Abstract
Modulating T cell homeostatic mechanisms with checkpoint blockade can efficiently promote endogenous anti-tumor T cell responses1,2,3,4,5,6,7,8,9,10,11. However, many patients still do not benefit from checkpoint blockade12, highlighting the need for targeting of alternative immune pathways13. Glucocorticoid-induced tumor necrosis factor receptor-related protein (GITR) is an attractive target for immunotherapy, owing to its capacity to promote effector T cell (Teff) functions14,15 and hamper regulatory T cell (Treg) suppression16,17,18,19,20. On the basis of the potent preclinical anti-tumor activity of agonist anti-GITR antibodies, reported by us and others16,21,22, we initiated the first in-human phase 1 trial of GITR agonism with the anti-GITR antibody TRX518 (NCT01239134). Here, we report the safety profile and immune effects of TRX518 monotherapy in patients with advanced cancer and provide mechanistic preclinical evidence to rationally combine GITR agonism with checkpoint blockade in future clinical trials. We demonstrate that TRX518 reduces circulating and intratumoral Treg cells to similar extents, providing an easily assessable biomarker of anti-GITR activity. Despite Treg reductions and increased Teff:Treg ratios, substantial clinical responses were not seen. Similarly, in mice with advanced tumors, GITR agonism was not sufficient to activate cytolytic T cells due to persistent exhaustion. We demonstrate that T cell reinvigoration with PD-1 blockade can overcome resistance of advanced tumors to anti-GITR monotherapy. These findings led us to start investigating TRX518 with PD-1 pathway blockade in patients with advanced refractory tumors (NCT02628574).
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The TCR sequencing data that support the findings are available on the immuneACCESS Analyzer portal, https://clients.adaptivebiotech.com/pub/zappasodi-2019-natmed. All other relevant data are available upon reasonable request.
References
Hodi, F. S. et al. Improved survival with ipilimumab in patients with metastatic melanoma. N. Engl. J. Med. 363, 711–723 (2010).
Larkin, J. et al. Combined nivolumab and ipilimumab or monotherapy in untreated melanoma. N. Engl. J. Med. 373, 23–34 (2015).
Robert, C. et al. Nivolumab in previously untreated melanoma without BRAF mutation. N. Engl. J. Med. 372, 320–330 (2015).
Weber, J. S. et al. Nivolumab versus chemotherapy in patients with advanced melanoma who progressed after anti-CTLA-4 treatment (CheckMate 037): a randomised, controlled, open-label, phase 3 trial. Lancet Oncol. 16, 375–384 (2015).
Wolchok, J. D. et al. Overall survival with combined nivolumab and ipilimumab in advanced melanoma. N. Engl. J. Med. 377, 1345–1356 (2017).
Hellmann, M. D. et al. Nivolumab plus ipilimumab as first-line treatment for advanced non-small-cell lung cancer (CheckMate 012): results of an open-label, phase 1, multicohort study. Lancet Oncol. 18, 31–41 (2017).
Brahmer, J. et al. Nivolumab versus docetaxel in advanced squamous-cell non-small-cell lung cancer. N. Engl. J. Med. 373, 123–135 (2015).
Garon, E. B. et al. Pembrolizumab for the treatment of non-small-cell lung cancer. N. Engl. J. Med. 372, 2018–2028 (2015).
Le, D. T. et al. Mismatch-repair deficiency predicts response of solid tumors to PD-1 blockade. Science 357, 409–413 (2017).
Topalian, S. L. et al. Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N. Engl. J. Med. 366, 2443–2454 (2012).
Hellmann, M. D. et al. Nivolumab plus ipilimumab in lung cancer with a high tumor mutational burden. N. Engl. J. Med. 378, 2093–2104 (2018).
Zappasodi, R., Merghoub, T. & Wolchok, J. D. Emerging concepts for immune checkpoint blockade-based combination therapies. Cancer Cell 33, 581–598 (2018).
Chen, L. & Flies, D. B. Molecular mechanisms of T cell co-stimulation and co-inhibition. Nat. Rev. Immunol. 13, 227–242 (2013).
Kanamaru, F. et al. Costimulation via glucocorticoid-induced TNF receptor in both conventional and CD25+ regulatory CD4+ T cells. J. Immunol. 172, 7306–7314 (2004).
