Abstract
Adoptive cell therapy using tumor-infiltrating lymphocytes (TILs) has shown activity in melanoma, but has not been previously evaluated in metastatic non-small cell lung cancer. We conducted a single-arm open-label phase 1 trial (NCT03215810) of TILs administered with nivolumab in 20 patients with advanced non-small cell lung cancer following initial progression on nivolumab monotherapy. The primary end point was safety and secondary end points included objective response rate, duration of response and T cell persistence. Autologous TILs were expanded ex vivo from minced tumors cultured with interleukin-2. Patients received cyclophosphamide and fludarabine lymphodepletion, TIL infusion and interleukin-2, followed by maintenance nivolumab. The end point of safety was met according to the prespecified criteria of ≤17% rate of severe toxicity (95% confidence interval, 3–29%). Of 13 evaluable patients, 3 had confirmed responses and 11 had reduction in tumor burden, with a median best change of 35%. Two patients achieved complete responses that were ongoing 1.5 years later. In exploratory analyses, we found T cells recognizing multiple types of cancer mutations were detected after TIL treatment and were enriched in responding patients. Neoantigen-reactive T cell clonotypes increased and persisted in peripheral blood after treatment. Cell therapy with autologous TILs is generally safe and clinically active and may constitute a new treatment strategy in metastatic lung cancer.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
TRV-β sequencing of tumor and peripheral T cells as the project ‘TIL trial for NSCLC’ are available in the immuneACCESS free public database at https://clients.adaptivebiotech.com/immuneaccess. Tumor WES and RNA-seq raw data files are available on the public National Institutes of Health (NIH) dbGaP data browser (https://www.ncbi.nlm.nih.gov/projects/gapprev/gap/cgi-bin/preview1.cgi?GAP_phs_code=UgsrhvZ3dGC4uQSh; accession code phs002486.v1.p1). Raw data on expression, allelic frequency and predicted MHC affinity for all identified neoantigens are provided in the Excel spreadsheet in Supplementary Table 4. The study protocol is uploaded as a supplementary file. In the event that source data are not inferred from specified tables/figures, they are available upon request in a comma-delimited format from the study authors.
References
Man, J., Millican, J., Mulvey, A., Gebski, V. & Hui, R. Response rate and survival at key timepoints with PD-1 blockade versus chemotherapy in PD-L1 subgroups: meta-analysis of metastatic NSCLC trials. JNCI Cancer Spectrum https://doi.org/10.1093/jncics/pkab012 (2021).
Addeo, A., Banna, G. L., Metro, G. & Di Maio, M. Chemotherapy in combination with immune checkpoint inhibitors for the first-line treatment of patients with advanced non-small cell lung cancer: a systematic review and literature-based meta-analysis. Front. Oncol. 9, 264 (2019).
Hellmann, M. D. et al. Nivolumab plus ipilimumab in advanced non-small-cell lung cancer. N. Engl. J. Med. 381, 2020–2031 (2019).
Schoenfeld, A. J. & Hellmann, M. D. Acquired resistance to immune checkpoint inhibitors. Cancer Cell 37, 443–455 (2020).
Rosenberg, S. A. et al. Durable complete responses in heavily pretreated patients with metastatic melanoma using T-cell transfer immunotherapy. Clin. Cancer Res. 17, 4550–4557 (2011).
Tran, E. et al. Cancer immunotherapy based on mutation-specific CD4+ T cells in a patient with epithelial cancer. Science 344, 641–645 (2014).
Stevanović, S. et al. Complete regression of metastatic cervical cancer after treatment with human papillomavirus-targeted tumor-infiltrating T cells. J. Clin. Oncol. 33, 1543 (2015).
Tran, E. et al. T-cell transfer therapy targeting mutant KRAS in cancer. N. Engl. J. Med. 375, 2255–2262 (2016).
Zacharakis, N. et al. Immune recognition of somatic mutations leading to complete durable regression in metastatic breast cancer. Nat. Med. 24, 724–730 (2018).
