Abstract
The ontogeny and fate of stem cells have been extensively investigated by lineage-tracing approaches. At distinct anatomical sites, bone tissue harbors multiple types of skeletal stem cells, which may independently supply osteogenic cells in a site-specific manner. Periosteal stem cells (PSCs) and growth plate resting zone stem cells (RZSCs) critically contribute to intramembranous and endochondral bone formation, respectively. However, it remains unclear whether there is functional crosstalk between these two types of skeletal stem cells. Here we show PSCs are not only required for intramembranous bone formation, but also for the growth plate maintenance and prolonged longitudinal bone growth. Mice deficient in PSCs display progressive defects in intramembranous and endochondral bone formation, the latter of which is caused by a deficiency in PSC-derived Indian hedgehog (Ihh). PSC-specific deletion of Ihh impairs the maintenance of the RZSCs, leading to a severe defect in endochondral bone formation in postnatal life. Thus, crosstalk between periosteal and growth plate stem cells is essential for post-developmental skeletal growth.
Similar content being viewed by others
Introduction
The skeleton houses at least three sources of skeletal stem cells: the resting zone of the growth plate, the bone marrow and the periosteum/perichondrium1,2,3,4,5. Each of these stem cells has specific characteristics and contributes to bone homeostasis by serving as the local source of osteogenic cells and recent studies suggest an ontogenic hierarchy among these skeletal stem cells1,2,5. Mammalian bone is formed through two distinct growth processes: endochondral and intramembranous bone formation6. In endochondral bone formation, parathyroid hormone-related protein (PTHrP)-expressing RZSCs are the source of growth plate chondrocytes, which give rise to bone-forming osteoblasts as well as bone marrow skeletal stem cells1. Growth plate chondrocytes undergo differentiation into hypertrophic chondrocytes, which express Ihh, the master regulator of endochondral bone formation that controls chondrocyte proliferation, maturation and osteoblast differentiation1,2,5,6. Although conditional deletion of Ihh by means of Col2a1-Cre leads to a severe defect in bone development7, the fact that most of the mesenchymal lineage cells in bone originate from Col2a1-expressing cells8, raises the possibility that the cellular source of Ihh may not be limited to hypertrophic chondrocytes and could include the periosteum for instance.
A recent study identified cathepsin K (Ctsk)-Cre expressing PSCs as a unique class of skeletal stem cells residing in the periosteum3. PSCs are considered to exert their effects exclusively in intramembranous bone formation, since Ctsk-Cre-mediated deletion of Sp7, an essential transcriptional factor for osteoblast differentiation, impacted intramembranous but not endochondral bone formation3. In this system however, osteoblast differentiation of PSCs is selectively inhibited by Sp7 deficiency but PSCs are still present and may still play a role in skeletal growth.
Here we show that PSCs not only regulate intramembranous bone formation but also contribute significantly to endochondral bone formation. When exploring the role of protein arginine methyltransferase 5 (PRMT5) in osteoclasts, we serendipitously developed a mouse model in which PSCs are specifically abrogated. These mice display progressive defects in intramembranous and endochondral bone formation, the latter of which is caused by a deficiency in PSC-derived Ihh. Thus, the periosteum/perichondrium and the growth plate are engaged in a specific Ihh-dependent crosstalk by which the growth plate-derived Ihh acts on the periosteum/perichondrium at early stages of development9,10,11 and, as shown here, the periosteum/perichondrium-derived Ihh maintains growth plate homeostasis and ensures the skeletal growth in postnatal stages.
Results
Ctsk-Cre-mediated deletion of Prmt5 impacts bone growth
PRMT5 is a major enzyme responsible for symmetrical demethylation of arginine on target proteins12. Previous studies showed that Prmt5 is essential for homeostasis of various types of stem cells, such as ES cells, neural stem/progenitor cells, muscle stem cells and hematopoietic stem cells, suggesting that the requirement of Prmt5 may be one of the common characteristics shared by stem cells13. To explore the role of PRMT5 in bone homeostasis, and because our initial interest was osteoclastogenesis, we crossed Prmt5flox/Δ mice12 with Ctsk-Cre mice14 in which Cre recombinase is expressed not only in osteoclasts but also in PSCs3,15,16. Prmt5flox/Δ Ctsk-Cre mice were smaller than control mice in body size and exhibited a decrease in bone mass in the femur at the age of 11 weeks (Fig. 1a, b and Supplementary Fig. 1a, b). Prmt5flox/Δ Ctsk-Cre mice displayed an abnormal growth plate architecture with a reduced chondrocyte column length, indicating impaired endochondral bone formation (Fig. 1c, d). These mice also exhibited a reduction in bone width and calvarial bone volume, suggesting that intramembranous bone formation was also affected in Prmt5flox/Δ Ctsk-Cre mice (Fig. 1b, e). The altered skeletal phenotypes became more obvious with aging (Fig. 1f–i). Thus, Prmt5flox/Δ Ctsk-Cre mice postnatally displayed a severe defect in endochondral and intramembranous bone formation. The number of hematopoietic stem and progenitor cells in the bone marrow dramatically decreased in Prmt5flox/Δ Ctsk-Cre mice in the age of 40-63 weeks (Supplementary Fig. 1c). The serum concentrations of calcium and phosphate as well as serum parameters of nutritional status were normal in Prmt5flox/Δ Ctsk-Cre mice (Supplementary Fig. 2).
a Macroscopic image and body weight of Prmt5flox/+ Ctsk-Cre and Prmt5flox/Δ Ctsk-Cre mice (n = 5 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. b Representative μCT images and parameters of the femur in Prmt5flox/+ Ctsk-Cre and Prmt5flox/Δ Ctsk-Cre mice (n = 5 mice per group). The white arrow heads indicate bone width in the control mice. Scale bars, 1 mm. P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. c Toluidine blue staining of the growth plates in the proximal tibiae of 11-week-old female Prmt5flox/+ Ctsk-Cre and Prmt5flox/Δ Ctsk-Cre mice. Representative pictures of more than three independent experiments are shown. Scale bars, 50 μm. d Chondrocyte-column length in the growth plates in the proximal tibiae of 11-week-old female Prmt5flox/+ Ctsk-Cre and Prmt5flox/Δ Ctsk-Cre mice (n = 10 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. e Representative μCT images of the skull of more than three littermates at the age of 11 weeks. Scale bars, 7 mm. f Macroscopic image and body weight of female control and Prmt5flox/Δ Ctsk-Cre (n = 8 and 3 mice per group) mice at 63 weeks of age. Prmt5flox/+, Prmt5flox/Δ, and Prmt5flox/+ Ctsk-Cre mice were phenotypically identical, and so were grouped together and used as controls in (f–i). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. g Representative μCT images of the femur of male littermates at 63 weeks of age. Representative pictures of more than three independent experiments are shown. The white arrow heads indicate bone width in the control mice. Scale bars, 1 mm. h Body weight of female littermates at 3, 5, 8 and 11 weeks of age (3 weeks: n = 21 and 13, 5 weeks: n = 16 and 9, 8 weeks: n = 10 and 7, 11 weeks: n = 5 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. i Femur length in female littermates at 4, 6, 11 and 63 weeks of age (4 weeks: n = 4, 6 weeks: n = 4 and 3, 11 weeks: n = 3, 63 weeks: n = 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. Source data are provided as a Source Data file.
