Abstract
Unlike most tumor suppressor genes, the most common genetic alterations in tumor protein p53 (TP53) are missense mutations1,2. Mutant p53 protein is often abundantly expressed in cancers and specific allelic variants exhibit dominant-negative or gain-of-function activities in experimental models3,4,5,6,7,8. To gain a systematic view of p53 function, we interrogated loss-of-function screens conducted in hundreds of human cancer cell lines and performed TP53 saturation mutagenesis screens in an isogenic pair of TP53 wild-type and null cell lines. We found that loss or dominant-negative inhibition of wild-type p53 function reliably enhanced cellular fitness. By integrating these data with the Catalog of Somatic Mutations in Cancer (COSMIC) mutational signatures database9,10, we developed a statistical model that describes the TP53 mutational spectrum as a function of the baseline probability of acquiring each mutation and the fitness advantage conferred by attenuation of p53 activity. Collectively, these observations show that widely-acting and tissue-specific mutational processes combine with phenotypic selection to dictate the frequencies of recurrent TP53 mutations.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
All data sets analyzed in the current study are included in this published manuscript and its supplementary information files or can be found in the published works cited herein.
References
Hainaut, P. & Pfeifer, G. P. Somatic TP53 mutations in the era of genome sequencing. Cold Spring Harb. Perspect. Med. 6, a026179 (2016).
Petitjean, A. et al. Impact of mutant p53 functional properties on TP53 mutation patterns and tumor phenotype: lessons from recent developments in the IARC TP53 database. Hum. Mutat. 28, 622–629 (2007).
Milner, J. & Medcalf, E. A. Cotranslation of activated mutant p53 with wild type drives the wild-type p53 protein into the mutant conformation. Cell 65, 765–774 (1991).
Harvey, M. et al. A mutant p53 transgene accelerates tumour development in heterozygous but not nullizygous p53-deficient mice. Nat. Genet. 9, 305–311 (1995).
de Vries, A. et al. Targeted point mutations of p53 lead to dominant-negative inhibition of wild-type p53 function. Proc. Natl. Acad. Sci. USA 99, 2948–2953 (2002).
Olive, K. P. et al. Mutant p53 gain of function in two mouse models of Li–Fraumeni syndrome. Cell 119, 847–860 (2004).
Lang, G. A. et al. Gain of function of a p53 hot spot mutation in a mouse model of Li–Fraumeni syndrome. Cell 119, 861–872 (2004).
Freed-Pastor, W. A. & Prives, C. Mutant p53: one name, many proteins. Genes Dev. 26, 1268–1286 (2012).
Alexandrov, L. B. et al. Signatures of mutational processes in human cancer. Nature 500, 415–421 (2013).
Alexandrov, L. B. et al. Clock-like mutational processes in human somatic cells. Nat. Genet. 47, 1402–1407 (2015).
Tsherniak, A. et al. Defining a cancer dependency map. Cell 170, 564–576.e16 (2017).
Meyers, R. M. et al. Computational correction of copy number effect improves specificity of CRISPR–Cas9 essentiality screens in cancer cells. Nat. Genet. 49, 1779–1784 (2017).
Melnikov, A., Rogov, P., Wang, L., Gnirke, A. & Mikkelsen, T. S. Comprehensive mutational scanning of a kinase in vivo reveals substrate-dependent fitness landscapes. Nucleic Acids Res. 42, e112 (2014).
Brenan, L. et al. Phenotypic characterization of a comprehensive set of MAPK1/ERK2 missense mutants. Cell Rep. 17, 1171–1183 (2016).
Majithia, A. R. et al. Prospective functional classification of all possible missense variants in PPARG. Nat. Genet. 48, 1570–1575 (2016).
Drost, J. et al. Sequential cancer mutations in cultured human intestinal stem cells. Nature 521, 43–47 (2015).
Vassilev, L. T. et al. In vivo activation of the p53 pathway by small-molecule antagonists of MDM2. Science 303, 844–848 (2004).
Fang, S., Jensen, J. P., Ludwig, R. L., Vousden, K. H. & Weissman, A. M. Mdm2 is a RING finger-dependent ubiquitin protein ligase for itself and p53. J. Biol. Chem. 275, 8945–8951 (2000).
