Abstract
The development of effective therapies against brain metastasis is currently hindered by limitations in our understanding of the molecular mechanisms driving it. Here we define the contributions of tumour-secreted exosomes to brain metastatic colonization and demonstrate that pre-conditioning the brain microenvironment with exosomes from brain metastatic cells enhances cancer cell outgrowth. Proteomic analysis identified cell migration-inducing and hyaluronan-binding protein (CEMIP) as elevated in exosomes from brain metastatic but not lung or bone metastatic cells. CEMIP depletion in tumour cells impaired brain metastasis, disrupting invasion and tumour cell association with the brain vasculature, phenotypes rescued by pre-conditioning the brain microenvironment with CEMIP+ exosomes. Moreover, uptake of CEMIP+ exosomes by brain endothelial and microglial cells induced endothelial cell branching and inflammation in the perivascular niche by upregulating the pro-inflammatory cytokines encoded by Ptgs2, Tnf and Ccl/Cxcl, known to promote brain vascular remodelling and metastasis. CEMIP was elevated in tumour tissues and exosomes from patients with brain metastasis and predicted brain metastasis progression and patient survival. Collectively, our findings suggest that targeting exosomal CEMIP could constitute a future avenue for the prevention and treatment of brain metastasis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
RNA-seq raw data that support the findings of this study have been deposited in the Gene Expression Omnibus under accession code GSE136628. Mass spectrometry raw data have been deposited in ProteomeXchange with the primary accession code PXD015210. The mass spectrometry processed data of MDA-MB-231 parental (parental), brain-tropic (231-BR (BrT1) and 831 (BrT2)), lung-tropic (4175 (LuT1) and 4173 (LuT2)) and bone-tropic (1833 (BoT1)) exosomes (Fig. 1c) are available in Supplementary Table 2. The processed RNA sequencing data from Fig. 4d and Supplementary Tables 4, 5, 6, 7, for murine BrECs and microglia cells isolated from ex vivo brain slices treated with PBS, 231 BrT1 WT, 231 BrT1 CEMIP KO1 and KO2 exosomes, are available as Supplementary Table 3. The processed patient data from Fig. 5 and Supplementary Fig. 5 are available as Supplementary Table 8. Unprocessed scans and replicates for all immunoblots presented in the manuscript are available as Supplementary Fig. 6.
References
Valastyan, S. & Weinberg, R. A. Tumor metastasis: molecular insights and evolving paradigms. Cell 147, 275–292 (2011).
Maher, E. A., Mietz, J., Arteaga, C. L., DePinho, R. A. & Mohla, S. Brain metastasis: opportunities in basic and translational research. Cancer Res. 69, 6015–6020 (2009).
Eichler, A. F. et al. The biology of brain metastases—translation to new therapies. Nat. Rev. Clin. Oncol. 8, 344–356 (2011).
Valiente, M. et al. Serpins promote cancer cell survival and vascular co-option in brain metastasis. Cell 156, 1002–1016 (2014).
Sevenich, L. et al. Analysis of tumour- and stroma-supplied proteolytic networks reveals a brain-metastasis-promoting role for cathepsin S. Nat. Cell Biol. 16, 876–888 (2014).
Bos, P. D. et al. Genes that mediate breast cancer metastasis to the brain. Nature 459, 1005–1009 (2009).
Lorger, M. & Felding-Habermann, B. Capturing changes in the brain microenvironment during initial steps of breast cancer brain metastasis. Am. J. Pathol. 176, 2958–2971 (2010).
Thery, C., Ostrowski, M. & Segura, E. Membrane vesicles as conveyors of immune responses. Nat. Rev. Immunol. 9, 581–593 (2009).
Peinado, H. et al. Pre-metastatic niches: organ-specific homes for metastases. Nat. Rev. Cancer 17, 302–317 (2017).
Peinado, H. et al. Melanoma exosomes educate bone marrow progenitor cells toward a pro-metastatic phenotype through MET. Nat. Med. 18, 883–891 (2012).
