Abstract
Previous works highlighted the relevance of automated language analysis for predicting diagnosis in schizophrenia, but a deeper language-based data-driven investigation of the clinical heterogeneity through the illness course has been generally neglected. Here we used a semiautomated multidimensional linguistic analysis innovatively combined with a machine-driven clustering technique to characterize the speech of 67 individuals with schizophrenia. Clusters were then compared for psychopathological, cognitive, and functional characteristics. We identified two subgroups with distinctive linguistic profiles: one with higher fluency, lower lexical variety but greater use of psychological lexicon; the other with reduced fluency, greater lexical variety but reduced psychological lexicon. The former cluster was associated with lower symptoms and better quality of life, pointing to the existence of specific language profiles, which also show clinically meaningful differences. These findings highlight the importance of considering language disturbances in schizophrenia as multifaceted and approaching them in automated and data-driven ways.
Similar content being viewed by others
Introduction
Language disorders are a core feature of schizophrenia, with more than 70% of individuals showing linguistic and communicative impairments1,2. Disturbances might affect all levels of linguistic processing, from the “building blocks” of language, including speech characteristics, grammatical structures, and lexical components, up to more sophisticated aspects such as pragmatic interpretation3. In particular, schizophrenia has been associated with altered pausing and prosody, reduced grammatical processing skills, diminished lexical richness (e.g., lower type-token ratio), and defective semantic processes4,5,6,7,8. Studies reported also impairment in the ability to manage discourse and conversation, as well as to understand non-literal expressions9,10,11. These linguistic and communicative difficulties show extensive correlations with cognitive aspects1,2 and have been linked to both positive (in particular, formal thought disorder and disorganization) and negative (especially poverty of speech) symptoms4,5,12,13. Furthermore, language disturbances are associated with reduced daily functioning1,14. In particular, among the different domains of daily functioning, language and communication have been shown to impact especially community integration, interpersonal relations, and social functioning at large15,16. Taken together, this evidence makes language a relevant domain of assessment also for clinical purposes.
The last decades witnessed the rise of computational approaches to provide quick and fine-grained quantitative linguistic analysis. Although still not used on the large scale, these methods have already proven successful in different clinical applications on individuals with schizophrenia17,18,19. First, these approaches showed high accuracy levels in distinguishing individuals with schizophrenia from healthy controls20,21 and first-degree relatives22, as well as for differential diagnosis (e.g., schizophrenia vs. bipolar disorder)23. Furthermore, they were successfully applied also for prognostic purposes. In individuals at clinical high risk for psychosis, computational methods were able to predict conversion to psychosis with high levels of accuracy up to 100%24,25,26. Moreover, in individuals at first episode of psychosis, computational approaches were effective in predicting diagnostic outcome up to eighteen months27,28. Indeed, most of the current research in this domain focuses on at-risk individuals and in supporting diagnosis in first-episode psychosis, in line with the idea of linguistic impairment as a potential biomarker of schizophrenia18,19.
However, little research has examined via automated methods the linguistic characteristics exhibited by individuals with a long-term history of schizophrenia. Among the few studies documenting an application of computational methods in chronic schizophrenia, de Boer et al.29,30 showed that automatically extracted speech features (e.g., articulation rate, number and duration of pauses, and mean length of utterance) and lexical features (i.e., type-token ratio) were associated with negative symptoms as well as with the integrity of the white matter in the language tracts. Buck et al.31 used the Linguistic Inquiry and Word Count (LIWC)32 software to distinguish stories produced by patients vs. healthy controls, highlighting especially the correlations between the number of words, symptoms, and sociocognitive skills. Similarly, Minor et al.33 reported that altered use of emotional words extracted via LIWC was related to higher negative symptomatology and lower functioning in schizophrenia. In the same vein, other studies found that individuals with schizophrenia showed less words per sentence and increased use of self-reference pronouns compared to controls21,34, without a difference in lexical variety as measured with the type-token ratio21.
Notably, these studies focused on the associations between automatically-extracted linguistic features and participants’ psychopathological, functional, cognitive, or sociocognitive characteristics, while a deeper machine-driven investigation of the heterogeneity of the linguistic profile of chronic patients has been generally neglected. This is a limitation since individuals with a long history of schizophrenia are greatly heterogenous under several respects35,36,37. For instance, different machine-learning clustering techniques have been successfully applied to decompose the psychopathological heterogeneity of chronic schizophrenia into sub-groups of individuals characterized by different patterns of negative symptomatology38,39. Similarly, clustering algorithms have proven effective in identifying clusters of participants with distinct levels of severity in cognitive and sociocognitive deficits40,41,42. Importantly, these approaches showed that clusters of individuals with different psychopathological and cognitive profiles might have different functional outcomes, as well as different responses to treatment38,43,44. More recently, also speech features were used to automatically identify clusters of patients with different levels of language impairment, which in turn were associated with distinct profiles of cognitive dysfunction45. In this light, data-driven approaches combined with automatically-extracted linguistic features might be key to refine the identification of subtypes of individuals with schizophrenia and obtain more nuanced and sensitive information about psychopathology and its nature, as well as about treatment responsiveness in the long-term illness progression20.
The present study aimed at extending the application of semi-automated linguistic approaches to unravel the clinical heterogeneity of schizophrenia, by innovatively combining computational linguistic methods with data-driven clustering techniques. Specifically, the study objectives were: (i) to identify separate subgroups of individuals with chronic schizophrenia based on a set of (semi-)automatically-extracted linguistic features, targeting the core “building blocks” of the language faculty, and (ii) to test whether the obtained linguistic subtypes are associated with differences at the psychopathological, daily functioning, cognitive, and sociocognitive levels.
To do so, we first developed a multilevel semi-automated linguistic analysis that took into account different linguistic domains described as compromised in schizophrenia4,5,29,31,33, from speech to the lexicon, and then applied a machine-learning unsupervised algorithm to the output variables of the linguistic analysis to identify clusters of participants characterized by distinct linguistic profiles. Clusters were finally compared for psychopathological, cognitive, sociocognitive, and functional aspects. We expected to find evidence of distinct linguistic profiles, and that these might be indicative of underlying psychopathological, cognitive, sociocognitive, and functional differences, consistently with previous studies that emphasised a relationship between linguistic impairment and clinical and functional measures14,29,33 and between language and cognitive and sociocognitive aspects1,31,33.
Results
Sample description
The sample included 67 participants, which were 26 females and 41 males, with a mean age of 39.75 ± 11.04 years and a mean education of 11.94 ± 2.72 years. The mean illness duration was 15.60 ± 10.70 years, with a mean age of onset of 24.28 ± 6.36 years. All participants were treated with antipsychotic therapy for at least 3 months (atypical/typical antipsychotic treatment: 61/6), with a mean Chlorpromazine-equivalent dose of 440.98 ± 200.57 mg/d.
