Abstract
The European Collaborative on Personalized Early Detection and Prevention of Breast Cancer (ENVISION) brings together several international research consortia working on different aspects of the personalized early detection and prevention of breast cancer. In a consensus conference held in 2019, the members of this network identified research areas requiring development to enable evidence-based personalized interventions that might improve the benefits and reduce the harms of existing breast cancer screening and prevention programmes. The priority areas identified were: 1) breast cancer subtype-specific risk assessment tools applicable to women of all ancestries; 2) intermediate surrogate markers of response to preventive measures; 3) novel non-surgical preventive measures to reduce the incidence of breast cancer of poor prognosis; and 4) hybrid effectiveness–implementation research combined with modelling studies to evaluate the long-term population outcomes of risk-based early detection strategies. The implementation of such programmes would require health-care systems to be open to learning and adapting, the engagement of a diverse range of stakeholders and tailoring to societal norms and values, while also addressing the ethical and legal issues. In this Consensus Statement, we discuss the current state of breast cancer risk prediction, risk-stratified prevention and early detection strategies, and their implementation. Throughout, we highlight priorities for advancing each of these areas.
Similar content being viewed by others
Introduction
Worldwide, breast cancer is the second most commonly diagnosed cancer, with approximately 2.1 million new diagnoses and almost 627,000 breast cancer-related deaths estimated to have occurred in 2018 (ref.1). Breast cancer is a biologically and clinically heterogeneous disease, with several recognized histotypes and molecular subtypes that have different aetiologies, profiles of risk factors, responses to treatments and prognoses2,3,4,5,6,7,8. In high-income countries, approximately 75% of breast cancers are diagnosed in postmenopausal women, although around 5–7% are diagnosed in women younger than 40 years of age9,10.
The risk of developing breast cancer varies among women. Genetic susceptibility, factors affecting levels of endogenous hormones (early age at menarche, later age at menopause, nulliparity, late age at first birth, having fewer children and shorter durations of breastfeeding), exogenous hormone intake (hormonal contraceptive use and hormone replacement therapy), lifestyle patterns (high alcohol intake, smoking and physical inactivity), anthropometric characteristics (greater weight, weight gain during adulthood and higher central body fat distribution), a high mammographic breast density and benign breast diseases (non-proliferative disease, proliferative disease without atypia and atypical hyperplasia) are all associated with an increased risk of breast cancer11,12,13,14. At an individual level, the mechanisms and relative contributions of these different risk factors to the development of breast cancer and also to particular subtypes of the disease are increasingly understood15.
Women with pathogenic germline mutations in cancer susceptibility genes — that is, in BRCA1 or BRCA2 (BRCA1/2) — may opt to undergo prophylactic bilateral mastectomy; primary chemoprophylaxis with tamoxifen or other selective oestrogen receptor modulators has also been recommended in this group, albeit the uptake is low16. Historically, members of this high-risk group have been identified on an opportunistic basis following self-referral of women with a family history of breast or ovarian cancer, or on the basis of an ancestry associated with an increased prevalence of clinically significant pathogenic variants of BRCA1/2 (for example, in those of Jewish descent)16. Currently, genetic testing remains somewhat restricted for women with breast cancer; those with triple-negative, bilateral or young-onset disease might be offered a test at diagnosis, but most will be offered testing only if they also have a noted family history of the disease16. The 2019 US Preventive Services Task Force recommendations expand the population in which eligibility for genetic testing should be assessed to include women with a personal or family history of breast, ovarian, tubal or peritoneal cancer, in addition to women who have an ancestry associated with pathogenic BRCA1/2 variants17.
At present, the mammographic screening programmes used for early detection of breast cancer in most high-income countries are based on the results of trials conducted at least 20–30 years ago18,19,20,21,22 and have age as the only entry criterion, although the starting and stopping ages (varying from 40 to 74 years) and the frequency of screens (yearly to triennially) differ between countries. This ‘one-size-fits-all’ approach does not take into account the heterogeneity of the breast cancer subtypes and of the risk in the population. Three decades of mammographic early detection have witnessed an increase in the incidence of early stage cancers with a low-risk tumour biology and an increase in the detection of in situ disease, without a concomitant proportionate decrease in incidence of advanced-stage disease23,24. Increasingly, calls have been made for a new approach to early detection with a focus on the identification of more consequential cancers and on avoiding the detection of indolent or ultra-low-risk disease24,25.
Personalized approaches to the prevention or early detection of breast cancer have emerged as highly promising strategies26,27. These programmes require risk assessment of each woman in the population, stratification of the population into several risk groups, assignment of the individuals to a specific risk group and tailoring of prevention and early detection interventions to each risk group28 (Fig. 1). Several international research consortia (Table 1) are studying ways to better understand, estimate and reduce breast cancer risk29,30,31,32, to use risk-based stratification to prevent consequential cancers33,34, to evaluate the benefit–harm trade-offs of such strategies35 and to assess the acceptability and feasibility of implementing risk-stratified prevention and early detection programmes36,37,38.
Women entering a personalized early detection programme would initially be assessed using a validated tool to determine their estimated risk of breast cancer. Subsequently, the women would be stratified into appropriate risk groups such that they can receive tailored interventions. This approach might mean that some women start mammographic screening at a younger age, have different screening intervals or have supplemental screening with another imaging modality, such as MRI. Women deemed to be at higher risk of breast cancer could, in addition, be offered prophylactic treatment. A healthy lifestyle would be recommended to all women, independent of risk level.
To fulfil the promise of risk-stratified breast cancer prevention and screening, it is important not only to generate evidence on the individual component ‘jigsaw pieces’ of prevention and early detection programmes, but also to bring these pieces together in a complex adaptive system39. The European Collaborative on Personalized Early Detection and Prevention of Breast Cancer (ENVISION) comprises leading international research consortia working in this specific field (Table 1). In 2019, the ENVISION network organized a consensus conference to identify research priorities and recommend actions required to enable evidence-based risk-stratified prevention and early detection programmes for breast cancer (Box 1; Supplementary Table 1).
In this Consensus Statement, we review the current knowledge, explore the barriers and opportunities, and define key areas for the development and implementation of risk assessment, risk-stratified prevention and early detection programmes for breast cancer. As representatives of the ENVISION network, we also present herein the recommendations formulated at the 2019 consensus conference (Box 2) in the hope that they stimulate and guide such programmes.
Risk assessment for breast cancer
Established risk factors
Breast cancer risk can be predicted using a combination of common genetic variants, mostly single-nucleotide polymorphisms (SNPs); rare coding variants of susceptibility genes, including BRCA1/2, PALB2, CHEK2 and ATM; mammographic breast density; benign abnormalities in breast biopsy specimens; hormonal, anthropometric and lifestyle factors; family history of the disease; and, potentially, epigenetic markers11,13,40,41,42,43. Genome-wide association studies (GWAS) have resulted in the identification of >180 independent common genetic variants that together account for ~20% of the familial relative risk of breast cancer and ~40% of the heritability attributed to all common variants on genome-wide SNP arrays40,41. Each variant confers a small risk, but their effects can be combined into polygenic risk scores (PRSs) that are predictive of the risk of developing breast cancer, thereby enabling breast cancer risk stratification in the general population44,45,46.
The performance of current PRSs has been thoroughly validated in European populations44. The relative risks associated with individual SNPs and PRSs vary between breast cancer subtypes, with oestrogen receptor-positive (ER+) disease being more strongly predicted than other forms of the disease40,41,44. The current best performing PRS is based on 313 SNPs (PRS313): women in the highest 1% of the risk distribution have an approximately fourfold and threefold greater risk of developing ER+ and ER− breast cancers, respectively, compared with women in the middle quintile (40–60th percentile)44. The risk reflected in the PRSs seems to be independent of other established risk factors — that is, the effects are approximately multiplicative43. PRS313 provides the highest level of breast cancer risk stratification in the population, followed by mammographic breast density and the other risk factors45,47.
Protein-truncating variants (PTVs) in approximately 12 genes are associated with breast cancer risk42,48; for some, the strength of association has been demonstrated to differ between ER+ and ER− disease49,50. The risk estimates for PTVs of some genes are, however, very imprecise (Table 2). Missense mutations in a subset of these genes have also been associated with an increased risk of breast cancer42,51,52,53. Evidence from in silico and functional studies can help to define this subset of cancers with non-truncating variants54,55,56. For rare individual variants associated with risk, however, the level of risk that they impart remains uncertain. Most genes tested using commercial multigene panels have not been systematically investigated as breast cancer susceptibility genes. The Clinical Genome Resource (ClinGen) framework has assessed the strength of evidence between selected putative susceptibility genes and breast cancer and established definitive clinical validity classifications for only 10 of 31 genes commonly tested when evaluating breast cancer risk57 (Table 2).
Emerging risk factors
The epigenome consists of various ‘layers’, including non-coding RNAs, histone modification and DNA methylation, and has an essential role in establishing the identity and function of any given cell by determining which genes remain silent and which are transcribed. A plethora of changes in DNA-methylation patterns have been described in breast cancers, and several of these changes are often also present in the non-malignant breast tissue adjacent to the cancer58, supporting the principle that an epigenetic field defect renders cells of these tissues susceptible to malignant transformation59. In addition to genetic background60,61, a large variety of non-genetic factors, including age62 and endocrine disruption63,64, that are known to modulate breast cancer risk also alter patterns of DNA methylation. On the basis of these insights, one might speculate that epigenetic profiles could predict breast cancer risk.
To date, several groups have attempted to develop epigenetic risk classifiers for breast cancer but with only modest success, which could be due to several reasons65. First, the vast majority of the studies to date used only blood samples for DNA-methylation analyses. Blood is readily available from participants of several large cohort studies61,66, but breast cancer is, by definition, an epithelial disease, and hence immune cells in the blood might not be an appropriate surrogate tissue for those of the breast. Second, unlike in germline genetic analyses, the timing of the sample collection for epigenetic analyses is crucial. For example, epigenetic analyses using samples obtained from women during cancer treatment are likely to produce results that reflect treatment effects and not cancer predisposition. Third, unlike PRSs, which are established by combining individual SNPs with risk associations that remain statistically significant after multiple test adjustment, epigenetic risk signatures are reflective of cell programmes; therefore, approaches that a priori select a large number of CpGs for inclusion in the epigenetic signatures are more likely to be appropriate. Fourth, the presence of a cancer can modify the epigenome of a particular surrogate tissue. For example, a higher granulocyte to lymphocyte ratio is detected in the blood of patients with ovarian cancer, which subsequently alters the DNA-methylation signature observed when assessing peripheral blood mononuclear cells67. Thus, validation of risk-predictive signatures in population-based cohorts is important; however, the majority of the existing cohorts do not have appropriate samples available (owing to non-standardized collection, storage conditions and times, and so on), which makes this validation process prone to producing false-negative results.
Nevertheless, DNA-methylation signatures in easy-to-collect surrogate tissues hold promise, not only in advancing risk-prediction strategies, but also, of equal importance, in providing novel opportunities to monitor the effects of cancer-preventive measures. In addition to epigenetic markers, serum levels of steroid hormones68,69,70 and a double-strand DNA break-repair phenotype of peripheral blood cells71,72 have substantial potential to identify women with a high risk of developing breast cancer.
