Abstract
Lung cancer has several genetic associations identified within the major histocompatibility complex (MHC); although the basis for these associations remains elusive. Here, we analyze MHC genetic variation among 26,044 lung cancer patients and 20,836 controls densely genotyped across the MHC, using the Illumina Illumina OncoArray or Illumina 660W SNP microarray. We impute sequence variation in classical HLA genes, fine-map MHC associations for lung cancer risk with major histologies and compare results between ethnicities. Independent and novel associations within HLA genes are identified in Europeans including amino acids in the HLA-B*0801 peptide binding groove and an independent HLA-DQB1*06 loci group. In Asians, associations are driven by two independent HLA allele sets that both increase risk in HLA-DQB1*0401 and HLA-DRB1*0701; the latter better represented by the amino acid Ala-104. These results implicate several HLA–tumor peptide interactions as the major MHC factor modulating lung cancer susceptibility.
Similar content being viewed by others
Introduction
Large scale genome wide association studies (GWAS) of lung cancer revealed different susceptibility loci across the main histological subtypes: adenocarcinoma (AD), squamous cell carcinoma (SCC), and small cell lung cancer (SCLC)1,2. This heterogeneity is particularly apparent for the Major Histocompatibility Complex (MHC), where associations have been observed specifically for SCC at 6p21.33 (rs3117582) in Europeans3,4, and for AC at 6p21.32 (rs2395185) in Asians5.
However, interpreting MHC associations is difficult as it is the most gene-dense region of the genome, is highly polymorphic, displays extensive linkage disequilibrium (LD), and genes are clustered by related functions6. In addition, this extreme variation is known to be shaped by population history and different infectious exposures7,8. Imputation of classical Human Leukocyte Antigen (HLA) at a four-digit resolution based on high-density SNP genotyping is an accurate and fast alternative to traditional HLA genotyping and permits the screening of large sample sets of different ethnicities9,10.
Understanding the role of HLA in lung cancer is important, as it may help to elucidate the causal aetiology beyond the predominant role of smoking. Class I and II HLA molecules are known critical mediators in disease defense through presenting intra- or extra-cellular peptides on the cell surface in a form that can be recognized by the T cell receptors (TCR) and to then activate a specific T cell response11. To avoid immune-mediated elimination, cancer cells may lose their antigenicity due to different possibilities12. One is the immune selection of cancer cells which lack or mutate immunogenic tumor antigens13. Therefore, certain MHC alleles and polymorphisms may target particular tumor antigens, resulting in the observed disease-specific associations. A recent example is the association between an extended HLA haplotype (HLA-DRB1*1301–HLA-DQA1*0103–HLA-DQB1*0603) and protection against HPV associated oropharynx cancer14, as well as cervical cancer15. These insights have the potential to inform tumor-specific immune responses and thus to be useful in developing immunotherapies. Tumor antigens can be derived from viral proteins, proteins encoded by cancer-germline genes, differentiation antigens and proteins arising from somatic mutations or gene rearrangements16. Identifying polymorphisms controlling expression of specific HLA molecules, affecting the peptide binding groove or the contact surface with the TCR may help to disentangle lung cancer MHC associations but also may provide new insights into cancer risk and possible immunotherapy targets12.
To this end, we analyze genetic variation in two populations of European and Asian ancestry densely genotyped across the MHC in relation to lung cancer risk. Our results suggest that the genetic risk of the MHC region on lung cancer is different by population and by histology which points to different exposures or mechanisms interacting with HLA.
Results
Imputation of the HLA region
After completion of imputation for the European and Asian series (18,924 cases/15,439 controls and 2324 cases/1656 controls, respectively) (Table 1), the final set of imputed variants used in association analysis were of high quality for Europeans, 92.5% of the variants had R2 ≥ 0.9, and 67.8% of the less common variants (MAF < 0.05) had R2 ≥ 0.9, but overall quality was less apparent for Asians as 60.5% of the total variants and 30.7% of the rare variants (MAF < 0.05) had R2 ≥ 0.9 for Asians. However common variants were well imputed (75% of the common variants and 98% of common HLA alleles (MAF > 0.05) had R2 ≥ 0.9). Given our sample size in Asians, our primary focus was on common variants for which the current imputation is satisfactory.
