Abstract
The airways of the lung are the primary sites of disease in asthma and cystic fibrosis. Here we study the cellular composition and hierarchy of the mouse tracheal epithelium by single-cell RNA-sequencing (scRNA-seq) and in vivo lineage tracing. We identify a rare cell type, the Foxi1+ pulmonary ionocyte; functional variations in club cells based on their location; a distinct cell type in high turnover squamous epithelial structures that we term ‘hillocks’; and disease-relevant subsets of tuft and goblet cells. We developed ‘pulse-seq’, combining scRNA-seq and lineage tracing, to show that tuft, neuroendocrine and ionocyte cells are continually and directly replenished by basal progenitor cells. Ionocytes are the major source of transcripts of the cystic fibrosis transmembrane conductance regulator in both mouse (Cftr) and human (CFTR). Knockout of Foxi1 in mouse ionocytes causes loss of Cftr expression and disrupts airway fluid and mucus physiology, phenotypes that are characteristic of cystic fibrosis. By associating cell-type-specific expression programs with key disease genes, we establish a new cellular narrative for airways disease.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Rock, J. R. et al. Basal cells as stem cells of the mouse trachea and human airway epithelium. Proc. Natl Acad. Sci. USA 106, 12771–12775 (2009).
Lump, A. Nunn’s Applied Respiratory Physiology, 8th edn (Elsevier, Edinburgh, 2016)
Ardini-Poleske, M. E. et al. LungMAP: The Molecular Atlas of Lung Development Program. Am. J. Physiol. Lung Cell. Mol. Physiol. 313, L733–L740 (2017).
Treutlein, B. et al. Reconstructing lineage hierarchies of the distal lung epithelium using single-cell RNA-seq. Nature 509, 371–375 (2014).
Nabhan, A. N., Brownfield, D. G., Harbury, P. B., Krasnow, M. A. & Desai, T. J. Single-cell Wnt signaling niches maintain stemness of alveolar type 2 cells. Science 359, 1118–1123 (2018).
Zepp, J. A. et al. Distinct mesenchymal lineages and niches promote epithelial self-renewal and myofibrogenesis in the lung. Cell 170, 1134–1148 (2017).
Plasschaert, L. W. et al. A single-cell atlas of the airway epithelium reveals the CFTR-rich pulmonary ionocyte. Nature https://doi.org/10.1038/s41586-018-0394-6 (2018).
Quigley, I. K., Stubbs, J. L. & Kintner, C. Specification of ion transport cells in the Xenopus larval skin. Development 138, 705–714 (2011).
Esaki, M. et al. Mechanism of development of ionocytes rich in vacuolar-type H+-ATPase in the skin of zebrafish larvae. Dev. Biol. 329, 116–129 (2009).
Pardo-Saganta, A. et al. Parent stem cells can serve as niches for their daughter cells. Nature 523, 597–601 (2015).
Tsao, P.-N. et al. Epithelial Notch signaling regulates lung alveolar morphogenesis and airway epithelial integrity. Proc. Natl Acad. Sci. USA 113, 8242–8247 (2016).
Sriuranpong, V. et al. Notch signaling induces rapid degradation of achaete-scute homolog 1. Mol. Cell. Biol. 22, 3129–3139 (2002).
Moriyama, M. et al. Multiple roles of Notch signaling in the regulation of epidermal development. Dev. Cell 14, 594–604 (2008).
Verzi, M. P., Khan, A. H., Ito, S. & Shivdasani, R. A. Transcription factor Foxq1 controls mucin gene expression and granule content in mouse stomach surface mucous cells. Gastroenterology 135, 591–600 (2008).
Li, M. J. et al. GWASdb v2: an update database for human genetic variants identified by genome-wide association studies. Nucleic Acids Res. 44, D869–D876 (2016).
Bochkov, Y. A. et al. Cadherin-related family member 3, a childhood asthma susceptibility gene product, mediates rhinovirus C binding and replication. Proc. Natl Acad. Sci. USA 112, 5485–5490 (2015).
Bansal, G., Xie, Z., Rao, S., Nocka, K. H. & Druey, K. M. Suppression of immunoglobulin E-mediated allergic responses by regulator of G protein signaling 13. Nat. Immunol. 9, 73–80 (2008).
Pardo-Saganta, A., Law, B. M., Gonzalez-Celeiro, M., Vinarsky, V. & Rajagopal, J. Ciliated cells of pseudostratified airway epithelium do not become mucous cells after ovalbumin challenge. Am. J. Respir. Cell Mol. Biol. 48, 364–373 (2013).
Roy, M. G. et al. Muc5b is required for airway defence. Nature 505, 412–416 (2014).
Danahay, H. et al. Notch2 is required for inflammatory cytokine-driven goblet cell metaplasia in the lung. Cell Reports 10, 239–252 (2015).
