Abstract
In Lewy body diseases—including Parkinson’s disease, without or with dementia, dementia with Lewy bodies, and Alzheimer’s disease with Lewy body co-pathology1—α-synuclein (α-Syn) aggregates in neurons as Lewy bodies and Lewy neurites2. By contrast, in multiple system atrophy α-Syn accumulates mainly in oligodendrocytes as glial cytoplasmic inclusions (GCIs)3. Here we report that pathological α-Syn in GCIs and Lewy bodies (GCI-α-Syn and LB-α-Syn, respectively) is conformationally and biologically distinct. GCI-α-Syn forms structures that are more compact and it is about 1,000-fold more potent than LB-α-Syn in seeding α-Syn aggregation, consistent with the highly aggressive nature of multiple system atrophy. GCI-α-Syn and LB-α-Syn show no cell-type preference in seeding α-Syn pathology, which raises the question of why they demonstrate different cell-type distributions in Lewy body disease versus multiple system atrophy. We found that oligodendrocytes but not neurons transform misfolded α-Syn into a GCI-like strain, highlighting the fact that distinct α-Syn strains are generated by different intracellular milieus. Moreover, GCI-α-Syn maintains its high seeding activity when propagated in neurons. Thus, α-Syn strains are determined by both misfolded seeds and intracellular environments.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 51 print issues and online access
$199.00 per year
only $3.90 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Lippa, C. F. et al. Lewy bodies contain altered α-synuclein in brains of many familial Alzheimer’s disease patients with mutations in presenilin and amyloid precursor protein genes. Am. J. Pathol. 153, 1365–1370 (1998).
Spillantini, M. G. et al. α-Synuclein in Lewy bodies. Nature 388, 839–840 (1997).
Tu, P. H. et al. Glial cytoplasmic inclusions in white matter oligodendrocytes of multiple system atrophy brains contain insoluble α-synuclein. Ann. Neurol. 44, 415–422 (1998).
Bousset, L. et al. Structural and functional characterization of two α-synuclein strains. Nat. Commun. 4, 2575 (2013).
Guo, J. L. et al. Distinct α-synuclein strains differentially promote tau inclusions in neurons. Cell 154, 103–117 (2013).
Peelaerts, W. et al. α-Synuclein strains cause distinct synucleinopathies after local and systemic administration. Nature 522, 340–344 (2015).
Prusiner, S. B. et al. Evidence for α-synuclein prions causing multiple system atrophy in humans with parkinsonism. Proc. Natl Acad. Sci. USA 112, E5308–E5317 (2015).
Woerman, A. L. et al. Propagation of prions causing synucleinopathies in cultured cells. Proc. Natl Acad. Sci. USA 112, E4949–E4958 (2015).
Fanciulli, A. & Wenning, G. K. Multiple-system atrophy. N. Engl. J. Med. 372, 249–263 (2015).
Koga, S. & Dickson, D. W. Recent advances in neuropathology, biomarkers and therapeutic approach of multiple system atrophy. J. Neurol. Neurosurg. Psychiatry 89, 175–184 (2018).
Fujiwara, H. et al. α-Synuclein is phosphorylated in synucleinopathy lesions. Nat. Cell Biol. 4, 160–164 (2002).
Gorbatyuk, O. S. et al. The phosphorylation state of Ser-129 in human α-synuclein determines neurodegeneration in a rat model of Parkinson disease. Proc. Natl Acad. Sci. USA 105, 763–768 (2008).
Covell, D. J. et al. Novel conformation-selective alpha-synuclein antibodies raised against different in vitro fibril forms show distinct patterns of Lewy pathology in Parkinson’s disease. Neuropathol. Appl. Neurobiol. 43, 604–620 (2017).
Duda, J. E., Giasson, B. I., Mabon, M. E., Lee, V. M. & Trojanowski, J. Q. Novel antibodies to synuclein show abundant striatal pathology in Lewy body diseases. Ann. Neurol. 52, 205–210 (2002).
