Abstract
L-type voltage-gated calcium channels are involved in multiple physiological functions. Currently available antagonists do not discriminate between L-type channel isoforms. Importantly, no selective blocker is available to dissect the role of L-type isoforms Cav1.2 and Cav1.3 that are concomitantly co-expressed in the heart, neuroendocrine and neuronal cells. Here we show that calciseptine, a snake toxin purified from mamba venom, selectively blocks Cav1.2 -mediated L-type calcium currents (ICaL) at concentrations leaving Cav1.3-mediated ICaL unaffected in both native cardiac myocytes and HEK-293T cells expressing recombinant Cav1.2 and Cav1.3 channels. Functionally, calciseptine potently inhibits cardiac contraction without altering the pacemaker activity in sino-atrial node cells, underscoring differential roles of Cav1.2− and Cav1.3 in cardiac contractility and automaticity. In summary, calciseptine is a selective L-type Cav1.2 Ca2+ channel blocker and should be a valuable tool to dissect the role of these L-channel isoforms.
Similar content being viewed by others
Introduction
By mediating calcium influx in a wide range of cell types, voltage-gated calcium channels (VGCCs) are critically involved in many physiological functions, including contraction in cardiac and smooth muscles, hormone secretion in endocrine cells, synaptic transmission in neurons, gene transcription and regulation of enzyme activity (for review see1, 2). VGCCs have been classified in three families, based on the pore-forming α1 subunit, i.e. Cav1, Cav2 and Cav33. VGCCs are hetero-oligomeric complexes constituted by the α1-subunits defining the Ca2+ channel subtype associated to different ancillary subunits (α2δ, β, and γ). The Cav1 family is formed by four distinct α1 subunit isoforms (Cav1.1-Cav1.4) underlying “long-lasting” (L)-type Ca2+ currents. The Cav2 family includes three α1 isoforms (Cav2.1-Cav2.3) encoding “high-voltage activated” Ca2+ currents referred to as P/Q-type, N-type and R-type. The Cav3 family of α1 subunit isoforms (Cav3.1 through Cav3.3) mediates “low-voltage activated” transient (T)-type Ca2+ currents and is not associated to ancillary subunits. While Cav2 channel isoforms are highly expressed in the nervous system1, cardiomyocytes can express T-type and L-type Ca2+ channels underlying ICaT and ICaL, respectively4.
The heart expresses two L-type Ca2+ channels isoforms, Cav1.2 and Cav1.35. Cav1.2 is ubiquitously expressed in the heart ventricular and supraventricular chambers, as well as in the sinoatrial (SAN) and atrioventricular (AVN) nodes5. Cav1.2 is also the predominant L-type isoform in adult ventricle, where it couples excitation to contraction and constitutes the target of the cAMP/PKA mediated positive inotropic effect on cardiac contractility exerted by catecholamines6, 7. Cav1.3 is expressed in the atria and is strongly expressed in the SAN and AVN. Cav1.3 plays a major role in SAN pacemaker activity and impulse conduction through the AVN. In this respect, mice in which Cav1.3 has been genetically ablated (Cav1.3−/−) show prominent SAN bradycardia, susceptibility to atrial fibrillation and atrioventricular blocks8, 9. In SAN pacemaker myocytes, Cav1.3-mediated ICaL (ICav1.3) is characterized by a more negative activation threshold and slower inactivation kinetics than Cav1.2-mediated ICaL (ICav1.2) and is essential for the generation of diastolic depolarization underlying SAN automaticity8, 10 (for review see11).
Despite the importance of dissecting the physiopathological roles of Cav1.2 and Cav1.3 channels in cardiac myocytes and neuronal cells, no selective pharmacological tool is currently available. Both Cav1.2 and Cav1.3 are sensitive to antagonist and agonist dihydropyridines (DHPs) and to non-DHP drugs, such as phenylalkylamine (i.e. Verapamil) and benzothiazepine-like compounds (i.e. Diltiazem) without significant selectivity1.
Animal venoms constitute an immense reservoir for identification of new toxins and toxin-derived tools for modulating the physiological function of ion channels. In particular, toxins showing three-fingers molecular scaffold class include several cardiotoxic peptides that abound in snake venoms. Three fingers toxin peptides potently block a variety of proteins including nicotinic receptors12, acetylcholinesterase13, acid-sensitive ion channels (ASIC)14, as well as cytotoxins that disrupt the lipid membrane15. More than 30 years ago, M. Lazdunski ‘s group purified a 60-amino acid three-fingers polypeptide from the venom of the black mamba (Dendroaspis polylepis) called calciseptine (Cas). Cas was shown to selectively block ICaL, to abolish all contraction in portal vein, thoracic aorta and uterine smooth muscle and to completely eliminate cardiac contractions16. These properties constitute clear adaptation to snake’s predatory behavior to induce very rapid and robust hypotension and dramatic negative inotropic effect in the prey, also in combination with the effects of the other venom components. Interestingly, Cas specifically blocks ICaL, without affecting N-type, T-type and also the skeletal muscle (Cav1.1) L-type Ca2+ channels isoforms16. In addition, previous data show that Cas does not affect voltage sensitive Na+ and K+ channels in cardiac ventricular cells, NlE115 neuroblastoma cells, RINmSF and HIT insulinomas and chicken dorsal root ganglia16.
In this work, we show that Cas selectively blocks Cav1.2 channels, while Cav1.3 is resistant to Cas. We show that Cas potently decreases cardiac contractility without affecting heart rate of Langendorff-perfused mouse heart. In line with potent inhibition of contraction, Cas blocks ICav1.2 in mouse ventricular myocytes. We show that while Cas partially inhibits total ICaL (ICav1.2+ICav1.3) in SAN myocytes from wild-type mice, it totally blocks ICaL in myocytes from Cav1.3−/− counterparts, where only Cav1.2 is functional. Selectivity of Cas blockade of Cav1.2 versus Cav1.3 is confirmed in HEK-293T expressing recombinant Cav1.2, Cav1.3 channels. Notably, the currents mediated by both Cav1.342a and Cav1.342 splice variants—-characterized by short and long C-terminus, respectively17- are totally resistant to Cas. Finally, while DHP nifedipine robustly slows pacemaker activity of SAN myocytes, selective blockade of ICav1.2 by Cas reduces the action potential amplitude, leaving unaffected the cell firing rate. In conclusion, our study shows that Cas selectively blocks Cav1.2 channels in the heart, providing an important tool in the panel of calcium channel modulators to help dissect the role of this channel isoform in heart physiology and automaticity.
