Abstract
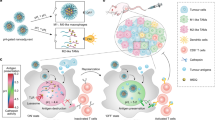
Cancer immunotherapies, particularly therapeutic vaccination, do not typically generate robust anti-tumour immune responses. Here, we show that the intratumoral burst release of the protein annexin A5 from intravenously injected hollow mesoporous nanoparticles made of diselenide-bridged organosilica generates robust anti-tumour immunity by exploiting the capacity of primary tumours to act as antigen depots. Annexin A5 blocks immunosuppressive apoptosis and promotes immunostimulatory secondary necrosis by binding to the phagocytic marker phosphatidylserine on dying tumour cells. In mice bearing large established tumours, the burst release of annexin A5 owing to diselenide-bond cleavage under the oxidizing conditions of the tumour microenvironment and the reducing intracellular conditions of tumour cells induced systemic cytotoxic T-cell responses and immunological memory associated with tumour regression and the prevention of relapse, and led to complete tumour eradication in about 50% of mice with orthotopic breast tumours. Reducing apoptosis signalling via in situ vaccination could be a versatile strategy for the generation of adaptive anti-tumour immune responses.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Data availability
The main data supporting the results in this study are available within the paper and its Supplementary Information. All data generated in this study, including source data and the data used to make the figures, are available from figshare with the identifier https://doi.org/10.6084/m9.figshare.12417110.v1.
References
Ying, Z. et al. A safe and potent anti-CD19 CAR T cell therapy. Nat. Med. 1, 947–953 (2019).
Rafiq, S. et al. Targeted delivery of a PD-1-blocking scFv by CAR-T cells enhances anti-tumour efficacy in vivo. Nat. Biotechnol. 36, 847–856 (2018).
Chen, Q. et al. In situ sprayed bioresponsive immunotherapeutic gel for post-surgical cancer treatment. Nat. Nanotechnol. 14, 89–97 (2019).
Wang, C. et al. In situ activation of platelets with checkpoint inhibitors for post-surgical cancer immunotherapy. Nat. Biomed. Eng. 1, 0011 (2017).
Gao, S. et al. Engineering nanoparticles for targeted remodeling of the tumour microenvironment to improve cancer immunotherapy. Theranostics 9, 126–151 (2019).
Balachandran, V. P. et al. Identification of unique neoantigen qualities in long-term survivors of pancreatic cancer. Nature 551, 512–516 (2017).
Zhang, L. et al. Peptide-based materials for cancer immunotherapy. Theranostics 9, 7807–7825 (2019).
De Palma, M., Biziato, D. & Petrova, T. V. Microenvironmental regulation of tumour angiogenesis. Nat. Rev. Cancer 17, 457–474 (2017).
Smyth, M. J., Ngiow, S. F., Ribas, A. & Teng, M. W. Combination cancer immunotherapies tailored to the tumour microenvironment. Nat. Rev. Clin. Oncol. 13, 143–158 (2016).
Beatty, G. L. & Gladney, W. L. Immune escape mechanisms as a guide for cancer immunotherapy. Clin. Cancer Res. 21, 687–692 (2015).
Lim, S. et al. Recent advances and challenges of repurposing nanoparticle-based drug delivery systems to enhance cancer immunotherapy. Theranostics 9, 7906–7923 (2019).
Guo, C. et al. Therapeutic cancer vaccines: past, present, and future. Adv. Cancer Res. 119, 421–475 (2013).
Wu, G. et al. A Mucin1 C-terminal subunit-directed monoclonal antibody targets overexpressed Mucin1 in breast cancer. Theranostics 8, 78–91 (2018).
Hu, Z., Ott, P. A. & Wu, C. J. Towards personalized, tumour-specific, therapeutic vaccines for cancer. Nat. Rev. Immunol. 18, 168–182 (2018).
Gudkov, A. V. & Komarova, E. A. The role of p53 in determining sensitivity to radiotherapy. Nat. Rev. Cancer 3, 117–129 (2003).
Wu, M. et al. Self-luminescing theranostic nanoreactors with intraparticle relayed energy transfer for tumour microenvironment activated imaging and photodynamic therapy. Theranostics 9, 20–33 (2019).
Johnstone, R. W., Ruefli, A. A. & Lowe, S. W. Apoptosis: a link between cancer genetics and chemotherapy. Cell 108, 153–164 (2002).
