Abstract
Antipsychotic drugs are widely prescribed medications, used for numerous psychiatric illnesses. However, antipsychotic drugs cause serious metabolic side effects that can lead to substantial weight gain and increased risk for type 2 diabetes. While individual drugs differ, all antipsychotic drugs may cause these important side effects to varying degrees. Given that the single unifying property shared by these medications is blockade of dopamine D2 and D3 receptors, these receptors likely play a role in antipsychotic drug-induced metabolic side effects. Dopamine D2 and dopamine D3 receptors are expressed in brain regions critical for metabolic regulation and appetite. Surprisingly, these receptors are also expressed peripherally in insulin-secreting pancreatic beta cells. By inhibiting glucose-stimulated insulin secretion, dopamine D2 and dopamine D3 receptors are important mediators of pancreatic insulin release. Crucially, antipsychotic drugs disrupt this peripheral metabolic regulatory mechanism. At the same time, disruptions to circadian timing have been increasingly recognized as a risk factor for metabolic disturbance. Reciprocal dopamine and circadian signaling is important for the timing of appetitive/feeding behaviors and insulin release, thereby coordinating cell metabolism with caloric intake. In particular, circadian regulation of dopamine D2 receptor/dopamine D3 receptor signaling may play a critical role in metabolism. Therefore, we propose that antipsychotic drugs’ blockade of dopamine D2 receptor and dopamine D3 receptors in pancreatic beta cells, hypothalamus, and striatum disrupts the cellular timing mechanisms that regulate metabolism. Ultimately, understanding the relationships between the dopamine system and circadian clocks may yield critical new biological insights into mechanisms of antipsychotic drug action, which can then be applied into clinical practice.
Similar content being viewed by others
Introduction
Antipsychotic drugs (APDs) are commonly prescribed across a range of psychiatric illnesses including schizophrenia, major depression, bipolar disorder (BD), aggressive behaviors, dementia, anxiety, and post-traumatic stress disorder (PTSD). Consequently, APDs are some of the most widely prescribed medications in the U.S. with 1.2% of the population filling APD prescriptions.1 Moreover, public spending on APDs has increased ~ 5-fold in under a decade to $4.6 billion annually.2 However, despite their many uses, APDs have significant metabolic side effects, causing weight gain, increased risk of type 2 diabetes (T2D), cardiovascular disease and metabolic disturbances characterized by abdominal obesity, glucose intolerance, insulin resistance, hypertension, and dyslipidemia. While second-generation APDs like olanzapine are well-known to cause substantial weight gain,3 even first-generation APDs such as haloperidol, commonly considered safer from a metabolic perspective, may produce significant metabolic disturbances.4 Indeed, a recent multi-center study, the European First Episode Schizophrenia Trial concluded that metabolic disturbances and weight gain are associated with many APDs—both first and second generation.4 These metabolic side effects have led to high rates of treatment discontinuation, requirements for careful monitoring, and worse clinical outcomes, putting considerable strain on health-care systems. Consequently, psychiatric patients treated with these medications have markedly elevated rates of mortality across the lifespan, even after correcting for elevated rates of suicide associated with the disorders.5 Much of the mortality risk is attributed to cardiovascular disease, obesity, and metabolic disease.6, 7 Thus, developing a better understanding of the mechanism(s) of APD-induced metabolic abnormalities may ultimately lead to novel clinical interventions, leading to fewer metabolic side effects and improved treatment compliance. However, to date, the mechanisms for APD-induced metabolic abnormalities remain poorly understood. This is likely due to complexity in the system, with the convergence of at least three of the biological pathways involved in regulating metabolism and weight homeostasis including: (1) insulin control of glucose metabolism in the pancreas (2) central nervous system (CNS) regulation of mechanisms involved in appetite, satiety, and feeding behaviors, and (3) the coordination among these factors to ensure optimal timing of metabolic functions across a range of circumstances (e.g., circadian rhythms in sleep/activity).
APDs target central and peripheral dopamine receptors
Although multiple cellular targets for APDs, including histamine and serotonin receptors8 have been identified, all clinically effective APDs act through dopamine D2 (D2R) and D3 (D3R) receptors, suggesting a critical role for dopamine in promoting not only the therapeutic actions of these drugs, but possibly also in causing their metabolic side effects. APDs achieve their effects as both antagonists and inverse agonists of D2R and D3R, able to inhibit cellular signaling even in the absence of endogenous dopamine.9, 10 In the CNS, there exist distinct populations of tyrosine hydroxylase (TH)-expressing, dopaminergic neurons. In the midbrain, these neurons include cells in the ventral tegmentum (VTA) that project to the ventral striatum and frontal cortical regions implicated in modulating reward,11 and a distinct population in the substantia nigra that project to the dorsal striatum to control motor activity.12 In the hypothalamus, dopaminergic neurons in the arcuate nucleus (ARC) project locally to pro-opiomelanocrotin (POMC)-containing neurons that play a critical role in central control of glucose and energy homeostasis, in part through regulation of appetite and feeding.13, 14 Therefore, D2R and D3R in these striatal and hypothalamic dopamine circuits mediate appetite and feeding behaviors by stimulating the neural pathways that govern motivation, motor activity, and reward.15 The distribution of D2R and D3R in the striatum and ARC suggests that APDs could induce metabolic dysfunction by interfering with the dopaminergic mechanisms involved in feeding and satiety in the CNS.16
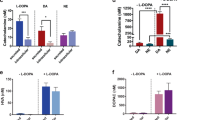
