Abstract
Dietary interventions may best be delivered at supermarkets, which offer convenience, accessibility, full food inventories and, increasingly, in-store registered dietitians, online shopping and delivery services. In collaboration with a large retail supermarket chain, we conducted a multisite supermarket and web-based intervention targeting nutrition trial (no. NCT03895580), randomizing participants (n = 247 (139 women and 108 men)) 2:2:1 to two levels of dietary education (Strategy 1 and Strategy 2) or an enhanced control group that included educational components beyond the routine standard of care. Both Strategies 1 and 2 included individualized, in-person, dietitian-led, purchasing data-guided interventions. Strategy 2 also included online tools for shopping, home delivery, selection of healthier purchases, meal planning and healthy recipes. The primary endpoint was change in dietary approaches to stop hypertension (DASH) score (a measure of adherence to the DASH diet) from baseline to 3 months. The primary endpoint was met because, at 3 months, the DASH score increased by 4.7 more for the combined Strategy 1 and Strategy 2 groups than for the control group (95% confidence interval (CI) (0.9, 8.5), P = 0.02). In a prespecified hierarchical test, at 3 months, DASH score increased by 3.8 more for the Strategy 2 group than for the Strategy 1 group (95% CI (0.8, 6.9), P = 0.01). This trial demonstrates the efficacy of data-guided, supermarket-based, dietary interventions and modern online shopping tools in improving dietary quality in a free-living, community-based population. The trial also demonstrates the opportunity for academic investigators to collaborate with retailers to design and rigorously test comprehensive healthcare interventions.
Similar content being viewed by others

Main
Supermarkets with expansive footprints and evolving healthcare operations may offer new opportunities to expand clinical care services beyond traditional medical settings. Intrinsically, grocery stores may be partners well suited to addressing unmet public health challenges, including unhealthy diets1. Over the past 10 years, nutrition counseling provided by registered dietitians has been introduced in supermarket-based retail clinics2,3. New retail technologies may further address barriers to healthy eating, including websites and mobile applications for online food shopping, home grocery delivery and nutrition support. Automatically, electronically collected purchasing data, refined to create visibility into unhealthy dietary behaviors and intake, may also provide value when used by consumers and healthcare providers.
The supermarket and web-based intervention targeting nutrition (SuperWIN) was designed to test two in-person, dietitian-led education interventions focused on the DASH dietary pattern4,5. Each intervention was guided and individualized by data on each participant’s food purchases. The first intervention focused on the in-store shopping environment, while the second added online shopping, home delivery and other technologies that might improve the quality of grocery purchases and dietary intake. To date, research collaborations between academia and supermarkets and grocery stores have been very limited in regard to rigorous testing of new strategies aimed at improving dietary quality.
Results
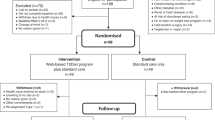
From March 2019 to the end of February 2021, 267 participants in total were randomized (Fig. 1). Due to the COVID-19 pandemic, the study was temporarily interrupted due to safety concerns about continued in-person intervention delivery. Study leadership withdrew 20 recently randomized participants who had not yet reached 3 months of follow-up (that is, the time point at which data required for the primary endpoint were collected). We prespecified that these participants would be excluded from all subsequent analyses. The overall cohort, including for assessment of the primary endpoint, consisted of 247 participants. For subsequent prespecified COVID-19 analyses, the prepandemic subgroup consisted of 109 participants.
In the overall cohort, 91% of participants provided 3-month dietary intake data. In Strategies 1 and 2, 96% of participants attended one or more intervention visits, with 80% attending all six scheduled intervention visits. To understand the disruption due to the pandemic, study conduct is also reported separately for the prepandemic and pandemic cohorts (Supplementary Tables 8 and 9). In the prepandemic cohort (n = 109), intervention visit completion was 97.8% (264 of 270 total visits) in Strategy 1 and 98.4% (248 of 252 total visits) in Strategy 2. In the pandemic cohort (n = 138), intervention visit completion dropped to 84.5% (279 of 330 total visits) in Strategy 1 and to 81.1% (287 of 354) in Strategy 2. Prepandemic, dietary data and biometrics collection at 3 months was 100.0% (109 of 109) and 100.0% (109 of 109), respectively. In the pandemic cohort, dietary data and biometrics collection at 3 months dropped to 84.1% (116 of 138) and 79.0% (109 of 138), respectively.
Participant characteristics
At baseline in the overall cohort, median age was 58 years, 69% of which were female and 21% self-identified as black or African American. In addition, 64.8% were married or living with a partner, 53.4% were employed full-time and 63.6% had at least a bachelor’s degree. Mean systolic blood pressure (SBP) was 129.3 (standard deviation (s.d.), 16.7) and hypertensive medication use was 72.9%. Obesity was present in 63.6%. Median non-high-density lipoprotein cholesterol (non-HDL-C) was 111 (min, 36; max, 216) and hypercholesterolemia medication use was 41.7%. Baseline characteristics were balanced across the groups (Table 1).
