Abstract
A total of 2,618,862 participants reported their potential symptoms of COVID-19 on a smartphone-based app. Among the 18,401 who had undergone a SARS-CoV-2 test, the proportion of participants who reported loss of smell and taste was higher in those with a positive test result (4,668 of 7,178 individuals; 65.03%) than in those with a negative test result (2,436 of 11,223 participants; 21.71%) (odds ratio = 6.74; 95% confidence interval = 6.31–7.21). A model combining symptoms to predict probable infection was applied to the data from all app users who reported symptoms (805,753) and predicted that 140,312 (17.42%) participants are likely to have COVID-19.
Similar content being viewed by others
Main
COVID-19 is an acute respiratory illness caused by the novel coronavirus severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Since its outbreak in China in December 2019, over 2,573,143 cases have been confirmed worldwide (as of 21 April 2020; https://www.worldometers.info/coronavirus/). Although many people have presented with flu-like symptoms, widespread population testing is not yet available in most countries, including the United States (https://www.cdc.gov/coronavirus/2019-ncov/cases-updates/testing-in-us.html) and United Kingdom1. Thus, it is important to identify the combination of symptoms most predictive of COVID-19, to help guide recommendations for self-isolation and prevent further spread of the disease2.
Case reports and mainstream media articles from various countries indicate that a number of patients with diagnosed COVID-19 developed anosmia (loss of smell)3,4. Mechanisms of action for the SARS-CoV-2 viral infection causing anosmia have been postulated5,6. Other studies indicate that a number of infected individuals present anosmia in the absence of other symptoms7,8, suggesting that this symptom could be used as screening tool to help identify people with potential mild cases who could be recommended to self-isolate9.
We investigated whether loss of smell and taste is specific to COVID-19 in 2,618,862 individuals who used an app-based symptom tracker10 (Methods). The symptom tracker is a free smartphone application that was launched in the United Kingdom on 24 March 2020, and in the United States on 29 March 2020. It collects data from both asymptomatic and symptomatic individuals and tracks in real time how the disease progresses by recording self-reported health information on a daily basis, including symptoms, hospitalization, reverse-transcription PCR (RT-PCR) test outcomes, demographic information and pre-existing medical conditions.
Between 24 March and 21 April 2020, 2,450,569 UK and 168,293 US individuals reported symptoms through the smartphone app. Of the 2,450,569 participants in the United Kingdom, 789,083 (32.2%) indicated having one or more potential symptoms of COVID-19 (Table 1). In total, 15,638 UK and 2,763 US app users reported having had an RT-PCR SARS-CoV-2 test, and having received the outcome of the test. In the UK cohort, 6,452 participants reported a positive test and 9,186 participants had a negative test. In the cohort from the United Kingdom, of the 6,452 participants who tested positive for SARS-CoV-2, 4,178 (64.76%) reported loss of smell and taste, compared with 2,083 out of 9,186 participants (22.68%) who tested negative (odds ratio (OR) = 6.40; 95% confidence interval (CI) = 5.96–6.87; P < 0.0001 after adjusting for age, sex and body mass index (BMI)). We replicated this result in the US subset of participants who had been tested for SARS-CoV-2 (adjusted OR = 10.01; 95% CI = 8.23–12.16; P < 0.0001) and combined the adjusted results using inverse variance fixed-effects meta-analysis (OR = 6.74; 95% CI = 6.31–7.21; P < 0.0001).
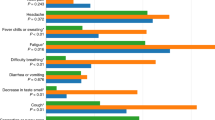
We re-ran logistic regressions adjusting for age, sex and BMI to identify other symptoms besides anosmia that might be associated with being infected by SARS-CoV-2. All ten symptoms queried (fever, persistent cough, fatigue, shortness of breath, diarrhea, delirium, skipped meals, abdominal pain, chest pain and hoarse voice) were associated with testing positive for COVID-19 in the UK cohort, after adjusting for multiple testing (Fig. 1a). In the US cohort, only loss of smell and taste, fatigue and skipped meals were associated with a positive test result.
a, Association between symptoms and the odds ratio of SARS-CoV-2 infection in 15,638 UK and 2,763 US participants who were tested via RT-PCR. Error bars represent 95% CIs. b,c, ROCs for prediction in the UK test set (b) and US validation set (c) of the risk of a positive test for SARS-CoV-2, using the following self-reported symptoms and traits: persistent cough, fatigue, skipped meals, loss of smell and taste, sex and age. Values for AUC, sensitivity (SE), specificity (SP), positive predictive value (PPV) and negative predictive value (NPV) are shown, with 95% CIs in parentheses.