Overview
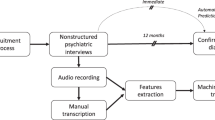
The linguistic features extracted via the semi-automated analysis targeted the following levels: (1) speech, (2) lexical richness, (3) occurrence of specific part-of-speech categories, in particular personal pronouns, and (4) occurrence of selected semantic classes, in particular within the psychological lexicon, as described in details in Table 1. A visual representation of audio file pre-processing and linguistic features extraction is provided in Fig. 1. The results of the analysis are presented in the following three sections, consistently with the three stages of the analysis: (i) the Principal Component Analysis (PCA), used to reduce data dimensionality and to identify Principal Components (PCs) emerging from the automatically extracted linguistic features, namely a smaller number of uncorrelated linguistic-based variables from the larger set of data; (ii) the cluster analysis, which used the linguistic-related variables obtained from the PCA to identify distinct clusters (i.e., sub-groups) of participants, characterized by high intra-class similarity and low inter-class similarity in their linguistic profiles; (iii) the comparison of the sub-groups resulting from the clustering process for clinical, neurocognitive, sociocognitive, and functional characteristics.
Speech samples were obtained via the semi-structured interviews of the APACS test (1), and then transcribed using the CLAN software (2). Afterwards, token-based values were automatically extracted from the transcripts: R Studio was used to automatically obtain lexical frequency values for each token in the text from the Corpus and Frequency Lexicon of Written Italian (CoLFIS) corpus (3a), Natural Language Toolkit (NTLK) was employed to compute the Type-Token ratio (3b), while the Linguistic Inquiry and Word Count (LIWC) software was used to obtain the frequency of affective words and words indicating cognitive mechanisms (i.e., Psychological Lexicon) and Personal Pronouns (3c). Finally, the speech samples were processed using the PRAAT software (4) to determine the number of utterances for the computation of the Mean Length of Utterance, as well as to extract pause and gap duration and the number of pauses, used for the computation of the Pause-to-word ratio.
Principal Component Analysis on linguistic features
The PCA performed on the linguistic features identified n = 4 meaningful PCs (with eigenvalue >1), describing respectively 39.80%, 13.52%, 12.23%, and 11.30%, for a total of 76.85% of data variance. To better characterize the unique contribution of the linguistic features on each PC, we considered only high factor loadings (|>0.50|)46. Lexical Richness features (type-token ratio and lexical frequency) and specific Fluency features (i.e., mean length of utterance, mean gap duration, and mean pause duration), reflecting lexical access and speech planning processes, loaded primarily on PC1. Fluency characteristics related to pauses (i.e., mean pause duration and pause-to-word ratio) loaded also on PC2, which intercepts speech planning and monitoring and speed processing. Frequency of Personal Pronouns loaded exclusively on PC3, while frequency of Psychological Lexicon (i.e., affective and cognitive mechanisms words) loaded selectively on PC4. The correlations between the linguistic features and each PC are shown in Fig. 2A.
A Associations between the four principal components (PCs) identified by the Principal Component Analysis and the linguistic features; green-colored boxes indicate a positive association, while red-colored boxes a negative association. B Silhouette width for participants included in both clusters (horizontal axis) and average silhouette width for the two-cluster solution (red dashed line). C Clusters distribution around centroids.
Cluster Analysis on linguistic-based PCs
The four linguistic-based PCs resulting from the PCA were used to run a cluster analysis using a k-means algorithm. The k-means algorithm identified two distinct clusters (see Supplementary Table 1 for the average silhouette width of different solutions). Figure 2B, C shows the silhouette profile of the two-cluster solution and participants’ distribution between clusters, respectively.
Participants were grouped by the k-means algorithm considering whether they showed higher (↑) or lower (↓) performance across the PCs associated with the different linguistic domains. The algorithm assigned participants to Cluster 1 (n = 47) if their speech was characterized by ↓Lexical Richness, ↑Fluency, ↑Pronouns, and ↑Psychological Lexicon. Conversely, participants were assigned to Cluster 2 (n = 20) if their speech was characterized by ↑Lexical Richness, ↓Fluency, ↓Pronouns, and ↓Psychological Lexicon. Clusters’ centroids are reported in Supplementary Table 2. Examples of participants for each cluster (i.e., excerpts of the transcripts of their interviews and individual data) are reported in Supplementary Tables 4, 5.
Validation of the cluster analysis
The optimal two-cluster solution identified through the k-means algorithm was validated using an independent algorithm by performing a Linear Discriminant Analysis (LDA) with two approaches: (a) a random-split samples procedure (to assess the degree of classification concordance over n = 50 iterations across different partitions), (b) a leave-one-out method.
As for the LDA with random-split samples procedure, with 75% of participants assigned to the training set, the mean training accuracy was 0.96 ± 0.02 and the mean testing accuracy was 0.95 ± 0.05; with 50% of participants randomly assigned to the training set, the mean training accuracy was 0.97 ± 0.02 and the mean testing accuracy was 0.93 ± 0.03; finally, with 25% of participants assigned to training, the mean training accuracy was 0.98 ± 0.03 against a mean testing accuracy of 0.89 ± 0.07. Overall, the algorithm showed a stable performance across training-testing partitions (see Fig. 3A; see Fig. 3B for a conceptual representation of the results of one replication with a 50% training-testing partition).
A Mean values of training and testing accuracy (error bars indicate standard deviations), computed on random samples with 75%, 50%, and 25% of participants of the original sample assigned to the training subset and the remaining to the testing subset (50 iterations performed using the same method). The general performance of the classification function remains high and stable across different training-testing partitions. B Conceptual representation of a replication with 50% of participants randomly assigned to the training subset and the other 50% to the testing subset (training accuracy: 100%; testing accuracy: 97%). The outcome of this single replication shows that in the testing subset only one participant from Cluster 2 is misclassified by the model.
The LDA with leave-one-out cross-validation confirmed the random-split samples procedure, highlighting an almost perfect level of agreement with the cluster solution identified through the k-means algorithm (with 94% of participants correctly assigned to the two clusters, see Supplementary Table 3).
Taken together, these validation methods support the stability of the two-cluster solution over several repetitions.
Cluster comparison
Since all dependent variables were normally distributed and had homogeneous variance, we proceeded to perform a series of t-tests to compare the two clusters. Participants in Cluster 1 and 2 did not differ for age, education, disease duration, age of onset, Chlorpromazine-equivalent dose, type of antipsychotic treatment, neurocognition as evaluated with the Brief Assessment of Cognition in Schizophrenia (BACS), or social cognition as evaluated with the Theory of Mind Picture Sequencing Task (ToM PST) (|ts|≤ 1.66; ps ≥ 0.102). Conversely, the two clusters were significantly different in psychopathology as evaluated with the Positive and Negative Syndrome Scale for Schizophrenia (PANSS) and in daily functioning as evaluated with the Quality of Life Scale (QLS) (Table 2).
In particular, participants in Cluster 1 exhibited higher QLS scores in the Interpersonal Relations (t(64) = 4.05; p < 0.001) and Personal Autonomy (t(64) = 5.17; p < 0.001) subscales, and in the Total (t(64) = 4.91; p < 0.001) score, even though they were not significantly different from participants in Cluster 2 in the Instrumental Role subscale (t(64) = 1.39; p = 0.169) (Fig. 4A). Moreover, participants in Cluster 1 exhibited a less severe symptomatology, as indicated by lower scores in the PANSS Positive (t(65) = −2.31; p = 0.024), Negative (t(65) = −3.14; p = 0.010), and General (t(65) = −2.67; p = 0.019) scales compared to Cluster 2, as well as by a lower score in the Disorganization dimension (t(65) = −2.49; p = 0.021) (Fig. 4B). A comprehensive summary of the linguistic, functional, and psychopathological profile of the two clusters is provided in Fig. 4C.