Primary endpoint, DASH score
The baseline mean DASH score was 45.4 (10.4), indicating that participants had on average approximately 50% adherence to the DASH dietary pattern goals. From baseline to 3 months, there were mean increases in DASH score of 5.8 (95% CI (2.5, 9.2), P = 0.0006), 8.6 (95% CI (6.4, 10.8), P < 0.0001) and 12.4 (95% CI (10.3, 14.6), P < 0.0001) for control, Strategy 1 and Strategy 2 groups, respectively (Table 2). From baseline to 3 months, the combined Strategies 1 and 2 showed a DASH score increased by 10.5 (95% CI (9.0, 12.1), P < 0.0001). The combined Strategies 1 and 2 resulted in a significant increase in DASH score by 4.7 (95% CI (0.9, 8.5), P = 0.02) compared with control (enhanced medical nutrition therapy) (Table 3). At 6 months (3 months post intervention), there were persistent increases in DASH score of 4.4 (95% CI (0.6, 8.1), P = 0.02), 6.6 (95% CI (4.0, 9.2), P < 0.0001) and 8.4 (95% CI (5.9, 11.0), P < 0.0001) for control, Strategy 1,and Strategy 2 groups, respectively (Table 2). At 6 months, the combined Strategies 1 and 2 had a persistently increased DASH score of 7.5 (95% CI (5.7, 9.3), P < 0.0001). However, the combined Strategies 1 and 2 no longer demonstrated a difference in DASH score (3.1, 95% CI (−1.0, 7.3), P = 0.14) compared with the enhanced control group (Table 3).
Individualized nutrition education, enhanced with online shopping technologies and training (Strategy 2), significantly increased DASH score by 3.8 (95% CI (0.8, 6.9), P = 0.01) compared with education without online enhancement (Strategy 1), from baseline to 3 months (Table 3). This increase was at least partially due to an increase in daily mean servings of fruits in Strategy 2 versus 1 (P < 0.05) (Table 4). From baseline to 6 months, Strategy 2 resulted in no difference in DASH score (1.8, 95% CI (− 1.9, 5.5), P = 0.34) compared with Strategy 1 (Table 3).
Prespecified secondary endpoints
From baseline to 3 months, SBP, diastolic blood pressure (DBP) and body mass index (BMI) did not decrease in the control group (Supplementary Table 14). From baseline to 3 months, SBP decreased in Strategy 1 and Strategy 2 groups by −6.6 (−9.8, −3.4) and −5.7 (−8.7, −2.8) mmHg, respectively. DBP decreased in Strategy 1 and Strategy 2 groups by −2.4 (−4.2, −0.6) and −2.0 (−3.9, −0.1) mmHg, respectively. BMI decreased in Strategy 1 and Strategy 2 groups by −0.4 (−0.7, −0.2) and −0.8 (−1.0, −0.5) kg m–2, respectively. In between-group comparisons, however, no differences were found.
From baseline to 6 months, SBP decreased in control, Strategy 1 and Strategy 2 groups by −5.4 (−10.7, −0.1), −5.2 (−8.8, −1.6) and −4.2 (−7.8, −0.5) mmHg, respectively (Supplementary Table 15). DBP decreased in control and Strategy 1 groups by −3.7 (−7.1, −0.3) and −4.4 (−6.7, −2.2) mmHg, respectively, but did not decrease in the Strategy 2 group. BMI decreased in Strategy 1 and Strategy 2 groups by −0.6 (−0.9, −0.3) and −0.7 (−1.1, −0.4) kg m–2, respectively. In between-group comparisons, however, no differences were found.
From baseline to either 3 months (Supplementary Table 16) or 6 months (Supplementary Table 17), non-HDL-C, total cholesterol and triglycerides (TG) were not reduced by the combined Strategies 1 and 2 versus the enhanced control.
COVID impact analyses
In the prepandemic cohort, from baseline to 3 months, the combined Strategies 1 and 2 increased the DASH score by 8.3 (95% CI (3.4, 13.3), P = 0.001) compared with the enhanced control (Supplementary Table 18). From baseline to 6 months, the combined Strategies 1 and 2 did not result in a significant difference in DASH score: 5.1 (95% CI (−0.8, 11.1), P = 0.09) compared with control (Supplementary Table 19).
Strategy 2 resulted in no significant difference in DASH score, at 3.1 (95% CI (−1.3, 7.6), P = 0.017), from baseline to 3 months compared with Strategy 1 (Supplementary Table 18). From baseline to 6 months, the increase in DASH score was nonsignificant at 1.2 (95% CI (−4.2, 6.6), P = 0.67) when comparing Strategy 2 with Strategy 1 (Supplementary Table 19).
