Abstract
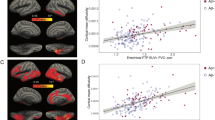
Animal models of Alzheimer’s disease have suggested that tau pathology propagation, facilitated by amyloid pathology, may occur along connected pathways. To investigate these ideas in humans, we combined amyloid scans with longitudinal data on white matter connectivity, hippocampal volume, tau positron emission tomography and memory performance in 256 cognitively healthy older individuals. Lower baseline hippocampal volume was associated with increased mean diffusivity of the connecting hippocampal cingulum bundle (HCB). HCB diffusivity predicted tau accumulation in the downstream-connected posterior cingulate cortex in amyloid-positive but not in amyloid-negative individuals. Furthermore, HCB diffusivity predicted memory decline in amyloid-positive individuals with high posterior cingulate cortex tau binding. Our results provide in vivo evidence that higher amyloid pathology strengthens the association between HCB diffusivity and tau accumulation in the downstream posterior cingulate cortex and facilitates memory decline. This confirms amyloid’s crucial role in potentiating neural vulnerability and memory decline marking the onset of preclinical Alzheimer’s disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Braak, H. & Braak, E. Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol. 82, 239–259 (1991).
Braak, H. & Braak, E. Development of Alzheimer-related neurofibrillary changes in the neocortex inversely recapitulates cortical myelogenesis. Acta Neuropathol. 92, 197–201 (1996).
Ahmed, Z. et al. A novel in vivo model of tau propagation with rapid and progressive neurofibrillary tangle pathology: the pattern of spread is determined by connectivity, not proximity. Acta Neuropathol. 127, 667–683 (2014).
Khan, U. A. et al. Molecular drivers and cortical spread of lateral entorhinal cortex dysfunction in preclinical Alzheimer’s disease. Nat. Neurosci. 17, 304–311 (2014).
Hu, W. et al. Hyperphosphorylation determines both the spread and the morphology of tau pathology. Alzheimers Dement. 12, 1066–1077 (2016).
Lewis, J. & Dickson, D. W. Propagation of tau pathology: hypotheses, discoveries, and yet unresolved questions from experimental and human brain studies. Acta Neuropathol. 131, 27–48 (2016).
Braak, H. & Del Tredici, K. Alzheimer’s pathogenesis: is there neuron-to-neuron propagation? Acta Neuropathol. 121, 589–595 (2011).
Wu, J. W. et al. Neuronal activity enhances tau propagation and tau pathology in vivo. Nat. Neurosci. 19, 1085–1092 (2016).
de Calignon, A. et al. Propagation of tau pathology in a model of early Alzheimer’s disease. Neuron 73, 685–697 (2012).
Walsh, D. M. & Selkoe, D. J. A critical appraisal of the pathogenic protein spread hypothesis of neurodegeneration. Nat. Rev. Neurosci. 17, 251–260 (2016).
Pooler, A. M. et al. Amyloid accelerates tau propagation and toxicity in a model of early Alzheimer’s disease. Acta Neuropathol. Commun. 3, 14 (2015).
Johnson, K. A. et al. Tau positron emission tomographic imaging in aging and early Alzheimer disease. Ann. Neurol. 79, 110–119 (2016).
Marquié, M. et al. Validating novel tau positron emission tomography tracer [F-18]-AV-1451 (T807) on postmortem brain tissue. Ann. Neurol. 78, 787–800 (2015).
Schöll, M. et al. PET imaging of tau deposition in the aging human brain. Neuron 89, 971–982 (2016).
Madden, D. J., Bennett, I. J. & Song, A. W. Cerebral white matter integrity and cognitive aging: contributions from diffusion tensor imaging. Neuropsychol. Rev. 19, 415–435 (2009).
Jones, D. K. & Leemans, A. Diffusion tensor imaging. Methods Mol. Biol. 711, 127–144 (2011).
Klunk, W. E. et al. Imaging brain amyloid in Alzheimer’s disease with Pittsburgh compound-B. Ann. Neurol. 55, 306–319 (2004).
Braak, H. & Del Tredici, K. The preclinical phase of the pathological process underlying sporadic Alzheimer’s disease. Brain 138, 2814–2833 (2015).
Villain, N. et al. Sequential relationships between grey matter and white matter atrophy and brain metabolic abnormalities in early Alzheimer’s disease. Brain 133, 3301–3314 (2010).
Jicha, G. A. et al. Neuropathologic outcome of mild cognitive impairment following progression to clinical dementia. Arch. Neurol. 63, 674–681 (2006).
