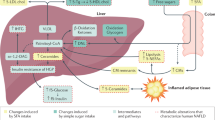
Abstract
The effect of dietary fats on cardiometabolic diseases, including cardiovascular diseases and type 2 diabetes mellitus, has generated tremendous interest. Many earlier investigations focused on total fat and conventional fat classes (such as saturated and unsaturated fats) and their influence on a limited number of risk factors. However, dietary fats comprise heterogeneous molecules with diverse structures, and growing research in the past two decades supports correspondingly complex health effects of individual dietary fats. Moreover, health effects of dietary fats might be modified by additional factors, such as accompanying nutrients and food-processing methods, emphasizing the importance of the food sources. Accordingly, the rapidly increasing scientific findings on dietary fats and cardiometabolic diseases have generated debate among scientists, caused confusion for the general public and present challenges for translation into dietary advice and policies. This Review summarizes the evidence on the effects of different dietary fats and their food sources on cell function and on risk factors and clinical events of cardiometabolic diseases. The aim is not to provide an exhaustive review but rather to focus on the most important evidence from randomized controlled trials and prospective cohort studies and to highlight current areas of controversy and the most relevant future research directions for understanding how to improve the prevention and management of cardiometabolic diseases through optimization of dietary fat intake.
Key points
-
In addition to their role as metabolic fuel, fatty acids modulate diverse cell processes including transcription regulation, cellular and organelle membrane structure and function, ion channel activity and electrophysiology.
-
Dietary fats comprise a wide range of fatty acids, and growing evidence demonstrates heterogeneity in the health effects of specific fatty acids as well as their food sources.
-
Robust evidence from multiple research studies demonstrates no health benefits of lowering total dietary fat in foods or overall diets.
-
For both saturated fatty acids and monounsaturated fatty acids, which have highly diverse dietary sources, considering the food sources and types separately might be most meaningful for understanding their health effects.
-
The overall evidence strongly supports cardiometabolic benefits of total polyunsaturated fatty acid (PUFA), n-6 PUFA and seafood-derived n-3 PUFA consumption.
-
People consume complex foods, not individual fatty acids; therefore, guidance and policies to improve general population diets should place greater emphasis on specific food sources of dietary fats.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Mozaffarian, D., Rosenberg, I. & Uauy, R. History of modern nutrition science-implications for current research, dietary guidelines, and food policy. BMJ 361, k2392 (2018).
Mozaffarian, D. & Forouhi, N. G. Dietary guidelines and health-is nutrition science up to the task? BMJ 360, k822 (2018).
Micha, R. & Mozaffarian, D. Saturated fat and cardiometabolic risk factors, coronary heart disease, stroke, and diabetes: a fresh look at the evidence. Lipids 45, 893–905 (2010).
Mozaffarian, D. Dietary and policy priorities for cardiovascular disease, diabetes, and obesity: a comprehensive review. Circulation 133, 187–225 (2016).
Mozaffarian, D. & Wu, J. H. Omega-3 fatty acids and cardiovascular disease: effects on risk factors, molecular pathways, and clinical events. J. Am. Coll. Cardiol. 58, 2047–2067 (2011).
Downs, S. M., Loeh, S. & Wu, J. H. in Preventive Nutrition: The Comprehensive Guide for Health Professionals 5th edn (eds Bendich, A. & Deckelbaum, R.) (Springer, 2016).
Harris, W. S. et al. Omega-6 fatty acids and risk for cardiovascular disease: a science advisory from the American Heart Association Nutrition Subcommittee of the Council on Nutrition, Physical Activity, and Metabolism; Council on Cardiovascular Nursing; and Council on Epidemiology and Prevention. Circulation 119, 902–907 (2009).
Joris, P. J. & Mensink, R. P. Role of cis-monounsaturated fatty acids in the prevention of coronary heart disease. Curr. Atheroscler. Rep. 18, 38 (2016).
Stark, A. H., Reifen, R. & Crawford, M. A. Past and present insights on alpha-linolenic acid and the omega-3 fatty acid family. Crit. Rev. Food Sci. Nutr. 56, 2261–2267 (2016).
Kihara, A. Very long-chain fatty acids: elongation, physiology and related disorders. J. Biochem. 152, 387–395 (2012).
Lemaire-Ewing, S., Lagrost, L. & Neel, D. Lipid rafts: a signalling platform linking lipoprotein metabolism to atherogenesis. Atherosclerosis 221, 303–310 (2012).
Lingwood, D. & Simons, K. Lipid rafts as a membrane-organizing principle. Science 327, 46–50 (2010).
Niu, S. L., Mitchell, D. C. & Litman, B. J. Trans fatty acid derived phospholipids show increased membrane cholesterol and reduced receptor activation as compared to their cis analogs. Biochemistry 44, 4458–4465 (2005).
Cheng, A. M. et al. Apolipoprotein A-I attenuates palmitate-mediated NF-kappaB activation by reducing Toll-like receptor-4 recruitment into lipid rafts. PLOS ONE 7, e33917 (2012).
Wong, S. W. et al. Fatty acids modulate Toll-like receptor 4 activation through regulation of receptor dimerization and recruitment into lipid rafts in a reactive oxygen species-dependent manner. J. Biol. Chem. 284, 27384–27392 (2009).
Kim, K. et al. Dietary omega-3 polyunsaturated fatty acids attenuate hepatic ischemia/reperfusion injury in rats by modulating toll-like receptor recruitment into lipid rafts. Clin. Nutr. 32, 855–862 (2013).
Mitchell, D. C., Niu, S. L. & Litman, B. J. Quantifying the differential effects of DHA and DPA on the early events in visual signal transduction. Chem. Phys. Lipids 165, 393–400 (2012).
Shaikh, S. R., Kinnun, J. J., Leng, X., Williams, J. A. & Wassall, S. R. How polyunsaturated fatty acids modify molecular organization in membranes: insight from NMR studies of model systems. Biochim. Biophys. Acta 1848, 211–219 (2015).
Takashima, A. et al. Combination of n-3 polyunsaturated fatty acids reduces atherogenesis in apolipoprotein E-deficient mice by inhibiting macrophage activation. Atherosclerosis 254, 142–150 (2016).
Turk, H. F. & Chapkin, R. S. Membrane lipid raft organization is uniquely modified by n-3 polyunsaturated fatty acids. Prostaglandins Leukot. Essent. Fatty Acids 88, 43–47 (2013).
Shaikh, S. R. & Teague, H. N-3 fatty acids and membrane microdomains: from model membranes to lymphocyte function. Prostaglandins Leukot. Essent. Fatty Acids 87, 205–208 (2012).
Aires, V., Hichami, A., Boulay, G. & Khan, N. A. Activation of TRPC6 calcium channels by diacylglycerol (DAG)-containing arachidonic acid: a comparative study with DAG-containing docosahexaenoic acid. Biochimie 89, 926–937 (2007).
Singh, T. U., Choudhury, S., Parida, S., Maruti, B. S. & Mishra, S. K. Arachidonic acid inhibits Na(+)-K(+)-ATPase via cytochrome P-450, lipoxygenase and protein kinase C-dependent pathways in sheep pulmonary artery. Vascul. Pharmacol. 56, 84–90 (2012).
Watanabe, H. et al. Anandamide and arachidonic acid use epoxyeicosatrienoic acids to activate TRPV4 channels. Nature 424, 434–438 (2003).
Antollini, S. S. & Barrantes, F. J. Fatty acid regulation of voltage- and ligand-gated ion channel function. Front. Physiol. 7, 573 (2016).
Borjesson, S. I. & Elinder, F. An electrostatic potassium channel opener targeting the final voltage sensor transition. J. Gen. Physiol. 137, 563–577 (2011).
Hoshi, T., Tian, Y., Xu, R., Heinemann, S. H. & Hou, S. Mechanism of the modulation of BK potassium channel complexes with different auxiliary subunit compositions by the omega-3 fatty acid DHA. Proc. Natl Acad. Sci. USA 110, 4822–4827 (2013).
Hoshi, T., Xu, R., Hou, S., Heinemann, S. H. & Tian, Y. A point mutation in the human Slo1 channel that impairs its sensitivity to omega-3 docosahexaenoic acid. J. Gen. Physiol. 142, 507–522 (2013).
Jump, D. B., Tripathy, S. & Depner, C. M. Fatty acid-regulated transcription factors in the liver. Annu. Rev. Nutr. 33, 249–269 (2013).
McIntosh, A. L., Petrescu, A. D., Hostetler, H. A., Kier, A. B. & Schroeder, F. Liver-type fatty acid binding protein interacts with hepatocyte nuclear factor 4alpha. FEBS Lett. 587, 3787–3791 (2013).
Petrescu, A. D. et al. Impact of L-FABP and glucose on polyunsaturated fatty acid induction of PPARalpha-regulated beta-oxidative enzymes. Am. J. Physiol. Gastrointest. Liver Physiol. 304, G241–G256 (2013).
