Abstract
Although recent years have seen large decreases in the overall global rate of suicide fatalities, this trend is not reflected everywhere. Suicide and suicidal behaviour continue to present key challenges for public policy and health services, with increasing suicide deaths in some countries such as the USA. The development of suicide risk is complex, involving contributions from biological (including genetics), psychological (such as certain personality traits), clinical (such as comorbid psychiatric illness), social and environmental factors. The involvement of multiple risk factors in conveying risk of suicide means that determining an individual’s risk of suicide is challenging. Improving risk assessment, for example, by using computer testing and genetic screening, is an area of ongoing research. Prevention is key to reduce the number of suicide deaths and prevention efforts include universal, selective and indicated interventions, although these interventions are often delivered in combination. These interventions, combined with psychological (such as cognitive behavioural therapy, caring contacts and safety planning) and pharmacological treatments (for example, clozapine and ketamine) along with coordinated social and public health initiatives, should continue to improve the management of individuals who are suicidal and decrease suicide-associated morbidity.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 1 digital issues and online access to articles
$119.00 per year
only $119.00 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
World Health Organization. Preventing suicide: a global imperative (WHO, 2014). A systematic overview of the global epidemiology of suicide and suicide attempts, including country-specific data and an assessment of key prevention strategies.
Naghavi, M. Global, regional, and national burden of suicide mortality 1990 to 2016: systematic analysis for the global burden of disease study 2016. BMJ 364, l94 (2019). This review, based on the Global Burden of Disease Study, provides the global and country-specific incidence (and trends in incidence) of suicide.
Cerel, J. et al. How many people are exposed to suicide? Not six. Suicide Life Threat. Behav. 49, 529–534 (2019).
Crosby, A. E., Ortega, L. & Melanson, C. Self-directed violence surveillance: uniform definitions and recommended data elements (CDC, 2011).
Brenner, L. A. et al. Implementation of a suicide nomenclature within two VA healthcare settings. J. Clin. Psychol. Med. Settings 18, 116–128 (2011).
Turecki, G. & Brent, D. A. Suicide and suicidal behaviour. Lancet 387, 1227–1239 (2016).
Mars, B. et al. Predictors of future suicide attempt among adolescents with suicidal thoughts or non-suicidal self-harm: a population-based birth cohort study. Lancet Psychiatry 6, 327–337 (2019).
Klonsky, E. D., May, A. M. & Saffer, B. Y. Suicide, suicide attempts, and suicidal ideation. Annu. Rev. Clin. Psychol. 12, 307–330 (2016).
O’Connor, R. C. & Kirtley, O. J. The integrated motivational-volitional model of suicidal behaviour. Phil. Trans. R. Soc. B Biol. Sci. 373, 20170268 (2018).
Van Orden, K. A. et al. The interpersonal theory of suicide. Psychol. Rev. 117, 575–600 (2010).
Kapur, N., Cooper, J., O’Connor, R. C. & Hawton, K. Non-suicidal self-injury v. attempted suicide: new diagnosis or false dichotomy? Br. J. Psychiatry 202, 326–328 (2013).
Nock, M. K. et al. Cross-national prevalence and risk factors for suicidal ideation, plans and attempts. Br. J. Psychiatry 192, 98–105 (2008). This epidemiological study is one of few to compare suicidal ideation and suicidal behaviour across low-income, middle-income and high-income countries (17 countries in total).
Seedat, S. et al. Cross-national associations between gender and mental disorders in the world health organization world mental health surveys. Arch. Gen. Psychiatry 66, 785–795 (2009).
Spallek, J. et al. Suicide among immigrants in Europe — a systematic literature review. Eur. J. Public Health 25, 63–71 (2015).
Gunnell, D. & Eddleston, M. Suicide by intentional ingestion of pesticides: a continuing tragedy in developing countries. Int. J. Epidemiol. 32, 902–909 (2003).
Mew, E. J. et al. The global burden of fatal self-poisoning with pesticides 2006-15: Systematic review. J Affect. Disord. 219, 93–104 (2017).
Pridemore, W. A., Chamlin, M. B. & Andreev, E. Reduction in male suicide mortality following the 2006 Russian alcohol policy: an interrupted time series analysis. Am. J. Public Health 103, 2021–2026 (2013).
Lin, C. Y., Hsu, C. Y., Gunnell, D., Chen, Y. Y. & Chang, S. S. Spatial patterning, correlates, and inequality in suicide across 432 neighborhoods in Taipei City, Taiwan. Soc. Sci. Med. 222, 20–34 (2018).
World Health Organization.World Health Statistics data visualizations dashboard. Noncommunicable diseases and mental health. Data tables (WHO, 2018).
Thomas, K. & Gunnell, D. Suicide in England and Wales 1861-2007: a time-trends analysis. Int. J. Epidemiol. 39, 1464–1475 (2010).
Caine, E. D. Suicide and attempted suicide in the united states during the 21st century. JAMA Psychiatry 74, 1087–1088 (2017).
Wang, C. W., Chan, C. L. & Yip, P. S. Suicide rates in China from 2002 to 2011: an update. Soc. Psychiatry Psychiatr. Epidemiol. 49, 929–941 (2014).
India State-Level Disease Burden Initiative Suicide Collaborators. Gender differentials and state variations in suicide deaths in India: the Global Burden of Disease Study 1990-2016. Lancet Public Health 3, e478–e489 (2018).
Chang, S. S., Stuckler, D., Yip, P. & Gunnell, D. Impact of 2008 global economic crisis on suicide: time trend study in 54 countries. BMJ 347, f5239 (2013).
Stuckler, D., Basu, S., Suhrcke, M., Coutts, A. & McKee, M. The public health effect of economic crises and alternative policy responses in Europe: an empirical analysis. Lancet 374, 315–323 (2009). A comprehensive assessment of the impact of economic crises and increases in unemployment on all-cause and suicide mortality in Europe, showing that rises in unemployment are associated with increases in suicide, but the extent of the rise may be offset by appropriate social policy measures, particularly active labour market programmes.
Gunnell, D. et al. The impact of pesticide regulations on suicide in Sri Lanka. Int. J. Epidemiol. 36, 1235–1242 (2007).
Kreitman, N. The coal gas story. United Kingdom suicide rates, 1960-71. Br. J. Prev. Soc. Med. 30, 86–93 (1976).
Niederkrotenthaler, T. et al. Changes in suicide rates following media reports on celebrity suicide: a meta-analysis. J. Epidemiol. Community Health 66, 1037–1042 (2012).
Turecki, G. The molecular bases of the suicidal brain. Nat. Rev. Neurosci. 15, 802–816 (2014).
Lutz, P. E., Mechawar, N. & Turecki, G. Neuropathology of suicide: recent findings and future directions. Mol. Psychiatry 22, 1395–1412 (2017).
Brent, D. A., Bridge, J., Johnson, B. A. & Connolly, J. Suicidal behavior runs in families. A controlled family study of adolescent suicide victims. Arch. Gen. Psychiatry 53, 1145–1152 (1996).
McGirr, A. et al. Familial aggregation of suicide explained by cluster B traits: a three-group family study of suicide controlling for major depressive disorder. Am. J. Psychiatry 166, 1124–1134 (2009). This paper is a key contributor to our understanding of how impulsive–aggressive behaviours contribute to the familial aggregation of suicidal behaviours.
O’Neill, S., Ennis, E., Corry, C. & Bunting, B. Factors associated with suicide in four age groups: a population based study. Arch. Suicide Res. 22, 128–138 (2018).
Brent, D. A. et al. Familial transmission of mood disorders: convergence and divergence with transmission of suicidal behavior. J. Am. Acad. Child Adolesc. Psychiatry 43, 1259–1266 (2004).
Kim, C. D. et al. Familial aggregation of suicidal behavior: a family study of male suicide completers from the general population. Am. J. Psychiatry 162, 1017–1019 (2005).
Tidemalm, D. et al. Familial clustering of suicide risk: a total population study of 11.4 million individuals. Psychol. Med. 41, 2527–2534 (2011).
Fu, Q. et al. A twin study of genetic and environmental influences on suicidality in men. Psychol. Med. 32, 11–24 (2002).
Brent, D. A. et al. Familial pathways to early-onset suicide attempt: a 5.6-year prospective study. JAMA Psychiatry 72, 160–168 (2015).
Burrell, L. V., Mehlum, L. & Qin, P. Sudden parental death from external causes and risk of suicide in the bereaved offspring: a national study. J. Psychiatr. Res. 96, 49–56 (2018).
Coon, H. et al. Genome-wide significant regions in 43 Utah high-risk families implicate multiple genes involved in risk for completed suicide. Mol. Psychiatry https://doi.org/10.1038/s41380-018-0282-3 (2018).