Irwin, D. J. et al. Neuropathologic substrates of Parkinson disease dementia. Ann. Neurol. 72, 587–598 (2012).
Montine, T. J. et al. Multisite assessment of NIA-AA guidelines for the neuropathologic evaluation of Alzheimer’s disease. Alzheimers Dement. 12, 164–169 (2016).
Volpicelli-Daley, L. A. et al. Exogenous α-synuclein fibrils induce Lewy body pathology leading to synaptic dysfunction and neuron death. Neuron 72, 57–71 (2011).
Luk, K. C. et al. Exogenous α-synuclein fibrils seed the formation of Lewy body-like intracellular inclusions in cultured cells. Proc. Natl Acad. Sci. USA 106, 20051–20056 (2009).
Karpowicz, R. J. Jr et al. Selective imaging of internalized proteopathic α-synuclein seeds in primary neurons reveals mechanistic insight into transmission of synucleinopathies. J. Biol. Chem. 292, 13482–13497 (2017).
Luk, K. C. et al. Pathological α-synuclein transmission initiates Parkinson-like neurodegeneration in nontransgenic mice. Science 338, 949–953 (2012).
Yazawa, I. et al. Mouse model of multiple system atrophy α-synuclein expression in oligodendrocytes causes glial and neuronal degeneration. Neuron 45, 847–859 (2005).
Giasson, B. I. et al. Neuronal α-synucleinopathy with severe movement disorder in mice expressing A53T human α-synuclein. Neuron 34, 521–533 (2002).
Miller, D. W. et al. Absence of α-synuclein mRNA expression in normal and multiple system atrophy oligodendroglia. J. Neural Transm. (Vienna) 112, 1613–1624 (2005).
Asi, Y. T. et al. Alpha-synuclein mRNA expression in oligodendrocytes in MSA. Glia 62, 964–970 (2014).
Reyes, J. F. et al. Alpha-synuclein transfers from neurons to oligodendrocytes. Glia 62, 387–398 (2014).
Giasson, B. I., Murray, I. V., Trojanowski, J. Q. & Lee, V. M. A hydrophobic stretch of 12 amino acid residues in the middle of α-synuclein is essential for filament assembly. J. Biol. Chem. 276, 2380–2386 (2001).
Volpicelli-Daley, L. A., Luk, K. C. & Lee, V. M. Addition of exogenous α-synuclein preformed fibrils to primary neuronal cultures to seed recruitment of endogenous α-synuclein to Lewy body and Lewy neurite-like aggregates. Nat. Protocols 9, 2135–2146 (2014).
Toledo, J. B. et al. A platform for discovery: the University of Pennsylvania Integrated Neurodegenerative Disease Biobank. Alzheimers Dement. 10, 477–484.e1 (2014).
Guo, J. L. & Lee, V. M. Seeding of normal Tau by pathological Tau conformers drives pathogenesis of Alzheimer-like tangles. J. Biol. Chem. 286, 15317–15331 (2011).
Lee, E. B., Skovronsky, D. M., Abtahian, F., Doms, R. W. & Lee, V. M. Secretion and intracellular generation of truncated Aβ in β-site amyloid-β precursor protein-cleaving enzyme expressing human neurons. J. Biol. Chem. 278, 4458–4466 (2003).
Richter-Landsberg, C. & Vollgraf, U. Mode of cell injury and death after hydrogen peroxide exposure in cultured oligodendroglia cells. Exp. Cell Res. 244, 218–229 (1998).
Duda, J. E. et al. Immunohistochemical and biochemical studies demonstrate a distinct profile of α-Synuclein permutations in Multiple System Atrophy. J. Neuropathol. 59, 830–841 (2000).
Luk, K. C. et al. Intracerebral inoculation of pathological α-synuclein initiates a rapidly progressive neurodegenerative α-syncleinopathy in mice. J. Exp. Med. 209, 975–986 (2012).