Peripheral dopamine outside the CNS may also be playing important roles in metabolic regulation. Surprisingly, D2R and D3R are also expressed in insulin-secreting pancreatic beta cells.17 These cells possess the machinery for both dopamine and insulin biosynthesis. We and colleagues showed that D2R/D3R can regulate both insulin and dopamine release directly in pancreatic beta cells from humans and rodents independently of CNS control.17–20 Specifically, we found that pancreatic dopamine inhibits glucose-stimulated insulin secretion (GSIS) via beta cell D2R/D3R, through an autocrine/paracrine mechanism.18, 20 Conversely, APD blockade of D2R/D3R significantly enhances GSIS.18 Importantly, this APD-induced increase in insulin secretion reproduces aspects of the chronic hyperinsulinemia found in T2D21 (Fig. 1). Rodent models of APD-administration recapitulate these findings, showing weight gain and peripheral insulin resistance.22 These studies point to direct action of APDs on peripheral dopamine targets, including insulin-secreting pancreatic beta cells as potentially important contributors to APD-induced metabolic dysfunction.20
Model for dopamine D2/3 receptor-mediated regulation of insulin release in the pancreatic beta cell. Dopamine acts through a dopamine D2/D3 receptor (D2/D3R)-mediated autocrine negative-feedback mechanism to inhibit further insulin release. Left unchecked following APD treatment, chronic insulin release may promote adipogenesis, weight gain, insulin resistance, and ultimately type 2 diabetes. The figure was adapted from Rubí and Maechler [Endocrinology 151(12): 5570–5581, 2010] with permission from Endocrinology and HighWire Press via Copyright Clearance Center
Many metabolic systems are rhythmic, under the control of central and peripheral circadian clocks. Therefore, in addition to the role of dopamine signaling, circadian rhythms may also significantly contribute to in APD-induced metabolic disturbances.23
Circadian rhythms are determined by the molecular clock
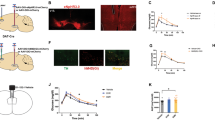
Most mammals show endogenous 24-h physiological rhythms, termed circadian rhythms, that synchronize the activity of organ systems with each other and the environment. The biological basis of circadian rhythms in mammals, including humans, is now well understood. The master timekeeper is located in the CNS, within the suprachiasmatic nucleus (SCN) of the hypothalamus and responds to light input from specialized photoreceptors in the retina as the primary signal that determines circadian phase.24 Circadian clocks are cell autonomous and ubiquitous across tissues, meaning that cells across a wide variety of brain regions outside the SCN,25–27 and peripheral organs have the ability to maintain daily rhythms in gene expression and physiology.28 A transcriptional/translational feedback loop made up of ~ 20 “core clock genes” exists to maintain essential functions underlying cellular circadian rhythms (Fig. 2). At the center of this loop, the proteins CLOCK and BMAL1 interact to form a heterodimeric transcriptional activator. Under some circumstances, another circadian transcription factor, NPAS2 can substitute for CLOCK within this dimer.29 The BMAL1 complex binds to E-box promoter elements, driving the expression of CRY1/2, and PER1/2/3 proteins, transcriptional repressors that inhibit their own expression to sustain circadian oscillators with a period length of ~ 24-h (Fig. 2). Additional negative feedback loops comprised of REV-ERB-α/β proteins play important supporting roles, acting through distinct promoter elements to sustain rhythmic expression of genes across the genome.30 Post-translational, bioenergetic and epigenetic factors can also contribute to the maintenance of rhythms.31 In particular, multiple signal transduction pathways (e.g., cyclic adenosine monophosphates, cAMP) and activated protein kinases such as extracellular signal-regulated kinase (ERK) and p38 serve as clock inputs,32 linking neurotransmitter systems (e.g., dopamine) to the circadian clock through post-translational modification of clock proteins and/or modulation of transcription factors that regulate clock gene promoter elements (Fig. 2).
The circadian transcription/translation loop is comprised of rhythmically expressed “clock genes”. Circadian protein complexes containing BMAL1 drive expression of rhythmic genes including period (PER) and cryptochrome (CRY) through E-box DNA elements in promoters. PER/CRY negatively regulate their own expression. As PER/CRY degrade over several hours, BMAL1 activity increases and the cycle repeats. Time of onset (phase), duration (period), and strength (amplitude) of the cycle is regulated by multiple signaling pathway inputs. The figure was adapted from Landgraf et al. [Behavioral Neuroscience 128(3): 344–359, 2014] with permission from the American Psychological Association
Peripheral circadian rhythms and metabolism
Food is a powerful time-keeping cue that can direct biological rhythms. In peripheral organs such as the liver, food may be a more important time cue than light under restricted feeding conditions.33 Under healthy physiological conditions, insulin secretion, target tissue insulin sensitivity, glucose metabolism, leptin signaling, and lipid metabolism follow circadian rhythms. These rhythms generally favor anabolic activity during the daily active period when feeding occurs, and catabolic activity at rest.23 Accordingly, circadian clocks in peripheral organs including adipocytes,34, 35 liver,36 and pancreas37, 38 regulate these metabolically relevant rhythms, helping the body adjust for the cycles of prolonged fasting associated with sleep or during periods of caloric restriction. Rhythms also mediate glucose utilization in insulin-sensitive target tissues such as skeletal muscle.39
Increasing evidence suggests that timing is critical for maintaining metabolic homeostasis.40–43 When temporal control over diurnal and/or circadian rhythms is lost, it may lead to an inability to process glucose effectively, and ultimately to the development of metabolic disturbances.40, 43 Indeed, in mice fed an unrestricted high-fat diet across the day, this loss of diurnal feeding rhythms resulted in profound metabolic disturbances (e.g., weight gain, hyperinsulinemia, hepatic steatosis, and elevated markers of inflammation).44 In contrast, when feeding was time restricted to the active cycle, the mice were protected from the adverse metabolic changes, despite consuming identical numbers of calories.44 These data suggest that besides the caloric and nutrient composition of the diets, optimal control of timing for food consumption may also contribute significantly in determining metabolic outcomes.