Ronchetti, S. et al. Glucocorticoid-induced TNFR-related protein lowers the threshold of CD28 costimulation in CD8+ T cells. J. Immunol. 179, 5916–5926 (2007).
Ko, K. et al. Treatment of advanced tumors with agonistic anti-GITR mAb and its effects on tumor-infiltrating Foxp3+CD25+CD4+regulatory T cells. J. Exp. Med. 202, 885–891 (2005).
Mitsui, J. et al. Two distinct mechanisms of augmented antitumor activity by modulation of immunostimulatory/inhibitory signals. Clin. Cancer Res. 16, 2781–2791 (2010).
Nishikawa, H. et al. Regulatory T cell-resistant CD8+ T cells induced by glucocorticoid-induced tumor necrosis factor receptor signaling. Cancer Res. 68, 5948–5954 (2008).
Shimizu, J., Yamazaki, S., Takahashi, T., Ishida, Y. & Sakaguchi, S. Stimulation of CD25+CD4+ regulatory T cells through GITR breaks immunological self-tolerance. Nature Immunol. 3, 135–142 (2002).
Valzasina, B. et al. Triggering of OX40 (CD134) on CD4+CD25+ T cells blocks their inhibitory activity: a novel regulatory role for OX40 and its comparison with GITR. Blood 105, 2845–2851 (2005).
Cohen, A. D. et al. Agonist anti-GITR monoclonal antibody induces melanoma tumor immunity in mice by altering regulatory T cell stability and intra-tumor accumulation. PLoS ONE 5, e10436 (2010).
Turk, M. J. et al. Concomitant tumor immunity to a poorly immunogenic melanoma is prevented by regulatory T cells. J. Exp. Med. 200, 771–782 (2004).
Rosenzweig, M. et al. Development of TRX518, an aglycosyl humanized monoclonal antibody (Mab) agonist of huGITR. J. Clin. Oncol. 28, e13028–e13028 (2010).
Schaer, D. A., Murphy, J. T. & Wolchok, J. D. Modulation of GITR for cancer immunotherapy. Curr. Opin. Immunol. 24, 217–224 (2012).
Nocentini, G., Ronchetti, S., Petrillo, M. G. & Riccardi, C. Pharmacological modulation of GITRL/GITR system: therapeutic perspectives. Br. J. Pharmacol. 165, 2089–2099 (2012).
Schaer, D. A. et al. GITR pathway activation abrogates tumor immune suppression through loss of regulatory T cell lineage stability. Cancer Immunol. Res. 1, 320–331 (2013).
Mahne, A. E. et al. Dual roles for regulatory t-cell depletion and costimulatory signaling in agonistic GITR targeting for tumor immunotherapy. Cancer Res. 77, 1108–1118 (2017).
Miyara, M. et al. Functional delineation and differentiation dynamics of human CD4+ T cells expressing the FoxP3 transcription factor. Immunity 30, 899–911 (2009).
Sukumar, S. et al. Characterization of MK-4166, a clinical agonistic antibody that targets human GITR and inhibits the generation and suppressive effects of T regulatory cells. Cancer Res. 77, 4378–4388 (2017).
Tigue, N. J. et al. MEDI1873, a potent, stabilized hexameric agonist of human GITR with regulatory T-cell targeting potential. Oncoimmunology 6, e1280645 (2017).
Gonzalez, A. M. et al. Abstract 3643: INCAGN1876, a unique GITR agonist antibody that facilitates GITR oligomerization. Cancer Res. 77, 3643 (2017).
Lin, Y. C. et al. Activated but not resting regulatory T cells accumulated in tumor microenvironment and correlated with tumor progression in patients with colorectal cancer. Int. J. Cancer 132, 1341–1350 (2013).
Saito, T. et al. Two FOXP3+CD4+ T cell subpopulations distinctly control the prognosis of colorectal cancers. Nat. Med. 22, 679–684 (2016).
He, R. et al. Follicular CXCR5-expressing CD8+ T cells curtail chronic viral infection. Nature 537, 412–416 (2016).
Im, S. J. et al. Defining CD8+ T cells that provide the proliferative burst after PD-1 therapy. Nature 537, 417–421 (2016).
