Abstract
Human memory is thought to depend on a circuit of connected brain regions, but this hypothesis has not been directly tested. We derive a human memory circuit using 53 case reports of strokes causing amnesia and a map of the human connectome (n = 1000). This circuit is reproducible across discovery (n = 27) and replication (n = 26) cohorts and specific to lesions causing amnesia. Its hub is at the junction of the presubiculum and retrosplenial cortex. Connectivity with this single location defines a human brain circuit that incorporates > 95% of lesions causing amnesia. Lesion intersection with this circuit predicts memory scores in two independent datasets (N1 = 97, N2 = 176). This network aligns with neuroimaging correlates of episodic memory, abnormalities in Alzheimer’s disease, and brain stimulation sites reported to enhance memory in humans.
Similar content being viewed by others
Introduction
In 1937 James Papez described a human brain circuit based on gross pathology that included the hippocampus, anterior thalamus, mammillary bodies of the hypothalamus, posterior cingulate, and fornix1. Although initially described as an emotion circuit, it was later noted that lesions to this circuit disrupted episodic memory2,3,4. The best-known example is patient H.M., who suffered severe anterograde amnesia following bilateral medial temporal lobe resections2,5.
Subsequent work with laboratory animals6,7,8 and human neuroimaging9,10,11 further supported these findings, leading to general acceptance that memory (specifically episodic memory) localizes to the circuit of Papez. Neuroimaging studies have also identified a partially overlapping circuit, termed the default mode network, hypothesized to mediate episodic memory10,12,13.
The exact location of this circuit has taken on new importance with the increased prevalence of memory disorders such as Alzheimer’s disease14,15 and efforts to identify new therapies16. For example, brain stimulation aimed at improving human memory has been directed at multiple different brain targets, both inside and outside the traditional circuit of Papez17,18,19,20. These studies highlight important unanswered questions regarding the localization of human memory including whether memory localizes to a brain circuit, which regions should be included in this circuit, and whether some nodes of this circuit are more important than others21. In fact, the hypothesis that human brain lesions that disrupt memory localize to a single connected brain circuit has never been formally tested.
Recently, new tools have become available that allow us to better address these questions. By combining lesion locations with a wiring diagram of the human brain termed the human connectome, we can determine whether lesion locations causing similar symptoms fall within a single brain circuit and the hub of this circuit. This technique, termed lesion network mapping, has been successfully applied to hallucinations, delusions, movement disorders, coma, and even criminality22,23,24. Here, we apply this technique to lesions disrupting memory.
Results
Identifying amnesia-causing lesions
In our literature search for amnesia-causing lesions, we identified 53 lesion locations causing clinically-evident deficits in episodic memory (Supplementary Table 1). Lesion location was heterogeneous and included numerous different brain regions (Fig. 1). As expected, many lesions occurred at classic locations within the circuit of Papez (Fig. 1a); however, many lesions did not (Fig. 1b).
All 53 lesion cases were classified as “severe” amnesia (the memory deficit was clinically apparent even without formal neuropsychological testing), involved anterograde memory loss, and included documented impairment in verbal memory (Supplementary Table 1).
Mapping amnesia-causing lesions to a common brain circuit
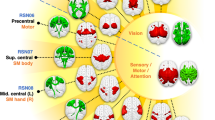
We computed the network of brain regions functionally connected to each lesion location (Fig. 2). Despite heterogeneity in lesion location, lesions causing amnesia were part of a common brain circuit. Over 95% of amnesia-causing lesion locations were functionally connected to a single location in the hippocampus (Fig. 2c). The connectivity pattern of lesions causing amnesia was highly reproducible when split into two randomized subsamples (spatial correlation r = 0.98, Fig. 2d, e), and when restricting analysis to sub-cohorts with formal score reports, retrograde amnesia, and visual memory impairment (Supplementary Fig. 2).
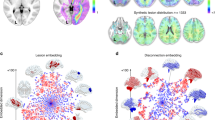
Lesion network mapping method and split half replication. Individual amnesia-causing lesions were mapped to a common brain template (a). Connectivity between each lesion location and the rest of the brain was computed using resting state functional connectivity from 1000 healthy control subjects (b). Positive correlations with the lesion location are shown in warm colors while negative correlations (anticorrelations) are shown in cool colors. Individual lesion network maps were thresholded, binarized, and overlapped to identify connections common to the lesion locations (c). Random splitting of our amnesia-causing lesion sample into two cohorts demonstrates high reproducibility of lesion network overlap (d, e). Additional iterations of random splitting were similar (Supplementary Figure 2)
This connectivity profile was specific to lesions causing amnesia compared to generic lesions (Fig. 3b, two-sample t-test voxelwise FWE p < 0.05) or lesions causing other non-memory symptoms (Fig. 3c, two-sample t-test voxelwise FWE p < 0.05). A conjunction analysis identified a focal region in the subiculum-retrosplenial continuum whose connectivity was both sensitive (connected to >95% of amnesia lesions) and specific (two-sample t-test voxelwise FWE p < 0.05 in both specificity analyses) for lesions causing amnesia (Fig. 3d). Note that only 10 of our 53 amnesia lesions physically intersected this location, but 51 of our 53 lesions were functionally connected to this location. A small anticorrelated region in the intraparietal sulcus also survived this analysis (Supplementary Fig. 3).
