Abstract
Phosphorylation networks intimately regulate mechanisms of response to therapies. Mapping the phospho-catalytic profile of kinases in cells or tissues remains a challenge. Here, we introduce a practical high-throughput system to measure the enzymatic activity of kinases using biological peptide targets as phospho-sensors to reveal kinase dependencies in tumour biopsies and cell lines. A 228-peptide screen was developed to detect the activity of >60 kinases, including ABLs, AKTs, CDKs and MAPKs. Focusing on BRAFV600E tumours, we found mechanisms of intrinsic resistance to BRAFV600E-targeted therapy in colorectal cancer, including targetable parallel activation of PDPK1 and PRKCA. Furthermore, mapping the phospho-catalytic signatures of melanoma specimens identifies RPS6KB1 and PIM1 as emerging druggable vulnerabilities predictive of poor outcome in BRAFV600E patients. The results show that therapeutic resistance can be caused by the concerted upregulation of interdependent pathways. Our kinase activity-mapping system is a versatile strategy that innovates the exploration of actionable kinases for precision medicine.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Data availability
The human melanoma data were derived from the TCGA Research Network (http://cancergenome.nih.gov/). The RNA-Seq dataset derived from this resource that supports the findings of this study is available in the TCGA, Skin Cutaneous Melanoma repository accessed and analysed online using cBioPortal (http://www.cbioportal.org). RNA-Seq data that support the findings of this study have been deposited in the Gene Expression Omnibus under accession code GSE129127. Source data for Figs. 1, 2, 3a, 4a,b, 5a, 6a and 7d and Supplementary Figs. 1e–h, 1k,l, 2–5, 6d–f and 7c have been provided as Supplementary Table 26. All other data supporting the findings of this study are available from the corresponding author on reasonable request.
References
Petricoin, E. F., Zoon, K. C., Kohn, E. C., Barrett, J. C. & Liotta, L. A. Clinical proteomics: translating benchside promise into bedside reality. Nat. Rev. Drug Discov. 1, 683–695 (2002).
Blume-Jensen, P. & Hunter, T. Oncogenic kinase signalling. Nature 411, 355–365 (2001).
Fleuren, E. D., Zhang, L., Wu, J. & Daly, R. J. The kinome ‘at large’ in cancer. Nat. Rev. Cancer 16, 83–98 (2016).
Johnson, S. A. & Hunter, T. Kinomics: methods for deciphering the kinome. Nat. Methods 2, 17–25 (2005).
Krogan, N. J., Lippman, S., Agard, D. A., Ashworth, A. & Ideker, T. The Cancer Cell Map Initiative: defining the hallmark networks of cancer. Mol. Cell 58, 690–698 (2015).
Hoadley, K. A. et al. Multiplatform analysis of 12 cancer types reveals molecular classification within and across tissues of origin. Cell 158, 929–944 (2014).
Akbani, R. et al. A pan-cancer proteomic perspective on The Cancer Genome Atlas. Nat. Commun. 5, 3887 (2014).
Chandarlapaty, S. et al. AKT inhibition relieves feedback suppression of receptor tyrosine kinase expression and activity. Cancer Cell 19, 58–71 (2011).
Coppe, J. P. et al. Senescence-associated secretory phenotypes reveal cell-nonautonomous functions of oncogenic RAS and the p53 tumor suppressor. PLoS Biol. 6, 2853–2868 (2008).
Huttlin, E. L. et al. The BioPlex Network: a systematic exploration of the human interactome. Cell 162, 425–440 (2015).
Rikova, K. et al. Global survey of phosphotyrosine signaling identifies oncogenic kinases in lung cancer. Cell 131, 1190–1203 (2007).
Zhang, B. et al. Proteogenomic characterization of human colon and rectal cancer. Nature 513, 382–387 (2014).
Uhlen, M. et al. Proteomics. Tissue-based map of the human proteome. Science 347, 1260419 (2015).
Drake, J. M. et al. Phosphoproteome integration reveals patient-specific networks in prostate. Cancer Cell 166, 1041–1054 (2016).
Sharma, K. et al. Ultradeep human phosphoproteome reveals a distinct regulatory nature of Tyr and Ser/Thr-based signaling. Cell Rep. 8, 1583–1594 (2014).
Duncan, J. S. et al. Dynamic reprogramming of the kinome in response to targeted MEK inhibition in triple-negative breast cancer. Cell 149, 307–321 (2012).
Sos, M. L. et al. Oncogene mimicry as a mechanism of primary resistance to BRAF inhibitors. Cell Rep. 8, 1037–1048 (2014).
Bantscheff, M. et al. Quantitative chemical proteomics reveals mechanisms of action of clinical ABL kinase inhibitors. Nat. Biotechnol. 25, 1035–1044 (2007).
Daub, H. et al. Kinase-selective enrichment enables quantitative phosphoproteomics of the kinome across the cell cycle. Mol. Cell 31, 438–448 (2008).
Kubota, K. et al. Sensitive multiplexed analysis of kinase activities and activity-based kinase identification. Nat. Biotechnol. 27, 933–940 (2009).
Nomura, D. K., Dix, M. M. & Cravatt, B. F. Activity-based protein profiling for biochemical pathway discovery in cancer. Nat. Rev. Cancer 10, 630–638 (2010).
Ren, W., Damayanti, N. P., Wang, X. & Irudayaraj, J. M. Kinase phosphorylation monitoring with i-motif DNA cross-linked SERS probes. Chem. Commun. (Camb.) 52, 410–413 (2016).
Anastassiadis, T., Deacon, S. W., Devarajan, K., Ma, H. & Peterson, J. R. Comprehensive assay of kinase catalytic activity reveals features of kinase inhibitor selectivity. Nat. Biotechnol. 29, 1039–1045 (2011).
