Abstract
Alzheimer’s disease is a pervasive neurodegenerative disorder, the molecular complexity of which remains poorly understood. Here, we analysed 80,660 single-nucleus transcriptomes from the prefrontal cortex of 48 individuals with varying degrees of Alzheimer’s disease pathology. Across six major brain cell types, we identified transcriptionally distinct subpopulations, including those associated with pathology and characterized by regulators of myelination, inflammation, and neuron survival. The strongest disease-associated changes appeared early in pathological progression and were highly cell-type specific, whereas genes upregulated at late stages were common across cell types and primarily involved in the global stress response. Notably, we found that female cells were overrepresented in disease-associated subpopulations, and that transcriptional responses were substantially different between sexes in several cell types, including oligodendrocytes. Overall, myelination-related processes were recurrently perturbed in multiple cell types, suggesting that myelination has a key role in Alzheimer’s disease pathophysiology. Our single-cell transcriptomic resource provides a blueprint for interrogating the molecular and cellular basis of Alzheimer’s disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
Data availability
The snRNA-seq data are available on The Rush Alzheimer’s Disease Center (RADC) Research Resource Sharing Hub at https://www.radc.rush.edu/docs/omics.htm (snRNA-seq PFC) or at Synapse (https://www.synapse.org/#!Synapse:syn18485175) under the doi 10.7303/syn18485175. The ROSMAP metadata can be accessed at https://www.synapse.org/#!Synapse:syn3157322. The data are available under controlled use conditions set by human privacy regulations. To access the data, a data use agreement is needed. This registration is in place solely to ensure anonymity of the ROSMAP study participants. A data use agreement can be agreed with either Rush University Medical Center (RUMC) or with SAGE, who maintains Synapse, and can be downloaded from their websites.
Code availability
Code used throughout this study is available upon reasonable request from the corresponding authors.
Change history
17 June 2019
Change history: In this Article, the Acknowledgements section should have included that the work was supported in part by the Cure Alzheimer’s Fund (CAF), and the final NIH grant acknowledged should have been ‘U01MH119509’ instead of ‘RF1AG054012’. In Supplementary Table 2, the column labels ‘early.pathology.mean’ and ‘late.pathology.mean’ were reversed in each worksheet (that is, columns Y and Z). These errors have been corrected online
References
Masters, C. L. et al. Alzheimer’s disease. Nat. Rev. Dis. Primers 1, 15056 (2015).
Hardy, J. & Selkoe, D. J. The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 297, 353–356 (2002).
Braak, H. & Braak, E. Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol. 82, 239–259 (1991).
De Strooper, B. & Karran, E. The cellular phase of Alzheimer’s disease. Cell 164, 603–615 (2016).
Canter, R. G., Penney, J. & Tsai, L.-H. The road to restoring neural circuits for the treatment of Alzheimer’s disease. Nature 539, 187–196 (2016).
Heneka, M. T. et al. Neuroinflammation in Alzheimer’s disease. Lancet Neurol. 14, 388–405 (2015).
Bishop, N. A., Lu, T. & Yankner, B. A. Neural mechanisms of ageing and cognitive decline. Nature 464, 529–535 (2010).
Pimenova, A. A., Raj, T. & Goate, A. M. Untangling genetic risk for Alzheimer’s disease. Biol. Psychiatry 83, 300–310 (2018).
Fisher, D. W., Bennett, D. A. & Dong, H. Sexual dimorphism in predisposition to Alzheimer’s disease. Neurobiol. Aging 70, 308–324 (2018).
Nativio, R. et al. Dysregulation of the epigenetic landscape of normal aging in Alzheimer’s disease. Nat. Neurosci. 21, 497–505 (2018).
Bossers, K. et al. Concerted changes in transcripts in the prefrontal cortex precede neuropathology in Alzheimer’s disease. Brain 133, 3699–3723 (2010).
Zhang, B. et al. Integrated systems approach identifies genetic nodes and networks in late-onset Alzheimer’s disease. Cell 153, 707–720 (2013).
Miller, J. A., Woltjer, R. L., Goodenbour, J. M., Horvath, S. & Geschwind, D. H. Genes and pathways underlying regional and cell type changes in Alzheimer’s disease. Genome Med. 5, 48 (2013).
Gjoneska, E. et al. Conserved epigenomic signals in mice and humans reveal immune basis of Alzheimer’s disease. Nature 518, 365–369 (2015).