Risk-prediction models
Several breast cancer risk-prediction models are available. Empirical models such as the Gail model73, the Breast Cancer Surveillance Consortium (BCSC) risk calculator74 and the Individualized Coherent Absolute Risk Estimator (iCARE)75,76,77 do not consider explicit genetic models of inheritance and are primarily intended for use in women in the general population. By contrast, genetic models such as Tyrer–Cuzick78 and BOADICEA45,79 can, in principle, accommodate detailed family history information (including the exact pedigree structure and information on distant relatives) and can, therefore, be applied both at the general population level and in women with a strong family history of breast cancer. These models all vary in terms of the risk factors considered, the study designs and types of data used in their development, and their analytical methods. The validity and clinical utility of these risk-assessment tools must be demonstrated before they are implemented routinely in the clinical setting80.
Validity
Analytical validity refers to the accuracy of the test in measuring the underlying genotypes (for example, through gene-panel testing or sequencing assay for rare mutations), PRSs (for example, using SNP-genotyping technologies) and other lifestyle and hormonal risk factors (which can be self-reported or available through electronic health records). Importantly, the analytical validity of comprehensive breast cancer risk-prediction models also depends on having reliable relative risk estimates for the effects of the various risk factors; having precise risk estimates of the associations with individual rare and common genetic variants; as well as estimates of the joint effects of common genetic variants, the joint effects of common and rare genetic variants, and the combined effects of genetic and other risk factors, including a family history of cancer. Clinical validity refers to the accuracy of the tool in predicting the occurrence of breast cancer.
Ideally, the individual and combined associations of the various risk factors should be derived from large, well-designed cohort studies that are representative of the population in which the models are intended to be applied. However, cohorts with data that include information on all known risk factors are not widely available; therefore, synthetic mathematical approaches have been developed that combine the risk-factor distributions from separate cohorts45,75,76. Data generated by the B-CAST29, BRIDGES30, BCAC81 and CIMBA82 consortia (Table 1) provide a platform for estimating the individual and combined risk-factor distributions and breast cancer risk and have been used in the development of the iCARE77 and BOADICEA45 breast cancer risk-predication models. Some empirical models, which are commercially available, have been modified to incorporate breast cancer PRSs, but without accounting for the fact that PRSs explain a large fraction of the familial relative risk of breast cancer. The failure to adjust these models to account for family history of breast cancer results in substantial levels of miscalibration in different risk categories and subsequently compromises the clinical validity of the model46.
With regard to clinical validity, several validation studies assessing model calibration (that is, the agreement between the predicted and the observed risk) or discrimination (the ability of a risk score to discriminate between those who will and those who will not develop the disease) in large independent cohorts have been published83,84. The interpretation of the literature is challenging, however, because these studies have not necessarily assessed both model calibration and discrimination in the same sample. Moreover, head-to-head comparisons of risk models using the same datasets are lacking. Often the published validation studies have used older versions of the risk models without data on all model components (in particular, mammographic breast density), have limited sample sizes and have varying timescales over which predictions are made, which depend on the follow-up duration of the study.
Ongoing studies by B-CAST29 and BRIDGES30 aim to address these issues by evaluating risk-assessment models in multiple prospective cohorts of women initially without breast cancer in diverse settings. Preliminary results indicate that the iCARE77,85 and BOADICEA45 models have well calibrated categories of predicted risk and discriminate well between women who develop breast cancer over 5–10 years of follow-up study from those who do not84. As such, these models provide valid risk-prediction tools that can be used in clinical practice.
Clinical utility
Conceptually, clinical utility refers to the usefulness, benefits and harms of an intervention86,87. Clinical utility is a multidimensional construct covering effectiveness and cost-effectiveness, as well as the psychosocial, ethical and legal implications of an intervention86. Risk assessment per se does not have inherent clinical utility; the subsequent adoption of a risk-based intervention based on the results of the assessment is what influences the health outcomes88. The use of such a strategy depends on whether the risk-based intervention is appropriate, accessible, practicable and acceptable86. The interactions of these factors and challenges in assessing them are discussed in more detail in later sections of this article (Fig. 2).
Various questions will define the risk-stratified programme, including which risk factors to include in risk assessments, what risk threshold to use for risk stratification, how many risk groups to have, when to do risk assessments, how often to screen and to whom screening should be offered, as well as which interventions should be used in individuals deemed to be at high risk. Decision-making regarding these questions will be influenced by the research evidence, the available resources, the health-care setting and societal values, preferences and social norms. The choices made in addressing each of these questions will determine whether the programme will be effective in reducing cancer-specific death and improving the benefit–harm balance of screening and be cost-effective, acceptable, accessible and feasible to implement. Dynamic interactions exist between each of these factors, and thus a change in one factor affects all others. Hence, the importance of a holistic, ‘systems thinking’ approach.
Future directions in risk prediction
We have identified several key areas for development in breast cancer risk modelling (Box 2). These research priorities include models that better predict the risk of specific subtypes of breast cancer and with improved risk stratification of women of all ancestries, particularly non-European ancestries, who have been understudied to date.
Subtyping of breast cancer is currently used routinely in prognostication and treatment, although its use in the context of prevention and early detection of the disease is limited. The ability to predict susceptibility to the typically more aggressive, ER− forms of breast cancer would enable selection of women for enhanced surveillance. Better datasets containing both clinical and genetic data are essential to develop and validate models that can more accurately predict subtype-specific risk, pathobiological behaviour and clinical outcomes. For example, B-CAST29 and BRIDGES30 are developing such data sources that integrate genetic, epidemiological, pathological and clinical data.
Multiancestry GWAS and targeted DNA-sequencing data from individuals of various ethnicities will enable translation of PRS-based and gene-based risks to populations of non-European ancestry. Heritability analyses indicate that breast cancer is a highly polygenic disease, with thousands of variants conferring a small effect on risk, and that larger studies would result in new discoveries89. The Confluence project89 aims to build a dataset comprising >300,000 patients with breast cancer and 300,000 individuals without the disease in order to conduct a multiancestry GWAS. This study will enable better understanding of the aetiology of distinct breast cancer subtypes, more powerful modelling of the underlying polygenic risk and improve risk stratification across groups of women with different ancestries.
A large fraction of the unexplained heritability of breast cancer might be attributable to rare variants (allele frequency <0.1%) not captured on SNP arrays90. Exome sequencing and replication studies with large cohorts, such as those being conducted by BRIDGES30 and PERSPECTIVE I&I36, should be informative in determining whether additional susceptibility genes, with risk-defining coding variation, exist. For non-protein-coding variants, however, much larger whole-genome sequencing datasets, coupled with genomic risk prediction (genotype imputation), will be required.
Other promising approaches to improve breast cancer risk prediction include imaging and blood-based biomarkers. Improved use of mammography or MRI to predict risk is a particularly attractive area of research91,92,93; parenchymal textual features beyond simple mammographic breast density, such as the co-occurrence matrix and multiresolution spectral features, have been shown to be important94 and might be independently predictive of the development of breast cancer92,95,96. Screening programmes provide longitudinal data that can facilitate studies to identify such imaging biomarkers. Potential blood-based biomarkers include microRNAs, tumour-educated platelets and circulating tumour DNA97,98,99. However, these markers might be more suitable for short-term early detection than long-term risk prediction (since they are perhaps more likely to reflect the presence of cancer rather than cancer susceptibility), and large longitudinal collections of samples will be required to study them.
Comprehensive models incorporating genetic and epidemiological risk factors and mammographic breast density enable more accurate risk stratification in the general population, as well as in carriers of germline pathogenic variants, than is possible with models that consider only PRS45,47. Repeat collection of information on the non-genetic risk factors at a population level raises further complexities in the logistics of risk assessment. The feasibility, clinical utility, costs and cost-effectiveness of risk-based programmes using a comprehensive model versus a model with only PRS need to be evaluated.
To enhance the credibility of a given model, and thus confidence in the results, transparency (that is, a clear description of the model structure, equations, parameter values and assumptions) and validation in relevant settings are essential. The challenge lies in having a consensus on the criteria for sufficient evidence to declare a model as ‘valid’ for a particular application100.
Risk-stratified prevention
In high-income countries that have implemented strategies to prevent or mitigate cardiovascular disease (CVD), cancer has superseded CVD to become the most common cause of death101. In the context of CVD, clinical parameters indicative of risk (for example, blood pressure and serum lipid levels) can be successfully targeted and subsequently used to monitor preventive actions102. However, mirroring these concepts in the context of cancer has not been possible to date. Cancer development is a multifactorial process that occurs at various stages of life and sometimes decades in advance of diagnosis. Avoiding certain risk factors for breast cancer (for example, hormone replacement therapy, particularly those containing progesterone103), as well as adopting healthier lifestyle patterns (such as limiting alcohol consumption104,105 and maintaining a healthy weight106), can have long-term cancer-preventive effects. Nevertheless, many of the risk factors for breast cancer (including a family history of the disease and genetic predisposition, birthweight, age at menarche, age at first live birth and age at menopause) are not modifiable, and in many cases the biological mechanism underlying the associated increase in breast cancer risk remains unknown. Notwithstanding, several active strategies have been shown to modify breast cancer risk.
Chemoprevention with anti-oestrogens
The results of prospective randomized controlled trials (RCTs) evaluating primary prevention of breast cancer using selective oestrogen receptor modulators or aromatase inhibitors have consistently shown a reduced incidence in hormone receptor-positive subtypes of the disease107,108,109,110,111,112,113,114,115,116,117,118,119. However, in order to prevent one breast cancer in the next 20 years, 22 women needed to take tamoxifen daily for 5 years117. The considerable adverse effects of anti-oestrogens and the fact that none of these trials has shown any overall or breast cancer-specific survival benefits or a reduction in the incidence of aggressive, hormone receptor-negative forms of breast cancer make it difficult to judge whether treating healthy women with these drugs is a more effective strategy than reserving them for the adjuvant treatment of only those who actually develop breast cancer. Nevertheless, the US Preventive Services Task Force have judged that serious adverse effects, such as thrombosis and endometrial cancer, are uncommon and the more common toxicities, such as vasomotor symptoms, are reversible and were only marginally more frequent in women on active treatment than in those receiving placebo in the aforementioned RCTs120. Accordingly, several international guidelines recommend the use of anti-oestrogens as chemopreventives for women at increased risk of breast cancer16,121. Whether improved risk stratification would reduce the number of healthy women who need to take anti-oestrogens in order to achieve the same preventive effect will need to be established in future RCTs.
Surgical prevention
Prophylactic bilateral mastectomy is certainly the most effective way of preventing breast cancer and reducing breast cancer-specific deaths in the small minority of women (perhaps 3%)122 with a germline pathogenic BRCA1/2 variant123. Nipple-sparing mastectomies are a safe option for these women, with no known detriment to the risk reduction124. General complications include wound dehiscence, infection, implant loss or flap necrosis, asymmetry and capsular contracture125. For nipple-sparing mastectomies, the overall complication rate has been reported to be 22.3%, and the rate of nipple necrosis was 5.9%126. However, surgery can be associated with other complications and adverse effects, including psychological distress with body image change, and has implications relating to resources. Thus, clinical utility, feasibility and acceptability need to be evaluated in order to set the risk threshold for surgical intervention.