Li, M. O., Sarkisian, M. R., Mehal, W. Z., Rakic, P. & Flavell, R. A. Phosphatidylserine receptor is required for clearance of apoptotic cells. Science 302, 1560–1563 (2003).
Yoshida, H. et al. Phosphatidylserine-dependent engulfment by macrophages of nuclei from erythroid precursor cells. Nature 437, 754–758 (2005).
Fadok, V. A. et al. A receptor for phosphatidylserine-specific clearance of apoptotic cells. Nature 405, 85–90 (2000).
Huynh, M.-L. N., Fadok, V. A. & Henson, P. M. Phosphatidylserine-dependent ingestion of apoptotic cells promotes TGF-β1 secretion and the resolution of inflammation. J. Clin. Invest. 109, 41–50 (2002).
Wu, Z., Ma, H. M., Kukita, T., Nakanishi, Y. & Nakanishi, H. Phosphatidylserine-containing liposomes inhibit the differentiation of osteoclasts and trabecular bone loss. J. Immunol. 184, 3191–3201 (2010).
Proskuryakov, S. Y., Gabai, V., Konoplyannikov, A., Zamulaeva, I. & Kolesnikova, A. Immunology of apoptosis and necrosis. Biochemistry 70, 1310–1320 (2005).
Silva, M. T., Do Vale, A. & dos Santos, N. M. Secondary necrosis in multicellular animals: an outcome of apoptosis with pathogenic implications. Apoptosis 13, 463–482 (2008).
Edinger, A. L. & Thompson, C. B. Death by design: apoptosis, necrosis and autophagy. Curr. Opin. Cell Biol. 16, 663–669 (2004).
Ouyang, L. et al. Programmed cell death pathways in cancer: a review of apoptosis, autophagy and programmed necrosis. Cell Prolif. 45, 487–498 (2012).
Krysko, D. V. et al. Immunogenic cell death and DAMPs in cancer therapy. Nat. Rev. Cancer 12, 860–875 (2012).
Davidovich, P., Kearney, C. J. & Martin, S. J. Inflammatory outcomes of apoptosis, necrosis and necroptosis. Biol. Chem. 395, 1163–1171 (2014).
Boersma, H. H. et al. Past, present, and future of annexin A5: from protein discovery to clinical applications. J. Nucl. Med. 46, 2035–2050 (2005).
Narula, J. et al. Annexin-V imaging for noninvasive detection of cardiac allograft rejection. Nat. Med. 7, 1347–1352 (2001).
Logue, S. E., Elgendy, M. & Martin, S. J. Expression, purification and use of recombinant annexin V for the detection of apoptotic cells. Nat. Protoc. 4, 1383–1395 (2009).
van Genderen, H. O. et al. Extracellular annexin A5: functions of phosphatidylserine-binding and two-dimensional crystallization. Biochim. Biophys. Acta 1783, 953–963 (2008).
Schutters, K. & Reutelingsperger, C. Phosphatidylserine targeting for diagnosis and treatment of human diseases. Apoptosis 15, 1072–1082 (2010).
Schlegel, R. & Williamson, P. Phosphatidylserine, a death knell. Cell Death Differ. 8, 551–563 (2001).
Martin, S. et al. Immunologic stimulation of mast cells leads to the reversible exposure of phosphatidylserine in the absence of apoptosis. Int. Arch. Allergy Immunol. 123, 249–258 (2000).
Dillon, S. R., Mancini, M., Rosen, A. & Schlissel, M. S. Annexin V binds to viable B cells and colocalizes with a marker of lipid rafts upon B cell receptor activation. J. Immunol. 164, 1322–1332 (2000).
Kroemer, G. et al. Classification of cell death: recommendations of the Nomenclature Committee on Cell Death 2009. Cell Death Differ. 16, 3–11 (2009).
Frey, B. & Gaipl, U. S. The immune functions of phosphatidylserine in membranes of dying cells and microvesicles. Semin. Immunopathol. 33, 497–516 (2011).
Barroso, G. et al. Mitochondrial membrane potential integrity and plasma membrane translocation of phosphatidylserine as early apoptotic markers: a comparison of two different sperm subpopulations. Fertil. Steril. 85, 149–154 (2006).
Mura, S., Nicolas, J. & Couvreur, P. Stimuli-responsive nanocarriers for drug delivery. Nat. Mater. 12, 991–1003 (2013).
