Abstract
Molecular glue compounds induce protein–protein interactions that, in the context of a ubiquitin ligase, lead to protein degradation1. Unlike traditional enzyme inhibitors, these molecular glue degraders act substoichiometrically to catalyse the rapid depletion of previously inaccessible targets2. They are clinically effective and highly sought-after, but have thus far only been discovered serendipitously. Here, through systematically mining databases for correlations between the cytotoxicity of 4,518 clinical and preclinical small molecules and the expression levels of E3 ligase components across hundreds of human cancer cell lines3,4,5, we identify CR8—a cyclin-dependent kinase (CDK) inhibitor6—as a compound that acts as a molecular glue degrader. The CDK-bound form of CR8 has a solvent-exposed pyridyl moiety that induces the formation of a complex between CDK12–cyclin K and the CUL4 adaptor protein DDB1, bypassing the requirement for a substrate receptor and presenting cyclin K for ubiquitination and degradation. Our studies demonstrate that chemical alteration of surface-exposed moieties can confer gain-of-function glue properties to an inhibitor, and we propose this as a broader strategy through which target-binding molecules could be converted into molecular glues.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Structural data have been deposited in the PDB under the accession code 6TD3. Proteome quantification data are available in the PRIDE repository (PXD016187 and PXD016188). Additional ITC data are provided in Supplementary Fig. 1. Uncropped gel and western blot source data are shown in Supplementary Fig. 2 and the flow cytometry gating strategy is shown in Supplementary Fig. 3.
Code availability
The code necessary to reproduce the statistical analysis is included in the Supplementary Information.
References
Stanton, B. Z., Chory, E. J. & Crabtree, G. R. Chemically induced proximity in biology and medicine. Science 359, eaao5902 (2018).
Chopra, R., Sadok, A. & Collins, I. A critical evaluation of the approaches to targeted protein degradation for drug discovery. Drug Discov. Today. Technol. 31, 5–13 (2019).
Yu, C. et al. High-throughput identification of genotype-specific cancer vulnerabilities in mixtures of barcoded tumor cell lines. Nat. Biotechnol. 34, 419–423 (2016).
Corsello, S. M. et al. Discovering the anticancer potential of non-oncology drugs by systematic viability profiling. Nat. Cancer 1, 235–248 (2020).
Ghandi, M. et al. Next-generation characterization of the Cancer Cell Line Encyclopedia. Nature 569, 503–508 (2019).
Bettayeb, K. et al. CR8, a potent and selective, roscovitine-derived inhibitor of cyclin-dependent kinases. Oncogene 27, 5797–5807 (2008).
Fink, E. C. & Ebert, B. L. The novel mechanism of lenalidomide activity. Blood 126, 2366–2369 (2015).
Lu, G. et al. The myeloma drug lenalidomide promotes the cereblon-dependent destruction of Ikaros proteins. Science 343, 305–309 (2014).
Krönke, J. et al. Lenalidomide causes selective degradation of IKZF1 and IKZF3 in multiple myeloma cells. Science 343, 301–305 (2014).
Matyskiela, M. E. et al. A novel cereblon modulator recruits GSPT1 to the CRL4CRBN ubiquitin ligase. Nature 535, 252–257 (2016).
Petzold, G., Fischer, E. S. & Thomä, N. H. Structural basis of lenalidomide-induced CK1α degradation by the CRL4CRBN ubiquitin ligase. Nature 532, 127–130 (2016).
Fischer, E. S. et al. Structure of the DDB1-CRBN E3 ubiquitin ligase in complex with thalidomide. Nature 512, 49–53 (2014).
Han, T. et al. Anticancer sulfonamides target splicing by inducing RBM39 degradation via recruitment to DCAF15. Science 356, eaal3755 (2017).
Uehara, T. et al. Selective degradation of splicing factor CAPERα by anticancer sulfonamides. Nat. Chem. Biol. 13, 675–680 (2017).
Faust, T. B. et al. Structural complementarity facilitates E7820-mediated degradation of RBM39 by DCAF15. Nat. Chem. Biol. 16, 7–14 (2020).
Bondeson, D. P. et al. Catalytic in vivo protein knockdown by small-molecule PROTACs. Nat. Chem. Biol. 11, 611–617 (2015).
Angers, S. et al. Molecular architecture and assembly of the DDB1-CUL4A ubiquitin ligase machinery. Nature 443, 590–593 (2006).
Lee, J. & Zhou, P. DCAFs, the missing link of the CUL4-DDB1 ubiquitin ligase. Mol. Cell 26, 775–780 (2007).