Results
Calciseptine inhibited contraction and spared automaticity of Langendorff perfused hearts
We studied the effects of Cas on cardiac contractility and automaticity in isolated hearts from mice before and after perfusion of native toxin (100 nM). Perfusion of Cas strongly reduced left ventricular (LV) contraction amplitude (51 ± 3 mmHg vs 9 ± 2 mmHg. Fig. 1a, b), without changing baseline diastolic pressure (8 ± 2 mmHg vs 8 ± 3 mmHg. Fig. 1a, b). Averaged inter-beat (RR) intervals were not affected by toxin perfusion (273 ± 17 ms vs 271 ± 17 ms, p > 0.05. Fig. 1c), indicating that Cas did not disrupt the cardiac pacemaker mechanism (automaticity). In addition, we did not observe episodes of arrhythmia upon perfusion of Cas. We then evaluated the effects of Cas on heart inotropism and lusitropism by measuring the contraction velocity (dP/dt max) and the relaxation velocity (dP/dt min), respectively. Perfusion of Cas (100 nM), significantly reduced dP/dt max (1.7 ± 0.2 mmHg/ms vs 0.4 ± 0.1 mmHg/ms) and dP/dt min (−1.2 ± 0.1 mmHg/ms vs −0.1 ± 0.1 mmHg/ms), indicating negative inotropic and lusitropic effects of the toxin (Fig. 1d). Furthermore, relaxation time constant (Ƭ) and time-to-peak interval (or time to maximal pressure), parameters related to contraction duration, were not affected by perfusion of Cas (10 ± 1 ms vs 13 ± 2 ms, and 54 ± 1 ms vs 50 ± 3 ms, respectively. Supplementary Fig. 1). Taken together these data demonstrated differential effect of Cas on heart contractility and automaticity, two distinct functions that are reliant on L-type voltage dependent Ca2+ channels subtypes expression and regulation.
a Time course of isolated perfused heart (n = 5) contraction amplitude recording before and after Cas 100 nM application. b Sample traces of pressure recordings (left) and histograms of left ventricular (LV) contraction amplitude and basal diastolic LV pressure before and after toxin perfusion (n = 5). c Representative ECG traces and averaged RR recorded from isolated perfused heart (n = 5) in ctrl condition and in presence of 100 nM Cas. d Sample traces of first derivative of LV pressure signal before and after toxin perfusion (left) and bar graphs showing inotropic (dP/dtmax) and lusitropic (dP/dtmin) negative effect of Cas 100 nM (right, n = 5). Statistics: paired two-sided Student t-test. Data are presented as mean values ± SEM.
Calciseptine potently and selectively blocked L-type Ca2+ current (ICav1.2) in isolated ventricular myocytes and ICav1.2 in HEK-293T cells expressing Cav1.2
We evaluated the effects of Cas on isolated adult mouse ventricular myocytes in which ICaL is mediated by Cav1.2 (ICav1.2)8. For voltages ranging from −25 mV to +40 mV, ICav1.2 in rod-shape ventricular myocytes was dose-dependently reduced by perfusion of Cas (Fig. 2). Application of nifedipine (3 µM), blocked residual Ca2+ current in myocytes exposed to Cas 100 nM and Cas 300 nM, but failed to have an effect when cells were previously perfused with Cas 1 µM (Supplementary Fig. 2).
a Representative Ca2+ current traces of the L-type Ca2+ current measured from a holding potential of −55 mV in Tyrode (black traces), or under Cas 100 nM (gray traces), Cas 300 nM (red traces), Cas 1 µM (blue traces) and Nife 3 µM (dotted black traces) perfusion in freshly isolated ventricular Wild-Type cardiomyocytes. Voltage clamp step protocol is reported in the inset of a. b Current-to-voltage (I–V) relationship of L-type Ca2+ current (Cav1.2) recorded from holding potential of −55 mV in ventricular cells before (n = 22/N = 3) and after 100 nM Cas (n = 9/N = 3), 300 nM Cas (n = 7/N = 3), 1 µM Cas (n = 6/N = 3) and 3 µM Nife (n = 12/N = 3) perfusion. Current densities are normalized to the maximal effect of nifedipine (a, blue traces). At peak: before vs 100 nM Cas, p = 0.0071; before vs 300 nM Cas, p < 0.0001; before vs 1 µM Cas, p < 0.0001. Statistics: one-way ANOVA test followed by Dunnet multiple comparisons test. Corresponding normalized dose-response of ICaL for peak current shown in (c). Data are presented as mean values ± SEM. n = number of cells; N = number of mice.
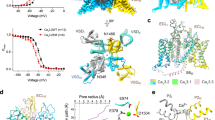
Whole cell recording of ICaL on recombinant Cav1.342a and Cav1.342 channels18 and Cav1.2 channels expressed in HEK-293T cells before and after perfusion is shown in Fig. 3. Using a one-step voltage clamp protocol (holding potential −60 mV, voltage test 0 mV) we showed that Cas exhibited an inhibitory effect on ICaL in Cav1.2 transfected cells in a dose dependent manner. 100 nM Cas inhibited the 37% of ICav1.2 (Supplementary Fig. 3a), while 300 nM and 1 µM Cas produced respectively an inhibition of 70% and 80% of ICav1.2 (Fig. 3a). Dose-effect relationship showed that Cas inhibits ICav1.2 with IC50 value of 92 ± 18 nM (Supplementary Fig. 3b). We then investigated Cas effects on recombinant Cav1.3 channels. We did not record a statistically significant reduction of recombinant ICav1.3-42a and ICav1.3-42 expressed in HEK-293T cells by Cas at all concentrations tested (up to 1 µM) (Fig. 3a). Averaged current-to-voltage (I-V) relationships recorded upon perfusion of 300 nM of Cas showed inhibition of ICav1.2 by ~60% at membrane voltages ranging from −20 mV to + 30 mV (Fig. 3b, Supplementary Fig. 4). Application of Cas significantly shifted the activation curve of ICav1.2. The V0.5 for activation was −3 ± 2 mV in control conditions and 3 ± 2 mV during Cas application, respectively (n = 8, Wilcoxon test, p = 0.0078). We observed no significant effect of Cas on both ICav1.3-42a and ICav1.3-42 at all voltages tested (Fig. 3b, Supplementary Fig. 4). These data clearly indicate that Cas is a potent inhibitor of Cav1.2 channels irrespective of the Cav1.3 channel variant. We next investigated Cas selectivity on recombinant Cav3.1 T-type, Cav2.2 N-type and Cav2.1 P/Q type calcium channels expressed in HEK-293T cells. Moreover, knowing the propensity for several calcium channel blockers to affect human ether-a-go-go-related gene (hERG)19 outward current, we also evaluated the effect of Cas on recombinant hERG current expressed in Xenopus oocytes. Cas had no effect on the aforementioned recombinant currents investigated (Supplementary Fig. 5 and Supplementary Fig. 6).
a Histograms represent the percentage of reduction of L-type Ca2+ peak current density after 300 nM and 1 µM Cas perfusion in HEK-293T cells transfected with Cav1.2 (circles, n = 14/N = 4 and n = 7/N = 4, respectively), Cav1.342a (squares, n = 13/N = 4 and n = 8/N = 4, respectively) or Cav1.342 (triangles, n = 6/N = 3 and n = 7/N = 3, respectively) channels. Peak current density was recorded starting from a holding potential of −60 mV using an activating voltage step at 0 mV. Examples of L-type Ca2+ current traces for each condition and for each clone tested are reported. Statistics: one-way ANOVA test followed by Tukey’s multiple comparisons test. b Current-to-voltage (I–V) relationship of L-type Ca2+ current recorded from holding potential of −60 mV in HEK-293T Cav1.2 (n = 11/N = 4), Cav1.342a (n = 9/N = 4) and Cav1.342 (n = 6/N = 3) transfected cells before (empty circles) and after (red filled circles) 300 nM Cas application. At peak: for Cav1.2 before vs 300 nM Cas, p = 0.0037; for Cav3.142a before vs 300 nM Cas, p = 0.8148; for Cav1.342 before vs 300 nM Cas, p = 0.5696. Statistics: paired two-sided Student t-test. Data are presented as mean values ± SEM. n = number of cells; N = number of independent transfections.