A Between-cluster comparisons for Quality of Life Scale (QLS), including Interpersonal Relations (IRe), Instrumental Role (IRo), and Personal Autonomy (PA) sub-scales and total score (Tot). B Between-cluster comparisons for PANSS scores (Positive, Negative, and General Scales and Disorganization dimension score). C Summary of the linguistic, psychopathological, and functional differences of the participants belonging to Cluster 1 and Cluster 2 (only significant differences are reported): arrows indicate higher (↑) or lower (↓) linguistic performance, psychopathological symptoms (as evaluated by the scores obtained in the PANSS Positive, Negative, and General scales and Disorganization score), and functioning (as evaluated with the QLS subscales and Total score).
Additional analysis on cognition and social cognition
We furtherly compared clusters across the subtasks of the BACS and the ToM PST, in order to investigate possible differences in cognition and social cognition between the two subgroups in a more fine-grained fashion. The t-tests revealed that the two clusters did not differ for BACS and ToM PST subscores (|ts|≤ 1.38; ps ≥ 0.172) (Table 3).
Then, we exploratively assessed the correlation between the BACS and ToM PST subscores on the one hand and the linguistic-based PCs on the other hand in each cluster separately, to assess patterns of association between participants’ linguistic profile and the other cognitive domains. No significant associations were observed between the linguistic PCs and the cognitive and sociocognitive measures for participants in Cluster 1 (|rs|≤ .21, ps ≥ 0.185) (Fig. 5A). Conversely, Cluster 2 exhibited an overall stronger pattern of correlations between linguistic and cognitive aspects. In particular, the correlations between PC1 scores (i.e., Fluency/Lexical Richness) and BACS Verbal Memory and Tower of London subscores, and between PC3 scores (i.e., Frequency of Personal Pronouns) and BACS Digit Sequencing and Tower of London subscores (Fig. 5B) reached significance. No other robust significant associations between the linguistic-based PCs and the ToM PST subscores were found in Cluster 2.
These data indicate that, although the distribution of cognitive and sociocognitive scores was not different across clusters, in Clusters 2 participants’ the linguistic profile was linked to a greater extent with cognitive characteristics, while in Cluster 1 linguistic and cognitive variables seem to be relatively independent.
Discussion
In this study, we used an innovative multidimensional semi-automated linguistic analysis combined with a data-driven clustering algorithm to identify different linguistic profiles in individuals with schizophrenia and test differences at psychopathological, cognitive, sociocognitive, and functional levels. This method identified two clusters of participants based on their linguistic features, which – in line with our expectations – turned out to show also different patterns of psychopathological, functional, and cognitive characteristics. On the one hand, Cluster 1 – characterized by higher Fluency, higher Frequency of Personal Pronouns, lower Lexical Richness but higher Psychological Lexicon – was associated with lower psychopathological symptomatology and better quality of life; on the other hand, Cluster 2 – characterized by lower Fluency, lower Frequency of Personal Pronouns, higher Lexical Richness but lower Psychological Lexicon – was associated with higher psychopathological symptomatology and worse quality of life. Moreover, relative to Cluster 1, the linguistic profile of participants belonging to Cluster 2 showed a stronger pattern of correlations with the underlying cognitive skills, with lower linguistic scores being associated with poorer cognitive functioning. These findings open up at least three different orders of considerations, concerning (i) the importance of multidimensional language assessment; (ii) the specific associations between linguistic profiles and psychopathological, functional, and cognitive domains; and (iii) the clinical implications and possible developments of this type of approach.
Concerning language assessment, the first aspect to notice is that the linguistic profiles emerged from a multilevel language analysis, spanning from speech characteristics to the occurrences of words in specific semantic classes. The PCA identified four meaningful components that targeted different dimensions, and all of them fed the clustering algorithm, indicating great intergroup variation on all four extracted components, as well as high within group homogeneity. The high number of characteristics which define the linguistic profiles of our participants supports the idea that language and communicative impairments in schizophrenia cover a wide range of phenomena and represent an important source of heterogeneity among individuals3,35.
To examine more in depth the outcome of the linguistic analysis, it is important to comment on the specific clusters of linguistic features that emerged from the automatic classification. Participants belonging to Cluster 1 showed longer utterances and shorter and less numerous pauses and fillers; consistently, functional words such as pronouns were also more numerous; despite the greater fluency, words were globally more common and less various (as indicated by the higher lexical frequency and the lower type-token ratio), yet the occurrence of specific words referring to emotional content or cognitive processes was higher. In short, this cluster includes individuals who are more fluent in their speech (and possibly verbose) and use more psychological terms, but overall exhibit lower lexical variety. The linguistic profile of Cluster 1 confirms previous descriptions of altered type-token ratio5 and sparse evidence of redundancy (i.e., overuse of the same highly frequent words)47 in schizophrenia, which might occur also in highly fluent individuals. Conversely, speech samples acquired from participants belonging to Cluster 2 were characterized by shorter utterances, longer and more frequent pauses and fillers, lower occurrence of pronouns and emotional and metacognitive words, but in the context of higher variety and rarity (i.e., low frequency) of the terms used. In short, this cluster includes individuals who are less fluent and use less pronouns and psychological terms, but overall exhibit a greater lexical variety. The characterization of this cluster confirms the evidence of diminished fluency and the presence of altered use of pronouns and emotional words in schizophrenia4,29,33,48. What is important to highlight is that, while the various aspects that characterize each cluster were already noted in the literature as domains of impairment in schizophrenia, our analysis unravels distinct ways in which these domains of impairment might cluster, rather than simply co-occur. Compared to previous studies that entered unitary language scores, we were able to reveal a novel separation of clusters across a set of different linguistic features. Importantly, Cluster 1 and Cluster 2 should not be interpreted as two subgroups with high and low severity of language impairment, but rather as different profiles where language difficulties pattern differently, resulting in very distinctive speech characteristics. The direction of the association between fluency and lexical richness (measured as type-token ratio) in the two clusters is particularly interesting. While at first sight the fact that more fluent participants exhibited also lower lexical variety might appear counterintuitive, speech excerpts from our sample (see Supplementary Tables 4, 5) clearly illustrate that more talkative individuals can be more repetitive and redundant at the lexical level, which results in a lower type-token ratio, and that by contrast less fluent individuals might use more rare and unusual terms, resulting in a higher type-token ratio. In line with this, recent literature reported that, compared to healthy controls, individuals with schizophrenia have reduced fluency (e.g., shorter utterances and longer pauses) as well as higher lexical variety in terms of type-token ratio29,30. Our data confirm this evidence and add also that participants’ global lexical richness in terms of unique lemmas might be dissociated from the frequency of use of words belonging to specific semantic classes (e.g., psychological lexicon), with these two dimensions capturing different aspects of language impairment. Indeed, participants in Cluster 2 exhibited lower lexical variety but greater use of affective or metacognitive words, whereas individuals in Cluster 1 were poorer in the psychological lexicon, despite greater lexical richness.