We also performed a laboratory validation of the variants identified by imputation using another genotyping platform, Affymetrix Axiom exome array17, in a subset of 5742 individuals from the European series. A separate laboratory validation was not available for the Asian populations although we did replicate our results among never smokers in an independent series and we validated imputed HLA alleles using a completely different imputation algorithm and reference panel. Statistical re-imputation was done in a random 10% subset of the samples (3000 European samples and 1000 Asian samples from Oncoarray) using HIBAG18. The average concordance between imputed genotypes and their validation results either from an alternative genotyping platform or re-imputation was >95% for all variants (Supplementary Table 10 and 11).
The best-guess genotype dosages (R2 ≥ 0.7) for two- and four-digit classical alleles, as well as amino acid polymorphisms and SNPs in the MHC region were tested for association with overall lung cancer and subtypes in European (Fig. 1 and Table 2) and Asian ancestries (Fig. 2 and Table 3).
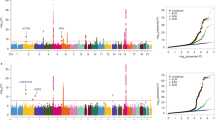
European regional association plots of variants in the MHC region and lung cancer overall and major histologies (a–d); plots of stepwise conditional analyses for squamous cell carcinoma (d.1–d.3). Each panel on the left shows the association plot for each unconditioned analysis a lung cancer overall, b adenocarcinoma, c small cell, d squamous cell carcinoma. The association for each locus used for conditioning is shown in green in each panel (d.1) unconditioned, (d.2) conditioned on HLA-B*0801, (d.3) conditioned on HLA-B*0801 and HLA-DQB1*06. Detailed association results in Table 2 and Supplementary Fig. 1. Circles represent –log10 (P values) for each binary marker using the imputed allelic dosage (between 0 and 2). The dashed black horizontal lines represent the study-wide significant threshold of P = 6 × 10−6. The physical positions of HLA genes on chromosome 6 are shown at the bottom. The color of the circles indicates the type of marker; light blue—SNPs outside HLA genes, green—classical HLA alleles and red—amino acid polymorphisms of the HLA genes; deep blue—SNP within HLA genes)
Asian regional association plots of variants in the MHC region and lung cancer overall and major histologies (a–c); plots of stepwise conditional analyses for lung adenocarcinoma (b. 1–b. 4). Each panel on the left shows the association plot for each analysis a lung cancer overall, b adenocarcinoma, c squamous cell carcinoma. The association for each locus used for conditioning is shown in green in each panel on the right (b. 1) unconditioned, (b. 2) conditioned on HLA-DQB1*0401, (b. 3) conditioned on HLA-DQB1*0401 and HLA-DRB1*0701, (b. 4) conditioned on HLA-DQB1*0401, HLA-DRB1*0701 and rs2256919 (SNP within HLA-A). Detailed association results in Table 3 and Supplementary Figure 1. Circles represent –log10 (P values) for each binary marker using the imputed allelic dosage (between 0 and 2). The dashed black horizontal lines represent the study-wide significant threshold of P = 6 × 10−6. The physical positions of HLA genes on chromosome 6 are shown at the bottom. The color of the circles indicates the type of marker; light blue—SNPs, green—classical HLA alleles, and red—amino acid polymorphisms of the HLA genes
HLA region association analyses
Multiple association signals were detected in Europeans within class I and class II regions for lung cancer overall (Fig. 1a). Stratified analyses showed that these associations were restricted to SCC (Fig. 1d) with little evidence of associations for AD (Fig. 1b) and SCLC (Fig. 1c). In contrast, MHC associations in Asians were less abundant in the overall analyses (Fig. 2a), and after stratifying by major histologies we observed the top association signals for lung AD (Fig. 2b). Therefore, subsequent explanations for Europeans and Asians will refer to SCC and AD results, respectively.
In Europeans, the most significant allele was the GT allele of a multiple nucleotide variation at Chr6: 31431982–31431983 (NCBI build 36), a complex variant affecting the first and second nucleotides of HLA-B codon 163 (OR = 1.20, p = 1.30 × 10−11; Fig. 1d. 1). This allele codes for Thr-163 or Glu-163 in HLA-B. Thus, the strongest MHC signal mapped to an amino acid change resulting in a Thr-163 in HLA-B, which is part of the sequence of the four-digit allele HLA-B *0801 that showed an equivalent association (Table 2).