Calciseptine selectively inhibited ICav1.2 in isolated mouse SAN myocytes
We studied the effects of Cas perfusion on total ICaL in isolated SAN pacemaker cells from wild-type and mutant Cav1.3−/− mice (Fig. 4). We recorded ICaL from a holding potential of −55 mV at which ICaT is inactivated4. We thus recorded ICaL flowing through L-type Cav1.3 and Cav1.2 isoforms. In Wild-Type SAN myocytes, Cas (1 µM) reduced ICaL density at voltages ranging from −35 mV to +40 mV, which corresponded to the activation range of ICav1.28. Residual ICaL, namely Cav1.3-mediated current, was totally blocked by prototypical L-type DHP blocker nifedipine (3 µM)20 (Fig. 4a, Supplementary Fig. 7). To further characterize the effect of the toxin on ICaL, we used SAN myocytes isolated from Cav1.3−/− mice, in which the only residual ICaL is ICav1.28. Cas (1 µM) totally blocked ICaL in isolated Cav1.3−/− SAN myocytes (Fig. 4b, Supplementary Fig. 8). We then measured, in Cav1.3−/− SAN myocytes, peak ICaL evoked by a voltage clamp step protocol at 0 mV from two different holding potentials, −60 mV and −40 mV respectively, in absence and after Cas 300 nM perfusion. We did not observe any statistically significant difference in the percentage of ICaL block (68 ± 3% vs 67 ± 4% of total Cav1.2-mediated current for holding potential of −40 mV and −60 mV, respectively. Supplementary Fig. 9a) suggesting no voltage dependence of Cas block on ICav1.2. In addition, we evaluated the frequency dependence of Cas block by modifying the frequency of the voltage clamp protocol (step to 0 mV from a holding potential of −60 mV). We did not observe any statistically significant difference in the degree of inhibition by 300 nM Cas in the three conditions tested (62 ± 6% at 0.2 Hz, 63 ± 6% at 1 Hz and 58 ± 8% at 5 Hz. Supplementary Fig. 9b). Taken together, these data show that Cas strongly discriminates between ICav1.2 and ICav1.3. The toxin selectively inhibits the Cav1.2 channels isoform, without showing dependency from holding potential or frequency of stimulation, indicating that inhibtion of ICav1.2 by Cas was not voltage- or use-dependent.
a Current-to-voltage (I–V) relationship and sample traces of L-type Ca2+ current recorded in isolated Wild-Type SAN cells (n = 8/N = 2) from a holding potential of −55 mV in control condition (black filled circles), after 1 µM Cas perfusion (blue circles) and after concomitant exposure to Cas 1 µM and Nife 3 µM (empty circles). At peak: before vs 1 µM Cas, p = 0.0168; 1 µM Cas vs Nife 3 µM, p = 0.0008 Statistics: one-way ANOVA test followed by Tukey multiple comparisons test. b Same as in a but in isolated SAN myocytes form Cav1.3−/−(n = 8/N = 2). At peak: before vs 1 µM Cas, p = 0.0018; 1 µM Cas vs Nife 3 µM, p = 0.1036. Statistics: one-way ANOVA test followed by Tukey multiple comparisons test. Voltage-clamp step protocol used is shown at the bottom of the sample traces. Data are presented as mean values ± SEM. n = number of cells; N = number of mice.
Calciseptine reduces the action potential amplitude and spares automaticity in SAN pacemaker myocytes
To examine the effect of the toxin on SAN cell automaticity, we recorded spontaneous action potentials (APs) in SAN myocytes from Wild-Type mice using the perforated patch-clamp technique (Fig. 5a; Fig. 5g). Consistently, 300 nM and 1 µM Cas did not affect AP firing rate (Fig. 5b, h, Table 1), but reduced AP amplitude (Fig. 5c, i, Table 1). Concomitant perfusion of Cas 300 nM and nifedipine 3 µM (Fig. 5b, Table 1) or of Cas 1 µM and nifedipine 3 µM (Fig. 5h, Table 1) induced a significantly decrease in the beating rate in SAN myocytes with respect either to control or to sole condition of Cas perfusion. Concomitant application of Cas and nifedipine 3 µM did not reduce AP amplitude further (Fig. 5c, i, Table 1). Slopes of linear (SLDD) and exponential (SEDD) part of diastolic depolarization did not change either following perfusion of Cas at 300 nM (Fig. 5d, e, Table 1) or at 1 µM (Fig. 5j, k, Table 1). Both SLDD and SEDD showed statistically significant decrease only when nifedipine 3 µM was added to the perfusion solutions (Fig. 5d, e and Fig. 5j, k, Table 1). Furthermore, we evaluated action potential duration in SAN myocytes exposed to Cas and Cas plus nifedipine 3 µM. While 300 nM Cas did not affect AP duration, we observed a reduction in action potential duration at 30%, 50% and 70% of repolarization only after concomitant application of Cas 300 nM and nifedipine 3 µM (Fig. 5f). By contrast, 1 µM Cas had statistically significant effect on AP duration at 30% and 50% of AP repolarization. Again, concomitant perfusion of Cas 1 µM and nifedipine 3 µM reduced AP duration at 30%, 50% and 70% of repolarization (Fig. 5l). We did not observe statistically significant differences in the maximum diastolic potential, the threshold potential and in action potential upstroke velocity of action potentials recorded in myocytes under control condition and after perfusion of Cas at either 300 nM or at 1 µM (Supplementary Fig. 10).
a Representative action potential recordings in Wild-Type SAN cells in Tyrode, during Cas 300 nM and Cas 300 nM + Nife 3 µM perfusion. Dotted line indicates the 0 mV. Histograms represent the average rate (b), the amplitude (APA) (c), the slope of the linear (SLDD) (d) and of the exponential (SEDD) (e) part of the diastolic depolarization of spontaneous action potentials recorded in SAN cells in Tyrode solution (Ctrl, black filled circles, n = 10/N = 4), during 300 nM Cas perfusion (Cas, red filled circles, n = 9/N = 4) and in Cas 300 nM + Nife 3 µM solution (Cas+Nife, white circles, n = 8/N = 4). Statistics: one-way ANOVA test followed by Tukey’s multiple comparisons test. f Action potential duration at 30%, 50%, 70% and 90% of the repolarization in control condition (n = 10/N = 4), during Cas 300 nM perfusion (n = 9/N = 4) and in Cas 300 nM + Nife 3 µM (n = 8/N = 4). *Ctrl vs Cas 300 nM, #Ctrl vs Cas 300 nM + Nife 3 µM, $Cas 300 nM vs Cas 300 nM + Nife 3 µM. Statistics: one-way ANOVA test followed by Tukey’s multiple comparisons test. g. Representative action potential recordings in Wild-Type SAN cells in Tyrode, during Cas 1 µM and Cas 1 µM + Nife 3 µM perfusion. Histograms represent the average rate (h), the amplitude (APA) (i), the slope of the linear (SLDD) (j) and of the exponential (SEDD) (k) part of the diastolic depolarization of spontaneous action potentials recorded in SAN cells in Tyrode SAN cells in Tyrode solution (Ctrl, black filled circles, n = 12/N = 3), during 1 µM CaS perfusion (Cas, blue filled circles, n = 12/N = 3) and in Cas 1 µM + Nife 3 µM solution (Cas+Nife, white circles, n = 10/N = 3). Statistics: one-way ANOVA test followed by Tukey’s multiple comparisons test. (l). Action potential duration at 30%, 50%, 70% and 90% of the repolarization were calculated in n = 12/N = 3 SAN cells in control condition, in n = 12/N = 3 SAN cells during Cas 1µM perfusion and in n = 9/N = 3 following Cas 1 µM + Nife 3 µM application. *Ctrl vs Cas 1 µM, #Ctrl vs Cas 1 µM + Nife 3 µM, $Cas 1 µM vs Cas 1 µM + Nife 3 µM. Statistics: one-way ANOVA test followed by Tukey’s multiple comparisons test. Data are presented as mean values ± SEM. n = number of cells; N = number of mice.
