Abstract
The survival benefits of aortic valve replacement (AVR) in the different flow-gradient states of severe aortic stenosis (AS) is not known. A comprehensive search in PubMed/MEDLINE, Embase, Cochrane Library, CNKI and OpenGrey were conducted to identify studies that investigated the prognosis of severe AS (effective orifice area ≤1.0 cm2) and left ventricular ejection fraction ≥50%. Severe AS was stratified by mean pressure gradient [threshold of 40 mmHg; high-gradient (HG) and low-gradient (LG)] and stroke volume index [threshold of 35 ml/m2; normal-flow (NL) and low-flow (LF)]. Network meta-analysis was conducted to assess all-cause mortality among each AS sub-type with rate ratio (RR) reported. The effects of AVR on prognosis were examined using network meta-regression. In the pooled analysis (15 studies and 9,737 patients), LF states (both HG and LG) were associated with increased mortality rate (LFLG: RR 1.88; 95% CI: 1.43-2.46; LFHG: RR: 1.77; 95% CI: 1.16-2.70) compared to moderate AS; and NF states in both HG and LG had similar prognosis as moderate AS (NFLG: RR 1.11; 95% CI: 0.81-1.53; NFHG: RR 1.16; 95% CI: 0.82-1.64). AVR conferred different survival benefits: it was most effective in NFHG (RR with AVR /RR without AVR : 0.43; 95% CI: 0.22-0.82) and least in LFLG (RR with AVR /RR without AVR : 1.19; 95% CI: 0.74-1.94).
Similar content being viewed by others
Introduction
The prevalence of calcific aortic stenosis (AS) increases with age, occurring in 3% to 5% of individuals 75 years and above1. Contemporary guidelines from the American Heart Association/American College of Cardiology and the European Society of Cardiology recommend aortic valve replacement (AVR) in patients with severe aortic stenosis and evidence of decompensation, either in the form of symptoms or left ventricular systolic dysfunction2, 3.
Severe AS is defined by an effective orifice area (EOA) of <1.0 cm2, and a mean pressure gradient (MPG) > 40 mmHg or peak aortic jet velocity (Vm) > 4 m/s4. It has recently been proposed that severe AS with preserved systolic function can be further stratified into 4 flow-gradient states: normal flow-low gradient (NFLG), low flow-low gradient (LFLG), normal flow-high gradient (NFHG), and low flow-high gradient (LFHG) severe AS5. Paradoxical low flow states (indexed stroke volumes <35 ml/m2) account for a proportion of patients with discordant small EOA and low mean pressure gradient (MPG) despite preserved systolic function6, 7. First described in 2007, LF with preserved systolic function (paradoxical LF) AS was associated with increased all-cause mortality compared to NF 8. Subsequent studies have suggested that paradoxical LG AS may be less severe compared to HG states and a prognosis more akin to moderate disease9, 10, yet others have reported that it had the worst prognosis compared to all the other flow-gradient states5, 11. Two meta-analyses demonstrated poor prognosis associated with LFLG AS; and prognosis of severe aortic stenosis (regardless of flow-gradient states) improved with AVR compared to conservative management12, 13. However, the relative benefits of AVR may be different in patients with different flow-gradient states.
Network meta-analysis is an approach that incorporates evidence from direct comparisons with indirect comparisons that are extracted from multiple studies14. Using network meta-analysis, we aimed to assess the prognosis associated with the different flow-gradient states of severe AS and preserved systolic function. We further examined the relative effects of AVR on survival in individuals with different flow-gradient states, with moderate AS as the reference.
Methods
Literature Search and Eligibility Criteria
A comprehensive literature search was performed on electronic databases: PubMed/MEDLINE (1946 onwards), Embase (1974 onwards), Cochrane library (1992 onwards), China Knowledge Research Integrated Database (CNKI; 1979 onwards) and OpenGrey (2000 onwards) until 28 February 2017. The specific concepts used in the search strategy were “severe aortic stenosis”, “flow”, “gradient” and “prognosis”. We conducted literature search using Medical Subject Headings (MeSH) or Emtree, and free text terms (see online supplemental data). There were no restrictions on language. All the bibliography listed in review papers and included publications were also checked.