Costa-Silva, B. et al. Pancreatic cancer exosomes initiate pre-metastatic niche formation in the liver. Nat. Cell Biol. 17, 816–826 (2015).
Hoshino, A. et al. Tumour exosome integrins determine organotropic metastasis. Nature 527, 329–335 (2015).
Lowery, F. J. & Yu, D. Brain metastasis: unique challenges and open opportunities. Biochim. Biophys. Acta Rev. Cancer 1867, 49–57 (2017).
Polleux, F. & Ghosh, A. The slice overlay assay: a versatile tool to study the influence of extracellular signals on neuronal development. Sci. STKE 2002, pl9 (2002).
Yoneda, T., Williams, P. J., Hiraga, T., Niewolna, M. & Nishimura, R. A bone-seeking clone exhibits different biological properties from the MDA-MB-231 parental human breast cancer cells and a brain-seeking clone in vivo and in vitro. J Bone Miner. Res. 16, 1486–1495 (2001).
Carbonell, W. S., Ansorge, O., Sibson, N. & Muschel, R. The vascular basement membrane as ‘soil’ in brain metastasis. PLoS One 4, e5857 (2009).
Lorger, M., Krueger, J. S., O’Neal, M., Staflin, K. & Felding-Habermann, B. Activation of tumor cell integrin αvβ3 controls angiogenesis and metastatic growth in the brain. Proc. Natl Acad. Sci. USA 106, 10666–10671 (2009).
Abe, S., Usami, S. & Nakamura, Y. Mutations in the gene encoding KIAA1199 protein, an inner-ear protein expressed in Deiters’ cells and the fibrocytes, as the cause of nonsyndromic hearing loss. J. Hum. Genet. 48, 564–570 (2003).
Yoshida, H. et al. KIAA1199, a deafness gene of unknown function, is a new hyaluronan binding protein involved in hyaluronan depolymerization. Proc. Natl Acad. Sci. USA 110, 5612–5617 (2013).
Evensen, N. A. et al. Unraveling the role of KIAA1199, a novel endoplasmic reticulum protein, in cancer cell migration. J. Natl Cancer Inst. 105, 1402–1416 (2013).
Birkenkamp-Demtroder, K. et al. Repression of KIAA1199 attenuates Wnt-signalling and decreases the proliferation of colon cancer cells. Br. J. Cancer 105, 552–561 (2011).
Zhang, Y., Jia, S. & Jiang, W. G. KIAA1199 and its biological role in human cancer and cancer cells (review). Oncol. Rep. 31, 1503–1508 (2014).
Yang, X. et al. KIAA1199 as a potential diagnostic biomarker of rheumatoid arthritis related to angiogenesis. Arthritis Res. Ther. 17, 140 (2015).
Yoshino, Y. et al. Distribution and function of hyaluronan binding protein involved in hyaluronan depolymerization (HYBID, KIAA1199) in the mouse central nervous system. Neuroscience 347, 1–10 (2017).
Zhang, H. et al. Identification of distinct nanoparticles and subsets of extracellular vesicles by asymmetric flow field-flow fractionation. Nat. Cell Biol. 20, 332–343 (2018).
Winkler, F. Hostile takeover: how tumours hijack pre-existing vascular environments to thrive. J. Pathol. 242, 267–272 (2017).
Fidler, I. J. The role of the organ microenvironment in brain metastasis. Semin. Cancer Biol. 21, 107–112 (2011).
Arnold, T. & Betsholtz, C. The importance of microglia in the development of the vasculature in the central nervous system. Vasc. Cell 5, 4 (2013).
Tran, Q. K., Ohashi, K. & Watanabe, H. Calcium signalling in endothelial cells. Cardiovasc. Res. 48, 13–22 (2000).
Liebner, S. et al. Wnt/beta-catenin signaling controls development of the blood–brain barrier. J. Cell Biol. 183, 409–417 (2008).