Discussion
Our study shows that the black mamba venom toxin Cas selectively inhibits Cav1.2 channels underlying ICav1.2, without affecting ICav1.3 in the heart. Cas displays selectivity between the two cardiac of L-type Ca2+ channel subunits, enabling pharmacologic distinction between the functional roles of these L-type Ca2+ channel isoforms.
L-type Ca2+ channels are required for multiple functions in the heart, including regulation of early organogenesis, structural development, cardiac physiology and automaticity21, 22. A variety of arrhythmias including inherited QT syndrome23 have been associated with alterations in L-type channels4. Consequently, Cav1 class channels members have been, are and will be prime targets for medical therapy21, 24,25,26. Pharmacological inhibition of Cav1.2 channels accounts for most of therapeutically relevant antihypertensive and anti-ischemic effects, predominantly by reducing peripheral vascular resistance and negative inotropy. Dihydropyridines (DHPs) are among the most used Cav1 channel antagonists27 with a long history of success in the treatment of several cardiovascular pathologies28, 29. However, one potential limitation of DHPs in therapeutic perspective is their lack of selectivity for different isoforms of the Cav1 family. To date, over 100 DHPs were screened in an attempt to identify a selective antagonist able to distinguish among Cav1.2 and Cav1.330. However, no candidate molecule issued from this screen study showed selectivity for one or the other isoform. This same study indicated highly similar DHP binding site at both Cav1.2 and Cav1.3 channels, suggesting that other classes of compounds needed to be identified to achieve selectivity30. Other potent synthetic blockers with completely different structure as compared to DHPs have been identified for their action on L-type Ca2+ channels31,32,33, but to the best of our knowledge, they have not been tested for their specificity for the different isoforms of Cav1 channels. Animal toxins have played an essential role in the physiological exploration of the bioelectric mechanisms of the heart and the brain. Over the last five decades, toxins have allowed investigation and characterization of the functional roles of several classes of ion channels; e.g. tetrodotoxin for the voltage-sensitive Na+ channel34, apamin for Ca2+-sensitive K+ channels35, omega conotoxins for N-type Ca2+ channels36, psalmotoxin for ASIC channels37. Since the discovery of these leading toxins, tremendous information has accumulated on the molecular identification of L-type Ca2+ channel isoforms in the brain, neuroendocrine and cardiovascular tissues. Thus, new pharmacological tools to dissect the roles played by different Ca2+ channels that discriminate between isoforms belonging to the L-type Cav1 gene family are needed. This is of particular importance in the heart in which two L-type isoforms Cav1.2 and Cav1.3 could not be distinguished pharmacologically so far.
In this work, we investigated if Cas can discriminate between cardiac Cav1.2 and Cav1.3, and if potential selectivity could be used to study the respective physiological functions of Cav1.2 and Cav1.3 in determination of heart rate and contractility.
Our results show that Cas has selective negative inotropic effect on isolated perfused heart without affecting heart rate or inducing arrhythmia in isolated hearts. A previous study reported sinus bradycardia with unaltered contractile properties in isolated heart from Cav1.3−/− mice38 suggesting that while Cav1.2 is the only L-type Ca2+ channel isoform involved in heart contractility, Cav1.3 plays a major role in heart automaticity and conduction. In addition, the evidence that, contrary to what was observed in Cav1.3−/− mice, perfusion of Cas does not induce arhythmias, sinus bradycardia or heart block is in line with the hypothesis that Cas does not affect the ICav1.3. Consequently, these results indicate that pure negative inotropic effect of Cas is due to selective block of Cav1.2 vs Cav1.3 L-type Ca2+ channels. We provide further evidence for selective Cav1.2 inhibition by Cas in SAN myocytes isolated from wild-type and Cav1.3−/− mice. Indeed, voltage clamp recordings in Wild-Type SAN myocytes showed that Cas account for around 45% reduction of total ICaL. Considering that previous data reported that in SAN cells the ICav1.2 /ICav1.3 current density ratio is between 1:28 to 1:110, it is reasonable to postulate that the residual ICaL current recorded in SAN wild-type cells correspond to ICav1.3. This point is supported by our recordings of ICaL in isolated Cav1.3−/− SAN myocytes before and after Cas perfusion. In control conditions ICaL peak current density in Cav1.3−/− SAN cells was quantitively similar to the amount of current blocked by Cas in Wild-Type SAN myocytes, further indicating that Cas acted selectively on ICav1.2. No residual ICaL was recorded in Cav1.3−/− SAN myocytes after Cas perfusion, confirming the role of Cas as pure Cav1.2 L-type Ca2+ current blocker. Results obtained on recombinant L-type Cav1.3 currents mediated by short and long variants, T-type Cav3.1, N-type Cav2.2, P/Q-type Cav2.1 expressed in HEK-293T and on L-type Cav1.2 channels in isolated ventricular myocytes further strengthen this conclusion. Since Cav1.2 plays a major role in shaping the AP in cardiac myocytes39 we studied the impact of Cas application on the different parameters in spontaneous SAN AP. Cas affects both AP amplitude and duration, without affecting the slope of diastolic depolarization phase which is known to be a Cav1.3-dependent feature40, stressing again the efficiency and the selectivity of the toxin. Our results are consistent with previous studies on the functional role of Cav1.2 in the heart using global or conditional genetic ablation of Cav1.2 channels. Indeed, while these studies demonstrated obligatory role of this isoform in cardiac contraction41, 42 and regulation of blood pressure43, they also reported lack of effect on heart rate.
The study by Teramoto and coll44 on Cas effect on unitary Ba2+ currents in the guinea-pig portal vein cells, suggested that the action site of Cas was outside the membrane. DHPs are prototypical organic blockers of L-type calcium channels widely used in therapeutical applications. A previous study reported that Cas at a rather high concentration could inhibit binding of DHPs in brain synaptosomes suggesting that the toxin is located in the proximity of DHP binding site45.
To investigate if the binding site of Cas was overlapping with that of DHPs we used isolated ventricular myocytes from mice in which Cav1.2 channels have been rendered insensitive to DHPs by knock-in of a point mutation in the drug binding site (Cav1.2DHP−/−)46. ICav1.2 recorded in Cav1.2DHP−/− myocytes showed similar sensitivity to Cas than that those isolated from Wild-Type myocytes, suggesting that DHPs and CaS do not share the same binding site on Cav1.2 channels (Supplementary Fig. 11a). To futher explore the binding properties of Cas on Cav1.2, we also used an electrophysiological approach aimed to indicate if a toxin inhibiting a neuronal Ca2+ channel was acting as a gating modifier47. We investigated the Cas-induced block of Cav1.2 expressed in HEK-293T cells at a moderate depolarizing potential (0 mV) and at a very positive potential (+150 mV) leading to maximal current activation. Our data show that Cas has almost no effect on outward-going ICav1.2, recorded at +150 mV—likely carried by Cs+ ions—suggesting a gating modifier behavior. By contrast, using the same protocol, 3 µM Nifedipine partially inhibited the ICav1.2 elicited at +150 mV, again showing that Cas inhibits Cav1.2 channels with a different mechanism than DHPs (Supplementary Fig. 11b).