Duinkerken, C. W. et al. Sensorineural hearing loss after adoptive cell immunotherapy for melanoma using MART-1 specific T cells: a case report and its pathophysiology. Otol. Neurotol. 40, e674–e678 (2019).
Blumenschein, G. et al. 278 Phase I clinical trial evaluating the safety of ADP-A2M10 SPEAR T-cells in patients with MAGE-A10+ advanced non-small cell lung cancer. J. Immunother. Cancer https://doi.org/10.1136/jitc-2020-SITC2020.0278 (2020).
Lu, Y.-C. et al. Treatment of patients with metastatic cancer using a major histocompatibility complex class II-restricted T-cell receptor targeting the cancer germline antigen MAGE-A3. J. Clin. Oncol. 35, 3322 (2017).
D’Angelo, S. P. et al. Antitumor activity associated with prolonged persistence of adoptively transferred NY-ESO-1 c259T cells in synovial sarcoma. Cancer Discov. 8, 944–957 (2018).
Xia, Y. et al. Treatment of metastatic non‑small cell lung cancer with NY‑ESO‑1 specific TCR engineered‑T cells in a phase I clinical trial: a case report. Oncol. Lett. 16, 6998–7007 (2018).
Haas, A. R. et al. Phase I study of lentiviral-transduced chimeric antigen receptor-modified T cells recognizing mesothelin in advanced solid cancers. Mol. Ther. 27, 1919–1929 (2019).
Yeh, S. et al. Ocular and systemic autoimmunity after successful tumor-infiltrating lymphocyte immunotherapy for recurrent, metastatic melanoma. Ophthalmology 116, 981–989. e981 (2009).
Kast, F., Klein, C., Umaña, P., Gros, A. & Gasser, S. Advances in identification and selection of personalized neoantigen/T-cell pairs for autologous adoptive T cell therapies. OncoImmunology 10, 1869389 (2021).
Renkvist, N., Castelli, C., Robbins, P. F. & Parmiani, G. A listing of human tumor antigens recognized by T cells. Cancer Immunol. Immunother. 50, 3–15 (2001).
Ahmed, M., Flannery, A., Daneshvar, C. & Breen, D. PET and neck ultrasound for the detection of cervical lymphadenopathy in patients with lung cancer and mediastinal lymphadenopathy. Respiration 96, 138–143 (2018).
Fultz, P. J. et al. Detection and diagnosis of nonpalpable supraclavicular lymph nodes in lung cancer at CT and US. Radiology 222, 245–251 (2002).
Niwa, H. et al. Patterns of mediastinal and supraclavicular metastases in apical invasive lung cancer–importance of supraclavicular lymph node dissection. Nihon Kyobu Geka Gakkai 42, 1142–1147 (1994).
Doebele, R. C. et al. Oncogene status predicts patterns of metastatic spread in treatment-naive nonsmall cell lung cancer. Cancer 118, 4502–4511 (2012).
Guerra, J. L. L. et al. Changes in pulmonary function after three-dimensional conformal radiotherapy, intensity-modulated radiotherapy, or proton beam therapy for non-small-cell lung cancer. Int. J. Radiat. Oncol. Biol. Phys. 83, e537–e543 (2012).
Weber, J. S. et al. Safety profile of nivolumab monotherapy: a pooled analysis of patients with advanced melanoma. J. Clin. Oncol. https://doi.org/10.1200/JCO.2015.66.1389 (2017).
Katz, S. I. et al. Radiologic pseudoprogression during anti-PD-1 therapy for advanced non-small cell lung cancer. J. Thorac. Oncol. 13, 978–986 (2018).
Jurtz, V. et al. NetMHCpan-4.0: improved peptide-MHC class I interaction predictions integrating eluted ligand and peptide binding affinity data. J. Immunol. 199, 3360–3368 (2017).
Forde, P. M. et al. Neoadjuvant PD-1 blockade in resectable lung cancer. N. Engl. J. Med. 378, 1976–1986 (2018).
