Abstract
After over a billion of vaccinations with messenger RNA-lipid nanoparticle (mRNA-LNP) based SARS-CoV-2 vaccines, anaphylaxis and other manifestations of hypersensitivity can be considered as very rare adverse events. Although current recommendations include avoiding a second dose in those with first-dose anaphylaxis, the underlying mechanisms are unknown; therefore, the risk of a future reaction cannot be predicted. Given how important new mRNA constructs will be to address the emergence of new viral variants and viruses, there is an urgent need for clinical approaches that would allow a safe repeated immunization of high-risk individuals and for reliable predictive tools of adverse reactions to mRNA vaccines. In many aspects, anaphylaxis symptoms experienced by the affected vaccine recipients resemble those of infusion reactions to nanomedicines. Here we share lessons learned over a decade of nanomedicine research and discuss the current knowledge about several factors that individually or collectively contribute to infusion reactions to nanomedicines. We aim to use this knowledge to inform the SARS-CoV-2 lipid-nanoparticle-based mRNA vaccine field.
Similar content being viewed by others
Main
Respiratory infections caused by viral pathogens (for example, influenza, respiratory syncytial virus and severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2)) cause substantial mortality and morbidity worldwide.
Despite being among the most effective instruments against infectious diseases, vaccines can cause side effects. Anaphylaxis is a severe adverse reaction that requires hospitalization and, when untreated, can be fatal. A detailed analysis of anaphylaxis occurrence after traditional vaccination in the United States revealed that among >25 million people vaccinated between 2009 and 2011, 33 (1.31 cases per 1,000,000 vaccinations) experienced anaphylaxis1, which in some cases was attributed to vaccine excipients such as gelatine and thimerosal2,3,4,5.
The US Centers for Disease Control and Prevention (CDC) established the Vaccine Adverse Event Reporting System (VAERS), which collects reports from healthcare workers and the public, and the CDC Wide-ranging Online Data for Epidemiologic Research (WONDER) database, which disseminates public health data and information6. According to these data systems, some people developed hypersensitivity reactions (HSRs) and anaphylaxis after immunization with SARS-CoV-2 messenger RNA (mRNA) vaccines7. In the United States, 99 out of 1,725 reports entered into VAERS by 1 March 2021 mention anaphylaxis6; this is a higher frequency than that reported for all seasonal flu vaccines during the past decade (447 out of 346,575 VAERS entries)1,3. According to the Israel Ministry of Health report of March 2021, 4 of 4,755,585 recipients of the first dose and 3 of 3,408,825 recipients of the second dose of the Pfizer-BioNTech vaccine developed anaphylaxis8. Delayed immune-mediated reactions were also reported9. According to the Israel Ministry of Health report of 8 August 2021, among 11.6 million individuals vaccinated with Pfizer-BioNTech formulation, 421,000 safely received a third dose8. Earlier reports of efficacy and safety are also available from other countries10,11,12,13. Although public adverse-event-collecting databases such as VAERS are passive in that they rely on individuals to enter the data and, consequently, may underestimate the actual incidence of adverse effects, they allow the identification of toxicities and promote the investigation of underlying causes. Given over a billion of vaccinated individuals14, the rate of anaphylaxis in mRNA SARS-CoV-2 vaccination is very low. However, recent reports suggest that the overall incidence of HSRs to SARS-CoV-2 vaccines is higher than that of traditional vaccines15,16, which makes a thorough analysis to understand the underlying cause(s) important.
Number of immunizations with SARS-CoV-2 vaccines in different countries is increasing; current data are available in ref. 14. The rate of anaphylaxis at the time of proof-reading this paper is between 2.5-4.7 per million. However, it should be noted that information on the prevalence of vaccine-related anaphylaxis can vary depending on the inclusion criteria, method of evaluation, passive surveillance and type of data analysis. For this reason, the above rate substantially varies in the literature. Some symptoms experienced by SARS-CoV-2 vaccine recipients in the United States and reported to VAERS by 8 January 2021, resemble the symptoms described in response to the systemically administered nanomedicine Doxil. The per cent of individuals on this graph refers to the proportion of individuals with this adverse effect among 100 reports entered in VAERS for the Pfizer-BioNTech and Moderna SARS-CoV-2 vaccines by 8 January 2021, or registered for Doxil by the FDA adverse event reporting system134 between 1995 (FDA approval of this formulation) and 2021.
Vaccine manufacturers and regulatory authorities have issued warnings calling for special attention to high-risk individuals, mandated 30-minute post-vaccination monitoring to provide pharmacological intervention in case anaphylaxis occurs and recommended excluding individuals with a known history of allergy to vaccine components from immunization. Examples of the high-risk category individuals disclosed to the public on the CDC website include cosmetic dermal filler recipients and persons with a history of anaphylaxis, autoimmune diseases, Guillain–Barré syndrome or Bell’s palsy17.
A close examination of adverse events recorded for these SARS-CoV-2 mRNA intramuscular (i.m.) vaccines revealed that many reactions resemble infusion reactions, commonly experienced in response to intravenously (i.v.) administered established nanomedicines18. Some reactions to SARS-CoV-2 mRNA vaccines (for example, rash, dyspnoea, chills, chest pain, tachycardia, hypotension, hypertension and anaphylaxis) were also reported for the systemically administered nanomedicine Doxil; however, the frequency of these reactions to vaccines was much lower than that to Doxil (Fig. 1). The higher rate of infusion reactions to nanomedicines could be explained by their route of administration (that is, i.v. versus i.m. in vaccines), higher dose per kilogram of body weight (that is, mg kg–1 versus μg kg–1 in vaccines) and different distribution over the body. Nevertheless, these notions raise several questions about a potential contribution to HSRs by the lipid nanoparticles (LNPs) used as carriers in SARS-CoV-2 mRNA vaccines and suggest that lessons learned from managing infusion reactions to nanomedicines may help in understanding and overcoming HSRs to otherwise highly effective SARS-CoV-2 mRNA vaccines. Unlike infusion reactions to nanomedicines, anxiety was suggested among causes of HSR symptoms in vaccine recipients19. Understanding the mechanisms that underlie HSRs would help the medical community develop means to manage these reactions and prevent major effects and deaths, and so reduce people’s anxiety and fears over these vaccines.
LNP–mRNA vaccines overview
Composition and physicochemical properties
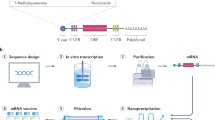
The Pfizer-BioNTech and Moderna products, used for SARS-CoV-2 prevention in the United States, Europe and other parts of the world20,21,22, use LNPs as mRNA delivery vehicles (Table 1). The vaccines’ mRNA molecules differ in nucleoside type and sequence. Pfizer-BioNTech (BNT162b2) mRNA is a modified nucleoside mRNA chain that contains 1-methylpseudouridine instead of uridine. It expresses the SARS-CoV-2 full-length P2 mutant prefusion spike glycoprotein with two proline mutations that fix the S1S2 spike protein in a prefusion conformation. Moderna’s vaccine mRNA is also modified with 1-methylpseudouridine and encodes the spike protein with two proline residues. The LNP carrier is made of an ionizable cationic lipid with apparent pKa values between 6 and 7, cholesterol, 1,2-distearoyl-sn-glycero-3-phosphocholine (DSPC) and a polyethylene glycol (PEG)-conjugated lipid intended to prevent LNP aggregation during storage as an aqueous dispersion. The ionizable cationic lipid serves two purposes: (1) to achieve an efficient encapsulation during the LNP preparation process and (2) after administration to provide a neutral particle surface at physiological pH but a positively charged particle surface once internalized by cells into more acidic intracellular compartments to facilitate intracellular mRNA trafficking. PEG terminal groups and the lipid conjugated to PEG differ between Pfizer-BioNTech and Moderna formulations. The mRNA dose is 30 μg and 100 μg in the Pfizer-BioNTech and Moderna vaccines, respectively. Although these LNP–mRNA vaccines’ structural features are not published, approximately 100 nm spherical structures with an electron-dense core have been described for LNPs with a similar composition; inside those spheres, mRNA, ionizable cationic lipid and water molecules form an inverted hexagonal phase, whereas the external shell contains the PEG–lipid, part of the cholesterol and DSPC23,24,25.