Other signals including HLA alleles were also detected across the MHC (Table 2; Fig. 1d. 1). A stepwise conditional logistic regression analysis was performed to identify variants that independently influence lung SCC susceptibility in Europeans. First, conditioning on HLA-B *0801, HLA-DQB1 *06 remained as the highest peak (OR = 0.85, p = 3.05 × 10−8; Fig. 1d. 2), while other variants were not significant. In a second step, we included both HLA-B *0801 and HLA-DQB1*06 as covariates in the analysis and did not detect any remaining independent signals (Fig. 1d. 3). In Asians from Oncoarray, we also observed several associations along class I and class II (Fig. 2b. 1). The A allele of rs3129860 located in an intergenic region within HLA class II was the top associated marker. As this SNP was highly correlated with HLA-DQB1*0401 (r2 = 0.75) and apparently not showing a potential regulatory function, we used this allele in subsequent steps. After conditioning on classical HLA-DQB1*0401 allele, HLA-DRB1*0701 remained as the most significant signal (Fig. 2b. 2). When we controlled for both alleles, rs2256919 (an HLA-A intronic variant) remained associated (Figure 2b. 3). Finally, after controlling for HLA-DQB1*0401, HLA-DRB1*0701 and rs2256919 no additional variants remained associated with AD risk with a significance threshold (conditioned P > 6 × 10−6; Figure 2b. 4).
Results of the stratified analyses by histology and by smoking status for each of the independent variants found in Europeans and Asians are summarized in Supplementary Fig. 1. We observed no significant differences by smoking status for any of the analyzed variants. However, AH8.1 showed a risk effect in the overall analysis as well as in the smoking groups, but a protective effect (OR = 0.88) in the never-smoking group which involved a significant heterogeneity (phet = 0.006, Supplementary Fig. 1a). We wanted to explore further the impact of this effect in the overall analysis by adding smoking as a covariate for AH8.1 and related markers, but also for the rest of associations in both ethnithities. As can be seen in Supplementary Tables 8 and 9, results are extremely similar to the original results in Tables 2 and 3, indicating that adjustment by smoking makes little difference, as expected. In consequence, we can consider all the associated markers practically independent on smoking status.
No significant result or trend was detected for the European associated variants when we checked their association in Asians or vice versa. A possible reason for certain alleles highlighted in our analysis might be their different frequencies and meaning in European and Asian populations (Tables 2 and 3; Supplementary Tables 2 and 3). For example, European hits like class I alleles and DQB1*06 are very rare in Asians (<2%) (Supplementary Table 2) but common in Europeans (>10%) (Table 2). However, other alleles showed similar frequencies (>10%) in both populations even they were associated just in one. Statistical power calculations (Supplementary Tables 12 and 13) showed that the Asian set sample size was insufficient for detecting some European hits but not the opposite. This suggests ethnic-specific effects due to population history although we cannot discard the same effects in squamous cell carcinoma in both populations. However, it seems that HLA is not playing a role in adenocarcinoma in Europeans, unless the effects are hidden in very rare variants
Haplotype analysis
Because of the broad LD of the region, we wanted to assess the physical genetic boundaries of these associations on the basis of haplotype patterns. Supplementary Figs. 2 and 3 include an overview of the haplotypes detected in cases and controls of European and Asian ancestry, respectively. In Europeans, the most frequent haplotype and the only one associated with any of the tested outcomes was the ancestral haplotype 8.1 (AH8.1) (~6 %). AH8.1 contains class I and class II HLA alleles (A*0101 - B*0801 - C*0701 - DRB1*0301 - DQB1*0201 - DQA1*0501) and showed increased risk for SCC in Europeans (Table 2; Supplementary Fig. 1a; Supplementary Fig. 2). Conditional analyses considering AH8.1 and HLA-DQB1 *06 in the same model, revealed the independence of both effects (Table 2). However, no significant differences were detected in haplotype frequencies for any of the outcomes for Asians.