Quezada, S. A., Peggs, K. S., Curran, M. A. & Allison, J. P. CTLA4 blockade and GM-CSF combination immunotherapy alters the intratumor balance of effector and regulatory T cells. J. Clin. Invest. 116, 1935–1945 (2006).
Huang, A. C. et al. T-cell invigoration to tumour burden ratio associated with anti-PD-1 response. Nature 545, 60–65 (2017).
Zappasodi, R. et al. Non-conventional inhibitory CD4+Foxp3−PD-1hi T cells as a biomarker of immune checkpoint blockade activity. Cancer Cell 33, 1017–1032 e1017 (2018).
Wolchok, J. D. et al. Guidelines for the evaluation of immune therapy activity in solid tumors: immune-related response criteria. Clin. Cancer Res. 15, 7412–7420 (2009).
Yarilin, D. et al. Machine-based method for multiplex in situ molecular characterization of tissues by immunofluorescence detection. Sci. Rep. 5, 9534 (2015).
Budhu, S. et al. CD8+ T cell concentration determines their efficiency in killing cognate antigen-expressing syngeneic mammalian cells in vitro and in mouse tissues. J. Exp. Med. 207, 223–235 (2010).
R Core Team. R: a language and environment for statistical computing. R Foundation for Statistical Computing (2013).
Acknowledgements
We thank the Immune Monitoring, Flow Cytometry and Molecular Cytology Core Facilities at Memorial Sloan Kettering Cancer Center for technical assistance. This research was funded in part through the NIH/NCI Cancer Center Support Grant P30 CA008748, NIH/NCI R01 CA056821, the Swim Across America, Ludwig Institute for Cancer Research, Ludwig Center for Cancer Immunotherapy at Memorial Sloan Kettering, Cancer Research Institute, Parker Institute for Cancer Immunotherapy and Breast Cancer Research Foundation. R.Z. was supported by the Parker Institute for Cancer Immunotherapy scholar award.
Author information
Authors and Affiliations
Contributions
R.Z., J.D.W. and T.M. and developed the concept and discussed experiments; R.Z. designed, performed and analyzed experiments, and wrote the manuscript; C.S. coordinated the clinical trial, compiled clinical data and discussed experiments; Y.L. provided assistance with immunofluorescent staining; S.B. contributed to the 3D killing assay design; M.A.-A. archived patient biopsies; C.L., X.Y. and H.Z. provided technical assistance; W.N. discussed experiments; R.Z., J.Q., D.S. and P.W. contributed to flow cytometry analyses of human samples; M.D.H. contibuted immunotherapy naive lung cancer specimens. H.K., V.V., M.A.P. and M.K.C. enrolled, treated and monitored patients.
Corresponding authors
Ethics declarations
Competing interests
R.Z. is inventor on patent applications related to work on GITR, PD-1 and CTLA-4. R.Z. is consultant for Leap Therapeutics. C.S. and W.N. are employed by Leap Therapeutics and report stock option ownership in Leap Therapeutics. P.W. is a consultant for Leap Therapeutics. V.V. reports consultant/advisory roles for Genentech, Bristol Myers Squibb, Merck, AstraZenca, Celgene, Alkermes, Nektar Therapeutics, Reddy labs, Foundation Medicine and Taekeda Oncology, and institutional research grants from Genentech, Bristol Myers Squibb, Merck, Astrazenca, Leap therapeutics, Alkermes and Altor Biosciences. M.D.H. has received research funding from Bristol-Myers Squibb; is paid a consultant to Merck, Bristol-Myers Squibb, AstraZeneca, Genentech/Roche, Janssen, Nektar, Syndax, Mirati, and Shattuck Labs; has received travel support/honoraria from AztraZeneca and BMS; and a patent has been filed by MSK related to the use of tumor mutation burden to predict response to immunotherapy (PCT/US2015/062208), which