Abstract
Toxic bacterial modules such as toxin–antitoxin systems hold antimicrobial potential, though successful applications are rare. Here we show that in Vibrio cholerae the cyclic-oligonucleotide-based anti-phage signalling system (CBASS), another example of a toxic module, increases sensitivity to antifolate antibiotics up to 10×, interferes with their synergy and ultimately enables bacterial lysis by these otherwise classic bacteriostatic antibiotics. Cyclic-oligonucleotide production by the CBASS nucleotidyltransferase DncV upon antifolate treatment confirms full CBASS activation under these conditions, and suggests that antifolates release DncV allosteric inhibition by folates. Consequently, the CBASS–antifolate interaction is specific to CBASS systems with closely related nucleotidyltransferases and similar folate-binding pockets. Last, antifolate resistance genes abolish the CBASS–antifolate interaction by bypassing the effects of on-target antifolate activity, thereby creating potential for their coevolution with CBASS. Altogether, our findings illustrate how toxic modules can impact antibiotic activity and ultimately confer bactericidal activity to classical bacteriostatic antibiotics.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The data supporting the findings of this study are available as Source Data. Raw OD600 measurements for the compound screen, MIC determinations and compound combinations are available from https://github.com/brochadolab/Brenzinger2024.
Code availability
The computational scripts used for screen data analysis, MIC determination, analysis of compound combinations, molecular structural simulation and docking, as well as genomic analysis is available from https://github.com/brochadolab/Brenzinger2024.
References
Jurėnas, D., Fraikin, N., Goormaghtigh, F. & Van Melderen, L. Biology and evolution of bacterial toxin–antitoxin systems. Nat. Rev. Microbiol. 20, 335–350 (2022).
Song, S. & Wood, T. K. A primary physiological role of toxin/antitoxin systems is phage inhibition. Front. Microbiol. 11, 1895 (2020).
Harms, A., Brodersen, D. E., Mitarai, N. & Gerdes, K. Toxins, targets, and triggers: an overview of toxin-antitoxin biology. Mol. Cell 70, 768–784 (2018).
Chan, W. T., Balsa, D. & Espinosa, M. One cannot rule them all: are bacterial toxins-antitoxins druggable? FEMS Microbiol. Rev. 39, 522–540 (2015).
Lee, K.-Y. & Lee, B.-J. Structure, biology, and therapeutic application of toxin–antitoxin systems in pathogenic bacteria. Toxins 8, 305 (2016).
López-Igual, R., Bernal-Bayard, J., Rodríguez-Patón, A., Ghigo, J.-M. & Mazel, D. Engineered toxin–intein antimicrobials can selectively target and kill antibiotic-resistant bacteria in mixed populations. Nat. Biotechnol. 37, 755–760 (2019).
Nichols, R. J. et al. Phenotypic landscape of a bacterial cell. Cell 144, 143–156 (2011).
Lopatkin, A. J. et al. Clinically relevant mutations in core metabolic genes confer antibiotic resistance. Science 371, eaba0862 (2021).
Doron, S. et al. Systematic discovery of antiphage defense systems in the microbial pangenome. Science 359, eaar4120 (2018).
Cohen, D. et al. Cyclic GMP–AMP signalling protects bacteria against viral infection. Nature 574, 691–695 (2019).
Vassallo, C. N., Doering, C. R., Littlehale, M. L., Teodoro, G. I. C. & Laub, M. T. A functional selection reveals previously undetected anti-phage defence systems in the E. coli pangenome. Nat. Microbiol. 7, 1568–1579 (2022).
Bobonis, J. et al. Bacterial retrons encode phage-defending tripartite toxin–antitoxin systems. Nature 609, 144–150 (2022).
Millman, A. et al. An expanded arsenal of immune systems that protect bacteria from phages. Cell Host Microbe 30, 1556–1569 (2022).
Burroughs, A. M., Zhang, D., Schäffer, D. E., Iyer, L. M. & Aravind, L. Comparative genomic analyses reveal a vast, novel network of nucleotide-centric systems in biological conflicts, immunity and signaling. Nucleic Acids Res. 43, 10633–10654 (2015).
Lopatina, A., Tal, N. & Sorek, R. Abortive infection: bacterial suicide as an antiviral immune strategy. Annu Rev. Virol. 7, 371–384 (2020).