Pancreatic release of insulin follows a circadian rhythm, peaking during the day in response to feeding and dropping at night during sleep.41 Although influenced by food intake, these rhythms operate independently and can anticipate regular changes in feeding behavior and/or activity.41 Recent evidence shows that cellular timing is critical for proper insulin release, and that a fundamental property of insulin-secreting beta cells is their capacity to synchronize, and function as rhythmic pacemakers.38, 40, 45 Interference with these beta cell rhythms may cause conditions that resemble T2D.45 Whole animal disruption of the circadian clock using CLOCKΔ19 mutants and BMAL1 knockouts leads to impaired glucose tolerance, deficits in insulin secretion, and excessive fat deposition,46, 47 indicating a major contribution of the circadian system to metabolic homeostasis. To disentangle the contributions of specific organ systems to these phenomena, more precise pancreatic beta cell-specific CLOCKΔ19 mutants and BMAL1 knockouts revealed that these beta cell clocks are directly responsible for the observed impairments in hyperglycemia, glucose tolerance, and GSIS.37 Moreover, it has been discovered that pancreatic clocks regulate the transcription of many of the genes responsible for the rhythmic release of insulin throughout the day,38 and that an intact circadian pacemaker intrinsic to beta cells is critical for regulating GSIS.48
Consistent with the animal data, disruptions in circadian cycles are a major risk factor for the development of obesity and metabolic health problems in humans.49 Epidemiological,50 observational51 and controlled laboratory studies52 have repeatedly demonstrated that disruption of circadian rhythms causes insulin resistance, elevated blood glucose and may ultimately lead to obesity and diabetes.53 Sleep loss has also been associated with metabolic disturbances.54, 55 These sleep and circadian disruptions are particularly problematic among populations engaged in shift work and/or frequent long haul travel—activities which disrupt rhythms, and, therefore, increase metabolic risk.23, 56, 57 Off-label prescription of APDs for insomnia has further exacerbated the preexisting metabolic risks stemming from job-related circadian disruptions within these populations,58 making this a particularly relevant public health issue. While the relationship of metabolic dysfunction to sleep is complex, circadian disruption may be an important factor. Understanding the biological mechanisms underlying these metabolic disturbances may shed light on several psychiatric illnesses where circadian disruptions are salient pathophysiological features.59
CNS circadian rhythms and metabolism
Disturbances in the dopamine and circadian systems have been implicated in the pathophysiology of BD and schizophrenia. Both disorders are associated with disruptions of sleep and activity, as well as obesity, independent of APD exposure.59, 60 Therefore, even in the absence of APD treatment, changes in circadian phase or loss of rhythms in the dopamine systems may contribute to metabolic problems in the mentally ill.59 Exposure to APDs may further worsen these metabolic effects, even as they treat psychiatric symptoms.61 Nevertheless, the precise mechanisms by which these systems contribute to metabolic dysfunction remain poorly understood.
There is evidence that CNS and peripheral circadian systems work closely with one another to maintain metabolic homeostasis.61, 62 The periphery communicates information to the CNS in a rhythmic manner. For example, adipocytes rhythmically release leptin, a neuroactive peptide that regulates satiety through its actions centrally in the ARC.35 When leptin rhythms are disrupted in mutant mice lacking both Per1 and Per2, or both Cry1 and Cry2, animals show profound, metabolic phenotypes (weight gain and weight loss, respectively). These changes are mediated by rhythmic behavior and feeding35 and highlight the role of the circadian system as a coordinator of physiology across peripheral organs and the CNS.
Metabolic homeostasis requires a balance between energy intake and expenditure.63, 64 Feeding behavior (intake) and locomotion (expenditure) have both motivational and motor aspects that are involved in striking this balance, and are controlled by two complementary dopamine systems in the striatum.65 Rhythmic dopamine signals that originate in the VTA and project to the ventral striatum [nucleus accumbens (NAc)] regulate the reward pathways underlying motivation, food craving, and anticipation.66 In parallel, dopamine neurons in the substantia nigra project to a distinct set of dorsal striatal neurons to regulate aspects of motor control, including locomotion. Similar to feeding, locomotor behaviors are rhythmic under constant conditions. Elimination of neurons projecting to the striatum using the dopamine-specific toxin 6-hydroxydopamine (6-OHDA) rendered locomotor activity arrhythmic, and disrupted the rhythmic expression of PER2 in the dorsal striatum, but not in the SCN.67
The ARC region of the hypothalamus also includes a distinct population of dopaminergic neurons that regulate satiety and appetitive behaviors.26, 68 The ARC exhibits strong rhythms in gene expression that shift phase in response to food deprivation.69 Furthermore, optogenetic stimulation of ARC dopaminergic neurons and D2R signaling in the ARC similarly regulates appetite and feeding behavior.13 Dopamine signaling also affects the rhythmic anticipatory behaviors that determine feeding time in mice.70 A significant component of this signaling is D2R/D3R-dependent, where receptor action affects the time of onset in feeding behaviors.71
Both D2R/D3R signaling and circadian pathways have been implicated in the temporal coordination of satiety and weight gain.72–75 Interestingly, repeated stimulation of the dopamine system by amphetamine administration is sufficient to sustain rhythmic anticipatory behaviors even when the SCN-driven master clock is impaired.76 This anticipation may reflect the activity of ultradian rhythm (i.e., shorter than 1 day) that are governed by the midbrain dopamine systems and striatal neurons. These rhythms typically run in 2–6 h cycles that harmonize with, and support the 24-h circadian rhythms. However, desynchronization of ultradian and circadian rhythms by excessive dopaminergic tone can lead to interference in rhythmic behaviors.77 Therefore, disruptions of the CNS dopamine and circadian systems may change reward systems in the NAc, alter satiety set points, and contribute to overeating and obesity.73, 75, 78 Overall, this evidence suggests that CNS dopamine, D2R and D3R play critical roles in mediating rhythmic feeding behaviors and satiety, and that the loss of circadian regulation may result in clinically relevant disturbances in maintaining weight control.
Dopamine receptors are localized to rhythmic brain areas
The bidirectional connections between the dopamine system and the circadian clock are determined in large part by D2R and D3R expression, which is widespread across brain regions that support circadian rhythms (Table 1). In particular, D2R/D3R expression is enriched in the striatum (NAc and caudate/putamen) and midbrain (substantia nigra, VTA). Expression of D2R (but not D3R) has been described in the ARC. Strikingly, there is no expression of D2R/D3R in the SCN. Correspondingly, there is a relative resistance of SCN rhythms to D2R/D3R signaling.79 Instead, dopamine D1 receptors (D1R) are the primary dopamine receptor in the SCN.80 These findings imply that there are dopaminergic mechanisms that distinguish SCN rhythms from the D2R/D3R-mediated mechanisms in the striatum and elsewhere in the hypothalamus.