Pharmacology and mechanism of action
LNP–mRNA’s fate in SARS-CoV-2 vaccines is not well understood, and detailed information about LNP–mRNA distribution and mRNA expression after i.m. injection in humans is not available. In mice, the route of administration is an important factor in determining the body sites in which the mRNA is translated, with the magnitude and duration of protein expression varying widely26. After i.m. injection, the produced protein was detectable at the injection site for 10 days and in the liver for 1–4 days26. A study in rhesus macaques on local immune events and protein expression after the i.m. administration of LNP loaded with mRNA-encoding influenza H10-haemagglutinin demonstrated a transient, local inflammation reaction that involved a rapid infiltration of immune cells, which included antigen-presenting cells (APCs), at the injection site and the draining lymph nodes. The injection of control LNP formulations showed that this immune cell influx effect occurs independently of the mRNA cargo. However, a marked activation of the adaptive immune system was observed only in the presence of LNP–mRNA. Monocytes and dendritic cells were the main cell types in which the protein was produced. The co-stimulatory receptors CD80 and CD86 were upregulated on the surface of the infiltrating APCs27. In a cynomolgus monkey model, no direct correlation was found between protein expression, immunogenicity and local tolerability for five LNP formulations with different ionizable cationic biodegradable lipids after i.m. injection. This suggests that inducing local irritation does not directly correlate with immunogenicity. Lipid H, which is identical to SM-102 in Moderna’s vaccine (Table 1), stood out in terms of a high immunogenicity but low local oedema and erythema formation28. A more recent study in cynomolgus macaques investigated the fate of i.m.-injected LNP–mRNA in which the carrier contained a cationic lipid, based on an amino sugar, but no PEG–lipid29. The mRNA in this study was dual-labelled with a radionuclide positron emission tomography–computed tomography marker and a near-infrared probe. Muscle tissue and three draining lymph nodes were monitored for the presence of mRNA. The APCs were the major carriers of mRNA in these locations. In some lymph nodes, mRNA-enriched B cells were found. The authors did not mention mRNA uptake by the liver or spleen29.
No data on what happens after i.m. LNP–mRNA vaccination in humans has been published. One might speculate that, after i.m. injection, the PEG–lipid (ALC-0159 in the Pfizer-BioNTech vaccine and PEG2000-DMG in the Moderna vaccine; Table 1) desorbs from the LNP, as happens with short interfering RNA–LNP after i.v. administration to rodents and non-human primates (NHPs). In the case of i.v. administration, the PEG–lipid component of the LNP carrier rapidly desorbs from the nanoparticles after injection. Adsorption of apolipoprotein E to the surface of the LNP also occurs, and leads to the rapid endocytosis of the in vivo modified LNP by hepatocytes in the liver24. However, as discussed above, after i.m. administration in NHPs, LNP–mRNA complexes are rapidly endocytosed by cells that reside at or enter the site of injection (that is, APCs). The LNP complexes disintegrate in the endosomes, and the mRNA escapes into the cytosol via an endosomal membrane destabilization mediated by the ionizable lipid, from which it travels to the rough endoplasmic reticulum for translation; DSPC and cholesterol are seen as ‘helper lipids’, as they are critical to the formation and maintenance of stable LNP–mRNA complexes30. In humans, mechanistic details of cellular uptake and LNP–mRNA processing by APCs are still hypothetical. Nevertheless, a strong immune response that involves antigen-specific CD4+ TH1 (type 1 T helper) cells, CD8+ cytotoxic T cells, B cells and plasma cells in vaccinated individuals is clearly documented12,31,32.
Collectively, despite variation in the mRNA structure, LNP type and NHP species (rhesus versus cynomolgus), the limited studies available provide important information on the spatiotemporal trafficking of LNP–mRNA and antibody formation, and suggest that local tolerability and protein expression levels do not correlate with immunogenicity27,28,29. The relationships between the initial innate immune responses, spike protein production, resulting antigen presentation and specific antiviral immunogenicity are yet to be better understood. Although the incorporation of pseudouridine into mRNA reduces the Toll-like-receptor-mediated innate immune response against mRNA33, additional studies demonstrated that other types of milder innate immune responses still occur and may reduce the mRNA translation34,35; these and other aspects regarding mRNA vaccines’ pharmacology and mode of action are extensively discussed elsewhere36.
Potential mechanisms that underlie HSR to LNP–mRNA vaccines
Although stimulation of innate and adaptive immune responses is a desirable outcome that underlies a vaccine’s efficacy, it may lead to immune-mediated adverse effects (IMAEs) when overwhelming and left uncontrolled. Anaphylaxis is a life-threatening IMAE that belongs to the type I immediate-type hypersensitivity (ITH) category37. Anaphylaxis symptoms occur within minutes of exposure to the triggering agent (for example, an environmental allergen, Hymenoptera venom, a drug or an excipient). The classical ITH is triggered when an allergen binds to the allergen-specific immunoglobulin E (IgE) on mast cells of individuals who were previously sensitized, with subsequent degranulation of these cells, which leads to the release of preformed and newly synthesized mediators, such as histamine, tryptase, prostaglandins, leukotrienes and interleukins, among others. Mediator binding to tissue and cellular receptors induces local and systemic symptoms that affect the skin and respiratory, gastrointestinal and cardiovascular systems. Typical symptoms include swelling of the face, eyes, tongue and throat, skin eruptions, haemodynamic changes, respiratory failure followed by hypotension with circulatory collapse (that is, shock) and death within minutes to hours, unless medical intervention is applied. Anaphylaxis can occur without IgE, by direct activation of mast cells and/or basophils and through the newly described G-coupled protein receptors, such as the Mas-related G-protein coupled receptor member X2. Anaphylaxis treatment requires early recognition of the symptoms and prompt use of i.m. epinephrine. Death varies depending on the trigger, and there is a 0.3% death rate from anaphylaxis of different origins38. The same symptoms and timeline could also occur due to the activation of the complement system39. This type of reaction is known as pseudoallergy, anaphylactoid reaction or complement activation-related pseudoallergy (CARPA)39. The enzymatic cleavage of complement proteins generates so-called anaphylatoxins (C3a, C4a and C5a) that act as cytokines and activate immune cells to produce secondary inflammation mediators39. Complement activation-generated anaphylatoxins can also activate mast cells, which results in classical anaphylaxis symptoms40. Allergen-specific IgM and IgG are known to activate the complement system; they also trigger type II and type III hypersensitivities, for which development takes minutes to hours and three to eight hours, respectively37. Complement activation also contributes to type III HSR37. Type IV HSR is delayed hypersensitivity mediated by T cells and can develop within 48–72 hours37. Although cytokines are produced by activated immune cells during ITH and other types of HSR and are considered part of the anaphylaxis phenotypes by some researchers41,42, certain institutions separate anaphylaxis from cytokine release syndrome43. Wide discrepancies also exist in HSR definitions between health organizations, countries and fields of training18; the symptoms and underlying cellular and molecular players of HSRs frequently overlap, which complicates diagnosis and management18. Biomarkers recently became available for diagnosis, and provide a mechanistic approach to define the genotypes that underlie the different phenotypes. Significant elevations of tryptase above the baseline are typical for IgE and non-IgE mast-cell-driven reactions, and interleukin-6 (IL-6) elevations are diagnostic of cytokine release syndrome44.
Despite recently described delayed reactions to SARS-CoV-2 vaccines45, which, according to the timeline of occurrence and symptoms, suggest type III and type IV HSR, no mechanistic data or other reports are available. Therefore, here we focus on ITH, most frequently mentioned by the media at the time when vaccination began at the end of 2020 and early 2021 (Box 1), and discuss the mechanisms that underlie these reactions through the current knowledge about infusion reactions to nanomedicines18. We interrogate the potential role of LNP carriers, mRNA, excipients and antigens expressed from mRNA. We also touch on delayed responses as the same components that contribute to ITH, although via different mechanisms, are involved in delayed responses, all of which have been reported in the context of IMAEs to SARS-CoV-2 mRNA vaccines7,10,46,47 (Box 1).
Systemic complement activation
There are three complement activation pathways—classical, mannose and alternative—that antibodies (IgM or some IgG isotypes), mannose-binding lectin and C3b binding trigger, respectively; additionally, autoactivation (via so-called C3 ‘tickover’) can occur39. A prominent frequent consequence of immunization is transient local tissue swelling associated with redness and pain at the injection site. It occurs due to the accumulation of protein-rich inflammatory exudate that contains complement proteins, and it explains the availability of complement proteins at the injection site.