Makarova, K. S., Wolf, Y. I., Snir, S. & Koonin, E. V. Defense islands in bacterial and archaeal genomes and prediction of novel defense systems. J. Bacteriol. 193, 6039–6056 (2011).
Gao, L. et al. Diverse enzymatic activities mediate antiviral immunity in prokaryotes. Science 369, 1077–1084 (2020).
Rousset, F. et al. Phages and their satellites encode hotspots of antiviral systems. Cell Host Microbe 30, 740–753 (2022).
Whiteley, A. T. et al. Bacterial cGAS-like enzymes synthesize diverse nucleotide signals. Nature 567, 194–199 (2019).
Millman, A., Melamed, S., Amitai, G. & Sorek, R. Diversity and classification of cyclic-oligonucleotide-based anti-phage signalling systems. Nat. Microbiol. 5, 1608–1615 (2020).
Kranzusch, P. J. cGAS and CD-NTase enzymes: structure, mechanism, and evolution. Curr. Opin. Struct. Biol. 59, 178–187 (2019).
Huiting, E. et al. Bacteriophages inhibit and evade cGAS-like immune function in bacteria. Cell 186, 864–876 (2023).
Duncan-Lowey, B., McNamara-Bordewick, N. K., Tal, N., Sorek, R. & Kranzusch, P. J. Effector-mediated membrane disruption controls cell death in CBASS antiphage defense. Mol. Cell 81, 5039–5051 (2021).
Ledvina, H. E. et al. An E1–E2 fusion protein primes antiviral immune signalling in bacteria. Nature https://doi.org/10.1038/s41586-022-05647-4 (2023).
Davies, B. W., Bogard, R. W., Young, T. S. & Mekalanos, J. J. Coordinated regulation of accessory genetic elements produces cyclic di-nucleotides for V. cholerae virulence. Cell 149, 358–370 (2012).
Severin, G. B. et al. Direct activation of a phospholipase by cyclic GMP–AMP in El Tor Vibrio cholerae. Proc. Natl Acad. Sci. USA 115, E6048–E6055 (2018).
Zhu, D. et al. Structural biochemistry of a Vibrio cholerae dinucleotide cyclase reveals cyclase activity regulation by folates. Mol. Cell 55, 931–937 (2014).
Kato, K., Ishii, R., Hirano, S., Ishitani, R. & Nureki, O. Structural basis for the catalytic mechanism of DncV, bacterial homolog of cyclic GMP–AMP synthase. Structure 23, 843–850 (2015).
Brochado, A. R. & Typas, A. High-throughput approaches to understanding gene function and mapping network architecture in bacteria. Curr. Opin. Microbiol. 16, 199–206 (2013).
Kompis, I. M., Islam, K. & Then, R. L. DNA and RNA synthesis: antifolates. Chem. Rev. 105, 593–620 (2005).
Örtengren, B., Magni, L. & Bergan, T. Development of sulphonamide–trimethoprim combinations for urinary tract infections. Infection 7, S371–S381 (1979).
Eyler, R. F. & Shvets, K. Clinical pharmacology of antibiotics. CJASN 14, 1080–1090 (2019).
Kwon, Y. K. et al. A domino effect in antifolate drug action in Escherichia coli. Nat. Chem. Biol. 4, 602–608 (2008).
Bushby, S. R. M. Trimethoprim–sulfamethoxazole: in vitro microbiological aspects. J. Infect. Dis. 128, S442–S462 (1973).
Phillips, I. & Warren, C. Activity of sulfamethoxazole and trimethoprim against Bacteroides fragilis. Antimicrob. Agents Chemother. 9, 736–740 (1976).
Chevereau, G. & Bollenbach, T. Systematic discovery of drug interaction mechanisms. Mol. Syst. Biol. 11, 807 (2015).
Loewe, S. Die quantitativen Probleme der Pharmakologie. Ergeb. Physiol. 27, 47–187 (1928).
Hall, M. J., Middleton, R. F. & Westmacott, D. The fractional inhibitory concentration (FIC) index as a measure of synergy. J. Antimicrob. Chemother. 11, 427–433 (1983).
Woods, D. D. The relation of p-aminobenzoic acid to the mechanism of the action of sulphanilamide. Br. J. Exp. Pathol. 21, 74–90 (1940).
Estrada, A., Wright, D. L. & Anderson, A. C. Antibacterial antifolates: from development through resistance to the next generation. Cold Spring Harb. Perspect. Med 6, a028324 (2016).