The most relevant aspects distinguishing the two clusters are their different associations with psychopathological and functional domains, as they emerged from the step 3 of the analysis. This is overall the most innovative finding of our work and deserves special considerations for its clinical implications. Individuals with the more talkative yet lexically poorer profile (Cluster 1) exhibited lower symptoms and better functioning compared with individuals with the opposite profile (Cluster 2). On the one hand, these patterns are in line with associations previously reported in the literature, in particular the well-documented link between reduced fluency (longer pauses and shorter utterances) and negative symptoms4,30 and between speech and language impairment at large and disorganization aspects, such as formal thought disorder5,49,50 and difficulty in abstract thinking10,11,51. Our data also strengthen the connection between worse quality of life and linguistic aspects such as poverty of speech and greater use of (especially negative) emotional words14,31,33. On the other hand, our results markedly expand the state of the art by showing that a multilevel linguistic profiling might evidence different subgroups of individuals who, in addition to speaking differently, are also different not just in one psychopathological dimension but in the overall clinical severity. Going more deeply in this, it is interesting to note that those individuals who are more fluent, although possibly repetitive, are also those with greater use of mental state terms: this might be indicative of a greater attention to interpersonal relations and effort to engage in social interaction and conversation on personal topics, consistently with the better functioning observed for this subgroup (including the Interpersonal Relations subscale of the QLS). Conversely, the poverty of speech and reduced use of psychological lexicon as observed in Cluster 2 might reflect social withdrawal and poorer emotional self-awareness, consistently with the lower functioning and higher symptomatology of this subgroup. In sum, it seems that it is not just the amount of speech produced, or just the quality of the words, that reflects the clinical state, but rather it is the global linguistic profile, from speech to the lexicon, that is associated with different clinical outcomes.
However, the two clusters did not show any straightforward difference in cognition and social cognition, namely the two clusters did not vary in the global cognitive score and in the ToM score. While this finding is at first sight unexpected, the non-significant difference between groups can be explained when considering that the two clusters are not to be intended as reflecting different levels of severity in language impairment but rather as different linguistic profiles. While previous studies that evidenced a link between language and cognition adopted a whole-group correlational approach1,2, here the two clusters reflect different configurations of language characteristics, which seem to be relatively independent of the degree of cognitive impairment. Importantly, when we performed an additional fine-grained correlational analysis, different patterns of associations between linguistic features and cognitive aspects emerged for the two clusters. Participants in Cluster 2 showed significant correlations between Fluency/Lexical Richness and both verbal memory and planning abilities, as well as between the Frequency of Personal Pronouns and working memory and planning skills, while this pattern was not observed in Cluster 1. The stronger link between language and cognitive skills observed in Cluster 2 seems to suggest that, in individuals with more severe symptoms and poorer functioning, language and cognition are mutually dependent and linguistic impairment goes hand in hand with cognitive deterioration. Conversely, in more preserved individuals language and cognitive abilities seem to be rather independent. This additional analysis clarifies that our findings are not in contrast with the literature that found a relationship between linguistic abilities and the cognitive domains based on whole-group analysis1,2, adding that the link between language and cognition might have different strengths in different subgroups of patients. As for social cognition, no significant associations were highlighted in the additional analysis. When looking at the literature, social cognition seems to be a robust determinant of high-level (e.g., pragmatic) language skills in schizophrenia1,2,15, but the association with the building blocks of language in the domains of speech and lexical features is less robust and often not found31,48,52. Our data align with such evidence of a relative interdependence between language profiling and sociocognitive skills. It should also be noted, however, that in this study sociocognitive assessment was based on a single test focusing on mentalizing skills, leaving out other facets of the sociocognitive domain (e.g., emotion recognition) that might be important for language.
Finally, a comment is needed on the absence of difference between clusters in terms of demographic variables and characteristics such as onset and duration of illness. While acknowledging that these factors often affect the severity of clinical outcome53,54, the literature reports also evidence of clusters based on linguistic and cognitive characteristics with no variation in illness duration and onset38,44,55 or in education38,44,45. As for our data, the sample was characterized by chronic patients with an adult onset (ranging mostly between 20 and 30 years), which might further motivate the absence of differences between the two clusters. Similarly, education was homogenously distributed in the sample (with most participants having 8–13 years of education), hence with little room for variation. We cannot exclude, however, that in a larger and more diverse sample, linguistic profiling might capture also differences in education and illness duration and onset. Taking all these considerations together, our results provide novel evidence on how language features might combine in different multidimensional profiles, highlighting in particular a more fluent yet repetitive subgroup and a less fluent and poor in mental terms type, with the latter associated with worse clinical outcome. The cluster analysis that we presented underwent an articulated validation procedure suggesting that the classification scheme is rather stable, but certainly further studies are needed to validate it with independent samples.
The last important point to discuss focuses precisely on the linguistic-driven cluster analysis. Here we tried to extend the potential of computational methods, by innovatively combining them with a data-driven clustering technique as used to subtyping schizophrenia along other dimensions such as symptoms and cognitive functions38,39,44. The outcome of this approach contributes to corroborating the view that automated linguistic approaches in schizophrenia are much more than “promising”56, and could be of great utility not simply to predict diagnosis but also to monitor and deconstruct clinical heterogeneity throughout the illness course. Their combination with data-driven clustering approaches, as implemented in this study, could actually contribute greatly to unraveling subgroups of individuals with different clinical characteristics starting from the building blocks of language. Given the multifaceted nature of language impairment, the automatic language- and data-driven approach could not only overcome the subjective biases of the assessor but also disclose a greater amount of variability embedded in the linguistic data57 and is hence particularly suited to describe the vastly heterogenous population of individuals diagnosed with schizophrenia.
The results obtained with this method suggest a number of possible clinical implications. First, they provide the possibility of better orienting treatment strategies according to the individual’s global linguistic profile, following theoretically motivated, personalized, and multilevel approaches. In particular, adopting the multidimensional analysis to unravel the individual’s linguistic profile could allow to go beyond the clinical evaluation of language impairment and the simple observation of a fluent vs. non-fluent distinction to take into account also more subtle problems in the domains of speech and the lexicon that might escape the routine assessment. For instance, individuals with a profile of marked fluency in discourse associated with reduced lexical richness could benefit from treatment programs targeting verbosity and, when present, speech disorganization, coupled with exercises aiming at improving lexical breadth. Conversely, individuals with reduced fluency and limited use of pronouns and psychological lexicon might benefit from the combination of activities promoting verbal initiative and remediating under-informativity and exercises prompting the use of referential expressions as well as words expressing emotional states and metacognitive processes. Although the field of language rehabilitation in schizophrenia is at its infancy, there are already some effective programs available, improving different language components, such as for instance semantic classes and fluency features58,59, or discourse and pragmatics60,61,62, which could be selected and combined in a personalized fashion to increase treatment efficacy.
Additionally, our results suggest that automated assessments of linguistic characteristics and patterns, if implemented in clinical practice, may represent a useful tool to monitor treatment response and clinical course. Indeed, automatically detected changes in speech patterns may be associated and even precede changes in the clinical status. Going even further, this approach may be exploited as potential endpoints for the evaluation of clinical trials57, providing a more objective, comparable, and operator-independent measure of psychopathological and functional outcomes.
Nonetheless, what we proposed is just a first step towards a more integrated automated and machine-learning approach to language in schizophrenia. There are indeed several limitations in our study, which also disclose possible challenges for future research. First, although we conducted a solid machine-driven validation of the cluster analysis, future studies are needed to test the replicability of the linguistic grouping proposed here on independent samples. To increase reproducibility, a more massive machine-learning approach with the inclusion of larger samples than the one used here would be recommended, possibly based on a consortium collaboration favoring generalizability and cross-cultural applicability63 (on this regard, see the recently established “Discourse in Psychosis (DISCOURSE)” consortium: https://discourseinpsychosis.org/). Also, we still need longitudinal observations to assess the stability of the linguistic profiles and their long-term applicability for monitoring and prognostic purposes. This represents the ultimate application of these methods, consistently with a growing body of evidence showing the viability of longitudinal applications of machine-learning methods for ambulatorial and remote neuropsychological testing63,64.