Sensitivity and specificity of lesion network mapping of amnesia. Using our full cohort of lesions causing amnesia (n = 53), >95% of lesion locations were functionally connected to the junction of the hippocampus and retrosplenial cortex (a). This connectivity was specific to lesions causing amnesia compared to a large cohort of control lesions causing non-specific symptoms (b) or lesions causing specific symptoms other than amnesia (c). (Specificity analyses compared unthresholded lesion network maps between amnesia and non-amnesia groups using a voxelwise two-sample t-test corrected for multiple comparisons with a conservative voxel-based Family Wise Error rate p < 0.05.) The conjunction of our sensitivity and specificity analyses identifies a focal region at the subiculum-retrosplenial continuum (d) that overlaps the posterior segment of the pre-subiculum
By definition, functional connectivity with our region in the subiculum-retrosplenial continuum defines a human brain circuit that encompasses >95% of lesion locations causing amnesia (Fig. 4a). This circuit includes classic nodes in the circuit of Papez and the default mode network, but also regions outside these networks (Fig. 4a, Table 1, Supplementary Fig. 4). For example, frontal and parietal cortical regions fall outside the classic circuit of Papez while cerebellar, thalamic, white matter, and occipital regions fall outside the classic default mode network.
Validation of our human memory circuit in independent lesion cohorts. Functional connectivity with the subiculum-retrosplenial continuum (see Fig. 3d) defines a human memory network that by definition encompasses 51/53 lesion locations causing amnesia (a, lesion locations shown in white). Intersection between lesion location and this network was associated with memory scores in an independent lesion dataset (n = 97), including the five patients with the worst verbal memory scores (b, lesion locations shown in purple) and the five patients with the best verbal memory scores (c, lesion locations shown in green)
Damage to circuit predicts memory in independent datasets
Overlap between lesion location and our memory circuit predicted continuous memory scores in an independent dataset of stroke lesions25 and in an independent dataset of lesions from penetrating head trauma26 (Fig. 4b, c). Immediately after stroke, intersection with our memory circuit was correlated with both verbal memory (Pearson correlation, r = −0.21, p < 0.04) and spatial memory scores (Pearson correlation, r = −0.36, p < 10−3). Following penetrating head trauma, intersection between lesion location and our memory circuit was correlated with remote memory scores for events that occurred close to the time of brain injury (Pearson correlation, r = −0.34, p < 10−5). All correlations remained significant after controlling for patient age, education, and lesion size (p < 0.05 for all analyses, Supplementary Table 2). Finally, we tested whether our memory circuit was a better predictor of lesion-induced memory deficits in these independent datasets than a priori maps of the default mode network. No matter which a priori map of the default mode network we used, which covariates we included, and which memory test we examined, intersection with our memory circuit was a significant independent predictor of lesion-induced memory deficits while intersection with the default network was not (p < 0.05 for all analyses, Supplementary Table 3).
Exploratory analyses restricted to brain lesions falling outside the classic circuit of Papez (e.g. in frontal and lateral parietal cortex) and outside the classic default mode network (e.g. in occipital cortex and brainstem), suggest that lesion locations intersecting peripheral nodes of our memory circuit are still associated with worse memory scores (spatial memory: Pearson correlation, r = −0.46, p < 5 × 10−4; verbal memory: Pearson correlation, r = −0.19, p < 0.17; Supplementary Fig. 5).
Relevance beyond brain lesions
Our lesion-derived memory circuit aligned well with neuroimaging correlates of episodic memory in normal subjects (Fig. 5a) and neuroimaging abnormalities in Alzheimer’s disease (Fig. 5b). Overlap with neuroimaging correlates of episodic memory was significantly stronger than for neuroimaging correlates of working memory (t (39) = 3.5, p < 0.005. 95% CI [13.0, 47.7]) or language (t (39) = 3.4, p < 0.002, 95% CI [11.8, 46.6]; two-sample t-test, Bonferroni corrected). Overlap with neuroimaging abnormalities in Alzheimer’s disease was significantly greater than for neuroimaging abnormalities in frontotemporal dementia (t (45) = 4.6, p < 5 × 10 −5, 95% CI [10.3, 26.7]) or primary progressive aphasia (t (39) = 2.9, p < 0.007, 95% CI [4.7, 30.0]; two-sample t-test, Bonferroni corrected).
Memory circuit alignment with other imaging and stimulation modalities. Our human memory circuit derived from amnesia-causing brain lesions aligns well with data from other modalities. Functional connectivity with the subiculum-retrosplenial continuum (See Fig. 3D) defines a brain network that aligns well with neuroimaging correlates of episodic memory based on functional neuroimaging (a, purple spheres), neuroimaging abnormalities in Alzheimer’s disease (b, purple spheres), and locations where brain stimulation has been reported to enhance memory performance in humans (c, green spheres)
We qualitatively explored the relationship between our lesion-derived memory circuit and brain stimulation sites reported to enhance memory in humans. Our search identified four stimulation sites meeting inclusion criteria17,18,19,20, all four of which clearly fell within our memory circuit (Fig. 5c).
Discussion
There are three major findings in this paper. First, lesions causing amnesia are part of a single functionally connected brain circuit. Second, this memory circuit can be defined based on connectivity to a single brain region, the subiculum-retrosplenial continuum. Finally, this memory circuit may be relevant beyond brain lesions, as it aligns with neuroimaging correlates of episodic memory, neuroimaging abnormalities in Alzheimer’s disease, and brain stimulation studies.