Schroeder, F. et al. Role of fatty acid binding proteins and long chain fatty acids in modulating nuclear receptors and gene transcription. Lipids 43, 1–17 (2008).
Nakamura, M. T., Yudell, B. E. & Loor, J. J. Regulation of energy metabolism by long-chain fatty acids. Prog. Lipid Res. 53, 124–144 (2014).
Trombetta, A. et al. Increase of palmitic acid concentration impairs endothelial progenitor cell and bone marrow-derived progenitor cell bioavailability: role of the STAT5/PPARgamma transcriptional complex. Diabetes 62, 1245–1257 (2013).
Cintra, D. E. et al. Unsaturated fatty acids revert diet-induced hypothalamic inflammation in obesity. PLOS ONE 7, e30571 (2012).
Oliveira, V. et al. Diets containing alpha-linolenic (omega3) or oleic (omega9) fatty acids rescues obese mice from insulin resistance. Endocrinology 156, 4033–4046 (2015).
Oh, D. Y. et al. GPR120 is an omega-3 fatty acid receptor mediating potent anti-inflammatory and insulin-sensitizing effects. Cell 142, 687–698 (2010).
Shearer, G. C., Savinova, O. V. & Harris, W. S. Fish oil — how does it reduce plasma triglycerides? Biochim. Biophys. Acta 1821, 843–851 (2012).
Mitchell, J. A. & Kirkby, N. S. Eicosanoids, prostacyclin and cyclooxygenase in the cardiovascular system. Br. J. Pharmacol. 176, 1038–1050 (2018).
Inceoglu, B., Bettaieb, A., Haj, F. G., Gomes, A. V. & Hammock, B. D. Modulation of mitochondrial dysfunction and endoplasmic reticulum stress are key mechanisms for the wide-ranging actions of epoxy fatty acids and soluble epoxide hydrolase inhibitors. Prostaglandins Other Lipid Mediat. 133, 68–78 (2017).
Romashko, M., Schragenheim, J., Abraham, N. G. & McClung, J. A. Epoxyeicosatrienoic acid as therapy for diabetic and ischemic cardiomyopathy. Trends Pharmacol. Sci. 37, 945–962 (2016).
Serhan, C. N. & Levy, B. D. Resolvins in inflammation: emergence of the pro-resolving superfamily of mediators. J. Clin. Invest. 128, 2657–2669 (2018).
Chen, W. et al. CYP2J2 and EETs protect against lung ischemia/reperfusion injury via anti-inflammatory effects in vivo and in vitro. Cell. Physiol. Biochem. 35, 2043–2054 (2015).
Kim, J., Imig, J. D., Yang, J., Hammock, B. D. & Padanilam, B. J. Inhibition of soluble epoxide hydrolase prevents renal interstitial fibrosis and inflammation. Am. J. Physiol. Renal Physiol. 307, F971–F980 (2014).
Li, R. et al. CYP2J2 attenuates metabolic dysfunction in diabetic mice by reducing hepatic inflammation via the PPARgamma. Am. J. Physiol. Endocrinol. Metab. 308, E270–E282 (2015).
Kain, V. et al. Resolvin D1 activates the inflammation resolving response at splenic and ventricular site following myocardial infarction leading to improved ventricular function. J. Mol. Cell. Cardiol. 84, 24–35 (2015).
Liu, G. et al. Early treatment with Resolvin E1 facilitates myocardial recovery from ischaemia in mice. Br. J. Pharmacol. 175, 1205–1216 (2018).
Spite, M., Claria, J. & Serhan, C. N. Resolvins, specialized proresolving lipid mediators, and their potential roles in metabolic diseases. Cell Metab. 19, 21–36 (2014).
Akintoye, E. et al. Effect of fish oil on monoepoxides derived from fatty acids during cardiac surgery. J. Lipid Res. 57, 492–498 (2016).
Barden, A. E., Mas, E. & Mori, T. A. n-3 Fatty acid supplementation and proresolving mediators of inflammation. Curr. Opin. Lipidol. 27, 26–32 (2016).
Elajami, T. K. et al. Specialized proresolving lipid mediators in patients with coronary artery disease and their potential for clot remodeling. FASEB J. 30, 2792–2801 (2016).
Gleim, S., Stitham, J., Tang, W. H., Martin, K. A. & Hwa, J. An eicosanoid-centric view of atherothrombotic risk factors. Cell. Mol. Life Sci. 69, 3361–3380 (2012).
Keys, A. et al. The diet and 15-year death rate in the seven countries study. Am. J. Epidemiol. 124, 903–915 (1986).
Hegsted, D. M., McGandy, R. B., Myers, M. L. & Stare, F. J. Quantitative effects of dietary fat on serum cholesterol in man. Am. J. Clin. Nutr. 17, 281–295 (1965).
Keys, A., Anderson, J. T. & Grande, F. Serum cholesterol response to changes in the diet: IV. Particular saturated fatty acids in the diet. Metabolism 14, 776–787 (1965).
Mozaffarian, D. & Ludwig, D. S. The 2015 US dietary guidelines: lifting the ban on total dietary fat. JAMA 313, 2421–2422 (2015).
Lu, M., Wan, Y., Yang, B., Huggins, C. E. & Li, D. Effects of low-fat compared with high-fat diet on cardiometabolic indicators in people with overweight and obesity without overt metabolic disturbance: a systematic review and meta-analysis of randomised controlled trials. Br. J. Nutr. 119, 96–108 (2018).
Schwingshackl, L. & Hoffmann, G. Comparison of effects of long-term low-fat versus high-fat diets on blood lipid levels in overweight or obese patients: a systematic review and meta-analysis. J. Acad. Nutr. Diet. 113, 1640–1661 (2013).
Huntriss, R., Campbell, M. & Bedwell, C. The interpretation and effect of a low-carbohydrate diet in the management of type 2 diabetes: a systematic review and meta-analysis of randomised controlled trials. Eur. J. Clin. Nutr. 72, 311–325 (2018).
Alhazmi, A., Stojanovski, E., McEvoy, M. & Garg, M. L. Macronutrient intakes and development of type 2 diabetes: a systematic review and meta-analysis of cohort studies. J. Am. Coll. Nutr. 31, 243–258 (2012).
Dehghan, M. et al. Associations of fats and carbohydrate intake with cardiovascular disease and mortality in 18 countries from five continents (PURE): a prospective cohort study. Lancet 390, 2050–2062 (2017).
Mente, A., de Koning, L., Shannon, H. S. & Anand, S. S. A systematic review of the evidence supporting a causal link between dietary factors and coronary heart disease. Arch. Intern. Med. 169, 659–669 (2009).
Howard, B. V. et al. Low-fat dietary pattern and risk of cardiovascular disease: the Women’s Health Initiative Randomized Controlled Dietary Modification Trial. JAMA 295, 655–666 (2006).
Tinker, L. F. et al. Low-fat dietary pattern and risk of treated diabetes mellitus in postmenopausal women: the Women’s Health Initiative randomized controlled dietary modification trial. Arch. Intern. Med. 168, 1500–1511 (2008).
Dong, J. Y., Zhang, Y. H., Wang, P. & Qin, L. Q. Meta-analysis of dietary glycemic load and glycemic index in relation to risk of coronary heart disease. Am. J. Cardiol. 109, 1608–1613 (2012).
Ma, X. Y., Liu, J. P. & Song, Z. Y. Glycemic load, glycemic index and risk of cardiovascular diseases: meta-analyses of prospective studies. Atherosclerosis 223, 491–496 (2012).
Vaccarino, V. et al. Ischaemic heart disease in women: are there sex differences in pathophysiology and risk factors? Position paper from the working group on coronary pathophysiology and microcirculation of the European Society of Cardiology. Cardiovasc. Res. 90, 9–17 (2011).
Estruch, R. et al. Primary prevention of cardiovascular disease with a mediterranean diet supplemented with extra-virgin olive oil or nuts. N. Engl. J. Med. 378, e34 (2018).
Salas-Salvado, J. et al. Prevention of diabetes with Mediterranean diets: a subgroup analysis of a randomized trial. Ann. Intern. Med. 160, 1–10 (2014).
2015 US Dietary Guidelines Advisory Committee. Scientific Report of the 2015 Dietary Guidelines Advisory Committee: Advisory Report to the Secretary of Health and Human Services and the Secretary of Agriculture (US Department of Agriculture, Agricultural Research Service, Washington, DC, 2015).
Trumbo, P., Schlicker, S., Yates, A. A. & Poos, M. Dietary reference intakes for energy, carbohydrate, fiber, fat, fatty acids, cholesterol, protein and amino acids. J. Am. Diet. Assoc. 102, 1621–1630 (2002).