Two investigators (CWLC and QSZ) independently screened for eligible studies based on pre-defined eligibility criteria. Full-text studies that examined the prognosis of severe AS (EOA ≤1.0 cm2 stratified by flow and gradient states) with preserved systolic function (LVEF ≥50%) and published after the introduction of the classification system in 2007 were included. We excluded studies that examined prognosis in AS with impaired systolic function (LVEF <50%) and those that did not specify flow-gradient states. Case reports, commentaries and letters-to-editors were also excluded. Flow states were categorized as according to low (<35 ml/m2) and normal flow (≥35 ml/m2). Low and high MPG were defined by a gradient of <40 mmHg and ≥40 mmHg, respectively. Therefore, 4 subgroups of severe AS were defined: LFLG, NFLG, LFHG and NFHG.
Data extraction and quality assessment
The following data were extracted from the included studies: (1) study characteristics (publication year, patient population and the type of cohort study); (2) baseline characteristics (mean age, proportion of symptomatic status, number of males/females and proportion of patients with hypertension, coronary artery disease and diabetes); (3) valve severity and flow states; and (4) outcome events (all-cause mortality regardless of AVR). In publications with survival curves, the cumulative survival rates were estimated by digitizing the plots15, 16.
The quality of each study was evaluated, using the Quality In Prognosis Studies tool (QUIPS tool), by two independent investigators (QSZ and LMS)17. Six domains (study participation study attrition, prognostic factor measurement, outcome measurement, study confounding and statistical analysis and reporting) were evaluated to assess the risk of bias in prognostic studies. For each of the 6 domains in the QUIPS tool, responses to the signaling questions are taken together to arrive at the judgment of “High”, “Moderate” or “Low” risk of bias. Any disagreement in quality assessment was resolved by discussion and consensus.
Statistical analysis
A network geometry was constructed based on the included studies for subgroups of severe AS. Each node represented a subgroup and its size was weighted by the number of subjects of each subgroup. The connecting line between two nodes meant direct comparison was existed and its thickness was determined by the number of studies included.
Network meta-analysis, comparing the prognosis of the different severe AS sub-groups, was performed using a multivariate meta-regression model with random-effects, adopting a frequentist approach18, 19. The model allows for the inclusion of potential covariates, and accounts for the correlations from multi-arm trials, and rate ratio (RR) of each subgroup was estimated20.
To rank the prognosis for all the groups, we used surface under the cumulative ranking (SUCRA) values21. Rank probabilities of all the groups were first estimated under a Bayesian framework. A step function was then applied to summarize the cumulative ranking for estimating the SUCRA values of each group, ranging from 0 to 1. Thus, a large SUCRA value indicated a better prognosis.
Meta-regression was used to investigate the effects of AVR on survival in the different flow-gradient patterns of AS19. The node-splitting approach and inconsistency model were used to test the consistency assumption22. The former method involved fitting a series of node-splitting models, with one model for each sub-group pairing for which there was direct and indirect evidence23. The latter method first fits an inconsistency model and then conduct a global Wald test to check whether there is significant inconsistency exists14.
The network meta-analyses and meta-regression were implemented by Stata/MP 13 with network and network graphs package14, 24, 25.
Results
Study characteristics and network geometry
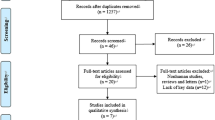
From 1,274 potential studies identified from the initial search, 15 cohort studies (n = 9,737 individuals) satisfied inclusion/exclusion criteria and were included in this meta-analysis10, 11, 26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47 (Fig. 1; Table 1). No randomized controlled studies were found. The mean age was 76±6 years and 43% were males. Of note, 29%, 38% and 63% of individuals had diabetes, coronary artery disease and hypertension respectively, with the duration of follow-up varied between 0.8 and 4.9 years (Tables 1 and 2). Twelve studies examined the effects of AVR on prognosis.
PRISMA flowchart of study selection. The systematic review and meta-analysis was conducted according to the guidelines recommended by PRISMA48.