Reciprocal links between dopamine signaling and the circadian clock
Dopamine neurotransmission in the brain is rhythmic and tightly regulated by the circadian clock.81 In the striatum, microdialysis experiments in animals indicate that dopamine release from presynaptic neurons undergoes rhythmic oscillations across the day.82 Similar work by multiple groups indicates that the regulatory sites underlying these oscillations may be distributed across multiple nodes in the dopamine system. In dopamine synthetic pathways of mouse midbrain neurons, circadian regulators CLOCK83 and REV-ERB84 regulate the expression of TH (the rate limiting step in dopamine biosynthesis). Moreover, in the striatum, D3R is expressed rhythmically under the control of the circadian regulator, NPAS2.66 Importantly, disrupting these circadian rhythms genetically or pharmacologically with APDs alters D3R expression and leads to behavioral disturbances affecting reward pathways.66 Finally, critical negative regulators of dopamine signaling are also rhythmically expressed throughout the day including the dopamine transporter82 as well as monoamine oxidase A.85
There is growing evidence showing that D2Rs and D3Rs are integrators of multiple signaling pathways including those associated with APD-induced metabolic abnormalities.61 Accordingly, the dopamine and circadian systems likely converge through their joint actions at dopamine receptors. As G-protein coupled receptors, both D2R and D3R have the capability of acting through both G-protein-dependent and -independent pathways.86 In the case of the G-protein-dependent pathways, D2R and D3R signaling is coupled to the downstream actions of stimulatory or inhibitory Gα subunits, which modulate intracellular levels of cyclic AMP (cAMP).87 G-protein independent/arrestin-dependent signaling modulates other classes of signaling molecules like the AKT kinase and intracellular calcium.86 These components of the dopamine signaling network provide inputs into the circadian clock. Indeed, we have shown previously that D1R modulate circadian period length in SCN slices from PER2::LUC mice,88 while others demonstrated that D2Rs and D3Rs affect modulation of the CLOCK/BMAL1 dimerization in the retina.89 Moreover, the same dopamine receptors determine the time of peak PER2 expression in the striatum.79
The extensive interplay between dopamine and circadian systems both in the CNS and periphery increases the probability that feeding behaviors and activity are coordinated. This ensures that dopamine-driven hunger and feeding behaviors occur at times of caloric need, to efficiently balance energy intake and expenditures. Misalignment of circadian rhythms results in metabolic changes similar to those induced by APDs, including changes in satiety, increased blood glucose and lipid levels, and the development of obesity and T2D.56 Taken together, temporal and reciprocal coordination between metabolic and dopamine systems may be critical to maintaining optimal control of insulin and blood glucose.
Clinical implications of reciprocal dopamine and circadian signaling
One of the most studied clinical models of dopamine signaling is Parkinson’s disease (PD). PD is characterized by a reduction of dopamine signaling in the dorsal striatum, leading to deficits in locomotion and cognition. Interestingly, in addition to these behavioral abnormalities, early clinical observations indicated that these patients also commonly exhibit disturbances in glucose homeostasis.90 Indeed, in PD patients, administration of L-DOPA, a dopamine precursor, acutely increased blood glucose.91 These data suggest that dopamine signaling may have physiological relevance beyond the CNS, including a role in glucose regulation and that disruption of this signaling may lead to pathological metabolic states. Emerging data from human clinical trials support a circadian and dopamine interaction in regulating, leptin, insulin, peripheral blood glucose and metabolism. Specifically, the D2R/D3R agonist bromocriptine has shown efficacy in T2D, and may act in part through a circadian mechanism.92 Bromocriptine has been shown in placebo-controlled studies to modulate circadian rhythms in obese subjects, reducing the peak amplitude and mean levels of rhythmic insulin levels across a 24-h cycle.93 Similar results have been reported for the effects of bromocriptine on rhythmic leptin levels, whereby bromocriptine treatment of obese subjects reduced the rhythm amplitude and mean levels of leptin over 24-h, and stimulated lipolysis.94 Since completion of these studies, bromocriptine has been approved by the FDA to treat T2D by restoring insulin sensitivity to target tissues. By elucidating the interactions between the dopamine and circadian systems, these bromocriptine studies may offer important preliminary clues to understand how APDs alter dopamine signaling and cause metabolic disease. However, considerably less is known about the effects of APDs at the convergence of dopamine and circadian pathways. There is a paucity of data to support the use of bromocriptine for the treatment of APD-induced metabolic disorders in psychiatric patients. The existing literature suggests that bromocriptine does not exacerbate psychosis in APD-treated patients,95–97 but larger studies to investigate the relative risks and benefits of dopaminergic agonists are clearly needed.
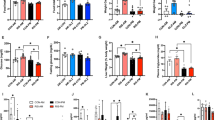
The data suggest that APDs may interfere with the coordination between circadian and metabolic systems to affect clinical outcomes in patients treated with APDs (Fig. 3). As a corollary, this also implies that the timing of dopamine blockade by APDs may determine their effects on brain and peripheral rhythms. In particular, given that a common side effect of APDs is somnolence, these medications are often dosed at night to promote sleep. Since rhythmic insulin release is typically lowest at night, blockade of dopamine signaling by APDs during this time would be expected to cause inappropriately high insulin release. This could ultimately lead to the activation of anabolic pathways during a period when catabolic pathways should predominate, and promotes the weight gain and insulin resistance commonly observed during APD administration (Fig. 4).
Bidirectional connections link circadian clock genes to dopamine. Rhythmic control of dopamine synthesis and signaling in pancreatic beta cells may be one mechanism by which insulin rhythms are maintained. In blocking dopamine signaling, APDs may interfere with (1) rhythmic insulin secretion and (2) dopamine receptor feedback to the beta cell circadian clock. The timing of feeding behaviors may influence rhythmic release of peripheral insulin
Model for antipsychotic drug disruption of circadian rhythms in insulin secretion. Insulin secretion follows a diurnal pattern with peaks during the day and lowest levels at night, corresponding to metabolic demands, periods of fasting and feeding behaviors in humans. By blocking dopamine D2 and D3 receptors, antipsychotic drugs (APDs) decrease the ability of dopamine receptors to negatively regulate insulin levels, raising overall insulin levels. At night time, during periods where catabolic states normally predominate, changes in insulin release by these drugs may be especially evident. Unique biological and pharmacological properties of different APDs (e.g., half-life) may alter the effects on insulin rhythms
We ultimately hypothesize that APD blockade of D2R and D3R disrupts circadian rhythms, disturbs the coordination of insulin release and feeding behaviors across the day in the CNS and pancreatic islet cells, and thereby induces metabolic dysfunction. This opens the door to several important questions: (1) Do APDs contribute to APD-induced metabolic disease by disrupting peripheral pancreatic circadian rhythms? Are these drug-induced disturbances dependent on pancreatic D2R/D3R? (2) By acting on D2R/D3Rs in the CNS, do APDs disturb circadian rhythms in brain regions that regulate feeding and activity to produce the changes in satiety and feeding that contribute to APD-induced obesity and metabolic disturbances? (3) What are the relative contributions of CNS and peripheral circadian D2R/D3R signaling to APD-induced disturbances to metabolism in vivo, and are there synergistic effects across CNS and peripheral mechanisms? (4) Do changes to the timing of administration alter the propensity of APDs to cause weight gain and metabolic dysfunction in humans?