World Health Organization. Fact sheets: healthy diet. WHO http://www.who.int/news-room/fact-sheets/detail/healthy-diet (2018).
The Nielsen Company. Nielsen global health & wellness report. Nielsen https://www.nielsen.com/content/dam/nielsenglobal/eu/nielseninsights/pdfs/Nielsen%20Global%20Health%20and%20Wellness%20Report%20-%20January%202015.pdf (2015).
Hu, T. et al. Effects of low-carbohydrate diets versus low-fat diets on metabolic risk factors: a meta-analysis of randomized controlled clinical trials. Am. J. Epidemiol. 176, S44–S54 (2012).
Tobias, D. K. et al. Effect of low-fat diet interventions versus other diet interventions on long-term weight change in adults: a systematic review and meta-analysis. Lancet Diabetes Endocrinol. 3, 968–979 (2015).
Kodama, S. et al. Influence of fat and carbohydrate proportions on the metabolic profile in patients with type 2 diabetes: a meta-analysis. Diabetes Care 32, 959–965 (2009).
Schwingshackl, L. & Hoffmann, G. Comparison of the long-term effects of high-fat v. low-fat diet consumption on cardiometabolic risk factors in subjects with abnormal glucose metabolism: a systematic review and meta-analysis. Br. J. Nutr. 111, 2047–2058 (2014).
Bazzano, L. A. et al. Effects of low-carbohydrate and low-fat diets: a randomized trial. Ann. Intern. Med. 161, 309–318 (2014).
Hooper, L. et al. Effect of reducing total fat intake on body weight: systematic review and meta-analysis of randomised controlled trials and cohort studies. BMJ 345, e7666 (2012).
Estruch, R. et al. Effect of a high-fat Mediterranean diet on bodyweight and waist circumference: a prespecified secondary outcomes analysis of the PREDIMED randomised controlled trial. Lancet Diabetes Endocrinol. 4, 666–676 (2016).
Forouhi, N. G., Krauss, R. M., Taubes, G. & Willett, W. Dietary fat and cardiometabolic health: evidence, controversies, and consensus for guidance. BMJ 361, k2139 (2018).
Forouhi, N. G., Misra, A., Mohan, V., Taylor, R. & Yancy, W. Dietary and nutritional approaches for prevention and management of type 2 diabetes. BMJ 361, k2234 (2018).
Gardner, C. D. et al. Effect of low-fat versus low-carbohydrate diet on 12-month weight loss in overweight adults and the association with genotype pattern or insulin secretion: the DIETFITS Randomized Clinical Trial. JAMA 319, 667–679 (2018).
Seidelmann, S. B. et al. Dietary carbohydrate intake and mortality: a prospective cohort study and meta-analysis. Lancet Public Health 3, e419–e428 (2018).
Ordovas, J. M., Ferguson, L. R., Tai, E. S. & Mathers, J. C. Personalised nutrition and health. BMJ 361, k2173 (2018).
de Toro-Martin, J., Arsenault, B. J., Despres, J. P. & Vohl, M. C. Precision nutrition: a review of personalized nutritional approaches for the prevention and management of metabolic syndrome. Nutrients 9, 913 (2017).
Korem, T. et al. Bread affects clinical parameters and induces gut microbiome-associated personal glycemic responses. Cell Metab. 25, 1243–1253 (2017).
Brown, S., Ordovas, J. M. & Campos, H. Interaction between the APOC3 gene promoter polymorphisms, saturated fat intake and plasma lipoproteins. Atherosclerosis 170, 307–313 (2003).
Olivieri, O. et al. Apolipoprotein C-III, n-3 polyunsaturated fatty acids, and “insulin-resistant” T-455C APOC3 gene polymorphism in heart disease patients: example of gene-diet interaction. Clin. Chem. 51, 360–367 (2005).
Pollin, T. I. & Quartuccio, M. What we know about diet, genes, and dyslipidemia: is there potential for translation? Curr. Nutr. Rep. 2, 236–242 (2013).
Salas, J. et al. The SstI polymorphism of the apolipoprotein C-III gene determines the insulin response to an oral-glucose-tolerance test after consumption of a diet rich in saturated fats. Am. J. Clin. Nutr. 68, 396–401 (1998).
Carvalho-Wells, A. L., Jackson, K. G., Lockyer, S., Lovegrove, J. A. & Minihane, A. M. APOE genotype influences triglyceride and C-reactive protein responses to altered dietary fat intake in UK adults. Am. J. Clin. Nutr. 96, 1447–1453 (2012).
Garcia-Rios, A. et al. Genetic variations at the lipoprotein lipase gene influence plasma lipid concentrations and interact with plasma n-6 polyunsaturated fatty acids to modulate lipid metabolism. Atherosclerosis 218, 416–422 (2011).
Celis-Morales, C. et al. Effect of personalized nutrition on health-related behaviour change: evidence from the Food4Me European randomized controlled trial. Int. J. Epidemiol. 46, 578–588 (2017).
Lichtenstein, A. H. Dietary trans fatty acids and cardiovascular disease risk: past and present. Curr. Atheroscler. Rep. 16, 433 (2014).
Mensink, R. P. Effects of saturated fatty acids on serum lipids and lipoproteins: a systematic review and regression analysis (WHO, Geneva, 2016).
Gerber, P. A. & Berneis, K. Regulation of low-density lipoprotein subfractions by carbohydrates. Curr. Opin. Clin. Nutr. Metabol. Care 15, 381–385 (2012).
Siri, P. W. & Krauss, R. M. Influence of dietary carbohydrate and fat on LDL and HDL particle distributions. Curr. Atheroscler. Rep. 7, 455–459 (2005).
Bhatt, D. L. et al. Cardiovascular risk reduction with icosapent ethyl for hypertriglyceridemia. N. Engl. J. Med. 380, 11–22 (2019).
Do, R. et al. Common variants associated with plasma triglycerides and risk for coronary artery disease. Nat. Genet. 45, 1345–1352 (2013).
Nordestgaard, B. G. Triglyceride-rich lipoproteins and atherosclerotic cardiovascular disease: new insights from epidemiology, genetics, and biology. Circ. Res. 118, 547–563 (2016).
Thomsen, M., Varbo, A., Tybjaerg-Hansen, A. & Nordestgaard, B. G. Low nonfasting triglycerides and reduced all-cause mortality: a mendelian randomization study. Clin. Chem. 60, 737–746 (2014).
Varbo, A. et al. Remnant cholesterol as a causal risk factor for ischemic heart disease. J. Am. Coll. Cardiol. 61, 427–436 (2013).
Institute of Medicine. Evaluation of Biomarkers and Surrogate Endpoints in Chronic Disease (The National Academies Press, Washington, DC, 2010).
Imamura, F. et al. Effects of saturated fat, polyunsaturated fat, monounsaturated fat, and carbohydrate on glucose-insulin homeostasis: a systematic review and meta-analysis of randomised controlled feeding trials. PLOS Med. 13, e1002087 (2016).
Chowdhury, R. et al. Association of dietary, circulating, and supplement fatty acids with coronary risk: a systematic review and meta-analysis. Ann. Intern. Med. 160, 398–406 (2014).
de Souza, R. J. et al. Intake of saturated and trans unsaturated fatty acids and risk of all cause mortality, cardiovascular disease, and type 2 diabetes: systematic review and meta-analysis of observational studies. BMJ 351, h3978 (2015).
Jakobsen, M. U. et al. Major types of dietary fat and risk of coronary heart disease: a pooled analysis of 11 cohort studies. Am. J. Clin. Nutr. 89, 1425–1432 (2009).
Farvid, M. S. et al. Dietary linoleic acid and risk of coronary heart disease: a systematic review and meta-analysis of prospective cohort studies. Circulation 130, 1568–1578 (2014).
Meyer, K. A., Kushi, L. H., Jacobs, D. R. Jr & Folsom, A. R. Dietary fat and incidence of type 2 diabetes in older Iowa women. Diabetes Care 24, 1528–1535 (2001).
Salmeron, J. et al. Dietary fat intake and risk of type 2 diabetes in women. Am. J. Clin. Nutr. 73, 1019–1026 (2001).
van Dam, R. M., Willett, W. C., Rimm, E. B., Stampfer, M. J. & Hu, F. B. Dietary fat and meat intake in relation to risk of type 2 diabetes in men. Diabetes Care 25, 417–424 (2002).
McGee, D. et al. The relationship of dietary fat and cholesterol to mortality in 10 years: the Honolulu Heart Program. Int. J. Epidemiol. 14, 97–105 (1985).
Takeya, Y. et al. Epidemiologic studies of coronary heart disease and stroke in Japanese men living in Japan, Hawaii and California: incidence of stroke in Japan and Hawaii. Stroke 15, 15–23 (1984).
Iso, H. et al. Fat and protein intakes and risk of intraparenchymal hemorrhage among middle-aged Japanese. Am. J. Epidemiol. 157, 32–39 (2003).
