Abstract
Tuberculosis (TB) remains the deadliest infectious disease1, and the widely used Bacillus Calmette–Guérin (BCG) vaccine fails to curb the epidemic. An improved vaccination strategy could provide a cost-effective intervention to break the transmission cycle and prevent antimicrobial resistance2,3. Limited knowledge of the host responses critically involved in protective immunity hampers the development of improved TB vaccination regimens. Therefore, assessment of new strategies in preclinical models to select the best candidate vaccines before clinical vaccine testing remains indispensable. We have previously established in rhesus macaques (Macaca mulatta) that pulmonary mucosal BCG delivery reduces TB disease where standard intradermal injection fails4,5. Here, we show that pulmonary BCG prevents infection by using a repeated limiting-dose Mycobacterium tuberculosis challenge model and identify polyfunctional T-helper type 17 (TH17) cells, interleukin-10 and immunoglobulin A as correlates of local protective immunity. These findings warrant further research into mucosal immunization strategies and their translation to clinical application to more effectively prevent the spread of TB.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The datasets generated and analyzed in this study are available from the corresponding authors upon reasonable request. Likewise, upon request biomaterials that are still available from this study could be shared for further research.
References
World Health Organization. Global Tuberculosis Report 2018. (WHO, Geneva, 2018).
Kaufmann, S. H. et al. Progress in tuberculosis vaccine development and host-directed therapies: a state of the art review. Lancet. Respir. Med. 2, 301–320 (2014).
Knight, G. M. et al. Impact and cost-effectiveness of new tuberculosis vaccines in low- and middle-income countries. Proc. Natl Acad. Sci. USA 111, 15520–15525 (2014).
Verreck, F. A. W. et al. Variable BCG efficacy in rhesus populations: pulmonary BCG provides protection where standard intra-dermal vaccination fails. Tuberculosis (Edinb) 104, 46–57 (2017).
Aguilo, N. et al. Pulmonary but not subcutaneous delivery of BCG vaccine confers protection to tuberculosis-susceptible mice by an interleukin 17-dependent mechanism. J. Infect. Dis. 213, 831–839 (2016).
McShane, H. & Williams, A. A review of preclinical animal models utilised for TB vaccine evaluation in the context of recent human efficacy data. Tuberculosis (Edinb) 94, 105–110 (2014).
Hawn, T. R. et al. Tuberculosis vaccines and prevention of infection. Microbiol. Mol. Biol. Rev. 78, 650–671 (2014).
Roederer, M. Parsimonious determination of the optimal infectious dose of a pathogen for nonhuman primate models. PLoS Pathog. 11, e1005100 (2015).
Simmons, J. D. et al. Immunological mechanisms of human resistance to persistent Mycobacterium tuberculosis infection. Nat. Rev. Immunol. 18, 575–589 (2018).
Hessell, A. J. et al. Effective, low-titer antibody protection against low-dose repeated mucosal SHIV challenge in macaques. Nat. Med. 15, 951–954 (2009).
Hudgens, M. G. et al. Power to detect the effects of HIV vaccination in repeated low-dose challenge experiments. J. Infect. Dis. 200, 609–613 (2009).
White, A. G. et al. Analysis of 18FDG PET/CT imaging as a tool for studying Mycobacterium tuberculosis infection and treatment in non-human primates. J. Vis. Exp. 127, e56375 (2017).
Rogers, P. M. A study of the blood monocytes in children with tuberculosis. N. Engl. J. Med. 198, 740–749 (1928).
Naranbhai, V. et al. The association between the ratio of monocytes:lymphocytes at age 3 months and risk of tuberculosis (TB) in the first two years of life. BMC Med. 12, 120 (2014).
Pitcher, C. J. et al. Development and homeostasis of T cell memory in rhesus macaque. J. Immunol. 168, 29–43 (2002).
Moguche, A. O. et al. ICOS and Bcl6-dependent pathways maintain a CD4 T cell population with memory-like properties during tuberculosis. J. Exp. Med. 212, 715–728 (2015).
Kauffman, K. D. et al. Defective positioning in granulomas but not lung-homing limits CD4 T-cell interactions with Mycobacterium tuberculosis-infected macrophages in rhesus macaques. Mucosal Immunol. 11, 462–473 (2018).