A very homologous snake venom peptide (FS2) from black mamba was reported to have a similar action in muscle relaxation and hypotensive properties than Cas48. A common short peptide between two Prolines at position 42 and 47 (PTAMWP) was predicted as the binding site for Cas and FS2 by Kini and co-workers49. These authors reported that this peptide called L-calchin acts like Cas and FS2 in reducing peak systolic pressure in isolated rat hearts and reducing calcium channel amplitude in rabbit cardiac myocytes but with lower potency (IC50 ≈ 5 µM). Similar to Cas, block by L-calchin had no effect on heart rate in ex vivo rat isolated hearts. We thus synthetized L-calchin and conducted preliminary experiments on dissociated mouse ventricular myocytes (Supplementary Fig. 12). Our results showed ≈30% reduction of ICav1.2, in line with these previous data. Taken together, our data and comparison with previous studies on this class of peptides indicate that Cas and Cas-derived peptides are a promising starting point to develop selective inhibitors of Cav1 channel subtypes.
L-type Ca2+ channels are widely expressed in the brain and, in many neuronal types, Cav1.2 and Cav1.3 are co-expressed (see ref. 50 for review)50. Both distinct and complementary functions for Cav1.2 and Cav1.3 have been proposed in the central nervous system. For example, Cav1.2 is involved in hippocampal firing51, spatial memory and LTP52, as well as in the myelinisation process53. It is very likely that Cas, with its high specificity for the Cav1.2 channel, and its high flexibility of use due to the fact that it can be stereotoxally injected in specific sites in the brain will constitute a very useful tool for future explorations of the role of Cav1.2 in the nervous system. Beside playing a major role in cardiac pacemaker activity, Cav1.3 appear to be an important player in coupling spontaneous neuronal firing with mitochondrial metabolism54. It has been proposed that Cav1.3 channels are involved in firing-dependent oxidative stress of dopaminergic neurons of substantia nigra, suggesting that these channels could constitute a potential target for Parkinson disease55. This has sparkled studies in the search for selective Cav1.3 antagonists (for review see1, 56). Recently, a molecule named compound 8 was described as selective for Cav1.357 with affinity ~24 µM. However, the selectivity of compound 8 is controversial58, 59. In particular, Huang et al. 201458 reported that selectivity of compound 8 for Cav1.3 versus Cav1.2 is modest and dependent on the nature of the associated β subunit and possibly dependent from the Cav1.3 splice variants. It will thus be interesting to study selectivity of Cas in neurons coexpressing Cav1.2 and Cav1.3.
Methods
Care and use of animals
The study is in accordance with the Guide for the Care and Use of Laboratory Animals published by the US National Institute of Health (NIH Publication No. 85-23, revised 1996) and European directives (2010/63/EU). Experimental procedures were approved by the Ethical Panel of the University of Montpellier and the French Ministry of Agriculture (protocol no: 2017010310594939). Animals were housed in the IGF animal facility with free access to food and water and were exposed to 12 h light/dark cycles in a thermostatically controlled room (21–22 °C) with 40−60% humidity.
Whole heart contractility
Hearts were isolated from adult male mice anaesthetized with a first intraperitoneal injection of a mixture comprising ketamine (100 mg/kg) and xylazine (10 mg/kg), and a second one of sodium pentobarbital (45 mg/kg; Ceva Santé Animale, France). An intraperitoneal injection of heparin (7500IU/kg; Sanofi Aventis, France) was administered in order to avoid thrombus formation. A thoracotomy was performed and beating hearts were quickly removed and excised into ice-cold modified Krebs-Henseleit buffer containing (mM): NaCl 116; KCl 5; MgSO4 1.1; NaH2P04 0.35; NaHCO3 27; CaC12 1.8 and glucose 10. Buffer was gassed with 95% O2 and 5% CO2, giving a pH of 7.4 at 37 °C. Before use, the buffer was initially passed through a 0.2 µm filter (Sarstedt, USA). The aorta was cannulated under magnification and hearts were quickly mounted and perfused on the Langendorff perfusion system (Isolated heart system, EMKA Technologies, France). The coronary circulation was perfused at a constant pressure (70 mmHg) over a 1 to 4 ml/min flow range with modified Krebs-Henseleit buffer. During the stabilization phase, the heart was continuously perfused with modified Krebs-Henseleit and the electrocardiogram (ECG) was recorded through Ag/AgCl electrodes positioned on the right atrium and near the apex. Heart temperature was of 37 °C as continuously assessed by a probe positioned on the base of the heart and recorded by using a TH-5 monitoring thermometer (Phymep, USA). LV pressure was continuously measured by a home-made balloon inserted into the LV cavity by the left atrium and connected to the EMKA amplifier. After 20 min of stabilization (baseline), 100 nM Cas was perfused into the heart for 7 min. Then, the modified Krebs-Henseleit buffer was perfused for 1 h allowing to wash the effects of the Cas toxin. During the whole ex vivo protocol, the left ventricular pressure signals were continuously digitized at 0.1 Hz and recorded using an IOX data acquisition system (EMKA Technologies, France). Data were analyzed using ecgAUTOv3.3.3.12 (EMKA technologies) and MATLAB-R2021b (The MathWorks) custom-made script
Cell culture and transfection protocols
HEK-293T (RRID:CVCL_2737) were obtained from the European Collection of Authenticated Cell Cultures (ECACC 96121229). The identity of HEK-293T has been confirmed by STR profiling and the cells have been eradicated from mycoplasma at ECACC. We routinely tested the cells for the absence of the mycoplasma contamination. Cells were cultivated at 37 °C in DMEM supplemented with GlutaMax, 10% fetal bovine serum and 1% penicillin/streptomycin (Invitrogen, Fisher Scientific, France). Transfections were performed using jet-PEI (Ozyme, France) with a DNA mix containing either the plasmids that code for Cav1.2-GFP, β2a and α2δ (0.8 µg of each) or either the plasmids that code for Cav1.3 (with and without exon 42a), or Cav2.1, or either Cav2.2 combined with β2a and α2δ (0.8 µg of each supplemented with 0.025 µg of a plasmid coding for GFP). For Cav3.1 expression β2a and α2δ subunits were omitted. Plasmids coding for β2a, α2δ and Cav1.3 were created as described previously58. Plasmid coding for Cav1.2-GFP was obtained from Dr. Catalucci60. After transfection cells were placed at 30 °C for 2–3 days and dissociated with Versene (Invitrogen, Fisher Scientific, France) and plated at a density of ~35 × 103 cells per 35 mm Petri dish for electrophysiological recordings, which were performed the following day.