Houseman, B. T., Huh, J. H., Kron, S. J. & Mrksich, M. Peptide chips for the quantitative evaluation of protein kinase activity. Nat. Biotechnol. 20, 270–274 (2002).
Karaman, M. W. et al. A quantitative analysis of kinase inhibitor selectivity. Nat. Biotechnol. 26, 127–132 (2008).
Fang, C. et al. Integrated microfluidic and imaging platform for a kinase activity radioassay to analyze minute patient cancer samples. Cancer Res. 70, 8299–8308 (2010).
Li, X. et al. The reverse in-gel kinase assay to profile physiological kinase substrates. Nat. Methods 4, 957–962 (2007).
Wu, J., Barbero, R., Vajjhala, S. & O’Connor, S. D. Real-time analysis of enzyme kinetics via micro parallel liquid chromatography. Assay Drug Dev. Technol. 4, 653–660 (2006).
Sanz, A. et al. Analysis of Jak2 catalytic function by peptide microarrays: the role of the JH2 domain and V617F mutation. PLoS ONE 6, e18522 (2011).
Olow, A. et al. An atlas of the human kinome reveals the mutational landscape underlying dysregulated phosphorylation cascades in cancer. Cancer Res. 76, 1733–1745 (2016).
Hornbeck, P. V. et al. PhosphoSitePlus, 2014: mutations, PTMs and recalibrations. Nucleic Acids Res. 43, D512–D520 (2015).
Yang, X. et al. Widespread expansion of protein interaction capabilities by alternative splicing. Cell 164, 805–817 (2016).
Prahallad, A. et al. Unresponsiveness of colon cancer to BRAF(V600E) inhibition through feedback activation of EGFR. Nature 483, 100–103 (2012).
Corcoran, R. B. et al. EGFR-mediated re-activation of MAPK signaling contributes to insensitivity of BRAF mutant colorectal cancers to RAF inhibition with vemurafenib. Cancer Discov. 2, 227–235 (2012).
Yang, H. et al. Antitumor activity of BRAF inhibitor vemurafenib in preclinical models of BRAF-mutant colorectal cancer. Cancer Res. 72, 779–789 (2012).
Van Geel, R. M., Beijnen, J. H., Bernards, R. & Schellens, J. H. Treatment individualization in colorectal cancer. Curr. Colorectal Cancer Rep. 11, 335–344 (2015).
Corcoran, R. B. et al. Combined BRAF, EGFR, and MEK inhibition in patients with BRAF(V600E)-mutant colorectal cancer. Cancer Discov. 8, 428–443 (2018).
Ursem, C., Atreya, C. E. & Van Loon, K. Emerging treatment options for BRAF-mutant colorectal cancer. Gastrointest. Cancer 8, 13–23 (2018).
Bernards, R. A missing link in genotype-directed cancer therapy. Cell 151, 465–468 (2012).
Flaherty, K. T. et al. Combined BRAF and MEK inhibition in melanoma with BRAF V600 mutations. N. Eng. J. Med. 367, 1694–1703 (2012).
Larkin, J. et al. Combined vemurafenib and cobimetinib in BRAF-mutated melanoma. N. Eng. J. Med. 371, 1867–1876 (2014).
Van Allen, E. M. et al. The genetic landscape of clinical resistance to RAF inhibition in metastatic melanoma. Cancer Discov. 4, 94–109 (2014).
Wagle, N. et al. MAP kinase pathway alterations in BRAF-mutant melanoma patients with acquired resistance to combined RAF/MEK inhibition. Cancer Discov. 4, 61–68 (2014).
Cancer Genome Atlas Network. Genomic classification of cutaneous melanoma. Cell 161, 1681–1696 (2015).
Kemper, K. et al. BRAF(V600E) kinase domain duplication identified in therapy-refractory melanoma patient-derived xenografts. Cell Rep. 16, 263–277 (2016).
Johannessen, C. M. et al. COT drives resistance to RAF inhibition through MAP kinase pathway reactivation. Nature 468, 968–972 (2010).
Janne, P. A., Gray, N. & Settleman, J. Factors underlying sensitivity of cancers to small-molecule kinase inhibitors. Nat. Rev. Drug Discov. 8, 709–723 (2009).
Ruiz-Saenz, A. & Moasser, M. M. Targeting HER2 by combination therapies. J. Clin. Oncol. 36, 808–811 (2018).
Cohen, R. L. & Settleman, J. From cancer genomics to precision oncology—tissue’s still an issue. Cell 157, 1509–1514 (2014).
Holohan, C., Van Schaeybroeck, S., Longley, D. B. & Johnston, P. G. Cancer drug resistance: an evolving paradigm. Nat. Rev. Cancer 13, 714–726 (2013).
Brunen, D. et al. TGF-β: an emerging player in drug resistance. Cell Cycle 12, 2960–2968 (2013).
Garnett, M. J. et al. Systematic identification of genomic markers of drug sensitivity in cancer cells. Nature 483, 570–575 (2012).
Kemper, K. et al. Intra- and inter-tumor heterogeneity in a vemurafenib-resistant melanoma patient and derived xenografts. EMBO Mol. Med. 7, 1104–1118 (2015).
Breitinger, H.-G. Drug Synergy—Mechanisms and Methods of Analysis (InTech, 2012).
Chou, T. C. & Talalay, P. Quantitative analysis of dose–effect relationships: the combined effects of multiple drugs or enzyme inhibitors. Adv. Enzyme Regul. 22, 27–55 (1984).