has received licensing fees from PGDx. M.A.P. is a consultant for Bristol Myers Squibb, Merck, Array BioPharma, Novartis, Incyte, NewLink Genetics and Aduro. M.A.P. reports grants from RGenix, Infinity, Bristol Myers Squibb, Merck, Array BioPharma, AstraZeneca and Novartis, and honoraria from Bristol Myers Squibb and Merck. M.K.C. reports grants from and employment of a family member by Bristol Myers Squibb; personal fees for advisory/consulting role from AstraZeneca/MedImmune, Incyte, Moderna and Merck. T.M. is a consultant for Leap Therapeutics, Immunos Therapeutics and Pfizer, and co-founder of Imvaq therapeutics. T.M. has equity in Imvaq therapeutics. T.M. reports grants from Bristol Myers Squibb, Surface Oncology, Kyn Therapeutics, Infinity Pharmaceuticals, Peregrine Pharmeceuticals, Adaptive Biotechnologies, Leap Therapeutics and Aprea. T.M. is inventor on patent applications related to work on oncolytic viral therapy, alphavirus-based vaccines, neo-antigen modeling, CD40, GITR, OX40, PD-1 and CTLA-4. J.D.W. is a consultant for Adaptive Biotech, Advaxis, Amgen, Apricity, Array BioPharma, Ascentage Pharma, Astellas, Bayer, Beigene, Bristol Myers Squibb, Celgene, Chugai, Elucida, Eli Lilly, F Star, Genentech, Imvaq, Janssen, Kleo Pharma, Linneaus, MedImmune, Merck Pharmaceuticals, Neon Therapuetics, Ono, Polaris Pharma, Polynoma, Psioxus, Puretech, Recepta, Trieza, Sellas Life Sciences, Serametrix, Surface Oncology and Syndax. J.D.W. reports grants from Bristol Myers Squibb, Medimmune, Merck Pharmaceuticals and Genentech. J.D.W. has equity in Potenza Therapeutics, Tizona Pharmaceuticals, Adaptive Biotechnologies, Elucida, Imvaq, Beigene, Trieza and Linneaus. J.D.W. is inventor on patent applications related to work on DNA vaccines in companion animals with cancer, assays for suppressive myeloid cells in blood, oncolytic viral therapy, alphavirus-based vaccines, neo-antigen modeling, CD40, GITR, OX40, PD-1 and CTLA-4. The other authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Peripheral T cell modulation in cancer patients treated with TRX518.
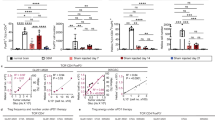
a, Patients with the indicated tumor types enrolled in the seven highest dose cohorts, for whom pre- and post-therapy PBMC samples were analyzed by flow cytometry. Asterisks indicate patients for whom pre- and post-therapy tumor biopsies were also available for immunofluorescent staining. b, Mean ± s.e.m. absolute numbers per ml of blood of the indicated cell subsets (CD3−CD56+ NK cells, CD3+CD8+ T cells, CD3+CD4+Foxp3− Teff, CD3+CD4+Foxp3+ Treg cells, GITR+ Treg cells, CD45RA-Foxp3hiCD4+ effector Treg (eTreg) cells and CD45RA+Foxp3lowCD4+ naive Treg (nTreg) cells) at baseline and at the indicated time points after treatment with TRX518. c, Fold changes relative to baseline of numbers per ml of blood of the same cell subsets as in b. For one patient in cohort 3, lymphocyte counts for the baseline sample used for FACS analysis are not available and it is not possible to calculate fold changes in cell numbers relative to baseline. Data are mean ± s.e.m. in patients grouped by dose cohort for each time point. d, Mean ± s.e.m. fold change in CD3+CD4+Foxp3+ Treg cells (percentage of CD3+CD4+) at the indicated time points after TRX518 relative to baseline in patients with the most prevalent tumor types grouped by dose cohort as reported in a. Treg cells were gated after exclusion of doublets, CD19+, CD14+ and dead cells. Wk, week; hrs, hours; Ca, cancer.
Extended Data Fig. 2 Modulation of GITR+ T cells after TRX518.