Bösken, C. A. et al. The structure and substrate specificity of human Cdk12/Cyclin K. Nat. Commun. 5, 3505 (2014).
Cheng, S.-W. G. et al. Interaction of cyclin-dependent kinase 12/CrkRS with cyclin K1 is required for the phosphorylation of the C-terminal domain of RNA polymerase II. Mol. Cell. Biol. 32, 4691–4704 (2012).
Dixon-Clarke, S. E., Elkins, J. M., Cheng, S. W. G., Morin, G. B. & Bullock, A. N. Structures of the CDK12/CycK complex with AMP-PNP reveal a flexible C-terminal kinase extension important for ATP binding. Sci. Rep. 5, 17122 (2015).
Oumata, N. et al. Roscovitine-derived, dual-specificity inhibitors of cyclin-dependent kinases and casein kinases 1. J. Med. Chem. 51, 5229–5242 (2008).
Meijer, L. et al. Biochemical and cellular effects of roscovitine, a potent and selective inhibitor of the cyclin-dependent kinases cdc2, cdk2 and cdk5. Eur. J. Biochem. 243, 527–536 (1997).
Zhang, T. et al. Covalent targeting of remote cysteine residues to develop CDK12 and CDK13 inhibitors. Nat. Chem. Biol. 12, 876–884 (2016).
Sedlacek, H. et al. Flavopiridol (L86 8275; NSC 649890), a new kinase inhibitor for tumor therapy. Int. J. Oncol. 9, 1143–1168 (1996).
Sievers, Q. L. et al. Defining the human C2H2 zinc finger degrome targeted by thalidomide analogs through CRBN. Science 362, eaat0572 (2018).
Jones, L. H. Small-molecule kinase downregulators. Cell Chem. Biol. 25, 30–35 (2018).
Schreiber, S. L. A chemical biology view of bioactive small molecules and a binder-based approach to connect biology to precision medicines. Isr. J. Chem. 59, 52–59 (2019).
Ito, T. et al. Identification of a primary target of thalidomide teratogenicity. Science 327, 1345–1350 (2010).
Fischer, E. S. et al. The molecular basis of CRL4DDB2/CSA ubiquitin ligase architecture, targeting, and activation. Cell 147, 1024–1039 (2011).
Johnson, S. F. et al. CDK12 inhibition reverses de novo and acquired PARP inhibitor resistance in BRCA wild-type and mutated models of triple-negative breast cancer. Cell Rep. 17, 2367–2381 (2016).
Dykes, G. W., Crepeau, R. H. & Edelstein, S. J. Three-dimensional reconstruction of the 14-filament fibers of hemoglobin S. J. Mol. Biol. 130, 451–472 (1979).
Garcia-Seisdedos, H., Empereur-Mot, C., Elad, N. & Levy, E. D. Proteins evolve on the edge of supramolecular self-assembly. Nature 548, 244–247 (2017).
Sievers, Q. L., Gasser, J. A., Cowley, G. S., Fischer, E. S. & Ebert, B. L. Genome-wide screen identifies cullin-RING ligase machinery required for lenalidomide-dependent CRL4CRBN activity. Blood 132, 1293–1303 (2018).
Doench, J. G. et al. Optimized sgRNA design to maximize activity and minimize off-target effects of CRISPR–Cas9. Nat. Biotechnol. 34, 184–191 (2016).
Sanjana, N. E., Shalem, O. & Zhang, F. Improved vectors and genome-wide libraries for CRISPR screening. Nat. Methods 11, 783–784 (2014).
Donovan, K. A. et al. Thalidomide promotes degradation of SALL4, a transcription factor implicated in Duane Radial Ray syndrome. eLife 7, e38430 (2018).
Benjamini, Y. & Hochberg, Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J. R. Stat. Soc. B 57, 289–300 (1995).
Abdulrahman, W. et al. A set of baculovirus transfer vectors for screening of affinity tags and parallel expression strategies. Anal. Biochem. 385, 383–385 (2009).
Li, T., Pavletich, N. P., Schulman, B. A. & Zheng, N. High-level expression and purification of recombinant SCF ubiquitin ligases. Methods Enzymol. 398, 125–142 (2005).
Winn, M. D. et al. Overview of the CCP4 suite and current developments. Acta Crystallogr. D. 67, 235–242 (2011).
Tickle, I. J. et al. STARANISO (Global Phasing, 2018).