The circuit of Papez1, and more recently the default mode network10,12,13,27,28,29,30,31, have been proposed as neuroanatomical substrates for human memory. The topography of our circuit aligns remarkably well with this prior work. In fact, the alignment is so good that refinements based on our paper could be considered incremental. However, the most novel aspect of our paper is not refining the topography of this circuit but linking this circuit to human memory in a causal way. Unlike functional neuroimaging, lesion studies allow for causal links between neuroanatomy and brain function24,32. The hypothesis that human brain lesions causing amnesia localize to a connected brain circuit has never been formally tested. Here, we derive a human episodic memory circuit empirically, without a priori assumptions about the relevant brain regions, based on brain lesions that causally disrupt human memory. The technique used to perform this analysis, termed lesion network mapping, is still relatively new but has been validated and proven useful across a wide range of neuropsychiatric symptoms22,23,24. However, the current paper goes beyond these prior studies as it is the first to validate lesion network mapping results by predicting deficits on a continuous basis in independent lesion datasets. By definition, our memory circuit encompasses the original lesion locations used to derive this circuit. However, this is no guarantee that intersection with our memory circuit would predict continuous memory scores in independent lesion datasets. The fact that our circuit predicted memory scores in two independent datasets differing in lesion etiology and method of memory assessment is an important validation of our results and of lesion network mapping more generally.
Despite strong similarity, the topography of our lesion-derived memory circuit is not identical to either the circuit of Papez or the default mode network as classically defined. Regions in frontal cortex, lateral parietal cortex, occipital cortex, cerebellum, basal ganglia, and white matter fall outside the traditional circuit of Papez, while regions in the anterior thalamus, basal ganglia, cerebellum, occipital cortex, white matter, and midbrain fall outside the standard default mode network. The role of many of these regions in human memory has remained controversial despite supporting evidence13,25,33,34,35,36,37,38. Our results suggest these regions may be important, as intersection with our lesion-based memory circuit, but not the default mode network, was an independent predictor of lesion-induced memory deficits. Similarly, peripheral nodes of our memory circuit outside the classic circuit of Papez still showed utility in predicting lesion-induced memory deficits (see Supplementary Fig. 5).
In addition to this memory circuit derived from positive functional connectivity, we observed that the intraparietal sulcus is anticorrelated with lesion locations that disrupt memory (Supplementary Fig. 3). It is possible that this region plays an antagonistic role in episodic memory, with increased activity actually impairing episodic memory. Such a hypothesis, while speculative, has some support from prior neuroimaging studies13, TMS studies39, and selective sparing of this region in AD40.
The hub of our human memory circuit is at the junction of the subiculum and the retrosplenial cortex, a region referred to as the subiculum-retrosplenial continuum41,42. Connectivity to this single brain location defines a human brain circuit that encompasses over 95% of our 53 lesions causing amnesia. It is not surprising that the hub of our human memory circuit resides in the hippocampus, but exactly which area of the hippocampus was unclear43. Historically, much more attention has been paid to CA1 than to the subiculum44,45, although recent evidence has provided increasing support for the importance of the subiculum-retrosplenial continuum41,42,46,47. Anatomically, the subiculum is the main outflow track of the hippocampus6 with widespread cortical connections48,49,50,51, which could explain its connectivity to the greatest number of brain lesions causing amnesia. However, connectivity to this region was also specific, as it was not connected to lesions that did not disrupt human memory. Interestingly, the subiculum-retrosplenial continuum seems to be particularly sensitive to the effects of diaschisis. For example, lesions to the anterior nucleus of the thalamus will produce long-term potentiation abnormalities in the subiculum-retrosplenial continuum52. Whether amnesia from brain lesions in our circuit comes from diachisis-like effects on the subiculum-retrosplenial continuum, or whether memory requires intact function of the entire circuit connected to this region is an important topic for future work.
Of our 53 amnesia lesions, only two cases were not connected to the subiculum-retrosplenial continuum (Coslett 1991 and Maeshima 2010 in Supplementary Table 1). One case had a severe language deficit, and the authors hypothesized that this may have been responsible for an apparent memory deficit (Coslett 1991 in Supplementary Table 1). The other case showed significant attention deficits, and the authors noted that symptoms differed from those typical of amnesia (Maeshima 2010 in Supplementary Table 1). Given the remarkable consistency across our other 51 lesion cases, we suspect other deficits may have led to apparent (but not actual) episodic memory impairment in these cases.
There are several important limitations. The 53 amnesia cases used to derive the circuit relied on existing case reports, subject to publication bias and often limited clinical assessment by the original authors. In fact, the two cases that fell outside our circuit were almost certainly not cases of lesion-induced amnesia on closer inspection. Similarly, our 53 lesion cases are not intended to be exhaustive. There are likely other lesion cases that met our criteria but that we failed to include. However, given the high reproducibility of our split cohort and sub-cohort analyses, it is unlikely that inclusion of further lesions or additional stratification based on clinical characteristics would alter our results. Similarly, clinical heterogeneity or errors in lesion tracing should bias us against the present findings of a common brain circuit. In our independent validation cohorts, we did not have pre-lesion memory testing to examine changes in memory directly associated with the lesion but were limited to a single assessment influenced by age, education, incipient disease, and undoubtedly many other factors. This limitation is most obvious for the penetrating head trauma dataset, in which memory was tested decades after the lesion, and the exact date of injury was unknown (making it unclear whether remote memory deficits from around the time of the lesion were anterograde or retrograde). Similarly, we were limited by the memory tests administered in these cohorts, limiting our ability to show specificity to episodic versus other forms of memory (e.g. semantic or implicit memory). Finally, we used resting state functional connectivity to define our circuit, consistent with prior lesion network mapping studies22,23,24, which is an indirect measure of neuronal activity with inherent limits in spatial resolution. For example, the subiculum-retrosplenial continuum lies in close anatomical proximity to the posterior cerebral artery which could introduce vascular artifact51. Finally, one could argue that functional connectivity data acquired during an episodic memory task (rather than during rest) would be more appropriate52. Future work using data from different episodic memory tasks to try and improve on our prediction of lesion-induced memory deficits should be considered. However, networks derived from resting state and task data are likely to be extremely similar53,54,55,56 and one must be careful to avoid confounds associated with task-based connectivity estimates57,58.