Galfalvy, H. et al. A genome-wide association study of suicidal behavior. Am. J. Med. Genet. B. Neuropsychiatr. Genet. 168, 557–563 (2015).
Galfalvy, H. et al. A pilot genome wide association and gene expression array study of suicide with and without major depression. World J. Biol. Psychiatry 14, 574–582 (2013).
Tombácz, D. et al. High-coverage whole-exome sequencing identifies candidate genes for suicide in victims with major depressive disorder. Sci. Rep. 7, 7106 (2017).
Anguelova, M., Benkelfat, C. & Turecki, G. A systematic review of association studies investigating genes coding for serotonin receptors and the serotonin transporter: II. Suicidal behaviour. Mol. Psychiatry 8, 646–653 (2003).
Brezo, J., Klempan, T. & Turecki, G. The genetics of suicide: a critical review of molecular studies. Psychiatr. Clin. North Am. 31, 179–203 (2008).
Erlangsen, A. et al. Genetics of suicide attempts in individuals with and without mental disorders: a population-based genome-wide association study. Mol. Psychiatry https://doi.org/10.1038/s41380-018-0218-y (2018).
Strawbridge, R. J. et al. Identification of novel genome-wide associations for suicidality in UK Biobank, genetic correlation with psychiatric disorders and polygenic association with completed suicide. EBioMedicine 41, 517–525 (2019).
Levey, D. F. et al. Genetic associations with suicide attempt severity and genetic overlap with major depression. Transl. Psychiatry 9, 22 (2019).
Kimbrel, N. A. et al. A genome-wide association study of suicide attempts and suicidal ideation in U.S. military veterans. Psychiatry Res. 269, 64–69 (2018).
Sokolowski, M., Wasserman, J. & Wasserman, D. Polygenic associations of neurodevelopmental genes in suicide attempt. Mol. Psychiatry 21, 1381–1390 (2016).
Ruderfer, D. M. et al. Significant shared heritability underlies suicide attempt and clinically predicted probability of attempting suicide. Mol. Psychiatry https://doi.org/10.1038/s41380-018-0326-8 (2019).
Consortium, E. P. An integrated encyclopedia of DNA elements in the human genome. Nature 489, 57–74 (2012).
PsychENCODE Consortium. Revealing the brain’s molecular architecture. Science 362, 1262–1263 (2018).
Brezo, J. et al. Differences and similarities in the serotonergic diathesis for suicide attempts and mood disorders: a 22-year longitudinal gene-environment study. Mol. Psychiatry 15, 831–843 (2010).
Caspi, A. et al. Influence of life stress on depression: moderation by a polymorphism in the 5-HTT gene. Science 301, 386–389 (2003).
Brezo, J. et al. Predicting suicide attempts in young adults with histories of childhood abuse. Br. J. Psychiatry 193, 134–139 (2008).
Fergusson, D. M., Woodward, L. J. & Horwood, L. J. Risk factors and life processes associated with the onset of suicidal behaviour during adolescence and early adulthood. Psychol. Med. 30, 23–39 (2000).
McGowan, P. O. et al. Epigenetic regulation of the glucocorticoid receptor in human brain associates with childhood abuse. Nat. Neurosci. 12, 342–348 (2009). This work was the first to show biological mechanisms for the lasting impact of social trauma in humans and has been the basis for reconciling the effects of genetics and environment on behaviour.
Labonte, B. et al. Differential glucocorticoid receptor exon 1(B), 1(C), and 1(H) expression and methylation in suicide completers with a history of childhood abuse. Biol. Psychiatry 72, 41–48 (2012).
Turecki, G., Ota, V. K., Belangero, S. I., Jackowski, A. & Kaufman, J. Early life adversity, genomic plasticity, and psychopathology. Lancet Psychiatry 1, 461–466 (2014).
van Heeringen, K. & Mann, J. J. The neurobiology of suicide. Lancet Psychiatry 1, 63–72 (2014).
Mann, J. J. et al. Candidate endophenotypes for genetic studies of suicidal behavior. Biol. Psychiatry 65, 556–563 (2009).
Brezo, J. et al. Childhood trajectories of anxiousness and disruptiveness as predictors of suicide attempts. Arch. Pediatr. Adolesc. Med. 162, 1015–1021 (2008).
Brezo, J. et al. Broad and narrow personality traits as markers of one-time and repeated suicide attempts: a population-based study. BMC Psychiatry 8, 15 (2008).
Sareen, J. et al. Anxiety disorders and risk for suicidal ideation and suicide attempts: a population-based longitudinal study of adults. Arch. Gen. Psychiatry 62, 1249–1257 (2005).
Orri, M. et al. Association of childhood irritability and depressive/anxious mood profiles with adolescent suicidal ideation and attempts. JAMA Psychiatry 75, 465–473 (2018).
Bentley, K. H. et al. Anxiety and its disorders as risk factors for suicidal thoughts and behaviors: a meta-analytic review. Clin. Psychol. Rev. 43, 30–46 (2016).
Wanner, B., Vitaro, F., Tremblay, R. E. & Turecki, G. Childhood trajectories of anxiousness and disruptiveness explain the association between early-life adversity and attempted suicide. Psychol. Med. 42, 2373–2382 (2012).
Waltes, R., Chiocchetti, A. G. & Freitag, C. M. The neurobiological basis of human aggression: a review on genetic and epigenetic mechanisms. Am. J. Med. Genet. Part B Neuropsychiatric Genet. 171, 650–675 (2016).
Palumbo, S., Mariotti, V., Iofrida, C. & Pellegrini, S. Genes and aggressive behavior: epigenetic mechanisms underlying individual susceptibility to aversive environments. Front. Behav. Neurosci. 12, 117 (2018).
Provencal, N., Booij, L. & Tremblay, R. E. The developmental origins of chronic physical aggression: biological pathways triggered by early life adversity. J. Exp. Biol. 218, 123–133 (2015).
Smith, M. M. et al. The perniciousness of perfectionism: a meta-analytic review of the perfectionism–suicide relationship. J. Pers. 86, 522–542 (2018).
Batty, G. D. et al. Personality traits and risk of suicide mortality: findings from a multi-cohort study in the general population. World Psychiatry 17, 371–372 (2018).
Caldji, C. et al. Maternal care during infancy regulates the development of neural systems mediating the expression of fearfulness in the rat. Proc. Natl Acad. Sci. USA 95, 5335–5340 (1998).
Suomi, S. J. Early stress and adult emotional reactivity in rhesus monkeys. Ciba Found. Symp. 156, 171–183; discussion 183–178 (1991).
Weaver, I. C. et al. Epigenetic programming by maternal behavior. Nat. Neurosci. 7, 847–854 (2004).
van der Vegt, E. J., van der Ende, J., Ferdinand, R. F., Verhulst, F. C. & Tiemeier, H. Early childhood adversities and trajectories of psychiatric problems in adoptees: evidence for long lasting effects. J. Abnorm. Child Psychol. 37, 239–249 (2009).
Johnson, J. G. et al. Childhood adversities, interpersonal difficulties, and risk for suicide attempts during late adolescence and early adulthood. Arch. Gen. Psychiatry 59, 741–749 (2002).
Richard-Devantoy, S., Berlim, M. T. & Jollant, F. Suicidal behaviour and memory: a systematic review and meta-analysis. World J. Biol. Psychiatry 16, 544–566 (2015).
McGirr, A. et al. Dysregulation of the sympathetic nervous system, hypothalamic–pituitary–adrenal axis and executive function in individuals at risk for suicide. J. Psychiatry Neurosci. 35, 399–408 (2010).
Ding, Y. et al. Altered brain processing of decision-making in healthy first-degree biological relatives of suicide completers. Mol. Psychiatry 22, 1149–1154 (2017).
Grover, K. E. et al. Problem solving moderates the effects of life event stress and chronic stress on suicidal behaviors in adolescence. J. Clin. Psychol. 65, 1281–1290 (2009).
Sorberg Wallin, A. et al. Suicide attempt predicted by academic performance and childhood IQ: a cohort study of 26 000 children. Acta Psychiatr. Scand. 137, 277–286 (2018).
Gould, F. et al. The effects of child abuse and neglect on cognitive functioning in adulthood. J. Psychiatr. Res. 46, 500–506 (2012).
Lee, F. S. et al. Mental health. Adolescent mental health-opportunity and obligation. Science 346, 547–549 (2014).
Nock, M. K. et al. Prevalence, correlates, and treatment of lifetime suicidal behavior among adolescents: results from the national comorbidity survey replication adolescent supplement. JAMA Psychiatry 70, 300–310 (2013).
Carroll, R., Metcalfe, C. & Gunnell, D. Hospital presenting self-harm and risk of fatal and non-fatal repetition: systematic review and meta-analysis. PLOS ONE 9, e89944 (2014).