McCoy, A. J. et al. Phaser crystallographic software. J. Appl. Crystallogr. 40, 658–674 (2007).
Emsley, P., Lohkamp, B., Scott, W. G. & Cowtan, K. Features and development of Coot. Acta Crystallogr. D 66, 486–501 (2010).
Afonine, P. V. et al. Towards automated crystallographic structure refinement with phenix.refine. Acta Crystallogr. D 68, 352–367 (2012).
Bricogne, G. et al. BUSTER (Global Phasing, 2017).
Moriarty, N. W., Grosse-Kunstleve, R. W. & Adams, P. D. electronic Ligand Builder and Optimization Workbench (eLBOW): a tool for ligand coordinate and restraint generation. Acta Crystallogr. D 65, 1074–1080 (2009).
Chen, V. B. et al. MolProbity: all-atom structure validation for macromolecular crystallography. Acta Crystallogr. D 66, 12–21 (2010).
Krissinel, E. & Henrick, K. Inference of macromolecular assemblies from crystalline state. J. Mol. Biol. 372, 774–797 (2007).
Cer, R. Z., Mudunuri, U., Stephens, R. & Lebeda, F. J. IC 50-to-K i: a web-based tool for converting IC 50 to K i values for inhibitors of enzyme activity and ligand binding. Nucleic Acids Res. 37, W441–W445 (2009).
Sperling, A. S. et al. Patterns of substrate affinity, competition, and degradation kinetics underlie biological activity of thalidomide analogs. Blood 134, 160–170 (2019).
Acknowledgements
We thank S. Cavadini and A. Schenk for support during electron microscopy data collection and processing; M. Kolesnikov for help with ITC experiments; the Broad Institute PRISM (particularly M. Kocak); the Compound Management, Cancer Data Science, Walk-up Sequencing, Genetic Perturbation Platform and Flow Facility teams (particularly P. Rogers), K. DeRuff for the introduction to the Agilent BRAVO Automated Liquid Handling Platform, and J. Kennedy for providing sgRNA.SFFV.tBFP and sgRNA.EFS.RFP657 backbones. We acknowledge the Paul Scherrer Institute for provision of synchrotron radiation beam time at beamline PXI of the SLS and thank T. Tomizaki for assistance. We are grateful to all members of the Ebert group, particularly R. Belizaire, S. Koochaki, P. Miller and C. Zou; as well as R. Nowak and P. Tsvetkov, for discussions. This work was supported by the NIH (grants R01HL082945, P01CA108631 and P50CA206963), the Howard Hughes Medical Institute, the Edward P. Evans Foundation and the Leukaemia and Lymphoma Society (to B.L.E.); funding from the European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation program grant agreement no. 666068, the Gebert Rüf Stiftung (GRS-057/14) and the Novartis Research Foundation (to N.H.T.); and NIH grants NCI R01CA214608 and R01CA218278 and a Mark Foundation Emerging Leader Award (to E.S.F.). M.S. received funding from the European Union’s Horizon 2020 Research and Innovation Program under the Marie Skłodowska-Curie grant agreement no. 702642; Z.K. was supported by the European Union’s Horizon 2020 Research and Innovation Program under the Marie Skłodowska-Curie grant agreement no. 765445; G.P. was supported by the Human Frontier Science Program (HFSP Long-Term Fellowship LT000210/2014) and the European Molecular Biology Organization (EMBO Advanced Fellowship aALTF 761-2016); A.S.S. was supported by a DF/HCC K12 grant, a Conquer Cancer Foundation Young Investigator Award and an award from the Wong Family Foundation; R.S.S. was supported by an Intermediate Fellowship from the Kay Kendall Leukaemia Fund and an Advanced Clinician Scientist Fellowship from Cancer Research UK; and S.M.C. received funding from grants KL2 TR002542 and K08 CA230220.
Author information
Authors and Affiliations
Contributions
M.S. designed and performed functional genomics studies with the help of J.K., R.S.S. and E.C.F.; Z.K. and G.P. designed and carried out structural, biochemical and biophysical studies with the help of D.S.; M.S., Y.-D.L., M.M. and Q.L.S. designed and performed cell validation experiments with the help of A.S.S., J.A.G. and M.J.; K.A.D. performed the mass spectrometry experiments; M.S., L.R.W. and S.M.C. performed bioinformatic PRISM analysis; R.B. and G.P. performed structure refinement with the help of Z.K.; D.G., C.S., S.F., T.R.G., E.S.F., N.H.T. and B.L.E. supervised the project; and Z.K., G.P., M.S., B.L.E. and N.H.T. wrote the manuscript with input from all authors.