We performed stepwise logistic regression in the UK cohort, by randomly dividing it into training and test sets (ratio: 80:20) to identify independent symptoms most strongly correlated with COVID-19, adjusting for age, sex and BMI. A combination of loss of smell and taste, fatigue, persistent cough and loss of appetite resulted in the best model (with the lowest Akaike information criterion). We therefore generated a linear model for symptoms that included loss of smell and taste, fatigue, persistent cough and loss of appetite to obtain a symptoms prediction model for COVID-19:
where all symptoms are coded as 1 if the person self-reports the symptom and 0 if not. The sex feature is also binary, with 1 indicative of male participants and 0 representing females. The obtained value is then transformed into predicted probability using exp(x)/(1 + exp(x)) transformation followed by assigning cases of predicted COVID-19 for probabilities >0.5 and controls for probabilities <0.5.
In the UK test set, the prediction model had a sensitivity of 0.65 (0.62–0.67), a specificity of 0.78 (0.76–0.80), an area under the curve (AUC) of the receiver operating characteristic curve (ROC) (that is, ROC-AUC) of 0.76 (0.74–0.78), a positive predictive value of 0.69 (0.66–0.71) and a negative predictive value of 0.75 (0.73–0.77) (Fig. 1b). A cross-validation ROC-AUC was 0.75 (0.74–0.76) in the 15,638 UK users who were tested for SARS-CoV-2. In this model, the strongest predictor was loss of smell and taste (Fig. 1a). Excluding loss of smell and taste from the model resulted in reduced sensitivity (0.33 (0.30–0.35)) but increased specificity (0.84 (0.83–0.86)). We also computed the ROC-AUC with stratification for sex and age groups and found that the results were similar in all groups, with no significant differences between strata, suggesting that our model works similarly within different sex and age groups. We validated the model in the US cohort and found an ROC-AUC of 0.76 (0.74–0.78), a sensitivity of 0.66 (0.62–0.69), a specificity of 0.83 (0.82–0.85), a positive predictive value of 0.58 (0.55–0.62) and a negative predictive value 0.87 (0.86–0.89) (Fig. 1c).
We also queried whether the association between loss of smell and taste and COVID-19 was influenced by mainstream media reports. We assessed the correlation between loss of smell and taste and being COVID-19 positive in different date ranges: (1) 24 March to 3 April 2020, following a number of reports in the UK mainstream media (for example, ref. 11) reporting anosmia as a symptom of COVID-19; (2) the week of 4–10 April 2020; and (3) from 11–21 April 2020. In the United Kingdom, the OR (95% CI) values for the associations of self-reported loss of smell and taste and a positive test for COVID-19 across these periods were 4.98 (4.47–5.56), 6.64 (5.75–7.68) and 10.40 (9.08–11.91), respectively, suggesting that awareness of loss of smell and taste as symptoms of COVID-19 in the UK has increased following media reports. However, this association was not found in the US cohorts: 24 March to 3 April: 8.13 (5.18–12.78); 4–10 April: 12.30 (8.96–16.90); 11–21 April: 9.13 (6.73–12.38).
Finally, we applied the predictive model to the 805,753 UK and US symptom-reporting individuals who had not been tested for COVID-19 and found that, according to our model, 140,312 (116,400–164,224) of these 805,753 participants (17.42% (14.45–20.39%)) reporting some symptoms were likely to be infected by the virus, representing 5.36% as a proportion of the overall responders to the app.
We report that loss of smell and taste is a potential predictor of COVID-19 in addition to other, more established, symptoms including high temperature and a new, persistent cough. COVID-19 appears to cause problems of smell receptors in line with many other respiratory viruses, including previous coronaviruses thought to account for 10–15% of cases of anosmia7,9.
