Abstract
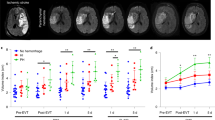
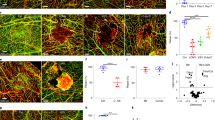
Mild traumatic brain injury (mTBI) can cause meningeal vascular injury and cell death that spreads into the brain parenchyma and triggers local inflammation and recruitment of peripheral immune cells. The factors that dictate meningeal recovery after mTBI are unknown at present. Here we demonstrated that most patients who had experienced mTBI resolved meningeal vascular damage within 2–3 weeks, although injury persisted for months in a subset of patients. To understand the recovery process, we studied a mouse model of mTBI and found extensive meningeal remodeling that was temporally reliant on infiltrating myeloid cells with divergent functions. Inflammatory myelomonocytic cells scavenged dead cells in the lesion core, whereas wound-healing macrophages proliferated along the lesion perimeter and promoted angiogenesis through the clearance of fibrin and production of the matrix metalloproteinase MMP-2. Notably, a secondary injury experienced during the acute inflammatory phase aborted this repair program and enhanced inflammation, but a secondary injury experienced during the wound-healing phase did not. Our findings demonstrate that meningeal vasculature can undergo regeneration after mTBI that is dependent on distinct myeloid cell subsets.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Nguyen, R. et al. The international incidence of traumatic brain injury: a systematic review and meta-analysis. Can. J. Neurol. Sci. 43, 774–785 (2016).
Gruenbaum, S. E., Zlotnik, A., Gruenbaum, B. F., Hersey, D. & Bilotta, F. Pharmacologic neuroprotection for functional outcomes after traumatic brain injury: a systematic review of the clinical literature. CNS Drugs 30, 791–806 (2016).
Corps, K. N., Roth, T. L. & McGavern, D. B. Inflammation and neuroprotection in traumatic brain injury. JAMA Neurol. 72, 355–362 (2015).
Engelhardt, B., Vajkoczy, P. & Weller, R. O. The movers and shapers in immune privilege of the CNS. Nat. Immunol. 18, 123–131 (2017).
Logsdon, A. F. et al. Role of microvascular disruption in brain damage from traumatic brain injury. Compr. Physiol. 5, 1147–1160 (2015).
Shechter, R. et al. Recruitment of beneficial M2 macrophages to injured spinal cord is orchestrated by remote brain choroid plexus. Immunity 38, 555–569 (2013).
Hsieh, C. L. et al. CCR2 deficiency impairs macrophage infiltration and improves cognitive function after traumatic brain injury. J. Neurotrauma 31, 1677–1688 (2014).
Russo, M. V. & McGavern, D. B. Inflammatory neuroprotection following traumatic brain injury. Science 353, 783–785 (2016).
Kigerl, K. A. et al. Identification of two distinct macrophage subsets with divergent effects causing either neurotoxicity or regeneration in the injured mouse spinal cord. J. Neurosci. 29, 13435–13444 (2009).
Hsieh, C. L. et al. Traumatic brain injury induces macrophage subsets in the brain. Eur. J. Immunol. 43, 2010–2022 (2013).
Ransohoff, R. M. & Engelhardt, B. The anatomical and cellular basis of immune surveillance in the central nervous system. Nat. Rev. Immunol. 12, 623–635 (2012).
Kim, J. V., Kang, S. S., Dustin, M. L. & McGavern, D. B. Myelomonocytic cell recruitment causes fatal CNS vascular injury during acute viral meningitis. Nature 457, 191–195 (2009).
Bartholomaus, I. et al. Effector T cell interactions with meningeal vascular structures in nascent autoimmune CNS lesions. Nature 462, 94–98 (2009).
Roth, T. L. et al. Transcranial amelioration of inflammation and cell death after brain injury. Nature 505, 223–228 (2014).
Park, E., Bell, J. D., Siddiq, I. P. & Baker, A. J. An analysis of regional microvascular loss and recovery following two grades of fluid percussion trauma: a role for hypoxia-inducible factors in traumatic brain injury. J. Cereb. Blood Flow Metab. 29, 575–584 (2009).
Gerner, M. Y., Kastenmuller, W., Ifrim, I., Kabat, J. & Germain, R. N. Histo-cytometry: a method for highly multiplex quantitative tissue imaging analysis applied to dendritic cell subset microanatomy in lymph nodes. Immunity 37, 364–376 (2012).