Jensen, K. H., Persson, G., Bondgaard, A. L. & Pøhl, M. Development of pulmonary tuberculosis following treatment with anti-PD-1 for non-small cell lung cancer. Acta Oncol. 57, 1127–1128 (2018).
Picchi, H. et al. Infectious complications associated with the use of immune checkpoint inhibitors in oncology: reactivation of tuberculosis after anti PD-1 treatment. Clin. Microbiol. Infect. 24, 216–218 (2018).
Purwar, R. et al. Resident memory T cells (TRM) are abundant in human lung: diversity, function, and antigen specificity. PLoS ONE 6, e16245 (2011).
Kumar, B. V. et al. Human tissue-resident memory T cells are defined by core transcriptional and functional signatures in lymphoid and mucosal sites. Cell Rep. 20, 2921–2934 (2017).
Zimmermann, N. et al. Human isotype-dependent inhibitory antibody responses against Mycobacterium tuberculosis. EMBO Mol. Med. 8, 1325–1339 (2016).
Logan, E. et al. Elevated IgG responses in infants are associated with reduced prevalence of Mycobacterium tuberculosis infection. Front. Immunol. 9, 1529 (2018).
Chen, T. et al. Association of human antibodies to arabinomannan with enhanced mycobacterial opsonophagocytosis and intracellular growth reduction. J. Infect. Dis. 214, 300–310 (2016).
Cruz, A. et al. BCG vaccination-induced long-lasting control of Mycobacterium tuberculosis correlates with the accumulation of a novel population of CD4+IL-17+TNF+IL-2+ T cells. Vaccine 33, 85–91 (2015).
Gopal, R. et al. Unexpected role for IL-17 in protective immunity against hypervirulent Mycobacterium tuberculosis HN878 infection. PLoS Pathog. 10, e1004099 (2014).
Wareham, A. S. et al. Evidence for a role for interleukin-17, Th17 cells and iron homeostasis in protective immunity against tuberculosis in cynomolgus macaques. PLoS ONE 9, e88149 (2014).
Lyadova, I. V. & Panteleev, A. V. Th1 and Th17 cells in tuberculosis: protection, pathology, and biomarkers. Mediators Inflamm. 2015, 854507 (2015).
Shen, H. & Chen, Z. W. The crucial roles of Th17-related cytokines/signal pathways in M. tuberculosis infection. Cell. Mol. Immunol. 15, 216–225 (2018).
Mourik, B. C., Lubberts, E., de Steenwinkel, J. E. M., Ottenhoff, T. H. M. & Leenen, P. J. M. Interactions between type 1 interferons and the Th17 response in tuberculosis: lessons learned from autoimmune diseases. Front. Immunol. 8, 294 (2017).
Scriba, T. J. et al. Sequential inflammatory processes define human progression from M. tuberculosis infection to tuberculosis disease. PLoS Pathog. 13, e1006687 (2017).
McGeachy, M. J. et al. TGF-β and IL-6 drive the production of IL-17 and IL-10 by T cells and restrain TH-17 cell-mediated pathology. Nat. Immunol. 8, 1390–1397 (2007).
Rakshit, S. et al. Circulating Mycobacterium tuberculosis DosR latency antigen-specific, polyfunctional, regulatory IL10+ Th17 CD4 T-cells differentiate latent from active tuberculosis. Sci. Rep. 7, 11948 (2017).
Redford, P. S., Murray, P. J. & O’Garra, A. The role of IL-10 in immune regulation during M. tuberculosis infection. Mucosal Immunol. 4, 261–270 (2011).
Ottenhoff, T. H., Verreck, F. A., Hoeve, M. A. & van de Vosse, E. Control of human host immunity to mycobacteria. Tuberculosis (Edinb) 85, 53–64 (2005).
Hoft, D. F. et al. PO and ID BCG vaccination in humans induce distinct mucosal and systemic immune responses and CD4+ T cell transcriptomal molecular signatures. Mucosal Immunol. 11, 486–495 (2018).
Cadena, A. M. et al. Concurrent infection with Mycobacterium tuberculosis confers robust protection against secondary infection in macaques. PLoS Pathog. 14, e1007305 (2018).