We also identify a combination of symptoms, including anosmia, fatigue, persistent cough and loss of appetite, that together might identify individuals with COVID-19.
A major limitation of the current study is the self-report nature of the data included, which cannot replace physiological assessments of olfactory and gustatory function or nucleotide-based testing for SARS-CoV-2. Both false negative and false positive reports could be included in the dataset12, and because of the way the questions are asked, gustatory and olfactory losses are conflated. Second, at present, we do not know whether anosmia was acquired before or after other COVID-19 symptoms, or during the illness or afterwards. This information could become available as currently healthy users track symptom development over time. As more accurate tests become available, we have the ability to optimize our model. One caveat of our study is that the individuals on which the model was trained are not representative of the general population because performing tests for SARS-CoV-2 is not random. Testing is more likely to be done if an individual develops severe symptoms requiring hospitalization, if an individual has been known to have had contact with people who have tested positive for SARS-CoV-2 infection, in health workers, and if an individual has traveled in an area of high risk of exposure. Therefore, our results may overestimate the number of expected positive cases of SARS-CoV-2 infection. Additionally, volunteers using the app are a self-selected group who might not be fully representative of the general population. Another limitation is the potential effect that mainstream media coverage of loss of smell and taste and COVID-19 might have had on app responses. We found that these reports might have influenced UK responders, for whom there was a temporal trend in the strength of the association. However, there was no such association in the US cohort; therefore, we conclude that regardless of any bias introduced by mainstream media reports, the association between COVID-19 and loss of smell and taste remains strong.
Our work suggests that loss of sense of smell and taste could be included as part of routine screening for COVID-19 and should be added to the symptom list currently developed by the World Health Organization (www.who.int/health-topics/coronavirus). A detailed study on the natural history of broader COVID-19 symptoms, especially according to timing and frequency, will help us to understand the usefulness of symptom tracking and modeling, and to identify probable clusters of infection.
Methods
Study setting and participants
The COVID Symptom Study smartphone-based app (previously known as COVID Symptom Tracker) was developed by Zoe Global, in collaboration with King’s College London and Massachusetts General Hospital, and was launched in the United Kingdom on 24 March 2020 and in the United States on 29 March 2020. After 3 weeks, it had reached 2,618,862 users. It enables the capture of self-reported information related to COVID-19, as described previously10. The survey questions are available in Supplementary Table 1. On first use, the app records self-reported location, age and core health risk factors. With continued use and notifications, participants provide daily updates on symptoms, health care visits, COVID-19 testing results and whether they are self-quarantining or seeking health care, including the level of intervention and related outcomes. Individuals without apparent symptoms are also encouraged to use the app.
Ethics
The King’s College London Ethics Committee approved the ethics for the app, and all users provided consent for non-commercial use. An informal consultation with TwinsUK members over email and social media before the app was launched found that they were overwhelmingly supportive of the project. The US protocol was approved by the Partners Human Research Committee.
Statistical analysis
Data from the app were downloaded to a server and only records where the self-reported characteristics fell within the following ranges were utilized for further analysis: age: 16–90 years (18 years in the United States); height: 110–220 cm; weight: 40–200 kg; BMI: 14–45 kg m−2; and temperature: 35–42 °C. The individuals whose data were included to develop and test the prediction model were those who had completed the report for symptoms in the app and who declared that they had been tested for SARS-CoV-2 by RT-PCR and received the result. Only individuals who answered at least nine of the ten symptom questions, and who answered about loss of smell and taste, were included.
Baseline characteristics are presented as the number (percentage) for categorical variables and the mean (standard deviation) for continuous variables. Multivariate logistic regression adjusting for age, sex and BMI was applied to investigate the correlation between loss of smell and taste and COVID-19 in 15,368 UK users of the symptom tracker app who were also tested in the laboratory for SARS-CoV-2 (6,452 UK individuals tested positive and 9,186 tested negative). The results were replicated in 726 US individuals who tested positive and 2,037 US individuals who tested negative. We then randomly split the UK sample into training and test sets with a ratio of 80:20. In the training set, we performed stepwise logistic regression combining forward and backward algorithms, to identify other symptoms associated with COVID-19 independent of loss of smell and taste. We included in the model ten other symptoms (fever, persistent cough, fatigue, shortness of breath, diarrhea, delirium, skipped meals, abdominal pain, chest pain and hoarse voice) as well as age, sex and BMI, and chose as the best model the one with the lowest Akaike information criterion. We then assessed the performance of the model both in the test set and via tenfold cross-validation in the entire UK sample of 15,638 individuals using the R package cvAUC13. We further validated the prediction model in the US cohort.