Schledzewski, K. et al. Lymphatic endothelium-specific hyaluronan receptor LYVE-1 is expressed by stabilin-1+, F4/80+, CD11b+ macrophages in malignant tumours and wound healing tissue in vivo and in bone marrow cultures in vitro: implications for the assessment of lymphangiogenesis. J. Pathol. 209, 67–77 (2006).
Cho, C. H. et al. Angiogenic role of LYVE-1-positive macrophages in adipose tissue. Circ. Res. 100, e47–e57 (2007).
Laurens, N., Koolwijk, P. & De Maat, M. Fibrin structure and wound healing. J. Thromb. Haemost. 4, 932–939 (2006).
Rømer, J. et al. Impaired wound healing in mice with a disrupted plasminogen gene. Nat. Med. 2, 287–292 (1996).
Adams, R. A., Passino, M., Sachs, B. D., Nuriel, T. & Akassoglou, K. Fibrin mechanisms and functions in nervous system pathology. Mol. Interv. 4, 163–176 (2004).
Motley, M. P. et al. A CCR2 macrophage endocytic pathway mediates extravascular fibrin clearance in vivo. Blood 127, 1085–1096 (2016).
Hubbard, N. E., Lim, D., Mukutmoni, M., Cai, A. & Erickson, K. L. Expression and regulation of murine macrophage angiopoietin-2. Cell. Immunol. 234, 102–109 (2005).
Jetten, N. et al. Anti-inflammatory M2, but not pro-inflammatory M1 macrophages promote angiogenesis in vivo. Angiogenesis 17, 109–118 (2014).
Krause, T. A., Alex, A. F., Engel, D. R., Kurts, C. & Eter, N. VEGF-production by CCR2-dependent macrophages contributes to laser-induced choroidal neovascularization. PLoS One 9, e94313 (2014).
Rundhaug, J. E. Matrix metalloproteinases and angiogenesis. J. Cell. Mol. Med. 9, 267–285 (2005).
Geissmann, F., Jung, S. & Littman, D. R. Blood monocytes consist of two principal subsets with distinct migratory properties. Immunity 19, 71–82 (2003).
Williams, W. H., Potter, S. & Ryland, H. Mild traumatic brain injury and postconcussion syndrome: a neuropsychological perspective. J. Neurol. Neurosurg. Psychiatry 81, 1116–1122 (2010).
Blixt, J., Svensson, M., Gunnarson, E. & Wanecek, M. Aquaporins and blood-brain barrier permeability in early edema development after traumatic brain injury. Brain Res. 1611, 18–28 (2015).
Tomkins, O. et al. Blood-brain barrier disruption in post-traumatic epilepsy. J. Neurol. Neurosurg. Psychiatry 79, 774–777 (2008).
Ho, K. M., Honeybul, S., Yip, C. B. & Silbert, B. I. Prognostic significance of blood-brain barrier disruption in patients with severe nonpenetrating traumatic brain injury requiring decompressive craniectomy. J. Neurosurg. 121, 674–679 (2014).
Salehi, A., Zhang, J. H. & Obenaus, A. Response of the cerebral vasculature following traumatic brain injury. J. Cereb. Blood Flow Metab. 37, 2320–2339 (2017).
Vannella, K. M. & Wynn, T. A. Mechanisms of organ injury and repair by macrophages. Annu. Rev. Physiol. 79, 593–617 (2017).
Gadani, S. P., Walsh, J. T., Lukens, J. R. & Kipnis, J. Dealing with danger in the CNS: the response of the immune system to injury. Neuron 87, 47–62 (2015).
Kumar, A., Alvarez-Croda, D. M., Stoica, B. A., Faden, A. I. & Loane, D. J. Microglial/macrophage polarization dynamics following traumatic brain injury. J. Neurotrauma 33, 1732–1750 (2016).
Gyoneva, S. et al. Ccr2 deletion dissociates cavity size and tau pathology after mild traumatic brain injury. J. Neuroinflammation 12, 228 (2015).
Morganti, J. M. et al. CCR2 antagonism alters brain macrophage polarization and ameliorates cognitive dysfunction induced by traumatic brain injury. J. Neurosci. 35, 748–760 (2015).
Landsman, L., Varol, C. & Jung, S. Distinct differentiation potential of blood monocyte subsets in the lung. J. Immunol. 178, 2000–2007 (2007).
Yona, S. et al. Fate mapping reveals origins and dynamics of monocytes and tissue macrophages under homeostasis. Immunity 38, 79–91 (2013).