Heilbronner, S. R. & Haber, S. N. Frontal cortical and subcortical projections provide a basis for segmenting the cingulum bundle: implications for neuroimaging and psychiatric disorders. J. Neurosci. 34, 10041–10054 (2014).
Sepulcre, J. et al. In vivo tau, amyloid, and gray matter profiles in the aging brain. J. Neurosci. 36, 7364–7374 (2016).
Von Der Heide, R. J., Skipper, L. M., Klobusicky, E. & Olson, I. R. Dissecting the uncinate fasciculus: disorders, controversies and a hypothesis. Brain 136, 1692–1707 (2013).
Price, J. L. & Morris, J. C. Tangles and plaques in nondemented aging and “preclinical” Alzheimer’s disease. Ann. Neurol. 45, 358–368 (1999).
Delacourte, A. et al. Tau aggregation in the hippocampal formation: an ageing or a pathological process? Exp. Gerontol. 37, 1291–1296 (2002).
Dagley, A. et al Harvard Aging Brain Study: dataset and accessibility. Neuroimage 144, 255–258 (2017).Pt B.
Fischl, B., Sereno, M. I. & Dale, A. M. Cortical surface-based analysis. II: Inflation, flattening, and a surface-based coordinate system. Neuroimage 9, 195–207 (1999).
Logan, J. et al. Graphical analysis of reversible radioligand binding from time-activity measurements applied to [N-11C-methyl]-(-)-cocaine PET studies in human subjects. J. Cereb. Blood Flow Metab. 10, 740–747 (1990).
Mormino, E. C. et al. Synergistic effect of β-amyloid and neurodegeneration on cognitive decline in clinically normal individuals. JAMA Neurol. 71, 1379–1385 (2014).
Braak, H. & Braak, E. Frequency of stages of Alzheimer-related lesions in different age categories. Neurobiol. Aging 18, 351–357 (1997).
Hyman, B. T. Amyloid-dependent and amyloid-independent stages of Alzheimer disease. Arch. Neurol. 68, 1062–1064 (2011).
Hardy, J. & Selkoe, D. J. The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 297, 353–356 (2002).
Götz, J., Chen, F., van Dorpe, J. & Nitsch, R. M. Formation of neurofibrillary tangles in P301l tau transgenic mice induced by Abeta 42 fibrils. Science 293, 1491–1495 (2001).
Lewis, J. et al. Enhanced neurofibrillary degeneration in transgenic mice expressing mutant tau and APP. Science 293, 1487–1491 (2001).
Wheeler-Kingshott, C. A. & Cercignani, M. About “axial” and “radial” diffusivities. Magn. Reson. Med. 61, 1255–1260 (2009).
Clavaguera, F. et al. Transmission and spreading of tauopathy in transgenic mouse brain. Nat. Cell Biol. 11, 909–913 (2009).
Takeda, S. et al. Neuronal uptake and propagation of a rare phosphorylated high-molecular-weight tau derived from Alzheimer’s disease brain. Nat. Commun. 6, 8490 (2015).
Harris, J. A. et al. Transsynaptic progression of amyloid-β-induced neuronal dysfunction within the entorhinal-hippocampal network. Neuron 68, 428–441 (2010).
Buckner, R. L. et al. Cortical hubs revealed by intrinsic functional connectivity: mapping, assessment of stability, and relation to Alzheimer’s disease. J. Neurosci. 29, 1860–1873 (2009).
Dillen, K. N. H. et al. Aberrant functional connectivity differentiates retrosplenial cortex from posterior cingulate cortex in prodromal Alzheimer’s disease. Neurobiol. Aging 44, 114–126 (2016).
Vann, S. D., Aggleton, J. P. & Maguire, E. A. What does the retrosplenial cortex do? Nat. Rev. Neurosci. 10, 792–802 (2009).
Rieckmann, A. et al. Accelerated decline in white matter integrity in clinically normal individuals at risk for Alzheimer’s disease. Neurobiol. Aging 42, 177–188 (2016).
Stancu, I. C., Vasconcelos, B., Terwel, D. & Dewachter, I. Models of β-amyloid induced Tau-pathology: the long and “folded” road to understand the mechanism. Mol. Neurodegener. 9, 51 (2014).
Iqbal, K., Liu, F. & Gong, C. X. Tau and neurodegenerative disease: the story so far. Nat. Rev. Neurol. 12, 15–27 (2016).
Hurtado, D. E. et al. Abeta accelerates the spatiotemporal progression of tau pathology and augments tau amyloidosis in an Alzheimer mouse model. Am. J. Pathol. 177, 1977–1988 (2010).