Nock, M. K. et al. Cross-national analysis of the associations among mental disorders and suicidal behavior: findings from the WHO World Mental Health Surveys. PLOS Med. 6, e1000123 (2009).
Arsenault-Lapierre, G., Kim, C. & Turecki, G. Psychiatric diagnoses in 3275 suicides: a meta-analysis. BMC Psychiatry 4, 37 (2004).
Lin, L. & Zhang, J. Impulsivity, mental disorder, and suicide in rural China. Arch. Suicide Res. 21, 73–82 (2017).
Phillips, M. R., Li, X. & Zhang, Y. Suicide rates in China, 1995-99. Lancet 359, 835–840 (2002).
Zhang, J., Xiao, S. & Zhou, L. Mental disorders and suicide among young rural Chinese: a case-control psychological autopsy study. Am. J. Psychiatry 167, 773–781 (2010).
Ahmed, H. U. et al. Suicide and depression in the World Health Organization South-East Asia Region: a systematic review. WHO South East Asia J. Public Health 6, 60–66 (2017).
Kapur, N. et al. Mental health service changes, organisational factors, and patient suicide in England in 1997-2012: a before-and-after study. Lancet Psychiatry 3, 526–534 (2016).
Hor, K. & Taylor, M. Suicide and schizophrenia: a systematic review of rates and risk factors. J. Psychopharmacol. 24, 81–90 (2010).
Holma, K. M. et al. Differences in incidence of suicide attempts between bipolar I and II disorders and major depressive disorder. Bipolar Disord. 16, 652–661 (2014).
McGirr, A., Renaud, J., Seguin, M., Alda, M. & Turecki, G. Course of major depressive disorder and suicide outcome: a psychological autopsy study. J. Clin. Psychiatry 69, 966–970 (2008).
Holma, K. M. et al. Incidence and predictors of suicide attempts in DSM-IV major depressive disorder: a five-year prospective study. Am. J. Psychiatry 167, 801–808 (2010).
Dumais, A. et al. Risk factors for suicide completion in major depression: a case-control study of impulsive and aggressive behaviors in men. Am. J. Psychiatry 162, 2116–2124 (2005).
Kim, C. et al. Patterns of co-morbidity in male suicide completers. Psychol. Med. 33, 1299–1309 (2003).
Seguin, M. et al. Life trajectories and burden of adversity: mapping the developmental profiles of suicide mortality. Psychol. Med. 37, 1575–1583 (2007).
Artenie, A. A. et al. Licit and illicit substance use among people who inject drugs and the association with subsequent suicidal attempt. Addiction 110, 1636–1643 (2015).
Artenie, A. A. et al. Associations of substance use patterns with attempted suicide among persons who inject drugs: can distinct use patterns play a role? Drug Alcohol Depend. 147, 208–214 (2015).
Chachamovich, E., Ding, Y. & Turecki, G. Levels of aggressiveness are higher among alcohol-related suicides: results from a psychological autopsy study. Alcohol 46, 529–536 (2012).
Schosser, A. et al. Genomewide association scan of suicidal thoughts and behaviour in major depression. PLOS ONE 6, e20690 (2011).
Fournier, C. et al. Association between binge drug use and suicide attempt among people who inject drugs. Substance Abuse 39, 315–321 (2018).
Qin, P., Agerbo, E. & Mortensen, P. B. Suicide risk in relation to socioeconomic, demographic, psychiatric, and familial factors: a national register-based study of all suicides in Denmark, 1981-1997. Am. J. Psychiatry 160, 765–772 (2003).
Webb, R. T. et al. Suicide risk in primary care patients with major physical diseases: a case–control study. Arch. Gen. Psychiatry 69, 256–264 (2012).
Seguin, M., Beauchamp, G., Robert, M., DiMambro, M. & Turecki, G. Developmental model of suicide trajectories. Br. J. Psychiatry 205, 120–126 (2014).
Bernert, R. A., Turvey, C. L., Conwell, Y. & Joiner, T. E. Jr. Association of poor subjective sleep quality with risk for death by suicide during a 10-year period: a longitudinal, population-based study of late life. JAMA Psychiatry 71, 1129–1137 (2014).
Morgan, C. et al. Self-harm in a primary care cohort of older people: incidence, clinical management, and risk of suicide and other causes of death. Lancet Psychiatry 5, 905–912 (2018).
Bernert, R. A., Kim, J. S., Iwata, N. G. & Perlis, M. L. Sleep disturbances as an evidence-based suicide risk factor. Curr. Psychiatry Rep. 17, 554 (2015).
Racine, M. Chronic pain and suicide risk: a comprehensive review. Prog. Neuropsychopharmacol. Biol. Psychiatry 87, 269–280 (2018).
Joiner, T. E. Jr., Brown, J. S. & Wingate, L. R. The psychology and neurobiology of suicidal behavior. Annu. Rev. Psychol. 56, 287–314 (2005).
O’Connor, R. C. & Nock, M. K. The psychology of suicidal behaviour. Lancet Psychiatry 1, 73–85 (2014).
Klonsky, E. D. & May, A. M. The three-step theory (3ST): a new theory of suicide rooted in the “ideation-to-action” framework. Int. J. Cognit. Ther. 8, 114–129 (2015).
Wetherall, K. et al. From ideation to action: differentiating between those who think about suicide and those who attempt suicide in a national study of young adults. J. Affect. Disord. 241, 475–483 (2018).
Batty, G. D. et al. Psychosocial characteristics as potential predictors of suicide in adults: an overview of the evidence with new results from prospective cohort studies. Transl. Psychiatry 8, 22 (2018).
Bjorkenstam, C., Andersson, G., Dalman, C., Cochran, S. & Kosidou, K. Suicide in married couples in Sweden: is the risk greater in same-sex couples? Eur. J. Epidemiol. 31, 685–690 (2016).
Brunstein Klomek, A., Sourander, A. & Gould, M. The association of suicide and bullying in childhood to young adulthood: a review of cross-sectional and longitudinal research findings. Can. J. Psychiatry 55, 282–288 (2010).
King, M. et al. A systematic review of mental disorder, suicide, and deliberate self harm in lesbian, gay and bisexual people. BMC Psychiatry 8, 70 (2008).
Neeleman, J. & Wessely, S. Ethnic minority suicide: a small area geographical study in south London. Psychol. Med. 29, 429–436 (1999).
Calati, R. et al. Suicidal thoughts and behaviors and social isolation: a narrative review of the literature. J Affect. Disord. 245, 653–667 (2019).
Niedzwiedz, C., Haw, C., Hawton, K. & Platt, S. The definition and epidemiology of clusters of suicidal behavior: a systematic review. Suicide Life Threat. Behav. 44, 569–581 (2014).
Yip, P. S. et al. Means restriction for suicide prevention. Lancet 379, 2393–2399 (2012).
Mann, J. J. The serotonergic system in mood disorders and suicidal behaviour. Phil. Trans. R. Soc. B Biol. Sci. 368, 20120537 (2013).
Antypa, N., Serretti, A. & Rujescu, D. Serotonergic genes and suicide: a systematic review. Eur. Neuropsychopharmacol. 23, 1125–1142 (2013).
Oquendo, M. A. et al. Toward a biosignature for suicide. Am. J. Psychiatry 171, 1259–1277 (2014).
Asberg, M., Thoren, P., Traskman, L., Bertilsson, L. & Ringberger, V. “Serotonin depression” – a biochemical subgroup within the affective disorders? Science 191, 478–480 (1976).
Arango, V. et al. Serotonin 1A receptors, serotonin transporter binding and serotonin transporter mRNA expression in the brainstem of depressed suicide victims. Neuropsychopharmacology 25, 892–903 (2001).
Mann, J. J. Neurobiology of suicidal behaviour. Nat. Rev. Neurosci. 4, 819–828 (2003).
Boldrini, M., Underwood, M. D., Mann, J. J. & Arango, V. More tryptophan hydroxylase in the brainstem dorsal raphe nucleus in depressed suicides. Brain Res. 1041, 19–28 (2005).
Bach-Mizrachi, H. et al. Elevated expression of tryptophan hydroxylase-2 mRNA at the neuronal level in the dorsal and median raphe nuclei of depressed suicides. Mol. Psychiatry 13, 507–513 (2008).
Sullivan, G. M. et al. Positron emission tomography quantification of serotonin1A receptor binding in suicide attempters with major depressive disorder. JAMA Psychiatry 72, 169–178 (2015).
Wang, L. et al. Serotonin-1A receptor alterations in depression: a meta-analysis of molecular imaging studies. BMC Psychiatry 16, 319 (2016).
Jokinen, J., Nordstrom, A. L. & Nordstrom, P. CSF 5-HIAA and DST non-suppression — orthogonal biologic risk factors for suicide in male mood disorder inpatients. Psychiatry Res. 165, 96–102 (2009).