Of the 9,737 individuals in the studies, 39% (n = 3,803), 29% (n = 2,842) and 32% (n = 3,092) of individuals had moderate, HG and LG severe AS, respectively. Amongst the individuals with LG AS, 57% (n = 1,762) and 43% (n = 1,330) had low and normal flow, respectively. Conversely, significantly more individuals with HG had normal flow (82%; n = 2,330) compared to low flow states (18%; n = 512). Moderate AS was used as the reference group for comparison in this study.
The quality of all the studies demonstrated low to moderate risk of bias in the six domains assessed (Table 3). The network geometry was constructed (Fig. 2).
Network meta-analysis results
In both HG and LG AS, low flow states were associated with increased all-cause mortality (LFLG: RR 1.88; 95% CI: 1.43 to 2.46; LFHG: RR: 1.77; 95% CI: 1.16 to 2.70; Table 4). Of note, both low flow subgroups had similar mortality rate (the ratio of LFHG and LFLG RRs was 0.94; 95% CI: 0.67 to 1.33). Conversely, normal flow states in both HG and LG had similar prognosis compared to moderate AS (NFLG: RR 1.11; 95% CI: 0.81 to 1.53; NFHG: RR 1.16; 95% CI: 0.82 to 1.64; Table 4). Based on the SUCRA values of each subgroup, the prognosis of the different flow-gradient states ranked from best to worst would be: NFLG, NFHG, LFHG and LFLG (Fig. 3). Results from both node-splitting method and inconsistency model showed no evidence of violating the assumption of consistency between direct and indirect comparison (P = 0.507; Fig. 4).
Comparative effects of AVR on survival
To examine the relative effects of AVR on survival in individuals with different flow-gradient states, we compared the RRs before and after adjusting for AVR (Fig. 5). In NFHG severe AS, the RR improved from 1.89 (95% CI: 1.25 to 2.84) to 1.16 (95% CI: 0.82 to 1.64) with AVR (RR with AVR /RR without AVR : 0.43; 95% CI: 0.22 to 0.82). Whilst AVR conferred a survival benefit for NFHG, it may not benefit all patients with LFLG equally. The mortality RR of LFLG increased from 1.59 (95% CI: 1.24 to 2.04) to 1.88 (95% CI: 1.43 to 2.46) with AVR (RR with AVR /RR without AVR : 1.19; 95% CI: 0.74 to 1.94; Fig. 5). There was a trend towards benefit in severe AS patients with LFHG (RR with AVR /RR without AVR : 0.63; 95% CI: 0.24 to 1.67) and NFLG (RR with AVR /RR without AVR : 0.87; 95% CI: 0.45 to 1.68).
Similar findings were observed when traditional pair-wise comparisons were performed (Fig. 6). Compared to medical therapy, AVR improved outcomes in all flow-gradient states of severe AS but with different relative benefits. NFHG severe AS derived the most relative benefits from AVR (RR: 0.11; 95% CI: 0.07 to 0.20) compared to LFLG severe AS (RR: 0.32; 95% CI: 0.25 to 0.42).
Discussion
Our network meta-analysis investigated the prognostic effects of AVR on the different flow-gradient states of severe AS. Overall, we demonstrated that the risk of all-cause mortality in severe AS was associated with low flow states, and not valvular gradients. Normal flow states had similar prognosis to moderate AS. Moreover, the relative survival benefits conferred by AVR were different in patients with severe AS, depending on flow-gradient states. Individuals with NFHG derived the greatest survival benefit from AVR among all the subgroups of severe AS.
The traditional pair-wise meta-analysis can only synthesize evidence from studies with direct comparisons of two arms being tested. However, it is difficult to rank the prognosis of each subgroup of severe AS, as such direct evidence is limited, i.e. only 4 out of 15 studies included all the flow-gradient states of interest (LFLG, NFLG, LFHG and NFHG). Therefore, the traditional pairwise approach is not ideal to comprehensively investigate the prognosis of the different flow-gradient states from the existing evidence. By synthesizing direct and indirect evidence using network meta-analysis, we were able to examine the prognosis of all the different flow-gradient states in severe AS.