Berenbaum, M. C. Synergy, additivism and antagonism in immunosuppression. A critical review. Clin. Exp. Immunol. 28, 1–18 (1977).
Foucquier, J. & Guedj, M. Analysis of drug combinations: current methodological landscape. Pharmacol. Res. Perspect. 3, e00149 (2015).
Berenbaum, M. C. What is synergy? Pharmacol. Rev. 41, 93–141 (1989).
Bliss, W. L. Early man in western and northwestern Canada. Science 89, 365–366 (1939).
Arao, T. et al. Small in-frame deletion in the epidermal growth factor receptor as a target for ZD6474. Cancer Res. 64, 9101–9104 (2004).
Yang, W. et al. Genomics of Drug Sensitivity in Cancer (GDSC): a resource for therapeutic biomarker discovery in cancer cells. Nucleic Acids Res. 41, D955–D961 (2013).
Daemen, A. et al. Modeling precision treatment of breast cancer. Genome Biol. 14, R110 (2013).
Moasser, M. M., Srethapakdi, M., Sachar, K. S., Kraker, A. J. & Rosen, N. Inhibition of Src kinases by a selective tyrosine kinase inhibitor causes mitotic arrest. Cancer Res. 59, 6145–6152 (1999).
Nazarian, R. et al. Melanomas acquire resistance to B-RAF(V600E) inhibition by RTK or N-RAS upregulation. Nature 468, 973–977 (2010).
Sun, C. et al. Reversible and adaptive resistance to BRAF(V600E) inhibition in melanoma. Nature 508, 118–122 (2014).
Girotti, M. R. et al. Paradox-breaking RAF inhibitors that also target SRC are effective in drug-resistant BRAF mutant melanoma. Cancer Cell 27, 85–96 (2015).
Poulikakos, P. I., Zhang, C., Bollag, G., Shokat, K. M. & Rosen, N. RAF inhibitors transactivate RAF dimers and ERK signalling in cells with wild-type BRAF. Nature 464, 427–430 (2010).
Ahronian, L. G. et al. Clinical acquired resistance to RAF inhibitor combinations in BRAF-mutant colorectal cancer through MAPK pathway alterations. Cancer Discov. 5, 358–367 (2015).
Mori, M., Pan, B. & Coppé, J. P. High-throughput kinase activity mapping (HT-KAM) system: biochemical assay. Nat. Protoc. Exch. https://doi.org/10.1038/protex.2019.029 (2019).
Yau, C., Wolf, D. M. & Coppé, J. P. High-throughput kinase activity mapping (HT-KAM) system: analysis of phospho-catalytic profiles. Nat. Protoc. Exch. https://doi.org/10.1038/protex.2019.030 (2019).
Acknowledgements
We thank E. Chow at the Center for Advanced Technologies at UCSF for technical support with setting up the liquid assay automation, as well as T. Kuwayama, S. Ortiz-Urda, A. Daud, L. Brown-Swigart, N. Koemans, C. van der Borden, J. Zhu, N. Choy and L. Sean for operational support, and C. Atreya for constructive feedback. This work was supported by grants from the US National Institute of Health (NIH U54CA209891, NIH TR000005 T1 Catalyst Award to J.-P.C. and NIH R01CA122216 to M.M.M.), Give Breast Cancer The Boot programme (to J.-P.C.), Friends for an Earlier Breast Cancer Test programme (to J.-P.C.), Tri-Valley SOCKs (to J.-P.C.), Natural Science Foundation of China (grant number 81001183 to B.P.), Dutch Cancer Society (KWF to R.B., and NKI-2013–5799 to D.S.P. and K.K.), Breast Cancer Research Foundation (to L.J.v.‘tV.), and Angela and Shu Kai Chan Endowed Chair (to L.J.v.‘tV.).
Author information
Authors and Affiliations
Contributions
J.-P.C. conceptualized the kinase activity screening system and supervised the study. M.M. automated the assay procedure. M.M., B.P., A.R.-S., D.B., A.P., P.C.-S., K.K., C.W. and C.A.D. generated the experimental samples and acquired the data. C.P. generated the clinical samples from melanoma patients. P.C.-S., K.K., O.K. and D.S.P. ran the melanoma PDXs and PDX-derived cell line studies. C.Y., D.M.W., C.W. and C.P. conducted the statistical analysis. Z.C. and J.-P.C. designed the sequences of peptide sensors. M.M., B.P., A.R.-S., K.K., C.A.D., D.S.P., R.B. and J.-P.C. contributed to the experimental designs. J.-P.C., M.M., C.Y., D.M.W., A.R.-S., R.B. and M.M.M. interpreted the results. J.-P.C., C.Y., D.M.W., L.J.v.‘tV., C.P., R.B. and M.M.M. wrote the manuscript. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Integrated supplementary information
Supplementary Figure 1 Origin of peptide sensors, assay repeatability, and comparison of dynamic range to data variability across peptides.