Shimizu, H. et al. Hyaluronan-binding protein involved in hyaluronan depolymerization is up-regulated and involved in hyaluronan degradation in human osteoarthritic cartilage. Am. J. Pathol. 188, 2109–2119 (2018).
Burri, P. H., Hlushchuk, R. & Djonov, V. Intussusceptive angiogenesis: its emergence, its characteristics, and its significance. Dev. Dyn. 231, 474–488 (2004).
Dimova, I. et al. Inhibition of Notch signaling induces extensive intussusceptive neo-angiogenesis by recruitment of mononuclear cells. Angiogenesis 16, 921–937 (2013).
Giacomini, A. et al. Brain angioarchitecture and intussusceptive microvascular growth in a murine model of Krabbe disease. Angiogenesis 18, 499–510 (2015).
Doron, H., Pukrop, T. & Erez, N. A blazing landscape: neuroinflammation shapes brain metastasis. Cancer Res. 79, 423–436 (2019).
Tominaga, N. et al. Brain metastatic cancer cells release microRNA-181c-containing extracellular vesicles capable of destructing blood–brain barrier. Nat. Commun. 6, 6716 (2015).
van der Vos, K. E. et al. Directly visualized glioblastoma-derived extracellular vesicles transfer RNA to microglia/macrophages in the brain. Neuro Oncol. 18, 58–69 (2016).
Acknowledgements
We thank M. Ginsberg, G. Marra, P. Raju and T. Milner for reagents and expert advice; L. Nogues Vera, M. Teixeira and S. Grass for help in the laboratory; M. Schaeffer for proofreading; T. Zhang and K. Gyan for help with bioinformatics analysis; L. Cohen-Gould, the MSKCC Molecular Cytology Core Facility and K. Uryu for imaging counselling; T. Miller and F. Fang at the MSKCC Flow cytometry Core Facility, and T. Baumgartner at the Weill Cornell Medicine Flow Cytometry Core, as well as R. Bowman, for expert cell sorting; and the MSKCC Gene Editing and Screening Core Facility for molecular cloning and gene editing advice. We gratefully acknowledge support from the following funding sources: the National Cancer Institute (CA169538 to D.L. and CA232093 to D.L.), the US Department of Defense (W81XWH-13-1-0427 to D.L.), the Breast Cancer Research Foundation (to D.L. and C.M.G.), the Champalimaud Foundation, the Daedalus Fund for Innovation (Weill Cornell Medicine, to D.L.), the Children’s Cancer and Blood Foundation, the Pediatric Oncology Experimental Therapeutics Investigator’s Consortium Foundation, the Nancy C. and Daniel P. Paduano Foundation, the Eileen and James A. Paduano Foundation, the Sohn Foundation, the Hartwell Foundation, the Manning Foundation, the Thompson Foundation, the Malcolm Hewitt Wiener Foundation and the Tortolani Foundation. G.R. has been supported by a Peter Oppenheimer Fellowship, awarded by the American Portuguese Biomedical Research Fund, and by the Fundação para a Ciência e a Tecnologia from Portugal. A.H. was supported by a Susan Komen Foundation for the Cure Fellowship. H.P. is supported by grants from MINECO (SAF2014-54541-R), Fundación Fero, Asociación Española Contra el Cáncer and Worldwide Cancer Research. C.M.G. is supported by a US Department of Defense Breast Cancer Research Program Era of Hope Scholar Award (W81XWH-15-1-0201), the US National Cancer Institute (CA193461-01), the National Breast Cancer Coalition’s Artemis Project and the Pink Gene Foundation.