Dal-Secco, D. et al. A dynamic spectrum of monocytes arising from the in situ reprogramming of CCR2+ monocytes at a site of sterile injury. J. Exp. Med. 212, 447–456 (2015).
Nahrendorf, M. et al. The healing myocardium sequentially mobilizes two monocyte subsets with divergent and complementary functions. J. Exp. Med. 204, 3037–3047 (2007).
Olingy, C. E. et al. Non-classical monocytes are biased progenitors of wound healing macrophages during soft tissue injury. Sci. Rep. 7, 447 (2017).
Xiong, Y., Mahmood, A. & Chopp, M. Animal models of traumatic brain injury. Nat. Rev. Neurosci. 14, 128–142 (2013).
Sköld, M. K., Gertten, C. V., Sandbergnordqvist, A.-C., Mathiesen, T. & Holmin, S. VEGF and VEGF receptor expression after experimental brain contusion in rat. J. Neurotrauma 22, 353–367 (2005).
Frautschy, S. A., Walicke, P. A. & Baird, A. Localization of basic fibroblast growth factor and its mRNA after CNS injury. Brain Res. 553, 291–299 (1991).
Davalos, D. et al. Fibrinogen-induced perivascular microglial clustering is required for the development of axonal damage in neuroinflammation. Nat. Commun. 3, 1227 (2012).
Mantovani, A., Biswas, S. K., Galdiero, M. R., Sica, A. & Locati, M. Macrophage plasticity and polarization in tissue repair and remodelling. J. Pathol. 229, 176–185 (2013).
Minutti, C. M., Knipper, J. A., Allen, J. E. & Zaiss, D. M. Tissue-specific contribution of macrophages to wound healing. in Seminars in Cell & Developmental Biology (eds Sweet, M. & Mansell, A.) 3–11 (Elsevier, New York, 2017).
Elkington, P. T., Green, J. A. & Friedland, J. S. Analysis of matrix metalloproteinase secretion by macrophages. Methods Mol. Biol. 531, 253–265 (2009).
McKee, A. C. et al. Chronic traumatic encephalopathy in athletes: progressive tauopathy after repetitive head injury. J. Neuropathol. Exp. Neurol. 68, 709–735 (2009).
Bryan, C. J. & Clemans, T. A. Repetitive traumatic brain injury, psychological symptoms, and suicide risk in a clinical sample of deployed military personnel. JAMA Psychiatry 70, 686–691 (2013).
Shitaka, Y. et al. Repetitive closed-skull traumatic brain injury in mice causes persistent multifocal axonal injury and microglial reactivity. J. Neuropathol. Exp. Neurol. 70, 551–567 (2011).
Mouzon, B. et al. Repetitive mild traumatic brain injury in a mouse model produces learning and memory deficits accompanied by histological changes. J. Neurotrauma 29, 2761–2773 (2012).
Weavers, H. et al. Systems analysis of the dynamic inflammatory response to tissue damage reveals spatiotemporal properties of the wound attractant gradient. Curr. Biol. 26, 1975–1989 (2016).
Zetterberg, H. & Blennow, K. Fluid biomarkers for mild traumatic brain injury and related conditions. Nat. Rev. Neurol. 12, 563–574 (2016).
Faust, N., Varas, F., Kelly, L. M., Heck, S. & Graf, T. Insertion of enhanced green fluorescent protein into the lysozyme gene creates mice with green fluorescent granulocytes and macrophages. Blood 96, 719–726 (2000).
Manglani, M. & McGavern, D.B. Intravital imaging of neuroimmune interactions through a thinned skull. Curr. Protoc. Immunol. 120, 24.2.1–24.2.12 (2018).
Kleinfeld, D., Mitra, P. P., Helmchen, F. & Denk, W. Fluctuations and stimulus-induced changes in blood flow observed in individual capillaries in layers 2 through 4 of rat neocortex. Proc. Natl Acad. Sci. USA 95, 15741–15746 (1998).
Acknowledgements
Supported by the US National Institutes of Health (NIH), the National Institute of Neurological Disorders and Stroke (NINDS) and the Center for Neuroscience and Regenerative Medicine (CNRM) at the Uniformed Services University of the Health Sciences, a collaborative effort among NIH, the Department of Defense, and Walter Reed National Military Medical Center to develop innovative approaches for brain injury diagnosis and recovery.
Author information
Authors and Affiliations
Contributions
M.V.R. designed and executed the animal studies, analyzed data and wrote the manuscript; L.L.L. designed the human studies and analyzed the resultant data; and D.B.M. conceived of the project, designed and interpreted the animal studies and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Acute neuroinflammation subsides within one week after mTBI.
