Abstract
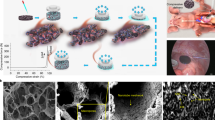
Despite advances in technologies for cardiac repair after myocardial infarction (MI), new integrated therapeutic approaches still need to be developed. In this study, we designed a perfusable, multifunctional epicardial device (PerMed) consisting of a biodegradable elastic patch (BEP), permeable hierarchical microchannel networks (PHMs) and a system to enable delivery of therapeutic agents from a subcutaneously implanted pump. After its implantation into the epicardium, the BEP is designed to provide mechanical cues for ventricular remodeling, and the PHMs are designed to facilitate angiogenesis and allow for infiltration of reparative cells. In a rat model of MI, implantation of the PerMed improved ventricular function. When connected to a pump, the PerMed enabled targeted, sustained and stable release of platelet-derived growth factor-BB, amplifying the efficacy of cardiac repair as compared to the device without a pump. We also demonstrated the feasibility of minimally invasive surgical PerMed implantation in pigs, demonstrating its promise for clinical translation to treat heart disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The Gene Ontology annotations were downloaded from the National Center for Biotechnology Information (http://www.ncbi.nlm.nih.gov/), UniProt (http://www.UniProt.org/) and Gene Ontology (http://www.geneontology.org/). The significant pathways of the DEGs were analyzed according to the KEGG database (https://www.genome.jp/kegg/kegg1.html). The data that support the findings of this study are available within the article and its Supplementary Information files. Imaging source data about cMRI, PET and Masson’s trichrome staining are provided in Supplementary Fig. 5a–c. Statistical source data of figures and extended data figures are provided with this paper. The data that support the findings of this study are available from the corresponding author upon reasonable request. Source data are provided with this paper.
References
Benjamin, E. J. et al. Heart disease and stroke statistics—2018 update: a report from the American Heart Association. Circulation 137, e67–e492 (2018).
Owens, A. T., Brozena, S. C. & Jessup, M. New management strategies in heart failure. Circ. Res. 118, 480–495 (2016).
Braunwald, E. The war against heart failure: the Lancet lecture. Lancet 385, 812–824 (2015).
Cohn, W. E., Timms, D. L. & Frazier, O. H. Total artificial hearts: past, present, and future. Nat. Rev. Cardiol. 12, 609–617 (2015).
Yacoub, M. Cardiac donation after circulatory death: a time to reflect. Lancet 385, 2554–2556 (2015).
Prabhu, S. D. & Frangogiannis, N. G. The biological basis for cardiac repair after myocardial infarction: from inflammation to fibrosis. Circ. Res. 119, 91–112 (2016).
Gao, L. et al. Large cardiac muscle patches engineered from human induced-pluripotent stem cell-derived cardiac cells improve recovery from myocardial infarction in swine. Circulation 137, 1712–1730 (2018).
Park, S. J. et al. Dual stem cell therapy synergistically improves cardiac function and vascular regeneration following myocardial infarction. Nat. Commun. 10, 3123 (2019).
Chachques, J.C. et al. Elastomeric cardiopatch scaffold for myocardial repair and ventricular support. Eur. J. Cardiothorac. Surg. 57, 545–555 (2019).
Feiner, R. et al. Engineered hybrid cardiac patches with multifunctional electronics for online monitoring and regulation of tissue function. Nat. Mater. 15, 679–685 (2016).
Engelmayr, G. C. Jr. et al. Accordion-like honeycombs for tissue engineering of cardiac anisotropy. Nat. Mater. 7, 1003–1010 (2008).
Liu, N. et al. Advances in 3D bioprinting technology for cardiac tissue engineering and regeneration. Bioact. Mater. 6, 1388–1401 (2021).
Serpooshan, V. et al. The effect of bioengineered acellular collagen patch on cardiac remodeling and ventricular function post myocardial infarction. Biomaterials 34, 9048–9055 (2013).
Lin, X. et al. A viscoelastic adhesive epicardial patch for treating myocardial infarction. Nat. Biomed. Eng. 3, 632–643 (2019).
Taylor, D. A., Chandler, A. M., Gobin, A. S. & Sampaio, L. C. Maximizing cardiac repair: should we focus on the cells or on the matrix? Circ. Res. 120, 30–32 (2017).