Author information
Authors and Affiliations
Contributions
G.R. designed the experimental approach, performed the experimental work, analysed the data, coordinated the project and wrote the manuscript. A.H. performed PT growth and exosome education in vivo studies, cancer cell proliferation in vitro studies, cancer cell culture and exosome isolation, coordinated the project and wrote the manuscript. C.M.K. generated CEMIP OE, performed molecular cloning work and genetic manipulation of cancer cells, cancer cell culture and exosome isolation, coordinated the project and wrote the manuscript. I.R.M. performed brain slice ex vivo FACS analysis and exosome education in vivo studies, cancer cell culture and exosome isolation, coordinated the project, and wrote and reviewed the manuscript. L.S. performed brain slice ex vivo experimental work, tissue processing and immunostaining, ex vivo and in vivo ImageJ data analysis and quantification, cancer cell invasion in vitro studies, western blot analysis, cancer cell culture and exosome isolation, and contributed to figure panel assembly. D.F. performed density gradient exosome isolation, characterization and analysis, western blot analysis and cancer cell culture. H.S.K. and P.R.O. performed RNA sequencing data analysis. I.S. performed tissue processing and immunostaining, ex vivo and in vivo ImageJ data analysis and quantification, cancer cell culture and exosome isolation. I.C.-S. performed western blot analysis and assisted in analysis of human data. J.D., C.R.B. and T.M.L. performed in vitro BrEC experimental work and FACS analysis. M.T.M., B.D.D. and H.M. performed exosome mass spectrometry and proteomic data analysis. A.B.-M. assisted in mouse studies and FACS analysis. H.W. and X.J. assisted in tissue processing and immunostaining, cancer cell culture and exosome isolation. L.B., K.O., Q.L., Y.A., W.B. and H.W. received and processed human samples. Y.A., W.B. and H.W. assisted in the maintenance of mouse colonies. Y.L., J.K.S., S.J.S., N.N., J.H.H., N.K.A., C.M.R., D.R.J. and D.P. provided human samples. V.K.R. generated and provided the N2LA human lung cancer cell line. S.E.W. provided the 231-HM human breast cancer cell line. B.G. and P.S.S. provided the 231BR human breast cancer cell line and gave feedback on the project. S.R. provided endothelial cell expertise and reagents. D.P. coordinated human studies and contributed to the experimental design. D.P., N.N. and P.S.G. analysed the human data. E.M. and H.Z. read the manuscript and gave feedback on the project. B.C.-S., H.P., C.M.G. and J.B. contributed to hypothesis discussion, experimental design, data interpretation and project coordination. M.d.S. coordinated the project, contributed to hypothesis discussion, experimental design, data interpretation and wrote the manuscript. D.L. conceived the hypothesis, led the project, interpreted the data and wrote the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Brain slice model to study the role of tumour exosomes in metastatic colonization.
a, Illustration of organotropic metastatic derivatives1,2,3,4,5,6 of MDA-MB-231 breast cancer cell model (parental (gray) and brain (purple), lung (orange), and bone (green) metastatic) and respective cell-derived exosomes analyzed. Schematic of the brain slice ex vivo model optimized for the study of exosome-mediated cancer cell brain colonization. b, Schematic of the brain slice model used to study the effects of exosome pre-treatment on the brain microenvironment and cancer cell phenotypes (left, cancer cell number—whole brain slice mount; and right, cancer cell invasion—brain slice transversal section). Invading cells (white arrows) inside the region of interest, denoted by the blue square, are comprised of all cancer cells below the first layer of brain cells on the top of the brain slice. c, Representative whole slice fluorescence images of BrT1 GFP+ cells growing on top of brain slices pre-treated with exosomes or PBS. d, Left, representative immunofluorescence microscopy images of proliferating Ki-67+ BrT1 GFP+ cells invading brain slices pre-treated with exosomes. White and red arrows indicate invading Ki-67- or Ki-67+ cells, respectively. Right, quantification of Ki-67+ invading cancer cell number. e, Left, representative fluorescence images of 231 parental mCherry+ cells growing on top of brain slices pre-treated with exosomes or PBS. Right, quantification of 231 parental mCherry+ cell number. f, Left, immunoblot of CEMIP, small EV and exosomal markers (HSP70, Syntenin-1 and CD81) and ACTB in fractions obtained by OptiPrep™ density gradient ultracentrifugation7 of BrT1 exosomes. Right, densitometry quantification of protein expression in the initial exosome population (Input) and across fractions with different density, given in arbitrary units [a.u.]. Small EV and exosome-containing fractions are shown between dashed lines. The number of cells per FOV are averages ± SEM, from n = 3, 4 (d) and n = 3 (e) individual brain slices, scoring two fields per slice. A representative experiment of three (d, e) or four (f) independent biological replicates is shown. Brain slice images (c) are representative of three independent biological replicates. Brain slice sections are stained with DAPI (blue), and dotted blue lines delineate the top and bottom limits of the brain slice (d). Scale bars, 500µm (c) and 100µm (d, e). Error bars depict mean ± SEM. P values were calculated by ANOVA (e) or two-sided Student’s t-test (d). See Supplementary Fig. 6 for unprocessed blots. See Supplementary Table 1 for statistics source data.