From baseline to 3 months, there were no reductions in SBP, DBP, BMI, non-HDL-C, total cholesterol or TG comparing the combined Strategies 1 and 2 versus the enhanced control (Supplementary Table 18).
Subgroup analysis
A prespecified exploratory subgroup analysis evaluating absolute mean DASH score difference for selected subgroups within Strategies 1 and 2 versus control was performed. Greater improvements in DASH diet adherence were associated with older age (51–75 versus 21–50 years), white race (white versus nonwhite) and baseline hypertension (with versus without) (Supplementary Table 20; interaction terms, P ≤ 0.01). There was no difference by gender (men versus women).
Discussion
In SuperWIN, all three study groups demonstrated increases in adherence to the DASH dietary pattern from baseline to 3 months, along with persistence of increased DASH adherence at 6 months. On top of a data-enhanced medical nutrition therapy session, the addition of an individualized, food-purchasing, data-guided, ‘teaching in the aisles’ nutrition intervention increased DASH adherence. Introduction to online shopping and technologies to improve purchases, meal planning and recipe quality further increased DASH adherence. Participant engagement before the pandemic was remarkably high for a community-based study. This was reflected by extremely high visit attendance and near-perfect dietary intake and biometrics collection. Even during the disruption of the pandemic6,7, visit attendance and data collection remained comparable to prepandemic community-based studies8.
Globally, suboptimal diet is accountable for more deaths than any other risk factor across age, sex and socioeconomic status9. While the scores used to measure DASH adherence have varied across studies, the association between DASH scores and clinical outcomes has been consistently demonstrated10. As an example, a recent meta-analysis found a linear dose–response for each five-point increase in DASH score and associations with lower all-cause, cardiovascular (CV), stroke and cancer mortality of 5, 4, 3 and 3%, respectively11. In both the PREDIMED trial and Western and non-Western observational studies, it has been shown that even small measures of increased diet quality result in large CV risk reductions over time12,13,14,15,16,17. While the validation studies of DASH were performed in a highly controlled environment (that is, feeding studies), the PREMIER trial, which enrolled free-living participants, demonstrated the impact on DASH adherence through an intensive 18-visit, 6-month program conducted at academic centers18,19. The 2021 update to the 2006 American Heart Association (AHA) guidelines continues to recommend evidence-based, heart-healthy dietary patterns, including DASH20.
Despite longstanding recommendations, adoption of DASH across the United States21 and many other countries1 remains low. From 2007 to 2012, using a different DASH adherence score and the National Health and Nutrition Examination Survey, it was estimated that, in the United States, individuals with hypertension scored only about 2.6–2.7 from a total score of 9 (ref. 22). A 2019 AHA Science Advisory concluded that ‘immediate action is needed’ to innovate new approaches to close this gap23. Specific recommendations included creation of new partnerships (including with retailers) for sponsored research. The need for research on the health benefits of online shopping and smart technologies (for example, nutrition and health applications) was also highlighted. We incorporated several such approaches through a supermarket-based partnership. SuperWIN may now be able to extend the findings of previous dietary trials through an innovative, dietitian-driven, grocery store-based model, with technologies that facilitate broad convenience and accessibility.
In SuperWIN, the interventions increased DASH score by a clinically meaningful 4.7 points from baseline to 3 months compared with the control group. The control group experienced a 5.8-point increase in DASH score, which is larger than the change in DASH (or DASH food group) adherence for standard-of-care interventions reported in other recent clinical trials24,25. It is likely that the standard of care delivered in SuperWIN had a more favorable impact on DASH adherence due to the use of the participants’ preferred stores, dietitians’ expertise and provision of DASH-focused dietary intake data. At 6 months, while DASH scores decreased slightly, they remained significantly increased from baseline by 4.4 (0.6, 8.1), 6.6 (4.0, 9.2) and 8.4 (5.9, 11.0) in the control, Strategy 1 and Strategy 2 groups, respectively. Additional research may identify opportunities to increase not only the initial post-intervention dietary improvements, but also to maximize their persistence over long-term follow-up. Opportunities include: (1) addition of more in-person visits, (2) use of telenutrition visits and (3) continued delivery of updated purchasing behavior data to the participant and/or dietitian.