Munitz, A., Brandt, E. B., Mingler, M., Finkelman, F. D. & Rothenberg, M. E. Distinct roles for IL-13 and IL-4 via IL-13 receptor α1 and the type II IL-4 receptor in asthma pathogenesis. Proc. Natl Acad. Sci. USA 105, 7240–7245 (2008).
Watson, J. K. et al. Clonal dynamics reveal two distinct populations of basal cells in slow-turnover airway epithelium. Cell Reports 12, 90–101 (2015).
Ng, F. S. P. et al. Annexin-1-deficient mice exhibit spontaneous airway hyperresponsiveness and exacerbated allergen-specific antibody responses in a mouse model of asthma. Clin. Exp. Allergy J. Br. Soc. Allergy Clin. Immunol. 41, 1793–1803 (2011).
Haber, A. L. et al. A single-cell survey of the small intestinal epithelium. Nature 551, 333–339 (2017).
Dixon, R. A. et al. Requirement of a 5-lipoxygenase-activating protein for leukotriene synthesis. Nature 343, 282–284 (1990).
Hase, K. et al. Uptake through glycoprotein 2 of FimH+ bacteria by M cells initiates mucosal immune response. Nature 462, 226–230 (2009).
Miklavc, P., Thompson, K. E. & Frick, M. A new role for P2X4 receptors as modulators of lung surfactant secretion. Front. Cell. Neurosci. 7, 171 (2013).
Bergström, J. H. et al. Gram-positive bacteria are held at a distance in the colon mucus by the lectin-like protein ZG16. Proc. Natl Acad. Sci. USA 113, 13833–13838 (2016).
Vidarsson, H. et al. The forkhead transcription factor Foxi1 is a master regulator of vacuolar H-ATPase proton pump subunits in the inner ear, kidney and epididymis. PLoS ONE 4, e4471 (2009).
Jonz, M. G. & Nurse, C. A. Epithelial mitochondria-rich cells and associated innervation in adult and developing zebrafish. J. Comp. Neurol. 497, 817–832 (2006).
Hoegger, M. J. et al. Impaired mucus detachment disrupts mucociliary transport in a piglet model of cystic fibrosis. Science 345, 818–822 (2014).
Engelhardt, J. F. et al. Submucosal glands are the predominant site of CFTR expression in the human bronchus. Nat. Genet. 2, 240–248 (1992).
Py, B. F. et al. Cochlin produced by follicular dendritic cells promotes antibacterial innate immunity. Immunity 38, 1063–1072 (2013).
Birket, S. E. et al. A functional anatomic defect of the cystic fibrosis airway. Am. J. Respir. Crit. Care Med. 190, 421–432 (2014).
Birket, S. E. et al. Development of an airway mucus defect in the cystic fibrosis rat. JCI Insight 3, e97199 (2018).
Tang, X. X. et al. Acidic pH increases airway surface liquid viscosity in cystic fibrosis. J. Clin. Invest. 126, 879–891 (2016).
Liu, L. et al. An autoregulatory mechanism governing mucociliary transport is sensitive to mucus load. Am. J. Respir. Cell Mol. Biol. 51, 485–493 (2014).
Shah, V. S. et al. Airway acidification initiates host defense abnormalities in cystic fibrosis mice. Science 351, 503–507 (2016).
Tarran, R. et al. Regulation of murine airway surface liquid volume by CFTR and Ca2+-activated Cl− conductances. J. Gen. Physiol. 120, 407–418 (2002).
Liu, X., Yan, Z., Luo, M. & Engelhardt, J. F. Species-specific differences in mouse and human airway epithelial biology of recombinant adeno-associated virus transduction. Am. J. Respir. Cell Mol. Biol. 34, 56–64 (2006).
Sun, X. et al. Disease phenotype of a ferret CFTR-knockout model of cystic fibrosis. J. Clin. Invest. 120, 3149–3160 (2010).
McCarron, A., Donnelley, M. & Parsons, D. Airway disease phenotypes in animal models of cystic fibrosis. Respir. Res. 19, 54 (2018).
Ostrowski, L. E. et al. Expression of CFTR from a ciliated cell-specific promoter is ineffective at correcting nasal potential difference in CF mice. Gene Ther. 14, 1492–1501 (2007).
Regev, A. et al. Science Forum: The Human Cell Atlas. eLife 6, e27041 (2017).
Rawlins, E. L. et al. The role of Scgb1a1+ Clara cells in the long-term maintenance and repair of lung airway, but not alveolar, epithelium. Cell Stem Cell 4, 525–534 (2009).
Salic, A. & Mitchison, T. J. A chemical method for fast and sensitive detection of DNA synthesis in vivo. P roc. Natl Acad. Sci. USA 105, 2415–2420 (2008).
Picelli, S. et al. Full-length RNA-seq from single cells using Smart-seq2. Nat. Protoc. 9, 171–181 (2014).