Second, there are several limitations connected to the linguistic task. Even though the semi-structured autobiographical interview used here can be easily administered, more ecological (e.g., based on spontaneous conversations)65 and longer tasks (e.g., not limited to 5–6 minutes) could be more effective to capture the participants’ usual mode of communication. Considering the practical difficulties connected with the clinical application of such tasks66, a possible way forward could be the combination of traditional speech elicitation tasks with corpus-based approaches67. The use of different speech elicitation tasks, capable of triggering a broader variety of linguistic uses, could also be important. For instance, Hong et al.21 reported a marked difference between individuals with schizophrenia and controls in a task eliciting autobiographical experiences of five different emotions, suggesting that tasks with a higher emotional valence than the one employed here might increase the possibility of distinguishing between groups. Finally, while we analyzed language from speech to semantic classes, a more comprehensive language profiling could come from the inclusion of higher-order levels of language processing, namely discourse and pragmatic aspects, which are known for being impaired in schizophrenia1,10.
Taken together, our results not only confirm but also expand previous evidence of a connection between language, psychopathology, and functioning in schizophrenia, showing that a multi-layered linguistic analysis combined with clustering techniques is able to predict a wider range of symptoms (including not only negative but also positive, general, and disorganized symptoms) and several domains of daily functioning. Specifically, the outcome of our analysis shows that specific patterns of linguistic impairment (e.g., dysfluencies, underuse of pronouns and emotional and metacognitive words, etc.) underlie complex clinical states and might have a strong negative impact on participants’ functional outcomes. These findings suggest that a comprehensive multidimensional exploration of language might be useful to capture the clinical heterogeneity of schizophrenia and might have a significant clinical impact on the development of rehabilitative intervention strategies and on the monitoring of the illness course.
Methods
Sample
Sixty-seven individuals with a diagnosis of schizophrenia based on DSM-5 criteria68 were recruited from the Department of Clinical Neurosciences, IRCCS San Raffaele Scientific Institute, Milan, Italy. All participants were Italian native speakers. Exclusion criteria were: severe traumatic brain injury or neurological disorders, intellectual disability, alcohol or substance abuse in the preceding 6 months, and severe psychotic exacerbation in the preceding 3 months. All participants provided informed consent. The study was approved by the local ethical committee, following the principles of the Declaration of Helsinki.
Assessment
Participants underwent a comprehensive assessment, including psychopathology, neurocognitive and mentalizing skills, and daily functioning. The assessment was conducted in three sessions, each lasting approximately one hour. Psychopathology was assessed by a trained psychiatrist using the PANSS69. A score for PANSS Positive, Negative, and General Total Scores was derived, alongside a composite score assessing the disorganization dimension13,70, obtained by summing the items of conceptual disorganization (P2), difficulty in abstraction (N5), stereotyped thinking (N7), mannerism (G5), disorientation (G10), poor attention (G11), lack of judgment and insight (G12), and disturbance of volition (G13). Neurocognitive abilities were assessed through the Italian version71 of the BACS72, which includes six subtests assessing Verbal Memory (VM), Digit Sequencing (DS), Token Motor Task (TMT), Semantic Fluency (SF), Symbol Coding (SC), and Tower of London (ToL). A subscore for each subtest was derived (adjusted for demographic variables), as well as an equivalent total BACS score. Sociocognitive skills were assessed via the ToM PST73, which includes a non-verbal ToM Sequencing Task and a ToM Questionnaire. Subscores for the Sequencing Task and the Questionnaire and a total score for global ToM abilities were derived. Finally, functioning was measured using the QLS74, from which a subscore for each of the three subscales (i.e., Interpersonal Relations, Instrumental Role, and Personal Autonomy) and a total score were calculated. Neurocognition, social cognition, and functioning were assessed by trained clinical psychologists.
Semi-automated linguistic analysis
To elicit speech production, participants were administered the Interview task from the Assessment of Pragmatic Abilities and Cognitive Substrates (APACS) test75, a validated tool developed to assess pragmatic skills (both expressive and receptive) using the original Italian version. This task, lasting at least five minutes according to the APACS manual, consists of a semi-structured interview on autobiographical topics (i.e., family, home, work, organization of the day). Speech samples were recorded using a one-channel audio-recorder oriented towards the participant. The recordings were acquired in a quiet room in a controlled laboratorial setting. The audio recordings were then converted into .wav files and imported into the PRAAT software76, with a standard quality of 44.10 kHz (capturing 44100 samples per second).
The total duration of the speech sample was 6 hours and 43 minutes, with a total duration of participants’ occupation floor of 4 hours and 29 minutes (the rest being occupied by the interviewer). The mean length of participants’ interviews was 6.15 ± 2.00 minutes, with a mean occupation floor of 4.24 ± 2.25 minutes per participant.
Afterwards, audio files underwent a pre-processing phase followed by the extraction of a number of linguistic features.
Audio file pre-processing
The audio files were first transcribed using the Computerized Language ANalysis (CLAN) software77 by a linguist with training in transcription. Interviewer turns, non-verbal vocalizations, and false starts were removed. Turns were manually divided following CLAN’s criteria77, segmenting utterances when word strings were (a) delimited by a 1-s (or longer) pause; or (b) characterized by a terminal intonational contour; or (c) identified as a complete grammatical structure. We used the PRAAT software76 to quantitatively check criteria (a) and (b). Another trained linguist transcribed 16 randomly-selected interviews (i.e., 25% of the entire sample) to assess the reliability of the transcription and the utterance segmentation procedures. The Intraclass correlation coefficient (ICC), based on a two-way mixed-effects model on single measures, showed that the two coders reached excellent absolute agreement on the number of words (ICC = 0.99, p < 0.001, 95% CI [.99, 1]) and moderate to excellent absolute agreement on the number of utterances (ICC = 0.80, p = 0.001, 95% CI [0.51, 0.91]).
Extraction of linguistic features
Linguistic features included nine measures across four different dimensions: (1) Lexical Richness (i.e., mean lexical frequency and type-token ratio), (2) Fluency (i.e., mean length of utterance, mean gap duration, mean silent and filled pause duration, and pause-to-word ratio), (3) Frequency of Personal Pronouns, and (4) Frequency of words belonging to the Psychological Lexicon (i.e., affective words and words related to cognitive mechanisms).
For the Lexical Richness dimension, lexical frequency values for each word in the transcripts were automatically extracted from the Corpus and Frequency Lexicon of Written Italian (CoLFIS)78 using the R Studio software (v. 1.3.1093)79 to compute the mean lexical frequency, while the type-token ratio was computed on the transcripts using Python’s Natural Language Toolkit (NLTK)80. As for the Fluency measures, we used PRAAT’s silence detection to automatically extract the number and the duration of silences (i.e., gaps at the beginning of turns and intra-turn pauses) from the audio files; the PRAAT software was used also to manually check the number and the duration of filled pauses, in order to determine the mean pause duration and the pause-to-word ratio. Then, we computed the mean length of utterance from the transcripts using the built-in “Words per sentence” function of the Linguistic Inquiry Word Count software (LIWC2015, v. 1.6.0)32, based on the utterances segmented following CLAN criteria77. Finally, the frequency values (in percentage) of Personal Pronouns and words expressing affective content and cognitive mechanisms (here grouped under the label of Psychological Lexicon)81 were extracted with the LIWC2015 software32 (using the Italian dictionary)82, which automatically analyzes raw texts word-by-word, counting the occurrences of each token included in the different lexical categories.