The rapid yearly increase in online shopping across all age groups in the United States26 may provide unique opportunities to address barriers to shopping and making better food choices. In addition, utilization of mobile health-focused applications in patients with CV risk factors is increasing27. In SuperWIN, the addition of online technologies increased DASH score by a clinically meaningful 3.8 points from baseline compared with education that did not incorporate them. Considering that SuperWIN enrolled a ‘late tech-adopters’ population, it is possible that early tech-adopters may experience even greater dietary improvements. As online shopping becomes even more common in the United States and other countries, retail platforms will offer increasingly comprehensive features and services at lower prices. Collectively, this may offer opportunities to mitigate challenges related to poor health literacy, busy schedules, inadequate personal or public transportation, distance to the nearest grocery retailer, disability and industry marketing28. In 2019, the Supplemental Nutrition Assistance Program launched its pilot program to understand whether online shopping might increase the purchase of healthy foods29,30.
In the overall cohort, secondary endpoints of blood pressure, lipids and BMI were not improved by the interventions compared with the enhanced control. However, as an example, SBP decreased by −6.6 and −5.7 mmHg at 3 months in the Strategy 1 and Strategy 2 arms, respectively, while SBP remained decreased by −5.2 and −4.2 mmHg at 6 months in the Strategy 1 and Strategy 2 arms, respectively. A similar pattern was found for BMI. More research will be needed to quantify the impact of these interventions on secondary outcomes.
Our trial has certain limitations. Our cohort was receiving routine primary care and was predominantly middle-aged, female, married or living with a partner and living in households with a reasonable total annual household income (for comparison, in 2020, median US household annual income was US$69,560 (ref. 31)). The COVID-19 pandemic dramatically not only impacted clinical trials but also shopping behavior and many other aspects of our participants’ lives (for example, work, childcare). In terms of evaluation of SBP, DBP and lipid changes, we did not collect data on medication doses at any time point. In addition, medication use was assessed by a survey rather than by a rigorous evaluation by the study dietitian. We also did not collect medication use at 3 months. We performed a limited number of BP measurements at each time point, which may have curtailed precision. Collectively these limitations, as well as the baseline levels in this cohort, may have reduced our ability to more rigorously assess changes in these secondary endpoints. In future, additional components (for example, exercise interventions, detailed medication assessments, medication titration or medication adherence counseling through the retail pharmacy) may be combined with ‘SuperWIN-like’ dietary interventions to target these outcomes.
In conclusion, all three study groups had higher DASH adherence at 3 months, which persisted until the final study assessments at 6 months. Individualized, in-person, dietitian-led nutrition education focusing on the DASH dietary pattern, guided by electronic food-purchasing data and delivered within each participant’s home supermarket, increased DASH adherence. The addition of technologies for online shopping with both grocery pick-up and home delivery options, as well as food comparisons and meal preparation, increased DASH adherence. More research will be needed to better understand the effects of these interventions on downstream secondary outcomes. These findings demonstrate the importance of sponsored research with the retail industry, the opportunities to enhance dietary quality through grocery stores and retail clinics, as well as the efficacy of specific types of new interventions.
Methods
SuperWIN was a randomized, parallel-assignment, active-control, efficacy trial. For the protocol and statistical analysis plan, refer to Supplementary Notes 1 and 2. The study was registered on Clinicaltrials.gov (NCT03895580). The University of Cincinnati (UC) Institutional Review Board approved the protocol, and all participants gave written informed consent. All participant visits were conducted across 13 Kroger supermarket locations in Ohio and Kentucky, each of which had a clinic that allowed for study visits and assessments. The authors vouch for the accuracy of the data, as well as for the fidelity of this report to the trial protocol. A detailed description of the methods of this trial has been published10.
Participants
All participants were required to have a primary care clinician at UC Health. Lists of UC Health patients likely to meet the eligibility criteria (for example, diagnosis code of hypertension) were generated from UC Health’s Clarity Database (Epic Systems Corp.). The UC study coordinator then mailed study materials to those patients living near the study stores. Phone calls, texting, emails and flyers were also used. Interested patients were phone-screened by the coordinator and, if eligible, were entered into the run-in period. Men and women aged between 21 and 75 years were eligible if they were the primary food planner for their household, were an existing shopper at one of the study Kroger supermarkets, were able to shop and prepare food independently and had a home computer (Supplementary Table 4). Participants were enrolled if they had at least one CV risk factor: (1) SBP >130 mmHg, DBP >80 mmHg and/or treatment with an antihypertensive medication; (2) obesity, defined as BMI ≥30kg m–2; and/or (3) non-HDL-C ≥130 mg dl–1 and/or treatment with a lipid-lowering medication. Key exclusion criteria included current treatment with another dietary or weight loss intervention, use of Kroger’s online shopping platform within 12 months, previous use of Kroger’s dietary counseling services, baseline SBP ≥190 mmHg, DBP ≥110 mmHg or non-HDL-C ≥190 mg dl–1. All participants provided verbal consent to enter the run-in period and written informed consent at the beginning of the first study visit. Participants were eligible to receive up to two incentives of US$25 throughout the trial.