Golubovskaya, V. & Wu, L. Different subsets of T cells, memory, effector functions, and CAR-T immunotherapy. Cancers 8, 36 (2016).
Precopio, M. L. et al. Immunization with vaccinia virus induces polyfunctional and phenotypically distinctive CD8+ T cell responses. J. Exp. Med. 204, 1405–1416 (2007).
Gainor, J. F. et al. EGFR mutations and ALK rearrangements are associated with low response rates to PD-1 pathway blockade in non-small cell lung cancer: a retrospective analysis. Clin. Cancer Res. 22, 4585–4593 (2016).
Lauss, M. et al. Mutational and putative neoantigen load predict clinical benefit of adoptive T cell therapy in melanoma. Nat. Commun. 8, 1–11 (2017).
Veatch, J. R. et al. Tumor-infiltrating BRAF V600E-specific CD4+ T cells correlated with complete clinical response in melanoma. J. Clin. Investig. 128, 1563–1568 (2018).
Tran, E. et al. Immunogenicity of somatic mutations in human gastrointestinal cancers. Science 350, 1387–1390 (2015).
Krishna, S. et al. Stem-like CD8 T cells mediate response of adoptive cell immunotherapy against human cancer. Science 370, 1328–1334 (2020).
Simpson-Abelson, M., D’Arigo, K., Hilton, F., Fardis, M. & Chartier, C. 1053P Iovance generation-2 tumour-infiltrating lymphocyte (TIL) product is reinvigorated during the manufacturing process. Ann. Oncol. 31, S720 (2020).
Simpson-Abelson, M., D’Arigo, K., Hilton, F., Fardis, M. & Chartier, C. Expanding Iovance’s tumor infiltrating lymphocytes (TIL) from core biopsies for adoptive T cell therapy using a 22-day manufacturing process. in SITC Annual Meeting (SITC, 2019).
Gros, A. et al. Recognition of human gastrointestinal cancer neoantigens by circulating PD-1+ lymphocytes. J. Clin. Investig. 129, 4992–5004 (2019).
Salas-Benito, D. et al. The mutational load and a T-cell inflamed tumour phenotype identify ovarian cancer patients rendering tumour-reactive T cells from PD-1+ tumour-infiltrating lymphocytes. Br. J. Cancer https://doi.org/10.1038/s41416-020-01218-4 (2021).
Malekzadeh, P. et al. Antigen experienced T cells from peripheral blood recognize p53 neoantigens. Clin. Cancer Res. 26, 1267–1276 (2020).
Cafri, G. et al. Memory T cells targeting oncogenic mutations detected in peripheral blood of epithelial cancer patients. Nat. Commun. 10, 1–9 (2019).
Carbone, D. P. et al. First-line nivolumab in stage IV or recurrent non-small-cell lung cancer. N. Engl. J. Med. 376, 2415–2426 (2017).
Yost, K. E. et al. Clonal replacement of tumor-specific T cells following PD-1 blockade. Nat. Med. 25, 1251–1259 (2019).
Sarnaik, A. et al. Long-term follow up of lifileucel (LN-144) cryopreserved autologous tumor infiltrating lymphocyte therapy in patients with advanced melanoma progressed on multiple prior therapies. J. Clin. Oncol. 38, 10006 (2020).
Andersen, R. et al. Long-lasting complete responses in patients with metastatic melanoma after adoptive cell therapy with tumor-infiltrating lymphocytes and an attenuated IL2 regimen. Clin. Cancer Res. 22, 3734–3745 (2016).
Xue, Q. et al. Single-cell multiplexed cytokine profiling of CD19 CAR-T cells reveals a diverse landscape of polyfunctional antigen-specific response. J. Immunother. Cancer 5, 85 (2017).
Danilova, L. et al. The mutation-associated neoantigen functional expansion of specific T cells (MANAFEST) assay: a sensitive platform for monitoring antitumor immunity. Cancer Immunol. Res. 6, 888–899 (2018).