Waldor, M. K., Tschäpe, H. & Mekalanos, J. J. A new type of conjugative transposon encodes resistance to sulfamethoxazole, trimethoprim, and streptomycin in Vibrio cholerae O139. J. Bacteriol. 178, 4157–4165 (1996).
Lau, R. K., Enustun, E., Gu, Y., Nguyen, J. V. & Corbett, K. D. A conserved signaling pathway activates bacterial CBASS immune signaling in response to DNA damage. EMBO J. 41, e111540 (2022).
Jenson, J. M., Li, T., Du, F., Ea, C.-K. & Chen, Z. J. Ubiquitin-like conjugation by bacterial cGAS enhances anti-phage defence. Nature 616, 326–331 (2023).
Minato, Y. et al. Mutual potentiation drives synergy between trimethoprim and sulfamethoxazole. Nat. Commun. 9, 1003 (2018).
Siegele, D. A. & Hu, J. C. Gene expression from plasmids containing the araBAD promoter at subsaturating inducer concentrations represents mixed populations. Proc. Natl Acad. Sci. USA 94, 8168–8172 (1997).
Maier, L. et al. Unravelling the collateral damage of antibiotics on gut bacteria. Nature 599, 120–124 (2021).
Severin, G. B. et al. Activation of a Vibrio cholerae CBASS anti-phage system by quorum sensing and folate depletion. mBio https://doi.org/10.1128/mbio.00875-23 (2023).
Cash, R. A., Northrup, R. S. & Mizanur Rahman, A. S. M. Trimethoprim and sulfamethoxazole in clinical cholera: comparison with tetracycline. J. Infect. Dis. 128, S749–S753 (1973).
Hughes, S. R., Kay, P. & Brown, L. E. Global synthesis and critical evaluation of pharmaceutical data sets collected from river systems. Environ. Sci. Technol. 47, 661–677 (2013).
Omuferen, L. O., Maseko, B. & Olowoyo, J. O. Occurrence of antibiotics in wastewater from hospital and convectional wastewater treatment plants and their impact on the effluent receiving rivers: current knowledge between 2010 and 2019. Environ. Monit. Assess. 194, 306 (2022).
Khlebnikov, A., Datsenko, K. A., Skaug, T., Wanner, B. L. & Keasling, J. D. Homogeneous expression of the PBAD promoter in Escherichia coli by constitutive expression of the low-affinity high-capacity AraE transporter. Microbiology 147, 3241–3247 (2001).
Stutzmann, S. & Blokesch, M. Comparison of chitin‐induced natural transformation in pandemic Vibrio cholerae O1 El Tor strains. Environ. Microbiol. 22, 4149–4166 (2020).
Lassak, J., Henche, A.-L., Binnenkade, L. & Thormann, K. M. ArcS, the cognate sensor kinase in an atypical arc system of Shewanella oneidensis MR-1. Appl. Environ. Microbiol. 76, 3263–3274 (2010).
Brenzinger, S. et al. Structural and proteomic changes in viable but non-culturable Vibrio cholerae. Front. Microbiol. 10, 793 (2019).
Gibson, D. G. et al. Enzymatic assembly of DNA molecules up to several hundred kilobases. Nat. Methods 6, 343–345 (2009).
Guzman, L. M., Belin, D., Carson, M. J. & Beckwith, J. Tight regulation, modulation, and high-level expression by vectors containing the arabinose PBAD promoter. J. Bacteriol. 177, 4121–4130 (1995).
Sinai, R., Hammerberg, S., Marks, M. I. & Pai, C. H. In vitro susceptibility of Haemophilus influenzae to sulfamethoxazole–trimethoprim and cefaclor, cephalexin, and cephradine. Antimicrob. Agents Chemother. 13, 861–864 (1978).
Ritz, C., Baty, F., Streibig, J. C. & Gerhard, D. Dose-response analysis using R. PLoS ONE 10, e0146021 (2015).
Wang, C.-Y. et al. Metabolome and proteome analyses reveal transcriptional misregulation in glycolysis of engineered E. coli. Nat. Commun. 12, 4929 (2021).
Chen, I.-M. A. et al. The IMG/M data management and analysis system v.7: content updates and new features. Nucleic Acids Res. 51, D723–D732 (2023).
Hahsler, M. rBLAST—R Interface for the Basic Local Alignment Search Tool (BLAST) https://github.com/mhahsler/r (2023).
