Abstract
Despite increasing knowledge of the significance of calcium-activated potassium (KCa) and canonical transient receptor potential (TRPC) channels in endothelial physiology, no studies so far have investigated the link between these two distinct types of channels in the control of vascular tone in pathological conditions. We previously demonstrated that hypoxia-reoxygenation (H-R) inhibits endothelial KCa and TRPC3 channels in porcine coronary arteries (PCAs). The present study further investigated whether modulation of TRPC3 is involved in H-R-induced KCa channel inhibition and associated vasodilatory dysfunction using approaches of wire myography, whole-cell voltage-clamp, and coimmunoprecipitation. Pharmacological inhibition or siRNA silencing of TRPC3 significantly suppressed bradykinin-induced intermediate- and small-conductance KCa (IKCa and SKCa) currents in endothelial cells of PCAs (PCAECs). TRPC3 protein exists in physical association with neither IKCa nor SKCa. In H-R-exposed PCAECs, the response of IKCa and SKCa to bradykinin-stimulation and to TRPC3-inhibition was markedly weakened. Activation of TRPC3 channels restored H-R-suppressed KCa currents in association with an improved endothelium-derived hyperpolarizing factor (EDHF)-type vasorelaxation. We conclude that inhibition of TRPC3 channels contributes to H-R-induced suppression of KCa channel activity, which serves as a mechanism underlying coronary endothelial dysfunction in ischemia-reperfusion (I-R) injury and renders TRPC3 a potential target for endothelial protection in I-R conditions.
Similar content being viewed by others
Introduction
The role of intermediate and small conductance calcium-activated K+ (IKCa and SKCa) channels of endothelial cells in the control of vascular tone has been well documented. Opening of IKCa and SKCa channels in response to increased cytosolic Ca2+ is the mechanism underlying the classical endothelium-derived hyperpolarizing factor (EDHF) pathway1. In addition, activation of these channels is also involved in the regulation of eNOS activity and NO function2, 3. Disturbed function of IKCa/SKCa channels has been reported to be associated with endothelial dysfunction in cardiovascular pathologies, e.g., hypertension and diabetes4.
Members of the transient receptor potential (TRP) protein superfamily form nonselective cation channels that are of great importance in [Ca2+]i regulation in vascular endothelial cells5, 6. It was reported that native canonical TRP3 (TRPC3) channels contribute to constitutive and ATP-dependent Ca2+ influx in human coronary artery endothelial cells7 and TRPC3-mediated Ca2+ influx was demonstrated to be essential for NO production and endothelium-dependent relaxation in porcine coronary and human arteries8, 9. Altered expression and/or activity of TRPC3 have been associated, directly or indirectly, with endothelial dysfunction and endothelium-related vascular disease10.
Ischemia-reperfusion (I-R) injury constitutes one of the major causes of cardiovascular morbidity and mortality11. Vascular endothelium is vulnerable to I-R injury12, 13. Previous research provided evidence in support of the role of KCa channel dysregulation in I-R-induced endothelial dysfunction14, 15. In our in vitro studies of I-R in porcine coronary arteries, we demonstrated that hypoxia-reoxygenation (H-R) suppresses IKCa and SKCa channel currents in endothelial cells and such inhibition is responsible for the compromised EDHF-mediated vasorelaxation and smooth muscle hyperpolarization16. In addition, through inhibiting the expression of TRPC3 protein on endothelial cell membrane, H-R significantly reduces TRPC3 channel activity and Ca2+ influx via TRPC3, leading to decreased NO production and vasorelaxation8.
Although knowledge of the significance of IKCa/SKCa and TRPC3 channels in endothelial pathophysiology has been growing, very few studies to date have attempted to explore the link between these two distinct types of channels in the control of vascular tone. With using pressure myograph and sharp electrode intracellular recording, Senadheera and colleagues first reported that TRPC3 facilitates IKCa/SKCa-dependent endothelial cell hyperpolarization and vasodilation in rat mesenteric arteries17. TRPC3-mediated regulation of SKCa channel activation was further revealed in mouse cerebral circulation18. In agreement with these findings, our study in porcine coronary arteries suggested an important role of TRPC3 channels in mediating EDHF-type relaxation19. Despite these pieces of evidence linking TRPC3 and KCa channels in endothelium physiology, whether the functional link between TRPC3 and KCa involves physical associations is yet to be examined in coronary vasculature. Furthermore, no studies so far have investigated the relationship of these channels in pathological conditions. Whether modulation of TRPC3 channels is involved in IKCa and SKCa channel dysfunction related to endothelial I-R injury remains unexplored. In the present study, by using multiple approaches, including whole-cell voltage-clamp recording of channel currents, myograph studies of vasorelaxation, and molecular biology methods, we aimed to provide answers to the above questions.
Results
Blockade and knockdown of TRPC3 channels inhibit endothelial IKCa and SKCa channel activity
We examined the role of TRPC3 channels in endothelial KCa channel activation with using pharmacological tools and siRNA knockdown technique. Pretreatment of PCAECs for 30 min with the specific TRPC3 channel blocker Pyr3 significantly suppressed bradykinin-induced whole-cell K+ currents (45.69 ± 2.77 vs. 65.45 ± 3.01 pA/pF, p < 0.01) with the IKCa channel current decreasing from 16.89 ± 0.93 pA/pF to 6.71 ± 0.85 pA/pF (p < 0.001) and the SKCa channel current from 10.63 ± 1.69 pA/pF to 5.51 ± 1.17 pA/pF (p < 0.05) (Fig. 1a and b). Further studies using gene silencing approach showed that in PCAECs transfected with TRPC3 specific siRNA, bradykinin-induced K+ currents decreased from 62.39 ± 2.06 pA/pF to 50.71 ± 3.49 pA/pF (p < 0.01) and both IKCa (9.46 ± 1.12 vs. 15.67 ± 1.29 pA/pF, p < 0.01) and SKCa (6.46 ± 0.84 vs. 9.63 ± 1.49 pA/pF, p < 0.05) currents in response to bradykinin were significantly inhibited (Fig. 1a and b). Successful silencing of the TRPC3 gene was confirmed by the dramatic reduction of channel expression (Supplementary Fig. S1a,b) and the significant inhibition of channel activity which is evidenced by the suppressed response to OAG stimulation (p < 0.05). In response to OAG, membrane current increased from 18.22 ± 2.25 to 23.96 ± 1.01 pA/pF (p < 0.05) in TRPC3 siRNA-transfected cells while increased to 31.04 ± 1.43 pA/pF (p < 0.01) in control cells from 19.19 ± 1.84 pA/pF (Supplementary Fig. S1c). With a subsequent application of Pyr3, the TRPC3 channel current was able to be differentiated and the data further confirmed the loss of TRPC3 channel activity in the gene knockdown cells (4.69 ± 1.08 vs. 8.50 ± 0.35 pA/pF in control, p < 0.05) (Supplementary Fig. S1c,d).