Fujimoto, K. L. et al. An elastic, biodegradable cardiac patch induces contractile smooth muscle and improves cardiac remodeling and function in subacute myocardial infarction. J. Am. Coll. Cardiol. 49, 2292–2300 (2007).
Yang, Y. et al. Elastic 3D-printed hybrid polymeric scaffold improves cardiac remodeling after myocardial infarction. Adv. Health. Mater. 8, e1900065 (2019).
Madden, L. R. et al. Proangiogenic scaffolds as functional templates for cardiac tissue engineering. Proc. Natl Acad. Sci. USA 107, 15211–15216 (2010).
Zieber, L., Or, S., Ruvinov, E. & Cohen, S. Microfabrication of channel arrays promotes vessel-like network formation in cardiac cell construct and vascularization in vivo. Biofabrication 6, 024102 (2014).
Dvir, T., Timko, B. P., Kohane, D. S. & Langer, R. Nanotechnological strategies for engineering complex tissues. Nat. Nanotechnol. 6, 13–22 (2011).
Hastings, C. L. et al. Drug and cell delivery for cardiac regeneration. Adv. Drug Deliv. Rev. 84, 85–106 (2015).
Lee, A. S. et al. Prolonged survival of transplanted stem cells after ischaemic injury via the slow release of pro-survival peptides from a collagen matrix. Nat. Biomed. Eng. 2, 104–113 (2018).
Nguyen, M. M. et al. Enzyme-responsive nanoparticles for targeted accumulation and prolonged retention in heart tissue after myocardial infarction. Adv. Mater. 27, 5547–5552 (2015).
Shen, X. et al. Sequential and sustained release of SDF-1 and BMP-2 from silk fibroin-nanohydroxyapatite scaffold for the enhancement of bone regeneration. Biomaterials 106, 205–216 (2016).
Whyte, W. et al. Sustained release of targeted cardiac therapy with a replenishable implanted epicardial reservoir. Nat. Biomed. Eng. 2, 416–428 (2018).
Zimmermann, W. H. et al. Engineered heart tissue grafts improve systolic and diastolic function in infarcted rat hearts. Nat. Med. 12, 452–458 (2006).
Vagnozzi, R. J. et al. An acute immune response underlies the benefit of cardiac stem cell therapy. Nature 577, 405–409 (2020).
Sun, X., Altalhi, W. & Nunes, S. S. Vascularization strategies of engineered tissues and their application in cardiac regeneration. Adv. Drug Deliv. Rev. 96, 183–194 (2016).
Lei, D. et al. 3D printing of biomimetic vasculature for tissue regeneration. Mater. Horiz. 6, 1197–1206 (2019).
Chen, Q. Z. et al. Characterisation of a soft elastomer poly(glycerol sebacate) designed to match the mechanical properties of myocardial tissue. Biomaterials 29, 47–57 (2008).
Galan, D. T. et al. Reduced mitochondrial respiration in the ischemic as well as in the remote nonischemic region in postmyocardial infarction remodeling. Am. J. Physiol. Heart Circ. Physiol. 311, H1075–h1090 (2016).
Carmeliet, P. & Jain, R. K. Molecular mechanisms and clinical applications of angiogenesis. Nature 473, 298–307 (2011).
Holmes, D. F. et al. Synchronized mechanical oscillations at the cell-matrix interface in the formation of tensile tissue. Proc. Natl Acad. Sci. USA 115, E9288–e9297 (2018).
Gullbrand, S. E. et al. Long-term mechanical function and integration of an implanted tissue-engineered intervertebral disc. Sci. Transl. Med. 10, eaau0670 (2018).
Kilarski, W. W., Samolov, B., Petersson, L., Kvanta, A. & Gerwins, P. Biomechanical regulation of blood vessel growth during tissue vascularization. Nat. Med. 15, 657–664 (2009).
Lesman, A., Rosenfeld, D., Landau, S. & Levenberg, S. Mechanical regulation of vascular network formation in engineered matrices. Adv. Drug Deliv. Rev. 96, 176–182 (2016).
Rodrigues, M., Kosaric, N., Bonham, C. A. & Gurtner, G. C. Wound healing: a cellular perspective. Physiol. Rev. 99, 665–706 (2019).