Analysis of polymorphic amino acid positions and best model selection
Although we identified a HLA haplotype and a 2-digit allele group independently associated with SCC in Europeans we aimed to answer the more refined question as to whether the association within the MHC resides with HLA alleles only, amino acids only, or a combination of both HLA alleles and amino acids. To answer this, we searched for the best combination of amino acids and/or HLA alleles that explained the HLA haplotype independently on the 2-digit allele group associated with SCC. Our model selection criterion was the Bayesian Information Criterion (BIC) since this has a heavy penalty for variable inclusion. However, the results did not differ from those obtained with the Akaike Information Criterion (AIC), a model-choice that uses a weaker penalty (when sample sizes are large) than does the BIC for the inclusion of variables.
As starting point, we ran an unconditional logistic regression (see Materials and methods) for each of the amino acids of the HLA genes and then searched for the best model from individual HLA allele or amino acid using the BIC criterion. We observed the most significant associations at HLA-B, HLA-DRB1 and HLA-DQB1 genes in Europeans.
HLA-B and HLA-DRB1 amino acids effects at Asp-9 (tagging HLA-B*0801), Thr-163 and Asp-156 in B and Lys-71, Arg-74 and Tyr-26 in DRB1 are located in protein binding grooves and part of the AH8.1 HLA alleles, which adds functional relevance to our data (Table 2, Fig. 3, Supplementary Table 4). Thr-163 and Arg-74 individual models were the ones that best explained the data in HLA-B and HLA-DRB1, respectively, as they presented the lowest BIC value.
Three-dimensional ribbon models for the HLA-B (a) and HLA-DR (b) proteins. These structures are based on Protein Data Bank entries 2bvp and 3pdo, respectively, with a direct view of the peptide-binding groove. Key amino acid positions identified by unconditioned association analyses (squamous cell carcinoma of European ancestry) are highlighted. This figure was prepared using UCSF Chimera (see URL)
Amino acids associated in HLA-DQB1 were shared exclusively by HLA-DQB1*06 molecules, i.e., not present in any other allele in HLA-DQB1 detected in the analyzed samples. As these were not located in protein binding grooves or any potential regulatory function and both two-digit allele and amino acid individual models showed similar support, we used HLA-DQB1*06 in subsequent analysis (Supplementary Table 4).
The following variables were consistently included in the combined models: B-Asp-9, B-Thr-163, B-Asp-156, HLA-B*0801, DRB1-Lys-71, DRB1-Arg-74 and DRB1-Tyr-26, HLA-DRB1*0301 and HLA-DQB1*06. Table 4 displays the combined models with the best fit to the data from this search using a stepwise conditional logistic regression approach. There is some uncertainty as to the best model that relates to whether we find evidence of a three signal model at B-Thr-163, DRB1-Arg-74 and HLA-DQB1*06 (model B), or just two signals at B-Thr-163 and HLA-DQB1*06 (model C). However, DRB1-Arg-74 does not seem to be an independent effect on B-Thr-163 since the effect was not significant and weaker within model B (OR = 1.11; p = 8.87 × 10−3), whereas the effect was stronger and significant in model D (OR = 1.19; p = 13 × 10−7) and in the individual model (OR = 1.25; p = 13 × 10−8). Accordingly, model C was considered the best model fitting the data. This implies that the amino acid Thr-163 in HLA-B*0801 is sufficient to explain the risk in the AH8.1 haplotype for lung SCC in Europeans (Table 2; Table 4; Supplementary Table 4; Fig. 3a).
In Asians, the most relevant amino acid positions for AD risk were Ala-104 and Glu-98 (in tight LD, r2 = 1) in HLA-DRB1 and Leu-23 in HLA-DQB1 (Supplementary Table 5); their individual models fitted the data as well as HLA-DRB1*0701 and HLA-DQB1*0401 alleles (Supplementary Table 5). However, when the amino acids were included instead of alleles the model had no support (Supplementary Table 6). In addition, these amino acids were not located in the binding groove of the corresponding molecules, thus a priori there is no functional relevance behind or motivation for considering these amino acid positions over the alleles as the best variants to explain the data.