Randomization and blinding
Following a run-in period consisting of collection of baseline dietary intake via phone, and survey information via email, participants attended a study visit at their assigned store location. All study visits were conducted in the store by a supermarket registered dietitian (‘study dietitian’) (Supplementary Table 5). At the end of visit, once eligibility and interest were confirmed, participants were randomized in a 2:2:1 ratio to: (1) individualized, in-store nutrition education (Strategy 1); (2) individualized, in-store nutrition education enhanced with online technologies and training (Strategy 2); or (3) no further education (control). Randomization was accomplished by the study dietitian using the preloaded, stratified randomization list in the Research Electronic Data Capture (REDCap) randomization module, which programmatically displayed the assignment. Randomization was stratified by characteristics reported to influence food choice: age (two levels), gender (two levels) and household size (three levels). The block size used was five.
The principal investigators and other key study staff at UC and Cincinnati Children’s Hospital and Medical Center (CCHMC) were not blinded; each could access REDCap and determine participant group assignment. Raw dietary intake data were not stored in REDCap. All calculations of DASH score during follow-up and changes in DASH score were performed only after completion of the study.
Procedures
All participants received a 30-min medical nutrition therapy session (standard of care) at the first study visit, before randomization. The dietitian educated participants on the evidence-based DASH diet in relation to CV risk factor reduction, set personal DASH dietary goals based on current intake and developed an action plan to meet those goals. Compared with typical practice, this session was enhanced by displaying each participant’s baseline dietary intake data (collected during the run-in period) via simple figures and tables. These highlighted the participant’s mean servings of each DASH food group, the mean serving goals per food group, the specific foods consumed, as well as the time and location of consumption. DASH food serving goals were established based on a caloric goal for either weight maintenance or loss.
Participants randomized to Strategies 1 and 2 were scheduled for six additional in-store educational sessions performed at 2-week intervals over the next 3 months. Educational visits in Strategies 1 and 2 utilized the physical supermarket environment (‘teaching within the aisles’). Strategy 2 participants were also trained by the study dietitians in a stepwise manner on the store’s online shopping platform, free home delivery services and two other healthcare applications (Supplementary Table 6). Nutrition education themes, learning outcomes and skill-building exercises were consistent across Strategies 1 and 2. Education in Strategies 1 and 2 was guided by dietitian and participant review of each participant’s updated, individualized, Kroger purchasing data (automatically collected via a store loyalty card) at the beginning of each session. These data, displayed via simple figures and tables, highlighted the purchases of food groups and specific food items, as well as counts of purchases and money spent since randomization.
All randomized participants were scheduled for in-store study assessments (interviews and biometric measurements) at baseline and at 3 and 6 months from randomization. Raw dietary intake data were collected by phone at baseline and at 3 and 6 months. Medication intake was collected via an emailed survey at baseline and at 6 months.
Endpoints
The primary endpoint was change in DASH score, which was calculated on a 0–90-point scale24 with a higher score indicating greater adherence to a DASH diet (Supplementary Table 7). In this trial, DASH score was calculated from 11 component scores based on the alignment between actual intake and the DASH serving recommendations (for example, whole grains, vegetables, fruits).
At baseline and at 3 and 6 months, three 24-dietary phone recalls (two weekday and one weekend) were collected at each time point by trained dietary interviewers from the Bionutrition Center at CCHMC. Only after completion of the study were these raw dietary intake data used to calculate DASH scores. DASH scores were first calculated for individual recalls followed by calculation of a participant’s mean DASH score at each time point. Use of dietary intake recalls, collection on multiple days and a comprehensive scoring system to reflect the multiple components of DASH were used to optimize measurement of DASH dietary pattern adherence.
Prespecified secondary endpoints included SBP, DBP, BMI, non-HDL-C, total cholesterol and TG measured during study visits by the study dietitians at baseline and at 3 and 6 months. COVID-19 impact analyses were prespecified before database lock. The prepandemic subgroup was defined as those participants who were randomized and had completed 3 months of follow-up before study cessation, when the United States declared a national emergency on 13 March 2020.