The UniProt Consortium. UniProt: the universal protein knowledgebase in 2023. Nucleic Acids Res. 51, D523–D531 (2023).
Chen, I.-M. A. et al. The IMG/M data management and analysis system v.6.0: new tools and advanced capabilities. Nucleic Acids Res. 49, D751–D763 (2020).
Rozewicki, J., Li, S., Amada, K. M., Standley, D. M. & Katoh, K. MAFFT-DASH: integrated protein sequence and structural alignment. Nucleic Acids Res. 47, W5–W10 (2019).
Price, M. N., Dehal, P. S. & Arkin, A. P. FastTree 2—approximately maximum-likelihood trees for large alignments. PLoS ONE 5, e9490 (2010).
Paradis, E. & Schliep, K. ape 5.0: an environment for modern phylogenetics and evolutionary analyses in R. Bioinformatics 35, 526–528 (2019).
Mirdita, M. et al. ColabFold: making protein folding accessible to all. Nat. Methods 19, 679–682 (2022).
Jumper, J. et al. Highly accurate protein structure prediction with AlphaFold. Nature 596, 583–589 (2021).
Suzek, B. E. et al. UniRef clusters: a comprehensive and scalable alternative for improving sequence similarity searches. Bioinformatics 31, 926–932 (2015).
Schrödinger, LLC. The PyMOL Molecular Graphics System, version 1.8. (2015).
Morris, G. M. et al. AutoDock4 and AutoDockTools4: automated docking with selective receptor flexibility. J. Comput. Chem. 30, 2785–2791 (2009).
Edgar, R. C. Muscle5: high-accuracy alignment ensembles enable unbiased assessments of sequence homology and phylogeny. Nat. Commun. 13, 6968 (2022).
Acknowledgements
We thank A. Typas (European Molecular Biology Laboratory, Heidelberg), P. Beltrao (Swiss Federal Institute of Technology, Zurich) and C. Beisel (Helmholtz Institute for RNA-based Infection Research, Würzburg) for providing feedback on the manuscript, and the Brochado lab members for discussions. We acknowledge K. Thormann, G. Moncalian Montes, U. Dobrindt, A. Briegel and K. Hanevik for sharing bacterial strains or genomic DNA. We thank L. Schönemann (University of Würzburg) for support with DncV protein purification. This work was supported by JMU Würzburg internal funding, by the Deutsche Forschungsgemeinschaft (German Research Foundation) under Germany´s Excellence Strategy—EXC 2124—390838134, and the Emmy Noether programme to A.R.B. (GO 3161/1-1). S.B. was additionally supported by the Graduate School of Life Sciences Postdoc plus programme at the University of Würzburg. A.J.O. and M.A. were supported by the Hector Research Career Development Award 2020 by the Hector Fellow Academy to A.R.B. and GO 3161/1-1, respectively.
Author information
Authors and Affiliations
Contributions
S.B. and A.R.B. conceived and designed the study. S.B., M.A., K.J. and M.K.A. performed the experiments. A.J.O. did the CD-NTases phylogenetic analysis, structure and molecular docking predictions. A.R.B. and S.B. analysed the data and wrote the manuscript. A.R.B. supervised the study.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Peer review
Peer review information
Nature Microbiology thanks the anonymous reviewers for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Schematic representation of the screen workflow and data processing.
a) Schematic screen workflow. Details described in Methods. b) Schematic of data processing. Details described in Methods. c) Pearson replicate correlation between the triplicates of each strain. d) Scatterplot for comparison of mean residuals of wt vs. wt (y-axis) and CBASS vs. wt (x-axis). Each point represents the mean residuals (of three replicates) of the lines of best fit for a given condition (compound, concentration. There are very few conditions for which wt vs. wt residuals (measure of noise) surpasses the stringent cut-off = 0.2. All conditions for which the CBASS vs. wt mean of residuals is higher than 0.2 are marked in blue. SMX = Sulfamethoxazole, TMP = Trimethoprim, Mero = Meropenem, PenG = Penicillin G, Amox = Amoxicillin. Note that only TMP, SMX and PenG were considered as truly CBASS dependent, as Amox and Mero were noisy and did not pass the additional cut-off of score vs wt-wt residuals of a two-sided t-test Benjamini-Hochberg adjusted p-val<0.05. n equals the number of independent biological replicates.