Future directions
Though much work has been done examining the dopamine and circadian systems individually, considerably more remains to be done in elucidating the interplay between these systems and its relevance to APD-induced metabolic disturbances. Given the importance of these two systems in the CNS and peripheral organs, it will be crucial to clarify their respective contributions both to behavioral and endocrine drivers of metabolic regulation. Understanding these factors will also shed considerable light on APD-induced metabolic disease. In the longer term, this knowledge may directly lead to the development of inexpensive and readily implemented treatment strategies to mitigate APDs’ metabolic side effects and reduce the morbidity and mortality from medication-associated T2D and cardiovascular disease. With fewer metabolic side effects, time-based interventions may also improve treatment compliance for disorders ranging from schizophrenia and BD to PTSD. Moreover, understanding interactions between dopamine and the circadian clock to regulate insulin release and feeding may also significantly contribute to our fundamental understanding of obesity and lead to novel treatments. Ultimately, further elucidating the mechanisms of APD-induced weight gain may also lead to better treatments for diabetes and obesity, which will directly impact the health of APD-treated patients.
References
Mohamed, S., Leslie, D. L. & Rosenheck, R. A. Use of antipsychotics in the treatment of major depressive disorder in the U.S. Department of Veterans Affairs. J. Clin. Psychiatry. 70, 906–912, doi:10.4088/JCP.08m04450 (2009).
Domino, M. E. & Swartz, M. S. Who are the new users of antipsychotic medications? Psychiatr. Serv. 59, 507–514, doi:10.1176/ps.59.5.507 (2008).
Newcomer, J. W. Metabolic considerations in the use of antipsychotic medications: a review of recent evidence. J. Clin. Psychiatry 68 Suppl 1, 20–27 (2007).
Fleischhacker, W. W. et al. Metabolic risk factors in first-episode schizophrenia: baseline prevalence and course analysed from the European First-Episode Schizophrenia Trial. Int. J. Neuropsychopharmacol. 1–9, doi: 10.1017/S1461145712001241 (2012).
Laursen, T. M., Munk-Olsen, T., Nordentoft, M. & Mortensen, P. B. Increased mortality among patients admitted with major psychiatric disorders: a register-based study comparing mortality in unipolar depressive disorder, bipolar affective disorder, schizoaffective disorder, and schizophrenia. J. Clin. Psychiatry 68, 899–907 (2007).
Goldstein, B. I., Schaffer, A., Wang, S. & Blanco, C. Excessive and premature new-onset cardiovascular disease among adults with bipolar disorder in the US NESARC cohort. J. Clin. Psychiatry 76, 163–169, doi:10.4088/JCP.14m09300 (2015).
Weiner, M., Warren, L. & Fiedorowicz, J. G. Cardiovascular morbidity and mortality in bipolar disorder. Ann. Clin. Psychiatry 23, 40–47 (2011).
Kroeze, W. K. et al. H1-histamine receptor affinity predicts short-term weight gain for typical and atypical antipsychotic drugs. Neuropsychopharmacology 28, 519–526, doi:10.1038/sj.npp.1300027 (2003).
Strange, P. G. Antipsychotic drug action: antagonism, inverse agonism or partial agonism. Trends Pharmacol. Sci. 29, 314–321, doi:10.1016/j.tips.2008.03.009 (2008).
Hall, D. A. & Strange, P. G. Evidence that antipsychotic drugs are inverse agonists at D2 dopamine receptors. Br. J. Pharmacol. 121, 731–736, doi:10.1038/sj.bjp.0701196 (1997).
Sulzer, D., Cragg, S. J. & Rice, M. E. Striatal dopamine neurotransmission: regulation of release and uptake. Basal Ganglia 6, 123–148, doi:10.1016/j.baga.2016.02.001 (2016).
Do, J., Kim, J. I., Bakes, J., Lee, K. & Kaang, B. K. Functional roles of neurotransmitters and neuromodulators in the dorsal striatum. Learn. Mem. (Cold Spring Harbor, N.Y.) 20, 21–28, doi:10.1101/lm.025015.111 (2012).
Zhang, X. & van den Pol, A. N. Hypothalamic arcuate nucleus tyrosine hydroxylase neurons play orexigenic role in energy homeostasis. Nat. Neurosci.. doi:10.1038/nn.4372 (2016).
Myers, M. G. Jr. & Olson, D. P. Central nervous system control of metabolism. Nature 491, 357–363, doi:10.1038/nature11705 (2012).
Marco, A., Schroeder, M. & Weller, A. Feeding and reward: ontogenetic changes in an animal model of obesity. Neuropharmacology. 62, 2447–2454, doi:10.1016/j.neuropharm.2012.02.019 (2012).
Kern, A., Albarran-Zeckler, R., Walsh, H. E. & Smith, R. G. Apo-ghrelin receptor forms heteromers with DRD2 in hypothalamic neurons and is essential for anorexigenic effects of DRD2 agonism. Neuron. 73, 317–332, doi:10.1016/j.neuron.2011.10.038 (2012).
Rubi, B. et al. Dopamine D2-like receptors are expressed in pancreatic beta cells and mediate inhibition of insulin secretion. J. Biol. Chem. 280, 36824–36832. doi:10.1074/jbc.M505560200 (2005).
Simpson, N. et al. Dopamine-mediated autocrine inhibitory circuit regulating human insulin secretion in vitro. Mol. Endocrinol. 26, 1757–1772, doi:10.1210/me.2012-1101 (2012).
Ustione, A. & Piston, D. W. Dopamine synthesis and D3 receptor activation in pancreatic beta-cells regulates insulin secretion and intracellular [Ca(2+)] oscillations. Mol. Endocrinol. 26, 1928–1940, doi:10.1210/me.2012-1226 (2012).
Farino, Z. J. et al. Development of a Rapid Insulin Assay by Homogenous Time-Resolved Fluorescence. PLoS ONE 11, e0148684, doi:10.1371/journal.pone.0148684 (2016).
Mehran, A. E. et al. Hyperinsulinemia drives diet-induced obesity independently of brain insulin production. Cell Metab. 16, 723–737, doi:10.1016/j.cmet.2012.10.019 (2012).
