Abstract
In multiple cancer types, high tumor mutational burden (TMB) is associated with longer survival after treatment with immune checkpoint inhibitors (ICIs). The association of TMB with survival outside of the immunotherapy context is poorly understood. We analyzed 10,233 patients (80% non-ICI-treated, 20% ICI-treated) with 17 cancer types before/without ICI treatment or after ICI treatment. In non-ICI-treated patients, higher TMB (higher percentile within cancer type) was not associated with better prognosis; in fact, in many cancer types, higher TMB was associated with poorer survival, in contrast to ICI-treated patients in whom higher TMB was associated with longer survival.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
All data needed to replicate the analyses in this study, including de-identified clinical data, TMB values, MSI status and DNA damage repair gene mutations have been deposited with Zenodo (https://doi.org/10.5281/zenodo.4074184; https://zenodo.org/record/4074184#.X5G-I-i6M2w). The data can also be accessed and analyzed online with the IOExplorer data portal (https://ioexplorer.net/valero).The original sequencing reads cannot be publicly deposited due to privacy restrictions since sequencing was performed as part of clinical care.
References
Samstein, R. M. et al. Tumor mutational load predicts survival after immunotherapy across multiple cancer types. Nat. Genet. 51, 202–206 (2019).
Rizvi, N. A. et al. Cancer immunology. Mutational landscape determines sensitivity to PD-1 blockade in non-small cell lung cancer. Science 348, 124–128 (2015).
Snyder, A. et al. Genetic basis for clinical response to CTLA-4 blockade in melanoma. N. Engl. J. Med. 371, 2189–2199 (2014).
Van Allen, E. M. et al. Genomic correlates of response to CTLA-4 blockade in metastatic melanoma. Science 350, 207–211 (2015).
Le, D. T. et al. Mismatch repair deficiency predicts response of solid tumors to PD-1 blockade. Science 357, 409–413 (2017).
Ghorani, E. et al. The T cell differentiation landscape is shaped by tumour mutations in lung cancer. Nat. Cancer 1, 546–561 (2020).
Hwang, W. L. et al. Clinical impact of tumor mutational burden in neuroblastoma. J. Natl. Cancer Inst. 111, 695–699 (2019).
Owada-Ozaki, Y. et al. Prognostic impact of tumor mutation burden in patients with completely resected non-small cell lung cancer: brief report. J. Thorac. Oncol. 13, 1217–1221 (2018).
Eder, T. et al. Interference of tumour mutational burden with outcome of patients with head and neck cancer treated with definitive chemoradiation: a multicentre retrospective study of the German Cancer Consortium Radiation Oncology Group. Eur. J. Cancer 116, 67–76 (2019).
Fernandez, E. M. et al. Cancer-specific thresholds adjust for whole exome sequencing-based tumor mutational burden distribution. JCO Precis. Oncol. 3, PO.18.00400 (2019).
Wu, H.-X. et al. Tumor mutational and indel burden: a systematic pan-cancer evaluation as prognostic biomarkers. Ann. Transl. Med. 7, 640 (2019).
Cheng, D. T. et al. Memorial Sloan Kettering-Integrated Mutation Profiling of Actionable Cancer Targets (MSK-IMPACT): a hybridization capture-based next-generation sequencing clinical assay for solid tumor molecular oncology. J. Mol. Diagn. 17, 251–264 (2015).
Popat, S., Hubner, R. & Houlston, R. S. Systematic review of microsatellite instability and colorectal cancer prognosis. J. Clin. Oncol. 23, 609–618 (2005).
Yang, G., Zheng, R.-Y. & Jin, Z.-S. Correlations between microsatellite instability and the biological behaviour of tumours. J. Cancer Res. Clin. Oncol. 145, 2891–2899 (2019).
Teo, M. Y. et al. DNA damage response and repair gene alterations are associated with improved survival in patients with platinum-treated advanced urothelial carcinoma. Clin. Cancer Res. 23, 3610–3618 (2017).