Momand, J., Zambetti, G. P., Olson, D. C., George, D. & Levine, A. J. The mdm-2 oncogene product forms a complex with the p53 protein and inhibits p53-mediated transactivation. Cell 69, 1237–1245 (1992).
Zhang, Y., Xiong, Y. & Yarbrough, W. G. ARF promotes MDM2 degradation and stabilizes p53: ARF-INK4a locus deletion impairs both the Rb and p53 tumor suppression pathways. Cell 92, 725–734 (1998).
Lin, A. W. & Lowe, S. W. Oncogenic ras activates the ARF-p53 pathway to suppress epithelial cell transformation. Proc. Natl. Acad. Sci. USA 98, 5025–5030 (2001).
Eischen, C. M., Weber, J. D., Roussel, M. F., Sherr, C. J. & Cleveland, J. L. Disruption of the ARF–Mdm2–p53 tumor suppressor pathway in Myc-induced lymphomagenesis. Genes Dev. 13, 2658–2669 (1999).
Khosravi, R. et al. Rapid ATM-dependent phosphorylation of MDM2 precedes p53 accumulation in response to DNA damage. Proc. Natl. Acad. Sci. USA 96, 14973–14977 (1999).
Friedman, P. N., Chen, X., Bargonetti, J. & Prives, C. The p53 protein is an unusually shaped tetramer that binds directly to DNA. Proc. Natl. Acad. Sci. USA 90, 3319–3323 (1993).
Wang, P. et al. p53 domains: structure, oligomerization, and transformation. Mol. Cell. Biol. 14, 5182–5191 (1994).
Clarke, A. R. et al. Thymocyte apoptosis induced by p53-dependent and independent pathways. Nature 362, 849–852 (1993).
Lowe, S. W., Schmitt, E. M., Smith, S. W., Osborne, B. A. & Jacks, T. p53 is required for radiation-induced apoptosis in mouse thymocytes. Nature 362, 847–849 (1993).
Lowe, S. W., Ruley, H. E., Jacks, T. & Housman, D. E. p53-dependent apoptosis modulates the cytotoxicity of anticancer agents. Cell 74, 957–967 (1993).
Lukin, D. J., Carvajal, L. A., Liu, W. J., Resnick-Silverman, L. & Manfredi, J. J. p53 promotes cell survival due to the reversibility of its cell-cycle checkpoints. Mol. Cancer Res. 13, 16–28 (2015).
Bunz, F. et al. Requirement for p53 and p21 to sustain G2 arrest after DNA damage. Science 282, 1497–1501 (1998).
Bunz, F. et al. Disruption of p53 in human cancer cells alters the responses to therapeutic agents. J. Clin. Invest. 104, 263–269 (1999).
Bouaoun, L. et al. TP53 variations in human cancers: new lessons from the IARC TP53 database and genomics data. Hum. Mutat. 37, 865–876 (2016).
Kato, S. et al. Understanding the function–structure and function–mutation relationships of p53 tumor suppressor protein by high-resolution missense mutation analysis. Proc. Natl. Acad. Sci. USA 100, 8424–8429 (2003).
Mathe, E. et al. Computational approaches for predicting the biological effect of p53 missense mutations: a comparison of three sequence analysis based methods. Nucleic Acids Res. 34, 1317–1325 (2006).
André, F. et al. AACR Project GENIE: powering precision medicine through an international consortium. Cancer Discov. 7, 818–831 (2017).
Rideout, W. M. 3rd, Coetzee, G. A., Olumi, A. F. & Jones, P. A. 5-Methylcytosine as an endogenous mutagen in the human LDL receptor and p53 genes. Science 249, 1288–1290 (1990).
Tornaletti, S., Rozek, D. & Pfeifer, G. P. The distribution of UV photoproducts along the human p53 gene and its relation to mutations in skin cancer. Oncogene 8, 2051–2057 (1993).
Aguilar, F., Hussain, S. P. & Cerutti, P. Aflatoxin B1 induces the transversion of G-- > T in codon 249 of the p53 tumor suppressor gene in human hepatocytes. Proc. Natl. Acad. Sci. USA 90, 8586–8590 (1993).
Puisieux, A., Lim, S., Groopman, J. & Ozturk, M. Selective targeting of p53 gene mutational hotspots in human cancers by etiologically defined carcinogens. Cancer Res. 51, 6185–6189 (1991).