Liu, L. et al. Method for quantitative study of airway functional microanatomy using micro-optical coherence tomography. PLoS ONE 8, e54473 (2013).
Schneider, C. A., Rasband, W. S. & Eliceiri, K. W. NIH Image to ImageJ: 25 years of image analysis. Nat. Methods 9, 671–675 (2012).
Birket, S. E. et al. Combination therapy with cystic fibrosis transmembrane conductance regulator modulators augment the airway functional microanatomy. Am. J. Physiol. Lung Cell. Mol. Physiol. 310, L928–L939 (2016).
Mou, H. et al. Dual SMAD signaling inhibition enables long-term expansion of diverse epithelial basal cells. Cell Stem Cell 19, 217–231 (2016).
Konermann, S. et al. Genome-scale transcriptional activation by an engineered CRISPR–Cas9 complex. Nature 517, 583–588 (2015).
Yan, Z. et al. Optimization of recombinant adeno-associated virus-mediated expression for large transgenes, using a synthetic promoter and tandem array enhancers. Hum. Gene Ther. 26, 334–346 (2015).
Brennecke, P. et al. Accounting for technical noise in single-cell RNA-seq experiments. Nat. Methods 10, 1093–1095 (2013).
Johnson, W. E., Li, C. & Rabinovic, A. Adjusting batch effects in microarray expression data using empirical Bayes methods. Biostatistics 8, 118–127 (2007).
Leek, J. T., Johnson, W. E., Parker, H. S., Jaffe, A. E. & Storey, J. D. The sva package for removing batch effects and other unwanted variation in high-throughput experiments. Bioinformatics 28, 882–883 (2012).
Langmead, B., Trapnell, C., Pop, M. & Salzberg, S. L. Ultrafast and memory-efficient alignment of short DNA sequences to the human genome. Genome Biol. 10, R25 (2009).
Li, B. & Dewey, C. N. RSEM: accurate transcript quantification from RNA-seq data with or without a reference genome. BMC Bioinformatics 12, 323 (2011).
Buja, A. & Eyuboglu, N. Remarks on parallel analysis. Multivariate Behav. Res. 27, 509–540 (1992).
Van Der Maaten, L. Accelerating t-SNE using tree-based algorithms. J. Mach. Learn. Res. 15, 3221–3245 (2014).
van der Maaten, L. & Hinton, G. Visualizing Data using t-SNE. J. Mach. Learn. Res. 9, 2579–2605 (2008).
Rosvall, M. & Bergstrom, C. T. Maps of random walks on complex networks reveal community structure. Proc. Natl Acad. Sci. USA 105, 1118–1123 (2008).
Levine, J. H. et al. Data-driven phenotypic dissection of AML reveals progenitor-like cells that correlate with prognosis. Cell 162, 184–197 (2015).
Shekhar, K. et al. Comprehensive classification of retinal bipolar neurons by single-cell transcriptomics. Cell 166, 1308–1323 (2016).
fgsea: Fast Gene Set Enrichment Analysis. (Computer Technologies Laboratory, 2018).
Coifman, R. R. et al. Geometric diffusions as a tool for harmonic analysis and structure definition of data: multiscale methods. Proc. Natl Acad. Sci. USA 102, 7432–7437 (2005).
Zhang, H.-M. et al. AnimalTFDB: a comprehensive animal transcription factor database. Nucleic Acids Res. 40, D144–D149 (2012).
Young, M. D., Wakefield, M. J., Smyth, G. K. & Oshlack, A. Gene ontology analysis for RNA-seq: accounting for selection bias. Genome Biol. 11, R14 (2010).
Liberzon, A. et al. Molecular signatures database (MSigDB) 3.0. Bioinformatics 27, 1739–1740 (2011).
Haghverdi, L., Buettner, F. & Theis, F. J. Diffusion maps for high-dimensional single-cell analysis of differentiation data. Bioinformatics 31, 2989–2998 (2015).
Buettner, F. et al. Computational analysis of cell-to-cell heterogeneity in single-cell RNA-sequencing data reveals hidden subpopulations of cells. Nat. Biotechnol. 33, 155–160 (2015).
Gelman, A & Hill, J. Data Analysis Using Regression and Multilevel/hierarchical Models (Cambridge Univ. Press, New York, 2007).
Schwarzer, G et al. (eds) Meta-Analysis with R (Springer, New York, 2015).
Koenker, R. & Hallock, K. F. Quantile regression. J. Econ. Perspect. 15, 143–156 (2001).
Ester, M., Kriegel, H.-P., Sander, J. & Xu, X. A density-based algorithm for discovering clusters in large spatial databases with noise. In Proc. of the 2nd International Conference on Knowledge Discovery and Data Mining (Simoudis E. et al. eds) 226–231 (AAAI, 1996).
Finak, G. et al. MAST: a flexible statistical framework for assessing transcriptional changes and characterizing heterogeneity in single-cell RNA sequencing data. Genome Biol. 16, 278 (2015).