For our predictive model, using the R packages pROC and epiR, we further computed the AUC (that is, the overall diagnostic performance of the model), sensitivity (positivity in disease; that is, the proportion of subjects who have the target condition (reference standard positive) and give positive test results) and specificity (negativity in health; that is, the proportion of subjects without a SARS-CoV-2 RT-PCR test who give negative model results).
Finally, we applied the predictive model to the 805,753 individuals reporting symptoms who had not had a SARS-CoV-2 test, to estimate the percentage of individuals reporting some COVID-19 symptoms who were likely to be infected by the virus. The proportion of estimated infections was calculated repeatedly by sampling the dataset (with replacement) to obtain the 95% CIs.
Reporting Summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
Data collected in the app are being shared with other health researchers through the NHS-funded Health Data Research UK (HDRUK)/SAIL consortium, housed in the UK Secure e-Research Platform (UKSeRP) in Swansea. Anonymized data collected by the symptom tracker app can be shared with bonafide researchers via HDRUK, provided the request is made according to their protocols and is in the public interest (see https://healthdatagateway.org/detail/9b604483-9cdc-41b2-b82c-14ee3dd705f6). US investigators are encouraged to coordinate data requests through the COPE Consortium (www.monganinstitute.org/cope-consortium). Data updates can be found at https://covid.joinzoe.com.
Code availability
The app code is publicly available from https://github.com/zoe/covid-tracker-react-native.
References
Whittington, A. M. et al. Coronavirus: rolling out community testing for COVID-19 in the NHS. BMJ Opinion https://blogs.bmj.com/bmj/2020/02/17/coronavirus-rolling-out-community-testing-for-covid-19-in-the-nhs/ (2020).
Rossman, H. et al. A framework for identifying regional outbreak and spread of COVID-19 from one-minute population-wide surveys. Nat. Med. https://doi.org/10.1038/s41591-020-0857-9 (2020).
Gane, S. B., Kelly, C. & Hopkins, C. Isolated sudden onset anosmia in COVID-19 infection. A novel syndrome? Rhinology https://doi.org/10.4193/Rhin20.114 (2020).
Iacobucci, G. Sixty seconds on… anosmia. Br. Med. J. 368, m1202 (2020).
Brann, D. et al. Non-neuronal expression of SARS-CoV-2 entry genes in the olfactory system suggests mechanisms underlying COVID-19-associated anosmia. Preprint at bioRxiv https://www.biorxiv.org/content/10.1101/2020.03.25.009084v3 (2020).
Sungnak, W. et al. SARS-CoV-2 entry factors are highly expressed in nasal epithelial cells together with innate immune genes. Nat. Med. https://doi.org/10.1038/s41591-020-0868-6 (2020).
Hopkiins, C. & Kumar, N. Loss of Sense of Smell as Marker of COVID-19 Infection (ENT UK, 2020).
Eliezer, M. et al. Sudden and complete olfactory loss function as a possible symptom of COVID-19. JAMA Otolaryngol. Head Neck Surg. https://doi.org/10.1001/jamaoto.2020.0832 (2020).
Spinato, G. et al. Alterations in smell or taste in mildly symptomatic outpatients with SARS-CoV-2 infection. J. Am. Med. Assoc. https://doi.org/10.1001/jama.2020.6771 (2020).
Drew, D. et al. Rapid implementation of mobile technology for real-time epidemiology of COVID-19. Science https://science.sciencemag.org/content/early/2020/05/04/science.abc0473/tab-article-info (2020).
Roberts, M. Coronavirus: are loss of smell and taste key symptoms? BBC News (1 April 2020).
Oleszkiewicz, A., Kunkel, F., Larsson, M. & Hummel, T. Consequences of undetected olfactory loss for human chemosensory communication and well-being. Phil. Trans. R. Soc. Lond. B Biol. Sci. 375, 20190265 (2020).