Supplementary Figure 2 Exosomal CEMIP modulates the brain vascular niche to support metastasis.
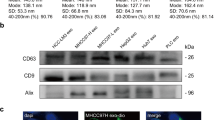
a, Left, immunoblot of CEMIP expression in cell and exosomal protein extracts from BrT1 WT and BrT1 CEMIP knockout (KO1 and KO2) cells. Immunoblotting for exosomal markers (Syntenin-1 and CD81) and ACTB is shown below. Right, densitometry quantification of CEMIP normalized to the CEMIP expression in BrT1 WT exosomes. CEMIP expression was normalized to ACTB expression for each sample. b, Transmission electron microscopy (TEM) of BrT1 WT and BrT1 CEMIP-KO1 and -KO2 exosomes. c, Size distribution and protein content analysis of BrT1 WT and BrT1 CEMIP-KO1 and -KO2 exosomes. Exosome size (mode, nm) and number were evaluated by NanoSight particle tracking. Protein content per exosome ([particle]/[protein]) was assessed by factoring in the protein concentration. d, Quantification of BrT1 WT and 231 BrT1 CEMIP-KO1 and -KO2 GFP+ cell number on top of brain slices. e, Left, representative fluorescence microscopy image of BrT1 GFP+ cells growing on top of the brain slice. Right, representative fluorescence microscopy image of BrT1 GFP+ cells invading the brain slice in transversal section. f, Quantification of proliferation of BrT1 WT and BrT1 CEMIP-KO1 and -KO2 cells in vitro over three days. g, Quantification of transwell Matrigel invasion of BrT1 WT and BrT1 CEMIP-KO1 and -KO2 cells in vitro over 24 hours. h, Quantification of BrT1 KO2 GFP+ cells on top of brain slices pre-treated with exosomes or PBS. The number of cells per FOV are averages ± SEM, from n = 8, 9, 9 (d), n = 9, 7, 9, 9 (h) individual brain slices, scoring two fields per slice; and the number of invading cells per FOV are averages ± SEM, from n=3 individual transwell cultures (g), scoring a representative field per transwell membrane. One of three (a - c, d, h) independent biological replicates is shown. Graphs depicting in vitro proliferation and invasion (f and g) display three independent biological replicates. TEM images and immunofluorescence brain slice images (b and e) are representative of three independent biological replicates. Scale bars, 200 nm (b), and 100 µm (e). Error bars depict mean ± SEM. P values were calculated by ANOVA (c - d, and f - h). See Supplementary Fig. 6 for unprocessed blots. See Supplementary Table 1 for statistics source data.
Supplementary Figure 3 CEMIP loss does not affect primary tumour growth or in situ growth in the brain.
a, Left, quantification of brain metastatic in situ growth in mice intracranially injected with BrT1 WT or BrT1 CEMIP-KO cells. Cranial bioluminescence signal (Total photon flux—photons/second (p/s)) in mice over 3-weeks post-intracranial injection of GFP-labelled BrT1 WT or BrT1 CEMIP-KO luciferase-positive cells. Right, representative IVIS image of brain signal at week 3. b, Quantification of primary tumour growth8 in mice injected with BrT1 WT or BrT1 CEMIP-KO cells. One experiment with n=5 mice per experimental group was performed (a, b). See Supplementary Table 1 for statistics source data.