In PCAECs pre-treated with the TRPC3 selective blocker Pyr3 or transfected with TRPC3 specific siRNA, both IKCa and SKCa currents in response to bradykinin (BK) were significantly inhibited. (a) Representative traces and current-voltage relationship of whole-cell K+ current in PCAECs from different treatment groups before and after BK stimulation with further application of the IKCa channel blocker TRAM-34 and the SKCa channel blocker apamin. *p < 0.05, **p < 0.01, BK vs. basal; #p < 0.05, ##p < 0.01, BK + TRAM-34 vs. BK; ^p < 0.05, ^^p < 0.01, BK + TRAM-34 + Apamin vs. BK + TRAM-34. (b) Summarized data of BK-induced IKCa and SKCa currents from 5 independent experiments, each obtained from cell isolates of different heart. *p < 0.05, **p < 0.01, ***p < 0.001, one-way ANOVA and Scheffe post-hoc test.
TRPC3 channels do not physically associate with KCa channels in PCAECs
The results of co-immunoprecipitation experiments showed that in PCAECs, TRPC3 protein co-precipitates with neither KCa3.1 nor KCa2.3 protein, suggesting that TRPC3 channels do not physically associate with KCa channels in PCAECs (Fig. 2).
TRPC3 channels do not physically interact with IKCa and SKCa channels in PCAECs. The cell lysates were incubated with anti-TRPC3 antibody, and the immunoprecipitates were subjected to immunoblot by anti-KCa3.1 and anti-KCa2.3 antibodies respectively (a and b). The immunoprecipitation and immunoblot experiments were further performed in reversed order (c and d). Lysate supernatant (20 μg of protein) was used as input control. Mouse IgG was used as a negative control. Full-length western blot images are presented in Supplementary Figure S2. Experiments in each order were performed for four times with using cell isolates from different hearts.
TRPC3 inhibition contributes to the inhibition of endothelial KCa activity under H-R condition
H-R (60-30 min) exposure inhibited the whole-cell K+ current in PCAECs. In comparison to cells without H-R exposure (35.58 ± 2.74 pA/pF), the basal K+ current declined to 23.77 ± 1.70 pA/pF (p < 0.05), which is consistent with our previous report16. Bradykinin-induced K+ current was suppressed by H-R exposure (40.19 ± 1.61 vs. 65.73 ± 2.87 in normoxia, p < 0.01), in which bradykinin-induced IKCa current was decreased from 19.05 ± 3.03 to 10.24 ± 1.96 pA/pF (p < 0.01) and SKCa current from 10.63 ± 1.69 to 4.62 ± 0.43 pA/pF (p < 0.05). Biotinylation assay showed that H-R exposure suppresses the surface expression of IKCa channels whereas has no significant effect on the surface expression of SKCa channels in PCAECs (Supplementary Fig. S3). Similar to PCAECs subjected to normoxic condition in which KCa channel activity was demonstrated to be suppressed by TRPC3 inhibition, pretreatment of the H-R-exposed cells with the TRPC3 channel blocker Pyr3 also reduced bradykinin-induced K+ current (31.73 ± 1.10 pA/pF vs. 40.19 ± 1.61 pA/pF in H-R, p < 0.05) with significant suppression of both IKCa (5.19 ± 0.48 vs. 10.24 ± 1.96 pA/pF in H-R, p < 0.05) and SKCa (1.79 ± 0.36 vs. 4.62 ± 0.43 pA/pF in H-R, p < 0.05) channel currents (Fig. 3a and b). However, Pyr3 exhibited less inhibition on both IKCa and SKCa channels when compared with the cells without H-R exposure. The IKCa and SKCa currents inhibited by Pyr3 were 9.06 ± 1.81 and 5.15 ± 1.21 pA/pF respectively in normoxic cells and 5.12 ± 1.22 pA/pF (p < 0.05) and 3.14 ± 0.49 pA/pF (p < 0.05) in H-R exposed cells (Fig. 3c), suggesting that inhibition of TRPC3 by H-R contributes to H-R-induced IKCa and SKCa channel inhibition in PCAECs. For experiments involving Pyr3, Pyr3 was added to the bath solution just before the onset of hypoxia and lasted throughout the H-R exposure period. After H-R exposure, the cells were moved to patch clamp recording chamber and the recording was usually completed within 1 hour.
Inhibition of TRPC3 channels contributes to H-R-induced suppression of IKCa and SKCa channel activity in PCAECs. Representative traces and current-voltage relationship of whole-cell K+ current in PCAECs from different treatment groups before and after bradykinin (BK) stimulation with further application of the IKCa channel blocker TRAM-34 and the SKCa blocker apamin (a). In H-R group, cells were exposed to 60-min hypoxia and 30-min reoxygenation before patch-clamp recording. *p < 0.05, **p < 0.01, BK vs. basal; #p < 0.05, ##p < 0.01, BK + TRAM-34 vs. BK; ^p < 0.05, ^^p < 0.01, BK + TRAM-34 + Apamin vs. BK + TRAM-34. Pre-treatment of PCAECs with the selective TRPC3 channel blocker Pyr3 significantly inhibited BK-induced IKCa and SKCa channel currents under both normoxic and H-R conditions (b). Pyr3 exhibited less inhibition on both components of IKCa and SKCa induced by BK when compared with the cells without H-R exposure (c). *p < 0.05, **p < 0.01, one-way ANOVA and Scheffe post-hoc test (a and b) and unpaired t test (c). n = 5 in each group. N indicates the number of independent experiments, each obtained from cell isolates of different hearts.