Lee, R. S., Proulx, J. F., Menzies, D. & Behr, M. A. Progression to tuberculosis disease increases with multiple exposures. Eur. Respir. J. 48, 1682–1689 (2016).
Urbanowski, M. E. et al. Repetitive aerosol exposure promotes cavitary tuberculosis and enables screening for targeted inhibitors of extensive lung destruction. J. Infect. Dis. 218, 53–63 (2018).
Lin, P. L. et al. Quantitative comparison of active and latent tuberculosis in the cynomolgus macaque model. Infect. Immun. 77, 4631–4642 (2009).
Talbot, E. A., Williams, D. L. & Frothingham, R. PCR identification of Mycobacterium bovis BCG. J. Clin. Microbiol. 35, 566–569 (1997).
Franken, K. L. et al. Purification of his-tagged proteins by immobilized chelate affinity chromatography: the benefits from the use of organic solvent. Protein Expr. Purif. 18, 95–99 (2000).
Coppola, M. et al. New genome-wide algorithm identifies novel in-vivo expressed Mycobacterium tuberculosis antigens inducing human T-cell responses with classical and unconventional cytokine profiles. Sci. Rep. 6, 37793 (2016).
R: A Language and Environment for Statistical Computing (R Core Team, 2018).
Acknowledgements
We thank G. Koopman and R. Bontrop for reviewing the manuscript. We thank the BPRC animal and veterinary care teams and the clinical laboratory personnel for their excellent expert contributions to this study. We thank K. Franken from the Ottenhoff laboratory at Leiden University Medical Centre for providing us with the recombinant ESAT6–CFP10 fusion protein. We thank F. van Hassel for her assistance with figure editing. The NR-15404 Mycobacterium tuberculosis Erdman K01 (TMC107) reagent was obtained through the NIH Biodefense and Emerging Infections Research Resources Repository, National Institute of Allergy and Infectious Diseases, NIH. The PET–CT infrastructure and TB team management was supported by a grant from the Bill & Melinda Gates Foundation, grant no. OPP1130668. This work was performed under the Tuberculosis Vaccine Initiative (TBVI)-governed TBVAC 2020 network program for advancing TB vaccine candidates, from early discovery through preclinical and into early clinical development, supported by the European Commission under the Horizon 2020 program, grant no. 643381 and a 2017 grant from the Norwegian Agency for Development Coordination (NORAD) to TBVI.
Author information
Authors and Affiliations
Contributions
The experimental strategy was conceived by F.A.W.V. The study design details were conceived by K.D. and F.A.W.V. R.A.W.V. coordinated work with the respective teams of the Animal Science Department. K.G.H. was responsible for overall project management. C.H.M.K. bore the overall responsibility as chair of the Department of Parasitology of the BPRC. I.K. supervised the pathology assessments, and M.A.K supervised the TB imaging and analysis. E.J.R. advised on the statistical analyses. T.H.M.O. gave advice on the immune analyses and reviewed and made suggestions to the manuscript. K.D., C.C.S., R.A.W.V., S.O.H., C.B., and M.P.M.V. were involved in biosampling, processing, and immunological and bacteriological analyses. K.D. and F.A.W.V. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Dose determination and quality control of Mtb Erdman.
a, Kaplan–Meier plot of the IGRA conversion dynamics of an Mtb Erdman dose-finding study in ten rhesus macaques displaying the percentage of IGRA conversion after each dose of Mtb. b, Recovery of CFUs from the Mtb Erdman stock as a percentage of the expected number of CFUs, as determined by plating of serial dilutions from the inoculum preparation process (n = 8 independent experiments, CFUs calculated from n = 3 replicates). Box-whisker plot indicating the 95% CI (box) and range (whiskers), with the line within the box indicating the median value.