Asian replication and meta-analyses
In order to give more reliability to Asian results we included an additional set of 8,537 samples obtained from published GWAs5. This is a multicenter collection of non-smoking women that serves as a replication collection as far as none of the hits were dependent on smoking status or gender in the discovery phase (Supplementary Fig. 1, Supplementary Tables 8 and 9). Therefore, we considered it reasonable to meta-analyze both Asian datasets and then extend our comparison between ethnicities.
In Asians from Lan et al., we did not observed any associations in the overall analysis (Supplementary Fig. 4a). As in the first phase, after stratifying by major histologies we observed the top association signals for lung AD (Supplementary Fig. 4b) and none for SCC (Supplementary Fig. 4c).The T allele of rs2856688 located in an intergenic region within HLA class II was the top associated marker. As this SNP was highly correlated with an amino acid change resulting in a Ala-104 in HLA-DRB1*0701 and HLA-DRB1*0401 (r2 = 0.95), we used this amino acid in subsequent steps. After conditioning on classical HLA-DQB1 Ala-104 no additional variants remained associated with AD risk with a significance threshold (conditioned P > 6 × 10−6; Supplementary Figure 4b. 2).
To gain insights into modest signals of association, we combined the imputed results of the Asian Oncoarray and Lan et al. using a random-effect meta-analysis approach. Results from top Asian associated variants are displayed in Table 5. There is a modest yet significant heterogeneity between the studies, with results from Oncoarray present stronger effects, even for the variant originally reported in Lan et al. (Ala104/Ser104 can be consider a surrogate (r2 = 0.99) of this variant, rs2395185). The two main HLA effects detected in Asian Oncoarray analysis, in HLA-DQB1 and HLA DRB1, exceed the threshold of significant in the combined analysis showing a consistence with the results of the first phase. The HLA-A intronic SNP rs2256919 was not however replicated.
Discussion
We have performed a comprehensive association analysis of HLA alleles, SNPs and polymorphic amino acid sites that identified several independent effects and their most likely causal variants that lead to the association of the MHC with lung cancer in Europeans and in Asians. In addition, our results suggest that the genetic risk of the MHC region on lung cancer is different between Asian and European populations.
Regarding the European data, the key findings are the AH8.1 haplotype association with SCC and a second independent signal involving several HLA-DQB1*06 alleles. The main signal driving the AH8.1 effect mapped to the HLA-B*0801 amino acid position 163 located in the protein binding groove.
In relation with previous findings, our analyses refined the association within BAG6/BAT3 susceptibility region encompassing rs3117582. This variant is in high LD (r2 = 0.76) with HLAB*0801, therefore within AH8.1, and was reported as associated with SCC in the largest lung cancer GWAs published to date3,4. It was not certain whether these genes themselves or others in linkage disequilibrium (LD) were primarily responsible for these findings. Here, we demonstrate that the presence of a threonine in the amino acid position 163 of HLA-B*0801 accounts for the main part of this effect as it fitted the data in the conditional model and it has biological significance. However, alleles within AH8.1 are in strong (but incomplete) LD19. For that reason we can’t exclude additional loci within the haplotype supporting or contributing additively to risk as probably is happening with the amino acid position 74 in HLA-DRB1*0301, also located in the protein binding groove.
AH8.1 is a well-known Caucasian haplotype commonly associated with immune-mediated diseases19,20,21. Typically defined by A*0101 - B*0801 - C*0701 - DRB1*0301 - DQB1*0201 - DQA1*0501, it is the second longest haplotype identified within the human genome. As it is common and stable in Caucasians, it might have been advantageous in past environments, resistant to recombination and positively selected over the time19. Similar genetic associations reported for several autoimmune diseases suggest common mechanisms of immune dysregulation21,22. The amino acid position 163 in HLA-B is a functionally important residue for TCR recognition and is also associated with TCR expression23. Future functional analyses are needed to confirm the impact of our findings.