Pre-existing anti-PEG IgG and IgM that bind to the PEG backbone or terminal methoxy group have been found in healthy people48,49. Similarly, naturally occurring anti-cholesterol antibodies capable of reacting with cholesterol components of liposomes have been detected in healthy individuals and people with atherosclerosis50,51. Prior exposure to PEG, PEGylated nanomedicines and LNPs induces PEG-reactive IgM and IgG formation52,53. These pre-existing and induced antibodies trigger the classical complement activation pathway51,52, which, when occurs in response to systemically administered PEGylated nanomedicines, leads to CARPA52,54. Nucleic acids also trigger the classical pathway55. Cationic lipids and LNPs activate the complement system in vitro and in vivo via the alternative pathway56,57,58,59. Anti-PEG antibody levels depend on the rate of PEG–lipid shedding off the LNP, with fast-shedding PEG–lipid being less immunogenic than its slow-shedding counterpart53. The LNP in both the Pfizer-BioNTech and Moderna vaccines contains a lipid conjugated to PEG2000, and local reactions in individuals with PEG-based cosmetic fillers have been reported (Box 1). Therefore, it is plausible that pre-existing anti-PEG antibodies contribute to complement-mediated anaphylactoid reactions to SARS-CoV-2 mRNA vaccines. However, as the lipid parts of the PEG2000-lipid and PEG terminal groups are different (2-((polyethylene glycol)-2000)-N,N-ditetradecylacetamide versus PEG-2000-DMG, and PEG versus methoxy-PEG (mPEG) in the Pfizer-BioNTech and Moderna formulations, respectively), these vaccines’ reactogenicity, if indeed mediated by anti-PEG antibodies, may also differ. PEG’s terminal group is a key contributor to its immunogenicity in that mPEG is more immunogenic than hydroxy-PEG60; therefore, it is critical to clarify PEG’s chemical identity in the Pfizer-BioNTech vaccine (2-((polyethylene glycol)-2000)-N,N-ditetradecylacetamide as stated in the package insert20,61 versus mPEG-N,N-ditetradecylacetamide in the research catalogue62 for ALC-0159). Some viruses (for example, mumps, parainfluenza, and SARS-CoV-2)63, purified spike protein of SARS-CoV-264, and certain excipients (for example, acetic acid)65 trigger the alternative pathway of complement activation. Spike protein, via direct binding to mannose-binding lectin, ficolin-2, and collectin-11, may also trigger the mannose pathway of complement activation66. Moreover, spike protein was detected in vaccinated individuals’ blood as early as day zero after the first dose, peaked at day five, and remained until day 1567. This would explain spike-protein-triggered complement activation in the systemic circulation, along with the delayed anaphylaxis and repeated reactions reported in affected individuals. Although complement activation by therapeutic nucleic acids was reported in vitro and in vivo, NHPs overpredicted complement-mediated toxicities in humans68, and no reliable data are available on nucleoside-modified mRNAs’ ability to activate the complement system. Although the role of complement-related pattern-recognition molecules, pentraxins (pentraxin 3 and C-reactive protein), in response to viral infections, including that to SARS-CoV-2, has been established69, it remains unknown for infusion reactions to nanomedicines and HSRs to LNP–mRNA-based vaccines.
Therefore, at least three components delivered by SARS-CoV-2 mRNA vaccines (PEGylated LNP carrier, mRNA payload and expressed spike protein antigen) can activate the complement system. Activation could occur after i.m. administration in the interstitial space and lymphatics, where complement is also present70, as well as after particle distribution to the systemic circulation (Fig. 2a and Cytokine-mediated responses). It is unknown whether or to what extent the i.m.-injected SARS-CoV-2 vaccines distribute to the systemic circulation. Understanding such distribution is warranted, as the amount of LNP–mRNA injected i.m. to a human is minuscule. A recent murine study of the Pfizer-BioNTech mRNA vaccination demonstrated that accidental administration into the peripheral blood may inadvertently occur during the i.m. injection and is responsible for the systemic inflammation that leads to myopericarditis71. Such unintended i.v. administration could be another mechanism that leads to complement-mediated anaphylaxis. Recent reports about a reaction-free second dose after anaphylaxis to the first dose of SARS-CoV-2 mRNA vaccines72,73 indirectly suggest complement is involved in the first reaction because a similar pattern of reduction in reactogenicity with repeated administration was reported for CARPA, but not for a true allergy to nanomedicines74.
a, Schematic of interaction between LNP–mRNA vaccine components and cells at the site of injection (1), along with a hypothetical mechanism of particle distribution to the systemic circulation (2). b, Cellular and molecular players responsible for the generation of an immune response to the LNP–mRNA vaccine that leads to both the desirable immunogenicity and, in some individuals, the adverse immune effects. c, Millions of people received vaccines, and only a very small proportion developed anaphylaxis. These individuals are currently either excluded from receiving the second dose of mRNA vaccine or the vaccination is done in hospitals under supervision. Studies outlined in this image would help to shed more light on the mechanisms of anaphylaxis and allow the immunization of more individuals.
Intracellular complement
Many human cell types can produce complement proteins, collectively known as intracellular or local complement, which are different from the systemic complement present in the plasma and produced by the liver in that they are located inside the cell and can be cleaved via intracellular proteases. Pro-inflammatory cytokines produced during innate and adaptive responses to an antigen potently trigger intracellular complement activation and upregulation of anaphylatoxin receptors (C3aR and C5aR) on the surface of these cells70. The formed anaphylatoxins are released and bind to their cognate receptors to amplify the APC–T-cell interactions via autocrine and paracrine positive feedback loops70. Activated APC and T cells also produce complement factors B and D70, which enables expansion of the chain reaction via the alternative pathway amplification loop. Although LNPs used in the Pfizer-BioNTech and Moderna vaccines have not been studied, cationic molecules and cationic nanoparticles are known to activate the intracellular complement system in a membrane-damage-related process similar to how cationic lipids enable mRNA escape from the lysosomes into the cytoplasm75. Thus, if the ionizable vaccine lipids indeed induce intracellular complement activation, it may coincide with the cytoplasmic translation of mRNA, just in time to stimulate APC–T-cell interactions. There are no data as to whether the excipients, mRNA or spike protein in vaccines can activate the intracellular complement; however, available knowledge about triggers of the intracellular complement70,75 and the established facts about cytokine induction by SARS-CoV-2 mRNA vaccines12,76 support this mechanism’s plausibility and call for additional investigation. It is conceivable that the process is also important to the immunogenicity of SARS-CoV-2 mRNA vaccines.
Mast-cell activation through IgE and non-IgE mechanisms
Mast cells are myeloid-lineage-derived granulocytes that reside in connective tissue and are staffed with granules containing histamine, heparin, proteases and cytokines. Antigen-specific IgE molecules trigger mast-cell degranulation. PEG-specific IgE cross-reacting with polysorbate 80 has recently been described in two individuals with ITH to PEG-containing medications; moreover, a review of the US Food and Drug Administration (FDA) adverse effects database suggested 53 additional cases of IgE-mediated ITH to PEG77. High titres of anti-PEG IgE were detected in nine patients with a history of anaphylaxis to PEG3350-containing laxative and to PEG8000-containing ultrasound gel; the patients’ blood also contained anti-PEG IgG78. Moreover, a recent computational study identified several spike protein epitopes as allergens79, and a few cases of anaphylaxis were attributed to anti-PEG IgE80,81. Therefore, true anaphylaxis to SARS-CoV-2 mRNA vaccines due to anti-PEG IgE does exist. Antibody screening and skin-prick test appear as reliable, clinically available procedures to identify individuals at high risk; however, their utility to identify SARS-CoV-2 vaccine HSR is incompletely understood. Individuals with clonal and non-clonal mast-cell disorders, which include mastocytosis, asthma, myelodysplastic syndrome and acute myelocytic leukaemia, may present elevated tryptase levels that associate with an increased mast-cell activation. Thus, they could be at higher risk of developing HSR to SARS-CoV-2 mRNA vaccines, although recent vaccinations of two patients with systemic mastocytosis followed by 19 patients with multiple mast-cell-activation syndromes and elevated tryptase did not trigger symptoms of anaphylaxis82,83. A recently described syndrome, hereditary alpha tryptasemia, is associated with duplication and triplication of the tryptase gene TPSAB1 on chromosome 16; elevated tryptase is linked to increased reactions to Hymenoptera venom, and patients with this genetic autosomal dominant trait may be more prone to reactions to vaccines and vaccine excipients84. Tryptase levels are a useful biomarker for diagnosing anaphylaxis85,86.