Hause, R. J., Pritchard, C. C., Shendure, J. & Salipante, S. J. Classification and characterization of microsatellite instability across 18 cancer types. Nat. Med. 22, 1342–1350 (2016).
Middha, S. et al. Reliable pan-cancer microsatellite instability assessment by using targeted next-generation sequencing data. JCO Precis. Oncol. 1, PO.17.0008 (2017).
Wang, J. et al. Clonal evolution of glioblastoma under therapy. Nat. Genet. 48, 768–776 (2016).
Jonna, S. et al. Impact of prior chemotherapy or radiation therapy on tumor mutation burden in NSCLC. J. Clin. Oncol. 37, 2627 (2019).
Pich, O. et al. The mutational footprints of cancer therapies. Nat. Genet. 51, 1732–1740 (2019).
Hsiehchen, D. et al. DNA repair gene mutations as predictors of immune checkpoint inhibitor response beyond tumor mutation burden. Cell Rep. Med. 1, 100034 (2020).
Zehir, A. et al. Mutational landscape of metastatic cancer revealed from prospective clinical sequencing of 10,000 patients. Nat. Med. 23, 703–713 (2017).
Bozic, I. et al. Evolutionary dynamics of cancer in response to targeted combination therapy. eLife 2, e00747 (2013).
Morris, L. G. T. et al. Pan-cancer analysis of intratumor heterogeneity as a prognostic determinant of survival. Oncotarget 7, 10051–10063 (2016).
Andor, N. et al. Pan-cancer analysis of the extent and consequences of intratumor heterogeneity. Nat. Med. 22, 105–113 (2016).
Nowak, M. A. et al. The role of chromosomal instability in tumor initiation. Proc. Natl Acad. Sci. USA 99, 16226–16231 (2002).
Thommen, D. S. et al. Progression of lung cancer is associated with increased dysfunction of T cells defined by coexpression of multiple inhibitory receptors. Cancer Immunol. Res. 3, 1344–1355 (2015).
Stensrud, M. J. & Hernán, M. A. Why test for proportional hazards? JAMA 323, 1401–1402 (2020).
Acknowledgements
We thank our patients and their families for their bravery and their support of cancer research. We thank members of the Molecular Diagnostics Service in the Department of Pathology and the Marie-Josée and Henry R. Kravis Center for Molecular Oncology and members of the Morris and Chan Laboratories for helpful discussions. We thank J. Novak for editing the manuscript. This study was funded by Fundación Alfonso Martín Escudero (to C.V.), National Institutes of Health (NIH) grant nos. K08 DE024774 and R01 DE027738, the Jayme and Peter Flowers Fund, Sebastian Nativo Fund, Catherine and Frederick Adler Chair for Junior Faculty and Cycle for Survival (to L.G.T.M.), Pershing Square Sohn Cancer Research Foundation, PaineWebber Chair, Stand Up To Cancer, Starr Cancer Consortium, NIH grant nos. R01 CA205426 and R35 CA232097 (to T.A.C.) and NIH/National Cancer Institute Cancer Center Support Grant no. P30 CA008748.
Author information
Authors and Affiliations
Contributions
C.V., M. Lee, D.H., T.A.C., V.E.S., L.G.T.M. conceived and designed the study. C.V., M. Lee, D.H., M.A.P., A.N.S., G.P., V.P.B., J.J.S., A.M.C., K.C.L.R., D.W.K., J.W., Z.N., N.P., R.M.S., S.R., I.G., R.J.W., A.A.H., M.F.B., A.Z., D.B.S., M. Ladanyi and N.R. acquired, analyzed and interpreted the data. C.V. and L.G.T.M. drafted the manuscript. All authors carried out a critical revision of the manuscript for important intellectual content. C.V., V.E.S. and L.G.T.M. carried out the statistical analysis. T.A.C. and L.G.T.M. obtained the funding. D.H. and D.W.K. provided administrative, technical or material support. T.A.C., V.E.S. and L.G.T.M. supervised the study.