In our study, low flow states (not valvular gradient) in severe AS were associated with an increased risk of all-cause mortality. Compared to two recent meta-analyses that have combined flow states in HG12, 13, we demonstrated that HG severe AS can further be risk-stratified based on flow patterns: the prognosis of NFHG was similar to moderate AS, and better than LFHG. These findings are consistent with a recent study that demonstrated a continuous association between adverse events and reduced stroke volumes in patients with AS and preserved systolic function, independent of valvular gradient49. The complex interaction of the valve, comorbid medical conditions and the myocardium account for the different flow-gradient states in AS50, 51. In the presence of preserved systolic function, low flow states can be present in individuals with significant myocardial hypertrophy. Other factors contributing to low flow states such as atrial fibrillation (41% in those with LFLG in the pooled studies), hypertension and concomitant valvular heart disease (mitral stenosis or mitral regurgitation) can also result in increased mortality.
Although patients with severe AS (regardless of flow or gradient) have improved outcomes with AVR compared to conservative management12, it is possible AVR would confer different survival benefits since the prognosis varied across the flow-gradient states. Our study adds novelty by demonstrating the relative survival benefits of AVR vary with flow-gradient states. Patients with classically severe (NFHG) AS derived the most benefit from AVR whilst the risk of mortality was not completely modified by AVR in those with paradoxical LFLG severe AS. These findings were confirmed using traditional pair-wise comparisons. The role of AVR in the other flow-gradient states should be interpreted with caution. There was a trend towards benefit in severe AS patients with LFHG and NFLG. The wide confidence limits may be explained by the relatively smaller number of individuals compared to other flow-gradient states.
Clinical Implications
These findings have important clinical implications. Paradoxical LG severe AS may be conceptualized as a heterogeneous condition akin to heart failure with preserved ejection fraction (HFpEF)51. Both conditions share similar clinical characteristics and mechanisms of cardiac adaptation12, 51, 52. Similar to paradoxical LG severe AS, a high proportion of adverse events are related to non-cardiovascular comorbidities in HFpEF52. Patients with paradoxical LFLG severe AS may benefit from AVR, as currently recommended by both the ACC/AHA and ESC (Class IIa)2, 3. For reasons discussed above, AVR may not completely ameliorate the risks in those with paradoxical LG severe AS. Therefore, it is crucial to confirm severity of disease and improve risk stratification using either imaging (stress echocardiography, aortic valve CT calcium score and cardiovascular magnetic resonance) or biochemical markers53,54,55,56,57,58,59. However, the benefits of AVR in at-risk individuals identified using such a strategy will need to be carefully tested in a clinical trial.
Study Limitations
Due to incomplete data we were unable to assess the prognosis on cardiovascular mortality. The adjustment of AVR in the current analysis can only be conducted at the study-level, which might not accurately reflect the prognosis of the individual patient. In the absence of any randomized controlled studies, the effects of AVR may be confounded by potential biases inherent to the observational nature of the studies. For example, AVR in individuals with LFLG may be delayed because of an uncertainty in diagnosis and management. Potential study inconsistency may affect the validity of the network meta-analysis. However, we have carefully assessed for any potential violation of the consistency assumption. Similar estimates from direct and indirect comparisons were demonstrated and formal statistical testing did not reveal violation of consistency.
Conclusions
Low flow states (regardless of valvular gradient) were associated with increased all-cause mortality amongst individuals with severe AS. Of all the flow-gradient states, NFHG was associated with the greatest survival benefit from AVR. Properly designed randomized studies are crucially needed to clarify the role of AVR in individuals with LFLG severe AS.
References
Nkomo, V. T. et al. Burden of valvular heart diseases: a population-based study. Lancet 368, 1005–1011 (2006).
Nishimura, R. A. et al. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 63, e57–e185 (2014).
Vahanian, A. et al. Guidelines on the management of valvular heart disease (version 2012). Eur Heart J. 33, 2451–2496 (2012).
Baumgartner, H. et al. Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr 22, 1–23 (2009).
Lancellotti, P. et al. Clinical outcome in asymptomatic severe aortic stenosis: insights from the new proposed aortic stenosis grading classification. J Am Coll Cardiol. 59, 235–243 (2012).