The HLA-DQB1*06 allele group showed a protective effect independent of AH8.1. This association is based in two amino acid positions (125 and 87) common to DQB1*06 4-digit alleles (HLA-DQB1*0601, HLA-DQB1*0602, HLA-DQB1*0603, HLA-DQB1*0604 and HLA-DQB1*0609) but not present in any other DQB1 alleles detected here. It is possible that one of them is driving the effect and the other is just in tight LD (R2 = 0.78). Alternatively, there may be a joint effect involving both amino acids, driven by combined selection. This is plausible given the important role of natural selection in the MHC22,24, even if these are not in a clear functional physical location. The allele showing the strongest association trend within DQB1*06 group is HLA-DQB1*0603, part of the HLA class II haplotype HLA-DRB1*1301–HLA-DQA1*0103–HLA-DQB1*0603 (in tight LD in Europeans, r2 > 0.9) and associated with head and neck14 and cervical cancer15, both squamous cell carcinomas linked to HPV infection. For lung SCC this haplotype showed a trend of association with the same protective effect as in the HPV associated cancers (Supplementary Table 14).
In contrast, in the Asians Oncoarray analysis we only observed associations between HLA class II alleles and risk of lung adenocarcinoma. We observed two independent HLA allele effects increasing risk, HLA-DQB1*0401 and HLA-DRB1*0701, as well as a protective intronic SNP in HLA-A (rs2256919). A potential limitation of our study is the relatively modest sample size of the Asian data set, compared with the European population. However, in the replication phase, we observed two of the three independent HLA allele effects that were described in the first phase. One is represented by the four-digit allele HLA-DQB1*0401 as in the discovery, and the other is better explained by the association of Ala-104/Glu-98/Gln-10, part of HLA-DRB1*0701 and HLA-DRB1*0401 protein sequence. This is the same effect as the one described by Lan et al. in the intergenic region in 6p21.32 (rs2395185) as all, SNP and amino acids changes, are in tight LD (r2 = 0.99). We could not confirm the association of the intronic SNP in HLA-A (rs2256919).
We also observed no overlap between Asian and European hits. While we cannot rule out the possibility that some of the observed differences could be due to the lack of power in the Asian collection, it is possible that differences in the spectrum of antigens in the two populations might introduce changes in which alleles might play the important role in disease susceptibility within each population. However, prevalence of never smokers is another important difference between the Asian and European data sets. While we consider it beyond doubt that Asian HLA associations are independent on smoking, especially as we have replicated our initial findings in nonsmoking Asian women, is true that the proportion of non-smokers in Asian AD (469/1192; 39%) is higher than in European AD (1004/7088; 14%) and this could represent a problem if there is a dependency on smoking. Despite this, we did not see the association in European AD non-smokers even though the absolute number of never-smokers among European AC cases was greater than among Asians, and we had enough power to detect the effects shown in Asian AD.
In summary, this evidence suggests a different aetiological role for the MHC by population and by histology which points to different exposures or mechanisms interacting with HLA. These differences are clear for AD; however differences between ethnicities for SCC still need confirmation. Taken together, our findings enhance the role of HLA variants in the immune pathogenesis of lung cancer, and may also have implications for cancer immunotherapies targeting the HLA antigen presentation pathway16,25,26.
Methods
Sample collections and genotypes
Participants were of either European or Asian ethnicity and came from 30 case-control studies that were included in the OncoArray study, and part of the Transdisciplinary Research of Cancer in Lung of the International Lung Cancer Consortium (TRICL-ILCCO) and the Lung Cancer Cohort Consortium (LC3) (Supplementary Table 1). After quality control, the European ethnicity series included 18,924 lung cancer cases and 15,439 controls, whilst the Asians series comprised 2324 cases and 1656 controls (Table 1). Informed consent was obtained for all participants, and studies were approved by respective institutional review boards.