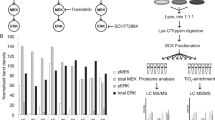
(a) Computational curation established the connectivity between kinase enzymes and their substrate proteins, phosphorylatable target sites, and related peptide sequences 30 (http://cancer.ucsf.edu/phosphoatlas; DOI: 10.1158/0008-5472.CAN-15-2325-T; US20120296880). (b) Projection of the coverage of biological peptides and generic positive control peptides per kinase. Generic CON+ peptides were systematically gathered from commonly available/advertised single-probe kinase assays/screens. (c) Schematic of the procedure. Details of the 228-peptide library we generated and used are available in Supplementary Tables 1–4. (d) Run-to-run comparison of kinases’ peptide-phosphorylation profiles demonstrating repeatability. (e-f) Example of JAK2’s peptide-phosphorylation signature. Four independent runs are analyzed. ‘Raw’ luminescence readouts are compared in (e) and Supplementary Table 5. Results transformed as internally normalized data by centering ATP-consumption profiles against the mean activity across all-228 peptides within each experiment, are shown in (f) and compared in Supplementary Table 6. The stacked bar graph in (f) shows that ATP-consumption profiles (y-axis) follow similar trends for each peptide probe (x-axis) across all runs: most bars follow the same activity trend of either “all medium” (around ‘0’, i.e. close to each experimental mean activity), or “all-high”, or “all-low”, for any individual peptide. This demonstrates run-to-run reproducibility, data consistency, and supports good correlation (>0.9) between experiments (see (d) and Supplementary Table 6). (g) Cumulative bar plots for other recombinant kinases we tested. Profiles support assay repeatability (within graphs) and kinases’ activity signature specificity/discernibility (between graphs; visually displayed in Fig. 1a). (h) Plot merging all kinase profiles from all experiments. (i-j) Dilution and time course validation. Commonly used generic CON+ peptides were interrogated to assess HT-KAM’s output for a set of kinases. Profiles match quality standards in the field. In (j): n≥3 biologically independent sample experiments per kinase; two-sided student t-test; box plot length: 25% and 75% of data, center line: median, whiskers 25% - (or 75% +) 1.5 x IQR). (k) Heatmaps of the top-20 peptides associated with highest measurable activities per kinase. For ~75% of kinases, biological peptides perform as better sensors of kinases’ activity than currently available/advertised CON+ peptides. (l) Comparisons of FDR-corrected t-test (top) and Z-factor profiles (bottom) across top activity-reporting peptides per peptide category. Results in (k-l) show that for many kinases, their best generic CON+ peptides have a good but not optimal ability to report on their enzymatic activity; performance is improved when using/including biological peptides; peptide sequences derived from biological substrate proteins are well suited to measure the phosphorylation activity of kinases.
Supplementary Figure 2 Including a multiplicity of peptide sensors considerably improves the performance of any enzyme activity assay designed to best differentiate and identify kinases.
(a-b) Profiles of AUC values calculated for increasing numbers of randomized combinations of peptide sensors (1 to 50 in (a); 1 to 100 in (b)). (c-e) Kinase phosphorylation activity measured with single generic CON+ peptides. In (c), activity levels compare what is ‘expected’ from advertised single-peptide assays (top panel), to what is experimentally measured (bottom panel; excerpt from kinases’ 228-peptide phospho-activity profiles). In principle, one may expect that the top red/blue kinase-peptide intersections would match the bottom ‘redder’/‘bluer’ patterns. In (d), percent concordances between expected and experimental activities are shown (average 52%). Kinases/peptides ‘cross-reactivity’ observed in (c-d) indicates that no single generic CON+ peptide would allow to accurately identify and differentiate a particular kinase from other kinases. In (e), we calculated the single-peptide AUC values of the 14 generic CON+ peptides to evaluate how specific/sensitive they are at identifying their respective kinases. The bottom panel displays AUCs for 14 individual biological peptides with highest measurable AUC for each kinase. Most single generic CON+ peptides do not provide highest possible specificity/sensitivity for kinases they are expected to report on. Single biological peptides vastly outperform single generic CON+ peptides. Although this does not undermine the utility of single generic CON+ peptide-based assays for pharmaceutical screens, this underlines why a multi-peptide approach is a valuable alternative to single-peptide measurements when investigators want to specifically and differentially identify a kinase from others. (f) ROC curves and AUC values of phospho-catalytic activity profiles established with distinct peptide sets: kinases’ biological peptides, kinases’ generic CON+ peptides, random peptides. (g-i) Combinatorial peptide sets that best differentiate between enzymatic signatures of kinases. Differential signatures (g-h) and their AUCs (i) were computed. The differential signatures of EGFR and SRC included 42 and 43 peptides (AUC’s: 0.840, 0.893) and passed p<0.05 for FDR-corrected t-test or Wilcoxon rank sum test (but not both concurrently). (j) AUCs measured with all-biological, all-positive, all-random, or all-differential peptide sets across all kinases/kinase families. The specificity/sensitivity provided by biological peptide subsets performed almost to the same degree as differential peptide pools, and significantly outperformed generic CON+ peptides. In the perspective of expanding the coverage of the platform to monitor more/other kinases, the computational analyses and modeled data in (a-b,f-j) and Fig. 1c–f demonstrate that including additional peptide probes (especially biological peptides) would only increase the capability of the HT-KAM-screen to accurately predict the identity of more/different kinases using their phospho-catalytic signatures.
Supplementary Figure 3 The phosphorylation activities of kinases measured with biological peptides derived from phosphorylatable substrate protein regions, are significantly higher than activity levels detected with control peptides.