Corresponding authors
Ethics declarations
Competing interests
D.H. receives funding from AstraZeneca. M.A.P. reports consulting fees from BMS, Merck, Array BioPharma, Novartis, Incyte, NewLink Genetics and Aduro, honoraria from BMS and Merck and research support from Rgenix, Infinity, BMS, Merck, Array BioPharma, Novartis and AstraZeneca. A.N.S. reports advisory board positions with BMS, Immunocore and Castle Biosciences and institutional research support from BMS, Immunocore and Xcovery. V.P.B. is a recipient of an immuno-oncology translational research grant from Bristol Myers Squibb and is an inventor on a patent application related to work on neoantigen modeling. J.J.S. has received travel support from Intuitive Surgical for fellow education and has served as a clinical advisor to Guardant Health. A.M.C. reports an advisory board position with SpringWorks Therapeutics. A.Z. reports honoraria from Illumina. N.R. reports research support from Pfizer and BMS and consulting fees from Repare Therapeutics, Mirati Therapeutics and Illumina. T.A.C. acknowledges grant funding from Bristol Myers Squibb, AstraZeneca, Illumina, Pfizer, AN2H and Eisai, has served as an advisor for Bristol Myers Squibb, Illumina, Eisai and AN2H, holds equity in AN2H and is a cofounder of Gritstone Oncology and holds equity in the company. L.G.T.M. reports laboratory research funding from Illumina and AstraZeneca. R.M.S., T.A.C. and L.G.T.M. are inventors on a patent held by the Memorial Sloan Kettering Cancer Center related to the use of TMB in cancer immunotherapy. The remaining authors declare no competing interests.
Additional information
Peer review information Nature Genetics thanks Douglas Johnson, J. Jack Lee and the other, anonymous, reviewer(s) for their contribution to the peer review of this work. Peer reviewer reports are available.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
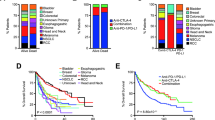
Extended Data Fig. 1 Association between tumor mutational burden (TMB) and overall survival (OS) with and without immune checkpoint inhibitor (ICI) treatment in the entire cohort (10,233 patients analyzed).
The forest plots compare the hazard ratios for OS for patients with TMB-high versus TMB-low tumors (using top 20th percentile within cancer type as cutoff) for patients who never received ICI treatment or before receiving ICI (black), and after receiving ICI (red). Error bars represent the 95% confidence intervals (95% CI). Cox proportional hazards regression was used with overall survival as the endpoint. All the hypothesis tests were 2-sided. No adjustments for multiple comparisons were made. Abbreviations: NSCLC, Non–small cell lung cancer; CNS, central nervous system; SCLC, small cell lung cancer.
Extended Data Fig. 2 Proportional hazards (PH) assumption testing using Schoenfeld residuals.
Abbreviations: TMB, Tumor mutational burden; ICI, immune checkpoint inhibitors.
Supplementary information
Rights and permissions
About this article
Cite this article
Valero, C., Lee, M., Hoen, D. et al. The association between tumor mutational burden and prognosis is dependent on treatment context. Nat Genet 53, 11–15 (2021). https://doi.org/10.1038/s41588-020-00752-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41588-020-00752-4
This article is cited by
-
Potential crosstalk between SPP1 + TAMs and CD8 + exhausted T cells promotes an immunosuppressive environment in gastric metastatic cancer
Journal of Translational Medicine (2024)
-
Cuprotosis clusters predict prognosis and immunotherapy response in low-grade glioma
Apoptosis (2024)
-
Strategies to Improve Drug Delivery Across the Blood–Brain Barrier for Glioblastoma
Current Neurology and Neuroscience Reports (2024)
-
Tissue-specific thresholds of mutation burden associated with anti-PD-1/L1 therapy benefit and prognosis in microsatellite-stable cancers
Nature Cancer (2024)
-
Pan-cancer analysis of NFE2L2 mutations identifies a subset of lung cancers with distinct genomic and improved immunotherapy outcomes
Cancer Cell International (2023)