Osteoclast phenotypes in Prmt5 flox/Δ Ctsk-Cre mice
Bone histomorphometric analyses and in vitro culture experiments showed that osteoclast differentiation and function were normal in Prmt5flox/Δ Ctsk-Cre mice (Supplementary Fig. 3). RNA-seq analysis revealed that Prmt5-deficiency did not affect the gene expression profile in osteoclasts (Supplementary Fig. 3h, i). The Prmt5 mRNA expression levels markedly decreased during osteoclastogenesis in bone marrow cells derived from Prmt5flox/Δ Ctsk-Cre mice, whereas the expression levels of osteoclast marker genes (Nfatc1, Acp5, Tnfrsf11a, Mmp9 and Dcstamp) did not change (Supplementary Fig. 3j). Furthermore, bone marrow transfer experiments revealed that osteoclasts were not responsible for the skeletal phenotypes in Prmt5flox/Δ Ctsk-Cre mice (Supplementary Fig. 4a–j). To further exclude the possibility of osteoclast contribution to the Prmt5-deficiency phenotype, we crossed Prmt5flox/flox mice with LysM-Cre mice17, in which Cre recombinase is expressed in myeloid cells including osteoclast precursors. Prmt5flox/flox LysM-Cre mice displayed normal body size and no decrease in bone mass, bone length or bone width (Supplementary Fig. 4k–p). In contrast to Prmt5flox/Δ Ctsk-Cre mice, Prmt5flox/flox LysM-Cre mice showed a slightly increased bone volume, suggesting that Prmt5 may be required for homeostasis of early stage osteoclast precursors (Supplementary Fig. 4n). Thus, the low bone mass phenotype in Prmt5flox/Δ Ctsk-Cre mice cannot be attributed to the Prmt5 deletion in osteoclast-lineage cells. We also crossed Prmt5flox/flox mice with Col2a1-Cre mice18 and Sp7-Cre mice19, in both of which Cre recombinase is expressed in most of mesenchymal lineage cells in bone including the periosteum8. Prmt5flox/flox Col2a1-Cre and Prmt5flox/flox Sp7-Cre mice were smaller than control mice in body size and exhibited a decrease in bone mass, bone length and bone width, recapitulating the phenotypes of Prmt5flox/Δ Ctsk-Cre mice (Supplementary Fig. 5). Collectively, these data indicated that Ctsk+ mesenchymal cells, but not osteoclasts, were responsible for the impaired bone growth in Prmt5flox/Δ Ctsk-Cre mice.
PSCs are selectively abrogated by Prmt5 deficiency
In Ctsk-Cre mice, Cre recombinase is reportedly expressed in osteogenic progenitors at the periosteum3,15,16. To detect periosteal osteogenic progenitors with EGFP, we crossed Prmt5flox/Δ Ctsk-Cre mice or Prmt5flox/+ Ctsk-Cre mice with CAG-CAT-EGFP mice (Supplementary Fig. 6). A previous report showed that Ter119–CD31−6C3−CD45−CD90−Ctsk+CD51+ periosteal osteogenic progenitors are composed of CD200+CD105− PSC and its descendants: CD200–CD105– periosteal progenitor 1 (PP1) and CD200variableCD105+ periosteal progenitor 2 (PP2)3. The expression levels of Prmt5 mRNA and protein decreased in PSCs, but not in growth plate chondrocytes in Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP mice (Supplementary Fig. 7a, b). We found that the frequency and number of PSCs, but not PP1 or PP2, markedly decreased in Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP mice (Fig. 2a, b). Intriguingly, the number of PSCs progressively decreased with aging in Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP mice, consistent with an age-dependent skeletal phenotype (Fig. 2c).
a Representative FACS plots of analyses in (b). b The frequency and number of periosteal osteogenic progenitors in 12-week-old littermates (n = 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. c PSC number in the littermates at multiple time points (n = 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. d Experimental settings for (e–h) (e) Representative pictures of more than three bone marrow chimeric mice. f Body weight of bone marrow chimeric mice (n = 4 and 6 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. g Femur length in bone marrow chimeric mice (n = 4 and 6 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. h Representative μCT images and parameters of the femur in bone marrow chimeric mice (n = 4 and 6 mice per group). The white arrow heads indicate bone width in the control mice. Scale bars, 1 mm. P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. i Representative pictures of the growth plates in control and Ctsk-Cre R26-iDTR mice at multiple time points after the bone marrow transfer and the first diphtheria toxin treatment. Representative images of more than three independent experiments are shown. Scale bars, 50 μm. j The length of chondrocyte-column presented in (i) was quantified (5 days: n = 3 and 4, 28 days: n = 6 and 4, 56 days: n = 4 and 6 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. k Experimental settings for (l–n). l Representative pictures of more than three bone marrow chimeric mice treated with diphtheria toxin (DT+) or saline (DT−). m Body weight of bone marrow chimeric mice (n = 3 mice per group). P value was calculated using one-sided Student’s t-test. n Femur length in bone marrow chimeric mice (n = 3 mice per group). P value was calculated using one-sided Student’s t-test. o Representative μCT images and parameters of the femur in bone marrow chimeric mice (n = 3 mice per group). Scale bars, 1 mm. P values were calculated using one-sided Student’s t-test. Source data are provided as a Source Data file.
Ablation of PSCs impacts on endochondral bone formation
To confirm the effect of PSC deletion on bone growth, we crossed Ctsk-Cre mice with mice containing a Cre-inducible diphtheria toxin (DT) receptor (Ctsk-Cre R26-iDTR mice), allowing for the DT-mediated depletion of Ctsk+ cells. When we transferred wild-type bone marrow cells into Ctsk-Cre R26-iDTR mice at the age of 3 weeks and then treated the mice with DT for 8 weeks, these mice displayed reduced body size, body weight, bone length, bone width and trabecular bone volume (Fig. 2d–h). In Ctsk-Cre R26-iDTR CAG-CAT-EGFP mice transferred with wild-type bone marrow cells, PSCs were efficiently deleted 5 days after DT treatment, while other cell types including osteoclasts, osteoblasts and chondrocytes were not affected at this stage (Fig. 2i, j and Supplementary Fig. 7c–f). After four weeks of the PSC deletion, the mice exhibited an impaired periosteal bone formation with a compensatory increase in endosteal bone formation (Supplementary Fig. 7g, h), which is consistent with other mouse models having impaired intramembranous bone formation such as Prmt5flox/Δ Ctsk-Cre mice (Supplementary Fig. 3c) and Sp7flox/flox Ctsk-Cre mice3. Histological analyses showed that intramembranous (Supplementary Fig. 7h) and endochondral bone formation (Fig. 2i, j) were progressively impaired after the postnatal deletion of PSCs.