a, HEK293 cells transfected with human GITR (HEK293-GITR) were incubated with TRX518 (blue) or the isotype control (ctrl, gray) (10 µg ml−1) and then stained with an AF647-conjugated anti-human Ig alone or together with the flow cytometry (FC) anti-human GITR monoclonal antibody (mAb) eBioAITR (black). In parallel, HER293-GITR were stained with the eBioAITR alone (red). Plot shows results of one representative out of two independent tests. b, Example in 1 of the 37 patients tested (Extended Data Fig. 1a) of GITR staining on circulating Treg cells at baseline and at the indicated time points after TRX518 treatment from a pancreatic cancer patient receiving the highest dose of TRX518 (cohort 9). c, Mean ± s.e.m. fold changes in circulating GITR+CD4+Foxp3− effector T cells (Teff) (percentage of CD3+CD4+Foxp3−) and GITR+CD8+ T cells (percentage of CD3+CD8+) at the indicated time points after TRX518 relative to baseline in patients grouped by dose cohort as detailed in Extended Data Fig. 1a. Cell subsets were gated after exclusion of doublets, CD19+, CD14+ and dead cells. d, Flow cytometry analysis of GITR expression in circulating CD4+ and CD8+ T cell subsets at baseline in patients enrolled in cohort 8 and 9 (naive, CCR7+CD45RA+; CM, central memory, CCR7+CD45RA-; EM, effector memory, CCR7−CD45RA−; TEMRA, terminally differentiated, CCR7−CD45RA+; Teff, CD4+Foxp3−). Representative FACS plots show GITR expression in total circulating CD8+ and CD4+ T cells. Mean ± s.e.m. (n = 10), two-sided paired t-test, **P < 0.01 (Treg cells versus CD8+ naïve, P = 0.0024; Treg cells versus CD8+ CM, P = 0.0042; Treg cells versus CD8+ EM, P = 0.0038; Treg cells versus CD8+ TEMRA, P = 0.0033; Treg cells versus Teff naive, P = 0.0029; Treg cells versus Teff CM, P = 0.0050; Treg cells versus Teff EM, P = 0.0044; Treg cells versus Teff TEMRA, P = 0.0030.
Extended Data Fig. 3 Changes in frequency of GITR+CD4+ T cell subsets and their expression of cytokine receptors after TRX518.
a,b, Frequency of GITR+ Teff (blue) and GITR+ Treg cells (red) (percentages of Teff or Treg cells respectively) (top) and expression of IL7 receptor (CD127) and IL-2 receptor alpha (CD25) on these cell subsets (bottom) in peripheral blood at baseline and after treatment with TRX518 at the indicated time points in cohort 5 (a) and cohort 7 (b) patients. CD127 and CD25 expression in GITR-negative Foxp3−CD4+ T cells (GITRneg Teff, black) is also reported as control. Mean ± s.d. values of PBMC samples tested in duplicate at each time point.
Extended Data Fig. 4 Effects of TRX518 on Foxp3low relative to Foxp3hi GITR+ Treg cells.
a, Representative gating strategy of Foxp3+ Treg cells (Foxp3+CD4+), GITR+ Treg cells (GITR+Foxp3+CD4+), Foxp3lowGITR+ Treg cells and Foxp3hiGITR+ Treg cells. Cell subsets were gated after exclusion of doublets, CD19+, CD14+ and dead cells. b, Fold changes in total Foxp3+GITR+ Treg cells (as in Fig. 1b), Foxp3low and Foxp3hi GITR+ Treg cells (percentage of Treg cells) at the indicated time points after treatment with TRX518 relative to baseline. c, Frequency of Foxp3low and Foxp3hi cells among GITR+ Treg cells at baseline and after treatment with TRX518 at the indicated time points. b,c, Mean ± s.d. values in one representative patient per dose cohort tested in duplicate.
Extended Data Fig. 5 Mechanisms leading to Treg loss after treatment with TRX518.