Xenopus oocyte preparation, DNA injection and electrophysiology
Xenopus laevis specimen were purchased from Tefor Paris Saclay. Animal handling and experiments fully conformed to French regulations and were approved by local governmental veterinary services (authorization number E06-152-5 delivered by the Ministère de l’Agriculture, Direction des Services Vétérinaires). Animals were anesthetized by exposure for 20 min to a 0.1% solution of 3-aminobenzoic acid ethyl ester (MS-222) (Sigma) buffered at pH 7.4. Oocytes were surgically removed and dissected away in a saline solution (ND96) containing (in mM) 96 NaCl, 2 KCl, 1.8 CaCl2, 2 MgCl2, and 5 HEPES at pH 7.4 with NaOH. Stage V and VI oocytes were treated for 3 h with collagenase (1 mg/ml, type Ia, Sigma) in the presence of trypsin inhibitor (Sigma) in ND96 to discard follicular cells. pSI-HERG plasmid solutions were injected in nucleus (100 ng/µl, 23 nl/oocyte) using a pressure microinjector. The oocytes were kept at 19 °C in the ND96 saline solution supplemented with penicillin (10 mg/L) and streptomycin (20 mg/L). Oocytes were studied within 2 days following injection of plasmid. In a 0.3-ml perfusion chamber, a single oocyte was impaled with two standard glass microelectrodes (1–2.5 MΩ resistance) filled with 3 M KCl and maintained under voltage- clamp using a Dagan TEV 200 amplifier. Stimulation of the preparation, data acquisition and analysis were performed using pClamp software (Axon Instruments). All experiments were performed at controlled room temperature (19-20 °C) in ND96 solutions. A perfusion system allowed local drugs external application. HERG currents were evoked every 10 s by 2.5 s depolarizing voltage steps ranging from -80 to +80 mV in 20 mV increments and then by a repolarizing step to -40 mV for 1.5 s. BeKm1 peptide was purchased from Smartox (Saint Martin d’Hères, France).
Isolation of adult ventricular cardiomyocytes
Excised hearts from C57Bl/6 J Wild-Type and mice carrying DHP insensitive Cav1.2 channels (Cav1.2DHP−/−) mice were quickly mounted on a Langendorff apparatus. Heart was perfused with a Ca2+-free Tyrode solution for 4 min followed by an enzymatic solution containing LiberaseTM (0.2 mg/ml) and Trypsin (0.14 mg/ml) for 3.5 min. Hearts were removed from the apparatus and stored in a “Stop solution” (10 mM BDM, 5.5 mM glucose, 12.5 μM CaCl2 and 5% Fetal Calf Serum) to block enzymatic digestion. Atria were quickly removed and the ventricles were chopped into small pieces (~1 mm3) using forceps and dissociated by gentle pipetting using a flame-forged Pasteur pipette. Cell suspension was then filtered using a medical gauze and myocytes gravity settle for 20 min. To restore Ca2+ concentration to physiological level, a Ca2+ reintroduction buffer containing (mM): NaCl, 140; KCl, 5.4; MgCl2, 1; CaCl2, 1.8; Hepes,5 and glucose, 5.5 (pH adjusted to 7.4 with NaOH) was added progressively. Then cardiomyocytes were plated on dishes for patch clamp recording.
Isolation of SAN cells
Hearts from Wild-Type and Cav1.3−/− mice were removed under general anesthesia consisting of 0.01 mg/g xylazine (2% Rompun; Bayer AG) and 0.1 mg/g ketamine (Imalgène;Merial) and immersed in a pre-warmed (36 °C) Tyrode solution containing (mM): 140 NaCl, 5.4 KCl, 1 MgCl2, 1.8 CaCl2, 5.5 D-glucose, and 5 Hepes (adjusted to pH 7.4 with NaOH). SAN region was identified using the superior and inferior vena cava, the crista terminalis, and the interatrial septum as landmarks. SAN tissue was excised and transferred into a low-Ca2+ solution containing (mM): 140 NaCl, 5.4 KCl, 0.5 MgCl2, 0.2 CaCl2, 1.2 KH2PO4, 50 taurine, 5.5 D-glucose, 1 mg/mL BSA, and 5 Hepes–NaOH (adjusted to pH 6.9 with NaOH) for 5 min. Then, enzymatic digestion was carried out for 20-25 min at 36 °C in the low-Ca2+ solution containing LiberaseTH Research Grade (0.15 mg/mL; Roche, Mannheim, Germany) and elastase (0.5 mg/mL; Worthington, Lakewood, NJ, USA). Digestion was stopped by washing the SAN in a “Kraftbrühe” (KB) medium containing (mM) 100 K-glutamate, 10 K-aspartate, 25 KCl, 10 KH2PO4, 2 MgSO4, 20 taurine, 5 creatine, 0.5 EGTA, 20 D-glucose, 5 Hepes, and 1 mg/mL BSA (adjusted to pH 7.2 with KOH). Single SAN cells were then dissociated from the SAN tissue by manual agitation using a flame-forged Pasteur’s pipette. To recover the automaticity of the SAN cells, Ca2+ was gradually reintroduced in the cell’s storage solution to a final concentration of 1.8 mM. SAN cells were then left to rest for 1 h before recordings.
Electrophysiological recordings
Macroscopic currents in HEK-293T cells were recorded at room temperature using an Axopatch 200B or Multiclamp 700B patchclamp amplifier (Molecular Devices, Sunnyvale CA). Borosilicate glass pipettes had a resistance of 1.5–2.5 MΩ when filled with an internal solution containing (in mM): 140 CsCl, 10 EGTA, 10 HEPES, 3 Mg-ATP, 0.6 GTPNa, and 3 CaCl2 (pH adjusted to 7.25 with KOH, ~315 mOsm, ~100 nM free Ca2+ using the Max-Chelator software, http://maxchelator.stanford.edu/). The extracellular solution contained (in mM): 135 NaCl, 20 TEACl, 5 BaCl2, 1 MgCl2, and 10 HEPES (pH adjusted to 7.25 with KOH, ~330 mOsm).
For patch-clamp recordings of SAN myocytes, cells were harvested in custom-made chambers with glass bottoms for cell attachment. Cells were then super-fused with Tyrode’s solution warmed at 36 °C before recording. Action potentials and ionic currents were recorded using an Axon multi-clamp patch-clamp 700B amplifier. Voltage-gated L-type Ca2+ currents (ICaL) were recorded using standard whole cell patch-clamp configuration. For recording ICaL, we used an extracellular recording solution contained (mM): 135 tetraethylammonium chloride (TEA-Cl), 10 4-aminopyridine (4-AP), 1 MgCl2, 0.03 tetrodotoxin (TTX), 1 g/L Glucose, 2 CaCl2, 10 Hepes, (adjusted to pH = 7.2 with TEAOH). Recording electrodes, pulled from borosilicate glass using a DMZ-Universal Electrode Puller (Zeitz Instruments), had a resistance of 3MΩ and were filled with a solution containing (in mM): 125 CsOH, 20 TEA-Cl, 1.2 CaCl2, 5 Mg-ATP, 0.1 Li2-GTP, 5 EGTA, and 10 HEPES (pH adjusted to 7.2 with CsOH). Pacemaker activity was recorded by the perforated patch-clamp technique using escin (40 µg/ml). For recording cell automaticity glass pipettes were filled with the intracellular solution contained (mM): 80 K-Aspartate, 50 KCl, 1 MgCl2, 5 HEPES, 2 CaCl2, 5 EGTA, 3 ATP-Na+ salt; pH was adjusted to 7.2 with KOH. Escin was dissolved in sterile H2O and added to the intracellular solution right before each experiment.