Statistical analyses
We evaluated change in DASH score within each group from baseline to 3 months and from baseline to 6 months. We formally tested two hypotheses in hierarchical fashion: (1) whether, from baseline to 3 months, Strategies 1 and 2 combined increased DASH score compared with an enhanced control; and (2) whether, from baseline to 3 months, Strategy 2 increased DASH score compared with Strategy 1 (see above). The second hypothesis was tested only if P < 0.05 was met for the first hypothesis, which preserved an experiment-wise error rate of 0.05. We used an intention-to-treat analysis to test both hypotheses. We used regression-based, multiple imputation techniques for missing follow-up outcome data. The primary comparisons used a mixed model for repeated measures, controlling for stratification and other previously selected baseline covariates (see legends in tables for the specific covariates used for each comparison), with DASH score as the dependent variable and treatment group, time and group × time interaction as independent variables. Residual plots were used to confirm that model assumptions had been met. We estimated that 100 participants in each intervention group (total, 200) and 50 participants for the control group would be required to provide 93 and 97% power to detect a five-point difference in change from baseline to 3 months in the DASH score for the first and second hypothesis tests, respectively. Power estimates were performed at two-sided alpha = 0.05 and assumed equal s.d. = 9 for the primary endpoint32. Although not powered to test subgroup treatment interactions, a separate analysis of variance model was used for each subgroup to compare Strategies 1 and 2 combined with control on DASH score at 3 months. Subgroups were selected using baseline characteristics (for example, male versus female) that might be associated with the efficacy of the interventions. Beyond the two formal hypotheses tested in this study, no corrections for multiple comparisons were performed. All analyses were performed using SAS 9.4 TS1M5.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The datasets generated during and/or analyzed during the current study are not publicly available, but may be made available upon reasonable request to the corresponding author.
References
Tsao C. W. et al. Heart disease and stroke statistics—2022 update: a report from the American Heart Association. Circulation https://doi.org/10.1161/CIR.0000000000001052 (2022).
Lewis, K. H., Roblin, D. W., Leo, M. & Block, J. P. The personal shopper – a pilot randomized trial of grocery store-based dietary advice. Clin. Obes. 5, 154–161 (2015).
Johnston, Y. A. et al. Working with grocers to reduce dietary sodium: lessions learned from the Broome County Sodium Reduction in Communities Pilot Project. J. Public Health Manage. Pract. 20, S54–S58 (2014).
Appel, L. J. et al. A clinical trial of the effects of dietary patterns on blood pressure. N. Engl. J. Med. 336, 1117–1124 (1997).
Sacks, F. M. et al. Effects of blood pressure of reduced dietary sodium and the dietary approaches to stop hypertension (DASH) Diet. N. Engl. J. Med. 344, 3–10 (2001).
Selvaraj, S. et al. The landscape of cardiovascular clinical trials in the United States initiated before and during COVID-19. J. Am. Heart Assoc. 9, e018274 (2020).
Wang, X. & Bhatt, D. L. COVID-19: an untended force for medical revolution? J. Invasive Cardiol. 32, E81–E82 (2020).
Mutsaerts, M. A. Q. et al. Randomized trial of a lifestyle program in obese infertile women. N. Engl. J. Med. 374, 1942–1953 (2016).
GBD 2017 Diet Collaborators. Health effects of dietary risks in 195 countries, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 393, 1958–1972 (2019).
Couch, S. C. et al. Design and rationale for the supermarket and web-based intervention targeting nutrition (SuperWIN) for cardiovascular risk reduction trial. Am. Heart J. 248, 21–34 (2022).
Soltani, S., Arablou, T., Jayedi, A. & Salehi-Abargouei, A. Adherence to the dietary approaches to stop hypertension (DASH) diet in relation to all-cause and cause-specific mortality: a systematic review and dose-response meta-analysis of prospective cohort studies. Nutr. J. 19, 37 (2020).
Estruch, R. et al. Primary prevention of cardiovascular disease with a Mediterranean diet supplemented with extra-virgin olive oil or nuts. N. Engl. J. Med. 378, e34 (2018).
Sotos-Prieto, M. et al. Association of changes in diet quality with total and cause-specific mortality. N. Engl. J. Med. 377, 143–153 (2017).
Du, H. et al. Fresh fruit consumption and major cardiovascular disease in China. N. Engl. J. Med. 374, 1332–1343 (2016).
Mozaffarian, D. et al. Global sodium consumption and death from cardiovascular causes. N. Engl. J. Med. 371, 624–634 (2014).
Bao, Y. et al. Association of nut consumption with total and cause-specific mortality. N. Engl. J. Med. 369, 2001–2011 (2013).
Mozaffarian, D., Hao, T., Rimm, E. B., Willett, W. C. & Hu, F. B. Changes in diet and lifestyle and long-term weight gain in women and men. N. Engl. J. Med. 364, 2392–2404 (2011).
Appel, L. J. et al. Effects of comprehensive lifestyle modification on blood pressure control: main results of the PREMIER clinical trial. JAMA 289, 2083–2093 (2003).
Maruthur, N. M., Wang, N. Y. & Appel, L. J. Lifestyle interventions reduce coronary heart disease risk: results from the PREMIER trial. Circulation 119, 2026–2031 (2009).
Lichtenstein, A. H. et al. Dietary guidance to improve cardiovascular health: a scientific statement from the American Heart Association. Circulation 144, e472–e487 (2021).
Steinberg, D., Bennett, G. G. & Svetkey, L. The DASH diet, 20 years later. JAMA 317, 1529–1530 (2017).