A recent study demonstrated basophil and mast-cell activation in anaphylactic individuals injected with SARS-CoV-2 mRNA vaccines in the absence of IgEs specific to PEG or other vaccine components87. This points towards a complement-mediated reaction as anaphylatoxins C3a and C5a are known triggers of basophil and mast-cell degranulation88; other mechanisms are also possible.
Cytokine-mediated responses
Cytokines are the biomarkers of immunostimulation, which is an important prerequisite of immunogenicity. Similar to the complement system, innate immune cell activation is desirable to promote vaccine efficacy. However, excessive activation may lead to cytokine storm and cytokine-mediated host-tissue damage. The human population’s genetic diversity leads to wide interindividual variability in cytokine responses89,90. A dose of the same immune adjuvant that results in the optimal cytokine response in one individual may be too strong or too weak for another individual because the innate and adaptive immune responses include multiple cellular and biochemical components and vary between individuals.
Lipids and lipid-based nanoparticles (for example, liposomes, LNPs and micelles) induce chemokines91, whereas therapeutic nucleic acids (for example, mRNA) induce interferon responses92. Cationic moieties in LNPs, along with foreign antigens expressed after vaccine delivery, generate both danger- and pathogen-associated molecular patterns that collectively activate innate immune cell and B-cell pattern-recognition receptors. This triggers inflammatory signalling pathways, major histocompatibility complex class II upregulation and costimulatory molecule expression on APCs, and thereby promotes antigen presentation and immunogenicity. Cationic lipids, common nanocarriers for experimental vaccines, induce a broad spectrum of cytokines, chemokines and danger signals93. Endosomal Toll-like receptors (TLR7 and TLR8) and cytosolic receptors (RIG-I (retinoic acid-inducible gene I), LGP-2 (Laboratory of Genetics and Physiology 2), MDA-5 (melanoma differentiation-associated protein 5) and MAVS (mitochondrial antiviral-signalling protein) initiate an interferon response to the single-stranded RNA. Cationic molecules also trigger inflammasome activation, which specifically contributes to the generation of IL-1 family cytokines, a common feature of promising vaccine adjuvants94,95. Chemokine-mediated neutrophil recruitment is essential for allergic sensitization96, whereas interferons provide antiviral immunity and orchestrate communication between innate and adaptive immunity97,98. Moreover, the SARS-CoV-2 spike protein contains the sequence and structural motif of a superantigen, which is responsible for the hyperinflammatory syndrome that involves direct T-cell stimulation and excessive cytokine production in some individuals99.
Clinical trials of both the Pfizer-BioNTech and Moderna vaccines demonstrated a clear TH1-specific cytokine response, including tumour necrosis factor, IL-1, IL-12 and interferon-gamma21,31, which, besides driving inflammation and innate–adaptive immunity cross-talk, activate the coagulation system and increase the endothelial layer permeability in a time- and dose-dependent manner100,101. Therefore, along with the complement activation described above, these cytokines contribute to both the desired vaccine efficacy and the interindividual variability in IMAEs, such as fever and chills. These cytokines interact with complement and coagulation systems via a bidirectional loop, promoting particle distribution to the systemic circulation, which contributes to elevated inflammation. This warrants a more detailed investigation of these pathways in the context of SARS-CoV-2 vaccines.
Platelets, coagulation and bradykinin systems
Platelets contribute to CARPA and HSR by releasing biologically active molecules (for example, ATP, thromboxane and chemokines) and lipid inflammatory molecules (for example, platelet-activating factor (PAF))40. Nanoparticles that contain cationic moieties activate platelets91,102. Both LNP–mRNA and spike protein also activate platelets103,104. PAF was recently proposed as a new biomarker of anaphylaxis41. Despite its short half-life, PAF has many potent biological effects on almost all tissues and organs; it is central in inflammation, triggers degranulation of perivascular mast cells, which leads to inflammatory responses and tissue injury, and induces the release of thromboxane and serotonins. Rupatadine and other anti-PAF drugs, alone or together with quercetin and luteolin, effectively manage PAF-mediated toxicities in SARS-CoV-2-infected individuals43,44,45 and could be helpful in controlling anaphylaxis to SARS-CoV-2 vaccines.
Bradykinin production is triggered by an increase in heparin and the coagulation-factor-XII-mediated pathway, which cytokines, activated mast cells, complement and platelets trigger. Bradykinin activation leads to the increased vascular permeability responsible for hypotension in anaphylactic individuals105 and therefore could contribute to particle distribution to the systemic circulation.
Oxidative stress
Oxidative stress, linked to HSR for some drugs (for example, sulfanilamides)106 is a common cause of nanoparticle-mediated toxicities107. The induction of a chemokine response by common lipid-based excipients (for example, Cremophor EL) was attributed to oxidative stress108 and is shared by lipid-based nanoparticles, which include LNPs91,109. Oxidative stress inhibits the negative regulation of complement, and so enhances complement-mediated toxicities110.
Common variable immunodeficiency
Common variable immunodeficiency (CVID) is a disorder characterized by excessive activity of the complement system intended to compensate for B cells’ deficient immunoglobulin production111. Persons with CVID, therefore, may be prone to complement-mediated toxicities triggered by LNP–mRNA vaccines, and reviewing the CVID history may help identify people with a high risk of HSR to SARS-CoV-2 mRNA vaccines.
Variability in human leukocyte antigens
Variability in the human leukocyte antigen (HLA) type is known to make some people more prone to developing HSR to certain types of drug products112,113,114,115,116. For example, individuals with HLA-B*57:01, HLA-B*15:02/A*31:01 and HLA-B*58:01 are at higher risk of T-cell-mediated reactions to abacavir, carbamazepine and allopurinol, respectively117. Anaphylaxis to PEG-asparaginase has been associated with HLA-DRB1*07:01118. Individuals with HLA-B*46:01 and HLA-B*15:03 have the lowest and the highest T-cell-mediated responses to SARS-CoV-2, respectively119. Similar variability in an individual’s reactivity to the spike protein antigen encoded by the LNP–mRNA vaccines could exist and contribute to the development of HSRs to SARS-CoV-2 mRNA vaccines. A recent report linked HLA-A*03:01 and HLA-DPB1*11:01 with a decreased and HLA-B*08:01, HLA-C*07:01, HLA-DQA1*05:01 and HLA-DRB1*03:01 with an increased likelihood of reactions to SARS-CoV-2 mRNA vaccines120.
Safety roadmap
In summary, all the components of LNP–mRNA vaccines (carrier, mRNA, excipients and expressed antigen) have various immunostimulatory effects on a broad spectrum of effector and target cells (myocytes, APCs, T and B lymphocytes, platelets and natural killer cells) and biochemical pathways (complement and coagulation) collectively required for vaccine efficacy (Fig. 2b). The same components, however, also contribute to HSR and other IMAEs due to the wide interindividual variability in both the quantity (for example, levels of cytokines, complement split products, tryptase and induced and pre-existing antibodies) and quality (for example, spectrum of inflammatory mediators) of immune responses.
Understanding the mechanisms behind HSR to SARS-CoV-2 mRNA vaccines and exchanging knowledge between the nanomedicine and vaccine fields, therefore, are beneficial not only for SARS-CoV-2 vaccines, but also for all mRNA-based vaccines and therapeutics for which nanoparticles are used as delivery vehicles. More basic research is needed to understand the Pfizer-BioNTech and Moderna vaccines’ mechanisms of action and pharmacokinetics after i.m. injection. Clinical studies to evaluate plasma levels of anti-PEG and anti-cholesterol IgG and IgM in vaccine recipients, along with in vitro exposure of the plasma samples to SARS-CoV-2 mRNA vaccines with a subsequent analysis for the presence of complement split products, would help verify both the involvement of the complement system and the contribution of the pre-existing PEG- and/or cholesterol-specific antibodies. Similar analysis of plasma IgE specific to one or more vaccine components, along with basophil activation, is also needed. Clinical studies to assess the levels of complement split products (anaphylatoxins), cytokines, PAF and tryptase in the blood of people after SARS-CoV-2 vaccination, with subsequent correlation analysis to determine the link (or lack thereof) between complement activation, tryptase and cytokine levels, and HSR would offer further insight (Fig. 2c). The skin-prick test’s applicability to identify individuals prone to developing HSR to SARS-CoV-2 vaccines requires verification. A clinical study to assess the safety of Pfizer-BioNTech and Moderna vaccine administrations to individuals with allergies recently began121. Supplementing it with basic research and clinical investigations that focus on the mechanisms underlying these reactions would further advance knowledge in this area.