LeDell, E., Petersen, M. & van der Laan, M. Computationally efficient confidence intervals for cross-validated area under the ROC curve estimates. Electron J. Stat. 9, 1583–1607 (2015).
Acknowledgements
We express our sincere thanks to all of the participants who entered data into the app, including study volunteers enrolled in cohorts within the Coronavirus Pandemic Epidemiology (COPE) consortium. We thank the staff of Zoe Global, the Department of Twin Research at King’s College London and the Clinical and Translational Epidemiology Unit at Massachusetts General Hospital for tireless work in contributing to the running of the study and data collection. We thank E. Segal and his laboratory for helpful input. This work was supported by Zoe Global. The Department of Twin Research receives grants from the Wellcome Trust (212904/Z/18/Z) and Medical Research Council/British Heart Foundation Ancestry and Biological Informative Markers for Stratification of Hypertension (AIMHY; MR/M016560/1), and support from the European Union, the Chronic Disease Research Foundation, Zoe Global, the NIHR Clinical Research Facility and the Biomedical Research Centre (based at Guy’s and St Thomas’ NHS Foundation Trust in partnership with King’s College London). C.M. is funded by the Chronic Disease Research Foundation and by the Medical Research Council AIM HY project grant. A.M.V. is supported by the National Institute for Health Research Nottingham Biomedical Research Centre. C.H.S. received an Alzheimer’s Society Junior Fellowship (AS-JF-17-011). S.O. and M.J.C. are funded by the Wellcome/EPSRC Centre for Medical Engineering (WT203148/Z/16/Z) and Wellcome Flagship Programme (WT213038/Z/18/Z). A.T.C. is the Stuart and Suzanne Steele MGH Research Scholar and is a team leader for the Stand Up to Cancer Foundation. A.T.C., L.H.N. and D.A.D. are supported by an Evergrande COVID-19 Response Fund Award through the Massachusetts Consortium on Pathogen Readiness (MassCPR). This work was also supported by the UK Research and Innovation London Medical Imaging & Artificial Intelligence Centre for Value-Based Healthcare.
Author information
Authors and Affiliations
Contributions
C.M., A.M.V., J.W., C.J.S. and T.D.S. conceived of and designed the experiments. C.M., M.B.F., C.H.S., S.G., and A.M.V. analyzed the data. T.V., S.O., M.J.C., R.C.E.B., A.V., J.S.E.S.-M., P.H., M.M., M.F., D.A.D., A.T.C. and L.H.N. contributed reagents, materials and/or analysis tools. C.M. and A.M.V. wrote the manuscript. All authors revised the manuscript.
Corresponding authors
Ethics declarations
Competing interests
T.D.S. and A.M.V. are consultants to Zoe Global. S.G. and J.W. are employees of Zoe Global.
Additional information
Peer review information Jennifer Sargent was the primary editor on this article and managed its editorial process and peer review in collaboration with the rest of the editorial team.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Table 1
Supplementary Table 1
Source data
Source Data Fig. 1
Statistical Source Data
Rights and permissions
About this article
Cite this article
Menni, C., Valdes, A.M., Freidin, M.B. et al. Real-time tracking of self-reported symptoms to predict potential COVID-19. Nat Med 26, 1037–1040 (2020). https://doi.org/10.1038/s41591-020-0916-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-020-0916-2
This article is cited by
-
Acute and persistent symptoms of COVID-19 infection in school-aged children: a retrospective study from China
BMC Public Health (2024)
-
Citizen data sovereignty is key to wearables and wellness data reuse for the common good
npj Digital Medicine (2024)
-
COVID-19 Virus Structural Details: Optical and Electrochemical Detection
Journal of Fluorescence (2024)
-
Incidence of long COVID and associated psychosocial characteristics in a large U.S. city
Social Psychiatry and Psychiatric Epidemiology (2024)
-
A double-blinded randomised controlled trial of vitamin A drops to treat post-viral olfactory loss: study protocol for a proof-of-concept study for vitamin A nasal drops in post-viral olfactory loss (APOLLO)
Pilot and Feasibility Studies (2023)