Activation of TRPC3 channels protects endothelial KCa channels from H-R-induced inhibition
Incubation of PCAECs with OAG during H-R exposure enhanced IKCa and SKCa channel activity. OAG was added to the bath solution just before the onset of hypoxia and the subsequent current recording was performed by moving the cells to patch clamp recording chamber after H-R exposure. Compared with the H-R-exposed cells, cells exposed to H-R and co-treated with OAG exhibited significantly larger current density of IKCa (15.08 ± 0.99 vs. 8.89 ± 0.86 pA/pF in H-R, p < 0.01) and SKCa (9.62 ± 0.89 vs. 4.92 ± 0.53 pA/pF in H-R, p < 0.05) upon bradykinin stimulation, leading to increased whole-cell K+ current (56.67 ± 1.79 vs. 39.79 ± 0.82 pA/pF in H-R, p < 0.01). Further experiments revealed that TRPC3 channel activation mediates OAG-induced protection against H-R on KCa channel activity, which is suggested by the findings of loss of enhancement of bradykinin-induced K+ (38.93 ± 1.22 pA/pF, p < 0.01) and IKCa (7.94 ± 0.32 pA/pF, p < 0.01) and SKCa (4.15 ± 0.27 pA/pF, p < 0.01) channel currents in OAG-incubated cells in which current recording was performed in the presence of Pyr3 (Fig. 4a and b). Under H-R condition, activation of TRPC3 also preserves the constitutive activity of IKCa and SKCa channels, suggested by the finding of an increase of basal K+ currents in OAG-treated cells (28.90 ± 1.42 vs. 23.59 ± 1.75 pA/pF in H-R, p < 0.05) that is diminished by Pyr3 (22.03 ± 2.32 pA/pF) (Fig. 4a).
Activation of TRPC3 channels protects IKCa and SKCa channels from H-R-induced inhibition in PCAECs. (a) Representative traces and current-voltage relationship of whole-cell K+ current in PCAECs from different treatment groups before and after bradykinin (BK) stimulation with further application of the IKCa channel blocker TRAM-34 and the SKCa channel blocker apamin. Under H-R condition, PCAECs treated with OAG shows enhanced basal and BK-induced K+ currents compared with the cells without OAG-treatment and such enhancement is diminished by Pyr3. *p < 0.05, **p < 0.01, BK vs. basal; #p < 0.05, ##p < 0.01, BK + TRAM-34 vs. BK; ^p < 0.05, ^^p < 0.01, BK + TRAM-34 + Apamin vs. BK + TRAM-34. (b) Summarized data of BK-induced IKCa and SKCa currents from 5 independent experiments, each obtained from cell isolates of different hearts. PCAECs were subjected to H-R exposure in the absence or presence of the TRPC3/6/7 activator OAG before patch-clamp recording. For cells subjected to H-R exposure and OAG treatment, the current recording was performed under the condition without (H-R + OAG-treated) or with Pyr3 application (H-R + OAG-treated + Pyr3). *p < 0.05, **p < 0.01; one-way ANOVA and Scheffe post-hoc test.
Activation of TRPC3 channels preserves vasodilatory function of endothelial KCa channels under H-R condition
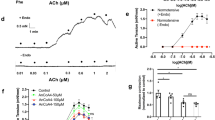
Porcine small coronary arteries pretreated with Pyr3 showed attenuated EDHF-type relaxation to bradykinin (Rmax: 43.3 ± 4.7% vs. 69.5 ± 3.8%, p < 0.01) (Fig. 5a). Exposure to H-R compromised bradykinin-induced EDHF-mediated relaxation (Rmax: 40.4 ± 5.1% vs. 70.1 ± 2.7% in normoxic control, p < 0.01). Treatment with OAG throughout the H-R exposure period prevented the inhibition of EDHF-mediated relaxant response (61.3 ± 3.5%, p < 0.05 vs. H-R), indicating that activation of TRPC3 channels preserves KCa channel-related endothelial function under H-R condition (Fig. 5b). No differences were observed among different treatment groups with regard to resting force and the U46619-induced pre-contraction (Supplementary Table S1).
TRPC3 channels play an important role in EDHF-mediated relaxation in porcine small coronary arteries (a, n = 8 in each group). H-R exposure impairs the EDHF-mediated vasorelaxation and activation of TRPC3 preserves the EDHF-type response under H-R condition (b, n = 8 in each group). The EDHF-response was induced by bradykinin in the presence of indomethacin, NG-nitro-L-arginine, and oxyhemoglobin. *p < 0.05, **p < 0.01 vs. control; #p < 0.05, ##p < 0.01 vs. H-R, unpaired t test (a), one-way ANOVA and Scheffe post-hoc test (b). Pyr3: TRPC3 selective blocker. OAG: TRPC3/6/7 activator.
Discussion
The present study demonstrated that in porcine coronary arteries (1) TRPC3 channels play a fundamental role in the regulation of KCa channel activity in endothelial cells; (2) the functional association between TRPC3 and KCa channels does not involve physical interaction; (3) reduction of membrane TRPC3 contributes to H-R-induced suppression of IKCa and SKCa channel activity; (4) activation of TRPC3 protects IKCa and SKCa channels from H-R-induced inhibition thereby preserving EDHF-type vasorelaxation.