Miettinen, M., Turpeinen, O., Karvonen, M. J., Elosuo, R. & Paavilainen, E. Effect of cholesterol-lowering diet on mortality from coronary heart-disease and other causes. A twelve-year clinical trial in men and women. Lancet 2, 835–838 (1972).
Turpeinen, O. et al. Dietary prevention of coronary heart disease: the Finnish Mental Hospital Study. Int. J. Epidemiol. 8, 99–118 (1979).
Ramsden, C. E. et al. Use of dietary linoleic acid for secondary prevention of coronary heart disease and death: evaluation of recovered data from the Sydney Diet Heart Study and updated meta-analysis. BMJ 346, e8707 (2013).
Ramsden, C. E. et al. Re-evaluation of the traditional diet-heart hypothesis: analysis of recovered data from Minnesota Coronary Experiment (1968–1973). BMJ 353, i1246 (2016).
Mozaffarian, D., Micha, R. & Wallace, S. Effects on coronary heart disease of increasing polyunsaturated fat in place of saturated fat: a systematic review and meta-analysis of randomized controlled trials. PLOS Med. 7, e1000252 (2010).
Jakobsen, M. U. et al. Intake of carbohydrates compared with intake of saturated fatty acids and risk of myocardial infarction: importance of the glycemic index. Am. J. Clin. Nutr. 91, 1764–1768 (2010).
Li, Y. et al. Saturated fats compared with unsaturated fats and sources of carbohydrates in relation to risk of coronary heart disease: a prospective cohort study. J. Am. Coll. Cardiol. 66, 1538–1548 (2015).
Bourdua-Roy, E. Low-carb, high-fat is what we physicians eat. You should, too. HuffPost https://www.huffingtonpost.ca/evelyne-bourdua-roy/low-carb-high-fat-is-what-we-physicians-eat-you-should-too_a_23232610/ (2017).
Gunnars, K. A low-carb diet meal plan and menu that can save your life. Healthline https://www.healthline.com/nutrition/low-carb-diet-meal-plan-and-menu (2018).
US Department of Health & Human Services & US Department of Agriculture. Dietary guidelines for americans — 2015–2020. 8th edition. Health https://health.gov/dietaryguidelines/2015/guidelines/ (2018).
World Health Organization. Draft guidelines on saturated fatty acid and trans-fatty acid intake for adults and children. WHO https://extranet.who.int/dataform/upload/surveys/666752/files/Draft%20WHO%20SFA-TFA%20guidelines_04052018%20Public%20Consultation(1).pdf (2018).
Sacks, F. M. et al. Dietary fats and cardiovascular disease: a presidential advisory from the American Heart Association. Circulation 136, e1–e23 (2017).
Mozaffarian, D. & Wu, J. H. Y. Flavonoids, dairy foods, and cardiovascular and metabolic health: a review of emerging biologic pathways. Circ. Res. 122, 369–384 (2018).
Heart and Stroke Foundation of Canada. Position statement on saturated fat, heart disease, and stroke. Heart & Stroke Foundation Canada https://www.heartandstroke.ca/-/media/pdf-files/canada/position-statement/saturatedfat-eng-final.ashx (2018).
Nordestgaard, B. G. & Langsted, A. Lipoprotein (a) as a cause of cardiovascular disease: insights from epidemiology, genetics, and biology. J. Lipid Res. 57, 1953–1975 (2016).
Berglund, L. et al. Comparison of monounsaturated fat with carbohydrates as a replacement for saturated fat in subjects with a high metabolic risk profile: studies in the fasting and postprandial states. Am. J. Clin. Nutr. 86, 1611–1620 (2007).
Faghihnia, N., Tsimikas, S., Miller, E. R., Witztum, J. L. & Krauss, R. M. Changes in lipoprotein(a), oxidized phospholipids, and LDL subclasses with a low-fat high-carbohydrate diet. J. Lipid Res. 51, 3324–3330 (2010).
Shin, M. J., Blanche, P. J., Rawlings, R. S., Fernstrom, H. S. & Krauss, R. M. Increased plasma concentrations of lipoprotein(a) during a low-fat, high-carbohydrate diet are associated with increased plasma concentrations of apolipoprotein C-III bound to apolipoprotein B-containing lipoproteins. Am. J. Clin. Nutr. 85, 1527–1532 (2007).
Ballantyne, C. M. et al. Icosapent ethyl (eicosapentaenoic acid ethyl ester): Effects on plasma apolipoprotein C-III levels in patients from the MARINE and ANCHOR studies. J. Clin. Lipidol. 10, 635–645 (2016).
Morton, A. M. et al. The effect of omega-3 carboxylic acids on apolipoprotein CIII-containing lipoproteins in severe hypertriglyceridemia. J. Clin. Lipidol. 10, 1442–1451 (2016).
Skulas-Ray, A. C., Alaupovic, P., Kris-Etherton, P. M. & West, S. G. Dose-response effects of marine omega-3 fatty acids on apolipoproteins, apolipoprotein-defined lipoprotein subclasses, and Lp-PLA2 in individuals with moderate hypertriglyceridemia. J. Clin. Lipidol. 9, 360–367 (2015).
Jensen, M. K. et al. High-density lipoprotein subspecies defined by presence of apolipoprotein C-III and incident coronary heart disease in four cohorts. Circulation 137, 1364–1373 (2018).
Mendivil, C. O., Rimm, E. B., Furtado, J. & Sacks, F. M. Apolipoprotein E in VLDL and LDL with apolipoprotein C-III is associated with a lower risk of coronary heart disease. J. Am. Heart Assoc. 2, e000130 (2013).
Archer, W. R. et al. Variations in plasma apolipoprotein C-III levels are strong correlates of the triglyceride response to a high-monounsaturated fatty acid diet and a high-carbohydrate diet. Metabolism 54, 1390–1397 (2005).
Furtado, J. D. et al. Effect of protein, unsaturated fat, and carbohydrate intakes on plasma apolipoprotein B and VLDL and LDL containing apolipoprotein C-III: results from the OmniHeart Trial. Am. J. Clin. Nutr. 87, 1623–1630 (2008).
Bohl, M., Bjornshave, A., Larsen, M. K., Gregersen, S. & Hermansen, K. The effects of proteins and medium-chain fatty acids from milk on body composition, insulin sensitivity and blood pressure in abdominally obese adults. Eur. J. Clin. Nutr. 71, 76–82 (2017).
Matualatupauw, J. C., Bohl, M., Gregersen, S., Hermansen, K. & Afman, L. A. Dietary medium-chain saturated fatty acids induce gene expression of energy metabolism-related pathways in adipose tissue of abdominally obese subjects. Int. J. Obes. 41, 1348–1354 (2017).
Wang, M. E. et al. Increasing dietary medium-chain fatty acid ratio mitigates high-fat diet-induced non-alcoholic steatohepatitis by regulating autophagy. Sci. Rep. 7, 13999 (2017).
Wein, S. et al. Medium-chain fatty acids ameliorate insulin resistance caused by high-fat diets in rats. Diabetes Metab. Res. Rev. 25, 185–194 (2009).
Hu, F. B. et al. Dietary saturated fats and their food sources in relation to the risk of coronary heart disease in women. Am. J. Clin. Nutr. 70, 1001–1008 (1999).
Liu, S., van der Schouw, Y. T., Soedamah-Muthu, S. S., Spijkerman, A. M. W. & Sluijs, I. Intake of dietary saturated fatty acids and risk of type 2 diabetes in the European Prospective Investigation into Cancer and Nutrition-Netherlands cohort: associations by types, sources of fatty acids and substitution by macronutrients. Eur. J. Nutr. https://doi.org/10.1007/s00394-018-1630-4 (2018).
Praagman, J. et al. The association between dietary saturated fatty acids and ischemic heart disease depends on the type and source of fatty acid in the European Prospective Investigation into Cancer and Nutrition-Netherlands cohort. Am. J. Clin. Nutr. 103, 356–365 (2016).
Praagman, J. et al. Dietary saturated fatty acids and coronary heart disease risk in a Dutch middle-aged and elderly population. Arterioscler. Thromb. Vasc. Biol. 36, 2011–2018 (2016).
Zong, G. et al. Intake of individual saturated fatty acids and risk of coronary heart disease in US men and women: two prospective longitudinal cohort studies. BMJ 355, i5796 (2016).
Ma, W. et al. Prospective association of fatty acids in the de novo lipogenesis pathway with risk of type 2 diabetes: the Cardiovascular Health Study. Am. J. Clin. Nutr. 101, 153–163 (2015).
Kabagambe, E. K., Baylin, A., Siles, X. & Campos, H. Individual saturated fatty acids and nonfatal acute myocardial infarction in Costa Rica. Eur. J. Clin. Nutr. 57, 1447–1457 (2003).