Other preventive strategies
In past few years, several new targets of potential preventive interventions for breast cancer have been discovered. In particular, progesterone has an essential role in the development of aggressive breast cancers. A meta-analysis of 58 studies revealed that women receiving a progesterone-containing menopausal hormone therapy not only have a higher incidence of breast cancer than women not receiving such therapy or those receiving oestrogen-only treatments, but also more cancers that had spread beyond the breast103. Furthermore, the data indicated that women receiving progesterone-containing therapy are more likely to die from breast cancer than women treated only with oestrogens127. Additional evidence for the role of progesterone in breast carcinogenesis comes from the observation that women with germline pathogenic BRCA1/2 variants have elevated levels of luteal phase progesterone compared with those observed in carriers of non-pathogenic BRCA1/2 variants128. This increase in progesterone levels leads to an increase in receptor activator of nuclear factor-κB ligand (RANKL) levels in the breast129,130,131,132,133, as well as reduced levels of the physiological RANKL antagonist osteoprotegerin129. These effects in turn lead to an expansion of ER− and progesterone receptor-negative mammary stem cells and eventual breast cancer formation134. In mouse models, Brca1/2-mediated breast cancer formation can be prevented by disrupting the progesterone signalling pathway using the competitive progesterone receptor antagonist mifepristone135. In addition, the findings of a case–control study involving women with germline BRCA1/2 mutations indicate that moderate use of dietary supplements containing folic acid and vitamin B12 can be protective against BRCA1/2-associated breast cancer136. Other potential risk-reducing chemotherapeutics include aspirin, metformin, statins or other agents137.
To date, clinical trial evidence supporting these chemoprevention strategies is lacking. Denosumab, a fully humanized antagonistic monoclonal antibody targeting RANKL, has been shown to reduce breast epithelial cell proliferation in three premenopausal volunteers134. In postmenopausal women with breast cancer, however, denosumab does not seem to alter the incidence of contralateral breast cancer138. A prevention study of this agent in carriers of pathogenic BRCA1 variants is underway139.
Future directions in prevention
Several challenges need to be addressed to advance the field of breast cancer prevention. First, drugs that can reduce the incidence of aggressive breast cancers, for example, of the triple-negative, HER2+ or luminal B subtypes, need to be identified.
Second, the required doses and frequency of administration of these potential preventive drugs need to be established. Unlike tamoxifen and aromatase inhibitors, the efficacy and safety of which have been tested in many thousands of women in the adjuvant treatment setting, no such data exist for the most promising novel preventive drugs (that is, progesterone antagonists and denosumab).
Third, efforts are needed to develop an effective approach to selecting women for whom breast cancer primary or secondary prevention measures will provide survival benefits. None of the current risk-prediction models intended to identify women at an increased risk of developing breast cancer in the absence of a familial predisposition (that is, mainly carriers of pathogenic BRCA1/2 variants) selectively identifies those women at risk of developing an aggressive cancer that, if not prevented, would likely lead to death.
Fourth, surrogate end points are required (Box 2). Demonstration of a reduction in breast cancer-related mortality is recommended before implementation of any early detection strategy140 whereas, for prevention strategies, robust evidence of a reduced cancer incidence seems to be sufficient to recommend clinical implementation141. The focus should not, however, be a reduction in the incidence of any breast cancer, but rather of breast cancers that hold a poor prognosis. Intermediate surrogate markers are urgently required to enable timely assessment of the efficacy of potential new breast cancer-preventive drugs, particularly in women at high risk of the disease so as not to substantially delay or preclude bilateral mastectomy that is a safe risk-reducing option. A reduction in mammographic breast density has proved to be an excellent predictor of response to tamoxifen in the preventive setting142. In addition, molecular biomarkers, assessed directly in breast tissue and reflective of a field defect58 or indirectly in a surrogate tissue or blood32, could potentially provide three essential advantages in prevention strategies for premenopausal women at high risk of breast cancer: 1) they can be measured frequently; 2) the dynamics of the molecular biomarkers in individual volunteers might reflect the cancer risk in real time, and thus individual adjustments to preventive measures could be made ad hoc; and 3) unlike many imaging-based markers, they do not require repeated exposure to x-rays (Fig. 3).
Various risk factors contribute to field defects in breast tissues that favour the development of breast cancer. The presence of such field defects can be assessed using biomarkers and/or imaging to guide personalized prevention strategies, the success of which can be monitored on an ongoing basis through intermediate surrogates (for example, reduction or resolution of the field defect) that reflect the ultimate goal of a decreased incidence of breast cancers with features indicative of a poor prognosis.
Finally, strategies should be developed to increase the acceptability and accessibility of interventions used for breast cancer prevention. Notably, the efficacy of weight loss programmes has been shown to be greater among individuals who are aware of being at high risk of developing breast cancer143. Importantly, weight loss144 and regular exercise145,146 not only decrease breast cancer risk but also the risks of other cancers and CVDs. Considering the general health benefits, lifestyle interventions could be recommended to women at all levels of breast cancer risk147. Thus, developing effective ways to make both lifestyle and chemoprevention options widely available (including within screening programmes), acceptable and better understood by health-care professionals and the public is essential148 (Box 2).
Risk-stratified early detection
The Cancer Control Joint Action European Guide on Quality Improvement in Comprehensive Cancer Control149 recommends that the benefits (cancer-specific deaths averted and quality-adjusted life years gained), harms (related to false screen findings and subsequent investigations, and overdiagnoses and the associated treatments) and cost-effectiveness of a screening programme should be estimated to guide decisions on implementation. RCTs should be used to generate the primary evidence on the effectiveness of a new screening programme in reducing cancer-specific mortality149. When modifying currently running programmes, however, questions remain regarding what constitutes supportive evidence (that is, the required level of evidence and study design)150 and how complete the evidence needs to be before recommendations for implementation can be made151.
Effectiveness
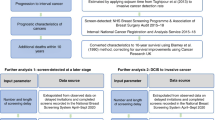
Two short-term RCTs evaluating the effectiveness of risk-stratified screening for breast cancer are currently ongoing: WISDOM in the USA152 and MyPeBS in Europe153. While the two trials share a similar design, with intermediate outcome measures (such as stage distribution) as end points, their protocols are adapted to the local health-care settings.
WISDOM152 is a multicentre, pragmatic, adaptive, preference-tolerant RCT comparing risk-based screening to annual screening in women aged 40–74 years. WISDOM is designed to determine whether risk-based screening is as safe as annual mammographic screening (number of stage ≥IIB cancers is no higher than that observed with annual screening), but with less morbidity (measured according to the number of breast biopsies performed) as well as greater acceptability, conductivity to preventive interventions and health-care value152. Women in the risk-based screening arm are receiving a personal risk assessment based on the BCSC risk calculator integrated with a PRS (which has been adapted during the course of the trial) and testing of a panel of nine susceptibility genes154. Those women are being stratified into four risk groups: highest risk, elevated risk, average risk and lowest risk. Each group is recommended a screening strategy that varies in starting age and the frequency and modality of screening — annual mammography with adjunctive MRI, annual mammography, biennial mammography and deferred screening until the age of 50 years (in the lowest risk group comprising women aged 40–49 years with 5-year absolute risk <1.3%), respectively155.
MyPeBS153 is a pragmatic, multicentre RCT that is being performed in five countries (Belgium, France, Israel, Italy and the UK) to determine if risk-based screening of women aged 40–70 years is non-inferior, in terms of the 4-year incidence of stage ≥II breast cancer, to the standard screening programme currently offered in each participating country (screening every 2–3 years beginning at 40–50 years of age and ending at 69–74 years of age). In MyPeBS, the frequency and modality of screening vary according to the level of risk predicted using PRS313 combined with the BCSC74 or the Tyrer–Cuzick78 risk calculator. The latter calculator is used only in women with more than one first-degree relative with a history of breast or ovarian cancer. In MyPeBS, women are also being classified into four risk groups153, although the risk thresholds differ from those used in WISDOM. However, the lead investigators of both trials are ensuring that data are collected in a similar way and have committed to pooling the data to improve the ability to learn from each study.
RCTs of screening interventions provide the strongest evidence of efficacy, although they have certain limitations. In particular, lifetime health effects cannot be observed in RCTs with limited follow-up durations. Thus, the observed benefit–harm trade-offs might not accurately reflect those expected with long-term population screening156. Moreover, the outcomes of screening depend on the screening strategy (including the choice of risk-assessment tool, risk thresholds, screening modalities, screen intervals and starting and stopping ages) and variables relating to the setting (such as the available infrastructure, levels of adherence and population preferences)149. Variations in any of these elements can alter the benefit–harm trade-offs. Finding the optimum strategy for a given population requires comparisons of several alternative screening strategies; however, RCTs — particularly of screening strategies that require very large cohorts and long follow-up durations — are inherently limited in their ability to compare more than a few approaches (typically two or three).
Simulations using natural history models and decision analysis models constitute useful tools to study the long-term benefits and harms as well as the cost-effectiveness of various screening strategies157,158,159. Such modelling studies can precede or follow RCTs of screening interventions. Lifetime health effects can be modelled using empirical data — for example, from RCTs of different approaches to screening, long-term observational studies and clinical registries160. Modelling studies that incorporate data on the population structure and preferences, the natural history and prevalence of disease, life expectancy, the available resources and costs can provide an indication of which screening strategies are likely to be optimal in a given setting160. Thereafter, the most promising strategies could be tested in RCTs. Thus, modelling studies can inform population-screening policies by extrapolating evidence beyond the time horizon of prospective trials and enabling the translation of evidence from one study population to another.
To date, evidence on the effectiveness of risk-stratified screening has come from model-based studies26,27,161. Modelling approaches have limitations, however. Models present a simplified representation of disease progression and intervention outcomes. Moreover, the accuracy of the results of modelling is dependent on the underlying assumptions and the degree of uncertainty in the input parameters162. Estimating overdiagnosis through simulations is particularly challenging163 and more so in the absence of data on the rates of disease progression for different risk groups.
Cost-effectiveness
Thus far, few studies have evaluated the cost-effectiveness and benefit–harm trade-offs of risk-stratified screening for breast cancer. Vilaprinyo et al.161 risk stratified women using several combinations of risk factors and showed that quinquennial or triennial screening for the low-risk or moderate-risk groups and annual screening for the high-risk group, from 50–74 years of age, would reduce costs, the number of false-positive findings and overdiagnosis, while averting the same number of deaths as biennial screening between the ages of 50 and 69 years. Trentham-Dietz et al.27 used a combination of mammographic breast density and four exemplar relative risk levels for risk stratification and showed that triennial screening of average-risk women with low breast density, starting at 50 years of age, and annual screening of higher-risk women of the same age with high breast density would be cost-effective at a threshold of $100,000 per quality-adjusted-life years gained and would maintain a similar or better balance of benefits and harms than biennial screening of average-risk women. Pashayan et al.26 used the distribution of polygenic risk in the population combined with other risk factors for stratification and showed that, compared with screening women from age 50–69 years triennially, not screening women at lower risk of developing breast cancer would improve the cost-effectiveness and benefit to harm ratio of the breast-screening programme.
Policy implications
When modifying an existing breast cancer screening programme, several considerations need to be taken into account. In particular, agreement should be reached on the framework of expected changes and acceptable trade-offs, whether in benefits, harms, net benefit, equity, cost or opportunity cost, in order to facilitate decisions on whether the evidence is supportive of the adapted programme. The ultimate aim is to implement risk-stratified screening that is justifiable from ethical, legal and societal viewpoints.
The policy priorities should be explicit: is the priority to maximize the return on investment or maximize the benefits of screening? That is, will the total number of screens and/or the budget allocated to the screening programme stay the same, but be utilized in a different way to maximize the benefits by focusing on higher-risk groups; or will the screening efforts and resources be increased to enable tailoring of screening to the risk level of each individual?