Benjamini, Y. & Hochberg, Y. 1995. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J. R. Stat. Soc. Ser. C 57, 289–300.
Acknowledgements
We thank L. Gaffney for help with figure preparation, P. Oyem for assistance with electrophysiological assays, the New England Organ Bank for facilitating the acquisition of donor lungs, and the HSCI Flow Cytometry Core and CNY Flow Cytometry Core facilities. This work was supported by the Klarman Cell Observatory at the Broad Institute (A.R. and J.R.), the Manton Foundation (A.R.), HHMI (A.R. and J.R.), New York Stem Cell Foundation (J.R.), NIH-NHLBI (J.R.), the Ludwig Cancer Institute at Harvard (J.R.), and the Harvard Stem Cell Institute (J.R.). M.B. was supported by a postdoctoral fellowship from the Human Frontiers Science Program. D.T.M. was supported by a predoctoral fellowship from NIH-NHLBI 1F31HL136128-01. P.R.T. is a Whitehead Scholar and was supported by a career development award from NHLBI/NIH (4R00HL127181) and funds from Regeneration NeXT Initiative at Duke University. S.M.R. was supported by NIH P30 DK072482 and R35 HL135816. J.F.E. was supported by P01 HL051670, R24 HL123482 and R01 DK047967. J.R. is a MGH Maroni Research Scholar, a Harrington Investigator of the NYSCF and HHMI Faculty Scholar.
Reviewer information
Nature thanks I. Amit and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
D.T.M., A.L.H., M.B., A.R. and J.R. conceived the study; J.R. and A.R. supervised research; A.L.H. designed and performed computational analysis; D.T.M. designed, carried out and analysed experiments with V.V., B.L., S.C., J.V. and P.R.T.; M.B. advised on experimental design and performed mouse single-cell experiments with N.R., G.B., L.N. and D.D.; H.B. and M.M. provided mouse electrophysiology data; S.B., H.M.L., G.J.T. and S.M.R. performed and interpreted μOCT experiments; S.B. performed and interpreted pH experiments. F.Y. and J.F.E. performed and interpreted ferret expression and electrophysiology data; A.T., A.W., M.Sl., J.W. and O.R.-R. contributed human single-cell data and analysis; H.M. assisted with cell culture. M.Sh. previously observed Krt13+ cells arranged as hillocks. D.T.M., A.L.H., A.R. and J.R. wrote the manuscript with input from all authors.
Corresponding authors
Ethics declarations
Competing interests
A.R. is a member of the SAB for Thermo Fisher Scientific, Syros Pharmaceuticals and Driver Group, and a founder of Celsius Therapeutics. D.T.M., A.L.H., M.B., O.R.-R., A.R. and J.R. are co-inventors on PCT/US2018/027337 filed by the Broad Institute relating to innovative advances in epithelial hierarchy and ionocytes described in this manuscript.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Identifying tracheal epithelial cell types in 3′ scRNA-seq.
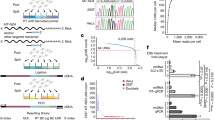
a, Quality metrics for the initial droplet-based 3′ scRNA-seq data. Distributions of the number of reads per cell (left), the number of the genes detected with non-zero transcript counts per cell (centre), and the fraction of reads mapping to the mm10 transcriptome per cell (right). Dashed line, median; blue line, kernel density estimate. b, Cell type clusters are composed of cells from multiple biological replicates. Fraction of cells in each cluster that originate from a given biological replicate (n = 6 mice). Post hoc annotation and number of cells are indicated above each pie chart. All biological replicates contribute to all clusters (except for wild-type mouse 1, which did not contain any of the very rare ionocytes (0.39% of all epithelial cells)), and no significant batch effect was observed. c, Reproducibility between biological replicates. Average gene expression values (log2(TPM+1)) across all cells of two representative 3′ scRNA-seq replicate experiments (r = Pearson correlation coefficient). Blue shading, gene (point) density. d, Post hoc cluster interpretation based on the expression of known cell type markers. t-SNE of 7,193 scRNA-seq profiles (points), coloured by cluster assignment (top left), by expression (log2(TPM+1)) of single marker genes, or by mean expression of several marker genes4 for a particular cell type. e, Cell type clusters. Pearson correlation coefficients (r, colour bar) between every pair of 7,193 cells (rows and columns) ordered by cluster assignment. Inset (right), zoom of 288 cells from the rare types. f, Gene signatures. Relative expression level (row-wise Z score of log2(TPM+1) expression values) of cell-type-specific genes (rows) in each epithelial cell (columns). Large clusters (basal, club) are down-sampled to 500 cells.