Our memory circuit was derived and validated using the lesion literature as focal brain lesions allow for causal inferences regarding localization of function24,32,59. However, our circuit is likely relevant for human memory in general, not just patients with brain lesions. First, our circuit aligns well with an extensive literature on neuroimaging correlates of episodic memory in normal subjects. In fact, several nodes of our circuit that go beyond the circuit of Papez (e.g. lateral parietal cortex, lateral temporal cortex) or the default mode network (e.g. midbrain, inferior frontal cortex) match these neuroimaging findings (see Fig. 5a). Second, our circuit aligns with pathology in other disorders of memory such as Alzheimer’s disease. While neuroimaging abnormalities in Alzheimer’s disease have not been consistent across different modalities60,61 these abnormalities map well to our memory circuit and to the default mode network27,28. Note that alignment of our memory circuit with neuroimaging correlates of episodic memory and Alzheimer’s pathology is not driven by the broad spatial extent of our memory circuit, as this alignment was specific compared to neuroimaging correlates of other functions or other diseases. Whether our memory circuit is a better predictor of Alzheimer’s pathology than the default mode network, and whether our circuit predicts memory deficits in Alzheimer’s as it does for brain lesions requires future work. Other disorders of memory including limbic encephalitis62 transient global amnesia63, and fentanyl overdose64 also appear to match our circuit well, although alignment with these pathologies was not formally tested.
Finally, our circuit aligns well with brain stimulation studies reported to enhance human memory17,18,19,20. Stimulation sites such as the fornix and medial temporal lobe are part of the classic circuit of Papez17,18, but lateral parietal cortex19 and precuneus20 are not, but still fall within our lesion-derived memory circuit. Future work is needed to determine whether our circuit can differentiate brain stimulation sites that do versus do not manipulate memory function. The current circuit topography could be useful as a guide for this future work, including providing a template for multifocal stimulation montages65.
Methods
Literature review and lesion tracing
The Medline database was searched through 2017 by combining the search terms “stroke,” or “cerebrovascular,” or “ischemia,” or “hemorrhage,” with the terms “amnesia,” or “memory”. The criteria not “subarachnoid,” not “dementia,” not “cardiac arrest,” not “transient global amnesia” were also added and search returns were limited to human studies. This search returned 4855 possible matches. These returns were limited to English language articles, and the titles of 1000 papers most related to the search criteria were reviewed, identifying the most relevant 500 papers. These abstracts were reviewed, identifying the most relevant English language papers. Abstract review looked for articles on human studies, primarily about a patient with memory loss, memory loss acquired by a lesion, and the etiology was not transient global amnesia, not Alzheimer’s disease-related, and not a brain tumor or other non-acquired lesions. From this set, we reviewed 250 full-text articles and included reports that fit the following criteria: (1) Case report format or individual case description; (2) Adult population; (3) Clinically relevant episodic memory deficits by bedside or neuropsychological tests attributed by the authors to an acute brain lesion; (4) Availability of a CT or MRI image depicting the lesion location(s) of sufficient quality that the lesion could be transcribed onto a standard brain template (Supplementary Fig. 1).
Fifty-three cases of amnesia were found with identifiable causative brain lesions (mean age 57.5 ± 13 years, range 27–72, 66% male). In three of 53 cases a second lesion was reported but was not thought to contribute to the acute memory deficit per the original authors (e.g. an old prior infarct) and was excluded. Brain lesions were mapped by hand onto a standard template brain from FSL (MNI152 asymmetric brain, 1 × 1 mm, http://fsl.fmrib.ox.ac.uk/fsldownloads/). Lesions from published figures were traced in the 2D plane(s) in which they were displayed, using neuroanatomical landmarks to accurately transfer the lesion location onto the template brain (Fig. 1).
Lesion network mapping
The network of brain regions functionally connected to each lesion location was identified using a previously validated technique termed lesion network mapping22,23,24 (Fig. 2). Briefly, resting state functional connectivity between each lesion location and the rest of the brain was computed using a publicly available connectome dataset from 1000 healthy right-handed subjects (42.7% male subjects, ages 18–35 years, mean age 21.3 years)28,66. Resting state MRI data were processed in accordance with the strategy of Fox et al., 200527, including global signal regression67. Both positive and negative correlations (anticorrelations) with the seed region of interest were included. Each of the 53 individual network maps was thresholded at a t-value of ±7 (corresponding to voxelwise FWE-corrected p < 10−6) consistent with prior work23,68. The resulting 53 network maps were binarized and overlapped to identify regions of shared connectivity and masked using a whole-brain template (MNI152 2009 asymmetric brain).