Future directions in early detection
We have identified several key areas for future research to improve early breast cancer detection (Box 2). The evidence from modelling studies indicates that risk-stratified screening approaches could potentially improve the efficiency and the benefit–harm balance of breast cancer screening programmes. Further data are required, however, on how the natural course of breast cancer, the sensitivity and specificity of mammography, as well as the probability of overdiagnosis vary according to the underlying risk of the disease. This information is needed to minimize the assumptions and uncertainties in the estimates used in models of risk-tailored screening strategies.
To have confidence in the validity of the outputs of modelling studies, the models have to be well calibrated, the structural assumptions and parameter estimates should be reported clearly and explicitly and the effects of alternative assumptions should be assessed in sensitivity analyses100,164,165,166. Having the code made open-source and easily accessible will enhance the transparency of the model158.
In countries with existing breast cancer screening programmes, randomized health service trial designs could be used to evaluate risk-based screening in routine health-care settings. Such trials enable the comparison of a new policy or intervention to the current standard approach within the context of an existing health service167. Indeed, although modelling, routine monitoring and observational studies can provide helpful evidence, they are not a replacement for randomized health service studies167.
Trading off benefits and harms of different screening strategies is a fundamentally value-laden activity. Discrete choice experiments (DCEs) provide a quantitative approach to eliciting women’s preferences168. In a DCE, participants are asked to choose between a series of alternative hypothetical scenarios described in terms of characteristics (or attributes) of the approach and associated levels of, for example, benefit and/or harm. In making these choices, participants are trading off between preferred and less preferred attributes presented in each alternative scenario. Incorporating the choice probability derived from DCEs for each screening approach into decision analytical modelling might facilitate the identification of optimal screening strategies.
In addition to cost-effectiveness analyses, budget-impact analyses will be needed to assess the affordability of a risk-stratified screening programme in a given setting169. Finally, although risk-stratified screening could potentially reduce overdiagnosis, a major need remains for tests that can differentiate, at diagnosis, tumours with progressive potential in order to reduce overtreatment. At present, no test is available for such differentiation at diagnosis. Biomarker-driven decisions regarding adjuvant therapy have, however, been incorporated into guidelines for the management of women with certain types of breast cancer170, which suggests that such an approach might be viable at diagnosis.
Implementation
Before risk-stratified prevention and early detection programmes for breast cancer can be implemented, health-care providers and policymakers would need to plan the resources, build the infrastructure for population-wide risk assessment, develop policies and regulations to protect the public from stigmatization and discrimination, and provide support for informed decision-making of individual women regarding whether or not to participate in the screening programme. Ultimately, these actions are needed to ensure the feasibility and affordability of providing a high-quality risk-stratified screening programme that is accessible to all and is aligned with public values and preferences. There will not be a single predefined way of organizing and delivering such programmes. The optimal approach will be context-specific to account for the idiosyncrasies of the health-care system, as well as the social, economic, cultural and political context (Fig. 4). Here, we are not dealing with a mathematical or technical problem; the implementation of risk-adapted breast cancer prevention and screening strategies does not constitute a simple change that has a simple solution, but rather necessitates complex adaptive changes that require all stakeholders, scientists, health-care professionals, the lay public and policymakers to work together.
The schematic illustrates the various multilevel interactions between the different components needed for the implementation of risk-stratified programmes for the early detection and prevention of cancer. The ultimate goal is an improvement in population health outcomes. To achieve this goal, the process has to be iterative within a learning health-care system.
Health-care organization readiness
Organizational readiness for systems change is widely recognized as being necessary for the successful implementation of complex changes in health-care settings171. This state reflects the extent to which those involved in implementing the new approach are primed, motivated and capable of achieving the required changes172. Organizational readiness is a dynamic process with pull and push factors between what is possible owing to constant emergence of new technological opportunities and what resources are available173.
To address the challenge of a constantly changing environment, health-care organizations should embrace an evolutionary approach, rather than espouse a sudden dramatic shift, by adopting a learning organizational culture and building on existing infrastructure65. In keeping with this concept, the adaptive design of WISDOM enables learning and adaptation of the risk-assessment model and the screening recommendations accordingly over the course of the trial, instead of waiting for certain new discoveries to emerge before starting the trial, or excluding participants of non-European ancestry (for whom limited relevant data are currently available)152. The coverage with evidence development (CED) model174 is a way of developing a ‘learning-based health-care system’. CED provides a mechanism for promising but unproven health technologies to enter practice sooner, through time-limited reimbursement that is conditional on a specific requirement for generation of further evidence on the performance of the new technology.
Readiness for change requires the commitment and engagement of all stakeholders, resources (including knowledge, skills, time, money and infrastructure) and governance171. To ensure the commitment of health-care organizations, the need for a change should be recognized and embedded in a shared vision, with leadership and coalition of all stakeholders171,175. To achieve a shared vision, the stakeholders have to agree on a framework of values that are aligned with those of the health-care organization. For example, health-care organizations value time-efficiency; therefore, successful implementation would require time-respecting strategies and tools, such as having one test to predict multiple cancers (which is a goal that FORECEE32 aims to achieve). Overall, vision, skills, incentives, resources and action plans are needed to achieve the systems change that will be required for implementation of risk-stratified prevention and early detection programmes for breast cancer176.
Stakeholder engagement
Given the diverse opinions on breast cancer screening among key stakeholders at present and the specific challenges of risk-stratified screening, engagement of all stakeholders is crucial to implementation of new programmes. A stakeholder is a person, group or organization involved in or affected by a decision177. Key stakeholders in breast cancer prevention and screening include the users and the providers of the service, health-care professionals, policymakers, payers, advocacy groups, researchers and others. Stakeholder engagement would enable the identification of potential misunderstandings among the various stakeholders regarding opposition to, and perspectives on, the implementation of a risk-stratified programme178. Using a multistakeholder approach to reach agreement on what would constitute sufficient evidence to change practice and on guidelines would increase the chances of implementing the research findings within the health-care system152. Such an approach would also help to articulate the values and preferences of the wider community and to build mutual trust, thereby facilitating the implementation of a programme that is accessible and acceptable. Stakeholder analysis179 would be useful to not only identify the key stakeholders, but also their interests and influences, and the level of involvement of each (whether it be provision of information, consultation, deliberation, participatory decision-making or delegated decisions)177.
Risk communication and its impact
Many women overestimate their risk of developing breast cancer180 and thus perceive screening as ‘almost always a good idea’181. This attitude is attributable to suboptimal levels of risk literacy among both patients and doctors as well as the limited transparency in the reporting of risks in the media and patient brochures182. Importantly, therefore, women should be transparently informed — for example, using fact boxes183,184 — about their baseline risks and the benefit to harm ratio of risk-based screening as compared to the existing options of a universal screening approach or no screening185. The development of risk-stratified programmes will need to include consideration of how to update risk assessments as risk-prediction models improve and how to communicate these changes to individuals.
Communicating information on breast cancer risk alone is unlikely to result in changes in health-related behaviours, such as smoking or low levels of physical activity148,186,187. Indeed, a methodical review of nine systematic reviews, encompassing at total of 36 unique studies, revealed no evidence that providing risk information would have strong, consistent or sustained effects on behaviour186. Changes in health-related behaviour can, however, be facilitated by including elements of interventions to alter the behaviour in question143.
Importantly, the available evidence suggests that providing women with their breast cancer risk estimates is unlikely to produce elevated distress188. Nevertheless, knowledge of whether providing risk estimates will promote informed choices regarding screening attendance is lacking, although the evidence base is starting to increase148. More definitive conclusions regarding the behavioural and emotional effects of receiving risk estimates require studies specifically designed to assess these questions (for example, PROCAS2 (ref.37), MyPeBS153 and PERSPECTIVE I&I36).
Acceptability
Acceptability is a complex and poorly defined concept189. The level of uptake is one index of the acceptability of a risk assessment. Many studies have addressed the issue of acceptability of risk-stratified screening for breast cancer from the perspective of women38,190 and of health-care professionals and policymakers191. The available evidence suggests that risk-stratified screening is broadly acceptable to women if it involves the potential for more frequent screening for those deemed to be at high risk192,193.
By contrast, a number of concerns exist among professionals working in this area, not least regarding costs and the available evidence base38. Similarly, major reservations surrounding the appropriateness of reducing the frequency of screening for women deemed to be at low risk have been expressed by health-care professionals, policymakers and women themselves194. A few high-quality ongoing studies36,37 are examining these issues empirically, rather than discussing the issues as hypothetical possibilities195. Further research is needed to determine the feasibility of risk-stratified screening, particularly studies on implementation of screening in a research context, such as PERSPECTIVE I&I36 and PROCAS2 (ref.37).
Workforce training
Effective delivery of risk-stratified prevention and screening services requires health-care professionals to be competent in the use of a risk tool, in interpreting and applying the risk scores and in communicating risk scores effectively to each individual, including discussion of the accuracy of the risk prediction and its future implications196. Risk-stratified approaches entail (epi)genetic testing for risk assessment. Health-care professionals need not become geneticists to effectively use the (epi)genomic information obtained197; however, they need to be sufficiently versed in (epi)genomics — for example, in understanding the contribution of common and rare coding variants to risk prediction, gene-panel testing and DNA-sequencing modalities and the implications of identifying pathogenic variants with poorly defined cancer risks or genetic variants of uncertain significance (VUS)198. Health-care systems should develop clear guidance related to the reporting of VUS in order to aid health-care professionals in the management of these variants, including descriptions of how patients with VUS should be informed if and when variants are found to confer an additional risk.
To engage with a new prevention and/or early detection scheme, the health-care professionals involved need to have a clear understanding of the rationale for risk stratification and risk-tailored interventions196, and have adequate knowledge of screening risk literacy199 and risk-communication skills; they should also have access to structured referral pathways for those women who need more detailed counselling. Accordingly, aspects of genomics and risk-stratified interventions should be integrated across the continuum of training for health-care professionals, from undergraduate education to broad specialty training to continuous professional development programmes. Educational-needs assessments should inform the educational requirements of each medical specialty200.
Ethical, legal and social implications
Ethical, legal and social issues need to be considered at every step of implementation of risk-based interventions, from health-service planning, invitation of participants and consent and sample collection, to risk calculation, communication of results and storage of data201,202. Some of the issues associated with risk-stratified screening will be dependent on the methods by which a programme is implemented202.
The four principles of bio-ethics promulgated by Beauchamp and Childress203 — autonomy, beneficence, non-maleficence and justice — provide a useful framework to understand the potential implications of risk-based screening, although these principles are more commonly applied to the doctor–patient relationship in the clinical context. Respecting autonomy requires that an individual has adequate knowledge and understanding to decide whether they wish to opt for a given intervention. The capacity of the individual to independently make an informed decision will depend on the information content, the communication tools used and the adequacy of workforce training in conveying the relevant information. Optimizing the balance between providing benefit (beneficence) and the potential for harm (maleficence) with a risk-based screening programme requires rigorous evaluation. This balance also requires consideration and mitigation of potential unintended harms of such programmes. These unintended harms might include the negative consequences of risk assessment for individuals (such as anxiety and breaches of confidential genetic and other personal data) or at a society level (stigmatization of and discrimination against some individuals because of their risk level and non-participation of some individuals in the programme, for example, because they perceive that health care is being rationed for those for whom less screening is recommended202). Finally, justice relates to the fairness of a programme. Screening programmes have the potential to increase health inequalities, owing to differences in the level of uptake between socioeconomic groups, including those covered under universal health systems204,205,206. Risk-based screening programmes might exacerbate these differences201, given their additional complexity and inherent selectivity relative to universal screening. Efforts are needed to mitigate this possibility, for example, through ‘proportionate universalism’207, whereby social inequalities are considered and programme resources are targeted commensurately208. Communication relating to screening and risk assessment has to be accessible and congruent to the literacy and numeracy level of the recipients while also accurately presenting both the potential benefits and risks209. Meeting these requirements will not only avoid misinterpretation of the information provided and subsequent inequitable use of screening services, but also enable each individual to make an informed decision201. In addition, robust legislation is necessary to prevent discrimination and stigmatization, in particular, by insurers and employers. Current approaches vary by country, but can be broadly divided into four categories: moratoria, industry self-regulation, legal limitations to the use of genetic information, and legal bans210,211. As an example, in the UK, an open-ended code of practice between insurers and the government exists, prohibiting the use of predictive genetic tests except in defined circumstances212.