Gene expression of inflammatory genes (Ccl2, Ccl12, Cxcl1, Cxcl10, Il1a, Il1b) in naïve mice vs. mTBI mice at 6 h, 24 h, 4 days and 7 days post-injury. Gene expression is relative to Gapdh and Tbp expression and represented as a fold change over the mean of the naïve group. Each symbol represents a single mouse. Data represented as mean ± s.e.m. NS, not significant *P ≤ 0.05, **P ≤ 0.01, ****P ≤ 0.0001 (one-way ANOVA with Tukey’s multiple comparisons test). Data are pooled from two independent experiments normalized to the naive group mean with four mice per group.
Supplementary Figure 2 Methodology to quantify blood flow.
(a,b) To quantify cerebral blood flow, mice were injected intravenously ~30 min prior to imaging with 20 μl of 0.5 μm polychromatic red fluorescent microspheres and 10 μl of Qtracker 655. The fluorescent microspheres were used to quantify blood flow velocities, and the Qtracker 655 was used to visualize blood vessels. (a) The representative two-photon image shows the Qtracker 665 signal (gray scale) in meningeal blood vessels captured through a thinned skull window. The area denoted with a red box is enlarged (b). Each vessel was imaged at a 6.3× zoom for clarity and consistency between individual mice/vessels. The midline of each vessel was chosen as the measurement plane for a continuous xt line scan (green line in b). (c) A representative image from a line scan shows individual lines (55 μm in length) compiled vertically over a 512-millisecond time interval. The movement of individual fluorescent microspheres (red) were used to calculate blood flow velocities. The microspheres appeared as bright red streaks moving diagonally across the line scan image (white box). (d) An enlarged image from c depicts a single microsphere as it traveled across the line scanned area. Blood flow velocity was calculated as the slope of this line, which was defined as the change in distance (x) divided by the change in time (t). Measurements were made in Leia LASX software using the line scan images. Images representative of two independent experiments with four mice per group.
Supplementary Figure 3 Example of the histo-cytometry approach used to analyze the lesion core and peri-lesion distribution of myeloid cells.
(a) A representative image from a meningeal whole mount shows the distribution of different myeloid cells within and surrounding the mTBI lesion 4 days post-injury. The meninges were stained with CD206 (green), CD11b (red) and i.v. tomato lectin (white). (b) Representative image of (a) with cell surfaces generated in Imaris software to define cells within the lesion core (red) or peri-lesion (green) areas. Lectin is shown in white. (c–e) Representative histo-cytometry plots generated in FlowJo depict the fluorescent intensities of the denoted surface markers. Myeloid cells were first gated on CD11b (c) and determined to be CD206 positive or negative (d). We then determined the anatomical position (lesion core vs. peri-lesion) of CD206+ and CD206– cells (e). Scale bar (a,b), 200 μm. Images and plots representative of two independent experiments with four mice per group.
Supplementary Figure 4 Majority of peri-lesion wound healing macrophages also express Lyve-1.
(a) Representative meningeal whole mount images of myeloid cell subsets within and surrounding the mTBI lesion 4 days post-injury. Meninges were stained with CD11b (red), CD206 (green), Lyve-1 (blue) and tomato lectin i.v. (white). (b,c) Quantification of Lyve-1 expression on CD206+ cells (b) and the anatomical positioning of Lyve-1+ cells (c) at the mTBI lesion 4 days post-injury. Each symbol represents a single mouse. Data represented as mean ± s.e.m. Scale bar (a), 200 μm. ****P ≤ 0.0001 (two-tailed Student’s t-test). Data are representative of three independent experiments with four mice per group.
Supplementary Figure 5 Peripheral immune cell depletion efficiencies in blood.
(a) Quantification of blood neutrophils, Ly6Chi monocytes, and Ly6Clo monocytes in isotype vs. anti-Gr-1 treated mice 4 days post-injury. anti-Gr-1 was injected i.p. daily beginning 24 h before mTBI (n = 3-4 mice per group). (b-d) Quantification of blood neutrophils, Ly6Chi monocytes, and Ly6Clo monocytes in control vs. single clodronate injected mice on the day of the mTBI (time point 0), 2 days, 5 days and 7 days post-injury. A single clodronate injection was given i.v. 24 h before mTBI (n = 4 mice per group). For all experiments, neutrophils were gated on CD11b+Ly6G+ and monocytes were gated on CD11b+CD115+Ly6G–Ly6C+/–. Each symbol represents a single mouse. Data represented as mean ± s.e.m. NS, not significant *P ≤ 0.05, **P ≤ 0.01, ***P ≤ 0.001, ****P ≤ 0.0001 (two-tailed Student’s t-test). Data are representative of one independent experiment with three to four mice per group (a, b–d).