Chin, C. W. L. et al. Echocardiography underestimates stroke volume and aortic valve area: implications for patients with small-area low-gradient aortic stenosis. Can J Cardiol. 30, 1064–1072 (2014).
Minners, J. et al. Inconsistencies of echocardiographic criteria for the grading of aortic valve stenosis. Eur Heart J. 29, 1043–1048 (2008).
Hachicha, Z., Dumesnil, J. G., Bogaty, P. & Pibarot, P. Paradoxical low-flow, low-gradient severe aortic stenosis despite preserved ejection fraction is associated with higher afterload and reduced survival. Circulation 115, 2856–2864 (2007).
Jander, N. et al. Outcome of patients with low-gradient “severe” aortic stenosis and preserved ejection fraction. Circulation 123, 887–895 (2011).
Maes, F. et al. Natural history of paradoxical low-gradient severe aortic stenosis. Circ Cardiovasc Imaging. 7, 714–722 (2014).
Eleid, M. F. et al. Flow-gradient patterns in severe aortic stenosis with preserved ejection fraction: clinical characteristics and predictors of survival. Circulation 128, 1781–9 (2013).
Dayan, V. et al. Outcome and impact of aortic valve replacement in patients with preserved LVEF and low-gradient aortic stenosis. J Am Coll Cardiol. 66, 2594–2603 (2015).
Bavishi, C., Balasundaram, K. & Argulian, E. Integration of flow-gradient patterns into clinical decision making for patients with suspected severe aortic stenosis and preserved LVEF: a systematic review of evidence and meta-analysis. JACC: Cardiovascular Imaging 9, 1255–1263 (2016).
White, I. R. Network meta-analysis. The Stata Journal 15, 951–985 (2015).
Parmar, M. K., Torri, V. & Stewart, L. Extracting summary statistics to perform meta‐analyses of the published literature for survival endpoints. Stat Med 17, 2815–2834 (1998).
WebPlotDigitizer v. 3.9 (2015).
Hayden, J. A., van der Windt, D. A., Cartwright, J. L., CÃ, P. & Bombardier, C. Assessing bias in studies of prognostic factors. Ann Intern Med. 158, 280–286 (2013).
Higgins, J. et al. Consistency and inconsistency in network meta‐analysis: concepts and models for multi‐arm studies. Res Synth Methods 3, 98–110 (2012).
White, I. R., Barrett, J. K., Jackson, D. & Higgins, J. Consistency and inconsistency in network meta‐analysis: model estimation using multivariate meta‐regression. Res Synth Methods 3, 111–125 (2012).
White, I. R. Multivariate random-effects meta-regression: updates to mvmeta. The Stata Journal 11, 255 (2011).
Salanti, G., Ades, A. & Ioannidis, J. P. Graphical methods and numerical summaries for presenting results from multiple-treatment meta-analysis: an overview and tutorial. Journal of clinical epidemiology 64, 163–171 (2011).
Dias, S., Welton, N., Caldwell, D. & Ades, A. Checking consistency in mixed treatment comparison meta‐analysis. Stat Med 29, 932–944 (2010).
Donegan, S., Williamson, P., D’Alessandro, U. & Tudur Smith, C. Assessing key assumptions of network meta‐analysis: a review of methods. Res Synth Methods 4, 291–323 (2013).
StataCorp. Stata Statistical Software: Release 13. (2013).
Chaimani, A., Higgins, J. P., Mavridis, D., Spyridonos, P. & Salanti, G. Graphical tools for network meta-analysis in STATA. PloS one 8, e76654 (2013).
Barasch, E. et al. Severe isolated aortic stenosis with normal left ventricular systolic function and low transvalvular gradients: pathophysiologic and prognostic insights. J Heart Valve Dis. 17, 81–88 (2008).
Belkin, R. N., Khalique, O., Aronow, W. S., Ahn, C. & Sharma, M. Outcomes and Survival with Aortic Valve Replacement Compared with Medical Therapy in Patients with Low‐, Moderate‐, and Severe‐Gradient Severe Aortic Stenosis and Normal Left Ventricular Ejection Fraction. Echocardiogr. 28, 378–387 (2011).