Extended Data Fig. 2 Confirmation of BCG take in both vaccinated groups.
a–c, Immune response analysis postvaccination to confirm vaccine take in both standard BCG and pulmonary BCG (BCG.muc) vaccinated animals (n = 8 animals per group, except for BCG.muc at week 8 in b, where n = 7 animals), as demonstrated by antigen-specific IFNγ secretion in PBMCs (a), cell proliferation in PBMCs (b), and cell proliferation in BAL cells (c). In a, IFNγ secretion by ELISpot is plotted as medium control-corrected SPM cells. b,c, Proliferation is shown as the stimulation index, that is, the ratio of incorporated 3H-thymidine by antigen-stimulated cells over culture medium-stimulated cells. d, BCG CFUs cultured from BAL samples taken after BCG vaccination. BCG recovery from BAL is calculated as CFUs in the total sample volume. The horizontal lines indicate the group medians. Statistically significant differences within groups are determined with a two-sided Wilcoxon signed-rank test; differences between groups with a two-sided Mann–Whitney U-test. The color coding per individual is consistent throughout (see also Supplementary Table 1).
Extended Data Fig. 3 Assessment of additional parameters of TB disease manifestation.
a, Single PET–CT images acquired online at week 8 postprimary Mtb challenge and corresponding pathology photographs taken at the end point of animals representing median lung and lymph node pathology within their respective groups with n = 8for each group (lung: Nv.ctrl: R1.8, BCG: R2.8, BCG.muc: R3.6; lymph nodes: Nv.ctrl: R1.8, BCG: R2.3, BCG.muc: R3.5; see also Supplementary Table 1). b, Granulomatous presentation by hematoxylin and eosin-stained histology slides from representatives of n = 8 in each treatment group. The colored dots in the pictures indicate the animal from which the sample originates (R1.1, R2.1, R3.1, R3.5, and R3.2, respectively; see also Supplementary Table 1). c–g, Change in body weight (c) and hematological parameters (d,e) associated with disease after Mtb infection. Change in serum albumin (f) and CRP levels (g) as markers of systemic inflammation. Change calculated as the delta of the preinfection value and each animal’s end point measurement. The lines indicate the group medians (n = 8 animals per group). A two-sided Mann–Whitney U-test adjusted for multiple comparisons was used to determine the significance of group differences. Šidák-Holm-adjusted P values are shown. The color coding per individual is consistent throughout (see also Supplementary Table 1).
Extended Data Fig. 4 Gating strategy applied to T cell analysis.
Gating strategy used to analyze cytokine production and phenotypic marker expression on PPD-stimulated CD4 and CD8 T cells in BAL (shown here) and PBMCs. After doublet exclusion, lymphocytes were gated based on size and granularity. Any anomalies indicative of unstable signal acquisition were excluded using the time parameter. Events from the combined time gates were plotted against the dump channel containing the viability, CD14 and CD20 markers, and subsequently gated as viable, CD14−, and CD20− cells. Cells were further selected for CD45 and CD3 positivity before CD4 and CD8 gating was applied.
Extended Data Fig. 5 Additional flow cytometric characterization of T cell responses after BCG vaccination.
a,b, Ex vivo enumeration of CD3+ T cells per ml recovered BAL in relation to total BAL cellular yield (a) and individual Boolean-gated CD4+ T cell cytokine-producing subsets (b) in response to PPD stimulation, eight weeks post-BCG vaccination. c–d, Percentage of PPD-specific cytokine responses in CD4+ (c) and CD8+ (d) T cells in the periphery, eight weeks post-BCG. e–h, Further characterization of mucosal response signatures. e, Breakdown of mucosal (from left to right) IFNγ-, TNFα-, IL2-, and IL17A-producing CD4+ T cells in BAL per treatment group into the CD28+CD95+ central memory phenotype. f, PD-1 expression of the cytokine-producing CD4+ T cells in BAL samples from the BCG.muc group, after stimulation with PPD. g, Ex vivo CD69 expression on CD4+ T cells from BAL. h, Percentage of granzyme B-expressing CD8+ T cells in BAL. a, Box-whisker plot indicating the 95% CI (box) and range (whiskers), with the line within the box indicating the median value. b–h, The lines indicate the group medians. For all figures n = 8 animals per group. A two-sided Mann–Whitney U-test adjusted for multiple comparisons was used to determine the significance of group differences. Šidák-Holm-adjusted P values are shown. The color coding per individual is consistent throughout (see also Supplementary Table 1).