Kromhout, D. et al. Dietary saturated and trans fatty acids and cholesterol and 25-year mortality from coronary heart disease: the Seven Countries Study. Prev. Med. 24, 308–315 (1995).
Volk, B. M. et al. Effects of step-wise increases in dietary carbohydrate on circulating saturated Fatty acids and palmitoleic acid in adults with metabolic syndrome. PLOS ONE 9, e113605 (2014).
Wu, J. H. et al. Fatty acids in the de novo lipogenesis pathway and risk of coronary heart disease: the Cardiovascular Health Study. Am. J. Clin. Nutr. 94, 431–438 (2011).
Lee, J. J. et al. Palmitoleic acid is elevated in fatty liver disease and reflects hepatic lipogenesis. Am. J. Clin. Nutr. 101, 34–43 (2015).
Imamura, F. et al. Fatty acid biomarkers of dairy fat consumption and incident diabetes: a pooled analysis of prospective cohort studies. PLOS Med. 15, e1002670 (2018).
Liang, J., Zhou, Q., Kwame Amakye, W., Su, Y. & Zhang, Z. Biomarkers of dairy fat intake and risk of cardiovascular disease: a systematic review and meta analysis of prospective studies. Crit. Rev. Food Sci. Nutr. 58, 1122–1130 (2018).
Huth, P. J., Fulgoni, V. L., Keast, D. R., Park, K. & Auestad, N. Major food sources of calories, added sugars, and saturated fat and their contribution to essential nutrient intakes in the U.S. diet: data from the National Health and Nutrition Examination Survey (2003–2006). Nutr. J. 12, 116 (2013).
Li, K. et al. Dietary fat intakes in Irish adults in 2011: how much has changed in 10 years? Br. J. Nutr. 115, 1798–1809 (2016).
O’Sullivan, T. A., Ambrosini, G., Beilin, L. J., Mori, T. A. & Oddy, W. H. Dietary intake and food sources of fatty acids in Australian adolescents. Nutrition 27, 153–159 (2011).
Shen, X. et al. Trends in dietary fat and fatty acid intakes and related food sources among Chinese adults: a longitudinal study from the China Health and Nutrition Survey (1997–2011). Public Health Nutr. 20, 2927–2936 (2017).
Abete, I., Romaguera, D., Vieira, A. R., Lopez de Munain, A. & Norat, T. Association between total, processed, red and white meat consumption and all-cause, CVD and IHD mortality: a meta-analysis of cohort studies. Br. J. Nutr. 112, 762–775 (2014).
Aune, D., Norat, T., Romundstad, P. & Vatten, L. J. Dairy products and the risk of type 2 diabetes: a systematic review and dose-response meta-analysis of cohort studies. Am. J. Clin. Nutr. 98, 1066–1083 (2013).
Chen, G. C., Lv, D. B., Pang, Z. & Liu, Q. F. Red and processed meat consumption and risk of stroke: a meta-analysis of prospective cohort studies. Eur. J. Clin. Nutr. 67, 91–95 (2013).
Chen, M. et al. Dairy consumption and risk of type 2 diabetes: 3 cohorts of US adults and an updated meta-analysis. BMC Med. 12, 215 (2014).
Hu, D., Huang, J., Wang, Y., Zhang, D. & Qu, Y. Dairy foods and risk of stroke: a meta-analysis of prospective cohort studies. Nutr. Metab. Cardiovasc. Dis. 24, 460–469 (2014).
Pan, A. et al. Red meat consumption and risk of type 2 diabetes: 3 cohorts of US adults and an updated meta-analysis. Am. J. Clin. Nutr. 94, 1088–1096 (2011).
Qin, L. Q. et al. Dairy consumption and risk of cardiovascular disease: an updated meta-analysis of prospective cohort studies. Asia Pac. J. Clin. Nutr. 24, 90–100 (2015).
Soedamah-Muthu, S. S. et al. Milk and dairy consumption and incidence of cardiovascular diseases and all-cause mortality: dose-response meta-analysis of prospective cohort studies. Am. J. Clin. Nutr. 93, 158–171 (2011).
Yuan, S., Li, X., Jin, Y. & Lu, J. Chocolate consumption and risk of coronary heart disease, stroke, and diabetes: a meta-analysis of prospective studies. Nutrients 9, 688 (2017).
de Oliveira Otto, M. C. et al. Dietary intake of saturated fat by food source and incident cardiovascular disease: the multi-ethnic study of atherosclerosis. Am. J. Clin. Nutr. 96, 397–404 (2012).
Micha, R., Wallace, S. K. & Mozaffarian, D. Red and processed meat consumption and risk of incident coronary heart disease, stroke, and diabetes mellitus: a systematic review and meta-analysis. Circulation 121, 2271–2283 (2010).
Wang, X. et al. Red and processed meat consumption and mortality: dose-response meta-analysis of prospective cohort studies. Public Health Nutr. 19, 893–905 (2016).
Micha, R., Michas, G. & Mozaffarian, D. Unprocessed red and processed meats and risk of coronary artery disease and type 2 diabetes—an updated review of the evidence. Curr. Atheroscler. Rep. 14, 515–524 (2012).
Fernandez-Real, J. M., McClain, D. & Manco, M. Mechanisms linking glucose homeostasis and iron metabolism toward the onset and progression of type 2 diabetes. Diabetes Care 38, 2169–2176 (2015).
Wang, X., Fang, X. & Wang, F. Pleiotropic actions of iron balance in diabetes mellitus. Rev. Endocr. Metab. Disord. 16, 15–23 (2015).
Berkey, C. S., Rockett, H. R., Willett, W. C. & Colditz, G. A. Milk, dairy fat, dietary calcium, and weight gain: a longitudinal study of adolescents. Arch. Pediatr. Adolesc. Med. 159, 543–550 (2005).
Gao, D. et al. Dairy products consumption and risk of type 2 diabetes: systematic review and dose-response meta-analysis. PLOS ONE 8, e73965 (2013).
Huh, S. Y., Rifas-Shiman, S. L., Rich-Edwards, J. W., Taveras, E. M. & Gillman, M. W. Prospective association between milk intake and adiposity in preschool-aged children. J. Am. Diet. Assoc. 110, 563–570 (2010).
Mozaffarian, D., Hao, T., Rimm, E. B., Willett, W. C. & Hu, F. B. Changes in diet and lifestyle and long-term weight gain in women and men. N. Engl. J. Med. 364, 2392–2404 (2011).
Noel, S. E., Ness, A. R., Northstone, K., Emmett, P. & Newby, P. K. Milk intakes are not associated with percent body fat in children from ages 10 to 13 years. J. Nutr. 141, 2035–2041 (2011).
Noel, S. E., Ness, A. R., Northstone, K., Emmett, P. & Newby, P. K. Associations between flavored milk consumption and changes in weight and body composition over time: differences among normal and overweight children. Eur. J. Clin. Nutr. 67, 295–300 (2013).
Pimpin, L., Wu, J. H., Haskelberg, H., Del Gobbo, L. & Mozaffarian, D. Is butter back? A systematic review and meta-analysis of butter consumption and risk of cardiovascular disease, diabetes, and total mortality. PLOS ONE 11, e0158118 (2016).
Scharf, R. J., Demmer, R. T. & DeBoer, M. D. Longitudinal evaluation of milk type consumed and weight status in preschoolers. Arch. Dis. Child. 98, 335–340 (2013).
Smith, J. D. et al. Changes in intake of protein foods, carbohydrate amount and quality, and long-term weight change: results from 3 prospective cohorts. Am. J. Clin. Nutr. 101, 1216–1224 (2015).
Wang, H. et al. Longitudinal association between dairy consumption and changes of body weight and waist circumference: the Framingham Heart Study. Int. J. Obes. 38, 299–305 (2014).
de Goede, J., Geleijnse, J. M., Ding, E. L. & Soedamah-Muthu, S. S. Effect of cheese consumption on blood lipids: a systematic review and meta-analysis of randomized controlled trials. Nutr. Rev. 73, 259–275 (2015).
Drouin-Chartier, J. P. et al. Comprehensive review of the impact of dairy foods and dairy fat on cardiometabolic risk. Adv. Nutr. 7, 1041–1051 (2016).
Fattore, E., Bosetti, C., Brighenti, F., Agostoni, C. & Fattore, G. Palm oil and blood lipid-related markers of cardiovascular disease: a systematic review and meta-analysis of dietary intervention trials. Am. J. Clin. Nutr. 99, 1331–1350 (2014).
Pedersen, A., Marckmann, P. & Sandstrom, B. Postprandial lipoprotein, glucose and insulin responses after two consecutive meals containing rapeseed oil, sunflower oil or palm oil with or without glucose at the first meal. Br. J. Nutr. 82, 97–104 (1999).