The available information suggests that excluding anxiety-mediated responses122, determining whether individuals have conditions known for their higher complement activity (for example, CVID) or hypersensitivity (for example, certain types of HLA and mastocytosis) and reviewing allergy history would further help to identify persons at high risk of HSR, and to develop strategies for safely vaccinating them. In the clinic, anaphylaxis is countered with antihistamines and adrenaline injections, such as the Mylan NV EpiPen. Premedicating patients with steroids, antihistamines and antipyretics similar to those used prior to nanomedicine infusion18 may also prove helpful. However, the applicability of these treatments to vaccines requires investigation to ensure that they do not affect vaccine efficacy; once verified as not interfering, they may allow vaccination of a broader population. A specific HSR condition may call for a specific treatment to prevent a chronic immune reaction; in such cases, and depending on the underlying mechanisms, additional tools, such as PAF and complement inhibitors, may become helpful. Moreover, a better understanding of spike protein immunogenicity and cross-reactivity with the host’s normal tissues, as recently described by two independent studies123,124, will help address the problem by improving the overall immunological properties of the antigen used in mRNA and other SARS-CoV-2 vaccines. Basic research studies are underway to investigate safer PEG alternatives and the chemical modification of mRNA to reduce their undesirable immunoreactivity125,126. Collectively, these strategies would help to safely vaccinate individuals with known HSR to vaccine components. Recent reports about the safe delivery of a second dose to individuals who experienced anaphylaxis to the first dose are encouraging72,73.
Note added in proof: Since this paper was accepted, a couple of studies were published that showed that the LNPs used in the mRNA vaccines cause a strong inflammatory response in mouse models127 and that pigs injected with the Pfizer/BioNtech vaccine undergo hemodynamic changes reminiscent of those caused by the infusion reaction to nanomedicines128.
References
Bardenheier, B. H., Duderstadt, S. K., Engler, R. J. & McNeil, M. M. Adverse events following pandemic influenza A (H1N1) 2009 monovalent and seasonal influenza vaccinations during the 2009–2010 season in the active component US military and civilians aged 17–44 years reported to the Vaccine Adverse Event Reporting System. Vaccine 34, 4406–4414 (2016).
Halsey, N. A. et al. Algorithm to assess causality after individual adverse events following immunizations. Vaccine 30, 5791–5798 (2012).
Halsey, N. A. et al. Immediate hypersensitivity reactions following monovalent 2009 pandemic influenza A (H1N1) vaccines: reports to VAERS. Vaccine 31, 6107–6112 (2013).
Johann-Liang, R., Josephs, S. & Dreskin, S. C. Analysis of anaphylaxis cases after vaccination: 10-year review from the National Vaccine Injury Compensation Program. Ann. Allergy Asthma Immunol. 106, 440–443 (2011).
Zheng, W. & Dreskin, S. C. Thimerosal in influenza vaccine: an immediate hypersensitivity reaction. Ann. Allergy Asthma Immunol. 99, 574–575 (2007).
Vaccine Adverse Event Reporting System (CDC, accessed 31 December 2021); https://vaers.hhs.gov/
Banerji, A. et al. mRNA vaccines to prevent COVID-19 disease and reported allergic reactions: current evidence and suggested approach. J. Allergy Clin. Immunol. Pract. 9, 1423–1437 (2021).
Summary of the Meetings of the Monitoring Committee on the Vaccination Campaign (Israel Ministry of Health, accessed 8 August 2021); https://govextra.gov.il/ministry-of-health/covid19-vaccine/covid-19-vaccine-efficacy-safety-follow-up-committee/
McMahon, D. E. et al. Cutaneous reactions reported after Moderna and Pfizer COVID-19 vaccination: a registry-based study of 414 cases. J. Am. Acad. Dermatol. 85, 46–55 (2021).
Castells, M. C. & Phillips, E. J. Maintaining safety with SARS-CoV-2 vaccines. N. Engl. J. Med. 384, 643–649 (2021).
Dagan, N. et al. BNT162b2 mRNA Covid-19 vaccine in a nationwide mass vaccination setting. N. Engl. J. Med. 384, 1412–1423 (2021).
Polack, F. P. et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N. Engl. J. Med. 383, 2603–2615 (2020).
Baden, L. R. et al. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N. Engl. J. Med. 384, 403–416 (2021).
Coronavirus (COVID-19) Vaccinations (Our World in Data, accessed 29 January 2022); https://ourworldindata.org/covid-vaccinations
Liotti, L. et al. COVID-19 vaccines in children with cow’s milk and food allergies. Nutrients 13, 2637 (2021).
Seneff, S. & Nigh, G. Worse than the disease? Reviewing some possible unintended consequences of the mRNA vaccines against COVID-19. Int. J. Vaccine Theory Pract. Res. 2, 402–443 (2021).
Interim Clinical Considerations for Use of COVID-19 Vaccines Currently Approved or Authorized in the United States (CDC, accessed 10 February 2021); https://www.cdc.gov/vaccines/covid-19/info-by-product/clinical-considerations.html
Szebeni, J., Simberg, D., González-Fernández, Á., Barenholz, Y. & Dobrovolskaia, M. A. Roadmap and strategy for overcoming infusion reactions to nanomedicines. Nat. Nanotechnol. 13, 1100–1108 (2018).
Gold, M. S. et al. Immunization stress-related response—redefining immunization anxiety-related reaction as an adverse event following immunization. Vaccine 38, 3015–3020 (2020).
Pfizer-BioNTech COVID-19 Vaccine Emergency Use Authorization Review Memorandum (USFDA, 2020); https://www.fda.gov/media/144416/download
FDA Briefing Document Moderna COVID-19 Vaccine (USFDA, 2020); https://www.fda.gov/media/144434/download
Ellis R. Pfizer: vaccine shown 100% effective in kids 12–15 WebMD (31 March 2021); https://www.webmd.com/vaccines/covid-19-vaccine/news/20210331/pfizer-vaccine-effectiveness-kids-twelve-to-fifteen
Yanez Arteta, M. et al. Successful reprogramming of cellular protein production through mRNA delivered by functionalized lipid nanoparticles. Proc. Natl Acad. Sci. USA 115, E3351–E3360 (2018).
Mui, B. L. et al. Influence of polyethylene glycol lipid desorption rates on pharmacokinetics and pharmacodynamics of siRNA lipid nanoparticles. Mol. Ther. Nucleic Acids 2, E139 (2013).
Viger-Gravel, J. et al. Structure of lipid nanoparticles containing siRNA or mRNA by dynamic nuclear polarization-enhanced NMR spectroscopy. J. Phys. Chem. B 122, 2073–2081 (2018).
Pardi, N. et al. Expression kinetics of nucleoside-modified mRNA delivered in lipid nanoparticles to mice by various routes. J. Control. Release 217, 345–351 (2015). Establishes the proof of principles for the LNP-mRNA delivery in vivo.
Liang, F. et al. Efficient targeting and activation of antigen-presenting cells in vivo after modified mRNA vaccine administration in rhesus macaques. Mol Ther 25, 2635–2647 (2017).
Hassett, K. J. et al. Optimization of lipid nanoparticles for intramuscular administration of mRNA vaccines. Mol. Ther. Nucleic Acids 15, 1–11 (2019).
Lindsay, K. E. et al. Visualization of early events in mRNA vaccine delivery in non-human primates via PET-CT and near-infrared imaging. Nat. Biomed. Eng. 3, 371–380 (2019). Provides insights into the fate of mRNA vaccine after the immunization.
Sabnis, S. et al. A novel amino lipid series for mRNA delivery: improved endosomal escape and sustained pharmacology and safety in non-human primates. Mol. Ther. 26, 1509–1519 (2018).
