Abstract
Dynamic remodelling of the extracellular matrix (ECM) is a key feature of cancer progression. Enzymes that modify the ECM, such as matrix metalloproteinases (MMPs), have long been recognised as important targets of anticancer therapy. Inflammatory cytokines are known to play a key role in regulating protease expression in cancer. Here we describe the identification of gamma-activated site (GAS)-like, signal transducer and activator of transcription (STAT) binding elements (SBEs) within the proximal promoters of the MMP-1 and MMP-3 genes, which in association with AP-1 components (c-Fos or Jun), bind STAT-1 in a homodimer like complex (HDLC). We further demonstrate that MMP expression and binding of this complex to SBEs can either be enhanced by interleukin (IL)-6, or reduced by interferon gamma (IFN-γ), and that IL-6 regulation of MMPs is not STAT-3 dependent. Collectively, this data adds to existing understanding of the mechanism underlying cytokine regulation of MMP expression via STAT-1, and increases our understanding of the links between inflammation and malignancy in colon cancer.
Similar content being viewed by others
Introduction
The cancer microenvironment is made up of many host derived non-tumor cells that play an important role in driving cancer progression by mediating processes as diverse as angiogenesis1, 2, fibrosis3, and metastatic spread4. They do this by producing growth factors and cytokines that drive malignant cancer cell gene expression changes5; principally via phosphorylation (activation) of a family of cytoplasmic effectors, the signal transducers and activators of transcription (STATs)6, 7. Upon activation STATs mobilise to the nucleus and recognise defined sequences within the promoters of target genes, referred to as STAT binding elements (SBEs).
Historically, SBEs were determined by identifying conserved sequences in the promoter regions of interferon (IFN) stimulated genes (ISGs)8, 9. DNA binding sites for STATs in the promoters of genes induced by type I IFN10, type II IFN and interleukin (IL)-6 were further confirmed by electrophoretic mobility shift assays (EMSA)11 and mutational analysis12. In this way, the type I IFN-activated complex (ISGF3) was found to recognise a direct repeat consensus sequence GAAANNGAAANN, referred to as the IFN-stimulated response element (ISRE), and the type II IFN-γ activated complex (aka γ-activated factor) was shown to recognise the sequence TT(C/A)CNN(G/T)AA, referred to as the IFN-γ-activated sequence (GAS). In addition, both STAT-3 homodimers and STAT-1/3 heterodimers are capable of binding to GAS-like sequences, but with subtle differences in affinity12. As a consequence, IL-6 treatment of a responsive tissue will lead to phosphorylation of either STAT-1 and/or STAT-3, which in turn bind to SBEs in either a homodimer, or heterodimeric formation13. While treatment with IFN-γ leads to activation of GAS-like SBEs in ISGs, through the activation and binding of homodimers containing phosphorylated STAT-1 (P-STAT-1)14, 15. Notably, unphosphorylated STATs (U-STATs) are also known to play various roles in regulating gene expression, although the mechanism for this remains relatively undefined16,17,18.
The Matrix Metalloproteinase (MMP) family have a diverse range of substrate specificities related to remodelling of the extracellular matrix (ECM). Aberrant MMP activity has been implicated in a range of malignancies, such as those of the colon and breast19, 20, where they act to promote malignancy by degrading basement membranes, and by activating ECM-bound growth factors and cytokines21. MMP family members have been identified as targets of inflammatory cytokinemediated gene regulation via STAT signaling22, 23. These include, Collagenase I (MMP-1), which is proposed to be regulated by Oncostatin M (OSM) via STAT-3 binding to an SBE located in a region of the human gene promoter proximal to the start site of transcription24, 25, as well as MMP-3 (Stromelysin), which appears to be regulated by IL-6 via a distal SBE26, 27. Gelatinase A (MMP-2) and Gelatinase B (MMP-9) gene activity are also thought to be regulated by cytokines via SBEs28.
In this study, we present data showing that IL-6 regulates MMP expression via proximal GAS-like SBEs, and that IL-6 treatment leads to binding of a novel complex, which contains both STAT-1 and components of activated protein (AP)-1, but not STAT-3. Notably, ablation or inhibition of STAT-1, not STAT-3 was found to inhibit IL-6-mediated induction of MMPs. This work complements previous studies that show a role for STAT-3 in maximal MMP induction via IL-629, 30, by suggesting that STAT-3 functionality is not a precondition for IL-6-mediated MMP expression. This finding also provides a novel insight into inflammatory cytokine signaling and represents an important consideration for the development of anti-cancer drugs targeting STAT-mediated cytokine signaling31.
Results
Protease and inflammatory cytokine signaling in colon cancer
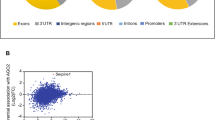
Patient colon tumor tissue and matched normal mucosa were collected and analyzed by specific expression analysis (Fig. 1A and Supplementary Table S1). Genes were chosen based on previous association with colorectal cancer, and included inflammatory factors as well as oncogenes. While mRNA from oncogenes with known regulatory links such as c-MYC/STAT-3 and c-MYC/CDK4 showed co-regulation of expression, analysis also revealed significant correlation in the mRNA levels of IL-6 and MMPs: MMP-1: P = 0.02 & MMP-3: P < 0.01, with generally higher levels in tumor tissue compared with normal mucosa (Supplementary Fig. S1A). Notably, specific comparison of gene expression revealed reduced levels of MMP and IL-6 mRNA in Dukes’ C compared with Dukes’ B tumors, suggesting that co-regulation was also linked to clinical pathology (P < 0.05) (Fig. 1B)32. To examine this link further, levels of known downstream targets of IL-6 such as BCL-2, STAT-3 and BCLXL 33, as well as MMP-1 and MMP-3, were then measured following treatment of colon cancer cell lines with IL-6. Notably, MMP-1 (~250-fold, P < 0.01) and IL-6 responsive BCLXL mRNAs were greatly increased after treatment with IL-6 (18 h) in SW480 colon cancer cells under conditions of high (10%) serum (Fig. 1C). In the presence of low (1%) serum, MMP-1 and MMP-3 mRNA expression remained inducible by IL-6, although the degree of induction was markedly reduced (~7-fold, P < 0.05). Similar results were obtained for MMP-3, and the IL-6 target gene, BCL-2 (not shown). Furthermore, both LS174T and SW480 colon cancer cell lines were confirmed to be responsive to IL-6: evidenced by the induction of IL-6 responsive genes, and expression of IL-6 receptors (gp130 & IL-6R). Notably, although all cell lines examined constitutively expressed LIF, as well as mRNA for both IL-6 receptors, IL-6 expression was found to be below the level of detection (Supplementary Fig. S1B). In addition, the HT29 cell line, which was the only cell line shown to express mRNA for the LIF receptor (LIFR), also showed an increase in MMP-1 levels after LIF treatment (5.6-fold, P < 0.02). The presence of a previously reported GAS-like SBE in the proximal promoter of MMP-1 (Supplementary Tables S2A)25, 34,35,36,37,38,39,40,41,42,43 also suggested that MMP-1 might respond positively to IFN-γ treatment. However, although all the tested colon cancer cell lines were responsive to IFN-γ, as revealed by induction of ISGs14, 15 such as STAT-1, STAT-3, interferon responsive factor (IRF-1), and BCLXL, unexpectedly MMP-1 mRNA levels were reduced following IFN-γ treatment (18 h) (Supplementary Fig. S1C).