For all samples, we had access to genome-wide SNP data at individual level from OncoArray genotyping platform27. The Illumina OncoArray custom was designed for cancer studies by the OncoArray Consortium, part of the Genetic Associations and Mechanisms in Oncology (GAME-ON) Network that includes fine-mapping of common cancer susceptibility loci with special emphasis on HLA region among others. Oncoarray genotyping and genotype quality controls procedure were done in the context of a large lung cancer genome-wide study using the OncoArray platform4. Briefly, genotype calls and quality control filters were made by the Dartmouth team in GenomeStudio software (Illumina) using a standardized cluster file for OncoArray. Standard quality control procedures were used to exclude underperforming genotyping assays (judged by success rate, genotype distributions deviated from that expected by Hardy Weinberg equilibrium). Additionally, individuals with low genotyping success rate (<95%) and individuals with a genetically inferred gender by X and Y markers did not match that reported gender, or had excess identity by descent sharing relative to other samples, were excluded. Principal components analysis (PCA) was done using FlashPCA3 and identified 10 and 3 significant eigenvectors on the European and the Asian dataset, respectively, that were used as covariates in the association analyses. PCA plots are displayed in Supplementary Fig. 5. Furthermore, generalized linear models showed that of the eigenvectors were significantly associated with the study of recruitment either in Asian or in European series (p-value: < 10−16). Therefore, we have used eigenvectors in lieu of study to better adjust for genetic/ethnic origin.
An additional Asian series including 4962 lung cancer cases and 3845 controls was downloaded from DbGaP5 (dbGaP reference: phs000716.v1.p1) and was used as a replication collection of the initial Asian results. Genome-wide data came from two sources in this study but we only used genotypes from the Illumina 660W SNP microarray as this was the source of the majority of the samples and of the same Asian origin. On top of the quality controls done5, 270 duplicated samples were excluded. To account for potential population stratification, we performed PCA in EIGENSTRAT28 using approximately 10,000 common markers in low LD (r2 < 0.004, minor allele frequency (MAF) > 0.05). Subsequently, we derived the 7 significant eigenvectors to adjust association analyses. PCA plots are displayed in Supplementary Fig. 5. Supplementary Table 7 shows demographic characteristics of the final replication set 4,741 lung cancer cases and 3,796 controls, after quality controls.
Imputation of the HLA system
Taking advantage of the high OncoArray SNP coverage in the HLA region, we used the genotyping data from 25 to 35 Kb at chromosome 6 (NCBI build 37) obtained to impute classical two and four digit HLA alleles and amino acid polymorphisms of the HLA genes along with the SNPs that were not directly genotyped.
For Europeans, we imputed HLA variants using the reference data collected by the Type 1 Diabetes Genetics Consortium (T1DGC)6,29. This is a panel composed of 5,225 individuals of European origin with genotyping data for 8,534 SNPs and 424 classical HLA alleles of class I (HLA-A, HLA-B and HLA-C) and class II (HLA-DRB1, HLA-DQB1, HLA-DQA1, HLA-DPB1 and HLA-DPA1) genes. For Asians, we used the Pan-Asian reference panel30,31 which contains genotype data for 8,245 SNPs and 273 classical HLA alleles tagging the entire MHC, as described above, in 530 unrelated individuals of Asian descent.
Imputation process was performed with the SNP2HLA v1.0.3 package using Beagle software32,33 (http://www.broadinstitute.org/mpg/snp2hla). It was conducted separately for each ethnic group and we imputed cases and controls together in randomized groups of approximately 1000 individuals. We applied post-imputation QC criteria of R2 < 0.3 for excluding variants in the association analysis.
Imputation validation
To confirm imputed HLA alleles, we re-imputed34 a random 10% subset of the samples (3000 European samples and 1000 Asian samples from Oncoarray) using HIBAG18,which employs another pre-trained referenced panel and a different statistical method based on multiple expectation-maximization-based classifiers to estimate the likelihood of HLA alleles (http://www.biostat.washington.edu/~bsweir/HIBAG/). Previous studies comparing the accuracy of HIBAG and SNP2HLA (among others imputation methods) to sequence data, concluded that they are the most robust programs with respect to maintaining accuracy35,36. In order to assess the accuracy of the imputation, we compared the imputed data for HLA alleles of class I (HLA-A, HLA-B and HLA-C) and class II (HLA-DRB1, HLA-DQB1, HLA-DQA1), of those HLA genotypes obtained in the same individuals with the two methods described above. Two parameters were considered for this comparison 1) a correlation coefficient (r), which is a measure of the reliability of the frequencies, and 2) the accuracy, to establish reproducibility of the typing in each individual, as described elsewhere37.