Statistical analysis
The statistical analysis followed three stages: (1) we first performed a Principal Component Analysis (PCA) on automatically extracted linguistic features to identify language-based principal components (PCs); (2) then, we used the PC scores to perform a data-driven cluster analysis to identify clusters of participants; (3) finally, the clusters identified by the cluster analysis were compared for demographics, psychopathology, neurocognition, social cognition, and functioning.
As for the first stage of the analysis, we performed a Principal Component Analysis (PCA) with varimax rotation on the standardized (i.e., z-centered) linguistic features obtained from the semi-automated linguistic analysis. We then selected the Principal Components (PCs) with eigenvalues greater than 183.
Afterwards, in order to identify subgroups of participants from the linguistic-based PCs (second stage of analysis), we performed the cluster analysis using the PC scores to feed a k-means algorithm, an unsupervised machine-learning clustering algorithm. The number of centers was determined using the silhouette method84 starting from 25 random centroids. We validated the final cluster solution with a Linear Discriminant Analysis (LDA), based on different replications with random-split samples55, cross-validated with a leave-one-out procedure. The random-split samples procedure randomly assigns a subset of the participants from the original sample to either a training or a testing subset, which are used to train and test the classification performance of the algorithm. Accordingly, we randomly assigned 75%, 50%, and 25% of the participants to the training subset (and 25%, 50%, and 75% of the participants to the testing subset, respectively), to evaluate the validation results over multiple rounds with progressively decreasing training observations. To test the robustness of the obtained measure, we iterated the procedure with a standard number of iterations of random samplings (i.e., n = 50, as in Hong et al.85) for each training-testing subset (75%-25%; 50%-50%; 25%-75%). The average performance (in proportion: 0–1) of the algorithm in both training and testing partitions is then used as a measure of classification quality. Moreover, the random validation procedure was cross-validated with the leave-one-out method, which tests the classification function using all but one participant of the sample, predicting the omitted participant’s cluster membership. Therefore, the cross-validation procedure was iterated once for each participant in our dataset, using all other participants as a trainining set and the selected participant as a single-item testing set.
As for the third stage of the analysis, we compared the clusters identified by the machine-driven algorithm on demographic, clinical, cognitive, sociocognitive, and functional variables via a series of t-tests. Prior to the analysis, normality assumption was checked by visual inspection of the distribution of the dependent variables, while homoskedasticity assumption was assessed using the F-test comparing two variances (tested with the var.test function in R). When appropriate, p-values of pairwise comparisons were FDR-adjusted. An additional analysis was conducted to explore in a more fine-grained fashion the associations between cognitive (i.e., BACS Verbal Memory, Digit Sequencing, Token Motor Task, Semantic Fluency, Symbol Coding, and Tower of London) and sociocognitive (i.e, ToM PST Sequencing Task and Questionnaire) subscores and the linguistic-based PCs across clusters. All statistical analysis were run in R, v. 4.0.379, with the R Studio editor, v. 1.3.1093.
Data availability
The data are not publicly available due to restrictions, as they contain information that could compromise the privacy of research participants. The data that support the findings of this study may be available on request from the corresponding author, upon case-by-case evaluation.
References
Bambini, V. et al. The communicative impairment as a core feature of schizophrenia: Frequency of pragmatic deficit, cognitive substrates, and relation with quality of life. Compr. Psychiatry 71, 106–120 (2016).
Parola, A., Berardinelli, L. & Bosco, F. M. Cognitive abilities and theory of mind in explaining communicative-pragmatic disorders in patients with schizophrenia. Psychiatry Res. 260, 144–151 (2018).
Covington, M. A. et al. Schizophrenia and the structure of language: The linguist’s view. Schizophr. Res. 77, 85–98 (2005).
Parola, A., Simonsen, A., Bliksted, V. & Fusaroli, R. Voice patterns in schizophrenia: A systematic review and Bayesian meta-analysis. Schizophr. Res. 216, 24–40 (2020).
Manschreck, T. C., Maher, B. A., Hoover, T. M. & Ames, D. The type—token ratio in schizophrenic disorders: clinical and research value. Psychol. Med. 14, 151–157 (1984).
Spitzer, M. et al. Semantic and phonological priming in schizophrenia. J. Abnorm. Psychol. 103, 485–494 (1994).
Moro, A. et al. Detecting syntactic and semantic anomalies in schizophrenia. Neuropsychologia 79, 147–157 (2015).
Barattieri di San Pietro, C., Barbieri, E., Marelli, M., de Girolamo, G. & Luzzatti, C. Processing argument structure and syntactic complexity in people with Schizophrenia spectrum disorders. J. Commun. Disord. 96, 106182 (2022).
Perlini, C. et al. Non literal language comprehension in a large sample of first episode psychosis patients in adulthood. Psychiatry Res. 260, 78–89 (2018).
Bambini, V. et al. A leopard cannot change its spots: A novel pragmatic account of concretism in schizophrenia. Neuropsychologia 139, 107332 (2020).
Mashal, N., Vishne, T., Laor, N. & Titone, D. Enhanced left frontal involvement during novel metaphor comprehension in schizophrenia: Evidence from functional neuroimaging. Brain Lang 124, 66–74 (2013).
Minzenberg, M. J., Ober, B. A. & Vinogradov, S. Semantic priming in schizophrenia: A review and synthesis. J. Int. Neuropsychol. Soc. 8, 699–720 (2002).
Lucarini, V. et al. Conversational metrics, psychopathological dimensions and self-disturbances in patients with schizophrenia. Eur. Arch. Psychiatry Clin. Neurosci. 272, 997–1005 (2022).
Bowie, C. R. & Harvey, P. D. Communication abnormalities predict functional outcomes in chronic schizophrenia: Differential associations with social and adaptive functions. Schizophr. Res. 103, 240–247 (2008).
Agostoni, G. et al. Communicative-pragmatic abilities mediate the relationship between cognition and daily functioning in schizophrenia. Neuropsychology 35, 42–56 (2021).
Muralidharan, A., Finch, A., Bowie, C. R. & Harvey, P. D. Thought, language, and communication deficits and association with everyday functional outcomes among community-dwelling middle-aged and older adults with schizophrenia. Schizophr. Res. 196, 29–34 (2018).
Cohen, A. S. & Elvevåg, B. Automated computerized analysis of speech in psychiatric disorders. Curr. Opin. Psychiatry 27, 203–209 (2014).
Corcoran, C. M. et al. Language as a biomarker for psychosis: A natural language processing approach. Schizophr. Res. 226, 158–166 (2020).
Hitczenko, K., Mittal, V. A. & Goldrick, M. Understanding Language Abnormalities and Associated Clinical Markers in Psychosis: The Promise of Computational Methods. Schizophr. Bull 47, 344–362 (2021).
Elvevåg, B., Foltz, P. W., Weinberger, D. R. & Goldberg, T. E. Quantifying incoherence in speech: An automated methodology and novel application to schizophrenia. Schizophr. Res. 93, 304–316 (2007).
