Abstract
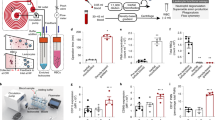
Current methods for the diagnosis of sepsis have insufficient precision, causing regular misdiagnoses. Microbiological tests can help to diagnose sepsis, but are usually too slow to have an impact on timely clinical decision-making. Neutrophils have a high sensitivity to infections, yet measurements of neutrophil surface markers, genomic changes and phenotype alterations have had only a marginal effect on sepsis diagnosis. Here, we report a microfluidic assay that measures, from one droplet of diluted blood, the spontaneous motility of neutrophils in the presence of plasma. We measured the performance of the assay in two independent cohorts of critically ill patients suspected of sepsis. Using data from a first cohort, we developed a machine-learning-based scoring system (sepsis score) that segregated patients with sepsis from those without sepsis. We then validated the sepsis score in a double-blind, prospective case–control study. For the 42 patients across the two cohorts, the assay identified sepsis patients with 97% sensitivity and 98% specificity. The neutrophil assay could potentially be used to accurately diagnose and monitor sepsis in larger populations of at-risk patients.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Vincent, J. L. et al. The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. Intensive Care Med. 22, 707–710 (1996).
Singer, M. et al. The third international consensus definitions for sepsis and septic shock (sepsis-3)J. Am. Med. Assoc. 315, 801–810 (2016).
Sharma, S. & Kumar, A. Antimicrobial management of sepsis and septic shock. Clin. Chest Med. 29, 677–687 (2008).
Kumar, A. et al. Duration of hypotension before initiation of effective antimicrobial therapy is the critical determinant of survival in human septic shock. Crit. Care Med. 34, 1589–1596 (2006).
Pierrakos, C. & Vincent, J.-L. Sepsis biomarkers: a review. Crit. Care 14, R15 (2010).
Liu, Y. et al. Biomarkers for diagnosis of sepsis in patients with systemic inflammatory response syndrome: a systematic review and meta-analysis. SpringerPlus 5, 2091 (2016).
Hsu, K. H., Chan, M. C., Wang, J. M., Lin, L. Y. & Wu, C. L. Comparison of Fcγ receptor expression on neutrophils with procalcitonin for the diagnosis of sepsis in critically ill patients. Respirology 16, 152–160 (2011).
Hassan, U. et al. A point-of-care microfluidic biochip for quantification of CD64 expression from whole blood for sepsis stratification. Nat. Commun. 8, 15949 (2017).
Stubljar, D. & Skvarc, M. Effective strategies for diagnosis of systemic inflammatory response syndrome (SIRS) due to bacterial infection in surgical patients. Infect. Disord. Drug Targets 15, 53–56 (2015).
Bone, R. C. et al. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Chest 101, 1644–1655 (1992).
Brown, K. A. et al. Neutrophils in development of multiple organ failure in sepsis. Lancet 368, 157–169 (2006).
Fazal, N. et al. CINC blockade prevents neutrophil Ca2+ signaling upregulation and gut bacterial translocation in thermal injury. Biochim. Biophys. Acta 1535, 50–59 (2000).
Weiss, S. J. Tissue destruction by neutrophils. N. Engl. J. Med. 320, 365–376 (1989).
Butler, K. L. et al. Burn injury reduces neutrophil directional migration speed in microfluidic devices. PloS ONE 5, e11921 (2010).
Jones, C. N. et al. Spontaneous neutrophil migration patterns during sepsis after major burns. PloS ONE 9, e114509 (2014).
Solomkin, J. S. Neutrophil disorders in burn injury: complement, cytokines, and organ injury. J. Trauma 30, S80–S85 (1990).
Kurihara, T. et al. Resolvin D2 restores neutrophil directionality and improves survival after burns. FASEB J. 27, 2270–2281 (2013).
Hoang, A. N. et al Measuring neutrophil speed and directionality during chemotaxis, directly from a droplet of whole blood. Technology (Singap. World Sci.) 1, 49 (2013).
Simpson, S. Q. Diagnosing sepsis: a step forward, and possibly a step back. Ann. Transl. Med. 5, 55 (2017).
Pepe, M. C. in The Statistical Evaluation of Medical Tests for Classification and Prediction 218–228 (Oxford Univ. Press, Oxford, 2004).
Ambravaneswaran, V., Wong, I. Y., Aranyosi, A. J., Toner, M. & Irimia, D. Directional decisions during neutrophil chemotaxis inside bifurcating channels. Integr. Biol. 2, 639–647 (2010).
Akhundov, A. G. On the problem of toxic granulation of the neutrophils in acute suppurative diseases and sepsis. Klin. Med. (Mosk.) 39, 84–89 (1961).
Povoa, P. C-reactive protein: a valuable marker of sepsis. Intensive Care Med. 28, 235–243 (2002).
Weng, X., Cloutier, G., Beaulieu, R. & Roederer, G. O. Influence of acute-phase proteins on erythrocyte aggregation. Am. J. Physiol. 271, H2346–H2352 (1996).