Future directions for implementation
The time is right to perform implementation research in a real-world setting of risk-stratified prevention and screening for breast cancer, with clearly defined criteria for success (for example, relating to the extent of adoption, appropriateness, acceptability, sustainability, cost implications and effectiveness of the programme). The research should be designed and conducted together with all stakeholder groups, taking into account the ethical, legal and social context as well as factors that affect implementation (such as the idiosyncrasies of the health-care system and organizational readiness). The process has to be iterative in a health-care system conducive to learning and adaptation213.
To reduce the time lag between obtaining evidence on the effectiveness of a programme and its implementation, studies with hybrid effectiveness–implementation design could be used214 (Box 2). WISDOM152 and MyPeBS153 are examples of studies with hybrid designs primarily focused on effectiveness while also exploring the ‘implementability’ of the intervention. Several strategies adopted in WISDOM, such as the adaptive design, multistakeholder approach215 and CED model174, will accelerate implementation of the findings. By contrast, PERSPECTIVE I&I36 has a hybrid design focused primarily on implementation outcomes (including the acceptability and feasibility of risk-based screening, uptake of genetic testing for risk assessment and screening behaviours); however, data on effectiveness (that is, screening outcomes of different risk groups) are also being collected, and simulation modelling is being performed to assess the efficiency, resource use, costs and cost-effectiveness of risk-based screening at a population level using real-world administrative data. A third type of hybrid design involves the simultaneous study of effectiveness and implementation strategies. This approach enables the demonstration of which implementation strategies work in a given context, as opposed to demonstrating the effects of a particular implementation strategy on the adoption or uptake of an intervention214.
The model of evidence-generating health care could be adopted to study the clinical utility of risk stratification in the prevention of breast cancer among carriers of pathogenic BRCA1/2 variants. This approach would require linking of genetic profiles and the outcomes of preventive interventions to cancer registries, training of treating physicians to develop a working knowledge of cancer risk and genetics, and the development of decision aids for patients.
Women with a family history of breast cancer constitute a ‘high-impact’ group in which to first pilot national level application of integrated breast cancer risk assessment. In this group, the intervention might not only substantially improve clinical management, but also provide valuable information on how risk-stratified programmes might perform in the general population. Thus, the results of this pilot approach could form the basis on which to build subsequent population-level risk-based interventions.
Conclusions
Substantial progress has been made in research focused on estimating an individual woman’s risk of developing breast cancer, applying risk stratification in breast cancer prevention studies, modelling the benefit–harm balance of risk-stratified early detection approaches, and assessing the acceptability and feasibility of implementing risk-based prevention and screening programmes. To translate this progress into improvements in population health outcomes, a systems approach to the evaluation of risk-based programmes is necessary, taking into account the health-care organization’s readiness for change, its openness to learning and adapting, the social context and the need for engagement of all stakeholders.
Change history
15 February 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41571-020-0412-0
References
Bray, F. et al. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 68, 394–424 (2018).
Sørlie, T. et al. Gene expression patterns of breast carcinomas distinguish tumor subclasses with clinical implications. Proc. Natl Acad. Sci. USA 98, 10869–10874 (2001).
Blows, F. M. et al. Subtyping of breast cancer by immunohistochemistry to investigate a relationship between subtype and short and long term survival: a collaborative analysis of data for 10,159 cases from 12 studies. PLoS Med. 7, e1000279 (2010).
Curtis, C. et al. The genomic and transcriptomic architecture of 2,000 breast tumours reveals novel subgroups. Nature 486, 346–352 (2012).
Yang, X. R. et al. Associations of breast cancer risk factors with tumor subtypes: a pooled analysis from the Breast Cancer Association Consortium studies. J. Natl Cancer Inst. 103, 250–263 (2011).
Broeks, A. et al. Low penetrance breast cancer susceptibility loci are associated with specific breast tumor subtypes: findings from the Breast Cancer Association Consortium. Hum. Mol. Genet. 20, 3289–3303 (2011).
Turkoz, F. P. et al. Association between common risk factors and molecular subtypes in breast cancer patients. Breast 22, 344–350 (2013).
Waks, A. G. & Winer, E. P. Breast cancer treatment: a review. JAMA 321, 288–300 (2019).
Cancer Research UK. Breast cancer incidence by age https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/breast-cancer/incidence-invasive (2019).
Netherlands Cancer Registry. Incidence of cancer in the Netherlands http://www.dutchcancerfigures.nl/ (2019).
Nelson, H. D. et al. Risk factors for breast cancer for women aged 40 to 49 years: a systematic review and meta-analysis. Ann. Intern. Med. 156, 635–648 (2012).
Brinton, L., Gaudet, M. & Gierach, G. in Cancer Epidemiology Prevention (eds Thun, M., Linet, M., Cerhan, J., Haiman, C. & Schottenfeld, D.) 861–888 (Oxford University Press, 2018).
Winters, S., Martin, C., Murphy, D. & Shokar, N. K. Breast cancer epidemiology, prevention and screening. Prog. Mol. Biol. Transl Sci. 151, 1–32 (2017).
Hartmann, L. C. et al. Benign breast disease and the risk of breast cancer. N. Engl. J. Med. 353, 229–237 (2005).
Moorthie, S. et al. Personalised Prevention in Breast Cancer: the Policy Landscape (University of Cambridge, 2017).
NICE. Familial Breast Cancer: Classification, Care and Managing Breast Cancer and Related Risks in People with A Family History of Breast Cancer (NICE, 2013).
Owens, D. K. et al. Risk assessment, genetic counseling, and genetic testing for BRCA-related cancer. JAMA 322, 652 (2019).
Alexander, F. E. et al. 14 years of follow-up from the Edinburgh randomised trial of breast-cancer screening. Lancet 353, 1903–1908 (1999).
Habbema, J. D., van Oortmarssen, G. J., van Putten, D. J., Lubbe, J. T. & van der Maas, P. J. Age-specific reduction in breast cancer mortality by screening: an analysis of the results of the Health Insurance Plan of Greater New York study. J. Natl Cancer Inst. 77, 317–320 (1986).
Nystrom, L. et al. Long-term effects of mammography screening: updated overview of the Swedish randomised trials. Lancet 359, 909–919 (2002).
Miller, A. B., To, T., Baines, C. J. & Wall, C. The Canadian National Breast Screening Study-1: breast cancer mortality after 11 to 16 years of follow-up. A randomized screening trial of mammography in women age 40 to 49 years. Ann. Intern. Med. 137, 305–312 (2002).
Moss, S. M. et al. Effect of mammographic screening from age 40 years on breast cancer mortality at 10 years’ follow-up: a randomised controlled trial. Lancet 368, 2053–2060 (2006).
Welch, H. G., Prorok, P. C., O’Malley, A. J. & Kramer, B. S. Breast-cancer tumor size, overdiagnosis, and mammography screening effectiveness. N. Engl. J. Med. 375, 1438–1447 (2016).
Drukker, C. A. et al. Mammographic screening detects low-risk tumor biology breast cancers. Breast Cancer Res. Treat. 144, 103–111 (2014).
Esserman, L., Shieh, Y. & Thompson, I. Rethinking screening for breast cancer and prostate cancer. JAMA 302, 1685–1692 (2009).
Pashayan, N., Morris, S., Gilbert, F. J. & Pharoah, P. D. P. Cost-effectiveness and benefit-to-harm ratio of risk-stratified screening for breast cancer a life-table model. JAMA Oncol. 4, 1–7 (2018).
Trentham-Dietz, A. et al. Tailoring breast cancer screening intervals by breast density and risk for women aged 50 years or older: collaborative modeling of screening outcomes. Ann. Intern. Med. 165, 700 (2016).
Burton, H. et al. Public health implications from COGS and potential for risk stratification and screening. Nat. Genet. 45, 349–351 (2013).
Horizon 2020. B-CAST. Breast cancer stratification: understanding the determinants of risk and prognosis of molecular subtypes https://cordis.europa.eu/project/rcn/193256/factsheet/en (2020).
Horizon 2020. BRIDGES. Breast cancer risk after diagnostic gene sequencing https://cordis.europa.eu/project/rcn/193315/factsheet/en (2019).
European Research Council. BRCA-ERC. Understanding cancer development in BRCA1/2 mutation carriers for improved Early detection and Risk Control https://cordis.europa.eu/project/rcn/210990/factsheet/en (2017).
Horizon 2020. FORECEE. Female cancer prediction using cervical omics to individualise screening and prevention https://cordis.europa.eu/project/rcn/193298/factsheet/en (2019).
Horizon 2020. MyPeBS. International randomized study comparing personalized, risk-stratified to standard breast cancer screening in women aged 40-70 https://cordis.europa.eu/project/rcn/212694/factsheet/en (2019).
WISDOM. The WISDOM study https://wisdom.secure.force.com/portal/ (2020).
Horizon 2020. EU-TOPIA. EU-TOPIA: towards improved screening for breast, cervical and colorectal cancer in all of europe https://cordis.europa.eu/project/rcn/193304/factsheet/en (2019).
GenomeQuébec. PERSPECTIVE I&I. Personalized risk assessment for prevention and early detection of breast cancer: integration and implementation http://www.genomequebec.com/211-en/project/personalized-risk-assessment-for-prevention-and-early-detection-of-breast-cancer-integration-and-implementation/ (2020).
Prevent Breast Cancer. PROCAS 2. Predicting the risk of cancer at screening 2nd stage https://preventbreastcancer.org.uk/breast-cancer-research/research-projects/early-detection-screening/procas/ (2016).
Rainey, L. et al. Are we ready for the challenge of implementing risk-based breast cancer screening and primary prevention? Breast 39, 24–32 (2018).
The Health Foundation. Evidence Scan: Complex Adaptive Systems (The Health Foundation, 2010).
Michailidou, K. et al. Association analysis identifies 65 new breast cancer risk loci. Nature 551, 92–94 (2017).
Milne, R. L. et al. Identification of ten variants associated with risk of estrogen-receptor-negative breast cancer. Nat. Genet. 49, 1767–1778 (2017).
Easton, D. F. et al. Gene-panel sequencing and the prediction of breast-cancer risk. N. Engl. J. Med. 372, 2243–2257 (2015).
Rudolph, A. et al. Joint associations of a polygenic risk score and environmental risk factors for breast cancer in the Breast Cancer Association Consortium. Int. J. Epidemiol. 47, 526–536 (2018).
Mavaddat, N. et al. Polygenic risk scores for prediction of breast cancer and breast cancer subtypes. Am. J. Hum. Genet. 104, 21–34 (2019).
Lee, A. et al. BOADICEA: a comprehensive breast cancer risk prediction model incorporating genetic and nongenetic risk factors. Genet. Med. 21, 1708–1718 (2019).
Läll, K. et al. Polygenic prediction of breast cancer: comparison of genetic predictors and implications for risk stratification. BMC Cancer 19, 557 (2019).