Extended Data Fig. 2 Identifying tracheal epithelial cell types in full-length scRNA-seq.
a, Quality metrics for full-length, plate-based scRNA-seq data. Distributions of the number of reads per cell (left), the number of the genes detected with non-zero transcript counts per cell (centre), and the fraction of reads mapping to the mm10 transcriptome per cell (right). b, c, High reproducibility between plate-based scRNA-seq data from biological replicates of tracheal epithelial cells. Average expression values (log2(TPM+1)) in two representative full-length scRNA-seq replicate experiments (left) and in the average of a full-length scRNA-seq dataset (right) and a population control (right) for cells extracted from proximal (b) and distal (c) mouse trachea. Blue shading: density of genes (points); r = Pearson correlation coefficient. d, Post hoc cluster annotation by the expression of known cell-type markers. t-SNE of 301 scRNA-seq profiles (points) coloured by region of origin (top left), cluster assignment (top, second from left), or, in the remaining plots, the expression level (log2(TPM+1)) of single marker genes or the mean expression of several marker genes for a particular cell type. All clusters are populated by cells from both proximal and distal epithelium except rare neuroendocrine cells, which were only detected in proximal experiments (top left).
Extended Data Fig. 3 High-confidence consensus cell type markers, and cell-type-specific expression of asthma-associated genes.
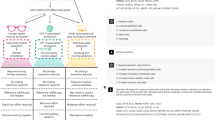
a, Cell type clusters in full-length plate-based scRNA-seq data. Cell–cell Pearson correlation coefficient (r) between all 301 cells (individual rows and columns) ordered by cluster assignment (as in Extended Data Fig. 2d). Right, magnified view of 17 cells (black border on left) from the rare types. b, High confidence consensus markers. Relative expression level (row-wise Z score of mean log2(TPM+1)) of consensus marker genes (rows, FDR <0.01 in both 3′-droplet and full-length plate-based scRNA-seq datasets; LRT) for each cell type (flanking colour bar) across 7,193 cells in the 3′ droplet data (columns, left) and the 301 cells in the plate-based dataset (columns, right). Top 15 markers shown, complete sets are in Extended Data Fig. 1f, Supplementary Table 3. c, Cluster-specific transcription factors in 3′ scRNA-seq data. Mean relative expression (row-wise Z score of mean log2(TPM+1), colour bar) of the top transcription factors (rows) that are enriched (FDR <0.01, LRT, two-sided) in cells (columns) of each cluster. d–f, Cell-type-specific expression of genes associated with asthma by GWAS. d, Relative expression (Z score of mean log2(TPM+1)) of genes that are associated with asthma in GWAS and enriched (FDR <0.01, LRT) for cell-type-specific expression in our 3′ scRNA-seq data. e, The significance (−log10(FDR), Fisher’s combined P value, LRT) and effect size (point size, mean log2(fold-change)) of cell-type-specific expression and its genetic association strength from GWAS15 for each gene from d. f, Distribution of expression levels (log2(TPM+1)) in the cells in each cluster (x axis, colour legend) for two asthma GWAS genes: Cdhr3 (top; specific to ciliated cells) and Rgs13 (bottom; specific to tuft cells) FDRs, LRT.
Extended Data Fig. 4 Krt13+ progenitors express a unique set of markers distinct from mature club cells.
a, Proximal versus distal specific club cell expression. Relative expression level (row-wise Z score, colour bar) for genes (rows) enriched in proximal and distal tracheal club cells (FDR <0.05, LRT) in the full-length scRNA-seq data. b, Distal epithelia differentiate into mucous metaplasia. Goblet cell quantification (ln(Muc5ac+/EGFP+ ciliated cells)) in Foxj1-EGFP mice (n = 6, dots) in each of four conditions in (Fig. 2a). P values, Tukey’s HSD test; black bars, mean; error bars, 95% CI. c, Krt8 does not distinguish pseudostratified club cell development from hillock-associated club cell development. Diffusion map embedding of 6,905 cells (as in Fig. 2b) coloured either by their Krt13+ hillock membership (left, green), or by expression (log2(TPM+1)) of specific genes (all other panels). d, Immunostaining of hillock strata. Left: Krt13+ (green) and Trp63+ (magenta) basal (solid outline) and suprabasal (dashed outline) cells. Right: Krt13+ (green) and Scgb1a1+ (magenta, solid outline) luminal cells. Representative immunostaining from 3 mice. e, f, Krt13+ hillock cells are highly proliferative. e, Co-stain of EdU (magenta) and Krt13 (green), representative of n = 4 mice. f, Fraction of EdU+ epithelial cells in hillock (mean, 7.7%, 95% CI [4.8–10.5%]) and non-hillock (mean, 2.4%, 95% CI [1.8–3.1%]) areas. P values: LRT, n = 4 mice; black bar, mean; error bars, 95% CI. g, Fraction of Krt13+ hillock cells that are club cell lineage labelled (%) decreases from day 5 (10.2%, 95% CI [0.07, 0.16]) to day 80 (5.2%, 95% CI [0.03, 0.08]). Error bars, 95% CI; n = 3 mice (dots); P values, LRT. h, Differential expression (log2(fold-change)) and associated significance (log10(FDR)) for each gene (dot) that is differentially expressed in Krt13+ cells (identified using clustering in diffusion map space) compared to all cells (FDR <0.05, LRT). Colour code, cell type with highest expression (for example, green shows genes that are most highly expressed in Krt13+ hillock cells). Dots show all the genes differentially expressed (FDR <0.05) between Krt13+ hillock cells and other cells. Genes with log2 fold-change >1 are marked with large points, whereas others are identified as small points (grey). i, Enriched pathways in Krt13+ hillock cells. Representative MSigDB gene sets (rows) that are significantly enriched (colour bar, −log10(FDR), hypergeometric test) in Krt13+ hillock cells.