Habib, N. et al. Massively parallel single-nucleus RNA-seq with DroNc-seq. Nat. Methods 14, 955–958 (2017).
Lake, B. B. et al. Neuronal subtypes and diversity revealed by single-nucleus RNA sequencing of the human brain. Science 352, 1586–1590 (2016).
Zhong, S. et al. A single-cell RNA-seq survey of the developmental landscape of the human prefrontal cortex. Nature 555, 524–528 (2018).
Lake, B. B. et al. Integrative single-cell analysis of transcriptional and epigenetic states in the human adult brain. Nat. Biotechnol. 36, 70–80 (2018).
Macosko, E. Z. et al. Highly parallel genome-wide expression profiling of individual cells using nanoliter droplets. Cell 161, 1202–1214 (2015).
Bennett, D. A. et al. Religious Orders Study and Rush Memory and Aging Project. J. Alzheimers Dis. 64, S161–S189 (2018).
He, Z. et al. Comprehensive transcriptome analysis of neocortical layers in humans, chimpanzees and macaques. Nat. Neurosci. 20, 886–895 (2017).
Lin, Y.-T. et al. APOE4 causes widespread molecular and cellular alterations associated with Alzheimer’s disease phenotypes in human iPSC-derived brain cell types. Neuron 98, 1141–1154 (2018).
Mathys, H. et al. Temporal tracking of microglia activation in neurodegeneration at single-cell resolution. Cell Reports 21, 366–380 (2017).
Krasemann, S. et al. The TREM2–APOE pathway drives the transcriptional phenotype of dysfunctional microglia in neurodegenerative diseases. Immunity 47, 566–581 (2017).
Keren-Shaul, H. et al. A unique microglia type associated with restricting development of Alzheimer’s disease. Cell 169, 1276–1290 (2017).
Fernandez-Enright, F. & Andrews, J. L. Lingo-1: a novel target in therapy for Alzheimer’s disease? Neural Regen. Res. 11, 88–89 (2016).
Mi, S. et al. LINGO-1 negatively regulates myelination by oligodendrocytes. Nat. Neurosci. 8, 745–751 (2005).
Liang, C. et al. Erbin is required for myelination in regenerated axons after injury. J. Neurosci. 32, 15169–15180 (2012).
Scott, R. et al. Loss of Cntnap2 causes axonal excitability deficits, developmental delay in cortical myelination, and abnormal stereotyped motor behavior. Cereb. Cortex 29, 586–597 (2019).
Poplawski, G. H. D. et al. Adult rat myelin enhances axonal outgrowth from neural stem cells. Sci. Transl. Med. 10, eaal2563 (2018).
Khazaei, M. R. et al. Bex1 is involved in the regeneration of axons after injury. J. Neurochem. 115, 910–920 (2010).
Seiradake, E. et al. Structural basis for cell surface patterning through NetrinG–NGL interactions. EMBO J. 30, 4479–4488 (2011).
Holtzman, D. M., Morris, J. C. & Goate, A. M. Alzheimer’s disease: the challenge of the second century. Sci. Transl. Med. 3, 77sr1 (2011).
Andrade, W. A. et al. Early endosome localization and activity of RasGEF1b, a toll-like receptor-inducible Ras guanine-nucleotide exchange factor. Genes Immun. 11, 447–457 (2010).
Balch, W. E., Morimoto, R. I., Dillin, A. & Kelly, J. W. Adapting proteostasis for disease intervention. Science 319, 916–919 (2008).
Labbadia, J. & Morimoto, R. I. The biology of proteostasis in aging and disease. Annu. Rev. Biochem. 84, 435–464 (2015).
Kohonen, T. The self-organizing map. Proc. IEEE 78, 1464–1480 (1990).
Karch, C. M. & Goate, A. M. Alzheimer’s disease risk genes and mechanisms of disease pathogenesis. Biol. Psychiatry 77, 43–51 (2015).
Davies, G. et al. Study of 300,486 individuals identifies 148 independent genetic loci influencing general cognitive function. Nat. Commun. 9, 2098 (2018).
Blondel, V. D., Guillaume, J.-L., Lambiotte, R. & Lefebvre, E. Fast unfolding of communities in large networks. J. Stat. Mech. 2008, P10008 (2008).
Ousman, S. S. et al. Protective and therapeutic role for αB-crystallin in autoimmune demyelination. Nature 448, 474–479 (2007).
