Abstract
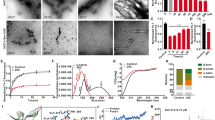
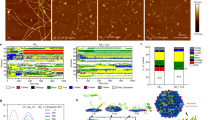
Though emerging evidence indicates that the pathogenesis of Parkinson’s disease is strongly correlated to the accumulation1,2 and transmission3,4 of α-synuclein (α-syn) aggregates in the midbrain, no anti-aggregation agents have been successful at treating the disease in the clinic. Here, we show that graphene quantum dots (GQDs) inhibit fibrillization of α-syn and interact directly with mature fibrils, triggering their disaggregation. Moreover, GQDs can rescue neuronal death and synaptic loss, reduce Lewy body and Lewy neurite formation, ameliorate mitochondrial dysfunctions, and prevent neuron-to-neuron transmission of α-syn pathology provoked by α-syn preformed fibrils5,6. We observe, in vivo, that GQDs penetrate the blood–brain barrier and protect against dopamine neuron loss induced by α-syn preformed fibrils, Lewy body/Lewy neurite pathology and behavioural deficits.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Dawson, T. M. & Dawson, V. L. Molecular pathways of neurodegeneration in Parkinson’s disease. Science 302, 819–822 (2003).
Spillantini, M. G. et al. Alpha-synuclein in Lewy bodies. Nature 388, 839–840 (1997).
Li, J. Y. et al. Lewy bodies in grafted neurons in subjects with Parkinson’s disease suggest host-to-graft disease propagation. Nat. Med. 14, 501–503 (2008).
Desplats, P. et al. Inclusion formation and neuronal cell death through neuron-to-neuron transmission of alpha-synuclein. Proc. Natl Acad. Sci. USA 106, 13010–13015 (2009).
Volpicelli-Daley, L. A. et al. Exogenous alpha-synuclein fibrils induce Lewy body pathology leading to synaptic dysfunction and neuron death. Neuron 72, 57–71 (2011).
Luk, K. C. et al. Pathological alpha-synuclein transmission initiates Parkinson-like neurodegeneration in nontransgenic mice. Science 338, 949–953 (2012).
Varela, L., Bell, C. H., Armitage, J. P. & Redfield, C. 1H, 13C and 15N resonance assignments for the response regulator CheY3 from Rhodobacter sphaeroides. Biomol. NMR Assign. 10, 373–378 (2016).
Bodner, C. R., Dobson, C. M. & Bax, A. Multiple tight phospholipid-binding modes of alpha-synuclein revealed by solution NMR spectroscopy. J. Mol. Biol. 390, 775–790 (2009).
Tuttle, M. D. et al. Solid-state NMR structure of a pathogenic fibril of full-length human alpha-synuclein. Nat. Struct. Mol. Biol. 23, 409–415 (2016).
Giasson, B. I., Murray, I. V. J., Trojanowski, J. Q. & Lee, V. M. Y. A hydrophobic stretch of 12 amino acid residues in the middle of alpha-synuclein is essential for filament assembly. J. Biol. Chem. 276, 2380–2386 (2001).
van Stokkum, I. H., Spoelder, H. J., Bloemendal, M., van Grondelle, R. & Groen, F. C. Estimation of protein secondary structure and error analysis from circular dichroism spectra. Anal. Biochem 191, 110–118 (1990).
Sreerama, N. & Woody, R. W. Estimation of protein secondary structure from circular dichroism spectra: comparison of CONTIN, SELCON, and CDSSTR methods with an expanded reference set. Anal. Biochem. 287, 252–260 (2000).
Lin, M. T. & Beal, M. F. Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443, 787–795 (2006).
Czupalla, C. J., Liebner, S. & Devraj, K. In vitro models of the blood–brain barrier. Methods Mol. Biol. 1135, 415–437 (2014).
Lee, M. K. et al. Human α-synuclein-harboring familial Parkinson’s disease-linked Ala-53→Thr mutation causes neurodegenerative disease with α-synuclein aggregation in transgenic mice. Proc. Natl Acad. Sci. USA 99, 8968–8973 (2002).
Brahmachari, S. et al. Activation of tyrosine kinase c-Abl contributes to α-synuclein-induced neurodegeneration. J. Clin. Invest. 126, 2970–2988 (2016).
Li, Q. et al. Modulating Aβ33–42 peptide assembly by graphene oxide. Chem. Eur. J. 20, 7236–7240 (2014).
Mahmoudi, M., Akhavan, O., Ghavami, M., Rezaee, F. & Ghiasi, S. M. A. Graphene oxide strongly inhibits amyloid beta fibrillation. Nanoscale 4, 7322–7325 (2012).
Liu, Y. et al. Graphene quantum dots for the inhibition of beta amyloid aggregation. Nanoscale 7, 19060–19065 (2015).
Yang, Z. X. et al. Destruction of amyloid fibrils by graphene through penetration and extraction of peptides. Nanoscale 7, 18725–18737 (2015).