In contrast, this protocol resulted in a severe high bone mass phenotype due to osteoclast deficiency without any evident change in body size, body weight or bone length in wild-type mice transferred with Ctsk-Cre R26-iDTR bone marrow cells (Fig. 2k–o). Collectively, these findings suggest that PSCs play a key role in both endochondral- and intramembranous-dependent postnatal bone growth.
Abnormal splicing of Periostin mRNA in Prmt5-deficient PSCs
In order to elucidate the role and target of Prmt5 in PSCs, we performed RNA-seq analysis on PSCs collected from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP mice or Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice. The RNA-seq data showed the gene expression pattern in Prmt5-deficient PSCs was very different from that in control PSCs (Fig. 3a, b). We found that the mRNA expression level of Postn (encoding periostin) was markedly decreased in Prmt5-deficient PSCs (Fig. 3c, d). We focused on periostin because periostin is known to be required for the self-renewal of osteogenic progenitors in the periosteum20,21. Previous studies have indicated that the primary role of Prmt5 is to regulate pre-mRNA splicing by mediating symmetrical demethylation of arginine residues in Sm proteins12,13. The mis-splicing of pre-mRNA due to Prmt5 deficiency can cause downregulation of mRNA expression by the nonsense-mediated mRNA decay mechanism12,13. RNA-seq analysis indicated that an abnormal splicing of Postn mRNA occurred in Prmt5-deficient PSCs (Fig. 3e). Immunohistochemistry confirmed the decreased POSTN protein levels in the periosteum in Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP mice (Fig. 3f and Supplementary Fig. 7i). The localization of EGFP+ POSTN+ cells adjacent to the growth plate is consistent with a previous report which identified PSCs3.
a Principal coordinate analysis (PCoA) performed on PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice (n = 3 mice per group). b MA plot of significant genes that were differentially expressed in the PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice (light blue dots). c Heatmap of the top 25 genes of which expression was highly altered in PSCs by the Prmt5-deficiency. The color bar indicates scaled normalized gene expression counts. d The expression level of Postn mRNA in PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice (n = 3 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. e The ratio of intron reads to total gene reads in Postn gene in PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice (n = 3 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. f Immunohistochemical analysis of the femur of Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice. Representative images of more than three independent experiments are shown. Scale bars, 100 μm. g Colony formation of PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice in the presence or absence of recombinant periostin (POSTN). Representative data of more than three independent experiments (left) and colony forming efficiency (right) are shown (n = 9 biologically independent samples). P values were calculated using ANOVA with Tukey’s multiple-comparison test. Data are presented as the mean ± S.D. h μCT images of the bone formed by PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP. Representative images of more than three independent experiments (left) and quantification of bone mineral content (right) are shown (n = 7 and n = 5 mice per group). Scale bars, 5 mm. P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. i Representative images from more than three independent Von Kossa staining (black) for mineralized bone formed by PSCs derived from Prmt5flox/Δ Ctsk-Cre CAG-CAT-EGFP and Prmt5flox/+ Ctsk-Cre CAG-CAT-EGFP mice. Scale bars, 200 μm. Black arrow heads indicate mineralized bone. Source data are provided as a Source Data file.
Similar to the finding in Postn-deficient periosteal osteogenic progenitors21, the colony forming ability was impaired in Prmt5-deficient PSCs (Fig. 3g). Treatment with exogenous periostin partially rescued the impaired self-renewal ability in Prmt5-deficient PSCs (Fig. 3g). In vivo transplantation experiments showed that PSCs derived from control mice exclusively formed intramembranous bones (Fig. 3h, i), as reported in a previous study3. In contrast, Prmt5-deficient PSCs formed minimal intramembranous bones but not cartilage or adipose tissue (Fig. 3h, i). These data suggested that the Prmt5/periostin axis is important for self-renewal of PSCs, but further studies are needed to clarify the role of Prmt5 in the later differentiation and lineage commitment stages in PSC-mediated bone formation. The mRNA expression levels of marker genes for periosteal osteogenic progenitors3,22,23,24 and skeletal stem cells5 did not change in Prmt5-deficient PSCs, suggesting that Prmt5 is important for the self-renewal but not for stem cell identity in PSCs (Supplementary Fig. 7j). These data suggest that abnormal post transcriptional regulation of Postn may cause, at least in part, a progressive reduction in the PSC number in Prmt5flox/Δ Ctsk-Cre mice. This hypothesis is consistent with a previous study showing that periostin-deficient mice exhibited postnatal defects in endochondral and intramembranous bone formation25.
PSCs orchestrate both types of bone growth via Ihh secretion
How do PSCs, located in the periosteum/perichondrium, control endochondral bone formation at the growth plate? A previous study concluded that PSCs’ role is exclusively limited to intramembranous bone formation under physiological conditions for the following reasons. First, Ctsk-Cre labels periosteal osteogenic cells, but not growth plate chondrocytes or marrow osteoblasts in a fate-mapping system, indicating that PSCs do not act as a source for the osteogenic cells that mediate endochondral bone formation3. Second, PSCs form bone via an intramembranous pathway in a transplantation system3. And third, Ctsk-Cre-mediated deletion of Sp7 results in bone loss in intramembranous bones such as the calvarium and cortical bone, but does not affect growth plate architecture or trabecular bone3. Because this is in contrast with our phenotype, where the growth plate is markedly altered during postnatal growth in PSC-deficient mice, we tested the hypothesis that PSCs could contribute indirectly to endochondral bone formation by locally producing soluble factors.