Cheng, C. A. et al. Supramolecular nanomachines as stimuli-responsive gatekeepers on mesoporous silica nanoparticles for antibiotic and cancer drug delivery. Theranostics 9, 3341–3364 (2019).
Brannon-Peppas, L. & Blanchette, J. O. Nanoparticle and targeted systems for cancer therapy. Adv. Drug Deliv. Rev. 64, 206–212 (2012).
Sadauskas, E. et al. Kupffer cells are central in the removal of nanoparticles from the organism. Part. Fibre Toxicol. 4, 10 (2007).
Tavares, A. J. et al. Effect of removing Kupffer cells on nanoparticle tumour delivery. Proc. Natl Acad. Sci. USA 114, E10871–E10880 (2017).
Xu, H., Cao, W. & Zhang, X. Selenium-containing polymers: promising biomaterials for controlled release and enzyme mimics. Acc. Chem. Res. 46, 1647–1658 (2013).
Kim, J. H., Lee, J., Park, J. & Gho, Y. S. Gram-negative and Gram-positive bacterial extracellular vesicles. Semin. Cell Dev. Biol. 40, 97–104 (2015).
Fogh-Andersen, N. et al. Composition of interstitial fluid. Clin. Chem. 41, 1522–1525 (1995).
Hoffmann, P. R. et al. Phosphatidylserine (PS) induces PS receptor–mediated macropinocytosis and promotes clearance of apoptotic cells. J. Cell Biol. 155, 649–659 (2001).
Somersan, S. & Bhardwaj, N. Tethering and tickling: a new role for the phosphatidylserine receptor. J. Cell Biol. 155, 501–504 (2001).
Xu, X. et al. Advances in engineering cells for cancer immunotherapy. Theranostics 9, 7889–7905 (2019).
Kim, O. Y. et al. Immunization with Escherichia coli outer membrane vesicles protects bacteria-induced lethality via Th1 and Th17 cell responses. J. Immunol. 190, 4092–4102 (2013).
Castrillo, A., Joseph, S. B., Marathe, C., Mangelsdorf, D. J. & Tontonoz, P. Liver X receptor-dependent repression of matrix metalloproteinase-9 expression in macrophages. J. Biol. Chem. 278, 10443–10449 (2003).
Inaba, K. et al. Generation of large numbers of dendritic cells from mouse bone marrow cultures supplemented with granulocyte/macrophage colony-stimulating factor. J. Exp. Med. 176, 1693–1702 (1992).
Acknowledgements
This work was supported by the Intramural Research Program of the National Institute of Biomedical Imaging and Bioengineering, National Institutes of Health, the Faculty of Health Sciences, University of Macau, a Start-up Research Grant of the University of Macau (SRG2018-00130-FHS) and the Science and Technology Development Fund (FDCT), Macao SAR (FDCT 0109/2018/A3). We thank V. Schram for help with confocal microscopy imaging, Henry S. Eden for proof-reading the manuscript and Guangzhou Sagene Biotech for help with making the pattern diagrams.
Author information
Authors and Affiliations
Contributions
X.C., L.L., W.F. and Z.Y. conceived the study, designed the experiments and wrote the manuscript. L.L., J.Z., W.F. and Z.Y. performed the experiments and analysed data. Y.D. and G.N. re-evaluated the anti-tumour activity.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary figures.
Rights and permissions
About this article
Cite this article
Li, L., Zou, J., Dai, Y. et al. Burst release of encapsulated annexin A5 in tumours boosts cytotoxic T-cell responses by blocking the phagocytosis of apoptotic cells. Nat Biomed Eng 4, 1102–1116 (2020). https://doi.org/10.1038/s41551-020-0599-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-020-0599-5
This article is cited by
-
Responsive biomaterials: optimizing control of cancer immunotherapy
Nature Reviews Materials (2023)
-
In situ generation of micrometer-sized tumor cell-derived vesicles as autologous cancer vaccines for boosting systemic immune responses
Nature Communications (2022)
-
Cancer nanomedicine
Nature Reviews Cancer (2022)
-
Catalytical nano-immunocomplexes for remote-controlled sono-metabolic checkpoint trimodal cancer therapy
Nature Communications (2022)
-
A hybrid semiconducting organosilica-based O2 nanoeconomizer for on-demand synergistic photothermally boosted radiotherapy
Nature Communications (2021)