Kuchibhotla, K. V. et al. Neurofibrillary tangle-bearing neurons are functionally integrated in cortical circuits in vivo. Proc. Natl. Acad. Sci. USA 111, 510–514 (2014).
Gordon, B. A. et al. The relationship between cerebrospinal fluid markers of Alzheimer pathology and positron emission tomography tau imaging. Brain 139, 2249–2260 (2016).
Frings, L. et al. Asymmetries of amyloid-β burden and neuronal dysfunction are positively correlated in Alzheimer’s disease. Brain 138, 3089–3099 (2015).
Stefanits, H., Budka, H. & Kovacs, G. G. Asymmetry of neurodegenerative disease-related pathologies: a cautionary note. Acta Neuropathol. 123, 449–452 (2012).
Hanseeuw, B. J. et al. Fluorodeoxyglucose metabolism associated with tau-amyloid interaction predicts memory decline. Ann. Neurol. 81, 583–596 (2017).
Morris, J. C. The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 43, 2412–2414 (1993).
Folstein, M. F., Folstein, S. E. & McHugh, P. R. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J. Psychiatr. Res. 12, 189–198 (1975).
Sheikh, J. & Yesavage, J. Geriatric Depression Scale (GDS): recent evidence and development of a shorter version. in Clinical Gerontology: A Guide to Assessment and Intervention (ed. Brink, T.L.) 165–173 (Haworth Press, New York, 1986).
Leemans, A., Jeurissen, B., Sijbers, J. & Jones, D.K. Explore DTI: a graphical toolbox for processing, analyzing, and visualizing diffusion MR data. in 17th Annual Meeting of Intl. Soc. Mag. Reson. Med. 3537 (Hawaii, USA, 2009).
Mori, S. et al. Stereotaxic white matter atlas based on diffusion tensor imaging in an ICBM template. Neuroimage 40, 570–582 (2008).
Klein, A. et al. Evaluation of 14 nonlinear deformation algorithms applied to human brain MRI registration. Neuroimage 46, 786–802 (2009).
Vos, S. B., Jones, D. K., Viergever, M. A. & Leemans, A. Partial volume effect as a hidden covariate in DTI analyses. Neuroimage 55, 1566–1576 (2011).
Nakagawa, S. & Schielzeth, H. Repeatability for Gaussian and non-Gaussian data: a practical guide for biologists. Biol. Rev. Camb. Philos. Soc. 85, 935–956 (2010).
Dale, A. M., Fischl, B. & Sereno, M. I. Cortical surface-based analysis. I. Segmentation and surface reconstruction. Neuroimage 9, 179–194 (1999).
Hedden, T. et al. Disruption of functional connectivity in clinically normal older adults harboring amyloid burden. J. Neurosci. 29, 12686–12694 (2009).
Amariglio, R. E. et al. Subjective cognitive complaints and amyloid burden in cognitively normal older individuals. Neuropsychologia 50, 2880–2886 (2012).
Shoup, T. M. et al. A concise radiosynthesis of the tau radiopharmaceutical, [(18) F]T807. J. Labelled Comp. Radiopharm. 56, 736–740 (2013).
Greve, D. N. et al. Cortical surface-based analysis reduces bias and variance in kinetic modeling of brain PET data. Neuroimage 92, 225–236 (2014).
Masur, D. M. et al. Distinguishing normal and demented elderly with the selective reminding test. J. Clin. Exp. Neuropsychol. 11, 615–630 (1989).
Wechsler, D. S. Wechsler Memory Scale-Revised. (Psychological-Corp, San Antonio, TX, USA, 1987).
Wechsler, D. S. WAIS-III, Wechsler Adult Intelligence Scale—Third Edition, Administration and Scoring Manual (The Psychological Corporation, New York, 1997).
Reitan, R. M. Manual for Administration of Neuropsychological Test Batteries for Adults and Children (Reitan Neuropsychology Laboratories, Tucson, AZ, USA, 1979).
Benton, A. L. Contributions to Neuropsychological Assessment: a Clinical Manual. (Oxford University Press, New York, 1983).
Domen, P. et al. Differential time course of microstructural white matter in patients with psychotic disorder and individuals at risk: a 3-year follow-up study. Schizophr. Bull. 43, 160–170 (2017).
Mormino, E. C. et al. Amyloid and APOE β4 interact to influence short-term decline in preclinical Alzheimer disease. Neurology 82, 1760–1767 (2014).
Wang, L. et al. Evaluation of tau imaging in staging Alzheimer disease and revealing interactions between β-amyloid and tauopathy. JAMA Neurol. 73, 1070–1077 (2016).