Previous investigations have shown the significance of TRPC3 channels in arterial tone and blood flow regulation in both animal and human vasculatures8, 9, 20, 21. In our prior studies in porcine coronary arteries, we reported that TRPC3 channels regulate vascular tone through promoting NO production8 and EDHF-type relaxation19. The present study further demonstrated that TRPC3 channels participate in EDHF-type relaxation through mediating activation of endothelial IKCa and SKCa channels, which is in agreement with the findings in rodent vascular beds17, 18. By using sharp electrode to measure membrane potential, Senadheera and colleagues observed that in the presence of cyclooxygenase and eNOS inhibitors, inhibition of TRPC3 channels with Pyr3 significantly reduced the amplitude of ACh-induced hyperpolarization in rat mesenteric artery endothelial cells, which was the first published electrophysiological evidence suggesting the functional role of TRPC3 in KCa-dependent EDHF mechanism. A subsequent study by the same group on mouse cerebral arteries yielded similar results18 and further linked TRPC3 channel activation and SKCa channel activation in the EDHF-response with support of channel current recording data. In the present study, we observed that in PCAECs, pharmacological inhibition of TRPC3 channels and gene silencing of TRPC3 significantly suppressed TRAM-34-sensitive and apamin-sensitive whole-cell K+ currents in response to bradykinin, suggesting the requirement of TRPC3 channels in the activation of both IKCa and SKCa channels in porcine coronary endothelium.
Given the knowledge that TRP channels may associate with other proteins to form a signaling complex, for example, colocalization of TRPC122 or TRPC3/623 with BKCa was found to underlie the role of these TRP members in the activation of BKCa channels. We investigated whether the functional link between TRPC3 and IKCa/SKCa channels involves direct physical association of the channel proteins. Our co-immunoprecipitation experiments showed that in PCAECs, TRPC3 protein neither binds with KCa3.1 nor KCa2.3 protein, suggesting that TRPC3 does not physically interact with IKCa/SKCa channels to regulate the KCa channel activity in porcine coronary endothelium. As to the study of SKCa channel proteins, among the three subtypes SK1 (KCa2.1), SK2 (KCa2.2) and SK3 (KCa2.3), we focused on SK3 (KCa2.3), which is because (1) previous investigation demonstrated that no mRNA encoding SK1 is detected in porcine coronary endothelium and the apamin-sensitive component of the EDHF-response is mediated by SK3 while not by SK224, and (2) our latest study added a further piece of evidence concerning the significance of KCa2.3 subtype in the regulation of endothelial function in this vasculature25.
It has been reported that in vascular endothelial cells IKCa channels predominantly reside in myoendothelial projections and SKCa channels preferentially locate at the sites of homocellular endothelial gap junctions and caveolin-rich domains26. In rat mesenteric arteries, based on the findings of strong expression of TRPC3 in myoendothelial contact regions, Senadheera and colleagues proposed that a close proximity of TRPC3 and IKCa channels facilitates IKCa activation via TRPC3-dependent Ca2+ signaling that may involve Ca2+ influx and/or refilling of the IP3R-mediated endoplasmic reticulum Ca2+ stores17. The exact localizations of TRPC3 and KCa channels were not characterized in the present study, however, with the findings of no binding of TRPC3 with KCa proteins whereas significant role of TRPC3 in KCa channel activity, the present study favors the theory of TRPC3-mediated Ca2+ signals for KCa channel activation in PCAECs. Further studies of how Ca2+ signals bridge TRPC3 and KCa, e.g., initiation and location of the signal, and/or cascades involved in Ca2+ signaling, need to be undertaken in order to fully understand the functional role of TRPC3 in KCa channel activation.
The most important and novel finding of the present study is that inhibition of TRPC3 channels contributes to H-R-induced suppression of channel activity of IKCa and SKCa. We previously reported that H-R suppresses KCa and TRPC3 channel activity in porcine coronary arterial endothelial cells8, 16. In the present study, given our demonstration that TRPC3 is integral to endothelial IKCa and SKCa channel activation in porcine coronary artery, we further explored the relationship between TRPC3 channel inhibition and KCa channel inhibition and its significance in endothelial dysfunction related to I-R injury. Patch-clamp data showed that in both control and H-R-exposed PCAECs, TRPC3 channel blocker Pyr3 inhibits bradykinin-induced IKCa and SKCa channel currents, however, the extent of inhibition is significantly less in H-R-exposed cells in comparison with cells without H-R exposure (Fig. 3). Further recordings showed that activation of TRPC3 channels effectively prevents H-R-induced suppression of endothelial KCa channel activity (Fig. 4). Both basal K+ currents and IKCa and SKCa currents in response to bradykinin were enhanced in cells exposed to H-R and co-treated with OAG, in which blocking TRPC3 channels with Pyr3 diminished the protective effect conferred by OAG. In our previous study, we demonstrated that in our preparation of PCAECs, the basal K+ current is predominantly composed of IKCa and SKCa currents16. Taken together, these results suggest that loss of TRPC3 channel activity contributes to H-R-induced IKCa and SKCa channel inhibition in coronary endothelium. In conjunction with the finding of decreased cell surface expression of IKCa (KCa 3.1) and insignificant change in cell surface expression of SKCa (KCa2.3) following H-R exposure, our results suggest that the inhibition of IKCa current induced by H-R is a combined effect of less IKCa in the membrane and less Ca2+ (due to less TRPC3) whereas H-R-induced inhibition of SKCa current is primarily due to the less Ca2+ for activation. The significance of TRPC3 inhibition in KCa inhibition therefore provided a mechanistic explanation for the beneficial effect of activation of TRPC3 channels on EDHF function in H-R-exposed coronary arteries (Fig. 5).
Recent evidence suggests that trafficking of TRPC3 to the plasma membrane facilitates SKCa channel activation in mouse cerebral endothelium18. In a prior study, we demonstrated that in H-R-exposed PCAECs, decreases of TRPC3 channel currents and TRPC3-mediated Ca2+ entry are attributable to the inhibition of TRPC3 trafficking that results in reduction of TRPC3 channels presented at the endothelial cell surface8. In light of these findings, we therefore propose that inhibition of TRPC3 trafficking is the likely mechanism underlying the pathological significance of TRPC3 in endothelial KCa channel dysfunction associated with H-R injury.