Comparative expression analysis. (A) Heat map showing relative fold differences in gene expression between tumor-tissue and patient matched normal mucosa. Clustering was based on nearest neighbor hierarchy analysis. Where expression was below the level of sensitivity for detection in either the normal mucosa or tumor, values were assigned numerically reflecting the upper and lower bounds of the data set (no expression in control, 800; no expression in tumor, −800). Data was analyzed by Spearman’s ρ correlation analysis (α = 0.05). Abbreviations for anatomical location: Cecum [C]; Colon Ascending [CA]; Colon Transverse [CT]; Colon Descending [CD]; and Sigmoid Colon [S]; for Dukes’ staging [B & C]; for differentiation: Low [L]; Medium High to Low [MH-L]; Medium High [MH]; and High [H]; for ulceration: Ulcerous [U]; Polypous [P]; Mixed Polypous-Ulcerous [P-U]. (B) Results of Q-PCR analysis showing differences in mRNA levels for MMP-1, MMP-3, MMP-7 and IL-6 between Dukes’ B and Dukes’ C tumors. Data is represented as box plots with median (thick line), first and third quartiles (boxed), upper and lower values (whiskers) and outliers (◊), and was analyzed by Mann Whitney U (α = 0.05, *P < 0.05). (C) Results of Q-PCR analysis following IL-6 treatment of SW480 colorectal cancer cells, showing significant up-regulation of MMP-1 mRNA. Notably, induction was enhanced under high (10%) serum conditions (Left), compared with low serum (1%) (Right). Similar results were obtained in other cell lines, including LS174T (not shown). Also shown, the effects of IL-6 on the known IL-6 target gene, BCLXL. Similar results were obtained for BCL-2 and STAT-3 (not shown). Each experiment was repeated showing similar results, and data represented as mean Log2(Fold) ± SEM, and was analyzed by Independent t test (α = 0.05, **P < 0.01).
Characterization of a non-canonical GAS-like SBE in the MMP-1 promoter
To further characterize the non-canonical GAS-like SBE element the MMP-1 promoter sequences from human, mouse, dog, chimpanzee and rat were examined. Alignment of these sequences showed that the GAS-like SBE present in the proximal human MMP-1 promoter25, as well as the nearby AP-1 binding element44 were highly conserved (Supplementary Fig. S2). We next cloned a 549 bp region of the MMP-1 promoter containing this GAS-like SBE, and subjected the construct to dual reporter luciferase analysis (Fig. 2A)45. The results of this analysis confirmed that the proximal MMP-1 promoter containing the GAS-like SBE was inducible by IL-6 in SW480 (1.2-fold) colon cancer cells, under conditions of low (1%) serum. This correlated with results seen in the cytokine responsive HepG2 liver cancer cell line, which showed a 3-fold induction. Next, to replicate the effects of serum response to MMP induction with IL-6 (Figs 1C and S3A) the activator of AP-1, phorbol myristyl acetate (PMA) was also added46. In this instance, addition of PMA provided significantly greater MMP-1 promoter activity than addition of IL-6 alone (Fig. 2A); a result that is consistent with PMA promoting the response of MMP-1 to IL-6 by co-stimulating AP-1 transcriptional activity.
Reporter analysis of human MMP SBEs. (A) Schematic representation of the SBE/AP-1 region from the MMP-1 promoter inserted into the pGL3-basic luciferase reporter vector (Left). Also shown, results of reporter activity in SW480 cells, transfected with the MMP-1 promoter (549 bp) reporter following treatment with either Interleukin (IL)-6 alone, or IL-6 plus phorbol myristyl acetate (PMA); as well as results of reporter activation in cytokine responsive liver cancer (HepG2) cells, treated with IL-6 alone or IL-6 plus PMA (5 mM). Data is represented as mean relative luminescence Units (RLU) ±SEM. (B) Left, Schematic of human MMP-3 promoter constructs used for dual reporter analysis, including the positions of SBEs and AP-1 binding elements. ‘*’Indicates mutations created in the SBEI and SBEII sites. Right, IL-6 induced promoter activity in HepG2 cells for each construct. Data is represented as mean fold induction ± SEM. (C) SW480 and HepG2 cells transfected with the proximal MMP-3 promoter were treated with: (i) IL-6 and soluble IL-6 receptor (IL-6R) (both 10 ng/ml, 18 h); (ii) IFN-γ (1000 U/ml, 18 h) alone; or (iii) with IFN-γ, 2 h before adding IL-6 and sIL-6R. Data is represented as mean RLU ± SEM. (D) Luciferase activity in HepG2 cells produced from the full length 607 bp proximal region (Left), and the shortest SBE I/II/AP-1 (Right) MMP-3 gene promoter construct. Shown, the cumulative effect of PMA (5 nM) plus IL-6 (10 ng/ml), versus IL-6 alone. Data is represented as mean RLU ± SEM. For (A–D), experiments were repeated showing similar results and data was analyzed by Independent t test (α = 0.05; *P < 0.05, **P < 0.01).
Characterization of novel SBEs in the human MMP-3 proximal promoter
Given the presence of an IL-6/cytokine responsive SBE in MMP-1 (Fig. 2A)25, the proximal promoter of MMP-3 was examined to determine if similar elements could also explain MMP-3 induction by IL-6. In this way, a spatially conserved region near the transcription start site was found to contain a putative GAS-like SBE (SBE I) in close proximity to a canonical AP-1 binding site. In addition, four other SBE-like sequences (SBEII-V) were identified upstream of the SBE/AP-1 motif in the MMP-3 promoter (Supplementary Fig. S2 and Supplementary Tables S2B,C). Notably, no SBEII-V matching sequences were identified in the MMP-1 proximal promoter. Next, to determine whether these novel non-canonical MMP-3 SBEs were responsive to IL-6 a 607 bp fragment, as well as successively smaller segments, were subjected to luciferase reporter analysis (Fig. 2B). Notably, a significant response to IL-6 treatment was identified in HepG2 cells transfected with the 607 bp region of the MMP-3 promoter that contained both SBEI/AP-1 and SBEII-V elements (3.4-fold). Mutation of both SBE I/II sites in the shortest fragment did not change the magnitude of induction by IL-6. However, extending the promoter length to include the other SBE sites [particularly SBE IV (−261)] showed a cumulative and positive effect on IL-6-induced luciferase activity. Activation by IL-6 of the full length construct containing all proximal SBEs was confirmed in SW480 cells, in the presence and absence of sIL-6R: added to ensure maximal induction (Fig. 2C). Significantly, IFN-γ treatment (18 h) reduced MMP-3 607 bp promoter activity in SW480 cells, while pre-treating cells for 2 h with IFN-γ before adding IL-6 then inhibited IL-6-induced promoter activation (Fig. 2C). Consistent with the supportive role played by AP-1 in IL-6-mediated MMP-1 expression, PMA also greatly enhanced the IL-6-mediated activation of both the 607 bp (6.4-fold), and the shorter SBE I/II/AP-1 (1.8-fold) MMP-3 promoter fragments (Fig. 2D). Notably, addition of sIL-6R did not significantly alter IL-6 induction of MMP-3 (607 bp) promoter (Supplementary Fig. S3B).