Stonehouse, W., Brinkworth, G. D. & Noakes, M. Palmolein and olive oil consumed within a high protein test meal have similar effects on postprandial endothelial function in overweight and obese men: a randomized controlled trial. Atherosclerosis 239, 178–185 (2015).
Teng, K. T., Nagapan, G., Cheng, H. M. & Nesaretnam, K. Palm olein and olive oil cause a higher increase in postprandial lipemia compared with lard but had no effect on plasma glucose, insulin and adipocytokines. Lipids 46, 381–388 (2011).
Vega-Lopez, S., Ausman, L. M., Jalbert, S. M., Erkkila, A. T. & Lichtenstein, A. H. Palm and partially hydrogenated soybean oils adversely alter lipoprotein profiles compared with soybean and canola oils in moderately hyperlipidemic subjects. Am. J. Clin. Nutr. 84, 54–62 (2006).
Tholstrup, T., Hjerpsted, J. & Raff, M. Palm olein increases plasma cholesterol moderately compared with olive oil in healthy individuals. Am. J. Clin. Nutr. 94, 1426–1432 (2011).
Kabagambe, E. K., Baylin, A., Ascherio, A. & Campos, H. The type of oil used for cooking is associated with the risk of nonfatal acute myocardial infarction in costa rica. J. Nutr. 135, 2674–2679 (2005).
Feskens, E. J., Sluik, D. & van Woudenbergh, G. J. Meat consumption, diabetes, and its complications. Curr. Diabetes Rep. 13, 298–306 (2013).
Wolk, A. Potential health hazards of eating red meat. J. Intern. Med. 281, 106–122 (2017).
Micha, R., Michas, G., Lajous, M. & Mozaffarian, D. Processing of meats and cardiovascular risk: time to focus on preservatives. BMC Med. 11, 136 (2013).
Rohrmann, S. & Linseisen, J. Processed meat: the real villain? Proc. Nutr. Soc. 75, 233–241 (2016).
Gunnars, K. Is red meat bad for you, or good? An objective look. Healthline https://www.healthline.com/nutrition/is-red-meat-bad-for-you-or-good (2018).
Teicholz, N. The Big Fat Surprise: Why Butter, Meat and Cheese Belong in a Healthy Diet (Simon & Schuster Inc, 2014).
Wang, Y. & Li, S. Worldwide trends in dairy production and consumption and calcium intake: is promoting consumption of dairy products a sustainable solution for inadequate calcium intake? Food Nutr. Bull. 29, 172–185 (2008).
Rodale News. 6 foods that cause inflammation. Women’s Health https://www.womenshealthmag.com/food/a19983367/inflammatory-foods/ (2014).
Campbell, T. C. & Campbell, T. M. The China Study (BenBella Books, 2006).
Myers, A. The dangers of dairy. MindBodyGreen https://www.mindbodygreen.com/0-8646/the-dangers-of-dairy.html (2019).
Chiu, S. et al. Comparison of the DASH (Dietary Approaches to Stop Hypertension) diet and a higher-fat DASH diet on blood pressure and lipids and lipoproteins: a randomized controlled trial. Am. J. Clin. Nutr. 103, 341–347 (2016).
Renaud, S. C., Ruf, J. C. & Petithory, D. The positional distribution of fatty acids in palm oil and lard influences their biologic effects in rats. J. Nutr. 125, 229–237 (1995).
Sun, G. et al. Effects of palm olein and olive oil on serum lipids in a Chinese population: a randomized, double-blind, cross-over trial. Asia Pac. J. Clin. Nutr. 27, 572–580 (2018).
Lucci, P. et al. Palm oil and cardiovascular disease: a randomized trial of the effects of hybrid palm oil supplementation on human plasma lipid patterns. Food Funct. 7, 347–354 (2016).
Odia, O. J., Ofori, S. & Maduka, O. Palm oil and the heart: a review. World J. Cardiol. 7, 144–149 (2015).
Quealy, K. & Sanger-Katz, M. Is sushi “healthy”? What about granola? Where Americans and nutritionists disagree. New York Times https://www.nytimes.com/interactive/2016/07/05/upshot/is-sushi-healthy-what-about-granola-where-americans-and-nutritionists-disagree.html (2016).
Sankararaman, S. & Sferra, T. J. Are we going nuts on coconut oil? Curr. Nutr. Rep. 7, 107–115 (2018).
Savilaakso, S. et al. Systematic review of effects on biodiversity from oil palm production. Environ. Evid. 3, 4 (2014).
Rosqvist, F. et al. Potential role of milk fat globule membrane in modulating plasma lipoproteins, gene expression, and cholesterol metabolism in humans: a randomized study. Am. J. Clin. Nutr. 102, 20–30 (2015).
Beulens, J. W. et al. The role of menaquinones (vitamin K(2)) in human health. Br. J. Nutr. 110, 1357–1368 (2013).
Fretts, A. M. et al. Plasma phospholipid saturated fatty acids and incident atrial fibrillation: the Cardiovascular Health Study. J. Am. Heart Assoc. 3, e000889 (2014).
Lemaitre, R. N. et al. Plasma phospholipid very-long-chain saturated fatty acids and incident diabetes in older adults: the Cardiovascular Health Study. Am. J. Clin. Nutr 101, 1047–1054 (2015).
Malik, V. S. et al. Circulating very-long-chain saturated fatty acids and incident coronary heart disease in US Men and Women. Circulation 132, 260–268 (2015).
Forouhi, N. G. et al. Differences in the prospective association between individual plasma phospholipid saturated fatty acids and incident type 2 diabetes: the EPIC-InterAct case-cohort study. Lancet Diabetes Endocrinol. 2, 810–818 (2014).
Yakoob, M. Y. et al. Circulating biomarkers of dairy fat and risk of incident diabetes mellitus among men and women in the United States in two large prospective cohorts. Circulation 133, 1645–1654 (2016).
Maceyka, M. & Spiegel, S. Sphingolipid metabolites in inflammatory disease. Nature 510, 58–67 (2014).
Pewzner-Jung, Y. et al. A critical role for ceramide synthase 2 in liver homeostasis: II. insights into molecular changes leading to hepatopathy. J. Biol. Chem. 285, 10911–10923 (2010).
Grosch, S., Schiffmann, S. & Geisslinger, G. Chain length-specific properties of ceramides. Prog. Lipid Res. 51, 50–62 (2012).
Huth, P. J., Fulgoni, V. L. 3rd & Larson, B. T. A systematic review of high-oleic vegetable oil substitutions for other fats and oils on cardiovascular disease risk factors: implications for novel high-oleic soybean oils. Adv. Nutr. 6, 674–693 (2015).
Schwingshackl, L. et al. Olive oil in the prevention and management of type 2 diabetes mellitus: a systematic review and meta-analysis of cohort studies and intervention trials. Nutr. Diabetes 7, e262 (2017).
Jones, P. J., Jew, S. & AbuMweis, S. The effect of dietary oleic, linoleic, and linolenic acids on fat oxidation and energy expenditure in healthy men. Metabolism 57, 1198–1203 (2008).
Kien, C. L. & Bunn, J. Y. Gender alters the effects of palmitate and oleate on fat oxidation and energy expenditure. Obesity 16, 29–33 (2008).
Kien, C. L. et al. Dietary intake of palmitate and oleate has broad impact on systemic and tissue lipid profiles in humans. Am. J. Clin. Nutr. 99, 436–445 (2014).
Schmidt, D. E., Allred, J. B. & Kien, C. L. Fractional oxidation of chylomicron-derived oleate is greater than that of palmitate in healthy adults fed frequent small meals. J. Lipid Res. 40, 2322–2332 (1999).
Ros, E. Health benefits of nut consumption. Nutrients 2, 652–682 (2010).
Venkatachalam, M. & Sathe, S. K. Chemical composition of selected edible nut seeds. J. Agric. Food Chem. 54, 4705–4714 (2006).
Del Gobbo, L. C., Falk, M. C., Feldman, R., Lewis, K. & Mozaffarian, D. Effects of tree nuts on blood lipids, apolipoproteins, and blood pressure: systematic review, meta-analysis, and dose-response of 61 controlled intervention trials. Am. J. Clin. Nutr. 102, 1347–1356 (2015).
Mahmassani, H. A., Avendano, E. E., Raman, G. & Johnson, E. J. Avocado consumption and risk factors for heart disease: a systematic review and meta-analysis. Am. J. Clin. Nutr. 107, 523–536 (2018).
Schwingshackl, L. & Hoffmann, G. Monounsaturated fatty acids, olive oil and health status: a systematic review and meta-analysis of cohort studies. Lipids Health Dis. 13, 154 (2014).
Zong, G. et al. Monounsaturated fats from plant and animal sources in relation to risk of coronary heart disease among US men and women. Am. J. Clin. Nutr. 107, 445–453 (2018).