Biner, S. et al. Outcome of transcatheter aortic valve implantation in patients with low-gradient severe aortic stenosis and preserved left ventricular ejection fraction. Am J Cardiol. 113, 348–354 (2014).
Clavel, M.-A. et al. Outcome of patients with aortic stenosis, small valve area, and low-flow, low-gradient despite preserved left ventricular ejection fraction. J Am Coll Cardiol. 60, 1259–1267 (2012).
Debry, N. et al. Transcatheter aortic valve implantation for paradoxical low‐flow low‐gradient aortic stenosis patients. Catheter Cardiovas Interv. 87, 797–804 (2016).
Herrmann, S. et al. Low-gradient aortic valve stenosis: myocardial fibrosis and its influence on function and outcome. J Am Coll Cardiol. 58, 402–412 (2011).
Kamperidis, V. et al. Impact of flow and left ventricular strain on outcome of patients with preserved left ventricular ejection fraction and low gradient severe aortic stenosis undergoing aortic valve replacement. Am J Cardiol. 114, 1875–1881 (2014).
Lauten, A. et al. TAVI for low-flow, low-gradient severe aortic stenosis with preserved or reduced ejection fraction: a subgroup analysis from the German Aortic Valve Registry (GARY). EuroIntervention. 10, 850–859 (2014).
Lopez-Marco, A. et al. Low-flow low-gradient aortic stenosis: surgical outcomes and mid-term results after isolated aortic valve replacement. Eur J Cardiothorac Surg. 49, 1685–90 (2016).
Maor, E. et al. Relation between stroke volume index to risk of death in patients with low-gradient severe aortic stenosis and preserved left ventricular function. Am J Cardiol. 114, 449–455 (2014).
Mehrotra, P. et al. Differential left ventricular remodelling and longitudinal function distinguishes low flow from normal-flow preserved ejection fraction low-gradient severe aortic stenosis. Eur Heart J. 34, 1906–1914 (2013).
Melis, G. et al. Systolic volume index by Doppler echocardiography is an useful marker for stratification and prognostic evaluation in patients with severe aortic stenosis and preserved ejection fraction. Rev Esp Cardiol (Engl Ed) 66, 261–268 (2013).
Mohty, D. et al. Outcome and Impact of Surgery in Paradoxical Low-Flow, Low-Gradient Severe Aortic Stenosis and Preserved Left Ventricular Ejection Fraction A Cardiac Catheterization Study. Circulation 128, S235–S242 (2013).
O’Sullivan, C. J. et al. Clinical outcomes of patients with low-flow, low-gradient, severe aortic stenosis and either preserved or reduced ejection fraction undergoing transcatheter aortic valve implantation. Eur Heart J. 34, 3437–3450 (2013).
Parikh, R. et al. Outcomes of surgical aortic valve replacement for severe aortic stenosis: Incorporation of left ventricular systolic function and stroke volume index. J Thorac Cardiovasc Surg. 149(1558–1566), e1551 (2015).
Reinthaler, M. et al. Paradoxical low-flow, low-gradient severe aortic valve stenosis: an entity with limited improvement following transcatheter aortic valve implantation. J Heart Valve Dis. 23, 441–449 (2014).
Rezzoug, N. et al. Prevalence and Prognostic Impact of Valve Area—Gradient Patterns in Patients ≥80 Years With Moderate-to-Severe Aortic Stenosis (from the Prospective BELFRAIL Study). Am J Cardiol. 116, 925–932 (2015).
Romero, J. et al. Outcomes in patients with various forms of aortic stenosis including those with low-flow low-gradient normal and low ejection fraction. Am J Cardiol. 114, 1069–1074 (2014).
Schewel, J. et al. Invasive hemodynamic assessments during transcatheter aortic valve implantation: comparison of patient outcomes in higher vs. lower transvalvular gradients with respect to left ventricular ejection fraction. Clin Res Cardiol. 105, 59–71 (2016).
Tribouilloy, C. et al. Low-gradient, low-flow severe aortic stenosis with preserved left ventricular ejection fraction: characteristics, outcome, and implications for surgery. J Am Coll Cardiol. 65, 55–66 (2015).
Xingli, F. et al. Impact of stroke volume and gradient on the clinical outcome of patients with aortic stenosis who underwent aortic valve replacement. International Journal of Cardiovascular Disease 3, 202–206 (2015).