Constitutive and enhanced binding of a novel complex containing STAT-1 and AP-1 components to the MMP-3 proximal promoter
To examine the mechanism for IL-6 activation of MMP-1 and MMP-3, oligonucleotides containing the AP-1-proximal SBE from the MMP-1 and MMP-3 promoters (SBE/AP-1 & SBE I/AP-1, respectively) were subjected to EMSA to investigate direct DNA binding. As controls for STAT-binding, extracts from IFN-γ and IL-6-treated cells were incubated with oligonucleotides containing the sis-inducible element (SIE) from the c-fos gene (m67 mutation) (Figs 3A and S4A)47. Notably, both untreated and IL-6-treated nuclear extracts probed with MMP-1 and MMP-3 oligonucleotides produced a single band with similar mobility to the SIE-bound STAT-1 homodimer. This homodimer-like complex (HDLC) was also found to bind to the novel MMP-3 SBEs (SBE II/III & SBE IV) (Fig. 3B). The abundance of the HDLC bound to SBE II/III was increased in IL-6-treated cells, and binding to SBE I/AP-1 was enhanced by PMA treatment. Furthermore, binding of the HDLC to the MMP-3 (SBE I/AP-1) and MMP-3 (SBE IV) sites became noticeably reduced following IFN-γ treatment, and was blocked entirely by an anti-STAT-1 antibody, but not anti-STAT-3 (Fig. 3C), or anti-STAT-5 antibodies (Supplementary Fig. S4B).
Identification of a HDLC binding non-canonical SBEs in MMP-1 and MMP-3 promoters. (A) Extracts from SW480 or HepG2 cells treated with IL-6 (50 ng/ml, 5 min) or IFN-γ (1000 U/ml, 1 h) were probed with the sis-inducible element (SIE) oligonucleotide. Arrows indicate the STAT-3 homodimer, the STAT-1/STAT-3 heterodimer and the STAT-1 homodimer. Also shown is binding of a novel STAT-1 HDLC constitutively to the MMP-1 SBE/AP-1 and MMP-3 SBE I/AP-1 probes. (B) EMSA showing a similar STAT-1 HDLC constitutively binding to the MMP-3 SBE II/III and MMP-3 SBE IV probes using extracts from HepG2 cells treated with PMA (100 nM, 90 min), IL-6 (50 ng/ml, 5 min) and IFN-γ (1000 U/ml, 60 min). (C) EMSA in the presence of anti-STAT-1, anti-pan-Fos and anti-c-Jun antibodies, respectively, as indicated. (D) EMSA of MMP1 (SBE) and (SBE/AP-1), MMP-3 (SBEI) and (SBE I/AP-1) probes using HepG2 cell extracts in the presence and absence of 1 μg poly-dI:dC showing dependence of STAT-1 HDLC binding on the AP-1 site. For (A–D), experiments were repeated showing similar results.
To determine whether AP-1 components were present in the HDLC, extracts were then incubated with either anti-Fos or anti-Jun antibodies. Notably, anti-c-Jun antibody reduced complex binding to the MMP-1 (SBE/AP-1) probe, and a pan-Fos antibody super-shifted the complex bound to the MMP-3 (SBE I/AP-1) probe. In addition, binding of the complex to the MMP-3 (SBE II/III) probe was reduced by anti-c-Jun antibody, suggesting that the HDLC also contained AP-1 (Fos/Jun) components. Notably, in the presence of the non-specific competitor DNA, poly dI:dC (1 μg), binding of the HDLC was only found to occur when the AP-1 binding element was also present (Fig. 3D)48. The presence of STAT-1 and AP-1 components binding proximal promoter MMP SBEs was confirmed by quantitative chromatin immunoprecipitation (ChIP) analysis (Supplementary Fig. S5).
STAT-1 not STAT-3 is required for IL-6-mediated induction of MMP expression
Given the positive response of the MMP promoter to IL-6 treatment, and the binding of STAT-1 to putative SBEs identified in both the MMP-1 and MMP-3 promoters, we next sought to determine whether STAT-1 was required for IL-6 induced MMP expression. Firstly, SW480 cells were stably infected with a lentiviral construct containing shRNA targeting STAT-1 (−838)49, 50. Control cells were prepared by infecting SW480 cells with a scrambled shRNA construct (Fig. 4A). Notably, STAT-1 knockdown (KD) SW480 cells showed an inability to induce MMP-1 or MMP-3 mRNA following treatment with hyper-IL-651; the recombinant form of IL-6, which contains both IL-6 and soluble IL-6 receptor, to ensure maximum activation (Fig. 4A). This contrasted with parental SW480 cells which showed a 3-fold (P = 0.0002) and 2.3-fold (P = 0.008) increase in MMP-1 and MMP-3 mRNA levels, respectively. Scrambled controls showed similar levels of hyper-IL-6-mediated MMP-1 and MMP-3 induction to that observed in parental controls (P = 0.032 and P = 0.01, respectively). This result is consistent with a requirement for STAT-1 in the IL-6-mediated activation of MMP-1 and MMP-3 genes in colon cancer.