(a) Activity profiles of recombinant kinases measured in presence of their respective biological peptide subsets. Individual peptide-phosphorylation activities measured with kinases’ biological peptides are significantly greater than activities measured with the 63-reference peptide set (27.2%: p≤0.01; 66.7%: p≤0.05), and >94% are greater than activities measured with the 5-random peptide set. The multi-peptide activity profiles of kinases measured with kinases’ biological peptide subsets are significantly different from profiles measured with the control set of 63-reference peptides (p<7E-11 for AKT1, AKT3, MAPK1/ERK2, FYNA, HCK, LYNA, ABL1, and JAK2; p<4E-2 for AKT2, MAPK14/p38a, BLK, BRK, LCK, LYNB, SRC, HER2, HER4; Supplementary Table 9). (b) Pairwise comparison of differences in levels of kinase activities measured in presence of biological peptides versus modified counterparts (results derived from all experimental readouts). (c-d) Overall comparison of activity profiles of Tyrosine Kinases or Serine/Threonine Kinases measured in presence of any of their predicted Y- or S/T- containing biological peptides, versus any Y- or S/T- free biological or reference peptides (see Supplementary Tables 11-12). Results in (a-d) show that kinases are significantly more capable of phosphorylating a vast majority of their biological peptides than control reference peptides, including mutated or pre-phosphorylated biological peptides (box plot length: 25% and 75% of data, center line: median, whiskers 25% - (or 75% +) 1.5 x IQR). As well, since (i) AUCs of kinase activity profiles calculated in Figs. 1d, 2d and Supplementary Fig. 2f, j show that kinases’ subsets of biological peptides systematically provide excellent specificity/sensitivity to identify kinases; and since (ii) computational analyses in Fig. 1e and Supplementary Fig. 2g, h show that the majority of peptides most capable of predictably discerning kinases’ unique and differential phospho-catalytic activities are biological peptides; and since (iii) our strategy utilizes peptide collections that inherently encompass a wide spectrum of biological peptide sensors that correspond to distinct peptide combinations specific to each individual kinase (owing kinases’ essentially exclusive pools of substrate proteins and phospho-target sites; as defined in PhosphoAtlas 30 (http://cancer.ucsf.edu/phosphoatlas) and represented in Supplementary Fig. 1b); then our findings collectively establish that libraries of biological peptides and control peptides are effective combinatorial sensors to functionally differentiate kinases from each other, and that the biological peptide subsets of kinases can reasonably be used to measure kinases’ enzymatic activity.
Supplementary Figure 4 Using HT-KAM as a discovery platform to identify best targets of kinases, establishes that biological peptides are systematically found as reporters of the most significantly high activity profiles of their respective kinases.
(a) Binary heatmap of peptides associated with most significantly high/low activity per kinase. Computational processes and statistical cut-offs comparing levels of ATP consumption per individual peptide to the pool of reference peptides for each kinase are described in Methods. This stringent selection finds 110 biological peptides act as robust sensors of kinases’ catalytic activities. (b) Analysis of activity profiles established in presence of inhibitors (n=3 per treatment condition). Here, the underlying postulate is that, when the activity of a kinase is measured in presence of an inhibitor, any peptide associated with a significant decrease in activity may be considered as a suitable sensor to detect the activity of this kinase. Results would assess the utility and reliability of kinases’ biological peptide targets and peptides defined in (a). For instance, for ABL1, quadrant A shows a strong correlation between levels of inhibition (y-axis; Pearson correlation coefficient between imatinib concentration and ATP consumption for each peptide), and the activity level per peptide in an untreated context (x-axis) (R2(Fisher(inhibition), activity)=-0.48; p=2.75e-14). Critically, peptides that report higher ABL1 activity levels (i.e. dots located toward the right-end of the x-axis, indicating highest ATP consumption) exhibit greater activity inhibition in presence of increasing concentrations of imatinib (i.e. dots located toward the bottom-end of the y-axis, indicating strongest negative correlation and thus strongest inhibition). These peptides largely overlap with peptides found in (a) (i.e. red dots located in the bottom-right area in quadrant A), and include ABL1’s biological peptides JUN Y170, CDK5 Y15, WASL Y256 or BTK Y223, confirming that ABL1 phosphorylation of its substrates is targetable by anti-ABL1 therapy. This analysis also finds that the other biological peptides of ABL1 (i.e. TP73 Y99, JAK2 Y1007, MAP4K1 Y232, ABL1 Y226, CDKN1B Y88, MDM2 Y394, RAD51 Y54; see Fig. 3a) are systematically and significantly associated with ABL1 kinase activity and measurable response to ABL1-inhibitors. This is further validated with results from dasatinib-treated ABL1 (quadrant B). The same logic applies to LYNA (quadrant C), and can be applied to any kinase, peptide set, and drug. (c-d) Comparison of most repeatable peptide-derived activities of ABL1 (x-axis; defined in (a)) to the spectrum of activities established from ABL1’s differential signature (y-axis; defined in Supplementary Fig. 2g–i). Areas (i)/(ii) in (c) and (d) match. Red-filled/outlined markers correspond to biological peptides of ABL1. Noticeably, all ABL1 biological peptides report on high ABL1 activity (top right corner in (c)). Peptides associated with significantly low ABL1 activity correspond to biological peptides of Ser/Thr-kinases (listed in (d)). This directly supports why libraries combining ‘disparate’ biological peptides are inherently good discriminators and identifiers of different kinases. (e-f) Venn diagrams intersecting results from analysis in (a) (robustness of peptide-phosphorylation activities) and in Fig. 1e, f and Supplementary Fig. 2h-i (most differential peptide activities). Results similar to ABL1 in (e) are found for the other kinases we tested (e.g. AKT1 in (f)). In all cases, biological peptides act as robust sensors of the differential and individual/specific phospho-catalytic activity signatures of kinases. (g) Comparing phospho-catalytic profiles of AKT1 versus AKT2. Activity differences are more significantly measurable with biological peptides than generic CON+ peptides, also revealing exploitable differences (e.g. AKT2-signaling networks). Based on results obtained from computational methods we developed and combinatorial peptide library system we designed to showcase our strategy, one valuable application of the HT-KAM approach is to serve as a discovery platform to find new biological substrates and signaling relationships to generate testable hypotheses and explore uncharted druggable pathways.
Supplementary Figure 5 Measuring the effects of kinase inhibitors using biological peptides.