Shin, Y.-J. et al. Clusterin enhances proliferation of primary astrocytes through extracellular signal-regulated kinase activation. Neuroreport 17, 1871–1875 (2006).
Olah, M. et al. A transcriptomic atlas of aged human microglia. Nat. Commun. 9, 539 (2018).
Caso, F. et al. White matter degeneration in atypical Alzheimer disease. Radiology 277, 162–172 (2015).
Ciryam, P. et al. A transcriptional signature of Alzheimer’s disease is associated with a metastable subproteome at risk for aggregation. Proc. Natl Acad. Sci. USA 113, 4753–4758 (2016).
Bennett, D. A. et al. Natural history of mild cognitive impairment in older persons. Neurology 59, 198–205 (2002).
Bennett, D. A. et al. Apolipoprotein E ε4 allele, AD pathology, and the clinical expression of Alzheimer’s disease. Neurology 60, 246–252 (2003).
Bennett, D. A., Schneider, J. A., Wilson, R. S., Bienias, J. L. & Arnold, S. E. Neurofibrillary tangles mediate the association of amyloid load with clinical Alzheimer disease and level of cognitive function. Arch. Neurol. 61, 378–384 (2004).
Bennett, D. A. et al. Neuropathology of older persons without cognitive impairment from two community-based studies. Neurology 66, 1837–1844 (2006).
Bennett, D. A. et al. Decision rules guiding the clinical diagnosis of Alzheimer’s disease in two community-based cohort studies compared to standard practice in a clinic-based cohort study. Neuroepidemiology 27, 169–176 (2006).
Swiech, L. et al. In vivo interrogation of gene function in the mammalian brain using CRISPR–Cas9. Nat. Biotechnol. 33, 102–106 (2015).
Wolf, F. A., Angerer, P. & Theis, F. J. SCANPY: large-scale single-cell gene expression data analysis. Genome Biol. 19, 15 (2018).
Ritchie, M. E. et al. limma powers differential expression analyses for RNA-sequencing and microarray studies. Nucleic Acids Res. 43, e47 (2015).
Wehrens, R. & Buydens, L. M. C. Self- and super-organizing maps in R: the kohonen package. J. Stat. Softw. 21, 1–19 (2007).
Zhou, Y. et al. Metascape provides a biologist-oriented resource for the analysis of systems-level datasets. Nat. Commun. 10, 1523 (2019).
Friston, K. J. et al. Spatial registration and normalization of images. Hum. Brain Mapp. 3, 165–189 (1995).
Griffanti, L. et al. BIANCA (Brain Intensity AbNormality Classification Algorithm): a new tool for automated segmentation of white matter hyperintensities. Neuroimage 141, 191–205 (2016).
Acknowledgements
We thank the study participants and staff of the Rush Alzheimer’s Disease Center; T. F. Andreassen for technical assistance; and S. J. Barker for discussions and comments. This work was supported in part by the Cure Alzheimer’s Fund (CAF), the JBP Foundation and by NIH grants RF1AG054321, RF1AG062377, RF1AG054012, U01NS110453, R01AG062335, and R01AG058002 (L.-H.T.); P30AG10161, R01AG15819, R01AG17917, U01AG46152, and R01AG57473 (D.A.B.); and U01NS110453, R01AG062335, R01AG058002, R01MH109978, R01HG008155, RF1AG054012, RF1AG062377, and U01MH119509 (M.K.). H.M. was supported by an Early Postdoc Mobility fellowship from the Swiss National Science Foundation (P2BSP3_151885).
Reviewer information
Nature thanks Hongjun Song and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
This study was designed by H.M., J.D.-V., D.A.B., M.K., and L.-H.T., and directed and coordinated by M.K. and L.-H.T. H.M., Z.P., M.M., F.A., X.J., and A.J.M. performed the experiments. M.M. performed the RNAscope experiment under the supervision of B.P.H. H.M. and J.D.-V. performed the bioinformatics analysis with help from F.G., S.M., and L.H. H.M., J.D.-V., J.Z.Y., R.M.R., D.A.B., M.K., and L.-H.T. wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Pathological status verification and physical integrity of isolated neuronal nuclei.
a, Immunohistochemistry with anti-β-amyloid antibody (D54D2, yellow) in the grey matter of Brodmann area 10 of no-pathology and AD-pathology individuals. b, Quantification of the β-amyloid immunostaining in a. Data are mean ± s.e.m.; *P = 0.030 (Student’s two-tailed t-test). c, High-resolution confocal microscopy images of neuronal nuclei isolated from no-pathology and AD-pathology individuals and stained with Hoechst. The experiment was performed once.