Cox, J. & Mann, M. MaxQuant enables high peptide identification rates, individualized ppb-range mass accuracies and proteome-wide protein quantification. Nat. Biotechnol. 26, 1367–1372 (2008).
Li, H. & Durbin, R. Fast and accurate short read alignment with Burrows–Wheeler transform. Bioinformatics 25, 1754–1760 (2009).
DePristo, M. A. et al. A framework for variation discovery and genotyping using next-generation DNA sequencing data. Nat. Genet. 43, 491 (2011).
Saunders, C. T. et al. Strelka: accurate somatic small-variant calling from sequenced tumor–normal sample pairs. Bioinformatics 28, 1811–1817 (2012).
Cibulskis, K. et al. Sensitive detection of somatic point mutations in impure and heterogeneous cancer samples. Nat. Biotechnol. 31, 213–219 (2013).
Wang, K., Li, M. & Hakonarson, H. ANNOVAR: functional annotation of genetic variants from high-throughput sequencing data. Nucleic Acids Res. 38, e164–e164 (2010).
Lek, M. et al. Analysis of protein-coding genetic variation in 60,706 humans. Nature 536, 285–291 (2016).
Dobin, A. et al. STAR: ultrafast universal RNA-seq aligner. Bioinformatics 29, 15–21 (2013).
Anders, S., Pyl, P. T. & Huber, W. HTSeq: a Python framework to work with high-throughput sequencing data. Bioinformatics 31, 166–169 (2015).
Anders, S. & Huber, W. Differential expression analysis for sequence count data. Genome Biol. https://doi.org/10.1186/gb-2010-11-10-r106 (2010).
Nielsen, M. et al. Reliable prediction of T‐cell epitopes using neural networks with novel sequence representations. Protein Sci. 12, 1007–1017 (2003).
Reynisson, B. et al. Improved prediction of MHC II antigen presentation through integration and motif deconvolution of mass spectrometry MHC eluted ligand data. J. Proteome Res. https://doi.org/10.1021/acs.jproteome.9b00874 (2020).
Vita, R. et al. The immune epitope database (IEDB): 2018 update. Nucleic Acids Res. 47, D339–D343 (2019).
Ivanova, A., Qaqish, B. F. & Schell, M. J. Continuous toxicity monitoring in phase II trials in oncology. Biometrics 61, 540–545 (2005).
Acknowledgements
This work was supported by a Catalyst Award Clinical Trial grant through the Stand Up to Cancer Foundation (SU2C-AACR-CT04-17; to E.B.H., S.J.A.); Barbara Bauer Prelude to a Cure Foundation grant to B.C.C.; ER Squibb for nivolumab supply; Iovance Biotherapeutics as a research grant, Clinigen for aldesleukin supply, an NCI Cancer Center Support Grant (P30-CA076292; to E.B.H.) and 2018 Young Investigator award from Adaptive Biotechnologies to B.C.C. Stand Up 2 Cancer is a program of the Entertainment Industry Foundation administered by the American Association for Cancer Research. We thank the patients and their families who participated in this research; members of the Moffitt Cell Therapies Facility, including L. Kelley and C. Cox for cell manufacturing; C. Yang and T. Mesa at the Moffitt Molecular Genomics Facility, M. Wloch, N. Smith and K. Fahrner at the Moffitt Tissue Core and P. Cano at the Moffitt Histocompatibility Leukocyte Antigen laboratory; T. Boyle and G. Zhang for assistance with clinical specimens; C. Ulge for grant administration; M. Avedon for translational project management; and other members of our clinical and laboratory research teams. Cell sorting for this project was performed on instruments in the Moffitt Flow Cytometry Core. Sequencing was performed by the Moffitt Molecular Genomics and Proteomics & Metabolomics Core Facilities (supported in part by NCI Cancer Center Support Grant P30-CA076292). Clinical care and trial coordination was provided by the Moffitt Immune and Cellular Therapies department. We thank B. Banbury for assistance with the graphs of T cell clonotypes.