Bressac, B., Kew, M., Wands, J. & Ozturk, M. Selective G to T mutations of p53 gene in hepatocellular carcinoma from southern Africa. Nature 350, 429–431 (1991).
Hsu, I. C. et al. Mutational hotspot in the p53 gene in human hepatocellular carcinomas. Nature 350, 427–428 (1991).
Brash, D. E. et al. A role for sunlight in skin cancer: UV-induced p53 mutations in squamous cell carcinoma. Proc. Natl. Acad. Sci. USA 88, 10124–10128 (1991).
Pierceall, W. E., Mukhopadhyay, T., Goldberg, L. H. & Ananthaswamy, H. N. Mutations in the p53 tumor suppressor gene in human cutaneous squamous cell carcinomas. Mol. Carcinog. 4, 445–449 (1991).
Barretina, J. et al. The Cancer Cell Line Encyclopedia enables predictive modelling of anticancer drug sensitivity. Nature 483, 603–607 (2012).
Garnett, M. J. et al. Systematic identification of genomic markers of drug sensitivity in cancer cells. Nature 483, 570–575 (2012).
Seashore-Ludlow, B. et al. Harnessing connectivity in a large-scale small-molecule sensitivity dataset. Cancer Discov. 5, 1210–1223 (2015).
Gao, J. et al. Integrative analysis of complex cancer genomics and clinical profiles using the cBioPortal. Sci. Signal. 6, pl1 (2013).
Jeay, S. et al. A distinct p53 target gene set predicts for response to the selective p53-HDM2 inhibitor NVP-CGM097. eL ife 4, e06498 (2015).
Cowley, G. S. et al. Parallel genome-scale loss of function screens in 216 cancer cell lines for the identification of context-specific genetic dependencies. Sci. Data 1, 140035 (2014).
Brinkman, E. K., Chen, T., Amendola, M. & van Steensel, B. Easy quantitative assessment of genome editing by sequence trace decomposition. Nucleic Acids Res. 42, e168 (2014).
Dyer, B. W., Ferrer, F. A., Klinedinst, D. K. & Rodriguez, R. A noncommercial dual luciferase enzyme assay system for reporter gene analysis. Anal. Biochem. 282, 158–161 (2000).
Bennett, R. P., Cox, C. A. & Hoeffler, J. P. Fusion of green fluorescent protein with the Zeocin-resistance marker allows visual screening and drug selection of transfected eukaryotic cells. Biotechniques 24, 478–482 (1998).
Acknowledgements
This work was funded in part by grants from the US National Cancer Institute (U01 CA176058, U01 CA199253). T.P.H. is the recipient of training grants from the US National Institutes of Health (T32GM007753 and T32GM007226). G.G. was partially funded by the Paul C. Zamecnik Chair in Oncology from the Massachusetts General Hospital Cancer Center.
Author information
Authors and Affiliations
Contributions
A.O.G. and W.C.H. designed the study. A.O.G., X.Y., and R.E.L. performed the experiments with help from T.P.H., D.Y.T., S.H.L., E.K., H.S.G., B.H., A.G., and B.F. A.O.G., X.Y., R.E.L., J.M.M., M.D., J.K., and D.E.R. analyzed the data with help from T.S., S.S., F.V., A.T., A.J.A., J.G.D., F.P., and G.G. A.O.G. and W.C.H. wrote the manuscript. D.E.R., C.M.J., M.M., and C.W.M.R. revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
M.M. is a consultant for OrigiMed and receives research support from Bayer. W.C.H. is a consultant for KSQ Therapeutics.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Suppression of endogenous wild-type but not mutant TP53 impacts cellular fitness in human cancer cells.
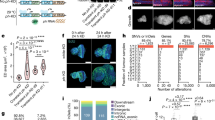
a,b, Comparison of enrichment scores (Cell 170, 564–576, 2017) for RNAi reagents targeting TP53 (a) or MDM2 (b) in cell lines with differing p53 status. The functional and genetic p53 status of each cell line was defined using publicly available p53 target gene expression, nutlin-3 sensitivity, and TP53 sequencing data (Supplementary Table 1). Only cell lines with concordant functional and genetic classifications were included in the analyses in a–c. Each point represents the gene-level score for a given cell line, and error bars indicate the mean and s.d. of each group. c, p53 protein expression in cancer cell lines as measured by reverse-phase protein array (RPPA). d–g, Comparison of enrichment scores for TP53-targeting reagents for cell lines with concordant (d,e) or discordant (f,g) genetic and functional TP53 status (*P < 0.05, ****P < 0.0001, two-tailed Welch’s t-test).