Miller, J. M. et al. Positron emission tomography quantification of serotonin transporter in suicide attempters with major depressive disorder. Biol. Psychiatry 74, 287–295 (2013).
Lutz, P. E. Multiple serotonergic paths to antidepressant efficacy. J. Neurophysiol. 109, 2245–2249 (2013).
Dracheva, S. et al. Increased serotonin 2C receptor mRNA editing: a possible risk factor for suicide. Mol. Psychiatry 13, 1001–1010 (2008).
Schmauss, C. Serotonin 2C receptors: suicide, serotonin, and runaway RNA editing. Neuroscientist 9, 237–242 (2003).
Di Narzo, A. F. et al. A unique gene expression signature associated with serotonin 2C receptor RNA editing in the prefrontal cortex and altered in suicide. Hum. Mol. Genet. 23, 4801–4813 (2014).
Weissmann, D. et al. Region-specific alterations of A-to-I RNA editing of serotonin 2C receptor in the cortex of suicides with major depression. Transl. Psychiatry 6, e878 (2016).
O’Connor, D. B., Ferguson, E., Green, J. A., O’Carroll, R. E. & O’Connor, R. C. Cortisol levels and suicidal behavior: a meta-analysis. Psychoneuroendocrinology 63, 370–379 (2016).
Melhem, N. M. et al. Blunted HPA axis activity in suicide attempters compared to those at high risk for suicidal behavior. Neuropsychopharmacology 41, 1447–1456 (2016).
Turecki, G. & Meaney, M. J. Effects of the social environment and stress on glucocorticoid receptor gene methylation: a systematic review. Biol. Psychiatry 79, 87–96 (2016).
Raison, C. L. & Miller, A. H. When not enough is too much: the role of insufficient glucocorticoid signaling in the pathophysiology of stress-related disorders. Am. J. Psychiatry 160, 1554–1565 (2003).
Roy, A., Gorodetsky, E., Yuan, Q., Goldman, D. & Enoch, M. A. Interaction of FKBP5, a stress-related gene, with childhood trauma increases the risk for attempting suicide. Neuropsychopharmacology 35, 1674–1683 (2010).
Lahti, J. et al. Associations between self-reported and objectively recorded early life stress, FKBP5 polymorphisms, and depressive symptoms in midlife. Biol. Psychiatry 80, 869–877 (2016).
Kaminsky, Z. et al. Epigenetic and genetic variation at SKA2 predict suicidal behavior and post-traumatic stress disorder. Transl. Psychiatry 5, e627 (2015).
Guintivano, J. et al. Identification and replication of a combined epigenetic and genetic biomarker predicting suicide and suicidal behaviors. Am. J. Psychiatry 171, 1287–1296 (2014).
Shopsin, B. The clinical antidepressant effect of exogenous agmatine is not reversed by parachlorophenylalanine: a pilot study. Acta Neuropsychiatr 25, 113–118 (2013).
Gawali, N. B. et al. Agmatine ameliorates lipopolysaccharide induced depressive-like behaviour in mice by targeting the underlying inflammatory and oxido-nitrosative mediators. Pharmacol. Biochem. Behav. 149, 1–8 (2016).
Dwivedi, Y. et al. Altered gene expression of brain-derived neurotrophic factor and receptor tyrosine kinase B in postmortem brain of suicide subjects. Arch. Gen. Psychiatry 60, 804–815 (2003).
Banerjee, R., Ghosh, A. K., Ghosh, B., Bhattacharyya, S. & Mondal, A. C. Decreased mRNA and protein expression of BDNF, NGF, and their receptors in the hippocampus from suicide: an analysis in human postmortem brain. Clin. Med. Insights Pathol. 6, 1–11 (2013).
Eisen, R. B. et al. Association between BDNF levels and suicidal behaviour: a systematic review and meta-analysis. Syst. Rev. 4, 187 (2015).
Grah, M. et al. Brain-derived neurotrophic factor as a suicide factor in mental disorders. Acta Neuropsychiatr. 26, 356–363 (2014).
Keller, S. et al. Increased BDNF promoter methylation in the Wernicke area of suicide subjects. Arch. Gen. Psychiatry 67, 258–267 (2010).
Kang, H. J. et al. BDNF promoter methylation and suicidal behavior in depressive patients. J. Affect. Disord. 151, 679–685 (2013).
Ernst, C., Chen, E. S. & Turecki, G. Histone methylation and decreased expression of TrkB.T1 in orbital frontal cortex of suicide completers. Mol. Psychiatry 14, 830–832 (2009).
Maussion, G. et al. Regulation of a truncated form of tropomyosin-related kinase B (TrkB) by Hsa-miR-185* in frontal cortex of suicide completers. PLOS ONE 7, e39301 (2012).
Stockmeier, C. A. et al. Cellular changes in the postmortem hippocampus in major depression. Biol. Psychiatry 56, 640–650 (2004).
Rajkowska, G. et al. Morphometric evidence for neuronal and glial prefrontal cell pathology in major depression. Biol. Psychiatry 45, 1085–1098 (1999).
Videbech, P. & Ravnkilde, B. Hippocampal volume and depression: a meta-analysis of MRI studies. Am. J. Psychiatry 161, 1957–1966 (2004).
Amaral, D. G. & Witter, M. P. The three-dimensional organization of the hippocampal formation: a review of anatomical data. Neuroscience 31, 571–591 (1989).
Chandley, M. J. et al. Gene expression deficits in pontine locus coeruleus astrocytes in men with major depressive disorder. J. Psychiatry Neurosci. 38, 276–284 (2013).
Chandley, M. J. et al. Elevated gene expression of glutamate receptors in noradrenergic neurons from the locus coeruleus in major depression. Int. J. Neuropsychopharmacol. 17, 1569–1578 (2014).
Sokolowski, M., Wasserman, J. & Wasserman, D. An overview of the neurobiology of suicidal behaviors as one meta-system. Mol. Psychiatry 20, 56–71 (2015).
Gray, A. L., Hyde, T. M., Deep-Soboslay, A., Kleinman, J. E. & Sodhi, M. S. Sex differences in glutamate receptor gene expression in major depression and suicide. Mol. Psychiatry 20, 1057–1068 (2015).
Zhao, J. et al. Prefrontal changes in the glutamate-glutamine cycle and neuronal/glial glutamate transporters in depression with and without suicide. J. Psychiatr. Res. 82, 8–15 (2016).
Price, R. B., Nock, M. K., Charney, D. S. & Mathew, S. J. Effects of intravenous ketamine on explicit and implicit measures of suicidality in treatment-resistant depression. Biol. Psychiatry 66, 522–526 (2009).
McGirr, A. et al. A systematic review and meta-analysis of randomized, double-blind, placebo-controlled trials of ketamine in the rapid treatment of major depressive episodes. Psychol. Med. 45, 693–704 (2015).
Ionescu, D. F. et al. Rapid and sustained reductions in current suicidal ideation following repeated doses of intravenous ketamine: secondary analysis of an open-label study. J. Clin. Psychiatry 77, e719–e725 (2016).
Ramaker, M. J. & Dulawa, S. C. Identifying fast-onset antidepressants using rodent models. Mol. Psychiatry 22, 656–665 (2017).
Wilkinson, S. T. et al. The effect of a single dose of intravenous ketamine on suicidal ideation: a systematic review and individual participant data meta-analysis. Am. J. Psychiatry 175, 150–158 (2018).
Stenovec, M. et al. Ketamine inhibits ATP-evoked exocytotic release of brain-derived neurotrophic factor from vesicles in cultured rat astrocytes. Mol. Neurobiol. 53, 6882–6896 (2016).
Grieco, S. F., Cheng, Y., Eldar-Finkelman, H., Jope, R. S. & Beurel, E. Up-regulation of insulin-like growth factor 2 by ketamine requires glycogen synthase kinase-3 inhibition. Prog. Neuropsychopharmacol. Biol. Psychiatry 72, 49–54 (2017).
Ren, Z. et al. Bidirectional homeostatic regulation of a depression-related brain state by gamma-aminobutyric acidergic deficits and ketamine treatment. Biol. Psychiatry 80, 457–468 (2016).
Klempan, T. A. et al. Altered expression of genes involved in ATP biosynthesis and GABAergic neurotransmission in the ventral prefrontal cortex of suicides with and without major depression. Mol. Psychiatry 14, 175–189 (2009).
Bunge, S. A., Klingberg, T., Jacobsen, R. B. & Gabrieli, J. D. A resource model of the neural basis of executive working memory. Proc. Natl Acad. Sci. USA 97, 3573–3578 (2000).
Zhang, J. X., Leung, H. C. & Johnson, M. K. Frontal activations associated with accessing and evaluating information in working memory: an fMRI study. Neuroimage 20, 1531–1539 (2003).