Extended Data Fig. 5 Genes associated with cell fate transitions.
a–h, Relative mean expression (loess-smoothed row-wise Z score of mean log2(TPM+1)) of significantly (P < 0.001, permutation test) varying genes (a–d) and transcription factors (e–h) across subsets of 6,905 (columns) basal, club and ciliated cells. Cells are pseudotemporally ordered (x axis, all plots) using diffusion maps (Fig. 2b, Extended Data Fig. 4c). Each cell was assigned to a cell fate transition if it was within d <0.1 of an edge of the convex hull of all points (in which d is the Euclidean distance in diffusion space) assigned to that edge.
Extended Data Fig. 6 Lineage tracing using pulse-seq.
a, Schematic of the pulse-seq experimental design. b, Post hoc cluster annotation by known cell type markers. t-SNE of 66,265 scRNA-seq profiles (points) from pulse-seq, coloured by the expression (log2(TPM+1)) of single marker genes for a particular cell type or cell-cycle score (bottom right) c, Pulse-seq lineage-labelled fraction of various cell populations over time. Linear quantile regression fits (trendline) to the fraction of lineage-labelled cells of each type (n = 3 mice per time point, dots) as a function of the number of days after tamoxifen-induced labelling. β, estimated regression coefficient, interpreted as daily rate of new lineage-labelled cells; p, P value for the significance of the relationship, Wald test. As expected, goblet and ciliated cells are labelled more slowly than club cells (Fig. 3d). d, Labelled fraction of basal cells is unchanged during pulse-seq time course, as expected. Estimated fraction (%) of cells of each type that are positive for the fluorescent lineage label (by FACS) in each of n = 3 mice (points) per time point. P values, LRT; error bars, 95% CI. e, Proportion of basal cell lineage-labelled tuft cells at day 0 (0%; n = 2 mice, dots) and day 30 (22.9%, 95% CI [0.17, 0.30]; bars, estimated proportions; n = 3 mice). Error bars, 95% CI; P values, LRT. f–h, Conventional Scgb1a1 (CC10) lineage trace of rare epithelial types shows minimal contribution to rare cell lineages. Fraction of Scb1a1 labelled (club cell trace) cells (%) of Gnat3+ tuft cells (f) at day 0 (n = 3 mice; 0.6%, 95% CI [0.00, 0.04]) and day 30 (n = 2 mice; 6.3%, 95% CI [0.04, 0.11]), EGFP(Foxi1)+ ionocytes at day 30 (n = 2 mice; 2.9%, 95% CI [0.01, 0.11]) (g), and Chga+ neuroendocrine cells at day 0 (n = 2 mice; 2.5%, 95% CI [0.01, 0.08]) and day 30 (n = 2 mice; 2.6%, 95% CI [0.01, 0.08]) (h) after club cell lineage labelling. P values, LRT; error bars, 95% CI.
Extended Data Fig. 7 Club cell heterogeneity and lineage tracing hillock-associated club cells using pulse-seq.
a, b, Principal components are associated with basal to club differentiation (PC-1), proximodistal heterogeneity (PC-2), and hillock gene modules (PC-2). a, PC-1 (x axis) versus PC-2 (y axis) for a PCA of 17,700 scRNA-seq profiles of club cells (points) in the pulse-seq dataset, coloured by signature scores for basal (left), proximal club cells (centre left), distal club cells (centre right), the Krt13+/Krt4+ hillock (right), or their cluster assignment (inset, right). b, Bar plots show the extent (normalized enrichment score) and significance of association of PC-1 (left) and PC-2 (right) for gene sets associated with different airway epithelial types (x axis), or gene modules associated with proximodistal heterogeneity (Extended Data Fig. 4a). Heat maps show the relative expression level (row-wise Z score of log2(TPM+1) expression values, colour bar) of the 20 genes with the highest and lowest loadings on PC-1 (left) and PC-2 (right) in each club cell (columns, down-sampled to 1,000 cells for visualization only). P values, permutation test. c, Pulse-seq lineage tracing of hillock-associated cells. Estimated fraction (%) of cells of each type that are positive for the fluorescent lineage label (by FACS) from n = 3 mice (points) per time point. P values, LRT. Error bars, 95% CI. d, Hillock-associated club cells are produced at a higher rate than all club cells. Estimated rate (%) based on the slope of quantile regression fits to the fraction of lineage-labelled cells of each type. P values, rank test; error bars, 95% CI. e, f, Club cells initially labelled by pulse-seq are associated with basal to club cell differentiation. e, Distribution of basal signature scores for individual club cells (points) from each pulse-seq time point and lineage label status. P value, Mann–Whitney U test. Violin plots show the Gaussian kernel probability densities of the data, large white point shows the mean. f, PC-1 versus PC-2 for a PCA of 17,700 scRNA-seq profiles of club cells (points), as in a, highlighting club cells that are lineage-labelled at the initial time point (legend). g, Schematic of the more rapid turnover of basal to club cells inside (top) and outside (bottom) hillocks.