Corresponding authors
Ethics declarations
Competing interests
B.L.E. has received research funding from Celgene and Deerfield and consulting fees from GRAIL. He serves on the scientific advisory boards for and holds equity in Skyhawk Therapeutics and Exo Therapeutics. E.S.F. is a founder and/or member of the scientific advisory board and equity holder of C4 Therapeutics and Civetta Therapeutics, and is a consultant to Novartis, AbbVie and Pfizer. N.H.T. receives funding from the Novartis Research Foundation and is a member of the scientific advisory board of Monte Rosa Therapeutics. The Fischer laboratory receives or has received research funding from Novartis, Deerfield and Astellas. S.F. has had a consulting or advisory role, received honoraria, research funding and/or travel/accommodation expenses funding from the following for-profit companies: Bayer, Roche, Amgen, Eli Lilly, PharmaMar, AstraZeneca and Pfizer. R.B. is now an employee of Monte Rosa Therapeutics. S.M.C. and T.R.G. receive research funding from Bayer HealthCare. T.R.G. was formerly a consultant and equity holder in Foundation Medicine (acquired by Roche). T.R.G. also is a consultant to GlaxoSmithKline and is a founder of Sherlock Biosciences.
Additional information
Peer review information Nature thanks Ivan Dikic, Frank Sicheri and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 CR8-induced degradation of cyclin K correlates with DDB1 expression.
a, Schematic of the bioinformatic screen for drug–E3 pairs. b, Box plot (centre, median; box, interquartile range (IQR); whiskers, 1.5 × IQR; points, outliers) for correlations between gene expression and drug sensitivity (CR8 n = 19,110; indisulam and tasisulam n = 19,109; DDB1 and DCAF15 n = 1,618). c, Example Pearson correlation of selected drug–E3 pairs: positive controls (indisulam and DCAF15; tasisulam and DCAF15) and no correlation controls (others) (indisulam n = 452; tasisulam n = 418; CR8 n = 471), area under the curve (AUC). d, Schematic of flow-based primary validation screen. e, Top three hits from the primary validation screen in five cell lines, performed according to the schematic in d. f, Whole-proteome quantification of MOLT-4 cells treated with 1 μM CR8 (n = 1) or DMSO (n = 3) for 1 h (two-sided moderated t-test, n = 3). g, Log2(protein levels CR8 treatment/protein levels DMSO treatment) in whole-proteome quantification after 1 h and 5 h of exposure to CR8 plotted against each other. h, mRNA levels quantified by qPCR in HEK293T-Cas9 cells after treatment with 1 μM CR8 for 2 h. Bars represent the mean (n = 9).
Extended Data Fig. 2 CDK12 is required for CR8-induced cyclin K degradation.
a, Schematic of the genome-wide CRISPR–Cas9 resistance screen. b, Bison CRISPR–Cas9 CR8 resistence screen. Guide counts were collapsed to gene level (n = 4 guides per gene; two-sided empirical rank-sum test statistics). c, Schematic of the cyclin K (CCNK) stability reporter. IRES, internal ribosome entry site. d, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells that were pretreated with 0.5 μM MLN7243, 1 μM MLN4924 or 10 μM MG132 for 4 h and then treated with 1 μM CR8 for 2 h (n = 3). e, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells treated with CR8 (n = 3). f, Immunoblots of cyclin K degradation in HEK293T-Cas9 cells treated with CR8 for 2 h (n = 2). g, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells treated with 1 μM of the indicated compounds for 2 h (n = 3). h, Schematic of the genome-wide CRISPR–Cas9 reporter screen for cyclin K stability. i, Genome-wide CRISPR–Cas9 reporter screen for cyclin KeGFP stability with DMSO treatment in HEK293T-Cas9 cells. Guide counts were collapsed to gene level (n = 4 guides per gene; two-sided empirical rank-sum test statistics). j, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells after treatment with 1μM CR8 for 2 h (n = 3). k, Flow analysis of full-length cyclin KeGFP or cyclin KeGFP(1–270) in HEK293T-Cas9 cells after treatment with 1 μM CR8 for 2 h (n = 3). Bars represent the mean in d, g, j, k.