Sahin, U. et al. COVID-19 vaccine BNT162b1 elicits human antibody and TH1 T cell responses. Nature 586, 594–599 (2020). Provides the proof of efficacy of Pfizer/Biontech vaccine in humans.
Anderson, E. J. et al. Safety and Immunogenicity of SARS-CoV-2 mRNA-1273 vaccine in older adults. N. Engl. J. Med. 383, 2427–2438 (2020). Reports the results of clinical trials accessing toxicity and efficacy of COVID-19 632 vaccine in humans.
Karikó, K. et al. Incorporation of pseudouridine into mRNA yields superior nonimmunogenic vector with increased translational capacity and biological stability. Mol. Ther. 16, 1833–1840 (2008).
Lokugamage, M. P. et al. Mild innate immune activation overrides efficient nanoparticle-mediated RNA delivery. Adv. Mater. 32, e1904905 (2020).
Pollard, C. et al. Type I IFN counteracts the induction of antigen-specific immune responses by lipid-based delivery of mRNA vaccines. Mol. Ther. 21, 251–259 (2013).
Pardi, N., Hogan, M. J., Porter, F. W. & Weissman, D. mRNA vaccines—a new era in vaccinology. Nat. Rev. Drug Discov. 17, 261–279 (2018).
Coombs R. R. A. & Gell P. G. H. in Clinical Aspects of Immunology 2nd edn (eds Gell P. G. H. & Coombs R. R. A.) 575–596 (Blackwell Scientific, 1968).
Simons, F. E. et al. 2012 Update: World Allergy Organization Guidelines for the assessment and management of anaphylaxis. Curr. Opin. Allergy Clin. Immunol. 12, 389–399 (2012).
Szebeni, J. Complement activation-related pseudoallergy: A stress reaction in blood triggered by nanomedicines and biologicals. Mol. Immunol. 61, 163–173 (2014). Provides a comprehensive literature review of complement-mediated infusion reactions to nanomedicines.
del Balzo, U., Polley, M. J. & Levi, R. Cardiac anaphylaxis. Complement activation as an amplification system. Circ. Res. 65, 847–857 (1989).
Castells, M. Diagnosis and management of anaphylaxis in precision medicine. J. Allergy Clin. Immunol. 140, 321–333 (2017).
Sloane, D. et al. Safety, costs, and efficacy of rapid drug desensitizations to chemotherapy and monoclonal antibodies. J. Allergy Clin. Immunol. Pract. 4, 497–504 (2016).
Common Terminology Criteria for Adverse Events (CTCAE) (US Department of Health and Social Services, 2017); https://ctep.cancer.gov/protocoldevelopment/electronic_applications/ctc.htm
Jacubovic, B. D., Sanchez-Sanchez, S., Hamadi, S., Lynch, D. & Castells, M. Interleukin-6: A novel biomarker for monoclonal antibody and chemotherapy-associated hypersensitivity confirms a cytokine release syndrome phenotype-endotype association. Allergy 76, 1571–1573 (2021).
Blumenthal, K. G. et al. Delayed large local reactions to mRNA-1273 vaccine against SARS-CoV-2. N. Engl. J. Med. 384, 1273–1277 (2021).
Garvey, L. H. & Nasser, S. Anaphylaxis to the first COVID-19 vaccine: is polyethylene glycol (PEG) the culprit? Br. J. Anaesth. 126, e106–e108 (2021).
Moghimi, S. M. Allergic reactions and anaphylaxis to LNP-based COVID-19 vaccines. Mol. Ther. 29, 898–900 (2021).
Chen, B. M. et al. Measurement of pre-existing IgG and IgM antibodies against polyethylene glycol in healthy individuals. Anal Chem 88, 10661–10666 (2016).
Neun, B. W., Barenholz, Y., Szebini, J. & Dobrovolskaia, J. M. Understanding the role of anti-PEG antibodies in the complement activation by doxil in vitro. Molecules 23, 1700 (2018).
Horváth, A. et al. Anti-cholesterol antibodies (ACHA) in patients with different atherosclerotic vascular diseases and healthy individuals. Characterization of human ACHA. Atherosclerosis 156, 185–192 (2001).
Alving, C. R. Natural antibodies against phospholipids and liposomes in humans. Biochem. Soc. Trans. 12, 342–344 (1984).
Kozma, G. T., Shimizu, T., Ishida, T. & Szebeni, J. Anti-PEG antibodies: properties, formation, testing and role in adverse immune reactions to PEGylated nano-biopharmaceuticals. Adv. Drug Deliv. Rev. 154-155, 163–175 (2020).
Suzuki, T. et al. PEG shedding-rate-dependent blood clearance of PEGylated lipid nanoparticles in mice: faster PEG shedding attenuates anti-PEG IgM production. Int J Pharm 588, 119792 (2020).
Kozma, G. T. et al. Pseudo-anaphylaxis to polyethylene glycol (PEG)-coated liposomes: roles of anti-PEG IgM and complement activation in a porcine model of human infusion reactions. ACS Nano 13, 9315–9324 (2019). Demonstrates the role of PEG-specific antibodies in complement activation related pseudoallergy. Reveals a similarity of hemodynamic changes in pigs to that of infusion reactions-related changes in humans
Jiang, H., Cooper, B., Robey, F. A. & Gewurz, H. DNA binds and activates complement via residues 14–26 of the human C1q A chain. J. Biol. Chem. 267, 25597–25601 (1992).
Pham, C. T. et al. Variable antibody-dependent activation of complement by functionalized phospholipid nanoparticle surfaces. J. Biol. Chem. 286, 123–130 (2011).
Sedic, M. et al. Safety evaluation of lipid nanoparticle-formulated modified mRNA in the Sprague-Dawley rat and cynomolgus monkey. Vet. Pathol. 55, 341–354 (2018).
Chonn, A., Cullis, P. R. & Devine, D. V. The role of surface charge in the activation of the classical and alternative pathways of complement by liposomes. J. Immunol. 146, 4234–4241 (1991).
Plank, C., Mechtler, K., Szoka, F. C. Jr. & Wagner, E. Activation of the complement system by synthetic DNA complexes: a potential barrier for intravenous gene delivery. Hum. Gene Ther. 7, 1437–1446 (1996).
Sherman, M. R., Williams, L. D., Sobczyk, M. A., Michaels, S. J. & Saifer, M. G. Role of the methoxy group in immune responses to mPEG-protein conjugates. Bioconjug. Chem. 23, 485–499 (2012).
Comirnaty: Tozinameran/COVID-19 mRNA Vaccine (Nucleoside Modified) (European Medicines Agency, accessed 15 April 2021); https://www.ema.europa.eu/en/medicines/human/EPAR/comirnaty
mPEG-N,N-Ditetradecylacetamide (ALC-0159) (BiochemPEG, 2021); https://www.biochempeg.com/product/mPEG-N,N-Ditetradecylacetamide.html
Johnson, J. B., Aguilar, H. C., Lee, B. & Parks, G. D. Interactions of human complement with virus particles containing the Nipah virus glycoproteins. J. Virol. 85, 5940–5948 (2011).
Yu, J. et al. Direct activation of the alternative complement pathway by SARS-CoV-2 spike proteins is blocked by factor D inhibition. Blood 136, 2080–2089 (2020).
Kenawy, H. I., Boral, I., Bevington, A. & Complement-Coagulation Cross-talk: a potential mediator of the physiological activation of complement by low pH. Front. Immunol. 6, 215 (2015).
Ali, Y. M. et al. Lectin pathway mediates complement activation by SARS-CoV-2 proteins. Front. Immunol. 12, 714511 (2021).
Ogata, A. F. et al. Circulating severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) vaccine antigen detected in the plasma of mRNA-1273 vaccine recipients. Clin. Infect. Dis. 2021, ciab465 (2021).
Crooke, S. T. et al. Integrated safety assessment of 2′-O-methoxyethyl chimeric antisense oligonucleotides in nonhuman primates and healthy human volunteers. Mol. Ther. 24, 1771–1782 (2016).
Schirinzi, A. et al. Pentraxin 3: potential prognostic role in SARS-CoV-2 patients admitted to the emergency department. J. Infect. 82, 84–123 (2021).
Kolev, M., Le Friec, G. & Kemper, C. Complement—tapping into new sites and effector systems. Nat Rev Immunol 14, 811–820 (2014).