(a-d) Methods evaluating the performance of biological peptides as sensors of kinases’ functionality based on effects of kinase-targeting drugs (3 independent replicates of each of the 8 different conditions for each kinase). In (a), all 228-peptide-activity signatures were first normalized against average activity level measured in the 14 peptide-free control wells, and then individual peptide activities were compared to levels measured in untreated sample (i.e. all activities from all peptides in untreated condition become the baseline ‘0’ value, as shown in the ‘untreated’ column; Student t-test). Data used to plot Fig. 3b. In (b), the 228-peptide activity profiles of imatinib- or dasatinib-treated ABL1T315I are investigated following methods explained in Supplementary Fig. 4b. To systematically cross-compare the relative drug sensitivities of kinases, the mean correlation coefficient (R2) relating ATP-consumption to drug concentration can be calculated using peptides associated with kinases’ highest catalytic activity (which includes biological peptides; red dots in Supplementary Fig. 4b, 5b). To more formally compare drug inhibition levels measured with peptides from the high-activity group to those from the 63-reference peptide group (red vs. blue dots in Supplementary Fig. 4b, 5b), a t-test (p-val) to the Fisher-transformed correlation coefficients calculated for each peptide from each group can be applied. For instance, imatinib inhibits the activity of ABL1 (mean(R2)=-0.847, SD(R2)=0.111, p=0.00252) a lot more than LYNA (mean(R2)=-0.462, SD(R2)=0.49, p=2.054e-06), and has no effect on ABL1T315I (mean(R2)=+0.66; SD(R2)=0.025, p=0.027), which relates to the failure of imatinib-therapy to treat chronic myeloid leukemia (CML) patients with an ABL1T315I-gatekeeper mutation that drives drug-resistance. Our analyses also show dasatinib inhibits significantly more ABL1 (mean(R2)=-0.997, SD(R2)=0.003, p=1.087e-07) than LYNA (mean(R2)=-0.766, SD(R2)=0.21, p=3.081e-06), and has some-limited-yet-measurable dampening effect on ABL1T315I (mean(R2)=-0.33, SD(R2)= 0.09, p=0.41). These analyses also define that dasatinib is a more potent drug than imatinib for these kinases. In (c), ATP-consumption levels measured in presence of peptides most robustly associated with high activity of ABL1 (established in Supplementary Fig. 4a, d) are analyzed. Results validate the gradually inhibited activity profiles found in (a) and Supplementary Fig. 4b. Box plot length: 25% and 75% of data, center line: median, whiskers 25% - (or 75% +) 1.5 x IQR. In (d), heatmaps show average levels of kinases’ activities calculated across their biological peptide subset (individual peptide levels available in Fig. 3a) or 63-reference peptide set. (e-f) Measuring the effects of SFK-inhibitors using SFK’s biological peptides as sensors of drug response (same method as in (a); 3 independent replicates of each of the different conditions for each kinase; ave+/-Stdev). In (e), activities of FYNA, HCK, LCK, and SRC treated with PP2 or SU6656 define their differential drug sensitivities (overall corroborated by previously reported IC50 ranges). In (f), HCK activities are monitored across SU6656 dilutions. Results show that biological peptides of SRC kinases are adequate sensors to monitor the effects of SRC kinase inhibitors.
Supplementary Figure 6 Peptide-phosphorylation signatures and kinase activity profiles of cancer cells in their native and drug-treated states: method validation and technical controls.
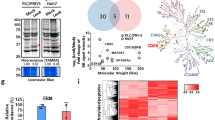
(a) Schematic of the procedure. (b) ATP and protein concentrations in WiDr extracts (ave+/-StDev). (c) Control western blots for MEK1/2, ERK1/2 and EGFR in WiDr (representative of n=4). (d) Comparing activity levels deconvoluted from kinases’ biological peptide subsets (x-axis) versus differential peptide sets identified in Fig. 1e–g and Supplementary Fig. 2g-i (y-axis) and using different normalization methods led to similar outputs (linear regression trend line; Pearson correlation). (e) Differential phosphorylation levels of biological peptides and their relationship to pathways. (f) Comparing changes in kinases’ phospho-catalytic activity (y-axis) measured with either kinases’ generic CON+ peptides (triangles), or biological peptide subsets (circles), or differential peptide subsets (squares), versus differences in phospho-protein levels monitored by western blot (x-axis). Activities established with kinases’ biological or differential peptide sets correlate with protein levels (top right quadrant: EGFR, AKT1, PDPK1, SGK1, PRKCA, PKN1/2; bottom left quadrant: MEK1, ERK2, p38a, GSK3B, RPS6KA), but not when using generic CON+ peptides (top left and bottom right quadrants; e.g. ERK2 and EGFR kinases). This validates Fig. 4a–c. Normalization: 228 peptides + 14 peptide-free readouts; n.a.: not available. (g) Western blot controls (WiDr). (h) Complementary validation of some kinase activity changes found by HT-KAM, using immuno-detection assessing protein phosphorylation levels for substrate protein targets of kinases. When available/tested, results in LIM2405 are shown alongside WiDr (representative of n=2). (i) Western blot controls (LIM2405) (n=1). (j) Summary of druggable kinases found by HT-KAM in VEM-treated BRAFV600E CRC cells. (k) ATP levels in peptide-free wells per cell line. (l-m) Cancer cells kinase activity profiles. Activities were averaged from phosphorylation activities measured with their biological peptides (panel l; for kinases with ≥3 biological peptides), versus generic CON+ peptides (panel m; any number of peptide(s) per kinase). In (m), the ‘blocky’ aspect of the heatmap and compressed differences between and within clusters indicate the signatures of many cells (and kinases) are only minimally distinguishable and display limited specificity, thus contrasting with profiles derived from biological peptides (visibly lost hierarchies in (l); see the more ‘extremely’ highly correlated or uncorrelated heatmaps and histograms in Fig. 5f). (n) Side-by-side comparison of kinase activity versus drug sensitivity in A375 (MEL) and WiDr (CRC) cells, which are respectively BRAF-therapy sensitive and resistant. (o-p) Western blot validation (representative of n=3) and baseline ATP/protein concentration controls (ave+/-StDev).