Reynolds, G. P. & Kirk, S. L. Metabolic side effects of antipsychotic drug treatment--pharmacological mechanisms. Pharmacol. Ther. 125, 169–179, doi:10.1016/j.pharmthera.2009.10.010 (2010).
Bass, J. & Takahashi, J. S. Circadian integration of metabolism and energetics. Science 330, 1349–1354, doi:10.1126/science.1195027 (2010).
Altimus, C. M. et al. Rod photoreceptors drive circadian photoentrainment across a wide range of light intensities. Nat. Neurosci. 13, 1107–1112, doi:10.1038/nn.2617 (2010).
Natsubori, A., Honma, K. & Honma, S. Differential responses of circadian Per2 rhythms in cultured slices of discrete brain areas from rats showing internal desynchronisation by methamphetamine. Eur. J. Neurosci. 38, 2566–2571, doi:10.1111/ejn.12265 (2013).
Guilding, C., Hughes, A. T., Brown, T. M., Namvar, S. & Piggins, H. D. A riot of rhythms: neuronal and glial circadian oscillators in the mediobasal hypothalamus. Mol. Brain 2, 28, doi:10.1186/1756-6606-2-28 (2009).
Landgraf, D., Long, J. E. & Welsh, D. K. Depression-like behaviour in mice is associated with disrupted circadian rhythms in nucleus accumbens and periaqueductal grey. Eur. J. Neurosci. 43, 1309–1320, doi:10.1111/ejn.13085 (2016).
Mohawk, J. A., Green, C. B. & Takahashi, J. S. Central and peripheral circadian clocks in mammals. Annu. Rev. Neurosci. 35, 445–462, doi:10.1146/annurev-neuro-060909-153128 (2012).
Landgraf, D., Wang, L. L., Diemer, T. & Welsh, D. K. NPAS2 compensates for loss of CLOCK in peripheral circadian oscillators. PLoS Genet. 12, e1005882, doi:10.1371/journal.pgen.1005882 (2016).
Cho, H. et al. Regulation of circadian behaviour and metabolism by REV-ERB-alpha and REV-ERB-beta. Nature 485, 123–127, doi:10.1038/nature11048 (2012).
Partch, C. L., Green, C. B. & Takahashi, J. S. Molecular architecture of the mammalian circadian clock. Trends Cell Biol. 24, 90–99, doi:10.1016/j.tcb.2013.07.002 (2014).
Hayashi, Y., Sanada, K., Hirota, T., Shimizu, F. & Fukada, Y. p38 mitogen-activated protein kinase regulates oscillation of chick pineal circadian clock. J. Biol. Chem. 278, 25166–25171, doi:10.1074/jbc.M212726200 (2003).
Stokkan, K. A., Yamazaki, S., Tei, H., Sakaki, Y. & Menaker, M. Entrainment of the circadian clock in the liver by feeding. Science 291, 490–493, doi:10.1126/science.291.5503.490 (2001).
Paschos, G. K. et al. Obesity in mice with adipocyte-specific deletion of clock component Arntl. Nat. Med. 18, 1768–1777, doi:10.1038/nm.2979 (2012).
Kettner, N. M. et al. Circadian dysfunction induces leptin resistance in mice. Cell Metab. 22, 448–459, doi:10.1016/j.cmet.2015.06.005 (2015).
Lamia, K. A., Storch, K. F. & Weitz, C. J. Physiological significance of a peripheral tissue circadian clock. Proc. Natl Acad. Sci. U.S.A. 105, 15172–15177, doi:10.1073/pnas.0806717105 (2008).
Marcheva, B. et al. Disruption of the clock components CLOCK and BMAL1 leads to hypoinsulinaemia and diabetes. Nature 466, 627–631, doi:10.1038/nature09253 (2010).
Perelis, M. et al. Pancreatic beta cell enhancers regulate rhythmic transcription of genes controlling insulin secretion. Science 350, aac4250, doi:10.1126/science.aac4250 (2015).
Liu, J. et al. CLOCK and BMAL1 regulate muscle insulin sensitivity via SIRT1 in male mice. Endocrinology, en20152027, doi:10.1210/en.2015-2027 (2016).
Panda, S. Circadian physiology of metabolism. Science 354, 1008–1015, doi:10.1126/science.aah4967 (2016).
McGinnis, G. R. & Young, M. E. Circadian regulation of metabolic homeostasis: causes and consequences. Nat. Sci. Sleep 8, 163–180, doi:10.2147/nss.s78946 (2016).
Bray, M. S. et al. Time-of-day-dependent dietary fat consumption influences multiple cardiometabolic syndrome parameters in mice. Int. J. Obes. (Lond). 34, 1589–1598, doi:10.1038/ijo.2010.63 (2010).
Arble, D. M., Bass, J., Laposky, A. D., Vitaterna, M. H. & Turek, F. W. Circadian timing of food intake contributes to weight gain. Obesity (Silver. Spring). 17, 2100–2102, doi:10.1038/oby.2009.264 (2009).
Hatori, M. et al. Time-restricted feeding without reducing caloric intake prevents metabolic diseases in mice fed a high-fat diet. Cell Metab. 15, 848–860, doi:10.1016/j.cmet.2012.04.019 (2012).
Johnston, N. R. et al. Beta cell hubs dictate pancreatic islet responses to glucose. Cell Metab. 24, 389–401, doi:10.1016/j.cmet.2016.06.020 (2016).
Turek, F. W. et al. Obesity and metabolic syndrome in circadian Clock mutant mice. Science 308, 1043–1045, doi:10.1126/science.1108750 (2005).
Rudic, R. D. et al. BMAL1 and CLOCK, two essential components of the circadian clock, are involved in glucose homeostasis. PLoS Biol. 2, e377, doi:10.1371/journal.pbio.0020377 (2004).
Lee, J. et al. Bmal1 and beta-cell clock are required for adaptation to circadian disruption, and their loss of function leads to oxidative stress-induced beta-cell failure in mice. Mol. Cell Biol. 33, 2327–2338, doi:10.1128/MCB.01421-12 (2013).
Bayon, V., Leger, D., Gomez-Merino, D., Vecchierini, M. F. & Chennaoui, M. Sleep debt and obesity. Ann. Med. 46, 264–272, doi:10.3109/07853890.2014.931103 (2014).