Supplementary Figure 2 Response to MDM2 inhibition and DNA damage in cells expressing exogenous wild-type or mutant p53.
a, p53WT and p53NULL A549 cells were infected with a lentivirus encoding wild-type p53, mutant p53 p.Pro278Ala, or Renilla luciferase as a negative control and treated with DMSO vehicle or nutlin-3 at 10 µM for 24 h. b–e, Immunoblots were performed on whole-cell lysate using antibodies targeting p53, p21, or β-actin and detected using HRP-conjugated secondary antibodies. Cells were seeded into the wells of 96-well dishes at 200 cells/well, treated with the indicated compounds and subjected to CellTiter-Glo assays 7 d later. Luminescence readings were normalized to those for DMSO-treated wells (100% luminescence) and wells lacking cells (0% luminescence). b, Nutlin-3, 2.5 µM. c, Nutlin-3, 5 µM. d, Etoposide, 5 µM. e, Etoposide, 5 µM. Data from 3–5 independent experiments are presented as the mean ± s.e.m. (*P < 0.05, **P < 0.01, ***P < 0.001, two-tailed paired t-test).
Supplementary Figure 3 Differential fitness of isogenic p53WT and p53NULL cells treated with chemotherapeutic agents.
a, Graphical overview of the LucifeRace competition assay. b, p53WT and p53NULL cells were infected at low MOI with lentivirus expressing either firefly (FF) or Renilla luciferase. Paired cell lines were mixed together at a 1:1 ratio (p53WT-Renilla with p53NULL-FF, and p53WT-FF with p53NULL-Renilla) and seeded into two replica plates. Twenty-four hours later, cells were treated with the indicated drugs at six doses and incubated for 2 d more. One of the plates was then subjected to a dual-luciferase assay and the other was used for continued passaging. Raw FF and Renilla luminescence values for each well were normalized to their respective DMSO vehicle-treated wells and are presented as a ratio. Drugs were delivered as a twofold-dilution series to achieve the following high doses: gemcitabine (100 nM), 5-fluorouracil (10 µM), actinomycin D (10 nM), oxaliplatin (25 µM), bleomycin (5 µM), doxorubicin (50 nM), etoposide (2.5 µM), nutlin-3 (20 µM), vinblastine (5 nM), and paclitaxel (10 nM). c,d, LucifeRace WT:KO luminescence ratios plotted over time for each dose of etoposide and doxorubicin. e–j, CellTiter-Glo assays were performed on cells treated with etoposide or doxorubicin and dose–response curves were fit using GraphPad Prism 7 software. Representative curves for each drug are shown (e,f), along with the best fit values for the curve midpoint (EC50; g,h) and minimum (Curve Bottom; i–,j) (mean ± s.e.m., three independent experiments, two-tailed paired t-test, **P< 0.01).
Supplementary Figure 4 Comparison of TP53 MITE screen data with existing datasets.
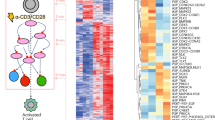
a–i, log2-normalized read counts (a,d,e) and Z-scores (b,e,h) were plotted for each experimental condition and replicate. The Pearson correlation (R2) was calculated for each plot using GraphPad Prism 7 software. c,f,i, Average Z-scores plotted at each codon position. j, Heat map of position-level average Z-scores for each screen condition plotted in line with position-level average transcriptional activity in yeast at the p21 promoter (Proc. Natl. Acad. Sci. USA 100, 8424–8429, 2003), evolutionary conservation scores derived using Align-GVGD (Nucleic Acids Res. 34, 1317–1325, 2006), and total number of mutations found at each codon in the IARC somatic TP53 mutation database (Human Mutation 37, 865–876, 2016; Human Mutation 28, 622–629, 2007). k, Pearson correlation matrices comparing the indicated datasets. Nut, nutlin-3; Eto, etoposide; EvoCon, evolutionary conservation. l, Density plots of combined phenotype scores for the indicated allele classes (left) with common somatic TP53 mutations and common TP53 germline polymorphisms highlighted along the distribution (right). m, Transcriptional activity of common somatic mutations and common germline polymorphisms measured in yeast (mean of eight activity reporters + s.e.m.) (Proc. Natl. Acad. Sci. USA 100, 8424–8429, 2003).