Iba, M. et al. Synthetic tau fibrils mediate transmission of neurofibrillary tangles in a transgenic mouse model of Alzheimer’s-like tauopathy. J. Neurosci. 33, 1024–1037 (2013).
Abeliovich, A. et al. Mice lacking α-synuclein display functional deficits in the nigrostriatal dopamine system. Neuron 25, 239–252 (2000).
Acknowledgements
We thank K. Brunden and J. Guo for critical reading of the manuscript; S. Xie for helping with statistics; L. Kwong and Y. Xu for helping with brain extraction; D. Riddle for providing primary neurons; L. Romero for helping with quantification; L. Changolkar for helping with ELISA and all the other members of the Center for Neurodegenerative Disease Research for their support; and J. Grinspan and C. Richter-Landsberg for advice on culturing oligodendrocytes. The anti-PLP antibody was provided by J. Grinspan. This work was supported by NIH/NINDS Udall Center grant NS53488, the Ofer Nimerovsky Family Fund, the Jeff and Anne Keefer Fund and the MSA Coalition Global Seed Grant.
Reviewer information
Nature thanks T. Baron and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
C.P. designed and performed the experiments, analysed the data and wrote the manuscript. R.J.G., C.M. and M.F.O. performed the animal experiments and did quantification analysis. R.J.G. also performed α-Syn ELISA and biochemical analysis. D.J.C. generated the Syn9027 and Syn7015 antibodies and α-Syn PFFs. A.S. generated the KOM2 mice and assisted in stereotaxic injections. J.L.R. scored stained human brain sections. B.Z., R.J.G. and M.F.O. performed stereotaxic injections. R.M.P. performed cell culture experiments. K.C.L performed experiments and reviewed the manuscript. J.Q.T. supervised the study and reviewed the manuscript. V.M.-Y.L. supervised the study, interpreted the data and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data figures and tables
Extended Data Fig. 1 Biochemical analysis of GCI-α-Syn and LB-α-Syn.
a, Schematic for sequential extraction of brains with α-synucleinopathy. Diseased brain samples were sequentially extracted with buffer of increasing extraction strengths (1% Triton X-100 followed by 1% sarkosyl) to remove soluble proteins. b, Proteinase K-digested GCI-α-Syn and LB-α-Syn were immunoblotted with a series of antibodies targeting specific domains of α-Syn that spanning the entire molecule. c, Summary of the results for experiments described in b. d, Thermolysin-digested and undigested sarkosyl-insoluble fractions from three cases of Lewy body disease (LB1–LB3) and three cases of MSA (GCI1–GCI3) were resolved on 12% Bis-Tris gel and immunoblotted with an antibody against α-Syn (Syn211). e, Sarkosyl-insoluble fractions from a pair of cases (one of Lewy body disease and one of MSA) were incubated with increasing concentrations of thermolysin (with a ratio of thermolysin to total protein that ranged from 1.25 × 10−2 to 5 × 10−2) and immunoblotted with antibody against α-Syn (Syn211). Undigested fractions were loaded on the same gel. f, Trypsin-digested and undigested sarkosyl-insoluble fractions from three cases of Lewy body disease (LB1–LB3) and three cases of MSA (GCI1–GCI3) were resolved on 12% Bis-Tris gel and immunoblotted with an antibody against α-Syn (Syn211). g, Sarkosyl-insoluble fractions from a pair of cases (one of Lewy body disease and one of MSA) were incubated with increasing concentrations of trypsin (with the ratio of trypsin versus total protein range from 1.25 × 10−2 to 5 × 10−2) and immunoblotted with an antibody against α-Syn (Syn211). Undigested fractions were loaded on the same gel. The experiments shown in b and d–g have been repeated three times with similar results. For gel source data, see Supplementary Fig. 1.