Li, C. et al. Intravenous injection of COVID-19 mRNA vaccine can induce acute myopericarditis in mouse model. Clin. Infect. Dis. 2021, ciab707 (2021).
Krantz, M. S. et al. Anaphylaxis to the first dose of mRNA SARS-CoV-2 vaccines: don’t give up on the second dose! Allergy 76, 2916–2920 (2021).
Krantz, M. S. et al. Safety evaluation of the second dose of messenger RNA COVID-19 vaccines in patients with immediate reactions to the first dose. JAMA Intern. Med. 181, 1530–1533 (2021).
Szebeni, J. Complement activation-related pseudoallergy: a new class of drug-induced acute immune toxicity. Toxicology 216, 106–121 (2005).
Ilinskaya, A. N. et al. Nanoparticle physicochemical properties determine the activation of intracellular complement. Nanomedicine 17, 266–275 (2019).
Oliver, S. E. et al. The Advisory Committee on Immunization Practices’ interim recommendation for use of Moderna COVID-19 vaccine—United States, December 2020. Morb. Mortal. Wkly Rep. 69, 1653–1656 (2021).
Stone, C. A. Jr. et al. Immediate hypersensitivity to polyethylene glycols and polysorbates: more common than we have recognized. J. Allergy Clin. Immunol. Pract. 7, 1533–1540.e8 (2019).
Zhou, Z. H. et al. Anti-PEG IgE in anaphylaxis associated with polyethylene glycol. J. Allergy Clin. Immunol. Pract. 9, 1731–1733.e3 (2021).
Selvaraj, G., Kaliamurthi, S., Peslherbe, G. H. & Wei, D. Q. Are the allergic reactions of COVID-19 vaccines caused by mRNA constructs or nanocarriers? Immunological insights. Interdiscip. Sci. 13, 344–347 (2021).
Kelso, J. M. IgE-mediated allergy to polyethylene glycol (PEG) as a cause of anaphylaxis to mRNA COVID-19 vaccines. Clin. Exp. Allergy 52, 10–11 (2021).
Sellaturay, P., Nasser, S., Islam, S., Gurugama, P. & Ewan, P. W. Polyethylene glycol (PEG) is a cause of anaphylaxis to the Pfizer/BioNTech mRNA COVID-19 vaccine. Clin. Exp. Allergy 51, 861–863 (2021).
Kaakati, R., Khokhar, D. & Akin, C. Safety of COVID-19 vaccination in patients with mastocytosis and monoclonal mast cell activation syndrome. J. Allergy Clin. Immunol. Pract. 9, 3198–3199 (2021).
Rama, T. A., Moreira, A. & Castells, M. mRNA COVID-19 vaccine is well tolerated in patients with cutaneous and systemic mastocytosis with mast cell activation symptoms and anaphylaxis. J. Allergy Clin. Immunol. 147, 877–878 (2021).
Lyons, J. J. et al. Elevated basal serum tryptase identifies a multisystem disorder associated with increased TPSAB1 copy number. Nat. Genet. 48, 1564–1569 (2016).
Passia, E. & Jandus, P. Using baseline and peak serum tryptase levels to diagnose anaphylaxis: a review. Clin. Rev. Allergy Immunol. 58, 366–376 (2020).
Pflipsen, M. C. & Vega Colon, K. M. Anaphylaxis: recognition and management. Am. Fam. Physician 102, 355–362 (2020).
Warren, C. M. et al. Assessment of allergic and anaphylactic reactions to mRNA COVID-19 vaccines with confirmatory testing in a US regional health system. JAMA Netw. Open 4, e2125524 (2021).
Ali, H. Regulation of human mast cell and basophil function by anaphylatoxins C3a and C5a. Immunol. Lett. 128, 36–45 (2010).
Li, Y. et al. Inter-individual variability and genetic influences on cytokine responses to bacteria and fungi. Nat. Med. 22, 952–960 (2016).
Li, Y. et al. A functional genomics approach to understand variation in cytokine production in humans. Cell 167, 1099–1110.e1014 (2016).
Dobrovolskaia, M. A. Pre-clinical immunotoxicity studies of nanotechnology-formulated drugs: challenges, considerations and strategy. J. Control Release 220, 571–583 (2015).
Van Hoecke, L. et al. The opposing effect of type I IFN on the T cell response by non-modified mRNA-lipoplex vaccines is determined by the route of administration. Mol. Ther. Nucleic Acids 22, 373–381 (2020).
Lei, H. et al. Cationic nanocarriers as potent adjuvants for recombinant S-RBD vaccine of SARS-CoV-2. Signal Transduct. Target. Ther. 5, 291 (2020).
Ivanov, K., Garanina, E., Rizvanov, A. & Khaiboullina, S. Inflammasomes as targets for adjuvants. Pathogens 9, 252 (2020).
Reinke, S., Thakur, A., Gartlan, C., Bezbradica, J. S. & Milicic, A. Inflammasome-mediated immunogenicity of clinical and experimental vaccine adjuvants. Vaccines 8, 554 (2020).
Hosoki, K., Itazawa, T., Boldogh, I. & Sur, S. Neutrophil recruitment by allergens contribute to allergic sensitization and allergic inflammation. Curr. Opin. Allergy Clin. Immunol. 16, 45–50 (2016).
Wittling, M. C., Cahalan, S. R., Levenson, E. A. & Rabin, R. L. Shared and unique features of human interferon-beta and interferon-alpha subtypes. Front. Immunol. 11, 605673 (2020).
Mezouar, S. & Mege, J. L. Changing the paradigm of IFN-γ at the interface between innate and adaptive immunity: macrophage-derived IFN-γ. J. Leukoc. Biol. 108, 419–426 (2020).
Cheng, M. H. et al. Superantigenic character of an insert unique to SARS-CoV-2 spike supported by skewed TCR repertoire in patients with hyperinflammation. Proc. Natl Acad. Sci. USA 117, 25254–25262 (2020).
Royall, J. A. et al. Tumor necrosis factor and interleukin 1 alpha increase vascular endothelial permeability. Am. J. Physiol. 257, L399–L410 (1989).
Burke-Gaffney, A. & Keenan, A. K. Modulation of human endothelial cell permeability by combinations of the cytokines interleukin-1 alpha/beta, tumor necrosis factor-alpha and interferon-gamma. Immunopharmacology 25, 1–9 (1993).
Dobrovolskaia, M. A. et al. Nanoparticle size and surface charge determine effects of PAMAM dendrimers on human platelets in vitro. Mol. Pharm. 9, 382–393 (2012).
Novakowski, S., Jiang, K., Prakash, G. & Kastrup, C. Delivery of mRNA to platelets using lipid nanoparticles. Sci. Rep. 9, 552 (2019).
Zhang, S. et al. SARS-CoV-2 binds platelet ACE2 to enhance thrombosis in COVID-19. J. Hematol. Oncol. 13, 120 (2020).
Jimenez-Rodriguez, T. W., Garcia-Neuer, M., Alenazy, L. A. & Castells, M. Anaphylaxis in the 21st century: phenotypes, endotypes, and biomarkers. J. Asthma Allergy 11, 121–142 (2018).
Elzagallaai, A. A. et al. Role of oxidative stress in hypersensitivity reactions to sulfonamides. J. Clin. Pharmacol. 60, 409–421 (2020).
Mocan, T. et al. Implications of oxidative stress mechanisms in toxicity of nanoparticles (review). Acta Physiol. Hung. 97, 247–255 (2010).
Ilinskaya, A. N., Clogston, J. D., McNeil, S. E. & Dobrovolskaia, M. A. Induction of oxidative stress by Taxol vehicle Cremophor-EL triggers production of interleukin-8 by peripheral blood mononuclear cells through the mechanism not requiring de novo synthesis of mRNA. Nanomedicine 11, 1925–1938 (2015).
Dobrovolskaia, M. A. & McNeil, S. E. Understanding the correlation between in vitro and in vivo immunotoxicity tests for nanomedicines. J. Control Release 172, 456–466 (2013).
Tezel, G. et al. Oxidative stress and the regulation of complement activation in human glaucoma. Invest. Ophthalmol. Vis. Sci. 51, 5071–5082 (2010).