Choudhury, P. P. et al. Comparative validation of breast cancer risk prediction models and projections for future risk stratification. J. Natl Cancer Inst. 112, 278–285 (2020).
LaDuca, H. et al. A clinical guide to hereditary cancer panel testing: evaluation of gene-specific cancer associations and sensitivity of genetic testing criteria in a cohort of 165,000 high-risk patients. Genet. Med. 22, 407–415 (2020).
Schmidt, M. K. et al. Age- and tumor subtype-specific breast cancer risk estimates for CHEK2*1100delC carriers. J. Clin. Oncol. 34, 2750–2760 (2016).
Foulkes, W. D. et al. Estrogen receptor status in BRCA1- and BRCA2-related breast cancer. Clin. Cancer Res. 10, 2029–2034 (2004).
Fletcher, O. et al. Missense variants in ATM in 26,101 breast cancer cases and 29,842 controls. Cancer Epidemiol. Biomarkers Prev. 19, 2143–2151 (2010).
Gao, P., Ma, N., Li, M., Tian, Q.-B. & Liu, D.-W. Functional variants in NBS1 and cancer risk: evidence from a meta-analysis of 60 publications with 111 individual studies. Mutagenesis 28, 683–697 (2013).
Weitzel, J. N. et al. Pathogenic and likely pathogenic variants in PALB2, CHEK2, and other known breast cancer susceptibility genes among 1054 BRCA negative Hispanics with breast cancer. Cancer 125, 2829–2836 (2019).
Parsons, M. T. et al. Large scale multifactorial likelihood quantitative analysis of BRCA1 and BRCA2 variants: an ENIGMA resource to support clinical variant classification. Hum. Mutat. 40, 1557–1578 (2019).
Kleiblova, P. et al. Identification of deleterious germline CHEK2 mutations and their association with breast and ovarian cancer. Int. J. Cancer 145, ijc.32385 (2019).
Boonen, R. A. C. M. et al. Functional analysis of genetic variants in the high-risk breast cancer susceptibility gene PALB2. Nat. Commun. 10, 5296 (2019).
Lee, K. et al. Clinical validity assessment of genes frequently tested on hereditary breast and ovarian cancer susceptibility sequencing panels. Genet. Med. 21, 1497–1506 (2019).
Teschendorff, A. E. et al. DNA methylation outliers in normal breast tissue identify field defects that are enriched in cancer. Nat. Commun. 7, 10478 (2016).
Curtius, K., Wright, N. A. & Graham, T. A. An evolutionary perspective on field cancerization. Nat. Rev. Cancer 18, 19–32 (2018).
Yang, Y. et al. Genetically predicted levels of DNA methylation biomarkers and breast cancer risk: data from 228,951 women of European descent. J. Natl Cancer Inst. 112, 295–304 (2020).
Xu, Z., Sandler, D. P. & Taylor, J. A. Blood DNA methylation and breast cancer: a prospective case-cohort analysis in the Sister study. J. Natl Cancer Inst. 112, 87–94 (2020).
Teschendorff, A. E. et al. Age-dependent DNA methylation of genes that are suppressed in stem cells is a hallmark of cancer. Genome Res. 20, 440–446 (2010).
Knower, K. C., To, S. Q., Leung, Y.-K., Ho, S.-M. & Clyne, C. D. Endocrine disruption of the epigenome: a breast cancer link. Endocr. Relat. Cancer 21, T33–T55 (2014).
Levine, M. E. et al. Menopause accelerates biological aging. Proc. Natl Acad. Sci. USA 113, 9327–9332 (2016).
Widschwendter, M. et al. Epigenome-based cancer risk prediction: rationale, opportunities and challenges. Nat. Rev. Clin. Oncol. 15, 292–309 (2018).
Bodelon, C. et al. Blood DNA methylation and breast cancer risk: a meta-analysis of four prospective cohort studies. Breast Cancer Res. 21, 62 (2019).
Teschendorff, A. E. et al. An epigenetic signature in peripheral blood predicts active ovarian cancer. PLoS One 4, e8274 (2009).
Key, T. J. et al. Sex hormones and risk of breast cancer in premenopausal women: a collaborative reanalysis of individual participant data from seven prospective studies. Lancet Oncol. 14, 1009–1019 (2013).
Key, T. J. et al. Body mass index, serum sex hormones, and breast cancer risk in postmenopausal women. J. Natl Cancer Inst. 95, 1218–1226 (2003).
Fourkala, E.-O. et al. Association of serum sex steroid receptor bioactivity and sex steroid hormones with breast cancer risk in postmenopausal women. Endocr. Relat. Cancer 19, 137–147 (2012).
Bau, D.-T., Mau, Y.-C., Ding, S.-L., Wu, P.-E. & Shen, C.-Y. DNA double-strand break repair capacity and risk of breast cancer. Carcinogenesis 28, 1726–1730 (2007).
Machella, N. et al. Double-strand breaks repair in lymphoblastoid cell lines from sisters discordant for breast cancer from the New York site of the BCFR. Carcinogenesis 29, 1367–1372 (2008).
Gail, M. H. et al. Projecting individualized probabilities of developing breast cancer for white females who are being examined annually. J. Natl Cancer Inst. 81, 1879–1886 (1989).
Tice, J. A. et al. Using clinical factors and mammographic breast density to estimate breast cancer risk: development and validation of a new predictive model. Ann. Intern. Med. 148, 337–347 (2008).
Garcia-Closas, M., Gunsoy, N. B. & Chatterjee, N. Combined associations of genetic and environmental risk factors: implications for prevention of breast cancer. J. Natl Cancer Inst. 106, 1–6 (2014).
Maas, P. et al. Breast cancer risk from modifiable and nonmodifiable risk factors among white women in the United States. JAMA Oncol. 2, 1295–1302 (2016).
Chatterjee, N., Shi, J. & García-Closas, M. Developing and evaluating polygenic risk prediction models for stratified disease prevention. Nat. Rev. Genet. 17, 392–406 (2016).
Tyrer, J., Duffy, S. W. & Cuzick, J. A breast cancer prediction model incorporating familial and personal risk factors. Stat. Med. 23, 1111–1130 (2004).
Antoniou, A. C. et al. The BOADICEA model of genetic susceptibility to breast and ovarian cancers: updates and extensions. Br. J. Cancer 98, 1457–1466 (2008).
Zimmern, R. L. & Kroese, M. The evaluation of genetic tests. J. Public. Health . 29, 246–250 (2007).
University of Cambridge. BCAC — The Breast Cancer Association Consortium http://bcac.ccge.medschl.cam.ac.uk/ (2020).
University of Cambridge. Centre for Cancer Genetic Epidemiology. CIMBA — Consortium of Investigators of Modifiers of BRCA1/2 http://cimba.ccge.medschl.cam.ac.uk/ (2020).
Louro, J. et al. A systematic review and quality assessment of individualised breast cancer risk prediction models. Br. J. Cancer 121, 76–85 (2019).
Terry, M. B. et al. 10-year performance of four models of breast cancer risk: a validation study. Lancet Oncol. 20, 504–517 (2019).
Choudhury, P. P. et al. iCARE: An R package to build, validate and apply absolute risk models. PLoS One 5, e0228198 (2020).
Smart, A. A multi-dimensional model of clinical utility. Int. J. Qual. Health Care 18, 377–382 (2006).
Sanderson, S. et al. How can the evaluation of genetic tests be enhanced? Lessons learned from the ACCE framework and evaluating genetic tests in the United Kingdom. Genet. Med. 7, 495–500 (2005).
Grosse, S. D. & Khoury, M. J. What is the clinical utility of genetic testing? Genet. Med. 8, 448–450 (2006).
Garcia-Closas, M. et al. Confluence: uncovering breast cancer genetics https://dceg.cancer.gov/research/cancer-types/breast-cancer/confluence-study-project.pdf (2019)
Wainschtein, P. et al. Recovery of trait heritability from whole genome sequence data. bioRxiv https://doi.org/10.1101/588020 (2019).
Yala, A., Lehman, C., Schuster, T., Portnoi, T. & Barzilay, R. A deep learning mammography-based model for improved breast cancer risk prediction. Radiology 292, 60–66 (2019).
Arasu, V. A. et al. Population-based assessment of the association between magnetic resonance imaging background parenchymal enhancement and future primary breast cancer risk. J. Clin. Oncol. 37, 954–963 (2019).
Malkov, S. et al. Mammographic texture and risk of breast cancer by tumor type and estrogen receptor status. Breast Cancer Res. 18, 122 (2016).
Gastounioti, A., Conant, E. F. & Kontos, D. Beyond breast density: a review on the advancing role of parenchymal texture analysis in breast cancer risk assessment. Breast Cancer Res. 18, 91 (2016).
Wang, C. et al. A novel and fully automated mammographic texture analysis for risk prediction: results from two case-control studies. Breast Cancer Res. 19, 114 (2017).
Nguyen, T. L. et al. Predicting interval and screen-detected breast cancers from mammographic density defined by different brightness thresholds. Breast Cancer Res. 20, 152 (2018).
Cohen, J. D. et al. Detection and localization of surgically resectable cancers with a multi-analyte blood test. Science 359, 926–930 (2018).
Wan, J. C. M. et al. Liquid biopsies come of age: towards implementation of circulating tumour DNA. Nat. Rev. Cancer 17, 223–238 (2017).
Best, M. G. et al. RNA-Seq of tumor-educated platelets enables blood-based pan-cancer, multiclass, and molecular pathway cancer diagnostics. Cancer Cell 28, 666–676 (2015).
Eddy, D. M. et al. Model transparency and validation: a report of the ISPOR-SMDM modeling good research practices task force — 7. Value Health 15, 843–850 (2012).
Dagenais, G. R. et al. Variations in common diseases, hospital admissions, and deaths in middle-aged adults in 21 countries from five continents (PURE): a prospective cohort study. Lancet 395, 785–794 (2020).
Fulcher, J. et al. Efficacy and safety of LDL-lowering therapy among men and women: meta-analysis of individual data from 174 000 participants in 27 randomised trials. Lancet 385, 1397–1405 (2015).
Collaborative Group on Hormonal Factors in Breast Cancer. Type and timing of menopausal hormone therapy and breast cancer risk: individual participant meta-analysis of the worldwide epidemiological evidence. Lancet 394, 1159–1168 (2019).
Hamajima, N. et al. Alcohol, tobacco and breast cancer — collaborative reanalysis of individual data from 53 epidemiological studies, including 58,515 women with breast cancer and 95,067 women without the disease. Br. J. Cancer 87, 1234–1245 (2002).
Bagnardi, V. et al. Alcohol consumption and site-specific cancer risk: a comprehensive dose–response meta-analysis. Br. J. Cancer 112, 580–593 (2015).
Renehan, A. G., Tyson, M., Egger, M., Heller, R. F. & Zwahlen, M. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet 371, 569–578 (2008).
Cuzick, J. Progress in preventive therapy for cancer: a reminiscence and personal viewpoint. Br. J. Cancer 118, 1155–1161 (2018).
Fisher, B. et al. Tamoxifen for prevention of breast cancer: report of the National Surgical Adjuvant Breast and Bowel Project P-1 Study. J. Natl Cancer Inst. 90, 1371–1388 (1998).
Cuzick, J. Aromatase inhibitors for breast cancer prevention. J. Clin. Oncol. 23, 1636–1643 (2005).