Salas-Salvado, J. et al. Reduction in the incidence of type 2 diabetes with the Mediterranean diet: results of the PREDIMED-Reus nutrition intervention randomized trial. Diabetes Care 34, 14–19 (2011).
Lama, A. et al. Polyphenol-rich virgin olive oil reduces insulin resistance and liver inflammation and improves mitochondrial dysfunction in high-fat diet fed rats. Mol. Nutr. Food Res. 61, 1600418 (2017).
Loffredo, L., Perri, L., Nocella, C. & Violi, F. Antioxidant and antiplatelet activity by polyphenol-rich nutrients: focus on extra virgin olive oil and cocoa. Br. J. Clin. Pharmacol. 83, 96–102 (2017).
Peyrol, J., Riva, C. & Amiot, M. J. Hydroxytyrosol in the prevention of the metabolic syndrome and related disorders. Nutrients 9, 306 (2017).
Valenzuela, R. et al. Molecular adaptations underlying the beneficial effects of hydroxytyrosol in the pathogenic alterations induced by a high-fat diet in mouse liver: PPAR-alpha and Nrf2 activation, and NF-kappaB down-regulation. Food Funct. 8, 1526–1537 (2017).
Degirolamo, C., Shelness, G. S. & Rudel, L. L. LDL cholesteryl oleate as a predictor for atherosclerosis: evidence from human and animal studies on dietary fat. J. Lipid Res. 50, S434–S439 (2009).
Jones, P. J. et al. High-oleic canola oil consumption enriches LDL particle cholesteryl oleate content and reduces LDL proteoglycan binding in humans. Atherosclerosis 238, 231–238 (2015).
Bolling, B. W., Blumberg, J. B. & Chen, C. O. The influence of roasting, pasteurisation, and storage on the polyphenol content and antioxidant capacity of California almond skins. Food Chem. 123, 1040–1047 (2010).
Cicerale, S., Conlan, X. A., Barnett, N. W., Sinclair, A. J. & Keast, R. S. Influence of heat on biological activity and concentration of oleocanthal—a natural anti-inflammatory agent in virgin olive oil. J. Agric. Food Chem. 57, 1326–1330 (2009).
Gomez-Alonso, S., Fregapane, G., Salvador, M. D. & Gordon, M. H. Changes in phenolic composition and antioxidant activity of virgin olive oil during frying. J. Agric. Food Chem. 51, 667–672 (2003).
Chandrasekara, N. & Shahidi, F. Effect of roasting on phenolic content and antioxidant activities of whole cashew nuts, kernels, and testa. J. Agric. Food Chem. 59, 5006–5014 (2011).
Farina, E. K. et al. Dietary intakes of arachidonic acid and alpha-linolenic acid are associated with reduced risk of hip fracture in older adults. J. Nutr. 141, 1146–1153 (2011).
Mann, N. J., Johnson, L. G., Warrick, G. E. & Sinclair, A. J. The arachidonic acid content of the Australian diet is lower than previously estimated. J. Nutr. 125, 2528–2535 (1995).
Bjermo, H. et al. Effects of n-6 PUFAs compared with SFAs on liver fat, lipoproteins, and inflammation in abdominal obesity: a randomized controlled trial. Am. J. Clin. Nutr. 95, 1003–1012 (2012).
Masson, C. J. & Mensink, R. P. Exchanging saturated fatty acids for (n-6) polyunsaturated fatty acids in a mixed meal may decrease postprandial lipemia and markers of inflammation and endothelial activity in overweight men. J. Nutr. 141, 816–821 (2011).
Johnson, G. H. & Fritsche, K. Effect of dietary linoleic acid on markers of inflammation in healthy persons: a systematic review of randomized controlled trials. J. Acad. Nutr. Diet. 112, 1029–1041 (2012).
Kelley, D. S. et al. Effects of dietary arachidonic acid on human immune response. Lipids 32, 449–456 (1997).
Kusumoto, A. et al. Effects of arachidonate-enriched triacylglycerol supplementation on serum fatty acids and platelet aggregation in healthy male subjects with a fish diet. Br. J. Nutr. 98, 626–635 (2007).
Nelson, G. J. et al. The effect of dietary arachidonic acid on plasma lipoprotein distributions, apoproteins, blood lipid levels, and tissue fatty acid composition in humans. Lipids 32, 427–433 (1997).
Hodson, L., Skeaff, C. M. & Fielding, B. A. Fatty acid composition of adipose tissue and blood in humans and its use as a biomarker of dietary intake. Prog. Lipid Res. 47, 348–380 (2008).
Wu, J. H. et al. Circulating omega-6 polyunsaturated fatty acids and total and cause-specific mortality: the Cardiovascular Health Study. Circulation 130, 1245–1253 (2014).
Virtanen, J. K., Wu, J. H. Y., Voutilainen, S., Mursu, J. & Tuomainen, T. P. Serum n-6 polyunsaturated fatty acids and risk of death: the Kuopio Ischaemic Heart Disease Risk Factor Study. Am. J. Clin. Nutr. 107, 427–435 (2018).
Wu, J. H. Y. et al. Omega-6 fatty acid biomarkers and incident type 2 diabetes: pooled analysis of individual-level data for 39 740 adults from 20 prospective cohort studies. Lancet Diabetes Endocrinol. 5, 965–974 (2017).
Marklund, M. et al. Biomarkers of dietary omega-6 fatty acids and incident cardiovascular disease and mortality: an individual-level pooled analysis of 30 cohort studies. Circulation. https://doi.org/10.17863/CAM.36839 (2019).
Marklund, M. et al. Biomarkers of n-6 polyunsaturated fatty acids and CVD risk: a global pooling project of 19 cohort studies. Circulation 133 (Suppl. 1), MP26 (2018).
Hooper, L., Martin, N., Abdelhamid, A. & Davey Smith, G. Reduction in saturated fat intake for cardiovascular disease. Cochrane Database Syst. Rev. 6, CD011737 (2015).
Skeaff, C. M. & Mann, J. I. Diet-heart disease hypothesis is unaffected by results of analysis of recovered data from Minnesota Coronary Experiment. Evid. Based Med. 21, 185 (2016).
de Lorgeril, M. & Salen, P. New insights into the health effects of dietary saturated and omega-6 and omega-3 polyunsaturated fatty acids. BMC Med. 10, 50 (2012).
Simopoulos, A. P. An increase in the omega-6/omega-3 fatty acid ratio increases the risk for obesity. Nutrients 8, 128 (2016).
Harris, W. S. The omega-6:omega-3 ratio: a critical appraisal and possible successor. Prostaglandins Leukot. Essent. Fatty Acids 132, 34–40 (2018).
Kronmal, R. A. Spurious correlation and the fallacy of the ratio standard revisited. J. R. Stat. Soc. A 156, 379–392 (1993).
United Nations Food and Agricultural Organization. Fats and fatty acids in human nutrition: report of an expert consultation (WHO, 2008).
Sifferlin, A. The 10 best and worst oils for your health. Time http://time.com/5342337/best-worst-cooking-oils-for-your-health/ (2018).
O’Connor, A. A decades-old study, rediscovered, challenges advice on saturated fat. Well https://well.blogs.nytimes.com/2016/04/13/a-decades-old-study-rediscovered-challenges-advice-on-saturated-fat/ (2016).
PaleoLeap. What’s wrong with industrial oils? PaleoLeap https://paleoleap.com/whats-wrong-industrial-oils/ (2019).
Konie, R. The ugly truth about vegetable oils (and why they should be avoided). Thank Your Body https://www.thankyourbody.com/vegetable-oils/ (2019).
Kreps, F., Vrbikova, L. & Schmidt, S. Influence of industrial physical refining on tocopherol, chlorophyll and beta-carotene content in sunflower and rapeseed oil. Eur. J. Lipid Sci. Technol. 116, 1572–1582 (2014).
Verleyen, T. et al. Influence of the vegetable oil refining process on free and esterified sterols. J. Am. Oil Chem. Soc. 79, 947–953 (2002).
Kraljic, K. et al. Changes in 4-vinylsyringol and other phenolics during rapeseed oil refining. Food Chem. 187, 236–242 (2015).
AbuMweis, S., Jew, S., Tayyem, R. & Agraib, L. Eicosapentaenoic acid and docosahexaenoic acid containing supplements modulate risk factors for cardiovascular disease: a meta-analysis of randomised placebo-control human clinical trials. J. Hum. Nutr. Diet. 31, 67–84 (2018).
Macartney, M. J., Hingley, L., Brown, M. A., Peoples, G. E. & McLennan, P. L. Intrinsic heart rate recovery after dynamic exercise is improved with an increased omega-3 index in healthy males. Br. J. Nutr. 112, 1984–1992 (2014).
Peoples, G. E., McLennan, P. L., Howe, P. R. & Groeller, H. Fish oil reduces heart rate and oxygen consumption during exercise. J. Cardiovasc. Pharmacol. 52, 540–547 (2008).