Extended Data Fig. 2 snRNA-seq profiling and cell-type characterization.
a, Study cohort and sample preparation. b, Clustering analysis workflow. c, Two-dimensional t-SNE projection of all annotated cells (n = 75,060 from 24 pathology and 24 no-pathology individuals). d, Correlation matrix (Pearson correlation coefficient; pcc) of the average expression profiles by cell type for each individual.
Extended Data Fig. 3 Consistency of cells of the same type across individuals.
a, Expression of known cell-type marker genes for each cell type. b, Left, expression of known cell-type marker genes in each cluster; right, fraction of cells in each cluster that express each marker gene. Vertical dashed blue line represents a scale bar referencing 0.5. c, Overrepresentation analysis (hypergeometric test) within each of the pre-cluster marker sets (rows) of genes previously identified as markers18 (columns, left; n = 1,729 total genes) and genes previously identified as markers of cortical layers21 (columns, right; n = 3,400 total genes). d, Fraction of cells of each type isolated across all (n = 48), no-pathology (n = 24), and AD-pathology (n = 24) individuals. e, Fraction of cells of each type isolated from each individual (columns; n = 48).
Extended Data Fig. 4 Expression values and validation of top DEGs.
a, Mean expression values of genes across the nuclei isolated from each individual. Each point represents one individual. DEGs were classified as low, mid, or high in expression, based on their median expression level across the cells of the corresponding cell type. Groups were defined based on k-means clustering (k = 3). The top three genes for each group (low-, mid-, and high-expression levels) and for each cell type are shown. For oligodendrocyte precursor cells and microglia, only one and two genes, respectively, were classified within the high-expression group. ATPIF1 is also known as ATP5IF1, NGFRAP1is also known as BEX3, TMEM2 is also known as CEMIP2, and ERBB2IP is also known as ERBIN. b, Left, RNA in situ hybridization (RNAscope) with probes that detect the excitatory neuron marker SLC17A7 (red) and NTNG1 (blue) in the grey matter of Brodmann area 10 of a no-pathology and an AD-pathology individual. The tissue was counterstained with haematoxylin. Right, quantification of RNA in situ hybridization on Brodmann area 10 tissue sections. Data are mean ± s.e.m.; *P = 0.047 (Student’s two-tailed t-test). n = 4 no-pathology and n = 4 AD-pathology individuals; n = 5 or 6 images per individual.
Extended Data Fig. 5 Overlap of genes that are altered in the progression of AD pathology.
Quantification of the overlap (Jaccard coefficient) between pairs of gene sets identified as differentially expressed in each of the major cell types when comparing cells isolated from AD-pathology individuals with cells isolated from no-pathology individuals, and combinations of early- and late-pathology individuals.
Extended Data Fig. 6 Cell-type-specific and phenotype-specific gene–trait correlation analysis.
a–e, SOM generated from transcriptome-wide gene-expression correlation of each gene with neuropathological signatures of AD. Genes with similar correlation patterns are mapped to the same SOM unit and similar units group close together. SOM grid layout is common and built jointly across all phenotypes and all cell types. Colour indicates the average Spearman’s rank correlation for genes in each unit. f, Selected SOM territories (M1–M10). g, Overlap (one-sided Fisher’s exact test) between gene–trait correlation-module genes (n = 1,472 genes (M3), n = 70 (M6), n = 80 (M7)) and AD GWAS-risk genes (top; n = 28 genes), as well as genes associated with general cognitive function (bottom; n = 709 genes). The P values have been adjusted for multiple hypothesis testing; −log10(Bonferroni-corrected P values) are shown.