Huang, S., Yang, Y., Yang, Q., Zhao, Q. & Ye, X. Engineered circulatory scaffolds for building cardiac tissue. J. Thorac. Dis. 10, S2312–S2328 (2018).
LaValley, D. J. & Reinhart-King, C. A. Matrix stiffening in the formation of blood vessels. Advances in Regenerative Biology 1, 25247 (2014).
Lesman, A. et al. Engineering vessel-like networks within multicellular fibrin-based constructs. Biomaterials 32, 7856–7869 (2011).
Urech, L., Bittermann, A. G., Hubbell, J. A. & Hall, H. Mechanical properties, proteolytic degradability and biological modifications affect angiogenic process extension into native and modified fibrin matrices in vitro. Biomaterials 26, 1369–1379 (2005).
van den Borne, S. W. et al. Myocardial remodeling after infarction: the role of myofibroblasts. Nat. Rev. Cardiol. 7, 30–37 (2010).
Frangogiannis, N. G. Pathophysiology of myocardial infarction. Compr. Physiol. 5, 1841–1875 (2015).
McWhorter, F. Y., Davis, C. T. & Liu, W. F. Physical and mechanical regulation of macrophage phenotype and function. Cell Mol. Life Sci. 72, 1303–1316 (2015).
Awada, H. K., Johnson, N. R. & Wang, Y. Sequential delivery of angiogenic growth factors improves revascularization and heart function after myocardial infarction. J. Control. Release 207, 7–17 (2015).
Hsieh, P. C., Davis, M. E., Gannon, J., MacGillivray, C. & Lee, R. T. Controlled delivery of PDGF-BB for myocardial protection using injectable self-assembling peptide nanofibers. J. Clin. Invest. 116, 237–248 (2006).
Tang, J. et al. Cardiac cell-integrated microneedle patch for treating myocardial infarction. Sci. Adv. 4, eaat9365 (2018).
Beck, R. W., Bergenstal, R. M., Laffel, L. M. & Pickup, J. C. Advances in technology for management of type 1 diabetes. Lancet 394, 1265–1273 (2019).
Yuan, Z. et al. Injectable citrate-based hydrogel as an angiogenic biomaterial improves cardiac repair after myocardial infarction. ACS Appl. Mater. Interfaces 11, 38429–38439 (2019).
Gu, X. et al. Sustained viral gene delivery from a micro-fibrous, elastomeric cardiac patch to the ischemic rat heart. Biomaterials 133, 132–143 (2017).
Huynh, K. Basic research: minimally invasive delivery of engineered cardiac patches for heart repair. Nat. Rev. Cardiol. 14, 568–569 (2017).
Liu, B. et al. Cardiac recovery via extended cell-free delivery of extracellular vesicles secreted by cardiomyocytes derived from induced pluripotent stem cells. Nat. Biomed. Eng. 2, 293–303 (2018).
Montgomery, M. et al. Flexible shape-memory scaffold for minimally invasive delivery of functional tissues. Nat. Mater. 16, 1038–1046 (2017).
Dorn, G. II Mitochondrial fission/fusion and cardiomyopathy. Curr. Opin. Genet. Dev. 38, 38–44 (2016).
Lei, D. et al. A general strategy of 3D printing thermosets for diverse applications. Mater. Horiz. 6, 394–404 (2019).
Yeh, Y. C., Highley, C. B., Ouyang, L. & Burdick, J. A. 3D printing of photocurable poly(glycerol sebacate) elastomers. Biofabrication 8, 045004 (2016).
Annabi, N. et al. Engineering a highly elastic human protein-based sealant for surgical applications. Sci. Transl. Med. 9, eaai7466 (2017).
Tang, X. et al. SIRT2 acts as a cardioprotective deacetylase in pathological cardiac hypertrophy. Circulation 136, 2051–2067 (2017).
Yan, X. et al. Dectin-2 deficiency modulates Th1 differentiation and improves wound healing after myocardial infarction. Circ. Res. 120, 1116–1129 (2017).
Du, J. et al. Time-phase sequential utilization of adipose-derived mesenchymal stem cells on mesoporous bioactive glass for restoration of critical size bone defects. ACS Appl. Mater. Interfaces 10, 28340–28350 (2018).