Fevang, B. et al. Common variable immunodeficiency and the complement system; low mannose-binding lectin levels are associated with bronchiectasis. Clin. Exp. Immunol. 142, 576–584 (2005).
Krebs, K. et al. Genome-wide study identifies association between HLA-B(∗)55:01 and self-reported penicillin allergy. Am. J. Hum Genet. 107, 612–621 (2020).
Nakatani, K. et al. Identification of HLA-A*02:06:01 as the primary disease susceptibility HLA allele in cold medicine-related Stevens–Johnson syndrome with severe ocular complications by high-resolution NGS-based HLA typing. Sci. Rep. 9, 16240 (2019).
Profaizer, T., Pole, A., Monds, C., Delgado, J. C. & Lázár-Molnár, E. Clinical utility of next generation sequencing based HLA typing for disease association and pharmacogenetic testing. Hum. Immunol. 81, 354–360 (2020).
Shirayanagi, T. et al. Detection of abacavir-induced structural alterations in human leukocyte antigen-B*57:01 using phage display. Biol. Pharm. Bull. 43, 1007–1015 (2020).
Tangamornsuksan, W. et al. HLA genotypes and cold medicine-induced Stevens–Johnson syndrome/toxic epidermal necrolysis with severe ocular complications: a systematic review and meta-analysis. Sci. Rep. 10, 10589 (2020).
Profaizer, T. & Eckels, D. HLA alleles and drug hypersensitivity reactions. Int. J. Immunogenet. 39, 99–105 (2012).
Fernandez, C. A. et al. HLA-DRB1*07:01 is associated with a higher risk of asparaginase allergies. Blood 124, 1266–1276 (2014).
Nguyen, A. et al. Human leukocyte antigen susceptibility map for severe acute respiratory syndrome coronavirus 2. J. Virol. 94, 13 (2020).
23andMe Releases Data on HLA-genetics of COVID-19 Vaccine Response (Inside Precision Medicine, 2021); https://www.clinicalomics.com/topics/patient-care/therapeutics/vaccines/23andme-releases-data-on-hla-genetics-of-covid-19-vaccine-response/?utm_medium=newsletter&utm_source=Clinical+OMICs+Update&utm_content=01&utm_campaign=Clinical+OMICs+Update_20211109&oly_enc_id=0917D2598689C8T
NIH Begins Study of Allergic Reactions to Moderna, Pfizer-BioNTech COVID-19 Vaccines (NIH News Releases, 2021); https://www.niaid.nih.gov/news-events/nih-begins-study-allergic-reactions-moderna-pfizer-biontech-covid-19-vaccines
Guidance for Health Care Providers: Understanding Severe Allergic Reactions to COVID-19 Vaccines (Toronto Public Health, 2021).
Lyons-Weiler, J. Pathogenic priming likely contributes to serious and critical illness and mortality in COVID-19 via autoimmunity. J. Transl. Autoimmun. 3, 100051 (2020).
Vojdani, A., Vojdani, E. & Kharrazian, D. Reaction of human monoclonal antibodies to SARS-CoV-2 proteins with tissue antigens: implications for autoimmune diseases. Front. Immunol. 11, 617089 (2020).
Thi, T. T. H. et al. The importance of poly(ethylene glycol) alternatives for overcoming PEG immunogenicity in drug delivery and bioconjugation. Polymers 12, 252 (2020).
Schoenmaker, L. et al. mRNA-lipid nanoparticle COVID-19 vaccines: structure and stability. Int. J. Pharm. 601, 120586 (2021).
Ndeupen, S. et al. The mRNA-LNP platform’s lipid nanoparticle component used in preclinical vaccine studies is highly inflammatory. Iscience 24, 103479 (2021). Demonstrated in a mouse model that LNPs used for the delivery of mRNA vaccines cause a strong inflammatory response that contributes to the vaccine efficacy but is also responsible for the side effects.
Dézsi, L. et al. A naturally hypersensitive porcine model may help understand the mechanism of COVID-19 mRNA vaccine-induced rare (pseudo) allergic reactions: complement activation as a possible contributing factor. GeroScience 1–22 (2022). Demonstrates in a pig model that injection of Comirnaty (Pfizer/BioNTech) vaccine causes hemodynamic changes in animals that are similar to the changes characteristic of infusion reactions to nanomedicines.
Pfizer-BioNTech COVID-19 Vaccine—Fact Sheet for Healthcare Providers Administering Vaccine (FDA, accessed 15 April 2021); https://www.fda.gov/emergency-preparedness-and-response/coronavirus-disease-2019-covid-19/pfizer-biontech-covid-19-vaccine#additional
Corbett K. S., et al. SARS-CoV-2 mRNA vaccine development enabled by prototype pathogen preparedness. Preprint at bioRxiv https://www.biorxiv.org/content/10.1101/2020.06.11.145920v1 (2020).
Vardi N. Moderna’s mysterious coronavirus vaccine delivery system. Forbes https://www.forbes.com/sites/nathanvardi/2020/07/29/modernas-mysterious-coronavirus-vaccine-delivery-system/?sh=3d2bcb8462d9 (2020).
Felgner, P. et al. Nomenclature for synthetic gene delivery systems. Human Gene Therapy 8, 511–512 (1997).
O’Shaughnessy J.A. Letter of Authorization to Pfizer (FDA, accessed 30 January 2022); https://www.fda.gov/media/150386/download
Adverse Events Reporting System (USFDA, accessed 15 March 2021); https://www.fda.gov/drugs/questions-and-answers-fdas-adverse-event-reporting-system-faers/fda-adverse-event-reporting-system-faers-public-dashboard
Acknowledgements
The study was funded in part by federal funds from the National Cancer Institute, National Institutes of Health, under contract 75N91019D00024 (M.A.D.), a NIH/NCI R01CA206220 grant (J.Y.L.), National Institutes of Health grants P50GM115305, R01HG010863, R01AI152183, R21AI139021 and U01AI154659 (E.J.P.) and NIH contract UAI109565 (E.J.P. and M.C.). The content of this publication does not necessarily reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products or organizations imply endorsement by the US Government. J.S. acknowledges support by the European Union Horizon 2020 projects 825828 (Expert) and 952520 (Biosafety), and the Department of Nanobiotechnology and Regenerative Medicine, Faculty of Health, Miskolc University, Miskolc, Hungary. The Hebrew University received royalties from Barenholz inventions; the Barenholz Fund established with a portion of these royalties is used to support research in the Barenholz Laboratory (Y.B. and K.T.). Funders played no role in any aspect of this review.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
G.S., K.T., Y.B., J.Y.L., M.C., M.A.D. and D.J.A.C. declare no competing interests. E.J.P. receives royalties and consulting fees from UpToDate, Janssen, Vertex, Biocryst and Regeneron; she is co-director of IIID Pty Ltd, which holds a patent for HLA-B*57:01/abacavir Australia and Canada testing for abacavir hypersensitivity (Canadian Patent 2,475,784 and Australian Patent 2003202657) and she has a patent pending for the Detection of Human Leukocyte Antigen-HLA-A*32:01/vancomycin in the U.S. (PCT/US2020/018420) in connection with Diagnosing Drug Reaction with Eosinophilia and Systemic Symptoms without any financial remuneration or direct relationship to the submitted work. J.S. is affiliated with SeroScience Ltd, an immune-toxicity-evaluating CRO.
Peer review
Peer review information
Nature Nanotechnology thanks Yizhou Dong, Bo Nilsson and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Szebeni, J., Storm, G., Ljubimova, J.Y. et al. Applying lessons learned from nanomedicines to understand rare hypersensitivity reactions to mRNA-based SARS-CoV-2 vaccines. Nat. Nanotechnol. 17, 337–346 (2022). https://doi.org/10.1038/s41565-022-01071-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41565-022-01071-x
This article is cited by
-
Strategies to reduce the risks of mRNA drug and vaccine toxicity
Nature Reviews Drug Discovery (2024)
-
Adjuvant and neoadjuvant immunotherapies in hepatocellular carcinoma
Nature Reviews Clinical Oncology (2024)
-
Targeted modulation of immune cells and tissues using engineered biomaterials
Nature Reviews Bioengineering (2023)
-
Duration of SARS-CoV-2 mRNA vaccine persistence and factors associated with cardiac involvement in recently vaccinated patients
npj Vaccines (2023)
-
mRNA-based cancer therapeutics
Nature Reviews Cancer (2023)