Extended Data Fig. 2 Syn7015 preferentially recognizes GCIs over Lewy bodies.
a, Immunohistochemistry using a series dilution of Syn303 or Syn7015 on serial sections of a DLB brain and a MSA brain. At 45 ng ml−1, Syn7015 recognized both Lewy bodies and GCIs. At lower concentrations—particularly 1.67 ng ml−1 and 0.56 ng ml−1—Syn7015 preferentially recognizes GCIs over Lewy bodies (repeated with four cases). b, Quantification of the area occupied by pathological α-Syn stained with serial dilutions of Syn7015 or Syn303 on serial sections of two cases of MSA-P, two cases of MSA-C, one case of AD, two cases of PDD and two cases of DLB. The results for each case are normalized to Syn303 staining at 45 ng ml−1 (GCI, n = 4 cases; LB, n = 5 cases). c, α-Syn pathology revealed by Syn303 or Syn7015 in adjacent sections from cases of Lewy body disease and MSA (repeated with seven cases). Results shown as mean ± s.e.m. *P < 0.05. Scale bar: 50 μm (a), 100 μm (c), 25 μm (c inset). See Supplementary Table 5 for statistical details.
Extended Data Fig. 3 GCI-α-Syn is more potent in inducing α-Syn pathology in primary oligodendrocytes.
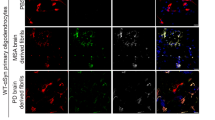
a, Oligodendrocytes treated with the same amount of GCI-α-Syn, LB-α-Syn or PFF were sequentially extracted with 1% Triton-X100 lysis buffer followed by 1% sarkosyl lysis buffer, which were combined together as the sarkosyl-soluble fraction. The sarkosyl-insoluble pellets were resuspended in Dulbecco’s PBS by sonication. Both soluble and insoluble fractions were immunoblotted with an antibody against total or pS129 α-Syn. b, Densitometric quantification of insoluble versus soluble α-Syn for experiments described in a (n = 3 biological replicates). c, d, Primary oligodendrocyte cultures were immunostained with antibodies against various cell-type specific markers: CNP (oligodendrocytes), olig2 (oligodendrocytes), Iba1 (microglial cells), NeuN (neurons), GFAP (astrocytes), PLP (oligodendrocytes) at day in vitro 3 (DIV 3) (c) or DIV 9 (d). e, Insoluble phosphorylated α-Syn, induced in primary oligodendrocytes overexpressing α-Syn, was co-stained with antibodies against various cell-type specific markers, demonstrating that the cells with α-Syn pathology are oligodendrocytes. f, Percentage of different type of cells (oligodendrocytes, microglial cells and astrocytes) in oligodendrocyte culture, at DIV 3 (the time point of virus infection), DIV 9 (the time point for misfolded α-Syn treatment) and DIV 23 (the time point for fixation) (n = 3 (DIV3) or 5 (DIV 9, DIV 23) coverslips from three independent experiments). g, Working hypotheses regarding the different cell-type distributions of GCI-α-Syn and LB-α-Syn strains in diseased brains. Hypothesis 1 states that the unique properties of GCI-α-Syn and LB-α-Syn strains determine their different cell-type distributions. The GCI-α-Syn strain (represented by red spheres) is more efficient in inducing α-Syn pathology in oligodendrocytes, whereas the LB-α-Syn strain (green spheres) is more efficient in inducing α-Syn pathology in neurons. Hypothesis 2 states that GCI-α-Syn and LB-α-Syn strains do not have cell-type preferences and that they could both be initiated by the same misfolded α-Syn seeds (grey spheres), but that the different intracellular environments of neurons and oligodendrocytes convert these α-Syn seeds to different strains. Results shown as mean ± s.e.m. **P < 0.01. Scale bars: 100 μm (c, d); 50 μm (e). The experiments shown in a and c–e have been repeated three times with similar results. See Supplementary Table 5 for statistical details. For gel source data, see Supplementary Fig. 1.
Extended Data Fig. 4 The seeding properties of GCI-α-Syn and LB-α-Syn do not show cell-type preference.