Buxton, O. M. & Marcelli, E. Short and long sleep are positively associated with obesity, diabetes, hypertension, and cardiovascular disease among adults in the United States. Soc. Sci. Med. 71, 1027–1036, doi:10.1016/j.socscimed.2010.05.041 (2010).
Wong, P. M., Hasler, B. P., Kamarck, T. W., Muldoon, M. F. & Manuck, S. B. Social jetlag, chronotype, and cardiometabolic risk. J. Clin. Endocrinol. Metab. 100, 4612–4620, doi:10.1210/jc.2015-2923 (2015).
Buxton, O. M. et al. Adverse metabolic consequences in humans of prolonged sleep restriction combined with circadian disruption. Sci. Transl. Med. 4, 129ra143, doi:10.1126/scitranslmed.3003200 (2012).
Dibner, C. & Schibler, U. Circadian timing of metabolism in animal models and humans. J. Intern. Med. 277, 513–527, doi:10.1111/joim.12347 (2015).
Broussard, J. L. & Van Cauter, E. Disturbances of sleep and circadian rhythms: novel risk factors for obesity. Curr. Opin. Endocrinol. Diabetes Obes. 23, 353–359, doi:10.1097/med.0000000000000276 (2016).
Cedernaes, J., Schioth, H. B. & Benedict, C. Determinants of shortened, disrupted, and mistimed sleep and associated metabolic health consequences in healthy humans. Diabetes 64, 1073–1080, doi:10.2337/db14-1475 (2015).
McHill, A. W. et al. Impact of circadian misalignment on energy metabolism during simulated nightshift work. Proc. Natl Acad. Sci. U. S. A. 111, 17302–17307, doi:10.1073/pnas.1412021111 (2014).
Molzof, H. E. et al. The impact of meal timing on cardiometabolic syndrome indicators in shift workers. Chronobiol. Int. 1–12, doi:10.1080/07420528.2016.1259242 (2017).
Thompson, W., Quay, T. A., Rojas-Fernandez, C., Farrell, B. & Bjerre, L. M. Atypical antipsychotics for insomnia: a systematic review. Sleep Med. 22, 13–17, doi:10.1016/j.sleep.2016.04.003 (2016).
Barandas, R., Landgraf, D., McCarthy, M. J. & Welsh, D. K. Circadian clocks as modulators of metabolic comorbidity in psychiatric disorders. Curr. Psychiatry Rep. 17, 98, doi:10.1007/s11920-015-0637-2 (2015).
Landgraf, D., McCarthy, M. J. & Welsh, D. K. Circadian clock and stress interactions in the molecular biology of psychiatric disorders. Curr. Psychiatry Rep. 16, 483, doi:10.1007/s11920-014-0483-7 (2014).
Ballon, J. S., Pajvani, U., Freyberg, Z., Leibel, R. L. & Lieberman, J. A. Molecular pathophysiology of metabolic effects of antipsychotic medications. Trends Endocrinol. Metab. doi:10.1016/j.tem.2014.07.004 (2014).
Shibata, S. Circadian rhythms in the CNS and peripheral clock disorders: preface. J. Pharmacol. Sci. 103, 133 (2007).
Galgani, J. & Ravussin, E. Energy metabolism, fuel selection and body weight regulation. Int. J. Obes. (Lond). 32 Suppl 7, S109–S119, doi:10.1038/ijo.2008.246 (2008).
Frago, L. M. & Chowen, J. A. Hypothalamic leptin and ghrelin signaling as targets for improvement in metabolic control. Curr. Pharm. Des. 21, 3596–3605 (2015).
Baik, J. H. Dopamine signaling in reward-related behaviors. Front. Neural Circuits 7, 152, doi:10.3389/fncir.2013.00152 (2013).
Ozburn, A. R. et al. Direct regulation of diurnal Drd3 expression and cocaine reward by NPAS2. Biol. Psychiatry 77, 425–433, doi:10.1016/j.biopsych.2014.07.030 (2015).
Gravotta, L., Gavrila, A. M., Hood, S. & Amir, S. Global depletion of dopamine using intracerebroventricular 6-hydroxydopamine injection disrupts normal circadian wheel-running patterns and PERIOD2 expression in the rat forebrain. J. Mol. Neurosci. 45, 162–171, doi:10.1007/s12031-011-9520-8 (2011).
Romero-Fernandez, W. et al. Dopamine D1 and D2 receptor immunoreactivities in the arcuate-median eminence complex and their link to the tubero-infundibular dopamine neurons. Eur. J. Histochem. 58, 2400, doi:10.4081/ejh.2014.2400 (2014).
Guilding, C., Hughes, A. T., Brown, T. M., Namvar, S. & Piggins, H. D. A riot of rhythms: neuronal and glial circadian oscillators in the mediobasal hypothalamus. Mol. Brain 2, 28, doi:10.1186/1756-6606-2-28 (2009).
Liu, Y. Y. et al. Dopamine is involved in food-anticipatory activity in mice. J. Biol. Rhythms 27, 398–409, doi:10.1177/0748730412455913 (2012).
Smit, A. N., Patton, D. F., Michalik, M., Opiol, H. & Mistlberger, R. E. Dopaminergic regulation of circadian food anticipatory activity rhythms in the rat. PLoS ONE 8, e82381, doi:10.1371/journal.pone.0082381 (2013).
Sun, X. et al. Basolateral amygdala response to food cues in the absence of hunger is associated with weight gain susceptibility. J. Neurosci. 35, 7964–7976, doi:10.1523/jneurosci.3884-14.2015 (2015).
Epstein, L. H. et al. Food reinforcement, the dopamine D2 receptor genotype, and energy intake in obese and nonobese humans. Behav. Neurosci. 121, 877–886, doi:10.1037/0735-7044.121.5.877 (2007).
Sargent, C., Zhou, X., Matthews, R. W., Darwent, D. & Roach, G. D. Daily rhythms of hunger and satiety in healthy men during one week of sleep restriction and circadian misalignment. Int. J. Environ. Res. Public Health 13, 170, doi:10.3390/ijerph13020170 (2016).
Shukla, C. & Basheer, R. Metabolic signals in sleep regulation: recent insights. Nat. Sci. Sleep 8, 9–20, doi:10.2147/nss.s62365 (2016).
Mohawk, J. A., Baer, M. L. & Menaker, M. The methamphetamine-sensitive circadian oscillator does not employ canonical clock genes. Proc. Natl Acad. Sci. U. S. A. 106, 3519–3524, doi:10.1073/pnas.0813366106 (2009).