Herman, J. P., Ostrander, M. M., Mueller, N. K. & Figueiredo, H. Limbic system mechanisms of stress regulation: hypothalamo-pituitary-adrenocortical axis. Prog. Neuropsychopharmacol. Biol. Psychiatry 29, 1201–1213 (2005).
Raison, C. L., Capuron, L. & Miller, A. H. Cytokines sing the blues: inflammation and the pathogenesis of depression. Trends Immunol. 27, 24–31 (2006).
Brundin, L., Bryleva, E. Y. & Thirtamara Rajamani, K. Role of inflammation in suicide: from mechanisms to treatment. Neuropsychopharmacology 42, 271–283 (2017).
Kayser, M. S. & Dalmau, J. The emerging link between autoimmune disorders and neuropsychiatric disease. J. Neuropsychiatry Clin. Neurosci. 23, 90–97 (2011).
Courtet, P. et al. Neuroinflammation in suicide: toward a comprehensive model. World J. Biol. Psychiatry 17, 564–586 (2016).
Serafini, G. et al. The role of inflammatory cytokines in suicidal behavior: a systematic review. Eur. Neuropsychopharmacol. 23, 1672–1686 (2013).
Janelidze, S. et al. Low IL-8 is associated with anxiety in suicidal patients: genetic variation and decreased protein levels. Acta Psychiatr. Scand. 131, 269–278 (2015).
Black, C. & Miller, B. J. Meta-analysis of cytokines and chemokines in suicidality: distinguishing suicidal versus nonsuicidal patients. Biol. Psychiatry 78, 28–37 (2015).
Isung, J. et al. High interleukin-6 and impulsivity: determining the role of endophenotypes in attempted suicide. Transl. Psychiatry 4, e470 (2014).
Bergmans, R. S., Kelly, K. M. & Mezuk, B. Inflammation as a unique marker of suicide ideation distinct from depression syndrome among U.S. adults. J. Affect. Disord. 245, 1052–1060 (2019).
Ohlsson, L. et al. Leaky gut biomarkers in depression and suicidal behavior. Acta Psychiatr. Scand. 139, 185–193 (2019).
Isung, J., Mobarrez, F., Nordstrom, P., Asberg, M. & Jokinen, J. Low plasma vascular endothelial growth factor (VEGF) associated with completed suicide. World J. Biol. Psychiatry 13, 468–473 (2012).
Erhardt, S. et al. Connecting inflammation with glutamate agonism in suicidality. Neuropsychopharmacology 38, 743–752 (2013).
Pedersen, M. G., Mortensen, P. B., Norgaard-Pedersen, B. & Postolache, T. T. Toxoplasma gondii infection and self-directed violence in mothers. Arch. Gen. Psychiatry 69, 1123–1130 (2012).
Arling, T. A. et al. Toxoplasma gondii antibody titers and history of suicide attempts in patients with recurrent mood disorders. J. Nerv. Ment. Dis. 197, 905–908 (2009).
Flegr, J. How and why Toxoplasma makes us crazy. Trends Parasitol. 29, 156–163 (2013).
Okusaga, O. et al. Combined Toxoplasma gondii seropositivity and high blood kynurenine — linked with nonfatal suicidal self-directed violence in patients with schizophrenia. J. Psychiatr. Res. 72, 74–81 (2016).
Cook, T. B. et al. “Latent” infection with Toxoplasma gondii: association with trait aggression and impulsivity in healthy adults. J. Psychiatr. Res. 60, 87–94 (2015).
Peng, X. et al. Moderation of the relationship between Toxoplasma gondii seropositivity and trait impulsivity in younger men by the phenylalanine-tyrosine ratio. Psychiatry Res. 270, 992–1000 (2018).
Hall, A. B., Tolonen, A. C. & Xavier, R. J. Human genetic variation and the gut microbiome in disease. Nat. Rev. Genet. 18, 690–699 (2017).
Foster, J. A. & McVey Neufeld, K.-A. Gut–brain axis: how the microbiome influences anxiety and depression. Trends Neurosci. 36, 305–312 (2013).
Valles-Colomer, M. et al. The neuroactive potential of the human gut microbiota in quality of life and depression. Nat. Microbiol. 4, 623–632 (2019).
Franklin, J. C. et al. Risk factors for suicidal thoughts and behaviors: a meta-analysis of 50 years of research. Psychol. Bull. 143, 187–232 (2017).
Ribeiro, J. D. et al. Self-injurious thoughts and behaviors as risk factors for future suicide ideation, attempts, and death: a meta-analysis of longitudinal studies. Psychol. Med. 46, 225–236 (2016).
Glenn, C. R. & Nock, M. K. Improving the short-term prediction of suicidal behavior. Am. J. Prev. Med. 47, S176–S180 (2014).
Runeson, B. et al. Instruments for the assessment of suicide risk: a systematic review evaluating the certainty of the evidence. PLOS ONE 12, e0180292 (2017).
Quinlivan, L. et al. Predictive accuracy of risk scales following self-harm: multicentre, prospective cohort study. Br. J. Psychiatry 210, 429–436 (2017).
Chan, M. K. et al. Predicting suicide following self-harm: systematic review of risk factors and risk scales. Br. J. Psychiatry 209, 277–283 (2016).
Steeg, S. et al. Accuracy of risk scales for predicting repeat self-harm and suicide: a multicentre, population-level cohort study using routine clinical data. BMC Psychiatry 18, 113 (2018).
Ahmedani, B. K. et al. Health care contacts in the year before suicide death. J. Gen. Intern. Med. 29, 870–877 (2014).
Betz, M. E. et al. Reducing suicide risk: challenges and opportunities in the emergency department. Ann. Emerg. Med. 68, 758–765 (2016).
Boudreaux, E. D. et al. Improving suicide risk screening and detection in the emergency department. Am. J. Prev. Med. 50, 445–453 (2016).
Ballard, E. D. et al. Identification of at-risk youth by suicide screening in a pediatric emergency department. Prev. Sci. 18, 174–182 (2017).
Boudreaux, E. D. et al. Predictive utility of an emergency department decision support tool in patients with active suicidal ideation. Psychol. Serv. 15, 270–278 (2018).
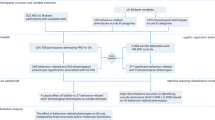
Miller, I. W. et al. Suicide prevention in an emergency department population: the ED-SAFE study. JAMA Psychiatry 74, 563–570 (2017). In this multicentre study conducted in 8 EDs, 1,376 patients were assigned to either usual care, univeral screen or universal screening plus a brief intervention, with only the latter resulting in a 5% risk reduction in suicide attempts in the subsequent year (OR = 0.72).
Simon, G. E. et al. Risk of suicide attempt and suicide death following completion of the Patient Health Questionnaire depression module in community practice. J. Clin. Psychiatry 77, 221–227 (2016).
King, C. A., Horwitz, A., Czyz, E. & Lindsay, R. Suicide risk screening in healthcare settings: identifying males and females at risk. J. Clin. Psychol. Med. Settings 24, 8–20 (2017).
Gibbons, R. D. et al. Development of a computerized adaptive test suicide scale — the CAT-SS. J. Clin. Psychiatry 78, 1376–1382 (2017).
Gibbons, R. D. et al. Computerized adaptive tests for rapid and accurate assessment of psychopathology dimensions in youth. J. Am. Acad. Child Adolesc. Psychiatry https://doi.org/10.1016/j.jaac.2019.08.009 (2019).
McCoy, T. H. Jr., Castro, V. M., Roberson, A. M., Snapper, L. A. & Perlis, R. H. Improving prediction of suicide and accidental death after discharge from general hospitals with natural language processing. JAMA Psychiatry 73, 1064–1071 (2016).
Anderson, H. D. et al. Monitoring suicidal patients in primary care using electronic health records. J. Am. Board Fam. Med. 28, 65–71 (2015).
Simon, G. E. et al. Predicting suicide attempts and suicide deaths following outpatient visits using electronic health records. Am. J. Psychiatry 175, 951–960 (2018). In this study of ~3 million patients, machine learning was used to predict suicide attempts and suicide deaths within 90 days of the last outpatient appointment in patients with a mental health diagnosis, with accuracy ranging between 0.83–0.85.
Belsher, B. E. et al. Prediction models for suicide attempts and deaths: a systematic review and simulation. JAMA Psychiatry 76, 642–651 (2019).
Silverman, M. M. & Felner, R. D. Suicide prevention programs: issues of design, implementation, feasibility, and developmental appropriateness. Suicide Life Threat. Behav. 25, 92–104 (1995).
Silverman, M. M. & Maris, R. W. The prevention of suicidal behaviors: an overview. Suicide Life Threat. Behav. 25, 10–21 (1995).