Extended Data Fig. 7 Overrepresentation analyses for cells in sub-clusters.
a, Cell composition of each identified sub-cluster (rows) across individuals (columns). Bars represent the fraction of cells corresponding to each individual. Bar colour indicates whether the corresponding value exceeds (black) or does not exceed (white) the average value measured across all the entries in the row. b, Overrepresentation analysis (hypergeometric test) within each pre-cluster (columns) of cells isolated from each individual (rows). c, Overrepresentation analysis within each sub-cluster of cells isolated from individuals with different values of discrete clinico-pathological variables (overall amyloid level, Braak stage, CERAD score (ceradsc), NIA–Reagan score (niareagansc), clinical consensus diagnosis of cognitive status at the time of death (cogdx), and sex). The scale bars on the right indicate the significance of the overrepresentation (hypergeometric test, −log10(P value), z-scaled, FDR multiple-testing correction). For quantitative variables, enrichment was computed based on an estimated z-score quantifying the deviation from random expected values using resampling (Methods). The quantitative variables considered were neuritic plaque count, neurofibrillary tangle burden, tangle density, overall amyloid level, and global cognitive function. For a detailed description of clinico-pathological variables, see Supplementary Information. d, Overrepresentation analysis (hypergeometric test) similar to that in a, but computed only across cells isolated from randomly chosen female and male individuals for AD-pathology and no-pathology groups (Methods). Scores represent aggregated P values (meta-p values, meanp method, metap R package) computed across 100 random realizations. Only scores with a FDR < 0.01 (correction across traits × subpopulations) are plotted.
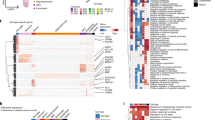
Extended Data Fig. 8 Cell-type subpopulations.
Cells from sub-clusters enriched (red) or depleted (blue) with cells for individuals with AD pathology and cognitive decline shown using t-SNE for major cell types (Ast1 n = 1,134, Ast0 n = 1,728, Oli0 n = 8,310, Oli1 n = 8,032, Ex4 n = 3,198, Ex6 n = 2,757, In0 n = 2,368, In2 n = 984, Opc0 n = 1,589, Opc1 n = 976, Mic1 n = 509, and Mic2 n = 169 cells). Left, corresponding marker genes (font proportional to enrichment level); right, enriched Gene Ontology terms. Gene Ontology enrichment was based on FDR-corrected cumulative hypergeometric P values, with P value-ranked gene-marker lists (FDR < 0.01, log2(mean gene expression across cells in sub-cluster/mean gene expression across cells in other sub-clusters) > 0.5, two-sided Wilcoxon rank-sum test) used as input (Ex4 n = 783, Ex6 n = 2,438, In0 n = 1,702, In2 n = 350, Ast1 n = 574, Ast0 n = 73, Oli0 n = 227, Oli1 n = 73, Opc0 n = 19, Opc1 n = 536, Mic1 n = 487, and Mic2 n = 646).
Extended Data Fig. 9 Immunohistochemistry of subpopulation markers in oligodendrocyte lineage cells and microglia.
a, Oligodendrocyte lineage cell subpopulation marked by alpha B-crystallin (CRYAB). Immunohistochemistry with anti-OLIG2 (red) and anti-CRYAB (green) antibodies in the white matter of Brodmann area 10 of a no-pathology and an AD-pathology individual (scale bars, 20 μm). A selected area of these images is shown in Fig. 3g. The experiment was performed once. b, Oligodendrocyte lineage cell subpopulation marked by quinoid dihydropteridine reductase (QDPR). Immunohistochemistry with anti-OLIG2 (red) and anti-QDPR (green) antibodies in the white matter of Brodmann area 10 of a no-pathology and an AD-pathology individual (scale bars, 20 μm). A selected area of these images is shown in Fig. 3h. The experiment was performed once. c, Immunohistochemistry with anti-IBA1 (red) and anti-MHC class II (green) antibodies in the white matter of Brodmann area 10 of a no-pathology and an AD-pathology individual (scale bars, 20 μm). The experiment was performed once. d, Overlap (one-sided Fisher’s exact test) between Mic1 marker genes and genes upregulated in mouse disease-associated microglia (left), in mouse late-response microglia (middle), and in aged human microglia (right).