Supplementary Figure 6 Macrophages acquire fibrinogen after mTBI.
(a, b) Representative meningeal whole mount images of the uninjured vs. injured meninges at 4 days post-injury injected depict the distribution of fluorescently-conjugated fibrinogen (green) and CD206+ macrophages (red). Fluorescent fibrinogen was injected i.v. 30 min before mTBI. Insets depict zoomed areas (denoted with white boxes) from the original image. Note that many CD206+ macrophages are positive for fibrinogen (and appear yellow) in the injured vs. uninjured meninges. Scale bars (a,b), 150 μm (left images) or 30 μm (right images). Images are representative of one independent experiment with four mice per group.
Supplementary Figure 7 MMP inhibition does not alter the accumulation of macrophages in meningeal lesions.
(a) Representative meningeal whole mount images of vehicle vs. SB-3CT treated mice 7 days post-injury depict the distribution of CD206+ macrophages (red) in relation to i.v. tomato lectin-labeled blood vessels (green). (b) Quantification of CD206+ macrophages at the lesion site as shown in (a) (n = 6; three independent experiments). Each symbol represents a single mouse. Data represented as mean ± s.e.m. NS, not significant (two-tailed Student’s t-test). Scale bar (a), 150 μm. Data are representative of three independent experiments with six mice per group (a–b).
Supplementary Figure 8 Blockade of new neutrophils and inflammatory monocytes does not improve re-vascularization after reinjury.
(a) Representative meningeal whole mount images of day 1 reinjured control vs. anti-Gr-1 treated animals 7 days post primary injury. Anti-Gr-1 was administered i.p. 3 h before reinjury. Meninges were stained laminin (red) and tomato lectin i.v. (green). (b) Quantification of lesioned area in 1 day reinjured control or anti-Gr-1 treated mice 7 days post primary injury. Each symbol represents a single mouse. Data represented as mean ± s.e.m. NS, not significant (two-tailed Student’s t-test). Scale bar (a), 200 μm. Data are pooled from four independent experiments and normalized to the control group mean. Each experiment contained four mice per group (a–b).
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1-8 and Supplementary Table 1
Supplementary Table 2
Complete raw gene expression data used to generate the graph shown in Supplementary Fig. 1
Supplementary Table 3
Complete raw gene expression data used to generate the graph shown in Fig. 6d
Supplementary Table 4
Complete raw gene expression data used to generate the graph shown in Figure 6e
Supplementary Video 1 Dynamics of meningeal vascular pathology and cell death following mTBI.
Representative time-lapse imaging of 3D reconstructions captured through the thinned skull show the rapid kinetics of vascular pathology and cell death in the meninges immediately following mTBI. Evans blue and NucGreen vital dye were injected intravenously just prior to imaging to visualize blood flow and cell death dynamics, respectively. Part 1. This time lapse demonstrates a massive amount of meningeal cell death (green) in areas of significant Evans blue leakage (red) into the extravascular space. Part 2. A time lapse capturing the relationship between meningeal vascular occlusion and cell death in the surrounding tissue. Note the spread of cell death (green) around a meningeal blood vessel that occludes and ceases to flow Evans blue (pink). Movies are representative of imaging from three mice.
Supplementary Video 2 Rapid deposition of fibrinogen in platelets following mTBI.
Representative 3D time-lapse imaging was captured through the thinned skull window of mice immediately following mTBI. Alexa Fluor488-conjugated fibrinogen, Evans blue, or anti-CD41-PE antibodies were injected 30 min prior to imaging. Part 1. mTBI induces immediate deposition of fibrinogen (green) on damaged and leaking blood vessels. Fibrinogen was also observed leaking out of meningeal blood vessels into the extravascular space (denoted with white arrowheads). Evans blue is shown in red. Part 2. Platelets (red) and fibrinogen (green) co-localize on damaged meningeal blood vessels. Part 3. Damaged vessels labeled with platelets (red) resided primarily in the meninges and were above the glial limitans. The glial limitans was identified by the presence of honeycombing Cx3cr1gfp/+ microglia (green) as described previously (3). Movies are representative of imaging from three mice.