Acknowledgements
This work was supported in part by the Athinoula A. Martinos Center for Biomedical Imaging, P41 EEB015896 and shared instrumentation grants S10RR021110, S10OD010364, S10RR023401, S10RR023043 and 1S10RR019307. The research was supported in major part by the Harvard Aging Brain Study (P01 AG036694). We thank all the participants of the Harvard Aging Brain Study. H.I.L.J. received funding from Alzheimer Nederland (WE.15-2014-06). T.H. received funding from NIH grant K01 AG040197, P01 AG036694, P50 AG005134, R01 AG053509 and R01 AG034556. J.S. received funding from NIH grant K23EB019023. K.P. is funded by NIA grant K23 AG053422-01 and the Alzheimer’s Association. K.J. received funding from NIH grants R01 EB014894, R21 AG038994, R01 AG026484, R01 AG034556, P50 AG00513421, U19 AG10483, P01 AG036694, R13 AG042201174210, R01 AG027435 and R01 AG037497 and the Alzheimer’s Association grant ZEN-10-174210. R.S. receives research support from the following grants: P01 AG036694, U01 AG032438, U01 AG024904, R01 AG037497, R01 AG034556, K24 AG0350007, P50 AG005134, U19 AG010483, R01 AG027435, Fidelity Biosciences, Harvard NeuroDiscovery Center and the Alzheimer’s Association.
Author information
Authors and Affiliations
Contributions
H.I.L.J. designed the study, analyzed the diffusion and behavioral data, performed statistical analyses and wrote the manuscript. T.H. performed the factor analyses and aided in data interpretation and manuscript preparation. A.P.S. analyzed the PET and structural data and aided in manuscript preparation. J.S. aided in the connectivity data analysis and manuscript preparation. R.D.P. aided in data analysis and manuscript preparation. R.E.A., K.V.P. and D.M.R. aided in study screening procedures, neuropsychological assessments and manuscript preparation. R.A.S. provided the participants and data analytic tools and aided in study design and manuscript preparation. K.A.J. designed the study, aided in data analyses and interpretation and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
A.S. has been a paid consultant for Janssen Pharmaceuticals and Biogen. K.P. has served as a paid consultant for Biogen.D. Rentz has done consulting for Eli Lilly and served on the Scientific Advisory Board for Neurotrack. K.J. has served as paid consultant for Bayer, GE Healthcare, Janssen Alzheimer’s Immunotherapy, Siemens Medical Solutions, Genzyme, Novartis, Biogen, Roche, ISIS Pharma, AZTherapy, GEHC, Lundberg and Abbvie; and he is a site co-investigator for Lilly/Avid, Janssen Immunotherapy and Pfizer. R.S. has served as a paid consultant for Abbvie, Biogen, Bracket, Genentech, Lundbeck, Roche and Sanofi; has served as co-investigator for Avid, Eli Lilly and Janssen Alzheimer Immunotherapy clinical trials; and has spoken at symposia sponsored by Eli Lilly, Biogen and Janssen. R.S. receives research support from Janssen Pharmaceuticals and Eli Lilly and Co.; these relationships are not related to the content in the manuscript.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Overview of the data acquisition.
. For each measurement, the number of observations is depicted per time point. For tau PET, the first measurement was acquired throughout the study, depending on the time the subject entered the study. Associations between amyloid burden and hippocampal volume where tested cross-sectionally using both baseline measures and longitudinal using amyloid burden at baseline and hippocampal volume over time. Associations between hippocampal volume and diffusion were tested using hippocampal volume at baseline and diffusion over time (for the reversed association, we used diffusion at baseline and hippocampal volume over time). Associations between diffusion and tau pathology were tested using diffusion at baseline and tau pathology over time. Finally, the associations with memory were investigated with memory longitudinally and diffusion at baseline and biomarker data dichotomized (using the Gaussian Mixture Modeling approach). Abbreviations: F/U = Follow-up; Hipp = Hippocampus; PET = Positron Emission Tomography.
Supplementary Figure 2 Associations between hippocampal volume and diffusivity of the HCB and UF at baseline.
. Associations between hippocampal volume and tract diffusivity of the hippocampal cingulum bundle (top row, n=256 independent participants) and uncinate fasciculus (bottom row, n=253 independent participants) for left (first two columns) and right sides (last two columns). Abbreviations: FA = Fractional Anisotropy; MD = Mean Diffusivity.
Supplementary Figure 3 Spaghetti plot of the relationship between HCB diffusivity over time and hippocampal volume at baseline for amyloid-positive and amyloid-negative individuals.