To test for reproducibility, the 53 amnesia-causing lesions were randomly sorted into two subgroups (Group A, n = 27; Group B, n = 26). Lesion network overlap maps were created separately for each subgroup, then compared using spatial correlation. This random splitting was performed multiple times to ensure reproducibility.
Next, we repeated our lesion network overlap analysis on lesion sub-cohorts including (1) cases with formal scores documenting amnesia severity (n = 30), (2) cases with documented retrograde memory impairment (n = 18), (3) cases with documented visual memory impairment (n = 20).
Sensitivity and specificity testing
The lesion network overlap map for the full group (n = 53) was thresholded to identify regions connected to >95% of lesion locations causing amnesia (Fig. 3a). Specificity was assessed by comparing lesion network maps from lesion locations causing amnesia (n = 53) to network maps from lesion locations not specific to memory deficits (n = 490)69. A second specificity analysis was conducted using a separate set of control lesions (n = 63) selected and traced in the same way as the current amnesia lesions, but which were selected for causing an assortment of different neurological symptoms including aphasia, hallucinations, and pain22. Both specificity analyses compared unthresholded lesion network maps between groups using a voxelwise two-sample t-test in SPM 12, correcting for multiple comparisons with a conservative voxel-based Family Wise Error rate p < 0.05.
To identify an ROI both sensitive and specific to lesion locations causing amnesia, a conjunction between our sensitivity map (voxels connected to >95% of lesion locations causing amnesia) and voxels surviving both specificity tests was computed. The resultant ROI was overlapped with an existing hippocampal subfield atlas70.
Defining a human episodic memory circuit
By definition, resting state functional connectivity with the above ROI defines a human brain circuit that encompasses lesion locations causing amnesia while avoiding control lesion locations. We derived this circuit using the above ROI as a seed region and the same resting state functional connectivity methods described earlier, including thresholding the map for significance at t > 7 (voxel-based FWE-corrected p < 10 −6). Local maxima in this map were identified using the FSL clustering algorithm and a peak identification threshold of t > 26. We refer to this functional connectivity map as our lesion-based human episodic memory circuit.
Validation using independent lesion datasets
To test the hypothesis that other lesions intersecting our lesion-based memory circuit would result in impaired memory, we used two independent lesion datasets in which formal memory testing was performed on each patient. Lesions in the first dataset (N1 = 97) were caused by ischemic stroke, with memory tests administered acutely following stroke25. We focused on acute factor scores for verbal and spatial memory based on prior work using this dataset25.
To ensure that results were not restricted to one lesion etiology (stroke), we repeated our analysis on a second independent dataset (N2 = 176) with lesions caused by penetrating head trauma during the Vietnam War. Memory tests were administered fifteen or more years after brain injury26,71. Memory for events around the time of brain injury was assessed using a previously published adaptation of the Marilyn Albert remote memory battery, restricted to events from the 1970s71,72.
We quantified the overlap between each lesion location and our memory circuit by adding the t-values of each voxel in our memory circuit that fell within each lesion mask. These values were then related to memory scores using Pearson correlation. Correlation analyses were repeated including age, education, and lesion size as covariates.
For visualization purposes, lesion locations from the five patients with the worst verbal memory factor scores and five patients with the best verbal memory factor scores (validation dataset 1, N1 = 97) were displayed overlaid on our human memory circuit.
To determine whether our memory circuit was a better predictor of lesion-induced memory deficits than the default mode network, we also computed lesion intersection with the default mode network. As there is no consensus on how best to define the default mode network, we defined it in three different ways based on previously published methods27,28 (Neurosynth meta-analysis term “default mode”). The default mode network seeds reported in Fox 200527 and Yeo 201128 were converted to default mode network maps using the same connectome that we used to generate our memory circuit and thresholded at t > 7. We compared the number of amnesia-causing lesions intersecting our lesion-derived memory circuit with the number of amnesia-causing lesions intersecting the three default mode network maps using a criteria of >50% of the lesion body intersecting the network of interest. Additionally, intersection between each lesion location and each default mode network map was quantified the same way we calculated intersection with our memory circuit. We then combined both measures of network intersection (memory circuit and default mode network) in a linear model to identify independent predictors of memory deficits. We repeated this analysis with age, education, and lesion size as covariates.
As an exploratory analysis, we tested whether lesions intersecting peripheral nodes of our memory circuit (i.e. regions outside the classic circuit of Papez) would also impair memory. We generated a subset of lesions from validation dataset 1 (n = 55 of 97) that fell outside the classic circuit of Papez by thresholding our lesion-based human memory circuit at t > 38 and selecting all lesions that failed to intersect any voxel. This threshold was chosen empirically by visual inspection to identify a set of lesions falling outside the classic circuit of Papez (Supplementary Fig. 5). The above Pearson correlation analyses were repeated on this lesion subset, focusing on acute verbal and spatial memory factor scores.
Relationship to prior functional neuroimaging studies
MNI coordinates were extracted from previously published neuroimaging meta-analyses of episodic memory73 and Alzheimer’s disease60. As a control, coordinates were also extracted from meta-analyses of working memory74, language75, frontotemporal dementia76, and primary progressive aphasia77. For each coordinate, we identified the t-value in our lesion-based human memory circuit at that coordinate. The t-values for episodic memory73, were compared to those for working memory74, and language75 using two-tailed t-tests and Bonferroni correction (for two comparisons). A similar analysis was used to compare the t-values for Alzheimer disease60 to those for frontotemporal dementia76 and primary progressive aphasia77.