Author information
Authors and Affiliations
Contributions
The trial protocol was designed and written by the authors (B.C.C., A.A.S. and S.J.A.). S.A.A. and F.J.K. obtained grant funding. L.B.M. and W.C. coordinated the trial initiation and study procedures. Z.J.T. and D.-T.C. analyzed the clinical data and performed statistical analysis. E.B., B.C.C. and S.J.A. interpreted clinical data. C.W. and D.R.N. performed immunologic assays. S.K. and C.W. performed and supervised flow cytometry. J.K.T. and J.Y. performed and interpreted bioinformatics analyses. J.T.S. performed immunohistochemical staining scoring. Work related to TIL production was conducted and supervised by A.M.L. RNA and DNA sequencing preparations were supervised by B.C.C. and C.W. Genomic sequencing was performed and supervised by S.J.Y. Proteomic sequencing was performed and supervised by J.M.K. and B.Y. T.T., A.N.S., A.A.C., S.J.A. and B.C.C. informed patients and were responsible for patient care. E.M.T. and J.E.M. performed TIL surgery. S.P.T., E.B.H., S.J.A. and J.C.G. provided scientific input during protocol design and interpretation of the study. The manuscript was written by B.C.C. and C.W., together with all co-authors, who vouch for the accuracy of the data reported and adherence to the protocol. All authors edited and approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
Moffitt Cancer Center (Principal Investigator B.C.C.) was the sponsor of the trial. The trial was primarily supported by Stand Up to Cancer Foundation through the AACR Catalyst grant mechanism. Nivolumab was supplied by ER Squibb & Sons. Aldesleukin (IL-2) was supplied by Clinigen Group. Funding to the Moffitt Cell Therapies Facility was provided by Iovance Biotherapeutics. The companies played no other role in the study or report. B.C.C. has received speaking fees from AstraZeneca, ARIAD Pharmaceuticals and Hoffmann-La Roche and consultant fees from Xilio, Achilles, ER Squibb, Hoffmann-La Roche, AstraZeneca, AbbVie, KSQ Therapeutics, GlaxoSmithKline, Gilead Sciences, Celgene. B.C.C. has received research funding from NeoGenomics Laboratories and Adaptive Biotechnologies and has a patent application (WO2020263919A1). A.A.C. has received speaking fees from Genentech, Merck, Celgene and Takeda; consultant fees from Amgen, Jazz, AstraZeneca, Pfizer, Novartis, AbbVie and BMS; and research funding from AstraZeneca, Novartis and BMS, outside the submitted work. J.R.C.G. has received consultant fees from Leidos, consultant and nonfinancial support from Anixa Biosciences; consultant fees and nonfinancial support from Compass Therapeutics; and has a patent (WO2020033923A1) pending. E.B.B. has received consultant fees from Amgen and Janssen, outside the submitted work. S.K. reports nonfinancial and research financial support from BMS and AstraZeneca. A.M.L. received financial support from by Iovance Biotherapeutics. J.E.M. reports laboratory research support from Iovance Biotherapeutics for research outside the submitted work and a patent (62668246) licensed to Iovance Biotherapeutics. S.A.P.T. reports grants from Swim Across America Foundation, V Foundation, American Cancer Society Research Scholar Grant, State of Florida Bankhead-Coley Grant, Iovance Biotherapeutics, Intellia Therapeutics, Myst Therapeutics, NIH-NCI (grant nos. U54 CA193489-01A1, CA241559, U01 CA244100-01, R01 CA239219-01A1) and Provectus Biopharmaceuticals, outside the submitted work. In addition, S.A.P.T. has a patent (61/973,006 61/978,112) with royalties paid to Iovance Biotherapeutics and a patent immunotherapy targeted to tumors expressing receptors with royalties paid to Tuhura Biopharma. A.N.S. received nonfinancial support and research grants from Daiichi Sankyo, Novartis, Mersana, Genmab and Eli Lilly, outside the submitted work. A.A.S. reports grants from NCI K23, Ocala Royal Dames and Swim Across America