STAT-1 is required for maximal IL-6 induction of MMPs. (A) Analysis of IL-6-induced MMP gene expression in STAT-1 knockdown (KD) human colon cancer cells. Upper, Western blot analysis of SW480 STAT-1 KD cells compared with controls, and probed with anti-STAT-1 and anti-α-tubulin antibodies. Lower, Wild-type SW480 and SW480 STAT-1 short hairpin shRNA KD cells treated with hyper-IL-6 (20 ng/ml, 18 h) a fusion protein comprising IL-6 and the soluble IL-6 receptor α chain, under conditions of low serum (1.5%). STAT-1 KD has a significantly negative effect on IL-6 induction of MMP-1 and MMP-3. Data is represented as mean Log2(Fold) ± S.E.M., for the difference in mRNA levels between treated and untreated cells (ΔCTuntreated−ΔCTtreated), analyzed by independent t test (α = 0.05; **P < 0.01, *P < 0.02).’ (B) Northern Blot analyses of human MMP gene expression in response to IL-6 in the DLD1 derived STAT-3 null A4 colon cancer cell line versus STAT-3 reconstituted A4 cells. Human colon cancer cells were treated with IL-6 (200 ng/ml), and soluble IL-6R (250 ng/ml) for up to 24 h. Shown, parallel induction of MMP mRNA in response to IL-6, in both A4 cells reconstituted with STAT-3 and STAT-3 null A4 cells. (C) No enhanced induction of MMP-1, or MMP-3 mRNA levels was observed in STAT hyper-activated gp130Y757F/Y757F (FF) animals following injection of IL-6 (after 90 min), compared with wild-type control animals (n = 5). Also shown, up-regulation of STAT-3 mRNA, as well as decreased levels of MMP-3 mRNA following IL-6 treatment in FF animals compared with controls. Data represented as Log2(Fold) ± S.E.M. and analyzed by independent t test (α = 0.05, *P < 0.05). (D) Results of dual-luciferase reporter analysis showing no significant effect on IL-6 (50 ng/ml) and cpt-cAMP (300 μM) induction of MMP-1 and MMP-3 full-length promoter constructs pre-treated (1 h) with the STAT-3 inhibitor, Stattic®, compared with c-Jun control construct. Constructs were transduced into HepG2 cells and treatment conducted in the presence of 1% serum. Data is represented as mean relative luminescence units (RLU) ± SEM. and analyzed by independent t test (α = 0.05, **P < 0.01). For (A–D), experiments were repeated showing similar results.
Although direct binding studies did not suggest a role for STAT-3 in MMP promoter activation we next examined the requirement, if any, for STAT-3 in IL-6 activation of MMP-1 and MMP-3 expression. To do this we first compared IL-6 treated DLD1 derived STAT-3 null A4 colon cancer cells versus STAT-3 reconstituted A4 cells52. In this case, the absence of STAT-3 had no obvious effect on IL-6 induction of MMP-1, MMP-3, MMP-19 or MMP-28 over a 24 hour time-course (Fig. 4B). We next examined MMP expression in the gp130 mouse model, which shows hyper-activation of both STAT-1 and STAT-3 in response to IL-653. Notably, following direct injection of IL-6 into the livers of these animals no significantly enhanced expression was identified in MMP expression in the tissues of STAT-3 hyper-activated homozygous (FF) animals when compared with wild-type controls (Fig. 4C).
The lack of dependence on STAT-3 for IL-6-induced MMP gene activation was further supported by experiments using the small molecule inhibitor of STAT-3 (Stattic®)54. Administration of Stattic® showed no significant effect on IL-6-induction of MMP-1 and MMP-3 proximal promoter constructs, compared with the STAT-3 inducible c-Jun control (Figs 4D and S6).
Discussion
In this study we have used comparative gene expression analysis and promoter mapping to demonstrate a direct link between IL-6 and MMP expression in colon cancer, via STAT-1 and novel non-canonical SBEs identified in the MMP-1 and MMP-3 proximal promoters. Firstly, in a patient matched study comparing tumor tissue with mucosa we determined that: (i) expression of cytokines (IL-6 and LIF) clustered with proteases, including MMP-1, MMP-3 and MMP-7; (ii) correlation was generally linked to pathophysiology of the tumor with higher levels in more restricted Duke’s B tumors compared with invasive Duke’s C tumor; and (iii) MMP-1 and MMP-3 were co-regulated with previously identified downstream targets of IL-6 in colon cancer cell lines (Fig. 1). While the reason for decreased expression in Duke’s C tumors is unclear the close correlation between IL-6 and MMP levels in vivo and in vitro, as well as the presence of potentially IL-6 responsive SBEs in the MMP promoters, did suggest a high degree of co-regulation between IL-6 and MMPs, which we examined further.
Notably, while known ISGs were positively regulated by IFN-γ in colon cancer cell lines, MMP-1, which also contains a GAS-like SBE in its proximal promoter, was down-regulated by IFN-γ. At least one previous report has shown that this element is responsive to IL-6/OSM/LIF25. Through reporter analysis we confirmed that this proximal SBE/AP-1 element was responsive to IL-6. Interestingly, MMP-3, which is also responsive to IL-6 and co-regulated with IL-6 in our study, has previously been shown to be regulated via STAT-3 through distal promoter elements26. After analysis of the proximal promoter of MMP-3, we identified five new non-canonical SBEs in the MMP-3 promoter, including a tandem SBE/AP-1 element, which were also responsive to IL-6 (Fig. 2). When direct binding studies were conducted they provided further evidence for the constitutive and enhanced binding of a protein complex (HDLC) to these SBEs, which shifted to the same size as the classical IFN-γ activated STAT-1 homodimer14, 15. HDLCs bound to these elements were found to contain STAT-1 protein, and either Fos (MMP-3) or c-Jun (MMP-1), and were negatively regulated by IFN-γ (Fig. 3). Notably, sIL-6R, or the hyper-IL-6 protein did not significantly alter IL-6 induction of MMP promoter elements (Figs 2C and S3B), or HDLC binding (Supplementary Fig. S4A), suggesting that endogenous sIL-6R was sufficient to ensure maximum promoter activation in response to IL-6.
Through the use of shRNAi knockdown we have also showed that STAT-1 is required for maximal activation of MMP-1 and MMP-3 in response to IL-6, while knockout of STAT-3 in a colon cancer cell line had little or no effect on IL-6 induction of MMP-1 and MMP-3. We also demonstrated that neither hyperactivation of STAT-3 in the gp130 mice, or inhibition of STAT-3 protein using the small molecule inhibitor Stattic®, did not significantly affect IL-6 activation of MMP-1 and MMP-3. These results collectively suggest that STAT-1, and not STAT-3, is required for IL-6 activation of MMP gene expression via proximal promoter SBEs (Fig. 4).
The discovery of a STAT-1 containing complex that cooperates with AP-1 to regulate MMPs through GAS-like SBEs in the MMP-1 and MMP-3 proximal promoters is novel. However, similar promoter regulatory complexes have previously been described including: (i) an IFN-γ-inducible complex comprising STAT-1 and c-Fos that binds to adjacent GAS and AP-1 binding elements in the human Nitric Oxide Synthase (NOS) 2 promoter55, and (ii) an IL-12 and IL-18 responsive c-Jun-STAT-4 complex that binds to an AP-1 binding element in the IFN-γ gene (IFNG) promoter56. Interestingly, in this last case only c-Jun appears to contact DNA directly, and promoter binding is dependent on the presence of STAT-4. In our study, while c-Fos was constitutively bound to the MMP-3 promoter prior to the addition of IL-6/PMA, it may be that PMA treatment also induced more STAT-1 to bind, given that PMA has previously been shown to activate JAK/STAT signaling57. We also found that STAT-1 binding to the MMP-3 proximal promoter was reduced by treatment of cells with IFN-γ.