Blum, I. D. et al. A highly tunable dopaminergic oscillator generates ultradian rhythms of behavioral arousal. Elife 3, doi:10.7554/eLife.05105 (2014).
Luck, C., Vitaterna, M. H. & Wevrick, R. Dopamine pathway imbalance in mice lacking Magel2, a Prader-Willi syndrome candidate gene. Behav. Neurosci. 130, 448–459, doi:10.1037/bne0000150 (2016).
Hood, S. et al. Endogenous dopamine regulates the rhythm of expression of the clock protein PER2 in the rat dorsal striatum via daily activation of D2 dopamine receptors. J. Neurosci. 30, 14046–14058, doi:10.1523/jneurosci.2128-10.2010 (2010).
Duffield, G. E., McNulty, S. & Ebling, F. J. Anatomical and functional characterisation of a dopaminergic system in the suprachiasmatic nucleus of the neonatal Siberian hamster. J. Comp. Neurol. 408, 73–96 (1999).
Mendoza, J. & Challet, E. Circadian insights into dopamine mechanisms. Neuroscience 282, 230–242, doi:10.1016/j.neuroscience.2014.07.081 (2014).
Ferris, M. J. et al. Dopamine transporters govern diurnal variation in extracellular dopamine tone. Proc. Natl Acad. Sci. U.S.A. 111, E2751–E2759, doi:10.1073/pnas.1407935111 (2014).
Sidor, M. M. et al. Daytime spikes in dopaminergic activity drive rapid mood-cycling in mice. Mol. Psychiatry 20, 1406–1419, doi:10.1038/mp.2014.167 (2015).
Chung, S. et al. Impact of circadian nuclear receptor REV-ERBalpha on midbrain dopamine production and mood regulation. Cell 157, 858–868, doi:10.1016/j.cell.2014.03.039 (2014).
Huang, J. et al. Circadian modulation of dopamine levels and dopaminergic neuron development contributes to attention deficiency and hyperactive behavior. J. Neurosci. 35, 2572–2587, doi:10.1523/jneurosci.2551-14.2015 (2015).
Beaulieu, J. M., Gainetdinov, R. R. & Caron, M. G. The Akt-GSK-3 signaling cascade in the actions of dopamine. Trends Pharmacol. Sci. 28, 166–172, doi:10.1016/j.tips.2007.02.006 (2007).
Beaulieu, J. M. & Gainetdinov, R. R. The physiology, signaling, and pharmacology of dopamine receptors. Pharmacol. Rev. 63, 182–217, doi:10.1124/pr.110.002642 (2011).
Landgraf, D. et al. The mood stabilizer valproic acid opposes the effects of dopamine on circadian rhythms. Neuropharmacology 107, 262–270, doi:10.1016/j.neuropharm.2016.03.047 (2016).
Yujnovsky, I., Hirayama, J., Doi, M., Borrelli, E. & Sassone-Corsi, P. Signaling mediated by the dopamine D2 receptor potentiates circadian regulation by CLOCK:BMAL1. Proc. Natl Acad. Sci. U.S.A. 103, 6386–6391, doi:10.1073/pnas.0510691103 (2006).
Ustione, A., Piston, D. W. & Harris, P. E. Minireview: Dopaminergic regulation of insulin secretion from the pancreatic islet. Mol. Endocrinol. 27, 1198–1207, doi:10.1210/me.2013-1083 (2013).
Sirtori, C. R., Bolme, P. & Azarnoff, D. L. Metabolic responses to acute and chronic L-dopa administration in patients with parkinsonism. N. Engl. J. Med. 287, 729–733, doi:10.1056/nejm197210122871501 (1972).
Shivaprasad, C. & Kalra, S. Bromocriptine in type 2 diabetes mellitus. Indian J. Endocrinol. Metab. 15, S17–S24, doi:10.4103/2230-8210.83058 (2011).
Kok, P. et al. Activation of dopamine D2 receptors simultaneously ameliorates various metabolic features of obese women. Am. J. Physiol. Endocrinol. Metab. 291, E1038–E1043, doi:10.1152/ajpendo.00567.2005 (2006).
Kok, P. et al. Activation of dopamine D2 receptors lowers circadian leptin concentrations in obese women. J. Clin. Endocrinol. Metab. 91, 3236–3240, doi:10.1210/jc.2005-2529 (2006).
Perovich, R. M., Lieberman, J. A., Fleischhacker, W. W. & Alvir, J. The behavioral toxicity of bromocriptine in patients with psychiatric illness. J. Clin. Psychopharmacol. 9, 417–422 (1989).
Lieberman, J. A., Alvir, J., Mukherjee, S. & Kane, J. M. Treatment of tardive dyskinesia with bromocriptine. A test of the receptor modification strategy. Arch. Gen. Psychiatry. 46, 908–913 (1989).
Lee, M. S. et al. Effect of bromocriptine on antipsychotic drug-induced hyperprolactinemia: eight-week randomized, single-blind, placebo-controlled, multicenter study. Psychiatry. Clin. Neurosci. 64, 19–27, doi:10.1111/j.1440-1819.2009.02032.x (2010).
Bouthenet, M. L. et al. Localization of dopamine D3 receptor mRNA in the rat brain using in situ hybridization histochemistry: comparison with dopamine D2 receptor mRNA. Brain Res. 564, 203–219 (1991).
Gurevich, E. V. & Joyce, J. N. Distribution of dopamine D3 receptor expressing neurons in the human forebrain: comparison with D2 receptor expressing neurons. Neuropsychopharmacology 20, 60–80, doi:10.1016/s0893-133x(98)00066-9 (1999).
Acknowledgements
This work is supported by a Department of Defense PRMRP Investigator Initiated Award PR141292 and the John F. and Nancy A. Emmerling Fund of The Pittsburgh Foundation (to ZF) as well as a Department of Veterans Affairs Career Development Award 1IK2BX001275 (to M.J.M.). We thank Drs. David Lewis, Yanhua Huang, Robert Sweet, Ann Germaine, Colleen McClung, and David Welsh for helpful comments during the development of the work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Freyberg, Z., McCarthy, M. Dopamine D2 receptors and the circadian clock reciprocally mediate antipsychotic drug-induced metabolic disturbances. npj Schizophr 3, 17 (2017). https://doi.org/10.1038/s41537-017-0018-4
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41537-017-0018-4