Relationships to prior brain stimulation studies
A literature search was performed on PubMed using the search term combinations “brain stimulation memory enhancement”, “TMS Alzheimer memory”, and “deep brain stimulation Alzheimer memory”. Reports containing MNI coordinates of memory stimulation sites or a clear anatomical depiction of memory stimulation sites were selected17,18,19,20. Correspondence between previously reported stimulation sites and our lesion-based memory circuit was assessed qualitatively.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Code availability
The code that support the findings of this study are available from the corresponding author upon reasonable request.
References
Papez, J. W. A proposed mechanism of emotion. Arch. Neurol. Psychiatry 38, 725–743 (1937).
Scoville, W. B. & Milner, B. Loss of recent memory after bilateral hippocampal lesions. J. Neurol. Neurosurg. psychiatry 20, 11 (1957).
Von Cramon, D. Y., Hebel, N. & Schuri, U. A contribution to the anatomical basis of thalamic amnesia. Brain 108, 993–1008 (1985).
Valenstein, E. et al. Retrosplenial amnesia. Brain 110, 1631–1646 (1987).
Corkin, S. What’s new with the amnesic patient HM? Nat. Rev. Neurosci. 3, 153 (2002).
Swanson, L. W. & Cowan, W. M. Hippocampo-hypothalamic connections: origin in subicular cortex, not ammon’s horn. Science 189, 303–304 (1975).
Zola-Morgan, S., Squire, L. R. & Mishkin, M. The neuroanatomy of amnesia: amygdala-hippocampus versus temporal stem. Science 218, 1337–1339 (1982).
Morris, R., Pandya, D. N. & Petrides, M. Fiber system linking the mid‐dorsolateral frontal cortex with the retrosplenial/presubicular region in the rhesus monkey. J. Comp. Neurol. 407, 183–192 (1999).
Choo, I. H. et al. Relationship of fibrillar beta-amyloid burden with age-at-onset in Alzheimer’s disease. Alzheimer’s. Dement. J. Alzheimer’s. Assoc. 6, S39–S40 (2010).
Vincent, J. L. et al. Coherent spontaneous activity identifies a hippocampal-parietal memory network. J. Neurophysiol. 96, 3517–3531 (2006).
Wang, L. et al. Changes in hippocampal connectivity in the early stages of Alzheimer’s disease: evidence from resting state fMRI. Neuroimage 31, 496–504 (2006).
Greicius, M. D., Srivastava, G., Reiss, A. L. & Menon, V. Default-mode network activity distinguishes Alzheimer’s disease from healthy aging: evidence from functional MRI. Proc. Natl Acad. Sci. USA 101, 4637–4642 (2004).
Sestieri, C., Corbetta, M., Romani, G. L. & Shulman, G. L. Episodic memory retrieval, parietal cortex, and the default mode network: functional and topographic analyses. J. Neurosci. 31, 4407–4420 (2011).
Alzheimer’s, A. 2015 Alzheimer’s disease facts and figures. Alzheimer’s. Dement. J. Alzheimer’s. Assoc. 11, 332 (2015).
Weuve, J., Hebert, L. E., Scherr, P. A. & Evans, D. A. Prevalence of Alzheimer disease in US states. Epidemiology 26, e4–e6 (2015).
Lanctôt, K. L. et al. Neuropsychiatric signs and symptoms of Alzheimer’s disease: new treatment paradigms. Alzheimer’s. Dement. Transl. Res. Clin. Interv. 3, 440–449 (2017).
Hamani, C. et al. Memory enhancement induced by hypothalamic/fornix deep brain stimulation. Annals of Neurology: Official. J. Am. Neurol. Assoc. Child Neurol. Soc. 63, 119–123 (2008).
Suthana, N. et al. Memory enhancement and deep-brain stimulation of the entorhinal area. New Engl. J. Med. 366, 502–510 (2012).
Wang, J. X. et al. Targeted enhancement of cortical-hippocampal brain networks and associative memory. Science 345, 1054–1057 (2014).
Koch, G. et al. Transcranial magnetic stimulation of the precuneus enhances memory and neural activity in prodromal Alzheimer’s disease. Neuroimage 169, 302–311 (2018).
Aggleton, J. P., Pralus, A., Nelson, A. J. & Hornberger, M. Thalamic pathology and memory loss in early Alzheimer’s disease: moving the focus from the medial temporal lobe to Papez circuit. Brain 139, 1877–1890 (2016).
Boes, A. D. et al. Network localization of neurological symptoms from focal brain lesions. Brain 138, 3061–3075 (2015).
Darby, R. R., Horn, A., Cushman, F. & Fox, M. D. Lesion network localization of criminal behavior. Proc. Natl Acad. Sci. USA 115, 601–606 (2018).
Fox, M. D. Mapping symptoms to brain networks with the human connectome. New Engl. J. Med. 379, 2237–2245 (2018).
Corbetta, M. et al. Common behavioral clusters and subcortical anatomy in stroke. Neuron 85, 927–941 (2015).
Raymont, V., Salazar, A., Krueger, F. & Grafman, J. “Studying injured minds”–the Vietnam head injury study and 40 years of brain injury research. Front. Neurol. 2, 15 (2011).