Supplementary Video 3 >Meningeal myeloid cell dynamics over the course of one week post-injury.
Representative time-lapse imaging of 3D reconstructions from Cx3cr1gfp/+Ccr2rfp/+ double reporter mice showing a dynamic myeloid response in the meninges over the first 7 days following mTBI. Immediately following injury, microglia (green) migrate to the glia limitans where they assume distinct morphologies such as ‘jellyfish’ or ‘honeycomb’ microglia. At 24 h post-injury, peripheral monocytes (green, red) invade the meninges and swarm within the lesion. The monocyte response is followed by differentiated macrophages (green, green + red) accumulating within the lesion from 4–7 days post-injury. Movies are representative of imaging from three mice per time-point.
Supplementary Video 4 Dynamics of macrophages positioned around lesion perimeter 4 days post-mTBI.
Representative time-lapse imaging from Cx3cr1gfp/+ mice show the dynamics of macrophages (green) in the peri-lesion area 4 days after mTBI. The core of the lesion is denoted with white asterisks. Blood vessels (red) were visualized by i.v. injection of Alexa Fluor 647-conjugated tomato lectin prior to imaging. Movie is representative of imaging from three mice.
Supplementary Video 5 Neutrophils and monocytes swarm the meninges after mTBI and interact with dead cells.
Representative time-lapse imaging of 3D reconstructions from LysMgfp/+ mice showing both neutrophils and monocytes (green) swarming within the meninges, attracted to and interacting with dead cells (red) 24 h post-mTBI. Dead cells were labeled by incubating with propidium iodide transcranially for 1 h prior to imaging. Movie is representative of imaging from four mice.
Supplementary Video 6 Macrophages acquire dead cells and extravascular fibrinogen.
Representative time-lapse imaging of 3D reconstructions from Cx3cr1gfp/+ mice demonstrate macrophages (green) acquiring dead cells (red) at 2 days post-injury (Part 1) and with extravascular fibrinogen (purple) in their cell bodies at 4 days post-injury (Part 2). An enlarged time lapse in Part 1 (denoted with a white box) shows a single macrophage extending a process towards and engulfing a dead cell (red; white arrowhead). Many active macrophages contain fibrinogen inside their cell bodies as shown in Part 2. Dead cells were labeled by incubating with propidium iodide transcranially for 1 h prior to imaging. Alexa Fluor 647-conjugated fibrinogen was injected 30 min prior to mTBI. Movies are representative of from imaging three mice (Part 1) or four mice (Part 2).
Supplementary Video 7 Neutrophil recruitment to the meninges following a primary or secondary meningeal re-injury.
Representative time-lapses demonstrate the kinetics of neutrophil (green) recruitment to the meninges following an initial mTBI, re-injury at 24 h, or re-injury at 4 days post-mTBI. In the first time-lapse representing a primary mTBI, a few neutrophils are observed entering the meninges toward the end of the 2-h film. This is because neutrophils typically require 2-3 h to enter an initial mTBI lesion. A similar response was observed in the meninges were re-injured at 4 days. By contrast, an incredibly rapid neutrophil response was seen when the meninges were re-injured at 24 h. A significant number of neutrophils enter the lesion within 20 min. Neutrophils were visualized by i.v. injection of Alexa Fluor 647-conjugated anti-Ly6G 30 min prior to injury. Movies are representative of imaging from five to seven mice at each time-point.
Rights and permissions
About this article
Cite this article
Russo, M.V., Latour, L.L. & McGavern, D.B. Distinct myeloid cell subsets promote meningeal remodeling and vascular repair after mild traumatic brain injury. Nat Immunol 19, 442–452 (2018). https://doi.org/10.1038/s41590-018-0086-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41590-018-0086-2
This article is cited by
-
Border-associated macrophages in the central nervous system
Journal of Neuroinflammation (2024)
-
Blood–brain borders: a proposal to address limitations of historical blood–brain barrier terminology
Fluids and Barriers of the CNS (2024)
-
Nervous System Response to Neurotrauma: A Narrative Review of Cerebrovascular and Cellular Changes After Neurotrauma
Journal of Molecular Neuroscience (2024)
-
The role of peripheral inflammatory insults in Alzheimer’s disease: a review and research roadmap
Molecular Neurodegeneration (2023)
-
Chronic social defeat alters brain vascular-associated cell gene expression patterns leading to vascular dysfunction and immune system activation
Journal of Neuroinflammation (2023)