Extended Data Fig. 10 Sex comparisons in pathology, gene expression, and white matter.
a, Quantitative clinico-pathological measurement comparison between male and female individuals (n = 24 female and n = 24 male individuals; two-sided Wilcoxon rank-sum test). Violin plots are centred around the median with interquartile ranges, and the shape represents individual distribution. The quantitative clinico-pathological variables considered were overall amyloid level, neuritic plaque burden, neurofibrillary tangle burden, tangle density, global cognitive function, and global AD pathology burden. b, Violin plots showing aggregate expression levels (z-scaled) across excitatory neurons in female (red) versus male (blue) individuals (n = 12 each) of the top 10 marker genes of the AD-associated Ex4 subpopulation of excitatory neurons. c, Hierarchical clustering of pathology-affected individuals (columns) based on average expression level (colour) of the top 10 marker genes (rows) of the AD-enriched Ex4 subpopulation of excitatory neurons for female versus male individuals. d, e, Statistical comparison of in vivo brain MRI imaging from ROSMAP cohorts. d, Intracranial volume-normalized WMH (wmh.icv) measures for female (n = 399) and male (n = 106) individuals and high-cognition (n = 252 female and n = 63 male individuals) and low-cognition (n = 147 female and n = 43 male individuals) groups. Groups were defined based on whether subjects had an overall cognition score lower (low.cog, z-score < 0) or higher (high.cog, z-score > 0) than the average. Mean rank-difference values between cognition groups were compared using the two-sided Wilcoxon rank-sum test. e, Statistical estimation of significant difference in WMH between low-cognition and high-cognition groups in females, and between low-cognition and high-cognition groups in males, assessed by bootstrap point and 95% confidence interval estimation of the effect size (mean difference) between groups. Bootstrap resampling was performed by resampling n = 40 observations per group 1,000 times. Horizontal line highlights zero difference. The positive effect-size points and confidence interval estimates do not overlap the zero line in the female group, which provides statistical evidence of an increment in WMH (wmh.icv) in the low-cognition group relative to the high-cognition group in females but not in males.
Supplementary information
Supplementary Information
This text file provides descriptions from the Rush Alzheimer’s Disease Center codebook of the clinico-pathological variables considered in this study.
Supplementary Table 1
Summary of individuals profiled with snRNA-seq. This table provides the main epidemiological and pathological characteristics of the participants of the Religious Order Study (ROS) cohort selected for the single-nucleus RNA-sequencing analysis (n=28).
Supplementary Table 2
Cell-type specific differential expression analyses. This table provides cell-type specific snRNA-seq differential expression results, comparisons between snRNA-seq differential expression models, and with bulk RNA-seq data (Fig. 1 and Fig. 2).
Supplementary Table 3
Clinico-pathological variables. This table provides clinico-pathological variables of the individuals profiled in the study, including those used to subdivide the 24 pathology individuals into early-pathology and late-pathology groups (Fig. 2a).
Supplementary Table 4
Gene-trait correlation modules. This table provides the identified gene-trait correlation modules and their overlap with AD risk genes and genes associated with cognitive function (Extended Data Fig. S6d).
Supplementary Table 5
Cell-type sub-population trait association analysis. This table provides FDR-corrected P-values measuring the overrepresentation of cells from individuals of a given phenotypic trait (columns) within cell subclusters (rows) (Extended Data Fig. S7d).
Supplementary Table 6
Cell-type sub-population signature genes. This table provides genes detected as significantly over-expressed in a specific subcluster relative to the other subclusters of the same cell-type.
Supplementary Table 7
Comparison with disease-associated microglia in mouse. This table provides the comparison between the gene signature of human AD-associated microglia subpopulation (Mic1) and existing gene signatures of disease-associated microglia states in mouse, and with the aged human microglia.
Supplementary Table 8
Female and male gene-trait correlation statistics. This table provides statistical descriptions of individual-level gene-trait correlations computed independently for female and for male individuals (Fig. 4).
Rights and permissions
About this article
Cite this article
Mathys, H., Davila-Velderrain, J., Peng, Z. et al. Single-cell transcriptomic analysis of Alzheimer’s disease. Nature 570, 332–337 (2019). https://doi.org/10.1038/s41586-019-1195-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-019-1195-2
This article is cited by
-
PICALO: principal interaction component analysis for the identification of discrete technical, cell-type, and environmental factors that mediate eQTLs
Genome Biology (2024)
-
Hotspots and trends of microglia in Alzheimer's disease: a bibliometric analysis during 2000–2022
European Journal of Medical Research (2024)
-
Identification of female-enriched and disease-associated microglia (FDAMic) contributes to sexual dimorphism in late-onset Alzheimer’s disease
Journal of Neuroinflammation (2024)
-
The interaction between ageing and Alzheimer's disease: insights from the hallmarks of ageing
Translational Neurodegeneration (2024)
-
Intestinal cell diversity and treatment responses in a parasitic nematode at single cell resolution
BMC Genomics (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.