This study has several limitations that must be acknowledged. The negative results of our co-immunoprecipitation experiments suggest that TRPC3 and KCa channels are not physically associated with each other in PCAECs. In the present study, the protein-protein interactions of TRPC3 and either IKCa and SKCa were only studied in endothelial cells under unstimulated condition and no further efforts were made to explore whether these may change when cells are upon stimulation, e.g., by agonists such as bradykinin, or by pathological factors such as I-R/H-R. Considering the fact that internal and external stimuli may dynamically regulate ion channels through mechanisms including, but not limited to, forward trafficking and endocytosis of channels, further studies of protein-protein interaction of TRPC3 and KCa in stimulated condition is therefore necessary to derive a complete and dynamic understanding of the relationship of these two channels in the control of coronary arterial tone. In addition, although we demonstrated that TRPC3 physically interacts with neither IKCa nor SKCa channels in PCAECs, current results could not answer the question whether TRPC3 and KCa channels are colocalized or located in close proximity in these cells. Further studies with double immunofluorescence staining and fluorescence resonance energy transfer measurement shall reveal the spatial proximity between these channels thereby deepen our understanding of how TRPC3 functions to regulate KCa channel activity under physiological condition and how H-R disrupts the functional interaction between TRPC3 and KCa.
In conclusion, the present study demonstrated that TRPC3 channels play an important role in IKCa and SKCa channel activation in coronary arterial endothelial cells. The functional association between TRPC3 and KCa channels does not involve physical interaction. Inhibition of TRPC3 channels contributes to H-R-induced suppression of IKCa and SKCa channel activity, which serves as a mechanism underlying endothelial dysfunction under H-R condition and renders TRPC3 channels a potential target for endothelial protection in ischemic status.
Materials and Methods
Fresh hearts of young adult pigs (~35 kg) were collected from a local slaughterhouse. Once excised, the hearts were placed in a container filled with cold (4 °C), pre-oxygenated (95%O2/5%CO2) Krebs solution and immediately transferred to the laboratory for dissection of small coronary arteries as in our previous studies8, 16, 19. All experiments were in accordance with institutional guidelines and approved by the Animal Experimentation Ethics Committee, and Safety Office of the Chinese University of Hong Kong (Ref. No. 14/010/GRF).
Isolation and primary culture of porcine coronary arterial endothelial cells (PCAECs)
PCAECs were isolated by enzymatic digestion from porcine small coronary arteries and cultured as previously described8, 16, 19. Briefly, small porcine coronary arteries taken from the branches of left anterior descending artery (LAD) were dissected into tiny strips and treated with 0.2% collagenase (type I, Sigma) at 37 °C for 15 min. The suspension was centrifuged at 1600 rpm for 5 min and cells were resuspended in 5 mL culture medium containing 90% RPMI and 10% FBS with 100 U/mL penicillin and 100 μg/mL streptomycin. After 2-hour incubation at 37 °C, the medium was replaced once to remove unattached cells. Attached endothelial cells were cultured in medium containing antibiotics in a humidified incubator with 5% CO2 at 37 °C for ~6 days. For maintaining electrophysiological properties of isolated coronary endothelial cells, only primary cells were used for experiments. The endothelial nature of the cultured cells was identified by immunostaining for von Willebrand Factor (vWF) as previously described8. Briefly, cultured cells seeded on glass coverslips were fixed with 4% formaldehyde for 15 min at room temperature and blocked in PBS containing 2% BSA for 60 min, then incubated overnight at 4 °C with rabbit anti-vWF antibody (1:200), followed by 1 hour incubation with Alexa Fluor® 488-conjugated goat anti-rabbit IgG (Abcam, 1:500) at room temperature in the dark. Immunostaining for alpha-smooth muscle actin (α-SMA) was used to evaluate the contamination by smooth muscle cells, which was performed by incubation of the cells with anti-α-SMA antibody (1:200) followed by Alexa Fluor® 555-conjugated donkey anti-rabbit antibody (Abcam, 1:500). The coverslip was placed on a microscope slide and covered with a drop of ProLong Gold antifade reagent with DAPI (Invitrogen). After rinsing with PBS, the cells were observed and photographed using a fluorescent microscope (Leica DM 6000 FS, Germany).
Whole-cell recording using the perforated patch-clamp technique for IKCa, SKCa, and TRPC3 channel currents in PCAECs
Whole-cell K+ currents of PCAECs were recorded by using the whole-cell perforated patch-clamp technique (EPC10, HEKA, Lambrecht, Germany) at room temperature (20–24 °C) with further differentiation of the IKCa and SKCa components16, 25. Briefly, patch pipettes with resistance of 3–5 MΩ were filled with a solution containing (mmol/L): NaCl 20, KCl 40, K-aspartate 80, MgCl2 1, Mg-ATP 3, EGTA 10, and K-HEPES 5 (pH adjusted to 7.2 using KOH). The pipette solution contains amphotericin B (500 μg/mL) as the perforating agent. The bath solution contains (mmol/L): NaCl 140, KCl 5.4, MgCl2 1, CaCl2 1.8 and Na-HEPES 10 (pH 7.4 adjusted with NaOH). Whole-cell currents were evoked by 500-ms voltage steps from −100 mV to +100 mV in 20 mV increments from a holding potential of −60 mV. K+ currents induced by bradykinin (100 nmol/L) were recorded with further application of the specific IKCa channel blocker TRAM-34 (1 μmol/L) followed by SKCa blocker apamin (100 nmol/L)24, 25, 27. Currents were recorded after achievement of the full perforation of the membrane patch that usually took 3–5 min, as judged from the development of repeatable currents in response to step depolarizations. Liquid junction potentials, series resistance, and cell capacitance were compensated. For recording of TRPC3 channel currents, patch pipettes were filled with a solution containing (mmol/L): Cs-methanesulphonate 120, CsCl 20, HEPES 10, MgCl2 1, and EGTA 1 (pH 7.2 with KOH). The bath solution contains (mmol/L): NaCl 137, KCl 5.4, HEPES 10, glucose 10, MgCl2 1, and CaCl2 2 (pH 7.4 with NaOH). Membrane currents were recorded in whole-cell mode using a voltage-clamp protocol (voltage ramps from −100 to +100 mV, 0.6 V/s, 0.2 Hz, holding potential −70 mV). Current in response to the TRPC3/6/7 activator 1-oleoyl-2-acetyl-sn-glycerol (OAG) (100 µmol/L) were recorded with further application of the TRPC3 selective blocker Pyr3 (10 µmol/L)8 to differentiate the TRPC3 component. Data were analyzed with PulseFit software (HEKA). The current was normalized by cell capacitance into current densities (pA/pF). Only recordings with seal resistance >500 MΩ, and series resistance <10 MΩ were included in the study and experiments were only analyzed if changes in series resistance were no more than 2 MΩ in the entire recording period.