We therefore screened for genes that are highly and specifically expressed in PSCs by analyzing a deposited RNA-seq dataset (GSE106237)3. We focused on soluble factors having much higher expression in PSCs than PP2 and PP1. Ihh was among the genes highly specific to PSCs and is known to be involved in the regulation of endochondral bone formation (Fig. 4a). The major producer of Ihh has been thought to be hypertrophic chondrocytes based on the in situ hybridization experiments using fetal bones, but the contribution of Ihh produced by other cells has never been reportedly explored6,7,9,10,11,26,27. More relevant to our observations is the fact that among the periosteal osteogenic progenitors (PP1, PP2 and PSC) and CTSK– bone marrow mesenchymal stem cells, Ihh is exclusively expressed in PSCs (Fig. 4b).
a Scatter plot of the gene expression ratio. b Ihh expression in periosteal osteogenic progenitors and CTSK– bone marrow mesenchymal stem cells (n = 4 biologically independent samples). P values were calculated using ANOVA with Tukey’s multiple-comparison test. Data are presented as the mean ± S.D. c Ihh expression in various periosteal cell types (n = 5 and 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. d Images of littermates. Ihhflox/+, Ihhflox/flox, Ihhflox/+ Ctsk-Cre mice were phenotypically identical, being grouped together and used as controls in (d–h). e Body weight of littermates (n = 11 and 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. f Representative femur images of more than three littermates. Scale bars, 2 mm. g Representative femur images analyzed in h. Scale bars, 1 mm. The white arrow heads indicate bone width in the control mice. h μCT analysis parameters of the femur in littermates (n = 11 and 3 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. i Representative skull images of more than three female littermates. Scale bars, 7 mm. j Representative haematoxylin and eosin staining pictures of the tibiae growth plate in more than three littermates. Scale bars, 100 μm. R: resting zone, P: proliferating zone, H: hypertrophic zone. k Frequency of RZSCs in 3-week-old littermates (n = 4 mice per group). P = 0.0051. P value was calculated using one-sided Student’s t-test. l RZSC number in 3-week-old littermates (n = 4 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. m Mean Fluorescence Intensity of CD73 in RZSCs (n = 4 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. n Ki67+ cell frequency in RZSCs in littermates (n = 4 mice per group). P value was calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. o The expression levels of Ptch and Gli1 in RZSCs (n = 4 mice per group). P values were calculated using one-sided Student’s t-test. Data are presented as the mean ± S.D. Source data are provided as a Source Data file.
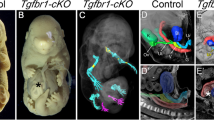
We therefore crossed Ihhflox/flox mice7 with Ctsk-Cre mice to investigate the physiological relevance of Ihh produced by PSCs. In Ihhflox/flox Ctsk-Cre CAG-CAT-EGFP mice, the expression levels of Ihh decreased specifically in PSCs, but not in the growth plate chondrocytes, periosteal CD90+ mature osteogenic cells or periosteal CD45+ hematopoietic cells (Fig. 4c and Supplementary Fig. 8a, b). Since Ihh is known to be expressed in hypertrophic chondrocytes, we rigorously excluded the possibility that Ctsk-Cre leaked in hypertrophic chondrocytes by using RANKL-floxed mice28. RANKL (encoded by Tnfsf11 gene), the master regulator of osteoclastogenesis, is essentially produced by hypertrophic chondrocytes, osteoblasts and osteocytes28,29. The deletion of RANKL in hypertrophic chondrocytes by Col10a1-Cre30 resulted in severe osteopetrosis due to a reduction of osteoclast number in the bone marrow (Supplementary Fig. 8c–e, g). In contrast, Tnfsf11flox/flox Ctsk-Cre mice did not exhibit osteopetrosis and a decrease in osteoclast number in these mice was observed only at the periosteal surface but not in the bone marrow (Supplementary Fig. 8f). If Ctsk-Cre deleted RANKL in hypertrophic chondrocytes, marrow osteoblasts or osteocytes, Tnfsf11flox/flox Ctsk-Cre mice would have exhibited severe osteopetrosis. These data clearly indicated that Ctsk-Cre does not leak in hypertrophic chondrocytes, marrow osteoblasts or osteocytes.
Notably, Ihhflox/flox Ctsk-Cre mice displayed a severe reduction in body size, body weight and bone length, indicating that endochondral bone formation was impaired (Fig. 4d–h). This phenotype became more readily apparent with aging (Fig. 4e, f), and Ihhflox/flox Ctsk-Cre mice showed a complete loss of trabecular bone and the growth plate at the age of 11 weeks (Fig. 4g, h). Ihhflox/flox Ctsk-Cre mice exhibited a marked reduction in bone width and calvarial bone volume (Fig. 4g, i), indicating that PSC-derived Ihh is also required for intramembranous bone formation. Bone marrow transfer experiments confirmed that Ctsk+ mesenchymal cells, but not hematopoietic cells, were responsible for the skeletal phenotype in Ihhflox/flox Ctsk-Cre mice (Supplementary Fig. 9a–d). Ihhflox/flox LysM-Cre mice displayed normal bone growth, indicating that the deletion of Ihh in osteoclast-lineage cells does not contribute to the skeletal phenotype in Ihhflox/flox Ctsk-Cre mice (Supplementary Fig. 9e–j).
PSC-derived Ihh is required for RZSC maintenance
At 3 weeks of age, Ihhflox/flox Ctsk-Cre mice retained normal growth plate architecture (Fig. 4j). Since Ihh is known to be a key regulator of RZSCs in the growth plate, we analyzed the CD73+ CD49e+ RZSCs2 in Ihhflox/flox Ctsk-Cre mice. Flow cytometry showed that the frequency and number of CD73+ CD49e+ RZSCs markedly decreased in the growth plate of Ihhflox/flox Ctsk-Cre mice (Fig. 4k, l). The expression levels of stem cell marker CD73 in RZSCs was unchanged (Fig. 4m), whereas the frequency of Ki67+ cells in RZSCs significantly decreased in Ihhflox/flox Ctsk-Cre mice (Fig. 4n). These data are consistent with a previous report showing that Ihh is critical for the self-renewal of RZSCs but not for their identity2. Given that 3-week-old Ihhflox/flox Ctsk-Cre mice did not display obvious bone abnormalities other than the reduction of RZSCs, it is likely that RZSCs are the direct target of PSC-derived Ihh. Indeed, the expression levels of Ihh target genes, Ptch and Gli1, were significantly decreased in RZSCs collected from Ihhflox/flox Ctsk-Cre mice (Fig. 4o).
To clarify the relative contribution between Ihh derived from PSCs and from hypertrophic chondrocytes, we crossed Ihhflox/flox mice with Col10a1-Cre mice. Ihhflox/flox Col10a1-Cre mice had already exhibited severe bone deformities with an abnormal growth plate architecture at 3 weeks of age (Supplementary Fig. 10a–c). These data indicate that hypertrophic chondrocyte-derived Ihh is essential and sufficient for bone development at the early stages of life, whereas the importance of PSC-derived Ihh increases over time in postnatal life. Since Ihhflox/flox Ctsk-Cre mice displayed a defect in intramembranous bone formation (Fig. 4g, i), we analyzed the PSC phenotypes in these animals and found that the frequency and number of PSC decreased in Ihhflox/flox Ctsk-Cre CAG-CAT-EGFP mice (Supplementary Fig. 10d, e). These data suggested that PSC-derived Ihh may also be important for the maintenance of PSC itself, but further studies are required to understand the role of PSC-derived Ihh in the periosteum homeostasis.