Wu, J. H., Cahill, L. E. & Mozaffarian, D. Effect of fish oil on circulating adiponectin: a systematic review and meta-analysis of randomized controlled trials. J. Clin. Endocrinol. Metab. 98, 2451–2459 (2013).
Xin, W., Wei, W. & Li, X. Y. Short-term effects of fish-oil supplementation on heart rate variability in humans: a meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 97, 926–935 (2013).
Akinkuolie, A. O., Ngwa, J. S., Meigs, J. B. & Djousse, L. Omega-3 polyunsaturated fatty acid and insulin sensitivity: a meta-analysis of randomized controlled trials. Clin. Nutr. 30, 702–707 (2011).
Abbott, K. A., Burrows, T. L., Thota, R. N., Acharya, S. & Garg, M. L. Do omega-3 PUFAs affect insulin resistance in a sex-specific manner? A systematic review and meta-analysis of randomized controlled trials. Am. J. Clin. Nutr. 104, 1470–1484 (2016).
Pan, A., Yu, D., Demark-Wahnefried, W., Franco, O. H. & Lin, X. Meta-analysis of the effects of flaxseed interventions on blood lipids. Am. J. Clin. Nutr. 90, 288–297 (2009).
Neale, E. P., Tapsell, L. C., Guan, V. & Batterham, M. J. The effect of nut consumption on markers of inflammation and endothelial function: a systematic review and meta-analysis of randomised controlled trials. BMJ Open 7, e016863 (2017).
Mozaffarian, D. & Rimm, E. B. Fish intake, contaminants, and human health: evaluating the risks and the benefits. JAMA 296, 1885–1899 (2006).
Zheng, J. et al. Fish consumption and CHD mortality: an updated meta-analysis of seventeen cohort studies. Public Health Nutr. 15, 725–737 (2012).
Chowdhury, R. et al. Association between fish consumption, long chain omega 3 fatty acids, and risk of cerebrovascular disease: systematic review and meta-analysis. BMJ 345, e6698 (2012).
Larsson, S. C., Orsini, N. & Wolk, A. Long-chain omega-3 polyunsaturated fatty acids and risk of stroke: a meta-analysis. Eur. J. Epidemiol. 27, 895–901 (2012).
Wu, J. H. et al. Omega-3 fatty acids and incident type 2 diabetes: a systematic review and meta-analysis. Br. J. Nutr. 107 (Suppl. 2), 214–227 (2012).
Pan, A. et al. α-Linolenic acid and risk of cardiovascular disease: a systematic review and meta-analysis. Am. J. Clin. Nutr. 96, 1262–1273 (2012).
Del Gobbo, L. C. et al. ω-3 polyunsaturated fatty acid biomarkers and coronary heart disease: pooling project of 19 cohort studies. JAMA Intern. Med. 176, 1155–1166 (2016).
Forouhi, N. G. et al. Association of plasma phospholipid n-3 and n-6 polyunsaturated fatty acids with type 2 diabetes: the EPIC-InterAct Case-Cohort Study. PLOS Med. 13, e1002094 (2016).
Wu, J. H. & Mozaffarian, D. ω-3 fatty acids, atherosclerosis progression and cardiovascular outcomes in recent trials: new pieces in a complex puzzle. Heart 100, 530–533 (2014).
Manson, J. E. et al. Marine n-3 fatty acids and prevention of cardiovascular disease and cancer. N. Engl. J. Med. 380, 23–32 (2018).
Kromhout, D., Giltay, E. J. & Geleijnse, J. M. n-3 fatty acids and cardiovascular events after myocardial infarction. N. Engl. J. Med. 363, 2015–2026 (2010).
Abdelhamid, A. S. et al. Omega-3 fatty acids for the primary and secondary prevention of cardiovascular disease. Cochrane Database Syst. Rev. 7, CD003177 (2018).
Aung, T. et al. Associations of omega-3 fatty acid supplement use with cardiovascular disease risks: meta-analysis of 10 trials involving 77917 individuals. JAMA Cardiol. 3, 225–234 (2018).
Rizos, E. C., Ntzani, E. E., Bika, E., Kostapanos, M. S. & Elisaf, M. S. Association between omega-3 fatty acid supplementation and risk of major cardiovascular disease events: a systematic review and meta-analysis. JAMA 308, 1024–1033 (2012).
Siscovick, D. S. et al. Omega-3 polyunsaturated fatty acid (fish oil) supplementation and the prevention of clinical cardiovascular disease: a science advisory from the American Heart Association. Circulation 135, e867–e884 (2017).
Bowen, K. J., Harris, W. S. & Kris-Etherton, P. M. Omega-3 fatty acids and cardiovascular disease: are there benefits? Curr. Treat. Opt. Cardiovasc. Med. 18, 69 (2016).
Mozaffarian, D. et al. Circulating long-chain omega-3 fatty acids and incidence of congestive heart failure in older adults: the cardiovascular health study: a cohort study. Ann. Intern. Med. 155, 160–170 (2011).
Saber, H. et al. Omega-3 fatty acids and incident ischemic stroke and its atherothrombotic and cardioembolic subtypes in 3 US cohorts. Stroke 48, 2678–2685 (2017).
Virtanen, J. K., Mursu, J., Voutilainen, S. & Tuomainen, T. P. Serum long-chain n-3 polyunsaturated fatty acids and risk of hospital diagnosis of atrial fibrillation in men. Circulation 120, 2315–2321 (2009).
Wu, J. H. et al. Association of plasma phospholipid long-chain omega-3 fatty acids with incident atrial fibrillation in older adults: the cardiovascular health study. Circulation 125, 1084–1093 (2012).
Djousse, L., Akinkuolie, A. O., Wu, J. H., Ding, E. L. & Gaziano, J. M. Fish consumption, omega-3 fatty acids and risk of heart failure: a meta-analysis. Clin. Nutr. 31, 846–853 (2012).
Mozaffarian, D. & Wu, J. H. (n-3) fatty acids and cardiovascular health: are effects of EPA and DHA shared or complementary? J. Nutr. 142, 614s–625s (2012).
Mensink, R. P., Zock, P. L., Kester, A. D. & Katan, M. B. Effects of dietary fatty acids and carbohydrates on the ratio of serum total to HDL cholesterol and on serum lipids and apolipoproteins: a meta-analysis of 60 controlled trials. Am. J. Clin. Nutr. 77, 1146–1155 (2003).
Lewington, S. et al. Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths. Lancet 370, 1829–1839 (2007).
Acknowledgements
J.H.Y.W. received support from a Scientia Fellowship from the University of New South Wales, Australia. R.M. and D.M. received funding from the US National Institutes of Health (NIH) and the US National Heart, Lung and Blood Institute (NHLBI) (R01HL130735 and R01HL115189).
Reviewer information
Nature Reviews Cardiology thanks G. Riccardi and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Author information
Authors and Affiliations
Contributions
J.H.Y.W. and D.M. researched data for the article, and J.H.Y.W. wrote the manuscript. All authors provided substantial contribution to the discussion of content and reviewed and/or edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
J.H.Y.W. and R.M. received research support from Unilever for projects on fatty acid biomarkers not related to the present article. D.M. received research funding from the US National Institutes of Health (NIH) and the Gates Foundation; received personal fees from Acasti Pharma, Amarin, America’s Test Kitchen, Bunge, DSM, GOED, Indigo Agriculture, Nutrition Impact and Pollock Communications; is on the scientific advisory board of DayTwo, Elysium Health and Omada Health; and received chapter royalties from UpToDate; none of these is related to the present article.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, J.H., Micha, R. & Mozaffarian, D. Dietary fats and cardiometabolic disease: mechanisms and effects on risk factors and outcomes. Nat Rev Cardiol 16, 581–601 (2019). https://doi.org/10.1038/s41569-019-0206-1
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41569-019-0206-1
This article is cited by
-
Avocado intake and cardiometabolic risk factors in a representative survey of Australians: a secondary analysis of the 2011–2012 national nutrition and physical activity survey
Nutrition Journal (2024)
-
Artificial neural networks optimize the establishment of a Brazilian germplasm core collection of winter squash (Cucurbita moschata D.)
Scientific Reports (2024)
-
Integrative analysis of hepatic transcriptional profiles reveals genetic regulation of atherosclerosis in hyperlipidemic Diversity Outbred-F1 mice
Scientific Reports (2023)
-
Trans-fatty acid blood levels of industrial but not natural origin are associated with cardiovascular risk factors in patients with HFpEF: a secondary analysis of the Aldo-DHF trial
Clinical Research in Cardiology (2023)
-
Effect of reduced-calcium and high-calcium cheddar cheese consumption on the excretion of faecal fat: a 2-week cross-over dietary intervention study
European Journal of Nutrition (2023)