siRNA knockdown of endogenous TRPC3 channels
Primary cultured PCAECs were transfected with the TRPC3-specific siRNA (sense: 5′GCUCGAGGAUCAAUGCCUATT3′, antisense: 5′UAGGCAUUGAUCCUCGAGCTT3′) by using LipofectamineTM 2000 (Invitrogen), according to manufacturer’s instructions. Knockdown efficiency of TRPC3 was determined at both mRNA level by RT-PCR and protein level by western blotting.
RT-PCR analysis of mRNA expression of TRPC3
Total RNA from PCAECs was extracted using RNAiso reagent (Takara) and mRNA was converted to cDNA using PrimeScriptTM RT Master Mix (Takara), according to manufacturer’s instructions. PCR amplification was performed using GoTaq® G2 Flexi DNA Polymerase (Promega). For TRPC3 amplification, PCR parameters were as follows: 95 °C activation (30 s) followed by 95 °C dissociation (30 s), 46.6 °C anneal (30 s), and 72 °C elongation (1 min) for 30 cycles. Primers used for TRPC3 amplification were: forward: 5′GCAACAAAGGCACAGCAGTA3′, reverse: 5′TTGAGCACAACGGAAGTCAC3′. As the internal loading control, GAPDH was amplified for 30 cycles with the forward primer 5′GGTCGGAGTGAACGGATTT3′ and the reverse primer 5′ATTTGATGTTGGCGGGAT3′ under the following condition: activation (95 °C, 30 s) - dissociation (94 °C, 30 s) - anneal (43.3 °C, 30 s) - elongation (72 °C, 1 min). Products were identified by electrophoresis and digitally imaged for analysis (Geliance 600 Imaging System, PerKinElmer, UK).
Western blot analysis of protein expression of TRPC3
Whole cell protein was extracted from primary cultured PCAECs with ice-cold RIPA lysis buffer, composed of 50 mmol/L Tris-HCl (pH 7.5), 150 mmol/L NaCl, 3.75 mmol/L KCl, 1% NP-40, 0.1% sodium dodecyl sulfate, and 0.5% sodium deoxycholate. Protease (1 tablet in 50 ml) and phosphatase (1 tablet in 10 ml) inhibitor cocktail tablets were freshly added to the buffer before use (Roche Diagnostics). The protein extraction was centrifuged at 4 °C for 20 min at 12000 rpm and the supernatant was then mixed with loading buffer, heated up to 100 °C for 10 min, then fractionated by denaturing 8% sodium-dodecyl-sulfate polyacrylamide-gel electrophoresis (25 µg per lane) for 90 min at 120 V and electro-transferred to polyvinylidene difluoride membrane (Thermo scientific) for 90 min at 100 V. The membrane was blocked with 5% BSA/TBST for 1 hour at room temperature and incubated with the primary antibody against TRPC3 (1:1000 dilution, Abcam) or β-tubulin (1:2500, Abcam) in 5% BSA/TBST overnight at 4 °C. The membrane was then washed in TBST followed by incubation with secondary IRDye800®-infrared fluorescent dye-conjugated goat anti-rabbit antibody (1:10000, Rockland) in TBST for 1 hour at room temperature. Imaging was performed by using Odyssey gel imaging scanner (Li-Cor Biosciences) at a wavelength of 800 nm and band intensities were analyzed by Quantity One imaging software (Version 4.6.6, Bio-Rad). β-tubulin served as internal loading control.
Co-immunoprecipitation
Experiments were performed using methods described elsewhere28 with slight modifications. Proteins were extracted from PCAECs using a detergent extraction buffer containing 1% (vol/vol) Nonidet P-40, 150 mmol/L NaCl, and 20 mmol/L Tris-HCl, pH 8.0, with the addition of protease and phosphatase inhibitor cocktail (Roche Diagnostics). Extracted protein (1000 μg) was incubated overnight with 10 μg of antibody against TRPC3 (Alomone Labs), KCa2.3 (Alomone Labs), or KCa3.1 (Alomone Labs) at 4 °C on a rocking platform. Protein A agarose was added and incubated at 4 °C for another 4 hours. Immunoprecipitates were then washed twice with saline and resolved on 8% sodium dodecyl sulphate-polyacrylamide electrophoresis gel. For immunoblots, the polyvinylidene difluoride membrane carrying the transferred proteins was incubated at 4 °C overnight with designated primary antibodies diluted (1:200) in TBST buffer containing 0.1% Tween 20 and 5% BSA. Immunodetection was accomplished by 1-hour incubation with secondary IRDye800®-infrared fluorescent dye-conjugated goat anti-rabbit antibody (1:10000, Rockland) in TBST at room temperature. Imaging was performed at a wavelength of 800 nm with using Odyssey gel imaging scanner (Li-Cor Biosciences). To complete the protein-protein interaction analysis of TRPC3 and KCa channels, immunoprecipitate obtained with anti-TRPC3 antibody was subjected to immunoblot analysis using anti-KCa3.1 or anti-KCa2.3 antibodies. The immunoprecipitation and immunoblot experiments were then performed in reversed order, i.e., immunoprecipitation with anti-KCa3.1 or anti-KCa2.3 antibody, followed by immunoblotting with anti-TRPC3 antibody.