Hong, K. et al. Lexical use in emotional autobiographical narratives of persons with schizophrenia and healthy controls. Psychiatry Res 225, 40–49 (2015).
Elvevåg, B., Foltz, P. W., Rosenstein, M. & DeLisi, L. E. An automated method to analyze language use in patients with schizophrenia and their first-degree relatives. J. Neurolinguistics 23, 270–284 (2010).
Mota, N. B. et al. Speech graphs provide a quantitative measure of thought disorder in psychosis. PLoS One 7, e34928 (2012).
Bedi, G. et al. Automated analysis of free speech predicts psychosis onset in high-risk youths. npj Schizophr 1, 15030 (2015).
Rezaii, N., Walker, E. & Wolff, P. A machine learning approach to predicting psychosis using semantic density and latent content analysis. npj Schizophr 5, 9 (2019).
Corcoran, C. M. et al. Prediction of psychosis across protocols and risk cohorts using automated language analysis. World Psychiatry 17, 67–75 (2018).
Mota, N. B., Copelli, M. & Ribeiro, S. Thought disorder measured as random speech structure classifies negative symptoms and schizophrenia diagnosis 6 months in advance. npj Schizophr 3, 18 (2017).
Figueroa-Barra, A. et al. Automatic language analysis identifies and predicts schizophrenia in first-episode of psychosis. Schizophrenia 8, 53 (2022).
de Boer, J. N. et al. Language in schizophrenia: relation with diagnosis, symptomatology and white matter tracts. npj Schizophr 6, 10 (2020).
de Boer, J. N., Voppel, A. E., Brederoo, S. G., Wijnen, F. N. K. & Sommer, I. E. C. Language disturbances in schizophrenia: the relation with antipsychotic medication. npj Schizophr 6, 24 (2020).
Buck, B. & Penn, D. L. Lexical Characteristics of Emotional Narratives in Schizophrenia. J. Nerv. Ment. Dis 203, 702–708 (2015).
Pennebaker, J. W., Boyd, R. L., Jordan, K. & Blackburn, K. The Development and Psychometric Properties of LIWC2015. (University of Texas at Austin, 2015).
Minor, K. S. et al. Lexical analysis in schizophrenia: How emotion and social word use informs our understanding of clinical presentation. J. Psychiatr. Res. 64, 74–78 (2015).
Tang, S. X. et al. Natural language processing methods are sensitive to sub-clinical linguistic differences in schizophrenia spectrum disorders. npj Schizophr 7, 25 (2021).
Docherty, N. M., Strauss, M. E., Dinzeo, T. J. & St-Hilaire, A. The Cognitive Origins of Specific Types of Schizophrenic Speech Disturbances. Am. J. Psychiatry 163, 2111–2118 (2006).
Seaton, B. E., Goldstein, G. & Allen, D. N. Sources of heterogeneity in schizophrenia: the role of neuropsychological functioning. Neuropsychol. Rev. 11, 45–67 (2001).
Bosia, M. et al. From cognitive and clinical substrates to functional profiles: Disentangling heterogeneity in schizophrenia. Psychiatry Res 271, 446–453 (2019).
Strauss, G. P. et al. Deconstructing negative symptoms of schizophrenia: Avolition–apathy and diminished expression clusters predict clinical presentation and functional outcome. J. Psychiatr. Res. 47, 783–790 (2013).
Paul, N. B. et al. Cluster analysis of negative symptoms identifies distinct negative symptom subgroups. Schizophr. Res. 246, 207–215 (2022).
Talpalaru, A., Bhagwat, N., Devenyi, G. A., Lepage, M. & Chakravarty, M. M. Identifying schizophrenia subgroups using clustering and supervised learning. Schizophr. Res. 214, 51–59 (2019).
Rocca, P. et al. Social cognition in people with schizophrenia: a cluster-analytic approach. Psychol. Med. 46, 2717–2729 (2016).
Bechi, M. et al. Intellectual and cognitive profiles in patients affected by schizophrenia. J. Neuropsychol. 13, 589–602 (2019).
Buonocore, M. et al. Cognitive Reserve Profiles in Chronic Schizophrenia: Effects on Theory of Mind Performance and Improvement after Training. J. Int. Neuropsychol. Soc. 24, 563–571 (2018).
Gilbert, E. et al. Cluster analysis of cognitive deficits may mark heterogeneity in schizophrenia in terms of outcome and response to treatment. Eur. Arch. Psychiatry Clin. Neurosci. 264, 333–343 (2014).
Oomen, P. P. et al. Characterizing speech heterogeneity in schizophrenia-spectrum disorders. J. Psychopathol. Clin. Sci. 131, 172–181 (2022).
Liu, C.-W., Lin, K.-H. & Kuo, Y.-M. Application of factor analysis in the assessment of groundwater quality in a blackfoot disease area in Taiwan. Sci. Total Environ. 313, 77–89 (2003).
Maher, B. A., Manschreck, T. C. & Molino, M. A. C. Redundancy, pause distributions and thought disorder in schizophrenia. Lang. Speech 26, 191–199 (1983).
Buck, B., Minor, K. S. & Lysaker, P. H. Differential lexical correlates of social cognition and metacognition in schizophrenia; a study of spontaneously-generated life narratives. Compr. Psychiatry 58, 138–145 (2015).
McKenna, P. J. & Oh, T. M. Schizophrenic Speech. (Cambridge University Press, 2005).
Çokal, D. et al. Disturbing the rhythm of thought: Speech pausing patterns in schizophrenia, with and without formal thought disorder. PLoS One 14, e0217404 (2019).
Silva, A., Limongi, R., MacKinley, M. & Palaniyappan, L. Small Words That Matter: Linguistic Style and Conceptual Disorganization in Untreated First-Episode Schizophrenia. Schizophr. Bull. Open 2, sgab010 (2021).
Minor, K. S., Willits, J. A., Marggraf, M. P., Jones, M. N. & Lysaker, P. H. Measuring disorganized speech in schizophrenia: automated analysis explains variance in cognitive deficits beyond clinician-rated scales. Psychol. Med. 49, 440–448 (2019).
Maglione, J. E., Thomas, S. E. & Jeste, D. V. Late-onset schizophrenia: do recent studies support categorizing LOS as a subtype of schizophrenia? Curr. Opin. Psychiatry 27, 173–178 (2014).
Buonocore, M. et al. Modeling the interplay of age at onset and sex on cognition in Schizophrenia. Asian J. Psychiatr. 75, 103202 (2022).
Carruthers, S. P. et al. Exploring heterogeneity on the wisconsin card sorting test in schizophrenia spectrum disorders: a cluster analytical investigation. J. Int. Neuropsychol. Soc. 25, 750–760 (2019).
Foltz, P. W., Rosenstein, M. & Elvevåg, B. Detecting clinically significant events through automated language analysis: Quo imus? npj Schizophr 2, 15054 (2016).
Marder, S. R. Natural language processing: its potential role in clinical care and clinical research. Schizophr. Bull. 48, 958–959 (2022).
Clegg, J., Brumfitt, S., Parks, R. W. & Woodruff, P. W. R. Speech and language therapy intervention in schizophrenia: a case study. Int. J. Lang. Commun. Disord. 42, 81–101 (2007).
Ryu, Y. et al. Deinstitutionalization of long-stay patients with schizophrenia: the 2-year social and clinical outcome of a comprehensive intervention program in Japan. Aust. New Zeal. J. Psychiatry 40, 462–470 (2006).