Kim, H. & Andrade, F. C. D. Diagnostic status of hypertension of the adherence to the Dietary Approaches to Stop Hypertension (DASH) diet. Prev. Med. Rep. 4, 525–531 (2016).
Anderson, C. A. M. et al. Innovation to create a healthy and sustainable food system: a science advisory from the American Heart Association. Circulation 139, e1025–e1032 (2019).
Couch, S. C. et al. Dietary Approaches to Stop Hypertension (DASH) dietary intervention improves blood pressure and vascular health in youth with elevated blood pressure. Hypertension 77, 241–251 (2021).
Blumenthal, J. A. et al. Effects of lifestyle modification on patients with resistant hypertension: results of the triumph randomized clinical Trial. Circulation 144, 1212–1226 (2021).
Food Marketing Institute. U.S. Grocery Shopper Trends 2022 https://www.fmi.org/our-research/research-reports/u-s-grocery-shopper-trends (2022).
Kozik, M., Isakadze, N. & Martin, S. S. Mobile health in preventive cardiology: current status and future perspective. Curr. Opin. Cardiol. 36, 580–588 (2021).
Smith, L. P., Ng, S. W. & Popkin, B. M. Trends in US home food preparation and consumption: analysis of national nutrition surveys and time use studies from 1965–1966 to 2007–2008. Nutr. J. 12, 45 (2013).
Bleich, S. N., Rimm, E. B. & Brownell, K. D. U. S. Nutrition assistance, 2018 – modifying SNAP to promote population health. N. Engl. J. Med. 376, 1205–1207 (2017).
USDA. Farm Bill (accessed 19 October 2022); https://www.usda.gov/farmbill
Unites States Census Bureau. Income and poverty in the United States: 2020 (accessed 19 October 2022); https://www.census.gov/library/publications/2021/demo/p60-273.html#:~:text=Median%20household%20income%20was%20%2467%2C521,and%20Table%20A%2D1
Couch, S. C. et al. The efficacy of a clinic-based behavioral nutrition intervention emphasizing a DASH-type diet for adolescents with elevated blood pressure. J. Pediatr. 152, 494–501 (2008).
Acknowledgements
We thank the leadership of The Kroger Company. We also thank the Kroger registered dietitians and analysts, whose professionalism, dedication and skill provided the opportunity to test these interventions. We thank the primary care clinicians of UC Health. Finally, we thank the participants who generously dedicated themselves to this trial. The Kroger Company was not involved in the overall design of the study, the analysis or interpretation of any data, the writing of this manuscript or the decision to submit this manuscript for publication. Personnel effort (including coprincipal investigators, D.L.S. and S.C.C.) commensurate with the study conduct and oversight was funded in part by The Kroger Company. The company also provided the time and effort of the study dietitians, the use of the store and clinic space and the electronic purchasing data for this study. This research was also supported in part by funding from CCHMC, UC (that is, Collaborative Research Advancement Grant, Rehn Family Research Award, College of Medicine Research/Pilot Grant, Strategic and Collaborative Grant, Junior Faculty Pilot Project, as well as nongrant funding) and UC Health (Innovative in Care Delivery Grant). R.N.H. received funding from K01DK128022 and UL1TR001998 during the time period of this work.
Author information
Authors and Affiliations
Contributions
D.L.S. and S.C.C. are jointly responsible for the conception and design of this study. D.L.S., R.N.H., S.S.S., M.F. and S.C.C. contributed to data acquisition. All authors contributed to the analysis and interpretation of the data. D.L.S. drafted the first version of the manuscript. All authors have reviewed, provided edits and approved the final version to be published.