Collectively, these findings demonstrate that as Ihh production by growth plate chondrocytes decreases during the progressive decline in growth with age, Ihh production by periosteal PSCs maintains RZSC proliferation in the growth plate, thereby playing a key role in the prolonged postnatal bone growth.
Discussion
This study shows that although PSCs are specialized into creating osteogenic progenitors for the intramembranous pathway that occurs on the periosteal surface, they are also essential for the prolonged endochondral bone formation that occurs in the growth plate via their ability to locally produce Ihh. It is well established that Ihh plays an essential role in endochondral bone formation at the growth plate by regulating the fate of RZSCs1,2. During development, growth plate-derived Ihh acts on cells in the periosteum/perichondrium, leading to the activation of PTHrP expression in the periarticular chondrocytes through a poorly understood mechanism10,11. PTHrP then maintains chondrocytes in a proliferative, less differentiated state and inhibits the production of Ihh from the growth plate. This Ihh/PTHrP loop coordinates the synchronized chondrocyte differentiation in the growth plate during early life stages6.
Here, we show a reverse crosstalk that occurs later, at a time when the growth plate decreases its proliferative activity and growth speed in postnatal life. PSC-derived Ihh controls growth plate RZSCs to ensure prolonged skeletal growth in postnatal life. This study therefore highlights the critical importance of a functional interaction between PSCs and RZSCs in post-developmental skeletal growth. This view is supported by the fact that Ihhflox/flox Ctsk-Cre mice displayed a severe defect in bone growth at the adult stage, but the phenotype was not apparent before 3 weeks of age (Fig. 4 and Supplementary Fig. 10). Given that the width of the hypertrophic zone starts to regress around 3 weeks of age31, we interpret this data to show that hypertrophic chondrocyte-derived Ihh is sufficient to ensure rapid bone growth during development and early postnatal life, whereas PSC-derived Ihh compensates for the progressive decrease in hedgehog signaling in RZSCs during postnatal life, ensuring continued bone growth.
We analyzed PSCs using the same Ctsk-Cre line and cell surface markers with a previous report which first identified and characterized PSCs3. Using the RNAseq dataset (GSE106237) produced by the study3, we identified the exclusive Ihh expression in PSCs among periosteal osteogenic cells (Fig. 4a, b). Thus, the PSC analyzed here is exactly the same population with the previous study3. Given that the PSCs are localized to adjacent to the growth plate3,15 (Fig. 3f), we suspect that PSC-derived Ihh may control RZSCs in a paracrine manner. A previous study showed that diffusion of Shh from the secondary ossification center (SOC) also contributes to the growth plate homeostasis2. Thus, vertical (from the SOC and hypertrophic zone) and horizontal (from the periosteum/perichondrium) regulation of hedgehog signaling in the growth plate may be required for the precise coordination of skeletal growth.
Intramembranous and endochondral bone formation have been considered to be independent processes. However, our data reveals that intramembranous and endochondral pathways cooperatively ensure proper development and maintenance of bone growth for a sufficient period of time to allow long bones to reach their adult size and shape. During fracture repair, PSCs were shown to undergo endochondral bone formation in response to bone injury due to an unknown mechanism3. We suspect that PSC-derived Ihh may also play a role in the context of fracture healing. Further studies are required to clarify the relevance and function of PSC-derived Ihh in fracture repair. Given that early vertebrates first acquired intramembranous pathway to form exoskeleton (dermal bone)32,33, we suspect that PSCs may have developed earlier than other types of skeletal stem cells, subsequently acquiring the capacity to regulate endochondral bone formation.
Collaborations between distinct types of stem cells have been previously documented in studies of Drosophila gonads34,35 and mammalian skin36. This study shows the importance of stem cell communication in bone growth and homeostasis, suggesting that the interactions that occur between and among stem cells may be a fundamental principle in the development and maintenance of mammalian organs in general. Investigation into the molecular mechanisms of the functional crosstalk between stem cells will be a key to ultimately understanding the physiology and pathology of complicated biological systems.
Methods
Mice and bone analysis
All animals were maintained under specific pathogen-free conditions, and all experiments were performed with the approval of the Institutional Review Board at The University of Tokyo. C57BL/6 mice were purchased from CLEA Japan. KSN/Slc Nude mice (6-8 week-old male) were purchased from SLC Japan. R26-iDTR mice, Ihhflox/flox mice and B6.SJL (CD45.1+) mice were obtained from the Jackson Laboratory. Prmt5flox/flox mice12, Ctsk-Cre mice14, CAG-CAT-EGFP mice37, Col2a1-Cre mice18, Sp7-Cre mice19, LysM-Cre mice17, Col10a1-Cre mice30 and Tnfsf11flox/flox mice28 were described previously. Three-dimensional microcomputed tomography analyses and bone morphometric analyses were performed as described38. Age and sex-matched littermates were used for all of the experiments unless otherwise noted. The sex and age of mice used are described in figures or figure legends. All animals were maintained at a constant ambient temperature of 22–26 degree Celsius, 40–65% of humidity under a 12 h light/dark cycle with free access to food and drink.
Cell isolation
For the isolation of periosteal cells, long bones without muscles were subjected to enzymatic digestion for 1 h with serum-free α-MEM medium containing Collagenase (1 mg/ml; Wako, cat. 032-22364), Dispase II (2 mg/ml; Roche, cat. 383-02281) and DNase I (1 mg/ml; SIGMA, cat. DN25-1G) at 37 °C with agitation. After the removal of the long bones without periosteum, the tubes were centrifuged to harvest periosteal cells as pellet cells. α-MEM medium containing 20% serum was added to the tube and the periosteal cells were resuspended thoroughly by pipetting and then filtered through 100-μm nylon mesh. Tubes were centrifuged and the resulting cell pellet was subjected to FACS using the gating strategy shown in Supplementary Fig. 6. For the isolation of growth-plate chondrocytes, a scalpel was used to cut between the hypertrophic zone and the primary spongiosa of the long bones. Then, the blunt side of the scalpel was used to carefully scrape out the cartilage until the blade reached the hard surface of the secondary ossification center. The pieces of cartilage were collected and treated with 0.15% collagenase II in serum-free α-MEM medium for 120 min at 37 °C with agitation. The collected growth plate cells were subjected to FACS and western blotting analyses. The absolute number of PSCs and RZSCs per two legs was measured by using FACSAria III (BD Biosciences). We observed higher numbers/percentages of PSCs than that in the previous report3. This may reflect that we performed a whole-bone periosteal digest whereas the previous study largely minced entire bones from younger mice3. We set the CD200 and CD105 gates based on the FACS plot of negative controls (non-staining periosteal cell) (Supplementary Fig. 10d).