Mrazek, P. & Haggerty, R. Reducing Risks for Mental Disorders: Frontiers for Preventive Intervention Research (National Academy Press, 1994).
Gordon, R. S. Jr. An operational classification of disease prevention. Public Health Rep 98, 107–109 (1983).
Gunnell, D. et al. Prevention of suicide with regulations aimed at restricting access to highly hazardous pesticides: a systematic review of the international evidence. Lancet Glob. Health 5, e1026–e1037 (2017).
Hawton, K. et al. Six-year follow-up of impact of co-proxamol withdrawal in England and Wales on prescribing and deaths: time-series study. PLOS Med. 9, e1001213 (2012).
Yip, P. S. et al. Restricting the means of suicide by charcoal burning. Br. J. Psychiatry 196, 241–242 (2010).
Studdert, D. M., Gurrin, L. C., Jatkar, U. & Pirkis, J. Relationship between vehicle emissions laws and incidence of suicide by motor vehicle exhaust gas in Australia, 2001-06: an ecological analysis. PLOS Med. 7, e1000210 (2010).
Pirkis, J. et al. The effectiveness of structural interventions at suicide hotspots: a meta-analysis. Int. J. Epidemiol. 42, 541–548 (2013).
Pirkis, J. et al. Interventions to reduce suicides at suicide hotspots: a systematic review and meta-analysis. Lancet Psychiatry 2, 994–1001 (2015).
Pirkis, J., Blood, R. W., Beautrais, A., Burgess, P. & Skehans, J. Media guidelines on the reporting of suicide. Crisis 27, 82–87 (2006).
Maloney, J. et al. How to adjust media recommentations on reporting suicidal behaviour to new media developments. Arch. Suicide Res. 18, 156–169 (2014).
Robinson, J. et al. The #chatsafe project. Developing guidelines to help young people communicate safely about suicide on social media: a Delphi study. PLOS ONE 13, e0206584 (2018).
Gunnell, D., Derges, J., Chang, S. S. & Biddle, L. Searching for suicide methods: accessibility of information about helium as a method of suicide on the internet. Crisis 36, 325–331 (2015).
Pirkis, J. et al. Suicide prevention media campaigns: a systematic literature review. Health Commun. 34, 402–414 (2019).
Nicholas, A., Rossetto, A., Jorm, A., Pirkis, J. & Reavley, N. Importance of messages for a suicide prevention media campaign. Crisis 39, 438–450 (2018).
Wasserman, D. et al. School-based suicide prevention programmes: the SEYLE cluster-randomised, controlled trial. Lancet 385, 1536–1544 (2015).
Roskar, S. et al. Effects of training program on recognition and management of depression and suicide risk evaluation for Slovenian primary-care physicians: follow-up study. Croat. Med. J. 51, 237–242 (2010).
Saewyc, E. M., Konishi, C., Rose, H. A. & Homma, Y. School-based strategies to reduce suicidal ideation, suicide attempts, and discrimination among sexual minority and heterosexual adolescents in western Canada. Int. J. Child Youth Family Stud. 5, 89–112 (2014).
Hawton, K. et al. Psychosocial interventions following self-harm in adults: a systematic review and meta-analysis. Lancet Psychiatry 3, 740–750 (2016).
Kawanishi, C. et al. Assertive case management versus enhanced usual care for people with mental health problems who had attempted suicide and were admitted to hospital emergency departments in Japan (ACTION-J): a multicentre, randomised controlled trial. Lancet Psychiatry 1, 193–201 (2014).
Kapur, N. et al. Messages from Manchester: pilot randomised controlled trial following self-harm. Br. J. Psychiatry 203, 73–74 (2013).
Ramchand, R. et al. Characteristics and proximal outcomes of calls made to suicide crisis hotlines in California. Crisis 38, 26–35 (2017).
Middleton, A., Gunn, J., Bassilios, B. & Pirkis, J. Systematic review of research into frequent callers to crisis helplines. J. Telemed. Telecare 20, 89–98 (2014).
Predmore, Z. et al. Expanding suicide crisis services to text and chat responders’ perspectives of the differences between communication modalities. Crisis 38, 255–260 (2017).
Baker, S. T., Nicholas, J., Shand, F., Green, R. & Christensen, H. A comparison of multi-component systems approaches to suicide prevention. Australas Psychiatry 26, 128–131 (2018). This paper introduces the systems-based approach to suicide prevention and provides some key examples of where this is being used around the world.
Hegerl, U., Rummel-Kluge, C., Varnik, A., Arensman, E. & Koburger, N. Alliances against depression – a community based approach to target depression and to prevent suicidal behaviour. Neurosci. Biobehav. Rev. 37, 2404–2409 (2013).
Labouliere, C. D. et al. “Zero Suicide” – A model for reducing suicide in United States behavioral healthcare. Suicidologi 23, 22–30 (2018).
Wyman, P. A. et al. An outcome evaluation of the Sources of Strength suicide prevention program delivered by adolescent peer leaders in high schools. Am. J. Public Health 100, 1653–1661 (2010).
Knox, K. L., Litts, D. A., Talcott, G. W., Feig, J. C. & Caine, E. D. Risk of suicide and related adverse outcomes after exposure to a suicide prevention programme in the US Air Force: cohort study. BMJ 327, 1376 (2003).
Zalsman, G. et al. Suicide prevention strategies revisited: 10-year systematic review. Lancet Psychiatry 3, 646–659 (2016). The most up-to-date, comprehensive systematic review of the evidence for specific suicide prevention approaches.
Hawton, K. & Pirkis, J. Suicide is a complex problem that requires a range of prevention initiatives and methods of evaluation. Br. J. Psychiatry 210, 381–383 (2017). This paper discusses the need for rigorous and innovative evaluation methods in suicide prevention.
Bustamante Madsen, L., Eddleston, M., Schultz Hansen, K. & Konradsen, F. Quality assessment of economic evaluations of suicide and self-harm interventions: a systematic review. Crisis 39, 82–95 (2018).
Calati, R. & Courtet, P. Is psychotherapy effective for reducing suicide attempt and non-suicidal self-injury rates? Meta-analysis and meta-regression of literature data. J. Psychiatr. Res. 79, 8–20 (2016).
Erlangsen, A. et al. Short-term and long-term effects of psychosocial therapy for people after deliberate self-harm: a register-based, nationwide multicentre study using propensity score matching. Lancet Psychiatry 2, 49–58 (2015). An important study that demonstrates that psychosocial therapy after self-harm is linked to lower risks of repeated self-harm and suicide.
Tarrier, N., Taylor, K. & Gooding, P. Cognitive-behavioral interventions to reduce suicide behavior a systematic review and meta-analysis. Behav. Modif. 32, 77–108 (2008).
Rudd, M. D. et al. Brief cognitive-behavioral therapy effects on post-treatment suicide attempts in a military sample: results of a randomized clinical trial with 2-year follow-up. Am. J. Psychiatry 172, 441–449 (2015).
Witt, K. et al. Treatment as usual (TAU) as a control condition in trials of cognitive behavioural-based psychotherapy for self-harm: impact of content and quality on outcomes in a systematic review. J. Affect. Disord. 235, 434–447 (2018).
Chang, N. A., Jager-Hyman, S., Brown, G. K., Cunningham, A. & Stanley, B. in The International Handbook of Suicide Prevention (eds O’Connor, R. & Pirkis, J.) 416–430 (Wiley, Blackwell, 2016).
Oud, M., Arntz, A., Hermens, M. L. M., Verhoef, R. & Kendall, T. Specialized psychotherapies for adults with borderline personality disorder: a systematic review and meta-analysis. Aust. NZ J. Psych. 52, 949–961 (2018).
Linehan, M. M. et al. Two-year randomized controlled trial and follow-up of dialectical behavior therapy vs. therapy by experts for suicidal behaviors and borderline personality disorder. Arch. Gen. Psychiatry 63, 757–766 (2006).
Jobes, D. A. Managing Suicide Risk: A Collaborative Approach 2nd edn (Guilford Press, 2016).
Hayes, S. C., Strosahl, K. & Wilson, K. G. Acceptance and Commitment Therapy: An Experiential Approach to Behavior Change (Guilford Press, 1999).
Jobes, D. A. et al. A randomized controlled trial of the collaborative assessment and management of suicidality versus enhanced care as usual with suicidal soldiers. Psychiatry 80, 339–356 (2017).
Andreasson, K. et al. Effectiveness of dialectical behavior therapy versus collaborative assessment and management of suicidality treatment for reduction of self-harm in adults with borderline personality traits and disorder: a randomized observer-blinded clinical trial. Depress. Anxiety 33, 520–530 (2016).
Chesin, M. et al. Reviewing mindfulness-based interventions for suicidal behavior. Arch. Suicide Res. 20, 507–527 (2016).