Supplementary Figure 7 Characterizing the phospho-catalytic signatures of melanoma tumors is relevant for patient diagnostic and treatment guidance.
(a) Schematic of the procedure. (b) Baseline ATP levels measured between experiments and tumors. (c) Unsupervised hierarchical clustering of peptide phosphorylation signatures of nine patient tumor biospecimens, tested in four independent replicates, and measured across 228 peptides. (d) Peptide phosphorylation profiles using top-25%-most-differential activities (alternative threshold-selection method complementing Fig. 6c, d). The related differential activities per peptide comparing specific patient groups are available in Supplementary Table 21. Results in (d) and Fig. 6c, d show that most significant and consistently high signals associated with fatal outcome were measured with biological peptides SMAD2 S465/S245/S250, KHDRBS1 Y440/Y435, MTOR T2446/S2448, CDKN1A T145/S146, BRCA1 S988/T509, ABL1 Y226 (i.e. Y245 in another ABL1 isoform), FCGR2B Y292, CHEK1 S280. Peptides displaying consistently low activity in fatal outcome patient tumors were biological peptides NOTCH2 S2070, JUN Y170, TERT Y707, GAB1 Y627, or reference/modified biological peptides PA_128, PA_134, PA_230. Poor outcome-associated high-activity signatures included peptides related to kinases such as MTOR, SFKs, or TGFBR-signaling, some of which conferred acquired resistance to BRAF-/MEK-inhibitors in melanoma cell lines 45,64-66. Activities measured with peptides of related amino-acid sequences behaved similarly, serving as internal controls validating repeatability (e.g. MTOR T2446/S2448; CDKN1A T145/S146; CDK5 Y15 and CON+ PA_240 derived from CDK1 Y15 conserved phospho-site). Thus, peptides can be used as robust phosphorylation activity sensors to generate clinically valuable signatures. (e) Kinase signature of tumors. (f) Waterfall plot showing kinases’ differential activities between patient groups. Some kinase activities identified by HT-KAM in (e-f) are corroborated by a gene over-expression study of RAF-inhibitor resistance in a melanoma cell line model 45, including upregulation of PRKCE, cRAF, MAP3K8/COT1 or PAK1, although the activity of these kinases were not as highly and significantly upregulated as PIM, RPS6KB or AKT in poor outcome/VEM-resistant patient tumors. (g) Comparing ABL1, AKT1, ERK2, p38a, HCK activities deconvoluted from kinases’ biological peptide subsets (x-axis) versus derived from kinases’ differential peptide sets (y-axis; peptides identified in Supplementary Fig. 2g–i) across different patient groups. Good concordance further validates our strategy. (h) Differential biological peptide-phosphorylation activity profiles complementing Fig. 7b. Results in (e-h) and Fig. 7a, b demonstrate that HT-KAM can measure differences in kinases’ activities (i) within a tumor biospecimen (i.e. for each patient), (ii) between different tumors (i.e. different patients), (iii) between different patient groups (e.g. outcome), which can reveal significantly hyperactive kinases predictive of survival, and identify druggable kinase vulnerabilities most tractable to treat patients unresponsive to BRAF-therapy and with highest likelihood of recurrence.
Supplementary Figure 8 Responses to combinatorial drug treatments in BRAFV600E melanoma cells validate HT-KAM-generated phospho-catalytic signatures, and initiate the translation of kinase hits into novel therapeutic opportunities.
We tested whether some of the kinases found as differentially active by HT-KAM screen in patient tumors (Fig. 7, Supplementary Fig. 7e–h) revealed druggable vulnerabilities capable of potentiating the response of BRAFV600E melanoma cell models to BRAF-targeted therapy. (a) Maps of cell growth responses (left) and combination indices (right) for A375 and Sk-Mel-28 maintained in 0.25% FBS. See Fig. 8a legend for details. (n≥3). (b-d) Evaluating drug combination effects on melanoma cell death. Fluorescence-Activated Cell Sorting (FACS) was used to measure cell death, as exemplified in (b) (n=1 per treatment condition). Graphs in (c-d) show percentages of apoptosis for Sk-Mel-28 and A375 (averages measured in 5% or 0.25% FBS conditions at GI50 concentrations of drugs). Numbers above grey bars indicate the percentage gain (+) or loss (-) in apoptosis when combining VEM with a 2nd kinase-targeting drug. (e) Response to VEM + 2nd kinase-targeting drug in six melanoma cell models maintained in 0.25% FBS media and measured at their respective GI50, GI50x2, and GI50x0.5 concentrations. See Fig. 8d for details. (n≥3). (f-h) Evaluating whether A375 cells expressing a constitutively active AKT1 oncogenic kinase remain sensitive to RPS6KB- or PIM-targeting. Control for myrAKT1 expression is shown in (f) (n=2). A375 myrAKT1 cell growth responses to drug treatments in both 5% and 0.25% FBS culture conditions are shown in (g), and cell death in (h). A375 myrAKT1 cells are less sensitive to VEM than their control counterpart (65% increase in GI50; p=2.77E-06, two-sided paired Student t-test). (i-k) The phospho-RPS6KB profiles of two patient-derived xenografts (PDXs) tumors and derived primary cell lines, as well as their sensitivity to RPS6KB-inhibitor PF-4708671 in 3-week colony formation assays are respectively shown in panels (i-k) (n=1). The PDX tumor M032R6.X1 and derived M032R6.X1.CL line display high levels of RPS6KB1 and is sensitive to RPS6KB1 targeting. Conversely, the PDX tumor M061R.X1 and derived M061R.X1.CL line display low levels of RPS6KB1 and don’t respond to RPS6KB1 targeting. Hence, targeting RPS6KB can be a successful therapeutic intervention in BRAFV600E melanoma tumors/tumor cells where RPS6KB1 is elevated. Such vulnerability may be valuable to restore therapeutic sensitivity in patients who do not respond to, or relapse from, current therapies.