RNA-seq analysis and quantitative RT-PCR analysis
Bulk-RNA sequencing and real-time quantitative PCR with reverse transcription (RT-PCR) analyses were performed as described12. In brief, total RNA was extracted using the Maxwell 16 LEV simply RNA Tissue Kit (Promega) according to the manufacturer’s instructions. cDNA was synthesized using Superscript III reverse transcriptase and a SMART-seq v4 Ultra Low Input RNA Kit for Sequencing (Clontech Laboratories) for RNA-seq and RT-PCR, respectively. In the RNA-seq analysis, cDNA and sequencing libraries were processed with FastQC (v0.1.1.8), TrimGalore (v0.6.4) and Kallisto (v0.46.0) using the mouse transcriptome index (mus musculus GRCm38.96), and analyzed by DESeq2 (v1.26) to quantify gene expression on the basis of PCA, hierarchical clustering and differential expression analysis (using log fold change shrinkage and an adjusted p value <0.05). For the analysis on bulk-RNA seq data of periosteal progenitors (GSE106235), scatter plot of the gene expression ratio between PSC/PP1 and PSC/PP2 was produced. The soluble factors highly and specifically expressed in PSCs (RPKM > 500 in PSCs, PSC/PP1 ratio >5, PSC/PP2 ratio >5 and RPKM > 0 in PSC, PP1 and PP2) are highlighted in the Fig. 4a. RT-PCR analysis was performed with a LightCycler (Roche) using SYBR Green (Toyobo) and the level of mRNA expression was normalized to Gapdh. All of the primer sequences are available upon request.
Flow cytometry and antibodies
The monoclonal antibodies used were purchased from BioLegend and eBioscience. For periosteal osteogenic progenitor analysis, cells were stained with PE anti-mouse CD51 (RMV-7), APC anti-mouse CD200 (OX-90), PB anti-mouse CD90.2 (53-2.1), PerCP-Cy5.5 anti-mouse CD105 (MJ7/18), APCcy7 anti-mouse CD45 (30-F11), biotinylated anti-mouse Ter119 (TER-119), biotinylated anti-mouse CD31 (390), biotinylated anti-mouse Ly-51 (6C3), and PEcy7 streptavidin (B278254). For analysis on resting zone stem cells, FITC anti-mouse CD73 (TY/11.8), PE anti-mouse CD49e (MFR5) and APC anti-mouse Ki67 (16A8) antibodies were used. The Foxp3 Staining Buffer Set (eBioscience) was used for intracellular Ki67 staining. For haematopoietic stem and progenitor cell analysis, cells were stained with PE anti-mouse Flk2 (A2F10), APC anti-mouse Sca-1 (D7), eFluor 450 anti-mouse CD34 (RAM34), PerCP-Cy5.5 anti-mouse CD150 (mShad150), PE-Cy7 anti-mouse CD48 (HM48-1), APCcy7 anti-mouse CD117/c-kit (2B8), FITC streptavidin (eBioscience), PE anti-mouse CD16/32 (93), PE anti-mouse Ter119 (TER-119), FITC anti-mouse CD71 (RI7217) and biotinylated anti-mouse CD3ε (145-2C11), CD4 (RM4-5), CD8a (53-6.7), CD11b (M1/70), CD11c (HL3), CD45R/B220 (RA3-6B2), TER119 (TER-119), Gr-1 (RB6-8C5), and CD49b (DX5). LT-HSCs, GMPs, CMPs, MEPs and Pro-E were defined as Lin–Sca1+c-Kit+CD150+CD34−CD48−Flk2− cells, Lin−Sca1+c-Kit+CD34+CD16/32hi cells, Lin–Sca1+c-Kit+CD34+CD16/32mid cells, Lin–Sca1+c-Kit+CD34−CD16/32− cells and c-Kit+CD71+Ter119lo cells, respectively39,40. FITC anti-mouse CD45.1 (A20) and PE anti-mouse CD45.2 (104) antibodies were used to examine bone marrow chimerism. Flow cytometric analysis and sorting were performed using FACSCanto II and FACSAria III (BD Biosciences). PerCP-Cy5.5 anti-mouse CD105 antibody was used at 1:50 dilution and other antibodies were used at 1:100 dilution. FlowJo V9.9.3 software (TreeStar) was used to analyze the FACS data.
Immunohistochemistry
Femurs and tibiae were fixed overnight at 4 °C in 4% paraformaldehyde for cryosection. Samples were washed twice in PBS and then embedded in OCT compound (Sakura Finetek). The frozen tissue blocks were cut into 20-μm-thick sections using a Cryostat (Leica). The sections were stained with anti-mouse periostin (Abcam, ab14041, 1:100 dilution), anti-GFP (invitrogen, A10262, 1:100 dilution) and DAPI (Molecular Probes). Multicolor images were obtained with a Nikon C2 confocal microscope (Nikon).
Western blot analysis
The PSCs and growth plate chondrocytes were lysed with RIPA buffer (nacalai tesque) containing protease inhibitor cocktail (Millipore Sigma). The lysate was mixed with Trident 4X Laemmli SDS Sample Buffer containing 8% 2-mercaptoethanol, then boiled at 95 °C for 5 mins. The proteins were subjected to SDS-PAGE (5-20% gradient gel, FUJIFILM) and transferred onto a PVDF membrane (Millipore). The antibodies used were as follows: anti-β-actin (A5441, 1:1000 dilution), Sigma-Aldrich; anti-PRMT5 (PRMT5-21, 1:200 dilution), Santa Cruz; anti-IHH (ab52919, 1:200 dilution), Abcam.
In situ hybridization
The in situ hybridization experiments were outsourced to Genostaff Co. Ltd. In brief, bone tissues were fixed with G-Fix (Genostaff), de-calcified with G-Chelate Mild (Genostaff), embedded in paraffin on a CT-Pro20 (Genostaff) using G-Nox (Genostaff) as a less toxic organic solvent for xylene, and sectioned at 5–8 μm. In situ hybridization was performed with the ISH Reagent Kit (Genostaff) according to the manufacturer’s instructions. Tissue sections were de-paraffined with G-Nox, and rehydrated through an ethanol series and phosphate-buffered saline (PBS). The sections were fixed with 10% NBF (10% formalin in PBS) for 30 min at 37 °C and washed in distilled water, placed in 0.2 N HCl for 10 min at 37 °C and washed in PBS, treated with 4 μg ml−1 ProteinaseK (Wako Pure Chemical Industries) in PBS for 10 min at 37 °C and washed in PBS, then placed within a coplin jar containing 1xG-Wash (Genostaff), equal to 1xSSC. Hybridization was performed with probes at concentrations of 250 ng ml−1 in G-Hybo-L (Genostaff) for 16 h at 60 °C. After hybridization, the sections were washed in 1xG-Wash for 10 min at 60 °C, 50% formamide in 1xG-Wash for 10 min at 60 °C. Then the sections were washed twice in 1xG-Wash for 10 min at 60 °C, twice in 0.1xG-Wash for 10 min at 60 °C and twice in TBST (0.1% Tween 20 in tris-buffered saline (TBS)) at room temperature (RT). After treatment with 1xG-Block (Genostaff) for 15 min at RT, the sections were incubated with anti-DIG AP conjugate (Roche Diagnostics) diluted 1:2000 with x50G-Block (Genostaff) in TBST for 1 h at RT. The sections were washed twice in TBST and then incubated in 100 mM NaCl, 50 mM MgCl2, 0.1% Tween 20, 100 mM Tris-HCl, pH 9.5. Coloring reactions were performed with NBT/BCIP solution (Sigma-Aldrich) overnight and then the samples were washed in PBS. The sections were counterstained with Kernechtrot stain solution (Muto Pure Chemicals), and mounted with G-Mount (Genostaff). The probes for Ihh was developed by Genostaff.