Fox, M. D. et al. The human brain is intrinsically organized into dynamic, anticorrelated functional networks. Proc. Natl Acad. Sci. USA 102, 9673–9678 (2005).
Yeo, B. T. et al. The organization of the human cerebral cortex estimated by intrinsic functional connectivity. J. Neurophysiol. 106, 1125–1165 (2011).
Raichle, M. E. et al. A default mode of brain function. Proc. Natl Acad. Sci. USA 98, 676–682 (2001).
Buckner, R. L., Andrews‐Hanna, J. R. & Schacter, D. L. The brain’s default network. Ann. N Y. Acad. Sci. 1124, 1–38 (2008).
Spreng, R. N. & Grady, C. L. Patterns of brain activity supporting autobiographical memory, prospection, and theory of mind, and their relationship to the default mode network. J. Cogn. Neurosci. 22, 1112–1123 (2010).
Rorden, C., Karnath, H. O. & Bonilha, L. Improving lesion-symptom mapping. J. Cogn. Neurosci. 19, 1081–1088 (2007).
Tulving, E. et al. Hemispheric encoding/retrieval asymmetry in episodic memory: positron emission tomography findings. Proc. Natl Acad. Sci. USA 91, 2016–2020 (1994).
Shallice, T. et al. Brain regions associated with acquisition and retrieval of verbal episodic memory. Nature 368, 633 (1994).
Wheeler, M. A., Stuss, D. T. & Tulving, E. Toward a theory of episodic memory: the frontal lobes and autonoetic consciousness. Psychol. Bull. 121, 331 (1997).
Packard, M. G. & Knowlton, B. J. Learning and memory functions of the basal ganglia. Annu. Rev. Neurosci. 25, 563–593 (2002).
Wagner, A. D., Shannon, B. J., Kahn, I. & Buckner, R. L. Parietal lobe contributions to episodic memory retrieval. Trends Cogn. Sci. 9, 445–453 (2005).
Schmahmann, J. D. & Caplan, D. Cognition, emotion and the cerebellum. Brain 129, 290–292 (2006).
Sestieri, C. et al. Interference with episodic memory retrieval following transcranial stimulation of the inferior but not the superior parietal lobule. Neuropsychologia 51, 900–906 (2013).
Liu, T. et al. Cortical gyrification and sulcal spans in early stage Alzheimer’s disease. PloS ONE 7, e31083 (2012).
Dalton, M. A. & Maguire, E. A. The pre/parasubiculum: a hippocampal hub for scene-based cognition? Curr. Opin. Behav. Sci. 17, 34–40 (2017).
Poppenk, J., Evensmoen, H. R., Moscovitch, M. & Nadel, L. Long-axis specialization of the human hippocampus. Trends Cogn. Sci. 17, 230–240 (2013).
Zeidman, P. & Maguire, E. A. Anterior hippocampus: the anatomy of perception, imagination and episodic memory. Nat. Rev. Neurosci. 17, 173 (2016).
Eichenbaum, H. Prefrontal–hippocampal interactions in episodic memory. Nat. Rev. Neurosci. 18, 547 (2017).
Rolls, E. T. The storage and recall of memories in the hippocampo-cortical system. Cell tissue Res. 373, 577–604 (2018).
Matsumoto, N., Kitanishi, T., & Mizuseki, K. The subiculum: unique hippocampal hub and more. Neurosci. Res. 143, 1–12 (2018).
Roy, D. S. et al. Distinct neural circuits for the formation and retrieval of episodic memories. Cell 170, 1000–1012 (2017).
O’Mara, S. The subiculum: what it does, what it might do, and what neuroanatomy has yet to tell us. J. Anat. 207, 271–282 (2005).
Wyass, J. M. & Van Groen, T. Connections between the retrosplenial cortex and the hippocampal formation in the rat: a review. Hippocampus 2, 1–11 (1992).
Child, N. D. & Benarroch, E. E. Anterior nucleus of the thalamus: functional organization and clinical implications. Neurology 81, 1869–1876 (2013).
Viviani, R. A digital atlas of middle to large brain vessels and their relation to cortical and subcortical structures. Front. Neuroanat. 10, 12 (2016).
Buckner, R. L., Krienen, F. M. & Yeo, B. T. Opportunities and limitations of intrinsic functional connectivity MRI. Nat. Neurosci. 16, 832 (2013).
Cole, M. W. et al. Intrinsic and task-evoked network architectures of the human brain. Neuron 83, 238–251 (2014).
Dosenbach, N. U. et al. Distinct brain networks for adaptive and stable task control in humans. Proc. Natl Acad. Sci. USA 104, 11073–11078 (2007).
Tavor, I. et al. Task-free MRI predicts individual differences in brain activity during task performance. Science 352, 216–220 (2016).
Ito, T. et al. Cognitive task information is transferred between brain regions via resting-state network topology. Nat. Commun. 8, 1027 (2017).
Cole, M. W. et al. Task activations produce spurious but systematic inflation of task functional connectivity estimates. NeuroImage 189, 1–18 (2019).
Fox, M. D. & Raichle, M. E. Spontaneous fluctuations in brain activity observed with functional magnetic resonance imaging. Nat. Rev. Neurosci. 8, 700 (2007).
Adolphs, R. Human lesion studies in the 21st century. Neuron 90, 1151–1153 (2016).