Extended Data Fig. 8 Heterogeneity of rare tracheal epithelial cell types.
a, Cell-type-enriched GPCRs. Relative expression (Z score of mean log2(TPM+1)) of the GPCRs that are most enriched (FDR <0.001, LRT) in the cells of each tracheal epithelial cell type based on full-length scRNA-seq data. b, Tuft cell-specific expression of type I and type II taste receptors. Expression level (mean log2(TPM+1)) of tuft-cell enriched (FDR <0.05, LRT) taste receptor genes in each tracheal epithelial cell type based on full-length scRNA-seq data. c, Tuft cell-specific expression of the type-2 immunity-associated alarmins Il25 and Tslp. Expression level, of Il25 (left) and Tslp (right) in each cell type. FDR, LRT. Violin plots show the Gaussian kernel probability densities of the data. d, Morphological features of tuft cells. Immunofluorescence staining of the tuft-cell marker Gnat3 (yellow) along with DAPI (blue). Arrowhead, ‘tuft’; arrows, cytoplasmic extension. e, f, Tuft-1 and tuft-2 sub-clusters. e, t-SNE visualization of 892 tuft cells (points) coloured either by their cluster assignment (left, colour legend), or by the expression level of marker genes for mature tuft cells (Trpm5), tuft-1 (Gng13), tuft-2 (Alox5ap) subsets. f, Distribution of expression levels of the top markers for each subset. Violin plots show the Gaussian kernel probability densities of the data, large white point shows the mean. FDR, LRT, n = 15 mice. g, Tuft-1 and tuft-2 subtypes are each generated from basal cell parents. Estimated fraction of cells of each type that are positive for the basal-cell lineage label (by FACS) from n = 3 mice (points) per time point in the pulse-seq experiment. P values, LRT; error bars, 95% CI. h, Differential expression of tuft cell-associated transcription factors between tuft cell subtypes. Labelled genes are differently expressed in the tuft cell subsets (FDR <0.01, LRT). i, j, Mature and immature subsets are identified using marker gene expression. The distribution of expression of scores (using top 20 marker genes, Supplementary Table 1, Methods) for tuft (i), goblet (j), basal and club cells (label on top) in each cell subset (basal and club cells down-sampled to 1,000 cells). P values, Mann–Whitney U test. k, l, Gene signatures for goblet-1 and goblet-2 subsets. The distribution (k) and relative expression level (l) of marker genes that distinguish (log2 fold-change >0.1, FDR <0.001, LRT) cells in the goblet-1 and goblet-2 sub-clusters (colour bar, top and left) from the combined 3′ scRNA-seq datasets. m, Immunofluorescence staining of the goblet-1 marker Tff2 (magenta), the known goblet cell marker Muc5ac (green) and DAPI (blue). Solid white line: boundary of a goblet-1 cell.
Extended Data Fig. 9 Ionocyte characterization in situ.
a, Immunofluorescence characterization of ionocytes. Ionocytes visualized in Foxi1-EGFP mouse. EGFP(Foxi1) appropriately marks Foxi1 antibody-positive cells (left, solid outline). EGFP(Foxi1)+ cells express canonical airway markers Ttf1 (Nkx2-1) and Sox2 (solid outlines). EGFP(Foxi1)+ cells do not label with basal (Trp63), club (Scgb1a1), ciliated (Foxj1), tuft (Gnat3), neuroendocrine (Chga) or goblet (Tff2) cell markers (dashed outlines). b, Ionocytes are sparsely distributed in the surface epithelium. Representative whole-mount confocal image of ionocytes EGFP(Foxi1) and ciliated cells (AcTub). c, Expression level of ionocyte markers (rows ordered as in Fig. 5a, FDR <0.05 LRT, full-length scRNA-seq dataset) in each airway epithelial cell type. d, EGFP(Foxi1)+ ionocytes extend cytoplasmic appendages (arrows). e–g, Immunofluorescence labelling of EGFP(Foxi1)+ cells in airway regions. Submucosal gland (SMG, e), nasal respiratory epithelium (f) and olfactory neuroepithelium (g). Dotted line separates surface epithelium (SA) from SMG.