Foundation; personal fees from Guidepoint and Gerson Lehrman Group; and consultant fees from Defined Health, Iovance Biotherapeutics, Physicians’ Educational Resource and Medscape, outside the submitted work. In addition, A.A.S. has a patent for Compositions and Methods for Improving Tumor-infiltrating Lymphocytes for Adoptive Cell Therapy (61/973,002) with royalties paid to Iovance Biotherapeutics, a patent for a Rapid Method for Culture of Tumor-infiltrating Lymphocytes from Core Needle Biopsies of Solid Tumors and a patent for Tumor-infiltrating Lymphocytes and Stapled Peptoid Peptide Hybrid Peptidomimetics (16/157,174). J.K.T. has grant support through P30-CA76292 and a patent pending for a Large Data Set Negative Information Storage Model. C.W. has a patent application filed for Generation of T Cell Receptors (TCRs) that React to Neoantigens. S.J.A. has received advisor fees from Achilles, Amgen, AstraZeneca, ER Squibb, Caris Life Sciences, Celsius Therapeutics, G1 Therapeutics, GlaxoSmithKline, Memgen, Merck & Co., Nektar Therapeutics, RAPT Therapeutics, Venn Therapeutics, Glympse, EMD Serano and Samyang Biopharm USA; and research funding from Cellular Biomedicine Group. The remaining authors declare no competing interests.
Additional information
Peer review information Nature Medicine thanks Pia Kvistborg, Solange Peters, Qian Wu and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Javier Carmona was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
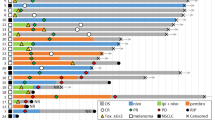
Extended Data Fig. 1 Clinical follow-up after initial nivolumab.
a, Sum of tumor diameters per RECIST v1.1 over time measured by serial CT scan. Patients with evidence of tumor enlargement or new lesions within 10 weeks of initial nivolumab were treated with TIL infusion. All enrolled patients (n = 20) are included. b, Clinical follow-up of patients after initial nivolumab with clinicopathologic features in a Swimmer’s plot. Pt 04 received bridging crizotinib due to rapid progression on nivolumab. Abbreviations: TPS denotes tumor proportion score using 22C3 PD-L1 antibody. TMB; estimated tumor mutation burden based upon exome sequencing. mut/MB mutations per mega-base. ‘Ex’ denotes exon, and ‘Δ’ denotes mutation conferring exon deletion. Smoking pack-years represents self-reported cigarette packs per day multiplied by total years.
Extended Data Fig. 2 Autologous reactivity screening of TIL cultured from individual tumor fragments in combination with baseline tumor cell suspensions.
Shown are the interferon-γ enzyme-linked immunosorbent assays conducted without (a) and with (b) CD3 bead positive controls. Each graph is labeled with the trial patient ID. The x-axis represents the TIL fragment selected for testing. Each fragment number represents an autologous T cell line generated from a unique tumor morsel cultured in IL-2 and media between 3 to 5 weeks. Each culture is labelled by its original fragment identification number, from 48 total per patient. Post-decimal numerals indicate the tumor number, if multiple tumor sites were harvested for the same patient. An asterisk denotes whether the fragment was deemed autologously reactive. Shown is the mean ± SEM of triplicate wells from a single ELISA experiment. Each bar denotes one biologically independent culture sample (n = 1). ‘≤10’ denotes a sample with absorbance reading below the lowest point of the standard curve performed for each assay. ‘TIL Ctrl’ denotes a TIL culture derived from an unrelated patient to serve as a positive control for the CD3 beads and a negative control for autologous substrate. Allogeneic cancer cell lines were selected as an optional control based on partial HLA class I allele compatibility with the patient. Patient ID 12 did not have sufficient TIL growth for manufacture, and ID 26 did not have sufficient tumor for autologous reactivity testing.