Extended Data Fig. 2 Impact of CBASS in antifolates treatment of V. cholerae.
a) Pearson correlation coefficient of four MIC curves per strain and drug (shown in Fig. 2b) obtained from growth experiments in 96 well plates. b) Pearson replicate correlation based on AUC10h for checkerboard assays. The experiments were performed in quadruplicates, thus all possible 6 unique pairwise correlations are shown (a & b). c) MIC curves acquired in identical conditions to checkerboard experiments (384 well plates, N = 16) for TMP (left) and SMX (right). Drug concentrations and fitness are represented in the x-axis and y-axis, respectively. Fitness was calculated as the ratio between AUC10h with and without added drug. d) Simplified visualization of synergy between antifolates. MIC curves for wild-type (right) and ΔCBASS (left) showing that low TMP concentration decreases SMX MIC (triangles) in comparison to SMX alone (circles) are shown. e) Estimation of minFICi for isobole 0.1: FICis are calculated along drug concentrations normalized by their respective MICs, to determine the minimal minFICi0.1. n equals the number of independent biological replicates (c, d & e).
Extended Data Fig. 3 CBASS triggers cell death by lysis upon TMP treatment.
a) ΔCBASS enables killing by TMP. Colony forming units (CFU) of wild-type V. cholerae and ΔCBASS treated with 1 µg/ml TMP for 9 h are shown. Data is represented by mean values across n independent biological replicates +/- S.D. shown by error bars. b) TMP decreases cell viability. Cell viability after 7 h treatment with increasing concentrations (normalized to strain MIC) is shown. ΔCBASS survival is higher than wild-type at all concentrations, and never goes below the pre-treated sample (Pre). Only the wild-type loses ∼1-log survival at >5x MIC. c) Wild-type V. cholerae containing CBASS lyse upon TMP treatment. Fluorescence imaging of V. cholerae wild-type and ΔCBASS treated with 5x MIC90 TMP for 6 h, stained with propidium iodide (PI). >70% of the wild-type cells have permeabilized inner membranes, as indicated by loss of contrast in bright field channel (black arrows) and red fluorescent PI staining (overlayed image). d) Quantification of PI staining from panel c. Fraction of ΔCBASS cells stained with PI is 5% compared to 75% for wild-type. Increasing treatment severity (concentration and time) did not significantly increase cell death of ΔCBASS. Data points indicate the fraction of PI-stained cells from individual images derived from n independent biological replicates, with horizontal lines representing the mean value. n equals the number of independent biological replicates (a, b & d).
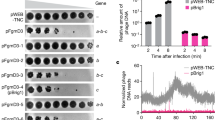
Extended Data Fig. 4 DncV is produced in V. cholerae and does not interact with SMX.
a) DncV is present in V. cholerae, and SMX treatment does not increase its levels. Immunoblot analysis of DncVAIA-6xHis (∼50 kDa) using anti-His antibodies. The experiment was done in Δcap3 background to avoid tag cleavage at the C-terminal24. Shown are three replicates of non-treated cells, and cells treated with 200 µg/ml SMX for 2 h (upper panel) or 5 h (lower panel) post SMX-addition. Overnight culture in both panels is shown as a reference. Total protein loaded per lane was controlled by Coomassie stain (Supplementary Fig. 1). b) Colony forming units of SMX treated cultures used for cGAMP quantification. Bar height represents mean over n independent biological replicates. c) CBASS overexpression exacerbates CBASS-antifolate interaction. Growth (AUC10h) of wild-type V. cholerae and CBASS-inducible mutant where the endogenous promoter region is replaced by araBAD promoter. L-arabinose and SMX concentrations are shown above and on the right side of the plot, respectively. d) Thermal shift assay confirms binding of 5-MTHF to DncV, but no direct SMX-DncV interaction. Shown are derivate melting curves (-dF/dT) over the applied temperature gradient of purified DncV treated with 5MTHF, SMX or buffer control. The maximum of the curves indicates the melting temperature (Tm) of DncV in each treatment, shifted to higher temperature only in the case of 5MTHF. e) Prevalence of CBASS and SMX resistance genes in all sequenced V. cholerae strains (Methods). n equals the number of independent biological replicates (b, c & d).