Ternacle, J. et al. Causes and consequences of longitudinal LV dysfunction assessed by 2D strain echocardiography in cardiac amyloidosis. JACC Cardiovasc. Imaging 9, 126–138 (2016).
Carmichael, B. B. et al. Effects of surgical ventricular restoration on left ventricular function: dynamic MR imaging. Radiology 241, 710–717 (2006).
Hsieh, P. C., MacGillivray, C., Gannon, J., Cruz, F. U. & Lee, R. T. Local controlled intramyocardial delivery of platelet-derived growth factor improves postinfarction ventricular function without pulmonary toxicity. Circulation 114, 637–644 (2006).
Ashburner, M. et al. Gene ontology: tool for the unification of biology. The Gene Ontology Consortium. Nat. Genet. 25, 25–29 (2000).
Draghici, S. et al. A systems biology approach for pathway level analysis. Genome Res. 17, 1537–1545 (2007).
Acknowledgements
We acknowledge financial support by the Natural Science Foundation of China (81671832, 81571826 and 21574019), the Shanghai Municipal Education Commission–Gaofeng Clinical Medicine Grant Support (826158), the Natural Science Foundation of Shanghai (20ZR1402500 and 18ZR1401900), Belt & Road Young Scientist Exchanges Project of Science and Technology Commission Foundation of Shanghai (20520741000), Science and Technology Commission of Shanghai Municipality (20DZ2254900 and 20DZ2270800), the Donghua University International Postdoctoral Program, the Shanghai Belt and Road Joint Laboratory of Advanced Fiber and Low-dimension Materials (Donghua University) (18520750400), the Fundamental Research Funds for the Central Universities and DHU Distinguished Young Professor Program (LZA2019001).
Author information
Authors and Affiliations
Contributions
S.H. designed the study, performed all experiments, analyzed the data and wrote and edited the manuscript and figures. D.L. designed and fabricated PerMeds, performed SEM characterization and mechanical testing and wrote the manuscript. Q.Y., Y.Y., C.J. and H.S. contributed to the animal experiments. W.C. contributed to mechanical testing. L.W. and W.H. instructed imaging study, including cMRI, micro-CT and PET–CT. Q.Z. designed and supervised the animal experiments and wrote the manuscript. Z.Y. designed and supervised the fabrication of PerMeds and testing of the materials and wrote the manuscript. X.Y. designed and supervised the whole work and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information Michael Basson was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Structure and hydrophilicity of BEPs and PHMs.
a, Gross images of BEPs with different proportions. The arrows indicate the phase separation of the PCL. b, SEM images from the side view (i) and the top view (ii) presenting the structural integrity of the PGS/PCL (9:1) BEP, n = 3 independent experiments. c,d, Contact angle of BEPs at 10 s; n = 6 independent experiments per group. e-h, Morphology and microstructure of PHMs, n = 3 independent experiments per group. i, Contact angle and dynamic contact angle of PHMs; n = 4 independent experiments. The data are expressed as mean ± s.d. NS indicates not significant. The data are expressed as mean ± s.d. ***p<0.001. Data were analysed by one-way ANOVA followed by Bonferroni’s post hoc test.
Extended Data Fig. 2 Characterization of BEPs and PHMs.
a, Tensile strain-stress curves of BEPs (The bottom black X axis and the left black Y axis correspond to PGS and PGS/PCL(9:1) BEPs. The top red X axis and the right red Y axis correspond to PCL BEP) (i); the tensile modulus of BEPs (ii); the compressive strain-stress curves of BEPs (iii); the compressive modulus of BEPs (iv); n = 4 independent experiments per group. b, SEM images of the sutured PGS/PCL (9:1) BEP (i) and PGS BEP (ii); mechanical testing (iii) and quantitative analysis of the maximum breaking load (N) (iv); n = 4 independent experiments per group. c, Compressive modulus of PHMs; n = 4 independent experiments per group. The data are expressed as mean ± s.d. ***p<0.001. Data in (a (iv)) and (c) were analysed by one-way ANOVA followed by Bonferroni’s post hoc test; data in (a (ii)) and (b) were analysed using a two-tailed Student’s t-test.