Supplementary Figure 4 Exosomal CEMIP affects BrEC biology and induces vascular remodeling.
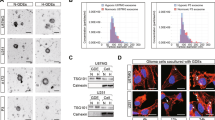
a, Schematic of the brain slice model setup for the study of exosome interaction with brain microenvironment resident cells. b, Representative fluorescence image of BrT1 exosomes (green) interacting with CD31+ BrECs (red) in vivo 24 hours post-intracardiac injection of labelled exosomes. c, Representative fluorescence image of BrT1 exosomes (green) and associated extravasated rhodamine-labelled Dextran (red) in the brain 24 hours post-intracardiac injection of labelled exosomes (right, enlarged inset). d, Schematic of the ETF assay setup for studying exosome-dependent vascular network formation by isolated BrECs9,10. e, Left, immunoblot of CEMIP expression in cells and exosomes of 231 parental Control and 231 parental CEMIP overexpressing (OE) models generated11,12. ACTB and the exosomal marker CD81 are shown below. Right, densitometry quantification of CEMIP expression is normalized to expression in 231 parental Control exosomes. CEMIP expression was normalized to ACTB expression for each sample. f, Quantification of junction (top) and isolated segment (bottom) number in the vasculature formed upon pre-treatment with exosomes or PBS. g, Left, representative fluorescence image of tumour vasculature (red) in BrT1 brain metastases (white). Right, quantification of metastatic tumour and normal vessel diameter in brains from mice injected intracardiacally with BrT1 WT, BrT1 CEMIP-KO1 or -KO2 cells. h, Schematic of the brain slice model setup for studying exosome-induced gene expression changes in stromal cells of the brain. Brain slices were pre-treated with BrT1 WT, BrT1 CEMIP-KO1 or -KO2 cell-derived fluorescently-labelled exosomes. i, Flow cytometry analysis of exosome uptake. Percentage of exosome-positive (Exo+) endothelial (CD45− CD31+) and microglial (CD45+ CD11blow CD49dlow)13 cells in brain slices is shown. j, Representative confocal images of the adhesion of fluorescently-labelled BrT1 WT, BrT1 CEMIP-KO1 or -KO2 exosomes with endothelial cells (CD31+) in the brain slice. Arrows indicate co-localization of exosomes (green) with endothelial cells (red). For in vivo experiments, n=4 mice were analyzed per group (g). Individual vessel diameter was obtained from the average of three measurements along the extension of the vessel. Metastatic tumour and normal brain vascular diameters were scored in up to 5 individual metastatic lesions across two sagittal sections from different brain areas per individual presenting brain metastases (g). The number of junctions and isolated segments per FOV are averages ± SEM, from n = 5, 7, 8, 7, 8, 8 individual µ-slide angiogenesis chamber wells (f), scoring a representative field per µ-slide well. A representative experiment is shown from three independent biological replicates (e - f). Graphs depicting endothelial and microglial cell exosome uptake and tumour vasculature diameter (i and g) display the average of three and two independent biological replicates, respectively. Immunofluorescence images of in vivo exosome uptake by BrECs, vascular leakiness and confocal images of the interaction and BrEC exosome uptake in the brain slice (b, c and j) are representative of three independent biological replicates. Scale bars, 50µm (b), 50μm and 100μm (c), 100µm (g) and 75µm (j). Error bars depict mean ± SEM. P values were calculated by ANOVA (f, g, i). See Supplementary Fig. 6 for unprocessed blots. See Supplementary Table 1 for statistics source data.