a, Quantification of Foxp3+CD4+ Treg cells, CD8+ T cells and CD4+Foxp3− Teff in seven-day mixed leukocyte reaction cultures with PBMCs from three different donors treated with 10 µg ml−1 soluble TRX518 or isotype control. Each data point is the mean of two to three technical replicates; paired data are isotype- and TRX518-treated samples from the same donor (two-sided ratio paired t-test; Treg cells absolute number, P = 0.0037; Treg cells percentage of live cells, P = 0.0364; Treg cells percentage of CD4+, P = 0.0200; n.s., not significant). b–d, Standard proliferation/suppression assays with anti-CD3/anti-CD28-stimulated CFSE-labeled autologous CD8+ T cells cultured alone or with CD4+CD25hi Treg cells (1:1 ratio), or CD4+CD25− Teff as control, immunomagnetically purified from donor-derived PBMCs, in the presence of 10 µg ml−1 plate-bound TRX518 or the isotype control. b, Frequency of proliferating activated CFSElow (top) and CD25+ (bottom) CD8+ T cells in each condition after 72 h incubation in one of two independent experiments with different donors are shown (mean ± s.d.; CD8 alone, n = 3; CD8:Teff, n = 3; CD8:Treg cells, n = 2). c, Proportion of CD4+ T cells (Teff or Treg cells) expressing Foxp3 and/or Tbet (left), and proportion of dead Treg cells expressing Foxp3 and/or Tbet (right) in the indicated T cell co-cultures from two biologically independent donor-derived PBMC samples after 72 h incubation (mean ± s.d., n = 3). d, Frequency of dead cells in proliferating (CellTraceViolet (CTV)low) and non-proliferating (CTVhi) Teff and Treg cells in the same cultures as in c. e, Proportion of cells stained with a caspase 3/7 fluorogenic substrate (casp) and/or 7AAD viability dye in monocultures of immunomagnetically purified CD4+CD25hi Treg cells, CD8+ and CD4+CD25− Teff activated with anti-CD3/-CD28 in the presence of 10 µg ml−1 plate-bound TRX518, isotype control (IgG), or a trimeric recombinant human GITRL (rhGITRL) after 16 and 32-hour incubation (mean ± s.d., n = 3 replicates). f, Schematic of the sequence of events leading to Treg loss after GITR stimulation. g, Expression of the anti-apoptotic gene BCL2L1 (BCL-XL) in eTreg cells sorted from two melanoma patients at baseline and at the indicated time points after treatment (mean ± s.d., n = 3). FACS plot depicts the gating strategy to sort viable eTreg cells on the basis of CD25 and CD45RA expression in CD4+ T cells. b–e,g, Two-sided unpaired t-test, *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001. n.a., not assessable.
Extended Data Fig. 6 Representative Treg modulations in peripheral blood and tumor after treatment with TRX518.
a, Flow cytometry plots of Foxp3, CD25 and CD45RA expression in circulating CD14−CD19−dead−CD3+CD4+ T cells from a patient with melanoma (0102-0003, left) and a patient with lung cancer (0002-0004, right) in cohort 7 (2 mg kg−1 TRX518) at baseline (Pre-Tx) and after treatment (Post-Tx) at the same time point as tumor biopsies were collected, as representative examples of patients showing Treg decreases or increases after TRX518 as shown in Fig. 2a. Gates showing frequencies of total Foxp3+ Treg cells and Foxp3hiCD45RA− eTreg cells are depicted. b, Immunofluorescent staining of Foxp3 (pink), CD4 (green) and DAPI (blue) on tumor tissue sections from the same patients and at the same time points shown in a, as representative examples of results shown in Fig. 2b for eight patients (scale bar, 50 µm; 40× original magnification; inset, 60× original magnification). White arrows indicate Foxp3+CD4+ Treg cells.
Extended Data Fig. 7 GITR stimulation cannot overcome T cell exhaustion in the setting of an immunosuppressive advanced tumor microenvironment.
a, B16F10-melanoma-bearing mice were treated with a single administration of the anti-GITR antibody DTA-1 (αGITR) or the matched isotype IgG control at day 4 or day 7 after tumor injection and 6 d later flow cytometry analyses of tumor infiltrating lymphocytes (TILs) were performed. Data are mean ± s.e.m. from one representative experiment out of those averaged in Fig. 3b (two-sided unpaired t-test; αGITR, n = 4; IgG, n = 5). b, B16F10-melanoma-bearing Foxp3-diphtheria-toxin-receptor transgenic mice were treated with diphtheria toxin (DT) to deplete Treg cells 4 d or 7 d after tumor implantation as indicated in the schema. A separate group of mice was injected with PBS as control. Mean ± s.e.m. averaged shortest and longest tumor diameters (n = 5; two-way analysis of variance with Bonferroni correction; P < 0.0001) and frequency of circulating Foxp3+ Treg cells at the indicated time points after treatment (n = 5; unpaired t-test) from one representative of two independent experiments. c, Frequencies, ratios and phenotype of CD8+ TILs and intra-tumor Foxp3+ Treg cells (TM-Treg) from B16F10-melanoma-bearing untreated mice at day 4 or day 7 after tumor implantation. Data are mean ± s.e.m. of five mice per group from one representative of two to four independent experiments depending on the parameter (two-sided unpaired t-test). d, Flow cytometry analysis of granzyme B (GzmB) and PD-1 expression in CD8+ TILs and PD-1 on GzmB+CD8+ TILs from B16F10 tumors harvested 6 d after optimal (αGITR day 4) or suboptimal (αGITR day 7) anti-GITR therapy or control treatments (IgG). Data are mean ± s.e.m. of four or five mice in αGITR- and IgG-treated groups respectively from one representative of two independent experiments (unpaired t-test). *P < 0.05, **P < 0.01, ***P < 0.001, ****P < 0.0001; n.s., not significant.