Bone marrow transfer
Single-cell suspensions were obtained from the bone marrow of donor mice. Recipient mice were sub-lethally irradiated and administered an injection of bone marrow cells (2 × 106 cells). Mice were provided antibiotic-containing water for two weeks and analyzed eight weeks later. Since the irradiation affects bone turnover and decreases baseline bone volume, control mice were also sub-lethally irradiated and subjected to the same experimental procedure in all bone marrow transfer experiments. Bone marrow chimerism was analyzed by FACS using B6.SJL (CD45.1+) mice and antibodies, FITC anti-mouse CD45.1 (A20) and PE anti-mouse CD45.2 (104). The bone marrow transfer system used in this study efficiently replaced bone marrow haematopoietic cells (>95% engraftment).
Kidney capsule transplantation
Six to eight-week-old male KSN/Slc Nude mice were anaesthetized. The kidney was externalized through a 1-cm incision and a 2-mm pocket was made in the renal capsule. A 5-µl Matrigel plug (Corning, 356231) containing 10,000 cells was implanted underneath the capsule and kidney was replaced back into the body cavity. Animals were euthanized after six weeks. After death, kidneys were fixed overnight with 4% PFA and bone formation was detected by μCT. Samples were subjected to infiltration, embedding and sectioning. Von Kossa staining was performed to detect the mineralized bones.
Cell culture
For in vitro osteoclastogenesis, primary bone marrow cells were cultured with M-CSF (R&D Systems) for two days. These cells were further cultured for three or five days with RANKL (Wako) in the presence of M-CSF, as previously reported41. The culture medium was changed every second day in all of the experiments. Osteoclastogenesis was evaluated by counting TRAP-positive multinucleated (more than three nuclei) cells and the bone resorbing activity was confirmed by analyzing the resorption area after staining the bone slices with 0.5% toluidine blue. For the colony-forming efficiency assay, primary PSCs were sorted and plated on 12-well pates at a concentration of 500 cells/well in culture medium (DMEM with 10% FBS) in the presence or absence of 200 ng/ml recombinant mouse periostin (2955-F2-050, R&D) for 14 days. Cells were cultured on the FALCON® tissue culture plate (tissue culture treated by vacuum gas plasma) at a constant ambient temperature of 37 degree Celsius and 5.0% CO2. We used α−MEM (Gibco, Thermo Fisher Scientific, Waltham, MA, USA) and DMEM (1.0 g/l Glucose with L-Gln and Sodium Pyruvate liquid, Nacalai Tesque) for culture of osteoclasts and PSCs, respectively.
Statistical analyses
Data were analyzed on GraphPad Prism software version 6.0 g. Statistical tests, n values, replicate experiments, and P values are all located in the figures and/or legends. All data are presented as the mean ± S.D. P values were calculated using Student’s t-test and analysis of variance (ANOVA) with Dunnett’s or Tukey’s multiple-comparison test.
Reporting summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
The data that support the plots within this paper and other findings of this study are available from the corresponding author upon reasonable request. The RNAseq data produced in this study were deposited to the public data base GSE146872. We also used the bulk-RNA seq data for periosteal progenitors GSE106235 and the mouse transcriptome index mus musculus GRCm38.96 [https://www.ncbi.nlm.nih.gov/assembly/GCF_000001635.20/]. Source data are provided with this paper.
References
Mizuhashi, K. et al. Resting zone of the growth plate houses a unique class of skeletal stem cells. Nature 563, 254–258 (2018).
Newton, P. T. et al. A radical switch in clonality reveals a stem cell niche in the epiphyseal growth plate. Nature 567, 234–238 (2019).
Debnath, S. et al. Discovery of a periosteal stem cell mediating intramembranous bone formation. Nature 562, 133–139 (2018).
Tsukasaki, M. & Takayanagi, H. Osteoimmunology: evolving concepts in bone-immune interactions in health and disease. Nat. Rev. Immunol. 19, 626–642 (2019).
Ono, N., Balani, D. H. & Kronenberg, H. M. Stem and progenitor cells in skeletal development. Curr. Top. Dev. Biol. 133, 1–24 (2019).
Kronenberg, H. M. Developmental regulation of the growth plate. Nature 423, 332–336 (2003).
Razzaque, M. S., Soegiarto, D. W., Chang, D., Long, F. & Lanske, B. Conditional deletion of Indian hedgehog from collagen type 2alpha1-expressing cells results in abnormal endochondral bone formation. J. Pathol. 207, 453–461 (2005).
Ono, N., Ono, W., Nagasawa, T. & Kronenberg, H. M. A subset of chondrogenic cells provides early mesenchymal progenitors in growing bones. Nat. Cell Biol. 16, 1157–1167 (2014).
Chung, U. I., Schipani, E., McMahon, A. P. & Kronenberg, H. M. Indian hedgehog couples chondrogenesis to osteogenesis in endochondral bone development. J. Clin. Invest 107, 295–304 (2001).
Lanske, B. et al. PTH/PTHrP receptor in early development and Indian hedgehog-regulated bone growth. Science 273, 663–666 (1996).
Vortkamp, A. et al. Regulation of rate of cartilage differentiation by Indian hedgehog and PTH-related protein. Science 273, 613–622 (1996).
Inoue, M. et al. Arginine methylation controls the strength of γc-family cytokine signaling in T cell maintenance. Nat. Immunol. 19, 1265–1276 (2018).
Lorton, B. M. & Shechter, D. Cellular consequences of arginine methylation. Cell Mol. Life Sci. 76, 2933–2956 (2019).
Nakamura, T. et al. Estrogen prevents bone loss via estrogen receptor alpha and induction of Fas ligand in osteoclasts. Cell 130, 811–823 (2007).
Yang, W. et al. Ptpn11 deletion in a novel progenitor causes metachondromatosis by inducing hedgehog signalling. Nature 499, 491–495 (2013).
Han, Y. et al. Lkb1 deletion in periosteal mesenchymal progenitors induces osteogenic tumors through mTORC1 activation. J. Clin. Invest 129, 1895–1909 (2019).