Extended Data Fig. 6 Additional characterization of T cell responses after RLD Mtb challenge.
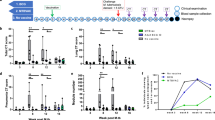
a,b, Ex vivo enumeration of CD3+ T cells per ml recovered BAL in relation to total BAL cellular yield (a), and individual Boolean-gated CD4+ T cell cytokine-producing subsets in response to PPD stimulation (b), eight weeks after the first Mtb inoculation. c–f, Percentage of cytokine-producing T cells in PPD-stimulated CD4+ and CD8+ PBMCs (c) and ESAT-CFP10-stimulated CD4+ (e) and CD8+ PBMCs (f). Samples from three animals (one from the BCG group, two from the BCG.muc group) were not acquired due to a technical error. The ‘+’ symbol indicates either PPD- (c,d) or ESAT6–CFP10-stimulated samples (e,f); the ‘−’ symbol indicates unstimulated culture medium-incubated samples as controls. g–j, Further characterization of mucosal response signatures. g, Breakdown of mucosal (from left to right) IFNγ, TNFα, IL2, and IL17A-producing CD4+ T cells in BAL per treatment group into CD28+CD95+ central memory phenotype. h, PD-1 expression of the cytokine-producing CD4+ T cells in BAL samples from the BCG.muc group after stimulation with PPD. i, Ex vivo CD69 expression on CD4+ T cells from BAL. j, Percentage of granzyme B-expressing CD8+ T cells in BAL. a, Box-whisker plot indicating the 95% CI (box) and range (whiskers), with the line within the box indicating the median value. b–j, The horizontal lines indicate the group medians. For all graphs n = 8 animals per group, unless otherwise indicated. The significance of group differences was determined with a two-sided Mann–Whitney U-test adjusted for multiple comparisons. Šidák-Holm-adjusted P values are shown. The color coding per individual is consistent throughout (see also Supplementary Table 1).
Extended Data Fig. 7 Luminex analysis of additional cytokines.
a–l, Characterization of cytokine responses in the supernatant taken after in vitro stimulation of BAL cells (a–d) or PBMCs (e–l), either eight weeks after vaccination with BCG (week 8) or eight weeks after initial RLD challenge (week 8+). Production of IFNγ (a), TNFα (b), IL2 (c), and IL17A (d) by BAL cells stimulated with PPD or ESAT6–CFP10 fusion protein. Production of IFNγ (e), TNFα (f), IL2 (g), IL17A (h), GM-CSF (i), IL6 (j), granzyme B (k), and IL10 (l) by PBMCs stimulated with PPD or ESAT6–CFP10 fusion protein. All cytokines are plotted as medium control-corrected values. The horizontal lines indicate the group medians, for all graphs n = 8 animals per group, except for (a–d) where n = 7 for the BCG group at week 8 post-BCG. The significance of group differences was determined with a two-sided Mann–Whitney U-test adjusted for multiple comparisons; Šidák-Holm-adjusted P values are reported. Within-group comparisons were tested with a Wilcoxon signed-rank test. The color coding per individual is consistent throughout (see also Supplementary Table 1).
Supplementary information
Supplementary Tables
Supplementary Tables 1–3
Rights and permissions
About this article
Cite this article
Dijkman, K., Sombroek, C.C., Vervenne, R.A.W. et al. Prevention of tuberculosis infection and disease by local BCG in repeatedly exposed rhesus macaques. Nat Med 25, 255–262 (2019). https://doi.org/10.1038/s41591-018-0319-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41591-018-0319-9
This article is cited by
-
BCG vaccination stimulates integrated organ immunity by feedback of the adaptive immune response to imprint prolonged innate antiviral resistance
Nature Immunology (2024)
-
Integrating spatial and single-nucleus transcriptomic data elucidates microglial-specific responses in female cynomolgus macaques with depressive-like behaviors
Nature Neuroscience (2023)
-
A protective, single-visit TB vaccination regimen by co-administration of a subunit vaccine with BCG
npj Vaccines (2023)
-
Key advances in vaccine development for tuberculosis—success and challenges
npj Vaccines (2023)
-
The role of engineered materials in mucosal vaccination strategies
Nature Reviews Materials (2023)