Cuzick, J. et al. Anastrozole for prevention of breast cancer in high-risk postmenopausal women (IBIS-II): an international, double-blind, randomised placebo-controlled trial. Lancet 383, 1041–1048 (2014).
Goss, P. E. et al. Exemestane for breast-cancer prevention in postmenopausal women. N. Engl. J. Med. 364, 2381–2391 (2011).
Cuzick, J. et al. First results from the International Breast Cancer Intervention Study (IBIS-I): a randomised prevention trial. Lancet 360, 817–824 (2002).
Cuzick, J. et al. Overview of the main outcomes in breast-cancer prevention trials. Lancet 361, 296–300 (2003).
Powles, T. et al. Interim analysis of the incidence of breast cancer in the Royal Marsden Hospital tamoxifen randomised chemoprevention trial. Lancet 352, 98–101 (1998).
Veronesi, U. et al. Prevention of breast cancer with tamoxifen: preliminary findings from the Italian randomised trial among hysterectomised women. Lancet 352, 93–97 (1998).
Powles, T. J., Ashley, S., Tidy, A., Smith, I. E. & Dowsett, M. Twenty-year follow-up of the Royal Marsden randomized, double-blinded tamoxifen breast cancer prevention trial. J. Natl Cancer Inst. 99, 283–290 (2007).
Cuzick, J. et al. Tamoxifen for prevention of breast cancer: extended long-term follow-up of the IBIS-I breast cancer prevention trial. Lancet Oncol. 16, 67–75 (2015).
Vogel, V. G. et al. Effects of tamoxifen vs raloxifene on the risk of developing invasive breast cancer and other disease outcomes: the NSABP study of tamoxifen and raloxifene (STAR) P-2 trial. JAMA 295, 2727–2741 (2006).
Vogel, V. G. et al. Update of the National Surgical Adjuvant Breast and Bowel Project Study of Tamoxifen and Raloxifene (STAR) P-2 Trial: preventing breast cancer. Cancer Prev. Res. 3, 696–706 (2010).
Nelson, H. D., Smith, M. E. B., Griffin, J. C. & Fu, R. Use of medications to reduce risk for primary breast cancer: a systematic review for the U.S. Preventive Services Task Force. Ann. Intern. Med. 158, 604 (2013).
Owens, D. K. et al. Medication use to reduce risk of breast cancer: US Preventive Services Task Force recommendation statement. JAMA 322, 857–867 (2019).
Armstrong, N., Ryder, S., Forbes, C., Ross, J. & Quek, R. G. A systematic review of the international prevalence of BRCA mutation in breast cancer. Clin. Epidemiol. 11, 543–561 (2019).
Heemskerk-Gerritsen, B. A. M. et al. Survival after bilateral risk-reducing mastectomy in healthy BRCA1 and BRCA2 mutation carriers. Breast Cancer Res. Treat. 177, 723–733 (2019).
Jakub, J. W. et al. Oncologic safety of prophylactic nipple-sparing mastectomy in a population with BRCA mutations. JAMA Surg. 153, 123 (2018).
Mota, B. S. et al. Nipple- and areola-sparing mastectomy for the treatment of breast cancer. Cochrane Database Syst. Rev. 11, CD008932 (2016).
Headon, H. L., Kasem, A. & Mokbel, K. The oncological safety of nipple-sparing mastectomy: a systematic review of the literature with a pooled analysis of 12,358 procedures. Arch. Plast. Surg. 43, 328–338 (2016).
Beral, V., Peto, R., Pirie, K. & Reeves, G. Menopausal hormone therapy and 20-year breast cancer mortality. Lancet 394, 1139 (2019).
Widschwendter, M. et al. The sex hormone system in carriers of BRCA1/2 mutations: a case-control study. Lancet Oncol. 14, 1226–1232 (2013).
Widschwendter, M. et al. Osteoprotegerin (OPG), the endogenous inhibitor of receptor activator of NF-kappaB ligand (RANKL), is dysregulated in BRCA mutation carriers. EBioMedicine 2, 1331–1339 (2015).
Schramek, D. et al. Osteoclast differentiation factor RANKL controls development of progestin-driven mammary cancer. Nature 468, 98–102 (2010).
Joshi, P. A. et al. Progesterone induces adult mammary stem cell expansion. Nature 465, 803–807 (2010).
Gonzalez-Suarez, E. et al. RANK ligand mediates progestin-induced mammary epithelial proliferation and carcinogenesis. Nature 468, 103–107 (2010).
Tanos, T. et al. Progesterone/RANKL is a major regulatory axis in the human breast. Sci. Transl Med. 5, 182ra55 (2013).
Nolan, E. et al. RANK ligand as a potential target for breast cancer prevention in BRCA1-mutation carriers. Nat. Med. 22, 933–939 (2016).
Poole, A. J. et al. Prevention of Brca1-mediated mammary tumorigenesis in mice by a progesterone antagonist. Science 314, 1467–1470 (2006).
Kim, S. J. et al. Folic acid supplement use and breast cancer risk in BRCA1 and BRCA2 mutation carriers: a case-control study. Breast Cancer Res. Treat. 174, 741–748 (2019).
Evans, D. G., Howell, S. J. & Howell, A. Personalized prevention in high risk individuals: managing hormones and beyond. Breast 39, 139–147 (2018).
Gnant, M. et al. Adjuvant denosumab in postmenopausal patients with hormone receptor-positive breast cancer (ABCSG-18): disease-free survival results from a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 20, 339–351 (2019).
European Medicines Agency. European Union Clinical Trials Register https://www.clinicaltrialsregister.eu/ctr-search/trial/2017-002505-35/AT (2018).
Sasieni, P. D., Duffy, S. W. & Cuzick, J. Ovarian cancer screening: UKCTOCS trial. Lancet 387, 2602 (2016).
Curtis, H. J., Walker, A. J. & Goldacre, B. Impact of NICE guidance on tamoxifen prescribing in England 2011–2017: an interrupted time series analysis. Br. J. Cancer 118, 1268–1275 (2018).
Cuzick, J. et al. Tamoxifen-induced reduction in mammographic density and breast cancer risk reduction: a nested case-control study. J. Natl Cancer Inst. 103, 744–752 (2011).
Harvie, M. et al. Breast cancer risk status influences uptake, retention and efficacy of a weight loss programme amongst breast cancer screening attendees: two randomised controlled feasibility trials. BMC Cancer 19, 1089 (2019).
Teras, L. R. et al. Sustained weight loss and risk of breast cancer in women ≥50 years: a pooled analysis of prospective data. J. Natl Cancer Inst. https://doi.org/10.1093/jnci/djz226 (2019).
Kyu, H. H. et al. Physical activity and risk of breast cancer, colon cancer, diabetes, ischemic heart disease, and ischemic stroke events: systematic review and dose-response meta-analysis for the Global Burden of Disease Study 2013. BMJ 354, i3857 (2016).
Guo, W., Fensom, G. K., Reeves, G. K. & Key, T. J. Physical activity and breast cancer risk: results from the UK Biobank prospective cohort. Br. J. Cancer 122, 726–732 (2020)
Rainey, L. et al. The impact of alcohol consumption and physical activity on breast cancer: the role of breast cancer risk. Int. J. Cancer https://doi.org/10.1002/ijc.32846 (2020).
French, D. P., Howell, A. & Evans, D. G. Psychosocial issues of a population approach to high genetic risk identification: behavioural, emotional and informed choice issues. Breast 37, 148–153 (2018).
Albhert, T., Kiasuwa, R. & van den Bulcke, M. European guide on quality improvement in comprehensive cancer control https://cancercontrol.eu/archived/uploads/images/Guide/pdf/CanCon_Guide_FINAL_Web.pdf (2017)
Lesko, L. J., Zineh, I. & Huang, S.-M. What is clinical utility and why should we care? Clin. Pharmacol. Ther. 88, 729–733 (2010).
Rychetnik, L., Frommer, M., Hawe, P. & Shiell, A. Criteria for evaluating evidence on public health interventions. J. Epidemiol. Community Health 56, 119–127 (2002).
Esserman, L. J. et al. The WISDOM study: breaking the deadlock in the breast cancer screening debate. NPJ Breast Cancer 3, 34 (2017).
US National Library of Medicine. Clinicaltrials.gov https://clinicaltrials.gov/ct2/show/NCT03672331 (2020)
Vachon, C. M. et al. The contributions of breast density and common genetic variation to breast cancer risk. J. Natl Cancer Inst. 107, dju397 (2015).
Shieh, Y. et al. Breast cancer screening in the precision medicine era: risk-based screening in a population-based trial. J. Natl Cancer Inst. 109, djw290 (2017).
Etzioni, R. D. & Thompson, I. M. What do the screening trials really tell us and where do we go from here? Urol. Clin. North. Am. 41, 223–228 (2014).
Getaneh, A. M., Heijnsdijk, E. A. & de Koning, H. J. The role of modelling in the policy decision making process for cancer screening: example of prostate specific antigen screening. Public. Health Res. Pract. 29, 2921912 (2019).
Karlsson, A. et al. A natural history model for planning prostate cancer testing: calibration and validation using Swedish registry data. PLoS One 14, e0211918 (2019).
Lew, J.-B. et al. Benefits, harms and cost-effectiveness of cancer screening in Australia: an overview of modelling estimates. Public Health Res. Pract. 29, 29121913 (2019).
Siebert, U. When should decision-analytic modeling be used in the economic evaluation of health care? Eur. J. Health Econ. 4, 143–150 (2003).
Vilaprinyo, E. et al. Cost-effectiveness and harm-benefit analyses of risk-based screening strategies for breast cancer. PLoS One 9, e86858 (2014).
Etzioni, R. et al. Limitations of basing screening policies on screening trials. Med. Care 51, 295–300 (2013).
Etzioni, R. & Gulati, R. Recognizing the limitations of cancer overdiagnosis studies: a first step towards overcoming them. J. Natl Cancer Inst. 108, djv345 (2015).
Weinstein, M. C. et al. Principles of good practice for decision analytic modeling in health-care evaluation: report of the ISPOR task force on good research practices — modeling studies. Value Health 6, 9–17 (2003).
Caro, J. J., Briggs, A. H., Siebert, U. & Kuntz, K. M. Modeling good research practices — overview. Med. Decis. Making 32, 667–677 (2012).
Briggs, A. H. et al. Model parameter estimation and uncertainty analysis. Med. Decis. Making 32, 722–732 (2012).
Hakama, M., Malila, N. & Dillner, J. Randomised health services studies. Int. J. Cancer 131, 2898–2902 (2012).
Ryan, M., Bate, A., Eastmond, C. J. & Ludbrook, A. Use of discrete choice experiments to elicit preferences. Qual. Saf. Health Care 10, i55–i60 (2001).
Mauskopf, J. A. et al. Principles of good practice for budget impact analysis: report of the ISPOR Task force on good research practices — budget impact analysis. Value Health 10, 336–347 (2007).
Krop, I. et al. Use of biomarkers to guide decisions on adjuvant systemic therapy for women with early-stage invasive breast cancer: American Society of Clinical Oncology clinical practice guideline focused update. J. Clin. Oncol. 35, 2838–2847 (2017).
Weiner, B. J. A theory of organizational readiness for change. Implement. Sci. 4, 67 (2009).
Holt, D. T., Helfrich, C. D., Hall, C. G. & Weiner, B. J. Are you ready? How health professionals can comprehensively conceptualize readiness for change. J. Gen. Intern. Med. 25, 50–55 (2010).
Andermann, A. Revisting Wilson and Jungner in the genomic age: a review of screening criteria over the past 40 years. Bull. World Health Organ. 86, 317–319 (2008).