Previous studies have also shown suppression of MMPs in response to IFN-γ, such as MMP-9, which like MMP-1 and MMP-3, also contains AP-1 sites (two) and putative SBEs58,59,60, and has been shown to be repressed following IFN-γ treatment in astrocytes, fibrosarcomas, and monocytes. In all of these cases, loss of MMP gene activity following IFN-γ treatment is likely to relate to changes in the phosphorylation status of STAT-1 post-activation, and suggests a possible novel mechanism of cytokine regulation of gene expression. In contrast to IFN-γ responsive genes such as IRF-1 15, which contain canonical GAS elements activated by P-STAT-1, STAT-1 regulation of MMP SBEs does not appear to be dependent on IFN-γ-mediated tyrosine phosphorylation. Instead, activation of STAT-1 by IFN-γ may lead to dimerization of STAT-1, a breakup of the U-STAT-1/AP-1 complex bound to the GAS-like SBEs present in the MMP-1 and MMP-3 promoters, as well as a reduction in gene promoter activity (Fig. 5). In this way, STAT-1 hyperactivation in the gp130 (FF) animals, which leads to a decrease in MMP-3 levels in response to IL-6 (Fig. 4C), may also be explained by reduced availability of U-STAT-1 for binding to the HDLC.
Proposed model for the regulation of MMPs by IL-6/PMA and IFN-γ. Fos/Jun and non-phosphorylated STAT-1 bind constitutively to AP-1 and SBEs elements in the MMP-1 and MMP-3 proximal promoters, maintaining a basal level of gene expression (A). In the presence of IL-6 or PMA, MMP expression is enhanced (green arrow) (B). In response to IFN-γ, STAT-1 is phosphorylated, increasing its affinity for binding to GAS elements in the promoters of IFN-γ responsive genes, displacing STAT-1 from the HDLCs in the MMP gene promoters, resulting in a reduction in expression of these genes (C).
Such a mechanism for explaining promoter regulation by STATs is supported by previously published data. Indeed it has been shown that STAT-1 exists in different homodimeric confirmations depending on whether, or not, it is tyrosine phosphorylated61, and unphosphorylated homodimer (U-STAT-1) differs in binding specificity (and genes induced) to those of the tyrosine phosphorylated P-STAT-1 homodimeric form activated by IFNs62. The fact that IFN treatment leads to a reduction in MMP expression and promoter activity, and that P-STAT-1 is not a significant contributor to IL-6 induced MMP expression in the hyperactivated model (FF) of STAT signalling (Fig. 4C), strongly suggests that U-STAT-1 plays an important role in contributing to the formation of the HDLC and regulation of noncanonical SBEs present in the proximal MMP promoters.
While the involvement of U-STAT-1 in regulating gene expression has been shown by others16, 62, 63, to the best of our knowledge this is the first report elucidating a novel STAT-1 binding complex to noncanonical SBEs and whose binding is constitutive, enhanced by IL-6, and inhibited by IFN-γ treatment. Furthermore, sensitivity to the presence of poly-dI:dC displayed by STAT-1 HDLC binding to the SBEs without the AP-1 motif suggests that formation of this complex is not robust and requires AP-1 components to facilitate STAT-1 binding. Intriguingly, despite previous reports showing primarily STAT-1, but also STAT-3 binding to the AP-1 proximal SBE element in the MMP-1 promoter25, as well as STAT-3 regulating MMP-3 via distal promoter elements26, we did not observe any STAT-3 dimer bands binding the MMP-3 SBE/AP-1 motif, and MMP induction by IL-6 was not significantly affected in Stat-3null cells. All of this evidence is consistent, and indicates that STAT-3 activation is not a precondition for IL-6 induction of either MMP-1 and/or MMP-3.
Conclusion
In this study, we present data from comparative biopsy analysis, confirming co-regulation of MMPs with inflammatory cytokines, such as IL-6, in colon cancer. We also show the results of the analysis of novel GAS-like SBEs in the proximal promoter of the MMP-3 gene, which bear sequence similarity to an element previously identified within the MMP-1 promoter25. Similar to the MMP-1 SBE, the proximal MMP-3 GAS-like SBEs bound a complex (HDLC) that contained both STAT-1, and components of AP-1 (c-Fos/Jun), but not STAT-3. Furthermore, while STAT-3 may play a role in maximal induction of MMP-3, we show that ablation or inhibition of STAT-3 does not substantially affect the IL-6 induction of MMPs. Instead, IL-6-mediated induction of MMPs was substantially affected by knockdown of STAT-1. Uniquely, for GAS-like SBEs, we also provide evidence for negative regulation of MMPs by IFN-γ. Collectively, the results suggest a mechanism of regulation of MMPs by IL-6 that relies on enhancing STAT-1 binding in a HDLC with AP-1 components, and which is negatively regulated following activation/phosphorylation of STAT-1 by IFN-γ. This does not contradict previous work26, 29, which has shown a requirement for STAT-3 activation of distal SBEs in maximal induction of MMPs by IL-6. Instead, functional STAT-3 may not be a precondition for IL-6-mediated MMP induction. This has important clinical implications, especially for the development of drugs (eg. Stattic®) that target STAT-3 activation and the expression of STAT-3 target genes31. Our findings also provide evidence to support future studies designed to more fully define the role of U-STAT-1 in inflammatory cytokine-mediated gene regulation and cancer malignancy.
Methods
Cell lines and Treatment
The human colorectal carcinoma cell lines HT29, SW480, LISP-1, LIM1215, HCT116, and LS174T, as well as the hepatocyte-derived HepG2 cell line, were obtained from the American Type Culture Collection (ATCC) (Manassas, VA, USA). Cells were grown in either RPMI 1640 (Sigma-Aldrich, St. Louis, MO) or DMEM (Sigma-Aldrich) under either standard serum [10% fetal calf serum (FCS), 5% CO2] or low serum (<1% FCS) growth conditions. Human DLD1 colon carcinoma cells used to derive a Stat-3null sub-line were also obtained from the ATCC and were grown in McCoy’s 5A medium with L-glutamine (Hyclone, Logan, UT). Unless otherwise indicated, media were supplemented with 10% FCS, penicillin (100 U/ml), and streptomycin (100 μg/ml) (Gibco-BRL, Carlsbad, CA). Cytokines used in this study include human type-I IFN (-β) (Biogen, Cambridge, MA), and type-II (-γ) (Hoffman-La Roche, Basel, Switzerland), as well as IL-6 (Peprotech, Rocky Hill, NJ), hyper-IL-6 (kind gift from Prof. Stefan Rose-John) and Leukaemia Inhibitory Factor (LIF) (Peprotech). Notably, while all cell lines were found to express gp-130 and IL-6 receptor, both of which are required for maximal induction of IL-6 target genes, addition of sIL-6R, and or the recombinant hyper-IL6 (a fusion of IL-6 & IL-6R) was used to ensure maximal IL-6/STAT activation51, and was used as indicated. Cells were also treated with the activator of AP-1, phorbol 12-myristate 13-acetate (PMA) (Sigma-Aldrich), at indicated concentrations.