We used an extracellular recording solution (Tyrode’s based) contained (mM): 140 NaCl, 5.4 KCl, 1 MgCl2, 1.8 CaCl2, 5 HEPES, 5.5 D-Glucose; pH was set to 7.4 with NaOH. AP parameters have been calculated as reported in Baudot et al.10. Data were analyzed using pCLAMP9 (Molecular Devices) and GraphPad Prism (GraphPad) software.
Toxin Calciseptine
In all experiments of cellular electrophysiology, we employed synthetized analog of Cas, commercially available at Latoxan (ID: L8109). The native peptide was purified from the venom of Dendroaspis polylepis purchased from Latoxan, as previoulsly described16. The pure peptide was obtained after gel filtration, cation exchange and C18 reversed phase chromatography. Its measured molecular mass (7036.26 Da average) was in accordance with the mass calculated from sequence data (7036.22 Da).
Statistical analysis
Statistical analysis was performed using Prism 10.0 (GraphPad Software). Data are represented as mean ± the standard error of the mean. p < 0.05 was considered statistically significant. Normality test was performed on each data set and appropriate statistical tests have been applied. Statistical tests used in each experiment are specified throughout the figure legends.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
All data that support the findings of this study are included in the manuscript. Original files of electrophysiological recordings and raw data are available upon request to the corresponding authors. A source data file is included with this manuscript. Source data are provided with this paper.
References
Zamponi, G. W., Striessnig, J., Koschak, A. & Dolphin, A. C. The physiology, pathology, and pharmacology of voltage-gated calcium channels and their future therapeutic potential. Sibl. DR Pharm. Rev. Am. Soc. Pharmacol. Exp. Therapeut. 67, 821–870 (2015).
Catterall, W. A. Voltage-gated calcium channels. Cold Spring Harb Perspect Biol. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3140680/ (2011).
Dolphin, A. C. Voltage-gated calcium channels and their auxiliary subunits: physiology and pathophysiology and pharmacology. J. Physiol. 594, 5369–5390 (2016).
Bers, D. Ca channels in cardiac myocytes: structure and function in Ca influx and intracellular Ca release. Cardiovasc. Res. 42, 339–360 (1999).
Marionneau, C. et al. Specific pattern of ionic channel gene expression associated with pacemaker activity in the mouse heart: Ion channel expression in the murine heart. J. Physiol. 562, 223–234 (2005).
Bers, D. M. Cardiac excitation–contraction coupling. Nature 415, 198–205 (2002).
Papa, A., Kushner, J. & Marx, S. O. Adrenergic regulation of calcium channels in the heart. Annu. Rev. Physiol. 84, 285–306 (2022).
Mangoni, M. E. et al. Functional role of L-type Cav1.3 Ca2+ channels in cardiac pacemaker activity. Proc. Natl Acad. Sci. USA 100, 5543–5548 (2003).
Mesirca, P. et al. G protein-gated IKACh channels as therapeutic targets for treatment of sick sinus syndrome and heart block. Proc. Natl Acad. Sci. USA 113, E932–E941 (2016).
Baudot, M. et al. Concomitant genetic ablation of L-type Cav1.3 (α1D) and T-type Cav3.1 (α1G) Ca2+ channels disrupts heart automaticity. Sci. Rep. 10, 18906 (2020).
Mangoni, M. E. & Nargeot, J. Genesis and regulation of the heart automaticity. Physiol. Rev. Am. Physiol. Soc. 88, 919–982 (2008).
Chicheportiche, R., Vincent, J.-P., Kopeyan, C., Schweitz, H. & Lazdunski, M. Structure-function relationship in the binding of snake neurotoxins to the torpedo membrane receptor? Biochemistry 14, 2081–2091 (1975).
Bourne, Y., Renault, L. & Marchot, P. Crystal structure of snake venom acetylcholinesterase in complex with inhibitory antibody fragment Fab410 bound at the peripheral site. J. Biol. Chem. 290, 1522–1535 (2015).
Diochot, S. et al. Black mamba venom peptides target acid-sensing ion channels to abolish pain. Nature 490, 552–555 (2012).
Vincent, J. P. et al. Molecular mechanism of cardiotoxin action on axonal membranes. Biochemistry 15, 3171–3175 (1976).
de Weille, J. R., Schweitz, H., Maes, P., Tartar, A. & Lazdunski, M. Calciseptine, a peptide isolated from black mamba venom, is a specific blocker of the L-type calcium channel. Proc. Natl Acad. Sci. USA 88, 2437–2440 (1991).
Bock, G. et al. Functional properties of a newly identified C-terminal splice variant of Cav1.3 L-type Ca2+ channels. J. Biol. Chem. 286, 42736–42748 (2011).
Singh, A. et al. Modulation of voltage- and Ca2+-dependent gating of CaV1.3 L-type calcium channels by alternative splicing of a C-terminal regulatory domain. J. Biol. Chem. 283, 20733–20744 (2008).
Chouabe, C., Drici, M.-D., Romey, G., Barhanin, J. & Lazdunski, M. HERG and KvLQT1/IsK, the Cardiac Kϩ channels involved in long QT syndromes, are targets for calcium channel blockers. Mol. Pharmacol. 54, 695–703 (1998).
Hockerman, G. H., Peterson, B. Z., Johnson, B. D. & Catterall, W. A. Molecular determinants of drug binding and action on l-type calcium channels. Annu. Rev. Pharm. Toxicol. 37, 361–396 (1997).
Moosmang, S., Lenhardt, P., Haider, N., Hofmann, F. & Wegener, J. W. Mouse models to study L-type calcium channel function. Pharmacol. Therapeut. 106, 347–355 (2005).
Shah, K., Seeley, S., Schulz, C., Fisher, J. & Gururaja Rao, S. Calcium channels in the heart: disease states and drugs. Cells 11, 943 (2022).
Splawski, I. et al. CaV1.2 calcium channel dysfunction causes a multisystem disorder including arrhythmia and autism. Cell 119, 19–31 (2004).
Striessnig, J. Pharmacology, structure and function of cardiac L-Type Ca2+ channels. Cell Physiol. Biochem 9, 242–269 (1999).
Eisenberg, M. J., Brox, A. & Bestawros, A. N. Calcium channel blockers: an update. Am. J. Med. 116, 35–43 (2004).
Striessnig, J., Ortner, N. & Pinggera, A. Pharmacology of L-type calcium channels: novel drugs for old targets? CMP 8, 110–122 (2015).
Triggle, D. J. 1,4-Dihydropyridines as calcium channel ligands and privileged structures. Cell. Mol. Neurobiol. 23, 293–303 (2003).
de Vries, R. J. M., van Veldhuisen, D. J. & Dunselman, P. H. J. M. Efficacy and safety of calcium channel blockers in heart failure: focus on recent trials with second-generation dihydropyridines. Am. Heart J. 139, 185–194 (2000).
Epstein, M. Calcium antagonists: still appropriate as first line antihypertensive agents. Am. J. Hypertens. 9, 110–121 (1996).
Chang, C.-C. et al. Antagonism of 4-substituted 1,4-dihydropyridine-3,5-dicarboxylates toward voltage-dependent L-type Ca2+ channels CaV1.3 and CaV1.2. Bioorg. Med. Chem. 18, 3147–3158 (2010).
Qar, J. et al. A novel high affinity class of Ca2+ channel blockers. Mol. Pharm. Am. Soc. Pharmacol. Exp. Therapeut. 33, 363–369 (1988).