Extended Data Fig. 3 Feasibility of TIL harvest and intermediate-dose interleukin-2 infusion for all patients.
a, Total hours of length of stay (LOS) for inpatient admissions after TIL harvest surgery. Two patients had postoperative air-leak requiring multiple days of inpatient observation. All enrolled patients (n = 20) are included. b, The total duration of infusional IL-2 for all 16 patients after TIL treatment. Patients received TIL infusion on Day 0, followed by continuous IL-2 infusion beginning 12 hours later at a dose of 18 million international units (MIU) per m2 over 6, then 12, and then 24 hours followed by 4.5 MIU/m2 over 24 hours for 3 consecutive days. c, Total inpatient length of stay for all patients. Some patients were discharged to outpatient between cyclophosphamide admission and TIL admission.
Extended Data Fig. 4 Treatment-emergent adverse events reported with cyclophosphamide, fludarabine, TIL, and IL-2.
a, Adverse events grouped by National Cancer Institute preferred term occurring in 20% or more of patients attributable to cyclophosphamide, fludarabine, TIL, or IL-2. All TIL treated patients (n = 16) are included. b, All adverse events grouped by date of onset within 3 months of TIL. Patients with multiple events for a given term are counted once, using the maximum grade under each preferred term. Abbreviations: AE denotes adverse events; AST denotes aspartate aminotransferase; ALT denotes alanine aminotransferase; IL-2, interleukin-2.
Extended Data Fig. 5 Change in lymphocytes and neutrophils with lymphodepletion, TIL, and IL2.
a, Initial peak followed by recovery of peripheral blood absolute lymphocyte count. b, peripheral blood absolute neutrophil count recovered by median of 7.5 days (range 4.7 – 20.6). Shown is absolute cell count (1000 cells per mm3). TIL infusion is ‘Day 0’. All TIL treated patients are shown (n = 16).
Extended Data Fig. 6 Radiographic enlargement of a target lesion in patient 14.
Patient had biopsy-proven lung adenocarcinoma biopsy proven from a lymph node metastasis and pleural mass. She had increase in her only target lesion pleural metastasis post-TIL and biopsy revealed fibrosis. Whole exome sequencing conducted on the original tumor showed over four hundred somatic mutations. Only 3 mutations could be detected in the post-TIL biopsy despite 200x depth of sequencing. She had new metastases appear 1.4 years later. Shown is a representative hematoxylin and eosin (H&E) image from 15 high-powered field views, selected by diagnostic clinical pathologists. Bar denotes approximately 100 μm. Pre-TIL biopsy comprises 5 separate preserved blocks from 1 tumor from a single procedure performed on one day. Post-TIL biopsy comprises 3 core needle samples obtained from 4 total passes from a single procedure performed on one day. Each somatic mutation count represents 1 biologically independent sample.
Extended Data Fig. 7 Overall survival from enrollment.
a, Overall survival of all enrolled patients (n = 20) from date of enrollment. b, Overall survival of patients who had not received any anti-cancer systemic therapy prior to enrollment (n = 12), and c, of patients who had received at least one line of previous systemic therapy (n = 8). Hashmarks denote 95% confidence intervals for survival probability. All patients were assessed for survival through the data cut-off of 10 Sept. 2020.
Extended Data Fig. 8 In vitro expansion of autologous T-cell clonotypes after stimulation with peptide antigens.
Clonotypes with significant increase using autologous T and dendritic cells from a, Patient 25 and b, Patient 9. T cells were co-cultured with autologous dendritic cells for 10 days and compared to controls wells including T cells only and no peptides. TCR Vβ CDR3 AA denotes T-cell receptor Vβ complementarity-determining region 3 amino acid. Fold expansion is relative to baseline control without peptide.