Patient samples
Tumor tissue and distal normal colonic mucosa from the primary surgical margins were obtained from patients who had undergone corrective surgery. The mean patient age was 74. All procedures were conducted under the guidelines outlined by the National Health & Medical Research Council, Australia, and approved by Linkoping University Hospital (Sweden), University of NSW (Australia) and Griffith University (Australia), Human Research Ethics Committees. Written informed consent was obtained from all patients and the healthy volunteer. Patients were chosen based on their clinical diagnosis.
Upon collection each sample was snap frozen and a representative region embedded in paraffin for histopathological examination. Samples were first assessed by PCR-single stranded conformational analysis (SSCA) and direct sequencing for point mutation analysis64. Total RNA was isolated (RNeasy® Mini Kit, Qiagen, CA) and first strand synthesis carried out using 1–5 μg of total RNA, SuperscriptTM (Invitrogen Corp., San Diego, CA). All reactions contained 1 × SYBR Green I mix (ABI) and custom primers (Supplementary Table 1). 18SrRNA was used as a normalization reference and data analyzed, as previously described65.
Dual-reporter assays
Transfections were performed using previously published methods44. Cultures were grown to subconfluence in antibiotic-free media (10% FCS). Each transfection contained a pGL3-MMP promoter construct (1 μg), 1.5 μl jetPEITM reagent (Polyplus Transfection, Illkirch, France), and 10 ng phRL-SV40, encoding the internal standard Renilla luciferase. Following transfection, cells were treated with: IL-6, soluble IL-6Rα (Peprotech), PMA and/or human IFN-γ. Luciferase activity was recorded using the BMG FLUOstarOPTIMA microplate reader (BMG Labtech, Melbourne, Australia) using Renilla luciferase as a normalization standard.
Direct DNA binding (EMSA) studies
Nuclear extracts were prepared using the detergent-free procedure described previously66. Oligonucleotide (Supplementary Table 3) were end labeled using a dNTP mix containing [α-32P] dCTP (Amersham, Piscataway, NJ). Nuclear extracts (5 μg) were incubated (20 min, RT) with probes in binding buffer (20 mM HEPES pH 7.8, 1 mM MgCl2, 0.5 mM DTT, KCl [40–80 mM] & 5% glycerol), and protein/DNA complexes resolved by PAGE (5% glycerol). Antibodies used for supershifting included anti-STAT-1 (polyclonal; #9172; Cell Signaling Technology Inc, Beverly, MA), anti-STAT-3 (polyclonal; #9132; Cell Signaling Technology Inc), anti-STAT-5 (polyclonal; #9310; Cell Signaling Technology Inc), anti-c-Jun (polyclonal; #9162; Cell Signaling Technology Inc) and anti-pan-Fos (K-25; #sc-253X; Santa Cruz Biotech Inc, Santa Cruz, CA).
Production of STAT-1 knockdown SW480 colon cancer cell line
293T cells were transfected with 15 μg pCMV-dR8.74 (gag-pol), 6 μg pMD-2G (VSV-G env) and 20 μg pLKO.1-puro containing STAT-1 (-838) or scrambled short hairpin RNA (shRNA). Viral supernatants were harvested after 48 h and concentrated by centrifugation. SW480 cells were infected with lentivirus particles in the presence of 8 μg/ml polybrene and selected with 2 μg/ml puromycin. Scrambled knockdown cells were pooled while STAT-1 knockdown cells were clonally selected. Antibodies used for western blotting included anti-STAT-1 (monoclonal, 9H2; #9176; Cell Signaling Technology Inc) and anti-α-tubulin (monoclonal, DM1A; #T9026; Sigma-Aldrich).
Data analysis
All experiments were repeated at least once, and included at least three to five experimental replicates for purposes of statistical analysis. Unless otherwise stated data was analyzed using GraphPad Prism™. The differences between control and test data was determined by an independent samples t test (α = 0.05). Hierarchical clustering was carried out using the nearest-neighbour method. Either mean fold or median (box plots) have been used to represent relative difference in gene expression between tumor and normal mucosa 2(ΔCTcontrol−ΔCTtest), and for promoter response to cytokine treatment (RLUtreated/RLUuntreated).
Data Availability
All data generated or analysed during this study are included in this published article (and its Supplementary Information files), or available from the corresponding author on reasonable request.
References
Gao, D. et al. Endothelial progenitor cells control the angiogenic switch in mouse lung metastasis. Science 319, 195–198 (2008).
Sax, M. J. et al. Cancer cell CCL5 mediates bone marrow independent angiogenesis in breast cancer. Oncotarget 7, 85347–49 (2016).
Zeisberg, M. & Kalluri, R. Cellular mechanisms of tissue fibrosis. 1. Common and organ-specific mechanisms associated with tissue fibrosis. Am J Physiol Cell Physiol 304, C216–25 (2013).
Quail, D. F. & Joyce, J. A. Microenvironmental regulation of tumor progression and metastasis. Nat Med 19, 1423–37 (2013).
Ricciardi, M. et al. Epithelial-to-mesenchymal transition (EMT) induced by inflammatory priming elicits mesenchymal stromal cell-like immune-modulatory properties in cancer cells. Br J Cancer 112, 1067–75 (2015).
Zhao, G. et al. IL-6 mediates the signal pathway of JAK-STAT3-VEGF-C promoting growth, invasion and lymphangiogenesis in gastric cancer. Oncol Rep 35, 1787–95 (2016).
Bharti, R., Dey, G. & Mandal, M. Cancer development, chemoresistance, epithelial to mesenchymal transition and stem cells: A snapshot of IL-6 mediated involvement. Cancer Lett 375, 51–61 (2016).
Friedman, R. L. & Stark, G. R. alpha-Interferon-induced transcription of HLA and metallothionein genes containing homologous upstream sequences. Nature 314, 637–9 (1985).
Porter, A. C., Chernajovsky, Y., Dale, T. C., Gilbert, C. S. & Stark, G. R. et al. Interferon response element of the human gene 6–16. Embo J 7, 85–92 (1988).
Kessler, D. S., Levy, D. E. & Darnell, J. E. Jr. Two interferon-induced nuclear factors bind a single promoter element in interferon-stimulated genes. Proc Natl Acad Sci USA 85, 8521–5 (1988).
Levy, D. E., Kessler, D. S., Pine, R., Reich, N. & Darnell, J. E. Jr. Interferon-induced nuclear factors that bind a shared promoter element correlate with positive and negative transcriptional control. Genes Dev 2, 383–93 (1988).
Lamb, P. et al. STAT protein complexes activated by interferon-gamma and gp130 signaling molecules differ in their sequence preferences and transcriptional induction properties. Nucleic Acids Res 23, 3283–9 (1995).