Extended Data Fig. 3 CR8-induced degradation of cyclin K is not dependent on a canonical DCAF substrate receptor.
a, Drug sensitivity of K562-Cas9, P31FUJ-Cas9, THP1-Cas9 and MM1S-Cas9 cells that were treated with CR8 for three days (n = 3). b, mRNA levels of genes in the DCAF library. The black vertical lines represent the mean (n = 4). c, Flow analysis of K562-Cas9, P31FUJ-Cas9, THP1-Cas9 and MM1S-Cas9 cells expressing sgRNAs and a BFP marker after a three-day treatment with 1 μM CR8. The black vertical lines represent the mean (n > 2).
Extended Data Fig. 4 Characterization of DDB1–CDK12–cyclin K complex formation.
a, Schematic of the TR-FRET set-up. Positions of FRET donor (terbium-coupled streptavidin (Tb)) and acceptor (Alexa488–SpyCatcher (A)) are indicated in the structural model. b, Titration of CDK12–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). c, Counter-titration of unlabelled wild-type CDK12–cyclin K (0–10 μM) into 50 nM DDB1terbium, 500 nM CDK12–cyclin KAlexa488 and 12.5 μM CR8 (n = 3). d, Counter-titration of unlabelled wild-type DDB1 (0–10 μM) into 50 nM DDB1terbium, 500 nM CDK12–cyclin KAlexa488 and 1 μM CR8 (n = 3). e, Titration of CDK12(R965K)–cyclin KAlexa488 (wild-type sequence of the canonical isoform of CDK12; 0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). The CDK12(K965R) variant, which was used throughout our in vitro studies (see Methods), shows a binding affinity indistinguishable from that of the canonical isoform of CDK12 (residue distal from the interface with DDB1 and cyclin K). f–k, ITC experiments. Specifications of the titrations are given in the panels. N.d., not determined. ΔS, entropy of binding. Kd values are referred to as Kapparent because not all data could be confidently fitted with binding curves. An asterisk marking the approximate Kapparent value in f denotes that the binding affinity was too high to allow precise affinity determination. n = 2 (f, g); n = 1 (h, k); n = 3 (i, j); additional replicates are provided in the Supplementary Information.
Extended Data Fig. 5 CDK12 contacts residues on DDB1 that are otherwise involved in DCAF binding.
a, Structure of the DDB1(ΔBPB)–(R)-CR8–CDK12 complex. The CDK12 C-terminal extension binds a cleft between the DDB1 BPA and BPC domains (arrow) and adopts an helix–loop–helix (HLH)-like fold. b, Diverse DCAFs bind DDB1 through HLH or HLH-like folds. c, Sequence alignment of identically positioned helices of different HLH domains. d, Overview of protein–protein interaction hotspots. e, Counter-titration of unlabelled wild-type or mutant DDB1 (0–10 μM) into the preassembled DDB1terbium–CR8–CDK12–cyclin KAlexa488 complex (n = 3). f, Counter-titration of unlabelled wild-type or mutant DDB1 (0–10 μM) into the preassembled DDB1terbium–CR8–CDK12–cyclin KAlexa488 complex (n = 3). g–i, Close-up views of DDB1 residues contacted by CDK12 (top) that are otherwise involved in DCAF binding (bottom).
Extended Data Fig. 6 The CDK12 C-terminal extension adopts different conformations.
a, Conformation of the C-terminal extension in the structure of the DDB1(ΔBPB)–CR8–CDK12 complex. b, Structure of CDK12 bound to adenylyl-imidodiphosphate (AMP-PNP) (PDB entry 4CXA) superimposed onto CDK12 in the DDB1(ΔBPB)–CR8–CDK12 complex. c, Titration of CDK12–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium in the presence of 10 μM THZ531, ATP or DMSO (n = 3). d, Structure of CDK12 bound to THZ531 (PDB entry 5ACB) superimposed onto CDK12 in the DDB1(ΔBPB)–CR8–CDK12 complex. e, THZ531-binding pose in the active site of CDK12 as in d. f, Chemical structure of THZ531.
Extended Data Fig. 7 Differences between CDK12 and other CDKs highlight the residues involved in CR8-induced recruitment of DDB1.
a, Sequence alignment of CDK12 and CDK13. b, Sequence alignment of CDK12 and CDK9. c, Multiple sequence alignment of different human CDKs. In a–c, asterisks denote contacts with CR8 and circles indicate contacts with DDB1 (coloured according to DDB1 domains; see Fig. 2). Arrows mark differences at the DDB1–CR8–CDK interface. d, Titration of CDK12–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). ‘No DDB1’ only contains terbium-coupled streptavidin and shows concentration-dependent fluorophore effects. e, Titration of CDK13–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). f, Titration of CDK9–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). g, CUL4NEDD8–RBX1–DDB1 in vitro ubiquitination of cyclin K bound to CDK12, CDK13 or CDK9 (n = 2). h, Titration of CDK12(L1033A/W1036A)–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). i, Titration of CDK12(ΔCTE)–cyclin KAlexa488 (0–3.75 μM) into 50 nM DDB1terbium and 10 μM CR8 or DMSO (n = 3). CDK12(ΔCTE) is a truncated version of CDK12 (amino acids 713–1032).