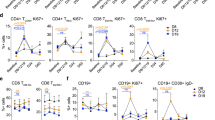
Extended Data Fig. 9 Expression of immune checkpoint ligands and cell composition of final infused TIL product.
a, Expression of immune checkpoint and cell activation markers assessed by flow cytometry as a proportion of either CD4+ or CD8+ T cells (n = 18 patients with 1 biologically independent experiment per patient, bar denotes median). b, Proportion of regulatory T cells (CD4+ CD25+CD127dim). (n = 18 patients with 1 biologically independent experiment per patient). c, TIL cell population stratified by t-distributed stochastic neighbor embedding (t-SNE) mapping of memory differentiation subsets. Defined cell populations were assigned specific colors. Each patient is labeled by Pt ID. There are 18 patients presented in total, with 1 biologically independent experiment per patient.
Extended Data Fig. 10 Phenotype and clonotype features of final infused TIL.
a, Best overall response (BORR) and proportion of tumor-specific fragments in the final product. All patients with sufficient TIL for autologous reactivity testing performance are shown (n = 18). Pt 26 had insufficient tumor digest for autologous reactivity testing, and Pt 12 had insufficient pre-REP TIL for testing. A proportion were tested for reactivity with autologous tumor suspension using ELISA for interferon-γ. Pink is the proportion of autologous-reactively cultures pooled for the final rapid expansion. Gray are either non-specific or negative cultures added to the pool, to ensure sufficient starting cell numbers. b, Patient BORR and dose of CD8+ or CD4+ cells in final expanded TIL product. All patients with final manufactured TIL are shown (n =18). Pt 30 pre-REP TIL is still cryopreserved, and Pt 12 had insufficient pre-REP TIL to manufacture. 48 minced tumor fragments were cultured in IL-2. c, Change in T cell clonotypic composition between original intratumor T cells and final infused TIL. Across patients, there were variable numbers of enriched clones in the TIL culture, with a range 13 to 1011 clones. A large proportion of clones in each patient were not detected in the baseline tumor. d, Comparison of the most prevalent one hundred clones in the manufactured TIL culture with baseline tumor, with total number shown on the x-axis and overlap in middle. High repertoire turnover during TIL culture was observed in most samples. Several cultures shared no high frequency clones with their baseline tumors. e, Productive clonality Simpson clonality increased from baseline tumor to final cultured TIL (Exact p = 0.000013, two-sided Wilcoxon signed rank test). Shown is the median and 95% confidence interval overlaying the individual values. All patients with manufactured TIL are shown (n =19). Abbreviations: NT; not treated. NE; not evaluable. uPR, unconfirmed partial response.
Supplementary information
Supplementary Information
Supplementary Tables 1 and 2 and Appendixes 1 and 2.
Supplementary Tables 3 and 4
Source data for neoantigen prediction priority (Table 3) and reactive peptide neoantigens with their predicted binding affinities (Table 4) as tabs of the spreadsheet.
Supplementary Protocol
Clinical trial protocol.
Source data
Source Data Extended Data Fig. 2
Source data for the screening of individual patient TIL fragments for autologous reactivity by IFN-g capture ELISA (each tab corresponds to the patient ID).
Rights and permissions
About this article
Cite this article
Creelan, B.C., Wang, C., Teer, J.K. et al. Tumor-infiltrating lymphocyte treatment for anti-PD-1-resistant metastatic lung cancer: a phase 1 trial. Nat Med 27, 1410–1418 (2021). https://doi.org/10.1038/s41591-021-01462-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-021-01462-y
This article is cited by
-
Functional CRISPR screens in T cells reveal new opportunities for cancer immunotherapies
Molecular Cancer (2024)
-
Enhanced cellular therapy: revolutionizing adoptive cellular therapy
Experimental Hematology & Oncology (2024)
-
Systematic investigation of chemo-immunotherapy synergism to shift anti-PD-1 resistance in cancer
Nature Communications (2024)
-
CAR T cell therapy for patients with solid tumours: key lessons to learn and unlearn
Nature Reviews Clinical Oncology (2024)
-
First cell therapy for solid tumours heads to the clinic: what it means for cancer treatment
Nature (2024)