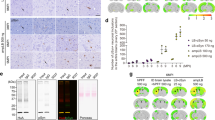
a, Soluble and insoluble fractions from primary neurons treated with the same amount of GCI-α-Syn, LB-α-Syn or PFF were immunoblotted with antibodies against total or pS129 α-Syn. b, Densitometric quantification of insoluble versus soluble α-Syn for experiments described in a (n = 3 biological replicates). c, Quantification of phosphorylated α-Syn in QBI-WT-Syn cells induced by an equal amount of GCI-α-Syn (MSA-C, MSA-P), LB-α-Syn (PDD, DLB and AD) or PFFs (GCI, n = 8 different preparations; LB, n = 9 different preparations). d, Soluble and insoluble fractions from QBI-Syn-WT cells treated with the same amount of GCI-α-Syn, LB-α-Syn or PFF were immunoblotted with an antibody against total or pS129 α-Syn. e, Densitometric quantification of insoluble versus soluble α-Syn for experiments described in d (n = 3 biological replicates). f, Quantification of insoluble phosphorylated α-Syn in primary neurons induced by various concentrations of GCI-α-Syn and LB-α-Syn before or after immunoprecipitation purification (n = 3 independent experiments). g, Quantification of insoluble phosphorylated α-Syn in primary neurons incubated with (1) GCI-α-Syn and LB-α-Syn preparations; (2) the same preparations after immunoprecipitation depletion to remove α-Syn; and (3) the depleted preparation to which the same amount of α-Syn PFFs (1 ng) was added (n = 3 independent experiments). h, PFFs combined with the GCI-α-Syn preparation depleted of α-Syn behave similarly to α-Syn PFFs alone. Quantification of insoluble phosphorylated α-Syn in primary neurons seeded by PFFs alone or PFFs combined with depleted GCI preparation (the amount of pathology induced by immunoprecipitation-depleted GCI preparation alone has been subtracted) (n = 3 independent experiments). i, j, Primary neuron were treated with GCI-α-Syn, LB-α-Syn or PFF and incubated with chloroquine (Ch) at the day of misfolded α-Syn treatment (‘DPT0’) or three days post-treatment (DPT3). The amount of insoluble phosphorylated α-Syn was quantified three days after chloroquine treatment (n = 3 (DPT0-GCI and PFF) or 4 (DPT0-LB, DPT3) independent experiments). k, Quantification of the number of cells with α-Syn pathology in wild-type mice inoculated with 50 ng of GCI-α-Syn or LB-α-Syn at six months post-injection. l, Representative photomicrographs of α-Syn pathology (stained by Syn506) in multiple brain regions ipsilateral to the injection site in GCI-α-Syn-, PFF- and LB-α-Syn-injected wild-type mice. Cortex, motor cortex; ENT, entorhinal cortex. Results shown as mean ± s.e.m. *P < 0.05; **P < 0.01; ****P < 0.0001; ns, not significant. Statistics shown in c represent two-tailed, unpaired t-test using the mean value of each case. Statistics shown in f represent one-way Anova with Tukey’s multiple comparison test. Statistics shown in g, h are two-tailed, unpaired t-test adjusted with Bonferroni correction for multiple comparison. Statistics shown in i, j are two-way ANOVA, with Sidak’s multiple comparisons test. The experiments in a, d and l have been repeated three times with similar results. Scale bar: 100 μm. See Supplementary Table 5 for statistical details. For gel source data, see Supplementary Fig. 1.
Extended Data Fig. 5 Distribution of α-Syn pathology in injected wild-type mice.
a, Representative photomicrographs of α-Syn pathologies stained by an antibody against pS129 α-Syn (81A) in multiple brain regions in GCI-α-Syn injected wild-type mice (experiment repeated three times). b, Heat map for the distribution of α-Syn pathology in wild-type mice injected with GCI-α-Syn, PFF or LB-α-Syn. GCI-α-Syn, LB-α-Syn and α-Syn PFF were unilaterally injected into the dorsal striatum of wild-type mice. The seeded α-Syn pathology was analysed and graded by immunohistochemistry with Syn506. The data were presented as heat maps to semiquantitatively demonstrate the central nervous system (CNS) distribution of α-Syn pathology. Each panel represents a coronal plane (bregma 4.28, 2.10, 0.98, −0.22, −1.22,−2.18, −2.92, −3.52 and −4.48 mm) for each treatment group (GCI-WT, n = 3 mice; PFF-WT, n = 4 mice; LB-WT, n = 3 mice). Scale bar: 100 μm.