Isometric force study
Porcine small coronary arteries with the diameter of 300~500 µm were dissected from the branches of LAD and cut into cylindrical rings with 2-mm in length. The rings were mounted, normalized, and equilibrated in a four-channel Mulvany myograph (Model 610 M, J.P. Trading, Aarhus, Denmark) as previously described8, 16, 19, 25. The IKCa and SKCa channel-dependent, EDHF-mediated relaxation was studied in U46619-preconstricted rings upon bradykinin (−10~−6.5 LogM) stimulation in the presence of cyclooxygenase inhibitor indomethacin (Indo, 7 μmol/L), NOS inhibitor NG-nitro-L-arginine (L-NNA, 300 μmol/L), and NO scavenger oxyhemoglobin (HbO, 20 μmol/L)29, 30.
Induction of H-R
As described in our previous studies8, 16, 31, small coronary arteries or primary cultured PCAECs (seeded on glass coverslips) were placed in a plastic cover-sealed chamber filled with bath solution that was continuously bubbled with 95%N2-5%CO2 at 37.0 ± 0.1 °C to induce hypoxia exposure (PO2 < 5 mmHg, monitored by Oxygen Meter Model 781, Strathkelvin Instrument, Glasgow, Scotland, UK) for 60 min, followed by 30 min of reoxygenation before isometric force study and voltage-clamp recording in relevant protocols. For studies using coronary arteries, the bath solution was Krebs solution (pH 7.4) that contains (in mmol/L): Na+ 143.4, K+ 5.9, Ca2+ 2.5, Mg2+ 1.2, Cl− 128.7, HCO3 − 25, SO4 2− 1.2, H2PO4− 1.2, and glucose 11.1. While in studies with PCAECs, the bath solution was RPMI-1640 medium.
Data analysis
Data were presented as mean ± s.e.m. Statistical analyses were performed using unpaired t test or one-way ANOVA followed by Scheffe test (SPSS, version 20) when appropriate. Differences were considered significant when p < 0.05.
References
Edwards, G., Feletou, M. & Weston, A. H. Endothelium-derived hyperpolarising factors and associated pathways: a synopsis. Pflugers Archiv: European journal of physiology 459, 863–879, doi:10.1007/s00424-010-0817-1 (2010).
Gaete, P. S., Lillo, M. A., Ardiles, N. M., Perez, F. R. & Figueroa, X. F. Ca2+ -activated K+ channels of small and intermediate conductance control eNOS activation through NAD(P)H oxidase. Free radical biology & medicine 52, 860–870, doi:10.1016/j.freeradbiomed.2011.11.036 (2012).
Sheng, J. Z. & Braun, A. P. Small- and intermediate-conductance Ca2+ -activated K+ channels directly control agonist-evoked nitric oxide synthesis in human vascular endothelial cells. American journal of physiology. Cell physiology 293, C458–467, doi:10.1152/ajpcell.00036.2007 (2007).
Grgic, I., Kaistha, B. P., Hoyer, J. & Kohler, R. Endothelial Ca+ -activated K+ channels in normal and impaired EDHF-dilator responses–relevance to cardiovascular pathologies and drug discovery. British journal of pharmacology 157, 509–526, doi:10.1111/j.1476-5381.2009.00132.x (2009).
Nilius, B. & Droogmans, G. Ion channels and their functional role in vascular endothelium. Physiological reviews 81, 1415–1459 (2001).
Yao, X. & Garland, C. J. Recent developments in vascular endothelial cell transient receptor potential channels. Circulation research 97, 853–863, doi:10.1161/01.RES.0000187473.85419.3e (2005).
Smedlund, K. & Vazquez, G. Involvement of native TRPC3 proteins in ATP-dependent expression of VCAM-1 and monocyte adherence in coronary artery endothelial cells. Arteriosclerosis, thrombosis, and vascular biology 28, 2049–2055, doi:10.1161/ATVBAHA.108.175356 (2008).
Huang, J. H. et al. TRPC3 channel contributes to nitric oxide release: significance during normoxia and hypoxia-reoxygenation. Cardiovascular research 91, 472–482, doi:10.1093/cvr/cvr102 (2011).
Gao, G. et al. Role of TRPC3 channel in human internal mammary artery. Archives of medical research 43, 431–437, doi:10.1016/j.arcmed.2012.08.010 (2012).
Smedlund, K., Bah, M. & Vazquez, G. On the role of endothelial TRPC3 channels in endothelial dysfunction and cardiovascular disease. Cardiovascular & hematological agents in medicinal chemistry 10, 265–274 (2012).
Moens, A. L., Claeys, M. J., Timmermans, J. P. & Vrints, C. J. Myocardial ischemia/reperfusion-injury, a clinical view on a complex pathophysiological process. International journal of cardiology 100, 179–190, doi:10.1016/j.ijcard.2004.04.013 (2005).
Veres, G. et al. Endothelial dysfunction of bypass graft: direct comparison of in vitro and in vivo models of ischemia-reperfusion injury. PloS one 10, e0124025, doi:10.1371/journal.pone.0124025 (2015).
Yang, Q., He, G. W., Underwood, M. J. & Yu, C. M. Cellular and molecular mechanisms of endothelial ischemia/reperfusion injury: perspectives and implications for postischemic myocardial protection. Am J Transl Res 8, 765–777 (2016).
Sanchez, A. et al. Goat cerebrovascular reactivity to ADP after ischemia-reperfusion. Role of nitric oxide, prostanoids and reactive oxygen species. Brain research 1120, 114–123, doi:10.1016/j.brainres.2006.08.061 (2006).
Feng, J. et al. Calcium-activated potassium channels contribute to human coronary microvascular dysfunction after cardioplegic arrest. Circulation 118, S46–51, doi:10.1161/CIRCULATIONAHA.107.755827 (2008).