Gawaz, M., Fateh-Moghadam, S., Pilz, G., Gurland, H. J. & Werdan, K. Platelet activation and interaction with leucocytes in patients with sepsis or multiple organ failure. Eur. J. Clin. Investig. 25, 843–851 (1995).
Mavrommatis, A. C. et al. Coagulation system and platelets are fully activated in uncomplicated sepsis. Crit. Care Med. 28, 451–457 (2000).
Ogura, H. et al. Activated platelets enhance microparticle formation and platelet–leukocyte interaction in severe trauma and sepsis. J. Trauma 50, 801–809 (2001).
Engelmann, B. & Massberg, S. Thrombosis as an intravascular effector of innate immunity. Nat. Rev. Immunol. 13, 34–45 (2013).
Frydman, G. H. et al. Technical advance: changes in neutrophil migration patterns upon contact with platelets in a microfluidic assay. J. Leukoc. Biol. 101, 797–806 (2017).
Jones, C. N. et al. Microfluidic platform for measuring neutrophil chemotaxis from unprocessed whole blood. J. Vis. Exp. 88, e51215 (2014).
Furey, T. S. et al. Support vector machine classification and validation of cancer tissue samples using microarray expression data. Bioinformatics 16, 906–914 (2000).
Suykens, J. A. K. & Vandewalle, J. Least squares support vector machine classifiers. Neural Process. Lett. 9, 293–300 (1999).
Vapnik, V. N. Statistical Learning Theory (ed Haykin, S.) (Wiley, New York, 1998).
Vapnik, V. in Nonlinear Modeling (eds Suykens, J. A. K. & Vandewalle, J.) 55–85 (Springer, Boston, 1998)..
Fan, J., Guo, S. & Hao, N. Variance estimation using refitted cross-validation in ultrahigh dimensional regression. J. R. Stat. Soc. Ser. B, Stat. Methodol. 74, 37–65 (2012).
Varma, S. & Simon, R. Bias in error estimation when using cross-validation for model selection. BMC Bioinformatics 7, 91 (2006).
Van Der Maaten, L. & Hinton, G. Visualizing data using t-SNE. J. Mach. Learn. Res. 9, 2579–2605 (2008).
Acknowledgements
We thank C. Holland and K. Brait for assistance in recruiting patients; M. Toner, H. S. Warren and M. Filbin for thoughtful discussions and advice; and D. Hayden for biostatistics assistance.This project was supported by funding from the National Institutes of Health, National Institute of General Medical Sciences (grant GM092804) and National Institute of Allergy and Infectious Diseases (grant AI113937), and Shriners Hospitals for Children. Biostatistics work was conducted in part with assistance from the Harvard Catalyst program, supported by a grant from the National Center for Advancing Translational Sciences (grant UL1 TR001102). Microfluidic devices were manufactured at the BioMEMS Resource Center at Massachusetts General Hospital, supported by a grant from the National Institute of Biomedical Imaging and Bioengineering (grant EB002503). F.E. was supported by a fellowship from Shriners Hospitals for Children.
Author information
Authors and Affiliations
Contributions
F.E. designed the study, designed and fabricated the microfluidic device, performed experiments, analysed the data and wrote the manuscript. J.J. performed experiments and cell tracking, analysed the data and applied machine-learning approaches to derive the sepsis score. J.J. and A.L.M. performed blood-spiking experiments. M.M.M., Y.M.L. and K.L.B. coordinated collection of patient samples for the first, derivation cohort and provided advice on the study design and manuscript. V.S. and J.L. coordinated collection of samples for the validation cohort and provided advice on the study design and wrote the manuscript. D.I. conceived, designed and supervised the study and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary Information
Supplementary figures, tables and video caption.
Supplementary Video 1
Spontaneous motility of neutrophils in the microfluidic device.
Rights and permissions
About this article
Cite this article
Ellett, F., Jorgensen, J., Marand, A.L. et al. Diagnosis of sepsis from a drop of blood by measurement of spontaneous neutrophil motility in a microfluidic assay. Nat Biomed Eng 2, 207–214 (2018). https://doi.org/10.1038/s41551-018-0208-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41551-018-0208-z
This article is cited by
-
Smartphone-based platforms implementing microfluidic detection with image-based artificial intelligence
Nature Communications (2023)
-
ComplexEye: a multi-lens array microscope for high-throughput embedded immune cell migration analysis
Nature Communications (2023)
-
Micro- and nanosensors for detecting blood pathogens and biomarkers at different points of sepsis care
Microchimica Acta (2022)
-
A microwell-based impedance sensor on an insertable microneedle for real-time in vivo cytokine detection
Microsystems & Nanoengineering (2021)
-
Leukocyte function assessed via serial microlitre sampling of peripheral blood from sepsis patients correlates with disease severity
Nature Biomedical Engineering (2019)