Rosenberg-Wohl, S. et al. Private payer participation in coverage with evidence development: a case study. Health Affairs Blog https://www.healthaffairs.org/do/10.1377/hblog20170314.059181/full/ (2017).
Kotter, J. Leading Change (Harvard Business Press, 1996).
Knoster, T., Villa, R. & Thousand, J. in Restructuring for Caring and Effective Education: Piecing the Puzzle together (eds Villa, R. & Thousands, J.) 93–128 (Paul H. Brookes, 2000).
Lemke, A. A. & Harris-Wai, J. N. Stakeholder engagement in policy development: challenges and opportunities for human genomics. Genet. Med. 17, 949–957 (2015).
Puzhko, S. et al. Health professionals’ perspectives on breast cancer risk stratification: understanding evaluation of risk versus screening for disease. Public. Health Rev. 40, 2 (2019).
Schmeer, K. Stakeholder analysis guidelines https://www.who.int/workforcealliance/knowledge/toolkit/33.pdf (2019).
Wegwarth, O. et al. What do European women know about their female cancer risks and cancer screening? A cross-sectional online intervention survey in five European countries. BMJ Open 8, e023789 (2018).
Waller, J., Osborne, K. & Wardle, J. Enthusiasm for cancer screening in Great Britain: a general population survey. Br. J. Cancer 112, 562–566 (2015).
Wegwarth, O. & Gigerenzer, G. Improving evidence-based practices through health literacy — reply. JAMA Intern. Med. 174, 1413 (2014).
McDowell, M., Rebitschek, F. G., Gigerenzer, G. & Wegwarth, O. A simple tool for communicating the benefits and harms of health interventions: a guide for creating a fact box. MDM Policy Pract. 1, 1–10 (2016).
McDowell, M., Gigerenzer, G., Wegwarth, O. & Rebitschek, F. G. Effect of tabular and icon fact box formats on comprehension of benefits and harms of prostate cancer screening: a randomized trial. Med. Decis. Making 39, 41–56 (2018).
Steckelberg, A., Berger, B., Kopke, S., Heesen, C. & Muhlhauser, I. Criteria for evidence-based patient information. Z. Arztl. Fortbild. Qualitatssich. 99, 343–351 (2005).
French, D. P., Cameron, E., Benton, J. S., Deaton, C. & Harvie, M. Can Communicating personalised disease risk promote healthy behaviour change? A systematic review of systematic reviews. Ann. Behav. Med. 51, 718–729 (2017).
Hollands, G. J. et al. The impact of communicating genetic risks of disease on risk-reducing health behaviour: systematic review with meta-analysis. BMJ 352, i1102 (2016).
French, D. P. et al. Psychological impact of providing women with personalised 10-year breast cancer risk estimates. Br. J. Cancer 118, 1648–1657 (2018).
Sekhon, M., Cartwright, M. & Francis, J. J. Acceptability of healthcare interventions: an overview of reviews and development of a theoretical framework. BMC Health Serv. Res. 17, 88 (2017).
Evans, D. G. et al. Improvement in risk prediction, early detection and prevention of breast cancer in the NHS breast screening programme and family history clinics: a dual cohort study. Program. Grants Appl. Res. https://doi.org/10.3310/pgfar04110 (2016).
Rainey, L. et al. Women’s perceptions of personalized risk-based breast cancer screening and prevention: an international focus group study. Psychooncology. 28, 1056–1062 (2019).
Meisel, S. F. et al. Adjusting the frequency of mammography screening on the basis of genetic risk: attitudes among women in the UK. Breast 24, 237–241 (2015).
Ghanouni, A. et al. Attitudes towards risk-stratified breast cancer screening among women in England: a cross-sectional survey. J. Med. Screen. https://doi.org/10.1177/0969141319883662 (2019).
Keogh, L. A. et al. Consumer and clinician perspectives on personalising breast cancer prevention information. Breast 43, 39–47 (2019).
Lévesque, E., Hagan, J., Knoppers, B. M. & Simard, J. Organizational challenges to equity in the delivery of services within a new personalized risk-based approach to breast cancer screening. N. Genet. Soc. 38, 38–59 (2019).
Chowdhury, S. et al. Do health professionals need additional competencies for stratified cancer prevention based on genetic risk profiling? J. Pers. Med. 5, 191–212 (2015).
Feero, W. G. & Green, E. D. Genomics education for health care professionals in the 21st century. JAMA 306, 989–990 (2011).
Kurian, A. W. et al. Gaps in incorporating germline genetic testing into treatment decision-making for early-stage breast cancer. J. Clin. Oncol. 35, 2232–2239 (2017).
Wegwarth, O., Schwartz, L. M., Woloshin, S., Gaissmaier, W. & Gigerenzer, G. Do physicians understand cancer screening statistics? A national survey of primary care physicians in the United States. Ann. Intern. Med. 156, 340–349 (2012).
Slade, I. & Burton, H. Preparing clinicians for genomic medicine. Postgrad. Med. J. 92, 369–371 (2016).
Lévesque, E. et al. Ethical, legal, and regulatory issues for the implementation of omics-based risk prediction of women’s cancer: points to consider. Public Health Genomics 21, 37–44 (2018).
Hall, A. E. et al. Implementing risk-stratified screening for common cancers: a review of potential ethical, legal and social issues. J. Public Health 36, 285–291 (2014).
Beauchamp, T. & Childress, J. Principles of Biomedical Ethics. (Oxford University Press, 2013)
Maheswaran, R., Pearson, T., Jordan, H. & Black, D. Socioeconomic deprivation, travel distance, location of service, and uptake of breast cancer screening in north Derbyshire, UK. J. Epidemiol. Community Health 60, 208–212 (2006).
Morris, M. et al. Ethnicity, deprivation and screening: survival from breast cancer among screening-eligible women in the West Midlands diagnosed from 1989 to 2011. Br. J. Cancer 113, 548–555 (2015).
Moutel, G. et al. Women’s participation in breast cancer screening in France — an ethical approach. BMC Med. Ethics 15, 64 (2014).
Marmot, M. Fair society, healthy lives: the marmot review; strategic review of health inequalities in England post-2010 http://www.instituteofhealthequity.org/resources-reports/fair-society-healthy-lives-the-marmot-review/fair-society-healthy-lives-full-report-pdf.pdf (2010).
Darquy, S., Moutel, G., Jullian, O., Barré, S. & Duchange, N. Towards equity in organised cancer screening: the case of cervical cancer screening in France. BMC Womens Health 18, 192 (2018).
Hersch, J. et al. Use of a decision aid including information on overdetection to support informed choice about breast cancer screening: a randomised controlled trial. Lancet 385, 1642–1652 (2015).
Prince, A. E. R. Comparative perspectives: regulating insurer use of genetic information. Eur. J. Hum. Genet. 27, 340–348 (2019).
Joly, Y., Feze, I. N., Song, L. & Knoppers, B. M. Comparative approaches to genetic discrimination: chasing shadows? Trends Genet. 33, 299–302 (2017).
HM Government and Association of British Insurers. Code on Genetic Testing and Insurance. (HM Government and Association of British Insurers, 2018).
Lu, C. Y. et al. A proposed approach to accelerate evidence generation for genomic-based technologies in the context of a learning health system. Genet. Med. 20, 390–396 (2018).
Landes, S. J., McBain, S. A. & Curran, G. M. An introduction to effectiveness-implementation hybrid designs. Psychiatry Res. 280, 112513 (2019).
D’Aunno, T., Hearld, L. & Alexander, J. A. Sustaining multistakeholder alliances. Health Care Manage Rev. 44, 183–194 (2019).
Acknowledgements
The ENVISION Conference was funded by a European Research Council (ERC) Advanced Grant (BRCA-ERC) and the following European Union Horizon 2020 (H2020) Programme (H2020/2014-2020) consortia: FORECEE, BRIDGES, B-CAST, EU-TOPIA and MyPeBS. N.P., G.S., O.W., D.R. and M.W. have received research funding from H2020 FORECEE (grant agreement number 634570) and The Eve Appeal charity. M.W. has also received support from the ERC Advanced Grant BRCA-ERC (grant agreement number 742432). D.F.E., P.H., J.S., R.S. and P.D. have received support from H2020 BRIDGES (grant agreement number 634935). A.C.A., D.F.E., P.H., M.G.-C., P.P., S.M. and M.K.S. have received support from H2020 B-CAST (grant agreement number 633784. U.I. and H.d.K. have received support from H2020 EU-TOPIA (grant agreement number 634753). D.F., D.G.E., S.D.M., C. Baron, C. Balleyguier, P.G.R., D. Ritchie and S.D. have received support from H2020 MyPeBS (grant agreement number 755394). The ENVISION Conference 2019 received additional funding from the Tirolean Government and was supported by UMIT — University for Health Sciences, Medical Informatics and Technology.
Reviewer information
Nature Reviews Clinical Oncology thanks Nehmat Houssami, Kala Visvanatha and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
M.W., P.D., S.D., M.S., H.d.K. and N.P. organized the ENVISION Conference 2019. N.P. and M.W. led the drafting of this manuscript. All authors contributed to the content through presentations at the Conference and draft sections, and edited and reviewed the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
P.G.R. is the Principal Investigator and research project data owner of an independent study, funded by the Italian Ministry of Health, and conducted negotiations with Becton Dickinson, Hologic and Roche to obtain reagents at a reduced price or for free; he is member of the MyPeBS steering committee. The other authors declare no competing interests.
Additional information
Disclaimer
The work of D.F. and D.G.E. is supported by the National Institute for Health Research (NIHR); the views expressed are those of the authors and not necessarily those of the UK National Health Service (NHS), the NIHR or the UK Department of Health. Z.H. is a member of the International Agency for Research on Cancer (IARC) and the following disclaimer applies: “Where authors are identified as personnel of the International Agency for Research on Cancer/World Health Organization, the authors alone are responsible for the views expressed in this article and they do not necessarily represent the decisions, policy or views of the International Agency for Research on Cancer/World Health Organization.” The work of M.G.-C. work is supported by Intramural Funds of the US National Cancer Institute. The work of Z.H. is supported by the Institut National du Cancer and EU Translational Cancer Research (TRANSCAN) Framework and the Fondation ARC pour la Recherche sur le Cancer.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Related links
BOADICEA: https://canrisk.org
ClinGen: https://clinicalgenome.org/
Tyrer–Cuzick IBIS Breast Cancer Risk Evaluation Tool: http://www.ems-trials.org/riskevaluator/
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pashayan, N., Antoniou, A.C., Ivanus, U. et al. Personalized early detection and prevention of breast cancer: ENVISION consensus statement. Nat Rev Clin Oncol 17, 687–705 (2020). https://doi.org/10.1038/s41571-020-0388-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41571-020-0388-9
This article is cited by
-
As a novel prognostic model for breast cancer, the identification and validation of telomere-related long noncoding RNA signatures
World Journal of Surgical Oncology (2024)
-
“For and against” factors influencing participation in personalized breast cancer screening programs: a qualitative systematic review until March 2022
Archives of Public Health (2024)
-
Genetic correlation and Mendelian randomization analyses support causal relationships between dietary habits and age at menarche
Scientific Reports (2024)
-
CYB561 promotes HER2+ breast cancer proliferation by inhibiting H2AFY degradation
Cell Death Discovery (2024)
-
A structured process for the validation of a decision-analytic model: application to a cost-effectiveness model for risk-stratified national breast screening
Applied Health Economics and Health Policy (2024)