Yang, Q., Huang, J. H., Man, Y. B., Yao, X. Q. & He, G. W. Use of intermediate/small conductance calcium-activated potassium-channel activator for endothelial protection. The Journal of thoracic and cardiovascular surgery 141, 501–510, 510 e501, doi:10.1016/j.jtcvs.2010.04.005 (2011).
Senadheera, S. et al. Transient receptor potential canonical type 3 channels facilitate endothelium-derived hyperpolarization-mediated resistance artery vasodilator activity. Cardiovascular research 95, 439–447, doi:10.1093/cvr/cvs208 (2012).
Kochukov, M. Y., Balasubramanian, A., Abramowitz, J., Birnbaumer, L. & Marrelli, S. P. Activation of endothelial transient receptor potential C3 channel is required for small conductance calcium-activated potassium channel activation and sustained endothelial hyperpolarization and vasodilation of cerebral artery. Journal of the American Heart Association 3, doi:10.1161/JAHA.114.000913 (2014).
Yang, Q., Huang, J. H., Yao, X. Q., Underwood, M. J. & Yu, C. M. Activation of canonical transient receptor potential channels preserves Ca2+ entry and endothelium-derived hyperpolarizing factor-mediated function in vitro in porcine coronary endothelial cells and coronary arteries under conditions of hyperkalemia. The Journal of thoracic and cardiovascular surgery 148, 1665–1673, e1661, doi:10.1016/j.jtcvs.2014.02.026 (2014).
Kochukov, M. Y., Balasubramanian, A., Noel, R. C. & Marrelli, S. P. Role of TRPC1 and TRPC3 channels in contraction and relaxation of mouse thoracic aorta. Journal of vascular research 50, 11–20, doi:10.1159/000342461000342461 (2013).
Liu, C. L., Huang, Y., Ngai, C. Y., Leung, Y. K. & Yao, X. Q. TRPC3 is involved in flow- and bradykinin-induced vasodilation in rat small mesenteric arteries. Acta pharmacologica Sinica 27, 981–990, doi:10.1111/j.1745-7254.2006.00354.x (2006).
Kwan, H. Y. et al. TRPC1 associates with BK(Ca) channel to form a signal complex in vascular smooth muscle cells. Circulation research 104, 670–678, doi:10.1161/CIRCRESAHA.108.188748 (2009).
Kim, E. Y., Alvarez-Baron, C. P. & Dryer, S. E. Canonical transient receptor potential channel (TRPC)3 and TRPC6 associate with large-conductance Ca2+ -activated K+ (BKCa) channels: role in BKCa trafficking to the surface of cultured podocytes. Molecular pharmacology 75, 466–477, doi:10.1124/mol.108.051912 (2009).
Burnham, M. P. et al. Characterization of an apamin-sensitive small-conductance Ca(2+)-activated K(+) channel in porcine coronary artery endothelium: relevance to EDHF. British journal of pharmacology 135, 1133–1143, doi:10.1038/sj.bjp.0704551 (2002).
Wang, X. C. et al. ER stress mediates homocysteine-induced endothelial dysfunction: Modulation of IKCa and SKCa channels. Atherosclerosis 242, 191–198, doi:10.1016/j.atherosclerosis.2015.07.021 (2015).
Sandow, S. L., Neylon, C. B., Chen, M. X. & Garland, C. J. Spatial separation of endothelial small- and intermediate-conductance calcium-activated potassium channels (K(Ca)) and connexins: possible relationship to vasodilator function? Journal of anatomy 209, 689–698, doi:10.1111/j.1469-7580.2006.00647.x (2006).
Bychkov, R. et al. Characterization of a charybdotoxin-sensitive intermediate conductance Ca2+ -activated K+ channel in porcine coronary endothelium: relevance to EDHF. British journal of pharmacology 137, 1346–1354, doi:10.1038/sj.bjp.0705057 (2002).
Zhang, P. et al. Nitric oxide and protein kinase G act on TRPC1 to inhibit 11, 12-EET-induced vascular relaxation. Cardiovascular research 104, 138–146, doi:10.1093/cvr/cvu190 (2014).
Ge, Z. D., Zhang, X. H., Fung, P. C. & He, G. W. Endothelium-dependent hyperpolarization and relaxation resistance to N(G)-nitro-L-arginine and indomethacin in coronary circulation. Cardiovascular research 46, 547–556 (2000).
Yang, Q., Ge, Z. D., Yang, C. Q., Huang, Y. & He, G. W. Bioassay of endothelium-derived hyperpolarizing factor with abolishment of nitric oxide and the role of gap junctions in the porcine coronary circulation. Drug Develop Res 58, 99–110, doi:10.1002/ddr.10137 (2003).
Xue, H. M., He, G. W., Huang, J. H. & Yang, Q. New strategy of endothelial protection in cardiac surgery: use of enhancer of endothelial nitric oxide synthase. World journal of surgery 34, 1461–1469, doi:10.1007/s00268-010-0520-6 (2010).
Acknowledgements
This work was supported by grants from Research Grant Council of Hong Kong (GRF CUHK4774/12M & CUHK14118414), National Natural Science Foundation of China 81200123, Lui Che Woo Institute of Innovative Medicine (CARE theme 8303303).
Author information
Authors and Affiliations
Contributions
X.-C.W., W.-T. S., J.F., and J.-H.H. performed experiments; C.-M.Y., M.-J.U., and G.-W.H., contributed to data analysis, involved in scientific discussion and paper writing; Q.Y. designed the study, supervised experiments, and wrote the paper.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, XC., Sun, WT., Fu, J. et al. Impairment of Coronary Endothelial Function by Hypoxia-Reoxygenation Involves TRPC3 Inhibition-mediated KCa Channel Dysfunction: Implication in Ischemia-Reperfusion Injury. Sci Rep 7, 5895 (2017). https://doi.org/10.1038/s41598-017-06247-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-06247-3
This article is cited by
-
Canonical Transient Receptor Potential Channel 3 Contributes to Febrile Seizure Inducing Neuronal Cell Death and Neuroinflammation
Cellular and Molecular Neurobiology (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.