Supplementary Figure 5 CEMIP is a biomarker of BrM and is present in exosomes from patients.
a, Kaplan-Meier survival curve for brain metastasis patients depicting time to last follow up (LFU) or death from time of primary tumour diagnosis based on low (green) or high (red) CEMIP expression in brain metastatic tumour. b, Representative image of CEMIP expression in 231 parental and BrT1 cells in vitro by immunohistochemistry. c, Immunoblot of CEMIP expression in exosomes collected from culture of human brain and bone metastatic tissue explants resected from patients. ACTB was used as loading control. Marker indicated by m. d, Immunoblot of CEMIP expression in exosomes collected from culture of human non-small cell lung cancer primary tumour tissue resected from patients. ACTB was used as a loading control. IHC images (b) and immunoblots (c, d) are representative of one experiment. Scale bars, 100µm (b). P values was calculated by Log-rank (Mantel-Cox) test (a). See Supplementary Fig. 6 for unprocessed blots. See Supplementary Table 1 for statistics source data.
Supplementary Figure 6 Unprocessed western blots continued.
Western blot replicates for Fig. 1e (Replicate C is shown in figure). Sample order is the same as specified in respective manuscript figure. Western blot replicates for Supplementary Fig. 1f (Replicate B is shown in figure). Sample order is the same as specified in respective manuscript figure. Western blot replicates for Supplementary Fig. 2a (Replicate A is shown in figure). Sample order is the same as specified in respective manuscript figure. Western blot replicates for Supplementary Fig. 4e (Replicate A is shown in figure). Sample order is the same as specified in respective manuscript figure. Western blots for Supplementary Fig. 5c. Sample order is the same as specified in respective manuscript figure. Western blots for Supplementary Fig. 5d. Sample order is the same as specified in respective manuscript figure.
Supplementary information
Supplementary Information
Supplementary Figures 1–6 and table titles/legends.
Supplementary Table 1
Statistics source data.
Supplementary Table 2
Mass spectrometry data.
Supplementary Table 3
RNA sequencing data.
Supplementary Table 4
Heatmap of significant genes differentially expressed in brain endothelial and microglial cells following BrT1 exosome treatment, relative to the WT condition.
Supplementary Table 5
Top significant IPA canonical pathways - BrECs and microglia – 231 BrT1 exosomes and exosomal CEMIP specific – List of canonical pathways affected by 231 BrT1 exosome and exosomal CEMIP treatment in BrECs and microglia.
Supplementary Table 6
Heatmap of significant genes differentially expressed in brain endothelial and microglial cells following exosomal CEMIP treatment, relative to the WT condition.
Supplementary Table 7
Top 10 significant Gene Ontology - Biological Processes - BrECs and microglia – exosomal CEMIP specific - List of significant Biological Processes affected by exosomal CEMIP treatment in BrECs and microglia.
Supplementary Table 8
Patient data.
Supplementary Table 9
Correlation of CEMIP expression in PTs and metastatic status.
Supplementary Table 10
Antibodies and primers.
Rights and permissions
About this article
Cite this article
Rodrigues, G., Hoshino, A., Kenific, C.M. et al. Tumour exosomal CEMIP protein promotes cancer cell colonization in brain metastasis. Nat Cell Biol 21, 1403–1412 (2019). https://doi.org/10.1038/s41556-019-0404-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41556-019-0404-4
This article is cited by
-
Protein cargo in extracellular vesicles as the key mediator in the progression of cancer
Cell Communication and Signaling (2024)
-
The incorporation of acetylated LAP-TGF-β1 proteins into exosomes promotes TNBC cell dissemination in lung micro-metastasis
Molecular Cancer (2024)
-
Synchronous double primary small cell lung cancer and invasive ductal breast carcinoma: a case report
BMC Pulmonary Medicine (2024)
-
Extracellular vesicle-mediated transfer of miRNA-1 from primary tumors represses the growth of distant metastases
Experimental & Molecular Medicine (2024)
-
A Prognostic Methylation-Driven Two-Gene Signature in Medulloblastoma
Journal of Molecular Neuroscience (2024)