Bambini, V. et al. It is time to address language disorders in schizophrenia: A RCT on the efficacy of a novel training targeting the pragmatics of communication (PragmaCom). J. Commun. Disord. 97, 106196 (2022).
Bosco, F. M., Gabbatore, I., Gastaldo, L. & Sacco, K. Communicative-pragmatic treatment in schizophrenia: A pilot study. Front. Psychol. 7, 166 (2016).
Riedl, L. et al. Multimodal speech-gesture training in patients with schizophrenia spectrum disorder: Effects on quality of life and neural processing. Schizophr. Res. 246, 112–125 (2022).
Chandler, C. et al. Machine learning for ambulatory applications of neuropsychological testing. Intell. Med. 1–2, 100006 (2020).
Liu, G., Henson, P., Keshavan, M., Pekka-Onnela, J. & Torous, J. Assessing the potential of longitudinal smartphone based cognitive assessment in schizophrenia: A naturalistic pilot study. Schizophr. Res. Cogn. 17, 100144 (2019).
McCabe, R., Heath, C., Burns, T. & Priebe, S. Engagement of patients with psychosis in the consultation: conversation analytic study. Br. Me 325, 1148–1151 (2002).
Li, C. et al. Investigating non lexical markers of the language of schizophrenia in spontaneous conversations. In Proceedings of the 2nd Workshop on Computational Approaches to Discourse 20–28 (Association for Computational Linguistics, 2021).
Parola, A. et al. Speech disturbances in schizophrenia: Assessing cross-linguistic generalizability of NLP automated measures of coherence. Schizophr. Res. (2022) https://doi.org/10.1016/j.schres.2022.07.002.
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. (American Psychiatric Association, 2013).
Kay, S. R., Fiszbein, A. & Opler, L. A. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr. Bull. 13, 261–276 (1987).
van der Gaag, M. et al. The five-factor model of the Positive and Negative Syndrome Scale II: A ten-fold cross-validation of a revised model. Schizophr. Res. 85, 280–287 (2006).
Anselmetti, S. et al. The Brief Assessment of Cognition in Schizophrenia. Normative data for the Italian population. Neurol. Sci. 29, 85–92 (2008).
Keefe, R. The Brief Assessment of Cognition in Schizophrenia: reliability, sensitivity, and comparison with a standard neurocognitive battery. Schizophr. Res. 68, 283–297 (2004).
Brüne, M. Theory of mind and the role of IQ in chronic disorganized schizophrenia. Schizophr. Res. 60, 57–64 (2003).
Heinrichs, D. W., Hanlon, T. E. & Carpenter, W. T. The Quality of Life Scale: An Instrument for Rating the Schizophrenic Deficit Syndrome. Schizophr. Bull. 10, 388–398 (1984).
Arcara, G. & Bambini, V. A test for the assessment of pragmatic abilities and cognitive substrates (APACS): normative data and psychometric properties. Front. Psychol. 7, 70 (2016).
Boersma, P. & Weenink, D. Praat: doing phonetics by computer (Version 6.1.36). http://www.praat.org/ (2021).
MacWhinney, B. The CHILDES project: Tools for analyzing talk: Transcription format and programs. (Lawrence Erlbaum Associates Publishers, 2000).
Bertinetto, P. M. et al. Corpus e Lessico di Frequenza dell’Italiano Scritto (CoLFIS). https://www.istc.cnr.it/en/grouppage/colfis (2005).
R Core Team. R: A language and environment for statistical computing. https://www.r-project.org/ (2021).
Bird, S., Klein, E. & Loper, E. Natural language processing with Python: analyzing text with the natural language toolkit. (O’Reilly Media, Inc., 2009).
Hughes, C., Lecce, S. & Wilson, C. “Do you know what I want?” Preschoolers’ talk about desires, thoughts and feelings in their conversations with sibs and friends. Cogn. Emot. 21, 330–350 (2007).
Alparone, F. R., Caso, S., Solano, L. & Prezza, M. Traduzione e adattamento al contesto linguistico italiano del ‘Linguistic Inquiry and Word Count’ (LIWC). In Emozioni: cultura, comunicazione, benessere 133–140 (Progedit, 2002).
Kaiser, H. F. The Application of Electronic Computers to Factor Analysis. Educ. Psychol. Meas. 20, 141–151 (1960).
Rousseeuw, P. J. Silhouettes: A graphical aid to the interpretation and validation of cluster analysis. J. Comput. Appl. Math. 20, 53–65 (1987).
Hong, Y.-G., Kim, H.-K., Son, Y.-D. & Ka, C.-K. Identification of breathing patterns through EEG signal analysis using machine learning. Brain Sci. 11, (2021).
Manschreck, T. C., Maher, B. A. & Ader, D. N. Formal thought disorder, the type-token ratio, and disturbed voluntary motor movement in Schizophrenia. Br. J. Psychiatry 139, 7–15 (1981).
Magyari, L., De Ruiter, J. P. & Levinson, S. C. Temporal preparation for speaking in question-answer sequences. Front. Psychol. 8, 211 (2017).
Acknowledgements
During part of the project, F.F., L.B., and F.Cu. were supported by the Italian Ministry of Health under Grant Number GR-2018-12366092 (“Assessment and treatment of communicative pragmatic abilities in neurological and psychiatric disorders: feasibility and clinical efficacy”) awarded to V.B. and M.B. The authors wish also to acknowledge Cristian Mevio, who participated in the transcribing of speech materials.
Author information
Authors and Affiliations
Contributions
V.B.: Conceptualization; Methodology; Data interpretation; Writing—Original Draft. F.F.: Methodology; Formal Analysis; Data interpretation; Writing – Original Draft; Visualization. L.B.: Methodology, Formal Analysis; Data interpretation; Writing – Original Draft (contributing to Methods and Results sections); Visualization. F.C.: Clinical Data Acquisition; Data Curation; Data interpretation; Writing – Original Draft (contributing to Introduction section). M.Be.: Methodology; Neuropsychological data Acquisition; Data Curation. M.Bu.: Methodology; Neuropsychological data Acquisition; Data Curation. G.A.: Methodology; Neuropsychological data Acquisition; Data Curation. I.F.: Clinical Data Acquisition; Data Curation. J.S.: Clinical Data Acquisition; Data Curation. F.M.: Clinical Data Acquisition; Data Curation. M.S.: Clinical Data Acquisition; Data Curation. G.B.: Clinical Data Acquisition; Data Curation. F.Co.: Patients Enrollment; Clinical Data Acquisition. R.C.: Resources; Supervision of Project Administration. M.Bo.: Conceptualization; Data interpretation; Writing—Review & Editing; Project Administration.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
41537_2022_306_MOESM1_ESM.docx
Supplementary information for the article “Deconstructing heterogeneity in schizophrenia through language: a semi-automated linguistic analysis and data-driven clustering approach”
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Bambini, V., Frau, F., Bischetti, L. et al. Deconstructing heterogeneity in schizophrenia through language: a semi-automated linguistic analysis and data-driven clustering approach. Schizophr 8, 102 (2022). https://doi.org/10.1038/s41537-022-00306-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41537-022-00306-z
This article is cited by
-
Assessment of pragmatic abilities and cognitive substrates (APACS) brief remote: a novel tool for the rapid and tele-evaluation of pragmatic skills in Italian
Language Resources and Evaluation (2023)