. Plots show longitudinal subject-specific values for the association between MD values of the HCB over time and hippocampal volumes (adjusted for intracranial volume). Cooler colors represent lower hippocampal volumes (right hemisphere: top panel, left hemisphere: bottom panel). Amyloid positive individuals (n=61 independent participants) are shown in dashed lines, while amyloid negative individuals (n=183 independent participants) in solid lines. Values are unadjusted, raw values. Abbreviations: MD: mean diffusivity, HCB: Hippocampal cingulum bundle.
Supplementary Figure 4 Associations between change in hippocampal volume and change in mean diffusivity in the HCB and UF.
. The line plots (top row = left, bottom row = right hemisphere) show that change in right hippocampal volume over time predicted increased MD of the right HCB over time (left bottom corner; n=256 independent participants). No significant associations were found between change in hippocampal volume and changes in MD of the UF (n=253 independent participants). In all line plots, estimated marginal means of the moderation by change in hippocampal volume are plotted at the mean and ± 1 standard deviation, but analyses were done continuously using mixed-effects linear models. Shaded areas around the fit lines show the 95% confidence interval. All p-values are two-sided and unadjusted for multiple comparisons.
Supplementary Figure 5 Spaghetti plot of the relationship between PCC tau binding over time and baseline HCB diffusivity for amyloid-positive and amyloid-negative individuals.
. Plots show longitudinal subject-specific values for the association between PCC tau binding over time and baseline MD of the hippocampal cingulum bundle (HCB) Cooler colors represent lower MD values (right hemisphere: top panel, left hemisphere: bottom panel). Amyloid positive individuals (n=36 independent participants) are shown in dashed lines, while amyloid negative (n=103 independent participants) individuals in solid lines. Values are unadjusted, raw values. Abbreviations: MD: mean diffusivity.
Supplementary Figure 6 Gaussian mixture modeling for the PCC and IT.
. Note: Multiple Gaussian distributions (i.e. mixtures) were fit to the PCC tau (top) or IT tau (bottom) signal of the baseline data (n=141 independent participants). The number of mixtures is plotted against the Bayesian Information Criterion (BIC, higher is better). Left panels show the distribution assuming unequal variances (red) or equal variances (blue). For the PCC: BIC=131.23, LRTS for 2 mixture components=16.95, p=0.025; LRTS for 3 mixture components =6.40, p=0.506 with a BIC=130.66. For the IT BIC=87.56, LRTS for 2 mixture components=11.11, p=0.044; LRTS for 3 mixture components =6.82, p=0.25 with a BIC=77.57. Right panels show the probability density function for the estimated Gaussian distribution superimposed on the baseline subject density histogram for PCC (top) or IT (bottom) tau values. The green vertical line indicates the optimal probability threshold (PCC tau = 1.28 SUVr partial volume corrected; IT tau = 1.73 SUVr partial volume corrected). Abbreviations: PCC = Posterior cingulate cortex, IT = Inferior Temporal cortex,LRTS= Likelihood ratio test statistic.
Supplementary Figure 7 Spaghetti plot of the relationship between memory performance over time and baseline HCB diffusivity for individuals with low versus high PCC tau.
Plots show longitudinal subject-specific values (n=141 independent participants) for the association between memory performance over time and baseline MD values of the hippocampal cingulum bundle (HCB). Cooler colors represent lower MD values (right HCB: top panel, left HCB: bottom panel). Individuals with high PCC tau values are shown in dashed lines, while individual with low PCC tau binding in solid lines. Values are unadjusted, raw values. Abbreviations: MD: mean diffusivity.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–7
Rights and permissions
About this article
Cite this article
Jacobs, H.I.L., Hedden, T., Schultz, A.P. et al. Structural tract alterations predict downstream tau accumulation in amyloid-positive older individuals. Nat Neurosci 21, 424–431 (2018). https://doi.org/10.1038/s41593-018-0070-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41593-018-0070-z
This article is cited by
-
Associations between cardiometabolic multimorbidity and cerebrospinal fluid biomarkers of Alzheimer’s disease pathology in cognitively intact adults: the CABLE study
Alzheimer's Research & Therapy (2024)
-
Spatiotemporal patterns of locus coeruleus integrity predict cortical tau and cognition
Nature Aging (2024)
-
Impact of APOE on amyloid and tau accumulation in argyrophilic grain disease and Alzheimer’s disease
Acta Neuropathologica Communications (2024)
-
Proteostasis failure exacerbates neuronal circuit dysfunction and sleep impairments in Alzheimer’s disease
Molecular Neurodegeneration (2023)
-
Neuroinflammation is independently associated with brain network dysfunction in Alzheimer’s disease
Molecular Psychiatry (2023)