Yamashita, E. et al. Prognostic value of paradoxical low-gradient severe aortic stenosis in Japan: Japanese Multicenter Aortic Stenosis Study, Retrospective (JUST-R) Registry. J Cardiol. 65, 360–368 (2015).
Annals of Internal Medicine (OPEN ACCESS) Moher, D., Liberati, A., Tetzlaff, J. & Altman, D. G. The PRISMA Group. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. Ann Intern Med, 151(4) (2009).
Eleid, M. F. et al. Survival by stroke volume index in patients with low-gradient normal EF severe aortic stenosis. Heart 101, 23–9 (2014).
Chin, C. W. et al. Markers of left ventricular decompensation in aortic stenosis. Exp Rev Cardiovasc Ther. 12, 901–12 (2014).
Chin, C. W., Ding, Z. P., Lam, C. S. & Ling, L. H. Paradoxical Low-Gradient Aortic Stenosis: The HFpEF of Aortic Stenosis. J Am Coll Cardiol. 67, 2447–2448 (2016).
Chan, M. M. & Lam, C. S. How do patients with heart failure with preserved ejection fraction die? Eur J Heart Fail. 15, 604–613 (2013).
Clavel, M. A. et al. Stress echocardiography to assess stenosis severity and predict outcome in patients with paradoxical low-flow, low-gradient aortic stenosis and preserved LVEF. JACC: Cardiovasc Imaging. 6, 175–183 (2013).
Clavel, M. A. et al. The complex nature of discordant severe calcified aortic valve disease grading: new insights from combined Doppler echocardiographic and computed tomographic study. J Am Coll Cardiol. 62, 2329–2338 (2013).
Clavel, M. A. et al. Impact of aortic valve calcification, as measured by MDCT, on survival in patients with aortic stenosis: results of an international registry study. J Am Coll Cardiol. 64, 1202–1213 (2014).
Dweck, M. R. et al. Midwall fibrosis is an independent predictor of mortality in patients with aortic stenosis. J Am Coll Cardiol. 58, 1271–1279 (2011).
Chin, C. W. et al. High-sensitivity troponin I concentrations are a marker of an advanced hypertrophic response and adverse outcomes in patients with aortic stenosis. Eur Heart J 35, 2312–21 (2014).
Chin, C. W. et al. Left ventricular hypertrophy with strain and aortic stenosis. Circulation 130, 1607–16 (2014).
Chin, C. W. et al. A clinical risk score of myocardial fibrosis predicts adverse outcomes in aortic stenosis. Eur Heart J 37, 713–23 (2015).
Author information
Authors and Affiliations
Contributions
QSZ screened for eligible studies based on pre-defined criteria, analyzed the data, assessed the quality of the included studies and drafted the manuscript. AD screened for eligible studies, extracted data from the studies and contributed to the intellectual content of the manuscript. EL screened for eligible studies, verified extracted data from the studies and contributed to the intellectual content of the manuscript. ZPD contributed to the study design and intellectual content of the manuscript. LHL contributed to the study design and intellectual content of the manuscript. LMS assessed the quality of the included studies, and contributed to the intellectual content of the study. ESYC contributed to the study design and intellectual content of the study. CWLC conceived the study idea, screened for eligible studies and drafted the manuscript with the first author.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zheng, Q., Djohan, A., Lim, E. et al. Effects of Aortic Valve Replacement on Severe Aortic Stenosis and Preserved Systolic Function: Systematic Review and Network Meta-analysis. Sci Rep 7, 5092 (2017). https://doi.org/10.1038/s41598-017-05021-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-017-05021-9
This article is cited by
-
Low-gradient severe aortic stenosis with preserved ejection fraction: how fast should we act?
The International Journal of Cardiovascular Imaging (2021)
-
Challenges and opportunities in improving left ventricular remodelling and clinical outcome following surgical and trans-catheter aortic valve replacement
Frontiers of Medicine (2021)
-
Hemodynamics of paradoxical severe aortic stenosis: insight from a pressure–volume loop analysis
Clinical Research in Cardiology (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.