Corresponding author
Ethics declarations
Competing interests
D.L.S. and S.C.C. received funding to support their effort on this study from The Kroger Company. D.L.S. also discloses the following relationships: Consultant, Sanofi; CEO, High Enroll, LLC. D.L.B. discloses the following relationships: Advisory Board, AngioWave, Bayer, Boehringer Ingelheim, Cardax, CellProthera, Cereno Scientific, Elsevier Practice Update Cardiology, High Enroll, Janssen, Level Ex, McKinsey, Medscape Cardiology, Merck, MyoKardia, NirvaMed, Novo Nordisk, PhaseBio, PLx Pharma, Regado Biosciences and Stasys; Board of Directors, AngioWave (stock options), Boston VA Research Institute, Bristol Myers Squibb (stock), DRS.LINQ (stock options), High Enroll (stock), Society of Cardiovascular Patient Care, TobeSoft; Chair, Inaugural Chair, American Heart Association Quality Oversight Committee; Consultant, Broadview Ventures; Data Monitoring Committees, Acesion Pharma, Assistance Publique-Hôpitaux de Paris, Baim Institute for Clinical Research (formerly Harvard Clinical Research Institute, for the PORTICO trial, funded by St. Jude Medical, now Abbott), Boston Scientific (Chair, PEITHO trial), Cleveland Clinic (including for the ExCEED trial, funded by Edwards), Contego Medical (Chair, PERFORMANCE 2), Duke Clinical Research Institute, Mayo Clinic, Mount Sinai School of Medicine (for the ENVISAGE trial, funded by Daiichi Sankyo; for the ABILITY-DM trial, funded by Concept Medical), Novartis, Population Health Research Institute; Rutgers University (for the NIH-funded MINT Trial); Honoraria, American College of Cardiology (Senior Associate Editor, Clinical Trials and News, ACC.org; Chair, ACC Accreditation Oversight Committee), Arnold and Porter law firm (work related to Sanofi/Bristol Myers Squibb clopidogrel litigation), Baim Institute for Clinical Research (formerly Harvard Clinical Research Institute; RE-DUAL PCI clinical trial steering committee funded by Boehringer Ingelheim; AEGIS-II executive committee funded by CSL Behring), Belvoir Publications (Editor in Chief, Harvard Heart Letter), Canadian Medical and Surgical Knowledge Translation Research Group (clinical trial steering committees), Cowen and Company, Duke Clinical Research Institute (clinical trial steering committees, including for the PRONOUNCE trial, funded by Ferring Pharmaceuticals), HMP Global (Editor in Chief, Journal of Invasive Cardiology), Journal of the American College of Cardiology (Guest Editor; Associate Editor), K2P (Co-Chair, interdisciplinary curriculum), Level Ex, Medtelligence/ReachMD (CME steering committees), MJH Life Sciences, Oakstone CME (Course Director, Comprehensive Review of Interventional Cardiology), Piper Sandler, Population Health Research Institute (for the COMPASS operations committee, publications committee, steering committee and USA national coleader, funded by Bayer), Slack Publications (Chief Medical Editor, Cardiology Today’s Intervention), Society of Cardiovascular Patient Care (Secretary/Treasurer), WebMD (CME steering committees), Wiley (steering committee); other, Clinical Cardiology (Deputy Editor), NCDR-ACTION Registry Steering Committee (Chair), VA CART Research and Publications Committee (Chair); patent, Sotagliflozin (named on a patent for sotagliflozin assigned to Brigham and Women’s Hospital who assigned to Lexicon; neither I nor Brigham and Women’s Hospital receive any income from this patent.); research funding, Abbott, Acesion Pharma, Afimmune, Aker Biomarine, Amarin, Amgen, AstraZeneca, Bayer, Beren, Boehringer Ingelheim, Boston Scientific, Bristol Myers Squibb, Cardax, CellProthera, Cereno Scientific, Chiesi, CinCor, CSL Behring, Eisai, Ethicon, Faraday Pharmaceuticals, Ferring Pharmaceuticals, Forest Laboratories, Fractyl, Garmin, HLS Therapeutics, Idorsia, Ironwood, Ischemix, Janssen, Javelin, Lexicon, Lilly, Medtronic, Merck, Moderna, MyoKardia, NirvaMed, Novartis, Novo Nordisk, Owkin, Pfizer, PhaseBio, PLx Pharma, Recardio, Regeneron, Reid Hoffman Foundation, Roche, Sanofi, Stasys, Synaptic, The Medicines Company, Youngene, 89Bio; Royalties: Elsevier (Editor, Braunwald’s Heart Disease); site coinvestigator, Abbott, Biotronik, Boston Scientific, CSI, Endotronix, St. Jude Medical (now Abbott), Philips, SpectraWAVE, Svelte, Vascular Solutions; trustee, American College of Cardiology; unfunded research, FlowCo, Takeda. S.C.C., R.N.H., B.E.S., M.H.E., S.S.S., M.F. and E.C.K. declare no competing interests.
Peer review
Peer review information
Nature Medicine thanks Larry Appel, Ellen Lee and Pao-Hwa Lin for their contribution to the peer review of this work. Primary Handling Editor: Michael Basson, in collaboration with the Nature Medicine team.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Tables 1–21, Notes 1 (protocol) and 2 (statistical analysis plan).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Steen, D.L., Helsley, R.N., Bhatt, D.L. et al. Efficacy of supermarket and web-based interventions for improving dietary quality: a randomized, controlled trial. Nat Med 28, 2530–2536 (2022). https://doi.org/10.1038/s41591-022-02077-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-022-02077-7
This article is cited by
-
Western diets and chronic diseases
Nature Medicine (2024)
-
Food as medicine: translating the evidence
Nature Medicine (2023)
-
Food as medicine: establishing a scalable foundation using data-guided and supermarket-based dietary interventions and modern online shopping tools
Journal of Thrombosis and Thrombolysis (2023)
-
Fixing America’s eating habits with effective stakeholder collaborations
Nature Medicine (2022)