Extended Data Fig. 3 In vitro biocompatibility of PHMs.
a,b, Quantification of ADSCs (a) and CFs (b) viability by CCK-8 assay on days 1, day 3 and day 7; n = 6 independent experiments per group. c, SEM images showing CF attachment to and retention on the interconnected microchannels of the PCL/gelatin (3:1) PHMs; n = 4 independent experiments. Arrow indicates CFs. d, 3D image of CFs on the surface of the PHMs by live/dead staining 7 days after cell seeding, n = 6 independent experiments per group. The data are expressed as mean ± s.d. *p<0.05 and ***p<0.001. Data were analysed by one-way ANOVA followed by Bonferroni’s post hoc test. CFs: cardiac fibroblasts; ADSCs: adipose-derived stem cells.
Extended Data Fig. 4 In vitro biocompatibility of BEPs.
a,b, Quantification of ADSCs (a) and CFs (b) viability by CCK-8 assay on days 1, 3 and 7; n = 6 independent experiments per group. c, Live/dead staining of ADSCs and CFs (i); immunofluorescence staining of NRCMs (α-actinin, red) and ADSCs (actin, green). d,e, Quantification of the ratio of live cells or dead cells to total cells for ADSCs (d) and CFs (e); n = 6 independent experiments per group. The data are expressed as mean ± s.d. NS indicates not significant. Data were analysed by one-way ANOVA followed by Bonferroni’s post hoc test. CFs: cardiac fibroblasts; ADSCs: adipose-derived stem cells; NRCMs: neonatal rat cardiomyocytes.
Extended Data Fig. 5 Histological assessment and evaluation of the angiogenic effect of PHMs and BEPs.
a, Representative Masson’s trichrome staining on day 28. b, Quantitative analysis of the wall thickness based on the Masson’s trichrome staining; n = 8 biologically independent samples per group. c, Representative staining in the IZ, BZ and in the BEP/PHMs for α-SMA (green), CD31 (red), and DAPI (blue) to visualize arteries on day 28. d-f, Quantitative analysis of the vessel number in all groups based on immunofluorescent staining for α-SMA (green), CD31 (red), and DAPI (blue); n = 6 biologically independent samples per group. HPF: high-power field; IZ: infarcted zone; BZ: border zone. The data are expressed as mean ± s.d. NS indicates not significant. ***p<0.001 and **p<0.01. Data were analysed by one-way ANOVA followed by Bonferroni’s post hoc test.
Extended Data Fig. 6 Illustration of cardiomyocyte apoptosis after PerMed implantation.
a, Representative images of cardiomyocyte apoptosis after PerMed implantation. b, Quantification of apoptotic cells in the IZ; n = 5 biologically independent samples per group. The data are expressed as mean ± s.d. IZ: infarcted zone; BZ: border zone.
Extended Data Fig. 7 Evaluation of capacity of PerMed for liquid distribution.
a, Representative in vivo CT images before and after the injection of contrast medium to assess the distribution of liquid on days 7, 14 and 28 (i); quantitative analysis of the ratio of the CT value after to before the injection of contrast medium (CT valueaft / CT valuebef) (ii); n = 3 biologically independent animals per group. b, Representative in vitro CT images before and after the injection of contrast medium to assess the distribution of liquid within PerMed on days 7, 14 and 28 (i); CT valueaft/CT valuebef was also analysed (ii); n = 3 biologically independent samples per group. c, Representative Masson’s trichrome staining in the IZ (i); assessment of PHMs porosity on days 7, 14 and 28 (ii); n = 7 biologically independent samples for Day 7 group, n = 8 biologically independent samples for Day 14 and 28 group. The data are expressed as mean ± s.d. NS indicates not significant. Data were analysed by one-way ANOVA followed by Bonferroni’ s post hoc test. IZ: infarcted zone.
Extended Data Fig. 8 Evaluation of the diffusion of a viral vector from the PerMed to the heart.
a, Representative images of immunofluorescence staining for GFP and α-actinin 7 and 28 days after implantation of the PerMed in the BZ. b, Representative images of immunofluorescence staining for GFP and α-SMA 7 and 28 days after implantation of the PerMed in the border zone. c, Quantitative analysis of the expression of GFP by the ratio of the GFP area to the ROI area; n = 5 biologically independent samples per group. The data are expressed as mean ± s.d. NS indicates not significant. Data in (c) were analysed using a two-tailed Student’s t-test. AAV9: adeno-associated virus 9; GFP: green fluorescent protein; ROI: region of interest; BZ: border zone.