Schroeter, M. L. & Neumann, J. Combined imaging markers dissociate Alzheimer’s disease and frontotemporal lobar degeneration–an ALE meta-analysis. Frontiers in Aging. Neuroscience 3, 10 (2011).
Darby, R., Dickerson, B. C. & Fox, M. Anti-correlated networks show paradoxical increased cortical thickness in alzheimer’s disease. Alzheimer’s. Dement. J. Alzheimer’s. Assoc. 14, P834 (2018).
Gultekin, S. H. et al. Paraneoplastic limbic encephalitis: neurological symptoms, immunological findings and tumour association in 50 patients. Brain 123, 1481–1494 (2000).
Bartsch, T. & Deuschl, G. Transient global amnesia: functional anatomy and clinical implications. Lancet Neurol. 9, 205–214 (2010).
Barash, J. A. et al. Acute amnestic syndrome associated with fentanyl overdose. New Engl. J. Med. 378, 1157–1158 (2018).
Fisher, D. B. et al. Network-targeted non-invasive brain stimulation with multifocal tdcs. Brain Stimul. Basic, Transl., Clin. Res. Neuromodulation 10, 411–412 (2017).
Holmes, A. J. et al. Brain Genomics Superstruct Project initial data release with structural, functional, and behavioral measures. Sci. Data 2, 150031 (2015).
Fox, M. D., Zhang, D., Snyder, A. Z. & Raichle, M. E. The global signal and observed anticorrelated resting state brain networks. J. Neurophysiol. 101, 3270–3283 (2009).
Horn, A. et al. Connectivity Predicts deep brain stimulation outcome in Parkinson disease. Ann. Neurol. 82, 67–78 (2017).
Wu, O. et al. Role of acute lesion topography in initial ischemic stroke severity and long-term functional outcomes. Stroke 46, 2438–2444 (2015).
Iglesias, J. E. et al. A computational atlas of the hippocampal formation using ex vivo, ultra-high resolution MRI: application to adaptive segmentation of in vivo MRI. Neuroimage 115, 117–137 (2015).
Grafman, J., Salazar, A. M., Weingartner, H., & Amin, D. Face memory and discrimination: An analysis of the persistent effects of penetrating brain wounds. Int. J. Neurosci. 29, 125–139 (1986).
Albert, M.S., Butters, N. and Levin, J. Temporal gradients in the retrograde amnesia of patients with alcoholic Korsakoff's disease. Arch Neurol. 36, 211–216 (1979).
Benoit, R. G. & Schacter, D. L. Specifying the core network supporting episodic simulation and episodic memory by activation likelihood estimation. Neuropsychologia 75, 450–457 (2015).
Rottschy, C. et al. Modelling neural correlates of working memory: a coordinate-based meta-analysis. Neuroimage 60, 830–846 (2012).
Ferstl, E. C., Neumann, J., Bogler, C. & Von Cramon, D. Y. The extended language network: a meta‐analysis of neuroimaging studies on text comprehension. Hum. brain Mapp. 29, 581–593 (2008).
Schroeter, M. L., Raczka, K., Neumann, J. & Von Cramon, D. Y. Neural networks in frontotemporal dementia—a meta-analysis. Neurobiol. Aging 29, 418–426 (2008).
Bisenius, S., Neumann, J. & Schroeter, M. L. Validating new diagnostic imaging criteria for primary progressive aphasia via anatomical likelihood estimation meta‐analyses. Eur. J. Neurol. 23, 704–712 (2016).
Author information
Authors and Affiliations
Contributions
M.A.F. conceptualized and developed methods, performed analyses, created figures and tables, and was the primary author of manuscript drafts and revisions. C.L. performed literature searches for amnesia-causing lesions, traced lesions, provided scientific expertise, authored manuscript text, and jointly supervised this work. D.C. provided technical support for lesion network derivations and analyses, and revised manuscript drafts. R.R.D. contributed data on Alzheimer Disease atrophy localization and revised manuscript drafts. Ona Wu provided control contrast lesions for analyses and revised manuscript drafts. Natalia S. Rost provided control contrast lesions for analyses and revised manuscript drafts. Maurizio Corbetta provided lesions with accompanying memory behavior and demographic data, contributed scientific expertise, and revised manuscript drafts. J.G. provided lesions with accompanying memory behavior and demographic data, contributed scientific expertise, and revised manuscript drafts. M.D.F. conceptualized and developed methods, mentored lesion network analyses, coordinated data sharing and use, authored manuscript text, revised manuscript drafts, and supervised this work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Peer review information: Nature Communications thanks the anonymous reviewer(s) for their contribution to the peer review of this work.
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ferguson, M.A., Lim, C., Cooke, D. et al. A human memory circuit derived from brain lesions causing amnesia. Nat Commun 10, 3497 (2019). https://doi.org/10.1038/s41467-019-11353-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-019-11353-z
This article is cited by
-
Multimodal neuroimaging to characterize symptom-specific networks in movement disorders
npj Parkinson's Disease (2024)
-
Cognitive effects of focal neuromodulation in neurological and psychiatric disorders
Nature Reviews Psychology (2024)
-
A transdiagnostic network for psychiatric illness derived from atrophy and lesions
Nature Human Behaviour (2023)
-
Heterogeneous neuroimaging findings across substance use disorders localize to a common brain network
Nature Mental Health (2023)
-
A tripartite view of the posterior cingulate cortex
Nature Reviews Neuroscience (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.