Extended Data Fig. 8 CDK inhibitors block the CR8-induced degradation of cyclin K.
a, Titration of CDK12–cyclin KAlexa488 into DDB1terbium in the presence of the indicated compounds (all 10 μM) (n = 3). b, NanoBRET of HEK293T cells transfected with NanoLuc-labelled CDK12(713–1052) and HaloTag-labelled DDB1(∆BPB) constructs and treated with the indicated compounds for 2 h. Bars represent the mean (n = 3). c, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells treated with 1 μM CR8 and competitive CDK inhibitor (n = 3).
Extended Data Fig. 9 Cytotoxicity of CR8 analogues does not depend on CRL4 components.
a, Drug sensitivity of HEK293T-Cas9 cells that were treated with different inhibitors for three days (n = 3). b, Drug sensitivity of HEK293T-Cas9 cells that were treated with 100 nM MLN4924 or DMSO in combination with the indicated compound for three days (n = 3). c, Immunoblots of HEK293T-Cas9 cells transfected with control (pRSF91-GFP) or CRBN overexpression (pRSF91-CRBN) vectors (n = 2). d, Immunoblots of HEK293T-Cas9 cells expressing pRSF91-GFP or pRSF91-CRBN and treated with CR8 for three days (n = 2). e, Drug sensitivity of HEK293T-Cas9 cells expressing pRSF91-GFP or pRSF91-CRBN and treated with CR8 for three days (n = 3). f, Immunoblots of HEK293T-Cas9 cells transfected with control (pLX307-Luc) or CRBN overexpression (pLX307-CRBN) vectors (n = 2). g, Flow analysis of cyclin KeGFP degradation in HEK293T-Cas9 cells expressing pLX307-Luc or pLX307-CRBN and treated with CR8 for 2 h (n = 3). h, Drug sensitivity of HEK293T-Cas9 cells expressing sgRNAs targeting DDB1 or luciferase and treated with the indicated inhibitor for three days (n = 3).
Supplementary information
Supplementary Figures
This file contains Supplementary Figures 1-3: 1) Supplementary isothermal titration calorimetry (ITC) data; 2) Uncropped Western blots and SDS-PAGE gels; 3) Gating strategy for flow cytometry.
Supplementary Table 1
This file contains the oligonucleotides used in this study.
Supplementary Data
This file contains 4 Supplementary Data files. It includes: Data for E3 gene-compound pairs identified in bioinformatic screen (n=158); Primary data for validation of 96 E3 gene-compound pairs; Proteome quantification using tandem mass tag spectrometry data treated with 1 µM CR8 (n=1) or DMSO (n=3) (two-sided moderated t-test, n=3); Functional genomics data (guide counts were collapsed to gene-level (n=4 guides/gene; two-sided empirical rank-sum test-statistics)).
Supplementary Data
This file contains the Supplementary Code. It includes 4 files: Code used for bioinformatic screen to identify E3-drug ligase pairs; Code used for validation of 96 E3 gene-compound pairs; Code used for identification of hits in genome wide CR8 resistance screen for single replicate; Code used for identification of hits in CR8 resistance and cyclin K stability screens for multiple replicates.
Rights and permissions
About this article
Cite this article
Słabicki, M., Kozicka, Z., Petzold, G. et al. The CDK inhibitor CR8 acts as a molecular glue degrader that depletes cyclin K. Nature 585, 293–297 (2020). https://doi.org/10.1038/s41586-020-2374-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-020-2374-x
This article is cited by
-
Ubiquitin-specific proximity labeling for the identification of E3 ligase substrates
Nature Chemical Biology (2024)
-
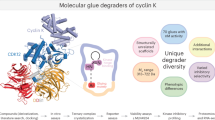
Unraveling the diversity of molecular glue degraders
Nature Chemical Biology (2024)
-
Targeted protein degradation via intramolecular bivalent glues
Nature (2024)
-
The glue degraders
Nature Biotechnology (2024)
-
Recent advances in targeted protein degraders as potential therapeutic agents
Molecular Diversity (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.