Extended Data Fig. 6 Characterization of KOM2 mice.
a, Brain sections from KOM2 mice were double-labelled with antibodies against α-Syn (LB509) and various cell-type specific markers: Olig2 (oligodendrocytes), Iba1 (microglial cells), GFAP (astrocytes) and NeuN (neurons). In KOM2 mice, α-Syn is expressed only in oligodendrocytes. b, Brain lysates of wild-type and KOM2 mice were immunoblotted with an antibody against total α-Syn (Syn 9027), mouse α-Syn (Cell Signalling) and β-tubulin. Scale bars: 50 μm (a), 25 μm (a inset). The experiments in a, b have been repeated three times with similar results. For gel source data, see Supplementary Fig. 1.
Extended Data Fig. 7 Induction of oligodendroglial α-Syn pathology in KOM2 mice.
a, Syn506-positive α-Syn aggregates seeded by equal amounts of GCI-α-Syn or LB-α-Syn (18.75 ng) in KOM2 mice at one, three and six month post-injection in fimbria and thalamus. b–e, Quantification of the number of oligodendrocytes with α-Syn pathology in the optic tract (b), cerebral peduncle (c), fimbria (d), and thalamus (e) at different time points (one month post-injection, n = 3 mice; three and six months post-injection, n = 5 mice). f, Brain sections from GCI-α-Syn injected KOM2 mice were double-labelled with antibodies against misfolded α-Syn (Syn506) and various cell-type specific markers. The induced α-Syn pathologies are located in oligodendrocytes in KOM2 mice. g, GCI-α-Syn-injected KOM2 mouse brain sections were stained with an antibody against phosphorylated α-Syn (81A). Results shown as mean ± s.e.m. Scale bars: 50 μm (a, f and g), 12.5 μm (a insets) and 25 μm (f insets). The experiments in a, f and g have been repeated three times with similar results. Statistics shown in b, c are two tailed unpaired t-test adjusted with Bonferroni correction. See Supplementary Table 5 for statistical details.
Extended Data Fig. 8 Distribution of α-Syn pathology in injected KOM2 mice.
Heat maps to semiquantitatively demonstrate the CNS distribution of α-Syn pathology in KOM2 mice unilaterally injected with GCI-α-Syn or LB-α-Syn into the thalamus. α-Syn pathologies were analysed and graded by immunohistochemistry with Syn506 at one month (n = 3), three months (n = 5) and six month (n = 5) post injection. Each panel represents a coronal plane (bregma −1.22, −2.18, −2.92, −3.52, −4.48 mm) for each treatment group. Because there is no α-Syn pathology in the contralateral side, only the ipsilateral side is shown.
Extended Data Fig. 9 Oligodendrocyte environment generates the GCI-α-Syn strain.
a, Immunohistochemistry of adjacent sections from human or mouse brains with Syn303 and Syn7015. First row, adjacent brain sections of cases of Lewy body disease and MSA used for the extraction of LB-α-Syn and GCI-α-Syn for injection. Second row, adjacent brain sections of KOM2 mice injected with LB-α-Syn prepared from the brain tissue shown in the first row. OPT and CP are shown. Whereas the LB-α-Syn used for the injections is Syn7015-negative, the oligodendrocyte pathology that is induced is Syn7015-positive. Third row, adjacent brain sections of KOM2 mice injected with GCI-α-Syn prepared from the brain sample shown in the first row. OPT and CP are shown. Fourth row, adjacent brain sections of M83 mice with α-Syn pathology. Midbrain (MB) and pons are shown. b, Brain sections from KOM2 mice injected with GCI-α-Syn or LB-α-Syn in the thalamus were double-labelled with Syn506 and antibodies against P62 (left panel) or ubiquitin (right panel). c, Brain sections from GCI-α-Syn- or LB-α-Syn-injected KOM2 mice were double-labelled with Syn506 and GFAP. Both ipsilateral and contralateral optic tracts are shown. d, Adjacent sections of substantia nigra and cortex from two different cases of MSA were stained with Syn7015 and Syn303. Scale bars: 50 μm (a–c), 12.5 μm (a insets), 20 μm (b inset) and 30 μm (d). The experiments in a–d have been repeated three times with similar results.