Extended Data Fig. 5 Assessment of CBASS-antifolate specificity across CD-NTases.
a) Heterologous expression of CBASS systems imposes higher burden than sfGFP. Growth curves of E. coli BW27783 expressing sfGFP or individual CBASS systems without arabinose. Data is represented by mean values across n independent biological replicates +/- S.D. shown by error bars (a & e). b) Predicted local distance difference test (pLDDT) of DncV and the selected CD-NTases from additional CBASS systems as quality control parameter for structure prediction by AlphaFold. DncV structure was also predicted as control. DncV structure was accurately predicted in comparison with the crystal structure27 (RMSD = 0.655 Å). The lowest confidence was observed for unstructured C-termini and a region found to form a flexible loop in the crystal structure of V. cholerae DncV27 (AA 203–238, indicated by black arrow), and the similar CD-NTase from E. coli TW11681 CBASS system 2. c) More than 80% of all protein sequences have a high confidence score (>80%), indicating a high global performance of the structure prediction. d) Isobolograms of arabinose-SMX combination treatment confirm high CBASS-antifolate interaction (concave lines) for the V. cholerae and E. coli TW11681 (2) systems, and weak or no interaction for E. coli 3234/A and E. coli TW11681 (1). Shown is one example out of four replicates per strain. Fitness is calculated by dividing AUC10h treated by AUC10h of the untreated samples. e) Restoring quorum sensing does not change CBASS-antifolate interaction in V. cholerae N16961. Minimum inhibitory concentration curves (AUC10h versus SMX concentration) for V. cholerae N16961 wild-type and HapRRep (quorum sensing positive after restoring hapR) are shown. Dashed line indicates 90% growth inhibition.
Supplementary information
41564_2023_1556_MOESM2_ESM.xlsx
Supplementary Table 1 Complete list of compounds used in the compound screen including purchase details, solvents used to prepare stock solutions and final screening concentrations. A brief description of the target and antibiotic class (when known and applicable) is also provided. Supplementary Table 2 All strains used and generated in this study including relevant genotype, plasmid construction details and primer sequences. Mutations of the CBASS locus of evolved SMX-resistant strains.
Source data
Source Data Fig. 1
Source data from compound screen with all calculated residuals, means and standard deviations, as well as two-sided t-test BH-adjusted P values.
Source Data Fig. 2
Source data for single-drug growth comparisons, MICs and drug combination effect of anti-folates.
Source Data Fig. 3
Source data for CFU and growth data under high SMX concentration, as well as microscopy cell counts of cells treated with SMX.
Source Data Fig. 4
Source data for MIC values of different mutants of the CBASS operon, measured cGAMP concentrations and growth data of CBASS expressing E. coli.
Source Data Fig. 5
Source data of MICs of spontaneously resistant mutants and evaluation of co-occurrence of CBASS components and sul1/sul2 genes.
Source Data Fig. 6
Source data for phylogenetic analysis of CD-NTases and fitness of E. coli expressing various CBASS variants.
Source Data Extended Data Fig. 1
Source data of replicate correlation and mean of residuals of the compound screen.
Source Data Extended Data Fig. 2
Source data of replicate correlations of MIC and combinatorial experiments, as well as growth data under TMP treatment, and FICi values over antifolate concentrations for determination of minFICi.
Source Data Extended Data Fig. 3
Source data for CFU measurements across various TMP concentrations and microscopy cell counts of cells treated with TMP.
Source Data Extended Data Fig. 4
Unprocessed western blots and SDS gels.
Source Data Extended Data Fig. 4
Source data of CFU measurements of cGAMP concentration determination samples, growth data of SMX-treated samples upon CBASS controlled induction, thermal shift assay data and fraction of sequenced V. cholerae strains encoding CBASS or sul1/sul2.
Source Data Extended Data Fig. 5
Source data of growth of untreated E. coli strains carrying CBASS expression plasmids, pLDDT values of CD-NTase predictions and corresponding confidence data, SMX–arabinose combination for E. coli strains carrying CBASS expression plasmids, and MIC data of V. cholerae-–HapR repaired strain.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Brenzinger, S., Airoldi, M., Ogunleye, A.J. et al. The Vibrio cholerae CBASS phage defence system modulates resistance and killing by antifolate antibiotics. Nat Microbiol 9, 251–262 (2024). https://doi.org/10.1038/s41564-023-01556-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41564-023-01556-y
This article is cited by
-
Reversible conjugation of a CBASS nucleotide cyclase regulates bacterial immune response to phage infection
Nature Microbiology (2024)