Heinrich, P. C., Behrmann, I., Müller-Newen, G., Schaper, F. & Graeve, L. Interleukin-6-type cytokine signalling through the gp130/Jak/STAT pathway. Biochem J 334, 297–314 (1998).
Ivashkiv, L. B. & Donlin, L. T. Regulation of type I interferon responses. Nat Rev Immunol 14, 36–49 (2014).
Platanias, L. C. Mechanisms of type-I- and type-II-interferon-mediated signalling. Nat Rev Immunol 5, 375–86 (2005).
Chatterjee-Kishore, M., Wright, K. L., Ting, J. P. & Stark, G. R. How Stat1 mediates constitutive gene expression: a complex of unphosphorylated Stat1 and IRF1 supports transcription of the LMP2 gene. EMBO J 19, 4111–22 (2000).
Yang, J. et al. Unphosphorylated STAT3 accumulates in response to IL-6 and activates transcription by binding to NFkappaB. Genes Dev 21, 1396–408 (2007).
Timofeeva, O. A. et al. Mechanisms of unphosphorylated STAT3 transcription factor binding to DNA. J Biol Chem 287, 14192–200 (2012).
Kessenbrock, K., Plaks, V. & Werb, Z. Matrix metalloproteinases: regulators of the tumor microenvironment. Cell 141, 52–67 (2010).
Mellick, A. S., Blackmore, D., Weinstein, S. R. & Griffiths, L. R. An Assessment of MMP and TIMP Gene Expression in Cell Lines and Stroma–Tumor Differences in Microdissected Breast Cancer Biopsies. Tumor Biol 24, 258–70 (2004).
Parks, W. C., Wilson, C. L. & López-Boado, Y. S. Matrix metalloproteinases as modulators of inflammation and innate immunity. Nat Rev Immunol 4, 617–29 (2004).
Gordon, G. M., Ledee, D. R., Feuer, W. J. & Fini, M. E. Cytokines and signaling pathways regulating matrix metalloproteinase-9 (MMP-9) expression in corneal epithelial cells. J Cell Physiol 221, 402–11 (2009).
Mauviel, A. Cytokine regulation of metalloproteinase gene expression. J Cell Biochem 53, 288–95 (1993).
Sundararaj, K. P. et al. Interleukin-6 released from fibroblasts is essential for up-regulation of matrix metalloproteinase-1 expression by U937 macrophages in coculture: cross-talking between fibroblasts and U937 macrophages exposed to high glucose. J Biol Chem 284, 13714–24 (2009).
Korzus, E., Nagase, H., Rydell, R. & Travis, J. The mitogen-activated protein kinase and JAK-STAT signaling pathways are required for an oncostatin M-responsive element-mediated activation of matrix metalloproteinase 1 gene expression. J Biol Chem 272, 1188–96 (1997).
Tsareva, S. A. et al. Signal transducer and activator of transcription 3 activation promotes invasive growth of colon carcinomas through matrix metalloproteinase induction. Neoplasia 9, 279–91 (2007).
Zugowski, C. et al. STAT3 controls matrix metalloproteinase-1 expression in colon carcinoma cells by both direct and AP-1-mediated interaction with the MMP-1 promoter. Biol Chem 392, 449–59 (2011).
Kossakowska, A. E. et al. Interleukin-6 regulation of matrix metalloproteinase (MMP-2 and MMP-9) and tissue inhibitor of metalloproteinase (TIMP-1) expression in malignant non-Hodgkin’s lymphomas. Blood 94, 2080–9 (1999).
Itoh, M. et al. Requirement of STAT3 activation for maximal collagenase-1 (MMP-1) induction by epidermal growth factor and malignant characteristics in T24 bladder cancer cells. Oncogene 25, 1195–204 (2006).
Hughes, K., Wickenden, J. A., Allen, J. E. & Watson, C. J. Conditional deletion of Stat3 in mammary epithelium impairs the acute phase response and modulates immune cell numbers during post-lactational regression. J Pathol 227, 106–17 (2012).
Miklossy, G., Hilliard, T. S. & Turkson, J. Therapeutic modulators of STAT signalling for human diseases. Nat Rev Drug Discov 12, 611–29 (2013).
Akkoca, A. N. et al. TNM and Modified Dukes staging along with the demographic characteristics of patients with colorectal carcinoma. Int J Clin Exp Med 7, 2828–35 (2014).
Quintanilla-Martinez, L. et al. Analysis of signal transducer and activator of transcription 3 (Stat 3) pathway in multiple myeloma: Stat 3 activation and cyclin D1 dysregulation are mutually exclusive events. Am J Pathol 162, 1449–61 (2003).
Cantwell, C. A., Sterneck, E. & Johnson, P. F. Interleukin-6-specific activation of the C/EBPdelta gene in hepatocytes is mediated by Stat3 and Sp1. Mol Cell Biol 18, 2108–17 (1998).
Yang, E., Lerner, L., Besser, D. & Darnell, J. E. Jr. Independent and cooperative activation of chromosomal c-fos promoter by STAT3. J Biol Chem 278, 15794–9 (2003).
Kiuchi, N. et al. STAT3 is required for the gp130-mediated full activation of the c-myc gene. J Exp Med 189, 63–73 (1999).
Ichiba, M., Nakajima, K., Yamanaka, Y., Kiuchi, N. & Hirano, T. Autoregulation of the Stat3 gene through cooperation with a cAMP-responsive element-binding protein. J Biol Chem 273, 6132–8 (1998).
Kojima, H., Nakajima, K. & Hirano, T. IL-6-inducible complexes on an IL-6 response element of the junB promoter contain Stat3 and 36 kDa CRE-like site binding protein(s). Oncogene 12, 547–54 (1996).
Look, D. C., Pelletier, M. R. & Holtzman, M. J. Selective interaction of a subset of interferon-gamma response element-binding proteins with the intercellular adhesion molecule-1 (ICAM-1) gene promoter controls the pattern of expression on epithelial cells. J Biol Chem 269, 8952–8 (1994).
Look, D. C., Pelletier, M. R., Tidwell, R. M., Roswit, W. T. & Holtzman, M. J. Stat1 depends on transcriptional synergy with Sp1. J Biol Chem 270, 30264–7 (1995).
Caldenhoven, E. et al. Activation of the STAT3/acute phase response factor transcription factor by interleukin-5. J Biol Chem 270, 25778–84 (1995).
Hattori, M., Abraham, L. J., Northemann, W. & Fey, G. H. Acute-phase reaction induces a specific complex between hepatic nuclear proteins and the interleukin 6 response element of the rat alpha 2-macroglobulin gene. Proc Natl Acad Sci USA 87, 2364–8 (1990).
Seidel, H. M. et al. Spacing of palindromic half sites as a determinant of selective STAT (signal transducers and activators of transcription) DNA binding and transcriptional activity. Proc Natl Acad Sci USA 92, 3041–5 (1995).
