuscript. Dr. R. Kim designed the research, analyzed the data, and made critical revisions to the manuscript.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kim, D.H., Jun, JS. & Kim, R. Ultrasonographic measurement of the optic nerve sheath diameter and its association with eyeball transverse diameter in 585 healthy volunteers. Sci Rep 7, 15906 (2017). https://doi.org/10.1038/s41598-017-16173-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-16173-z
This article is cited by
-
Evaluation of the effect of fluid management on intracranial pressure in patients undergoing laparoscopic gynaecological surgery based on the ratio of the optic nerve sheath diameter to the eyeball transverse diameter as measured by ultrasound: a randomised controlled trial
BMC Anesthesiology (2024)
-
Optic nerve sheath diameter at high altitude: standardized measures in healthy volunteers
The Ultrasound Journal (2022)
-
Optic nerve sheath diameter is associated with outcome in severe Covid-19
Scientific Reports (2022)
-
The role of sonographic optic nerve sheath diameter measurements in pediatric head trauma
Journal of Ultrasound (2022)
-
The clinical and prognostic values of optic nerve sheath diameter and optic nerve sheath diameter/eyeball transverse diameter ratio in comatose patients with supratentorial lesions
BMC Neurology (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.