Extended Data Fig. 8 Modulation of intratumoral T cell clonality.
CD8+ TILs pooled from five mice per group 6 d after αGITR day 4, αGITR day 7, αPD-1 day 7, αGITR + αPD-1 day 7 or isotype control treatments as in Fig. 4c were processed for TCR β-chain CDR3 sequencing analysis (ImmunoSEQ, Adaptive Biotechnology). a,b, Overview of TCR β-chain CDR3 clonality results (a) and frequencies of the indicated top rearrangements (b, productive frequency by amino acid sequences) in each treatment condition. Values for clonality range from 0 (polyclonal samples) to 1 (monoclonal or oligoclonal samples). Productive clonality is calculated by normalizing productive entropy using the total number of unique productive rearrangements and subtracting the result from 1. Accordingly, the higher is the frequency of top rearrangements within a sample the higher is the clonality.
Extended Data Fig. 9 PD-1 expression on human CD8+ TILs during TRX518 treatment.
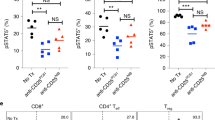
Representative immunofluorescent staining of PD-1 (green), GzmB (red), CD8 (white) and DAPI (blue) on tumor tissue sections from patient 0002–0009 (cohort 8, colon cancer) before (Pre-Tx) and after (Post-Tx) TRX518 treatment (scale bar, 20 µm; 40× original magnification). White arrows indicate PD-1+GzmB+CD8+ T cells (top). Box and whiskers (min to max and median) plots showing frequencies of PD-1-expressing CD8+ TILs and PD-1-expressing GzmB+CD8+ TILs and absolute numbers of PD-1+CD8+ and PD-1+GzmB+CD8+ TILs normalized relative to tumor area (µm2) (Pre-Tx, n = 10 optical fields; Post-Tx, n = 3 optical fields) (bottom).
Extended Data Fig. 10 Model of effects of anti-GITR therapy in combination with PD-1 blockade in the setting of advanced tumors.
Advanced tumors are generally characterized by abundant Treg infiltration and dysfunctional CD8+ T cells (1). Administration of anti-GITR in this setting can reduce intra-tumor Treg cells promoting increases in CD8+ T cell:Treg ratios (2–3). This however may be insufficient to cause effective anti-tumor T cell responses because T cells remain dysfunctional (3). Changes in tumor-infiltrating T cell quality is also key to ensure induction of anti-tumor immunity. This may be achieved by concurrent treatment with PD-1 blockade (4) that, leading to T cell reinvigoration/rejuvenation (5), allows for optimal anti-tumor T cell activation in the absence of Treg cells (6).
Supplementary information
Supplementary Information
Supplementary Tables 1–4
Rights and permissions
About this article
Cite this article
Zappasodi, R., Sirard, C., Li, Y. et al. Rational design of anti-GITR-based combination immunotherapy. Nat Med 25, 759–766 (2019). https://doi.org/10.1038/s41591-019-0420-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-019-0420-8
This article is cited by
-
Evaluation of regulatory T-cells in cancer immunotherapy: therapeutic relevance of immune checkpoint inhibition
Medical Oncology (2024)
-
Therapeutic Strategies in BRAF V600 Wild-Type Cutaneous Melanoma
American Journal of Clinical Dermatology (2024)
-
Expression patterns of novel immunotherapy targets in intermediate- and high-grade lung neuroendocrine neoplasms
Cancer Immunology, Immunotherapy (2024)
-
Predictive biomarkers for the responsiveness of recurrent glioblastomas to activated killer cell immunotherapy
Cell & Bioscience (2023)
-
Immunotherapy targeting different immune compartments in combination with radiation therapy induces regression of resistant tumors
Nature Communications (2023)