Extended Data Fig. 10 α-Syn pathology induced by passaged PFF and GCI.
a, Insoluble phosphorylated α-Syn in QBI-WT-Syn cells seeded by PFFs, PFFs that have been passaged in KOM2 mice (PFF-KOM2-Syn) or PFFs that were combined with the sarkosyl-insoluble fraction prepared from uninjected KOM2 mice (PFF + KOM2). b, Insoluble phosphorylated α-Syn in QBI-WT-Syn cells induced by an equal amount (200 pg) of PFF-oligo-Syn, PFF-HipN-Syn, PFF-CtxN-Syn, PFF-QBI-Syn and PFFs. c, Soluble and insoluble fractions from QBI-Syn-WT cells treated with the same amount of PFF-oligo-Syn, PFF-HipN-Syn, PFF-CtxN-Syn, PFF-QBI-Syn and PFF were immunoblotted with antibodies against total or pS129 α-Syn. d, Densitometric quantification of insoluble versus soluble α-Syn for experiments described in c (n = 3 biological replicates). e, Insoluble phosphorylated α-Syn in QBI-WT-Syn cells induced by GCI-α-Syn and GCI-α-Syn that has been passaged in primary neurons for multiple times (that is, GCI-N-P1, GCI-N-P2, GCI-N-P3). f, Soluble and insoluble fractions from QBI-Syn-WT cells treated with the same amount of GCI, GCI-N-P1, GCI-N-P2, GCI-N-P3 and PFF were immunoblotted with antibodies against total α-Syn or pS129 α-Syn. g, Densitometric quantification of insoluble versus soluble α-Syn for experiments described in f (n = 3 biological replicates). Statistics shown in d, g are one-way ANOVA followed by Dunnett’s post hoc test comparing each group with PFF-oligo-Syn in d or GCI in g. Results shown as mean ± s.e.m. **P < 0.01; ***P < 0.01; ns, not significant. Scale bars: 50 μm (a, b, e). The experiments in a–c and e–f have been repeated three times with similar results. See Supplementary Table 5 for statistical details. For gel source data, see Supplementary Fig. 1.
Supplementary information
Supplementary Information
This file contains Supplementary Tables 1-5, Supplementary Figure 1 and Supplementary References
Rights and permissions
About this article
Cite this article
Peng, C., Gathagan, R.J., Covell, D.J. et al. Cellular milieu imparts distinct pathological α-synuclein strains in α-synucleinopathies. Nature 557, 558–563 (2018). https://doi.org/10.1038/s41586-018-0104-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41586-018-0104-4
This article is cited by
-
The involvement of α-synucleinopathy in the disruption of microglial homeostasis contributes to the pathogenesis of Parkinson’s disease
Cell Communication and Signaling (2024)
-
Biases in α-synuclein immuno-quantitation: a core problem for basic and ancillary studies of Parkinson’s disease and multiple system atrophy
Translational Neurodegeneration (2024)
-
Aggregate-prone brain regions in Parkinson’s disease are rich in unique N-terminus α-synuclein conformers with high proteolysis susceptibility
npj Parkinson's Disease (2024)
-
Phosphorylation and O-GlcNAcylation at the same α-synuclein site generate distinct fibril structures
Nature Communications (2024)
-
LRP10 and α-synuclein transmission in Lewy body diseases
Cellular and Molecular Life Sciences (2024)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.