Tighe, J., Nicholas, J., Shand, F. & Christensen, H. Efficacy of acceptance and commitment therapy in reducing suicidal ideation and deliberate self-harm: systematic review. JMIR Ment. Health 5, 11 (2018).
Ougrin, D., Tranah, T., Stahl, D., Moran, P. & Asarnow, J. R. Therapeutic interventions for suicide attempts and self-harm in adolescents: systematic review and meta-analysis. J. Am. Acad. Child Adolesc. Psychiatry 54, 97–107 (2015).
Hawton, K. et al. Interventions for self-harm in children and adolescents. Cochrane Database Syst. Rev. 12, CD012013 (2015).
Glenn, C. R., Esposito, E. C., Porter, A. C. & Robinson, D. J. Evidence base update of psychosocial treatments for self-injurious thoughts and behaviors in youth. J. Clin. Child Adolesc. Psychol. 48, 357–392 (2019).
Iyengar, U. et al. A further look at therapeutic interventions for suicide attempts and self-harm in adolescents: an updated systematic review of randomized controlled trials. Front. Psychiatry 9, 583 (2018).
Malda-Castillo, J., Browne, C. & Perez-Algorta, G. Mentalization-based treatment and its evidence-base status: a systematic literature review. Psychol. Psychother. https://doi.org/10.1111/papt.12195 (2018).
Okolie, C., Dennis, M., Thomas, E. S. & John, A. A systematic review of interventions to prevent suicidal behaviors and reduce suicidal ideation in older people. Int. Psychogeriatr. 29, 1801–1824 (2017).
Gustavson, K. A. et al. Problem-solving therapy reduces suicidal ideation in depressed older adults with executive dysfunction. Am. J. Geriatr. Psychiatr. 24, 11–17 (2016).
Heisel, M. J., Talbot, N. L., King, D. A., Tu, X. M. & Duberstein, P. R. Adapting interpersonal psychotherapy for older adults at risk for suicide. Am. J. Geriatr. Psychiatr. 23, 87–98 (2015).
Riblet, N. B. V., Shiner, B., Young-Xu, Y. & Watts, B. V. Strategies to prevent death by suicide: meta-analysis of randomised controlled trials. Br. J. Psychiatry 210, 396-402 (2017).
Henderson, C., Evans-Lacko, S. & Thornicroft, G. Mental illness stigma, help seeking, and public health programs. Am. J. Public Health 103, 777–780 (2013).
Motto, J. A. Suicide prevention for high-risk persons who refuse treatment. Suicide Life Threat. Behav 6, 223–230 (1976).
Comtois, K. A. et al. Effect of augmenting standard care for military personnel with brief caring text messages for suicide prevention: a randomized clinical trial. JAMA Psychiatry 76, 474–483 (2019).
Stanford, E. J., Goetz, R. R. & Bloom, J. D. The no harm contract in the emergency assessment of suicidal risk. J. Clin. Psychiat. 55, 344–348 (1994).
Stanley, B. & Brown, G. K. Safety planning intervention: a brief intervention to mitigate suicide risk. Cognit. Behav. Pract. 19, 256–264 (2012).
Stanley, B. et al. Comparison of the safety planning intervention with follow-up vs usual care of suicidal patients treated in the emergency department. JAMA Psychiatry 75, 894–900 (2018). A landmark study that highlights the use of safety planning with telephone support.
Bryan, C. J. et al. Effect of crisis response planning vs. contracts for safety on suicide risk in U.S. Army soldiers: a randomized clinical trial. J. Affect. Disord. 212, 64–72 (2017).
Gysin-Maillart, A., Schwab, S., Soravia, L., Megert, M. & Michel, K. A novel brief therapy for patients who attempt suicide: a 24-months follow-up randomized controlled study of the attempted suicide short intervention program (ASSIP). PLOS Med. 13, e1001968 (2016).
O’Connor, R. C. et al. A brief psychological intervention to reduce repetition of self-harm in patients admitted to hospital following a suicide attempt: a randomised controlled trial. Lancet Psychiatry 4, 451–460 (2017).
King, C. A., Gipson, P. Y., Horwitz, A. G. & Opperman, K. J. Teen options for change: an intervention for young emergency patients who screen positive for suicide risk. Psychiatr. Serv. 66, 97–100 (2015).
Kennard, B. D. et al. As Safe as Possible (ASAP): a brief app-supported inpatient intervention to prevent postdischarge suicidal behavior in hospitalized, suicidal adolescents. Am. J. Psychiatry 175, 864–872 (2018).
Coppen, A. et al. Does lithium reduce the mortality of recurrent mood disorders? J. Affect. Disord 23, 1–7 (1991).
Felber, W., Bauer, M., Lewitzka, U. & Muller-Oerlinghausen, B. Lithium clinics in Berlin and Dresden: a 50-year experience. Pharmacopsychiatry 51, 166–171 (2018).
Ahearn, E. P. et al. Suicide attempts in veterans with bipolar disorder during treatment with lithium, divalproex, and atypical antipsychotics. J. Affect. Disord 145, 77–82 (2013).
Hayes, J. F. et al. Self-harm, unintentional injury, and suicide in bipolar disorder during maintenance mood stabilizer treatment: a UK population-based electronic health records study. JAMA Psychiatry 73, 630–637 (2016).
Song, J. et al. Suicidal behavior during lithium and valproate treatment: a within-individual 8-year prospective study of 50,000 patients with bipolar disorder. Am. J. Psychiatry 174, 795–802 (2017).
Lauterbach, E. et al. Adjunctive lithium treatment in the prevention of suicidal behaviour in depressive disorders: a randomised, placebo-controlled, 1-year trial. Acta Psychiatr. Scand. 118, 469–479 (2008).
Oquendo, M. A. et al. Treatment of suicide attempters with bipolar disorder: a randomized clinical trial comparing lithium and valproate in the prevention of suicidal behavior. Am. J. Psychiatry 168, 1050–1056 (2011).
Girlanda, F. et al. Effectiveness of lithium in subjects with treatment-resistant depression and suicide risk: results and lessons of an underpowered randomised clinical trial. BMC Res. Notes 7, 731 (2014).
Khan, A. et al. Differential pattern of response in mood symptoms and suicide risk measures in severely ill depressed patients assigned to citalopram with placebo or citalopram combined with lithium: role of lithium levels. J. Psychiatr. Res. 45, 1489–1496 (2011).
Cipriani, A., Hawton, K., Stockton, S. & Geddes, J. R. Lithium in the prevention of suicide in mood disorders: updated systematic review and meta-analysis. BMJ 346, f3646 (2013).
Gibbons, R. D., Hur, K., Brown, C. H. & Mann, J. J. Relationship between antiepileptic drugs and suicide attempts in patients with bipolar disorder. Arch. Gen. Psychiatry 66, 1354–1360 (2009).
Chen, T. Y. et al. Divalproex and its effect on suicide risk in bipolar disorder: a systematic review and meta-analysis of multinational observational studies. J. Affect. Disord 245, 812–818 (2019).
Meltzer, H. Y. et al. Clozapine treatment for suicidality in schizophrenia: International Suicide Prevention Trial (InterSePT). Arch. Gen. Psychiatry 60, 82–91 (2003).
Vermeulen, J. M. et al. Clozapine and long-term mortality risk in patients with schizophrenia: a systematic review and meta-analysis of studies lasting 1.1-12.5 years. Schizophr. Bull. 45, 315–329 (2018).
Warnez, S. & Alessi-Severini, S. Clozapine: a review of clinical practice guidelines and prescribing trends. BMC Psychiatry 14, 102 (2014).
Reinstatler, L. & Youssef, N. A. Ketamine as a potential treatment for suicidal ideation: a systematic review of the literature. Drugs R D 15, 37–43 (2015).
Duman, R. S. Ketamine and rapid-acting antidepressants: a new era in the battle against depression and suicide. F1000Res 7, https://doi.org/10.12688/f1000research.14344.1 (2018).
Murrough, J. W. et al. Ketamine for rapid reduction of suicidal ideation: a randomized controlled trial. Psychol. Med. 45, 3571–3580 (2015).
Grunebaum, M. F. et al. Ketamine for rapid reduction of suicidal thoughts in major depression: a midazolam-controlled randomized clinical trial. Am. J. Psychiatry 175, 327–335 (2018).
Grunebaum, M. F. et al. Ketamine versus midazolam in bipolar depression with suicidal thoughts: a pilot midazolam-controlled randomized clinical trial. Bipolar Disord. 19, 176–183 (2017).
Price, R. B. et al. Effects of ketamine on explicit and implicit suicidal cognition: a randomized controlled trial in treatment-resistant depression. Depress. Anxiety 31, 335–343 (2014).
Vande Voort, J. L. et al. Antisuicidal response following ketamine infusion is associated with decreased nighttime wakefulness in major depressive disorder and bipolar disorder. J. Clin. Psychiatry 78, 1068–1074 (2017).