Schmid, A., Romey, G., Barhanin, J. & Lazdunski, M. SR33557, an indolizinsulfone blocker of Ca2+ channels: identification of receptor sites and analysis of its mode of action. Mol. Pharm. Am. Soc. Pharmacol. Exp. Therapeut. 35, 766–773 (1989).
Triggle, D. L-type calcium channels. CPD 12, 443–457 (2006).
Narahashi, T., Moore, J. W. & Scott, W. R. Tetrodotoxin blockage of sodium conductance increase in lobster giant axons. J. Gen. Physiol. 47, 965–974 (1964).
Hugues, M., Romey, G., Duval, D., Vincent, J. P. & Lazdunski, M. Apamin as a selective blocker of the calcium-dependent potassium channel in neuroblastoma cells: voltage-clamp and biochemical characterization of the toxin receptor. Proc. Natl Acad. Sci. USA 79, 1308–1312 (1982).
McCleskey, E. W. et al. Omega-conotoxin: direct and persistent blockade of specific types of calcium channels in neurons but not muscle. Proc. Natl Acad. Sci. USA 84, 4327–4331 (1987).
Escoubas, P. et al. Isolation of a tarantula toxin specific for a class of proton-gated Na+ channels. J. Biol. Chem. 275, 25116–25121 (2000).
Matthes, J. et al. Disturbed atrio-ventricular conduction and normal contractile function in isolated hearts from Ca v 1.3-knockout mice. Naun. Schmiedeberg. Arch. Pharmacol. 369, 554–562 (2004).
Klugbauer, N., Welling, A., Specht, V., Seisenberger, C. & Hofmann, F. L-type Ca2+ channels of the embryonic mouse heart. Eur. J. Pharmacol. 447, 279–284 (2002).
Mesirca, P., Torrente, A. G. & Mangoni, M. E. Functional role of voltage gated Ca(2+) channels in heart automaticity. Front Physiol. 6, 19 (2015).
Seisenberger, C. et al. Functional embryonic cardiomyocytes after disruption of the L-type α1C (Ca 1.2) calcium channel gene in the mouse. J. Biol. Chem. 275, 39193–39199 (2000).
Rosati, B. et al. Robust L-type calcium current expression following heterozygous knockout of the Cav1.2 gene in adult mouse heart: Robust expression of L-type calcium current. J. Physiol. 589, 3275–3288 (2011).
Moosmang, S. et al. Dominant role of smooth muscle L-type calcium channel Cav1.2 for blood pressure regulation. EMBO J. John Wiley Sons Ltd. 22, 6027–6034 (2003).
Teramoto, N. et al. Effects of calciseptine on unitary barium channel currents in guinea-pig portal vein. Pflug. Arch. Eur. J. Physiol. 432, 462–470 (1996).
Yasuda, O. et al. Calciseptine binding to a 1,4-dihydropyridine recognition site of the L-type calcium channel of rat synaptosomal membranes. Biochem. Biophys. Res. Commun. 194, 587–594 (1993).
Sinnegger-Brauns, M. J. et al. Isoform-specific regulation of mood behavior and pancreatic β cell and cardiovascular function by L-type Ca2+ channels. J. Clin. Invest. 113, 1430–1439 (2004).
McDonough, S. I., Boland, L. M., Mintz, I. M. & Bean, B. P. Interactions among toxins that inhibit N-type and P-type calcium channels. J. Gen. Physiol. 119, 313–328 (2002).
Watanabe, T. X. et al. Smooth muscle relaxing and hypotensive activities of synthetic calciseptine and the homologous snake venom peptide FS2. Jpn. J. Pharmacol. 68, 305–315 (1995).
Kini, R. M. et al. Flanking proline residues identify the L-Type Ca 2+ channel binding site of calciseptine and FS2. Biochemistry 37, 9058–9063 (1998).
Striessnig, J., Pinggera, A., Kaur, G., Bock, G. & Tuluc, P. L-type Ca2+ channels in heart and brain. Wiley Interdiscip. Rev. Membr. Transp. Signal 3, 15–38 (2014).
Lacinova, L., Moosmang, S., Langwieser, N., Hofmann, F. & Kleppisch, T. Cav1.2 calcium channels modulate the spiking pattern of hippocampal pyramidal cells. Life Sci. 82, 41–49 (2008).
Moosmang, S. Role of hippocampal Cav1.2 Ca2+ channels in NMDA receptor-independent synaptic plasticity and spatial memory. J. Neurosci. 25, 9883–9892 (2005).
Santiago González, D. A. et al. Conditional deletion of the L-type calcium channel Cav1.2 in NG2-positive cells impairs remyelination in mice. J. Neurosci. 37, 10038–10051 (2017).
Zampese, E. et al. Ca2+ channels couple spiking to mitochondrial metabolism in substantia nigra dopaminergic neurons. Sci. Adv. 8, eabp8701 (2022).
Guzman, J. N. et al. Oxidant stress evoked by pacemaking in dopaminergic neurons is attenuated by DJ-1. Nature 468, 696–700 (2010).
Filippini, L., Ortner, N. J., Kaserer, T. & Striessnig, J. Cav1.3‐selective inhibitors of voltage‐gated L‐type Ca2+ channels: fact or (still) fiction? Br. J. Pharmacol. 180, 1289–1303 (2023).
Kang, S. et al. CaV1.3-selective L-type calcium channel antagonists as potential new therapeutics for Parkinson’s disease. Nat. Commun. 3, 1146 (2012).
Huang, H. et al. Modest CaV1.342-selective inhibition by compound 8 is β-subunit dependent. Nat. Commun. 5, 4481 (2014).
Ortner, N. J. et al. Pyrimidine-2,4,6-triones are a new class of voltage-gated L-type Ca2+ channel activators. Nat. Commun. 5, 3897 (2014).
Catalucci, D. et al. Akt regulates L-type Ca2+ channel activity by modulating Cavα1 protein stability. J. Cell Biol. 184, 923–933 (2009).
Acknowledgements
We thank Jörg Striessnig for sharing the Cav1.3-/- and Cav1.2DHP-/- mouse lines. This work has been supported by the Fondation Leducq (TNE FANTASY 19CV03 to M.E.M). The IGF group is a member of the Laboratory of Excellence Ion Channel Science and Therapeutics supported by a grant from ANR (ANR-11-LABX-0015). The IGF group thanks the Réseau d’Animaleries de Montpellier (RAM) of Biocampus facility for the management of mouse lines. We thank all the personnel of the PCEA mouse breeding facility and of iExplore facility in Montpellier.
Author information
Authors and Affiliations
Contributions
P.M., M.E.M. and J.N. designed the study and wrote the manuscript. P.M., J.N., J.C., C.B, E.T., L.G., A.M., S.D. and I.B. performed experiments. P.M, J.N, J.C. analyzed the results. S.D., M.L., T.W.S. and S.B.-L. contributed to study design and conceptualization. All authors contributed to data interpretation and manuscript review and editing.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests
Peer review
Peer review information
Nature Communications thanks the anonymous reviewers for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mesirca, P., Chemin, J., Barrère, C. et al. Selective blockade of Cav1.2 (α1C) versus Cav1.3 (α1D) L-type calcium channels by the black mamba toxin calciseptine. Nat Commun 15, 54 (2024). https://doi.org/10.1038/s41467-023-43502-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-023-43502-w
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.