Supplementary Figure 5 Identification of TP53 alleles that exhibit assay-specific functions.
a–c, Alleles were ranked according to the mean effect size from the two independent experiments with error bars representing the range of Z-scores. d–f, xy scatterplots of average Z-scores for the three pairs of screen conditions. g,h, Dominant-negative and loss-of-function alleles (defined by Z-scores that were 3 s.d. away from the mean Z-score of all silent mutations) showed a high degree of overlap, especially missense mutations in the DNA-binding domain. TAD, transactivation domain; PRD, proline-rich domain; DBD, DNA-binding domain; 4D, tetramerization domain; CTD, C-terminal domain.
Supplementary Figure 6 Mutational signatures and phenotypic selection dictate the spectrum of recurrent TP53 alterations.
Generalized linear models were used to estimate the contributions made by mutational processes and phenotypic selection to the TP53 mutation counts in the IARC somatic R18 database (Human Mutation 37, 865–876, 2016; Human Mutation 28, 622–629, 2007). a–c, Model predictions for each codon (a,b) or allele (c) are shown plotted against the observed mutation counts in the database. d–k, Tenfold cross-validation (h–k) yielded similar descriptive and predictive accuracies, standardized coefficients, and P values as the final combined model (d–g), indicating that the improved performance of the combined model was not due to overfitting to the training data. l–o, Examples of alleles characterized by high intrinsic mutability and strong phenotypic effects (Arg273His, Arg175His, and Arg248Trp), low intrinsic mutability but strong phenotypic effects (Thr125Pro, Cys124Gly, and Phe212Val), and high intrinsic mutability but weak phenotypic effects (Val157Ile, Arg290His, and Arg282Gln).
Supplementary Figure 7 Cancer cell lines harboring TP53 variants of uncertain significance display wild-type-like responses to p53 pathway perturbation.
a, p53 pathway scores were assigned to each cell line in the Project Achilles RNAi dataset using DEMETER scores for TP53, USP28, TP53BP1, CHEK2, ATM, CDKN1A, MDM2, MDM4, PPM1D, USP7, and UBE2D3. Density plots for cell lines with concordant genetic and functional p53 status are shown (left), and REH, RMUGS, and HCC2218, which bear the indicated TP53 mutations, are highlighted along the distribution (right). b, Combined phenotype scores were assigned to each TP53 allele using the data from all three MITE library screens. Density plots for the indicated allele classes are shown (left), and Arg181Cys, Arg283Cys, and Ala347Val alleles are highlighted along the distribution (right).
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–7 and Supplementary Note
Supplementary Data
Source data for Supplementary Figure 2
Supplementary Table 1
Cancer cell line TP53 classification matrix
Supplementary Table 2
Read counts for all TP53 codon variants
Supplementary Table 3
Z-scores, mutation probabilities and model predictions for all TP53 amino acid variants
Supplementary Table 4
Sequences of sgRNAs used to target TP53
Supplementary Table 5
Signature 4* mutation probabilities
Rights and permissions
About this article
Cite this article
Giacomelli, A.O., Yang, X., Lintner, R.E. et al. Mutational processes shape the landscape of TP53 mutations in human cancer. Nat Genet 50, 1381–1387 (2018). https://doi.org/10.1038/s41588-018-0204-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41588-018-0204-y
This article is cited by
-
Conserved methylation signatures associate with the tumor immune microenvironment and immunotherapy response
Genome Medicine (2024)
-
High-throughput evaluation of genetic variants with prime editing sensor libraries
Nature Biotechnology (2024)
-
ERK pathway agonism for cancer therapy: evidence, insights, and a target discovery framework
npj Precision Oncology (2024)
-
Pharmacological reactivation of p53 in the era of precision anticancer medicine
Nature Reviews Clinical Oncology (2024)
-
Targeting p53 gain-of-function activity in cancer therapy: a cautionary tale
Cell Death & Differentiation (2024)