Kearns, J. C. et al. Sleep problems and suicide risk in youth: a systematic review, developmental framework, and implications for hospital treatment. Gen. Hosp. Psychiatry https://doi.org/10.1016/j.genhosppsych.2018.09.011 (2018).
Canuso, C. M. et al. Efficacy and safety of intranasal esketamine for the rapid reduction of symptoms of depression and suicidality in patients at imminent risk for suicide: results of a double-blind, randomized, placebo-controlled study. Am. J. Psychiatry 175, 620–630 (2018).
Gonella, G., Baignoli, G. & Ecari, U. Fluvoxamine and imipramine in the treatment of depressive patients: a double-blind controlled study. Curr. Med. Res. Opin. 12, 177–184 (1990).
Kasper, S., Moller, H. J., Montgomery, S. A. & Zondag, E. Antidepressant efficacy in relation to item analysis and severity of depression: a placebo-controlled trial of fluvoxamine versus imipramine. Int. Clin. Psychopharmacol. 9 (Suppl. 4), 3–12 (1995).
Montgomery, S., Cronholm, B., Asberg, M. & Montgomery, D. B. Differential effects on suicidal ideation of mianserin, maprotiline and amitriptyline. Br. J. Clin. Pharmacol. 5 (Suppl. 1), 77S–80S (1978).
Mahapatra, S. N. & Hackett, D. A randomised, double-blind, parallel-group comparison of venlafaxine and dothiepin in geriatric patients with major depression. Int. J. Clin. Pract. 51, 209–213 (1997).
Sacchetti, E., Vita, A., Guarneri, L. & Cornacchia, M. in Serotonin-related Psychiatric Syndromes: Clinical and Therapeutic Links (eds G. B. Cassano et al.) 47–53 (R. Soc. Med. Services, 1991).
Marchesi, C., Ceccherininelli, A., Rossi, A. & Maggini, C. Is anxious-agitated major depression responsive to fluoxetine? A double-blind comparison with amitriptyline. Pharmacopsychiatry 31, 216–221 (1998).
Judd, F. K. et al. A multicentre double blind trial of fluoxetine versus amitriptyline in the treatment of depressive illness. Aust. NZ J. Psychiatry 27, 49–55 (1993).
Lapierre, Y. D. Controlling acute episodes of depression. Int. Clin. Psychopharmacol. 6 (Suppl. 2), 23–35 (1991).
Moller, H. J. & Steinmeyer, E. M. Are serotonergic reuptake inhibitors more potent in reducing suicidality? An empirical study on paroxetine. Eur. Neuropsychopharmacol. 4, 55–59 (1994).
Tollefson, G. D. et al. Is baseline agitation a relative contraindication for a selective serotonin reuptake inhibitor: a comparative trial of fluoxetine versus imipramine. J. Clin. Psychopharmacol. 14, 385–391 (1994).
Grunebaum, M. F. et al. Pilot randomized clinical trial of an SSRI vs bupropion: effects on suicidal behavior, ideation, and mood in major depression. Neuropsychopharmacology 37, 697–706 (2012).
Stone, M. et al. Risk of suicidality in clinical trials of antidepressants in adults: analysis of proprietary data submitted to US Food and Drug Administration. BMJ 339, b2880 (2009).
Yovell, Y. et al. Ultra-low-dose buprenorphine as a time-limited treatment for severe suicidal ideation: a randomized controlled trial. Am. J. Psychiatry 173, 491–498 (2016).
Ahmadi, J., Jahromi, M. S. & Ehsaei, Z. The effectiveness of different singly administered high doses of buprenorphine in reducing suicidal ideation in acutely depressed people with co-morbid opiate dependence: a randomized, double-blind, clinical trial. Trials 19, 462 (2018).
Lutz, P. E., Courtet, P. & Calati, R. The opioid system and the social brain: implications for depression and suicide. J. Neurosci. Res. https://doi.org/10.1002/jnr.24269 (2018).
Fairweather-Schmidt, A. K., Batterham, P. J., Butterworth, P. & Nada-Raja, S. The impact of suicidality on health-related quality of life: a latent growth curve analysis of community-based data. J. Affect. Disord. 203, 14–21 (2016).
Grendas, L. et al. Determinants of mental and physical health-related quality of life among patients hospitalized for suicidal behavior. Psychiatry Res. 257, 56–60 (2017).
Goldman-Mellor, S. J. et al. Suicide attempt in young people: a signal for long-term health care and social needs. JAMA Psychiatry 71, 119–127 (2014).
Stoddard, F. J. & Saxe, G. Ten-year research review of physical injuries. J. Am. Acad. Child Adolesc. Psychiatry 40, 1128–1145 (2001).
Mitchell, A. M., Sakraida, T. J., Kim, Y., Bullian, L. & Chiappetta, L. Depression, anxiety and quality of life in suicide survivors: a comparison of close and distant relationships. Arch. Psychiatr. Nurs. 23, 2–10 (2009).
Carpiniello, B. & Pinna, F. The reciprocal relationship between suicidality and stigma. Front. Psychiatry 8, 35 (2017).
Shepard, D. S., Gurewich, D., Lwin, A. K., Reed, G. A. Jr & Silverman, M. M. Suicide and suicidal attempts in the United States: costs and policy implications. Suicide Life Threat. Behav. 46, 352–362 (2016).
Borges, G. et al. Twelve-month prevalence of and risk factors for suicide attempts in the World Health Organization World Mental Health surveys. J. Clin. Psychiatry 71, 1617–1628 (2010).
Acknowledgements
G.T. holds a Canada Research Chair (Tier 1) and is supported by grants from the Canadian Institute of Health Research (CIHR) (FDN148374, EGM141899, ENP161427), and by the Fonds de Recherche du Québec – Santé (FRQS) through the Quebec Network on Suicide, Mood Disorders and Related Disorders. D.A.B. receives research support from US National Institute of Mental Health (NIMH), American Foundation for Suicide Prevention (AFSP), the Once Upon a Time Foundation and the Beckwith Foundation, and salary support from the University of Pittsburgh, University of Pittsburgh Physicians (UPP), NIMH and AFSP. The authors are indebted to Sylvanne Daniels, McGill University, for essential help in the preparation of this Primer.
Author information
Authors and Affiliations
Contributions
Aside from G.T., authors are listed in alphabetical order. Introduction (G.T.); Epidemiology (D.G.); Mechanisms/pathophysiology (G.T. and D.G.); Diagnosis, screening and prevention (D.A.B. and J.P.); Management (B.H.S., R.C.O’C. and M.A.O.); Quality of life (G.T.); Outlook (G.T.); Overview of Primer (G.T.).
Corresponding author
Ethics declarations
Competing interests
D.A.B. receives royalties from Guilford Press, from the electronic self-rated version of the Columbia Suicide Severity Rating Scale (C-SSRS) from eRT Inc., and from performing duties as an UptoDate Psychiatry Section Editor. He receives consulting fees from Healthwise, and receives honoraria from the Klingenstein Third Generation Foundation for scientific board membership and grant review. D.G. is a member of the Department of Health for England’s National Suicide Prevention Advisory Committee, Samaritans Policy and Research Committee and Movember’s Global Advisory Committee. M.A.O. receives royalties for commercial use of the C-SSRS and her family owns stock in Bristol Myers Squibb. B.H.S. receives royalties from the Research Foundation for Mental Hygiene, Inc., for the commercial use of the C-SSRS. The remaining authors declare no competing interests.
Additional information
Peer review information
Nature Reviews Disease Primers thanks E. Boudreaux, Y. Conwell, C. King and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
The Joint Commission: https://www.jointcommission.org/assets/1/6/NPSG_Chapter_HAP_Jan2019.pdf
Supplementary information
Rights and permissions
About this article
Cite this article
Turecki, G., Brent, D.A., Gunnell, D. et al. Suicide and suicide risk. Nat Rev Dis Primers 5, 74 (2019). https://doi.org/10.1038/s41572-019-0121-0
Accepted:
Published:
DOI: https://doi.org/10.1038/s41572-019-0121-0
This article is cited by
-
Sex-related inequalities in crude and age-standardized suicide rates: trends in Ghana from 2000 to 2019
BMC Public Health (2024)
-
The short-term effect of ambient particulate matter on suicide death
Environmental Health (2024)
-
Associations of altered leukocyte DDR1 promoter methylation and childhood trauma with bipolar disorder and suicidal behavior in euthymic patients
Molecular Psychiatry (2024)
-
Neural correlates of automatic emotion regulation and their association with suicidal ideation in adolescents during the first 90-days of residential care
Translational Psychiatry (2024)
-
Machine learning and the prediction of suicide in psychiatric populations: a systematic review
Translational Psychiatry (2024)