Volpicelli-Daley, L. A., Luk, K. C. & Lee, V. M. Addition of exogenous alpha-synuclein preformed fibrils to primary neuronal cultures to seed recruitment of endogenous alpha-synuclein to Lewy body and Lewy neurite-like aggregates. Nat. Protoc. 9, 2135–2146 (2014).
Delaglio, F. et al. NMRPipe: a multidimensional spectral processing system based on UNIX pipes. J. Biomol. NMR 6, 277–293 (1995).
Lee, W., Tonelli, M. & Markley, J. L. NMRFAM-SPARKY: enhanced software for biomolecular NMR spectroscopy. Bioinformatics 31, 1325–1327 (2015).
Abraham, M. J. et al. GROMACS: High performance molecular simulations through multi-level parallelism from laptops to supercomputers. SoftwareX 1-2, 19–25 (2015).
Mackerell, A. D.Jr., Feig, M. & Brooks, C. L. III Extending the treatment of backbone energetics in protein force fields: limitations of gas-phase quantum mechanics in reproducing protein conformational distributions in molecular dynamics simulations. J. Comput. Chem. 25, 1400–1415 (2004).
Yu, W., He, X., Vanommeslaeghe, K. & MacKerell, A. D. Jr. Extension of the CHARMM General Force Field to sulfonyl-containing compounds and its utility in biomolecular simulations. J. Comput. Chem. 33, 2451–2468 (2012).
Lee, M. K. et al. Human α-synuclein-harboring familial Parkinson’s disease-linked Ala-53→Thr mutation causes neurodegenerative disease with α-synuclein aggregation in transgenic mice. Proc. Natl Acad. Sci. USA 99, 8968–8973 (2002).
Peelaerts, W. et al. α-Synuclein strains cause distinct synucleinopathies after local and systemic administration. Nature 522, 340–344 (2015).
Mao, X. et al. Pathological α-synuclein transmission initiated by binding lymphocyte-activation gene 3. Science 353, aah3374 (2016).
Acknowledgements
This work was supported by BIOGRAPHENE Inc. and an NRF (National Research Foundation of Korea) grant funded by the Korean government (NRF-2014H1A2A1016534-Global PhD Fellowship Program, NRF-2011-357-C00119) and grants from NIH/NINDS NS082205, NIH/NINDS NS098006 and NIH/NINDS NS38377 from the Morris K. Udall Parkinson’s Disease Research Center. This work was made possible by support from the Johns Hopkins Medicine Discovery Fund. The authors acknowledge joint participation by the Diana Helis Henry Medical Research Foundation and the Adrienne Helis Malvin Medical Research Foundation through direct engagement in the continuous active conduct of medical research in conjunction with The Johns Hopkins Hospital and the Johns Hopkins University School of Medicine and the Foundation’s Parkinson’s Disease Program H-1, H-2013 and M-2014. The authors extend their sincere gratitude to H. Lee of Ewha Womans University for discussions and helpful advice.
Author information
Authors and Affiliations
Contributions
B.H.H. and H.S.K. supervised the project. B.H.H. and J.M.Y. conceived the original idea of using GQDs for Parkinson’s disease. B.H.H., H.S.K., D.K. and J.M.Y. contributed to the study design. D.K., J.M.Y., H.H., S.H.L., S.P.Y., M.J.P., S.C., S.H.K., S.L., S.-H.K., S.K., Y.J.P., S.J.L. and S.L. contributed to overall data collection and interpretation. J.L., M.K., Y.-H.L. and S.R.P. contributed to NMR data collection and interpretation. M.L. and S.S. contributed to MD simulation and analysis. J.M.Y., J.L., S.R.P. and B.H.H. contributed to CD measurements and analysis. D.K., J.M.Y., S.H.L., B.H.H. and H.S.K wrote the paper. All authors discussed and commented on the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary Methods, Supplementary Table 1, Supplementary Figures 1–13, Supplementary References
Rights and permissions
About this article
Cite this article
Kim, D., Yoo, J.M., Hwang, H. et al. Graphene quantum dots prevent α-synucleinopathy in Parkinson’s disease. Nature Nanotech 13, 812–818 (2018). https://doi.org/10.1038/s41565-018-0179-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41565-018-0179-y
This article is cited by
-
Halogen doped graphene quantum dots modulate TDP-43 phase separation and aggregation in the nucleus
Nature Communications (2024)
-
An artificial protein modulator reprogramming neuronal protein functions
Nature Communications (2024)
-
Multifunctional Nanocarriers for Alzheimer’s Disease: Befriending the Barriers
Molecular Neurobiology (2024)
-
Synthesis of a Fluorescent Sensor by Exploiting Nitrogen-Doped MXene Quantum Dots for the Detection of Dopamine
Korean Journal of Chemical Engineering (2024)
-
Hybrid graphene electrode for the diagnosis and treatment of epilepsy in free-moving animal models
NPG Asia Materials (2023)