Supplementary Figure 9 Unprocessed blots from key western blots from main Figs. 7e, 8f.
AKT, PIM and PRPS6KB protein levels in the 36 BRAF-therapy resistant PDXs (n=1 per PDX).
Supplementary information
Supplementary Information
Supplementary Figures 1–9, Supplementary table titles and legends.
Supplementary Table 1
List of the 228 peptides used in the assay.
Supplementary Table 2
Numerical-/colour-coded connectivity used in Supplementary Table 1.
Supplementary Table 3
Biological peptide/kinase connectivity.
Supplementary Table 4
Content of each 384-well assay plate.
Supplementary Table 5
Pearson correlation coefficient comparing ATP profiles across experimental runs for JAK2 kinase.
Supplementary Table 6
Pearson correlation coefficient comparing mean-centred ATP profiles across experimental runs for JAK2 kinase.
Supplementary Table 7
List of kinases whose activities are expected to be measured with the generic positive control peptides included in the assay.
Supplementary Table 8
Phospho-catalytic activity levels for each of the recombinant kinases measured with the 14 generic positive control peptides.
Supplementary Table 9
Table of significance comparing the phosphorylation activity profiles of kinases measured with their biological peptide subsets versus ‘control’ peptide groups (that is, random, or Y/S/T free, or reference).
Supplementary Table 10
Detailed list of 151 biological peptides corresponding to the unsupervised hierarchical clustering of kinases’ signatures.
Supplementary Table 11
Tables comparing the activity profiles of tested recombinant tyrosine kinases or serine/threonine kinases measured in the presence of any biological and CON+ peptides that contain phosphorylatable Y/S/T amino acids, versus other subsets of peptides containing or not phosphorylatable Y/S/T amino acids.
Supplementary Table 12
Tables comparing the activity profiles of tested recombinant tyrosine kinases or serine/threonine kinases measured in the presence of their biological peptide targets (that is, containing phosphorylatable Y/S/T amino acids) versus other subsets of peptides that do not contain phosphorylatable Y/S/T amino acids (whether corresponding to reference peptides, or of biological origin).
Supplementary Table 13
Table of IC50 concentrations of imatinib, dasatinib and staurosporine for ABL1, ABL1T315I, LYN A and AKT1 kinases.
Supplementary Table 14
Summary table listing the kinase-targeting drugs and BRAFV600E cell lines that we tested to validate kinase hits identified by HT-KAM profiling.
Supplementary Table 15
Protein concentrations in cell extracts.
Supplementary Table 16
Table of correlations comparing kinase activity (measured with their biological peptide subsets) and drug sensitivity across cancer cell lines.
Supplementary Table 17
Comparison of kinase activity versus drug sensitivity of cancer cells based on kinase activity signatures established with kinases’ generic positive control peptide subsets.
Supplementary Table 18
Melanoma biospecimens: table describing clinical details and treatments received by melanoma patients before and after biopsy from which the excised biospecimens were tested on the HT-KAM platform and retrospectively analysed.
Supplementary Table 19
Protein concentrations of tumour tissue extracts.
Supplementary Table 20
Subset of peptide probes that identify the predictive phospho-catalytic signatures of patients with poor survival outcome, including BRAFV600E-mutated patients resistant to BRAF therapy.
Supplementary Table 21
Differential peptide phosphorylation activities measured with the top 25% most variable peptides between patient groups.
Supplementary Table 22
Table of kinases whose biological peptides are significantly represented among the most differential peptides associated with survival outcome.
Supplementary Table 23
Gene expression profile across melanoma PDXs.
Supplementary Table 24
Characteristics of drug combination effects.
Supplementary Table 25
Combinatorial drug treatments ranked by their levels of synergistic/additive/antagonistic effects established from CI values.
Supplementary Table 26
Statistics source data.
Rights and permissions
About this article
Cite this article
Coppé, JP., Mori, M., Pan, B. et al. Mapping phospho-catalytic dependencies of therapy-resistant tumours reveals actionable vulnerabilities. Nat Cell Biol 21, 778–790 (2019). https://doi.org/10.1038/s41556-019-0328-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41556-019-0328-z
This article is cited by
-
The therapeutically actionable long non-coding RNA ‘T-RECS’ is essential to cancer cells’ survival in NRAS/MAPK-driven melanoma
Molecular Cancer (2024)
-
AXL activates YAP through the EGFR–LATS1/2 axis and confers resistance to EGFR-targeted drugs in head and neck squamous cell carcinoma
Oncogene (2023)
-
A reversible SRC-relayed COX2 inflammatory program drives resistance to BRAF and EGFR inhibition in BRAFV600E colorectal tumors
Nature Cancer (2023)
-
Transcriptomic datasets of cancer patients treated with immune-checkpoint inhibitors: a systematic review
Journal of Translational Medicine (2022)
-
An ultrasensitive fiveplex activity assay for cellular kinases
Scientific Reports (2019)