Eferl, R. & Wagner, E. F. AP-1: a double-edged sword in tumorigenesis. Nat Rev Cancer 3, 859–68 (2003).
Ghazawi, I., Cutler, S. J., Low, P., Mellick, A. S. & Ralph, S. J. Inhibitory effects associated with use of modified Photinus pyralis and Renilla reniformis luciferase vectors in dual reporter assays and implications for analysis of ISGs. J Interferon Cytokine Res 25, 92–102 (2005).
Mudduluru, G., Leupold, J. H., Stroebel, P. & Allgayer, H. PMA up-regulates the transcription of Axl by AP-1 transcription factor binding to TRE sequences via the MAPK cascade in leukaemia cells. Biol Cell 103, 21–33 (2010).
He, H. & Ping, F. The SIE, SRE, CRE, and FAP-1 four intracellular signal pathways between stimulus and the expression of c-fos promoter. J Cell Biochem 106, 764–8 (2009).
Larouche, K., Bergeron, M. J., Leclerc, S. & Guérin, S. L. Optimization of competitor poly(dI-dC).poly(dI-dC) levels is advised in DNA-protein interaction studies involving enriched nuclear proteins. Biotechniques 20, 439–44 (1996).
Salmon, P. et al. High-level transgene expression in human hematopoietic progenitors and differentiated blood lineages after transduction with improved lentiviral vectors. Blood 96, 3392–8 (2000).
Kumar, R., Conklin, D. S. & Mittal, V. High-throughput selection of effective RNAi probes for gene silencing. Genome Res 13, 2333–40 (2003).
Rose-John, S. IL-6 trans-signaling via the soluble IL-6 receptor: importance for the pro-inflammatory activities of IL-6. Int J Biol Sci 8, 1237–47 (2012).
Dasgupta, M., Dermawan, J. K., Willard, B. & Stark, G. R. STAT3-driven transcription depends upon the dimethylation of K49 by EZH2. Proc Natl Acad Sci USA 112, 3985–90 (2015).
Jenkins, B. J. et al. Hyperactivation of Stat3 in gp130 mutant mice promotes gastric hyperproliferation and desensitizes TGF-beta signaling. Nat Med 11, 845–52 (2005).
Schust, J., Sperl, B., Hollis, A., Mayer, T. U. & Berg, T. Stattic: a small-molecule inhibitor of STAT3 activation and dimerization. Chem Biol 13, 1235–42 (2006).
Xu, W. et al. STAT-1 and c-Fos interaction in nitric oxide synthase-2 gene activation. Am J Physiol Lung Cell Mol Physiol 285, L137–148 (2003).
Nakahira, M. et al. Synergy of IL-12 and IL-18 for IFN-gamma gene expression: IL-12-induced STAT4 contributes to IFN-gamma promoter activation by up-regulating the binding activity of IL-18-induced activator protein 1. J Immunol 168, 1146–53 (2002).
Hwang, M. N., Kim, K. S., Choi, Y. W., Jou, I. & Yoon, S. PMA activates Stat3 in the Jak/Stat pathway and induces SOCS5 in rat brain astrocytes. Mol Cells 23, 94–9 (2007).
Lewis, M., Amento, E. P. & Unemori, E. N. Transcriptional inhibition of stromelysin by interferon-gamma in normal human fibroblasts is mediated by the AP-1 domain. J Cell Biochem 72, 373–86 (1999).
Ma, Z., Qin, H. & Benveniste, E. N. Transcriptional suppression of matrix metalloproteinase-9 gene expression by IFN-gamma and IFN-beta: critical role of STAT-1alpha. J Immunol 167, 5150–9 (2001).
Nguyen, J., Knapnougel, P., Lesavre, P. & Bauvois, B. Inhibition of matrix metalloproteinase-9 by interferons and TGF-beta1 through distinct signalings accounts for reduced monocyte invasiveness. FEBS Lett 579, 5487–93 (2005).
Wenta, N., Strauss, H., Meyer, S. & Vinkemeier, U. Tyrosine phosphorylation regulates the partitioning of STAT1 between different dimer conformations. Proc Natl Acad Sci USA 105, 9238–43 (2008).
Yang, J. & Stark, G. R. Roles of unphosphorylated STATs in signaling. Cell Res 18, 443–51 (2008).
Meyer, T., Begitt, A., Lödige, I., van Rossum, M. & Vinkemeier, U. Constitutive and IFN-gamma-induced nuclear import of STAT1 proceed through independent pathways. EMBO J 21, 344–54 (2002).
Fransen, K. et al. Mutation analysis of the BRAF, ARAF and RAF-1 genes in human colorectal adenocarcinomas. Carcinogenesis 25, 527–33 (2004).
Rose’Meyer, R. B. et al. The measurement of adenosine and estrogen receptor expression in rat brains following ovariectomy using quantitative PCR analysis. Brain Res Protoc 11, 9–18 (2003).
Haan, S., Keller, J. F., Behrmann, I., Heinrich, P. C. & Haan, C. Multiple reasons for an inefficient STAT1 response upon IL-6-type cytokine stimulation. Cell Signal 17, 1542–50 (2005).
Acknowledgements
The authors would like to thank Peter Soderkvist, Åsa Schippert, and Karin Franzén (Linköping University, Linköping, Sweden) for support in tissue collection. George Stark (Cleveland Clinic, OH) for support, guidance as well as shRNA for STAT-1. Mathias Ernst, Olivia Newton-John Cancer Wellness & Research Centre (LaTrobe, Victoria, Australia) for tissues from the gp130 animals. We would also like to thank Paul DeSouza and Kieran Scott (Ingham Institute for Applied Medical Research, Liverpool, NSW, Australia) for advice in completing the manuscript. This research was supported by grants held by A.S.M and S.J.R: Australian Research Council (Grant No. 0988602), Queensland Cancer Fund (Grant No. 277014) and National Health & Medical Research Council (Grant No. 1011114). S.J.C. and I.G. were supported by Australian Postgraduate Research Awards.
Author information
Authors and Affiliations
Contributions
Designed research: L.R.G., S.J.C., S.J.R. and A.S.M. Performed experiments: A.S.M., I.G., S.J.C. and J.Y. Analyzed data: J.D.D., S.J.C., S.J.R. and A.S.M. Wrote the manuscript: A.S.M., S.J.C. and S.J.R. All authors reviewed the manuscript. A.S.M. and S.J.R. contributed equally as senior author.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Cutler, S.J., Doecke, J.D., Ghazawi, I. et al. Novel STAT binding elements mediate IL-6 regulation of MMP-1 and MMP-3. Sci Rep 7, 8526 (2017). https://doi.org/10.1038/s41598-017-08581-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-08581-y
This article is cited by
-
IL6/sIL6R regulates TNFα-inflammatory response in synovial fibroblasts through modulation of transcriptional and post-transcriptional mechanisms
BMC Molecular and Cell Biology (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.