Clausen, B. E., Burkhardt, C., Reith, W., Renkawitz, R. & Förster, I. Conditional gene targeting in macrophages and granulocytes using LysMcre mice. Transgenic Res 8, 265–277 (1999).
Ovchinnikov, D. A., Deng, J. M., Ogunrinu, G. & Behringer, R. R. Col2a1-directed expression of Cre recombinase in differentiating chondrocytes in transgenic mice. Genesis 26, 145–146 (2000).
Tsukasaki, M. et al. OPG Production Matters Where It Happened. Cell Rep. 32, 108124 (2020).
Horiuchi, K. et al. Identification and characterization of a novel protein, periostin, with restricted expression to periosteum and periodontal ligament and increased expression by transforming growth factor beta. J. Bone Min. Res. 14, 1239–1249 (1999).
Duchamp de Lageneste, O. et al. Periosteum contains skeletal stem cells with high bone regenerative potential controlled by Periostin. Nat. Commun. 9, 773 (2018).
Ortinau, L. C. et al. Identification of functionally distinct Mx1+αSMA+ periosteal skeletal stem cells. Cell Stem Cell 25, 784–796.e785 (2019).
Xu, J. et al. PDGFRα reporter activity identifies periosteal progenitor cells critical for bone formation and fracture repair. Bone Res. 10, 7 (2022).
Matthews, B. G. et al. Heterogeneity of murine periosteum progenitors involved in fracture healing. Elife 10, https://doi.org/10.7554/eLife.58534 (2021).
Rios, H. et al. periostin null mice exhibit dwarfism, incisor enamel defects, and an early-onset periodontal disease-like phenotype. Mol. Cell Biol. 25, 11131–11144 (2005).
Chung, U. I., Lanske, B., Lee, K., Li, E. & Kronenberg, H. The parathyroid hormone/parathyroid hormone-related peptide receptor coordinates endochondral bone development by directly controlling chondrocyte differentiation. Proc. Natl Acad. Sci. USA 95, 13030–13035 (1998).
Maeda, Y. et al. Indian Hedgehog produced by postnatal chondrocytes is essential for maintaining a growth plate and trabecular bone. Proc. Natl Acad. Sci. USA 104, 6382–6387 (2007).
Nakashima, T. et al. Evidence for osteocyte regulation of bone homeostasis through RANKL expression. Nat. Med 17, 1231–1234 (2011).
Xiong, J. et al. Matrix-embedded cells control osteoclast formation. Nat. Med 17, 1235–1241 (2011).
Kim, Y. et al. Generation of transgenic mice for conditional overexpression of Sox9. J. Bone Min. Metab. 29, 123–129 (2011).
Lui, J. C. et al. Differential aging of growth plate cartilage underlies differences in bone length and thus helps determine skeletal proportions. PLoS Biol. 16, e2005263 (2018).
Hirasawa, T. & Kuratani, S. Evolution of the vertebrate skeleton: morphology, embryology, and development. Zool. Lett. 1, 2 (2015).
Shimada, A. et al. Trunk exoskeleton in teleosts is mesodermal in origin. Nat. Commun. 4, 1639 (2013).
Decotto, E. & Spradling, A. C. The Drosophila ovarian and testis stem cell niches: similar somatic stem cells and signals. Dev. Cell 9, 501–510 (2005).
Kirilly, D. & Xie, T. The Drosophila ovary: an active stem cell community. Cell Res. 17, 15–25 (2007).
Rabbani, P. et al. Coordinated activation of Wnt in epithelial and melanocyte stem cells initiates pigmented hair regeneration. Cell 145, 941–955 (2011).
Tsukasaki, M. et al. Host defense against oral microbiota by bone-damaging T cells. Nat. Commun. 9, 701 (2018).
Hayashi, M. et al. Osteoprotection by semaphorin 3A. Nature 485, 69–74 (2012).
Terashima, A. et al. Sepsis-induced osteoblast ablation causes immunodeficiency. Immunity 44, 1434–1443 (2016).
Seike, M., Omatsu, Y., Watanabe, H., Kondoh, G. & Nagasawa, T. Stem cell niche-specific Ebf3 maintains the bone marrow cavity. Genes Dev. 32, 359–372 (2018).
Tsukasaki, M. et al. Stepwise cell fate decision pathways during osteoclastogenesis at single-cell resolution. Nat. Metab. 2, 1382–1390 (2020).
Acknowledgements
We thank K. Kusubata, S.Yin, Y. Morishita, T. Tsubokawa, K. Nagumo, A. Suematsu, M. Inoue, T. Asano and K. Kubo for thoughtful discussion and valuable technical assistance. This work was supported in part by a grant for the Grants-in-Aid for Specially Promoted Research (15H05703), Scientific Research B (18H02919, 21H03104), Challenging Research (18K19438), Young Scientists (19K18943), JSPS fellows (18J00744) and JSPS long term fellowship L20539 from the Japan Society for the Promotion of Science (JSPS), and by Japan Agency for Medical Research and Development (AMED) under grant number JP22ek0410073, AMED-CREST under Grant Number JP22gm1210008 and AMED-PRIME under Grant Number JP22gm6310029h0001.
Author information
Authors and Affiliations
Contributions
M.T. designed and performed most of the experiments, interpreted the results and wrote the manuscript. N.K., T.N.K., R.M., Y.A., T.Nitta, K.O. and S.O. contributed to experiments and data interpretation. N.C.N.H. and Y.S. performed computational analyses and contributed to data interpretation. A.T. and W.P. conducted bone histomorphometric analyses. T. Nakashima, T. Nakamura and H.A. contributed to generation of genetically modified mice and data interpretation. R.B contributed to data interpretation and manuscript preparation. H.T. directed the project and wrote the manuscript.
Corresponding author
Ethics declarations
Competing interests
The Department of Osteoimmunology is an endowed department supported by unrestricted grants from the AYUMI Pharmaceutical Corporation, Chugai Pharmaceutical Co., Ltd., MIKI HOUSE Co., Ltd. and Noevir Co., Ltd.
Peer review
Peer review information
Nature Communications thanks Geert Carmeliet, Matthew Greenblatt and the other anonymous reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Tsukasaki, M., Komatsu, N., Negishi-Koga, T. et al. Periosteal stem cells control growth plate stem cells during postnatal skeletal growth. Nat Commun 13, 4166 (2022). https://doi.org/10.1038/s41467-022-31592-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-022-31592-x
This article is cited by
-
Identification of an intronic enhancer regulating RANKL expression in osteocytic cells
Bone Research (2023)
-
The decisive early phase of bone regeneration
Nature Reviews Rheumatology (2023)
-
Generation of bicistronic Dmp1-Cre knock-in mice using a self-cleaving 2A peptide
Journal of Bone and Mineral Metabolism (2023)
-
Insights into skeletal stem cells
Bone Research (2022)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.