Extended Data Fig. 10 Functional characterization of ionocytes.
a, Ascl3(KO) moderately decreases ionocyte transcription factors and Cftr in ALI-cultured epithelia. Quantification (ΔΔCT) of expression in ionocyte (Cftr: −0.82 ΔΔCT, 95% CI [±0.20]; Foxi1: −0.75 ΔΔCT, 95% CI [±0.28]; Ascl3: −10.28 ΔΔCT, 95% CI [±1.85]) and basal (Trp63), club (Scgb1a1) or ciliated (Foxj1) markers in hetero- and homozygous Ascl3 KO (colour legend) are normalized to wild-type littermates. The mean of independent probes (p1 and p2) was used for Cftr. n = 10 (Ascl3+/−), 5 (Ascl3−/−), 4 (wild-type) mice. P values: Holm–Sidak test; error bars, 95% CI. b, Altered ASL reflectance intensity in Foxi1(KO) ALI culture compared to wild type. Representative μOCT image of ASL. Red bar, airway surface liquid depth (including the periciliary and mucus layers). Scale bar (white), 10 μm. c, d, Ionocyte depletion or disruption does not affect ASL depth (c) as determined by μOCT, nor pH (d) in cultured epithelia derived from homozygous Foxi1(KO) (n = 9) versus wild type littermates (n = 9 mice). P values, Mann–Whitney U test. e, f, Increased ΔIeq in Foxi1(KO) epithelia. ΔIeq (y axis) in ALI cultures of wild type (WT), heterozygous (HET) and Foxi1(KO) mice (n = 5 (WT), n = 4 (HET), n = 6 (KO)) that were characterized for their forskolin-inducible equivalent currents (e; Ieq) and for currents sensitive to CFTRinh-172 (f). The inhibitor-sensitive ΔIeq values reported may underestimate the true inhibitor-sensitive current, as the inhibitor response failed to reach a steady plateau for some samples during the time scale of the experiment. g–i, Foxi1 transcriptional activation (Foxi1-TA) in ferret increases Cftr expression and chloride transport. g, qRT–PCR expression quantification (ΔΔCT) of ionocyte markers in ferret Foxi1-TA ALI (n = 4 ferrets) normalized to mock transfection (Cftr: −1.39 ΔΔCT, 95% CI [±0.44]; Foxi1: −5.37 ΔΔCT, 95% CI [±0.91]; Ascl3: −0.87 ΔΔCT, 95% CI [±0.27]; Atp6v0d2: −1.18 ΔΔCT, 95% CI [±0.58] and Atp6v1e1: −0.070 ΔΔCT, 95% CI [±0.11]), P values, t-test; bars, means; error bar, 95% CI. h, i, Foxi1 activation in ferret cell cultures results in a CFTR inhibitor-sensitive short-circuit current (ΔIsc). Representative trace (h) and quantification (i) of short-circuit current (Isc) tracings from Foxi1-TA ferret ALI after sgRNA reverse transfection (n = 6, light blue) versus mock transfection (n = 5, black). j, Evolutionarily conserved ionocyte signatures. Difference in fraction of cells in which transcript is detected and log2 fold-change between human ionocytes and all other bronchial epithelial cells. Labelled genes are differentially expressed (log2 fold-change >0.25 and FDR <10−10, Mann–Whitney U test). Red, consensus ionocyte markers between mouse and human (log2 fold-change >0.25, FDR <10−5, LRT).
Supplementary information
Supplementary Information
This file contains Supplementary Figure 1: Representative FACS plot of primary mouse tracheal epithelial cells, including EpCAM+, tdTomato+ and EGFP+ gating strategies. Number of cells captured in each gate indicated, as well as the percentage of the parent population (schematic, bottom).
Supplementary Tables
This file contains Supplementary Tables 1-12 and a Supplementary Guide providing the table legends.
Rights and permissions
About this article
Cite this article
Montoro, D.T., Haber, A.L., Biton, M. et al. A revised airway epithelial hierarchy includes CFTR-expressing ionocytes. Nature 560, 319–324 (2018). https://doi.org/10.1038/s41586-018-0393-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-018-0393-7
This article is cited by
-
In vitro platform to model the function of ionocytes in the human airway epithelium
Respiratory Research (2024)
-
Biochemical and transcriptomic evaluation of a 3D lung organoid platform for pre-clinical testing of active substances targeting senescence
Respiratory Research (2024)
-
Culture and expansion of murine proximal airway basal stem cells
Stem Cell Research & Therapy (2024)
-
The implications of single-cell RNA-seq analysis in prostate cancer: unraveling tumor heterogeneity, therapeutic implications and pathways towards personalized therapy
Military Medical Research (2024)
-
Toward universal cell embeddings: integrating single-cell RNA-seq datasets across species with SATURN
Nature Methods (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.