Extended Data Fig. 9 Evaluation of the diffusion of a small molecule from the PerMed to the heart by PET-CT.
a, Representative PET-CT images every hour on the TRA, COR and SAG axis on days 7 and day 28. TRA: transverse; COR: coronal; SAG: sagittal; SUV: standardized uptake value.
Extended Data Fig. 10 Vision for clinical translation of the PerMed.
a, Schematic of the design and components of the PerMed equipped with the claw-shaped fixator. b, Design of the claw-shaped fixators with components of different types and sizes. The claw-shaped fixator consisted of a middle ring and three or four lateral arms with barbs (i, ii). The height of the arms was 4.0, 4.5, 5.0 and 6.0 mm (iii, iv); ‘h’ indicates the length of the arm, ‘w’ indicates the width of the arm, and ‘r’ indicates the diameter of the middle ring. c, Schematic of the clinical application of the PerMed. T1 indicates trocar 1; T2 indicates trocar 2; T3 indicates trocar 3. d, Schematic of the process of minimally invasive surgical implantation of the PerMed under thoracoscopic guidance, including compression of the PerMed (i), delivery of the PerMed through T2, stretching of the PerMed (iii), anchoring of the PerMed onto the surface of the porcine heart (iv, v) and extraction of the outer sheath (vi). Purple rings indicate the location of the PerMed. e, Image of the PerMed used in the porcine heart (3 cm in diameter and 2 mm in thickness). f, Top view of the PerMed anchored onto a porcine heart(i), closure of the pericardium, and conformability of the PerMed to the porcine heart (iii), n = 3 independent experiments.
Supplementary information
Supplementary Information
Supplementary Figs. 1–14, Supplementary Movie legends 1–8 and Supplementary Tables 1–4.
Supplementary Movie 1
Live and dead staining of CFs on the PCL/gelatin (3:1) PHMs.
Supplementary Movie 2
Continuous frames of cMRI cine sequence in the MI group.
Supplementary Movie 3
Continuous frames of cMRI cine sequence in the PerMed (PGS/PCL) group.
Supplementary Movie 4
3D reconstruction of the microvasculature within the PHMs (lower layer of the PerMed) 28 d after in vivo implantation.
Supplementary Movie 5
Perfusion of the PerMed with methylene blue liquid in vitro.
Supplementary Movie 6
Minimally invasive surgical implantation of the PerMed on the porcine heart under thoracoscopic guidance.
Supplementary Movie 7
Permanent ligation of the LAD to establish a rat MI model.
Supplementary Movie 8
Implantation of the PerMed onto the epicardial surface of the rat heart.
Source data
Source Data Fig. 1
Statistical source data.
Source Data Fig. 2
Statistical source data.
Source Data Fig. 3
Statistical source data.
Source Data Fig. 4
Statistical source data.
Source Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 1
Statistical source data
Source Data Extended Data Fig. 2
Statistical source data.
Source Data Extended Data Fig. 3
Statistical source data.
Source Data Extended Data Fig. 4
Statistical source data.
Source Data Extended Data Fig. 5
Statistical source data.
Source Data Extended Data Fig. 6
Statistical source data.
Source Data Extended Data Fig. 7
Statistical source data.
Source Data Extended Data Fig. 8
Statistical source data.
Rights and permissions
About this article
Cite this article
Huang, S., Lei, D., Yang, Q. et al. A perfusable, multifunctional epicardial device improves cardiac function and tissue repair. Nat Med 27, 480–490 (2021). https://doi.org/10.1038/s41591-021-01279-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-021-01279-9
This article is cited by
-
A mechanical-assisted post-bioprinting strategy for challenging bone defects repair
Nature Communications (2024)
-
Chronological adhesive cardiac patch for synchronous mechanophysiological monitoring and electrocoupling therapy
Nature Communications (2023)
-
Hydrogels with tunable mechanical plasticity regulate endothelial cell outgrowth in vasculogenesis and angiogenesis
Nature Communications (2023)
-
A topological polymer network with Cu(II)-coordinated reversible imidazole-urea locked unit constructs an ultra-strong self-healing elastomer
Science China Chemistry (2023)
-
Bio-manufacturing innovation lights up the future
Bio-Design and Manufacturing (2023)