We also performed a laboratory validation genotyping to confirm array imputed dosages of the associated variants using another genotyping platform Affymetrix Axiom exome array17 in a subset of 5,742 individuals from the European series. We considered the associated variants that achieved the study significance in Europeans. For these loci, the sentinel variant (or correlated proxy variant) was also genotyped on the custom Affymetrix Axiom exome array. We therefore considered the concordance between the OncoArray genotypes and the Affymetric array for these variants in the 5,742 individuals where genotyping was available for both platforms. Supplementary Table 11 describes the satisfactory concordance between OncoArray (imputation) genotypes and the validation genotypes.
Analysis across the MHC region
All the tested HLA variants were defined as binary markers as follow: for biallelic SNPs, classical HLA alleles and binary amino acid positions, the effect allele or variant was the minor allele, the presence of the HLA allele or the presence of the less frequent amino acid. For multi-allelic amino acid positions we defined composite markers where each possible individual allele and combination of alleles was tested for association.
To test for association within the HLA region and given the ancestral variation of our study, we evaluated associations separately for each ethnicity (European and Asian). For each marker we used dosages, which take uncertainty in imputation into account, in multivariate unconditional logistic regression models under a log-additive genetic model controlling for sex and principal components (as was described above). We assessed the association between the described variants and lung cancer risk, as well as predominant histological types and smoking behaviour. We set a study-wide significance threshold of P = 6 × 10−6, on the basis of the highest total number of genotyped SNPs, as well as imputed SNPs, HLA alleles and amino acid variants that were included in the analyses after passing QC for Europeans (0.05/8,291) and Asians (0.05/5,504). The number of markers that passed QC in the Asian series is less but we maintained in the Asian analysis the more conservative p-value cut-off adopted for Europeans. This correction far exceed number of independent test expected within this region given its high linkage disequilibrium, and it can be considered a very conservative p-value.
To assess whether there were independent effects outside of the main associated loci, we used a conditional additive logistic regression approach to test all markers across the MHC. In order to explore whether any of the significant variant identified in this process have any potential regulatory function if they are not in a critical location, we used the online tool HaploReg v4.138 to confirm location of each SNP in relation to annotated protein-coding genes and/or non-coding regulatory elements. As a first step, we included HLA alleles as covariates when they or their tag-SNPs (not annotated as functional) appeared as the best associated markers. If we identified other independently associated markers, we included them also as covariates in subsequent conditional analyses. All statistical analyses were performed in R version 3.2.3 (https://www.r-project.org/).
To help the interpretation of the results and the comparison between ethnicities, supplementary tables 12 and 13 display statistical power calculations for both populations but also imputation probabilities for the associated variants.
Meta-analysis of Asian datasets
We combined the results of Asian Oncoarray and Lan et al. studies using GWAMA (Genome-Wide Association Meta-Analysis)39 software to perform random-effect meta-analyses. The software incorporates error trapping, which facilities to identify strand alignment errors and allele flipping, and performs tests of heterogeneity of effects between studies.
Haplotype inference, visualization and association analyses
The results of HLA alleles and SNPs might not translate directly to a single locus as a result of the extended linkage disequilibrium (LD) known to exist in the MHC; it is possible that markers that seem to be acting independently with respect to genotype risk could be on a shared haplotype (http://www.ebi.ac.uk/ipd/imgt/hla/). We search for significant combination of HLA alleles using Haplo.stats package v.1.7.7 (https://cran.r-project.org/web/packages/haplo.stats/index.html) implemented in R software to generate population-based haplotypes from phased genotypes obtained from the imputed data. Haplo.stats uses the expectation-maximization algorithm and progressively inserts batches of loci into haplotypes. We inferred haplotypes frequencies within class I alleles, class II and along the MHC (class I and class II) for Asians and Europeans. Then, using the statistical framework and covariates defined above, we individually tested each of the haplotypes for association with lung cancer overall and in the subgroups described.
HLA linkage disequilibrium (LD) maps were obtained using Disentangler (http://kumasakanatsuhiko.jp/projects/disentangler/), a graphical tool suitable for visualization of haplotype configurations across multiallelic genetic markers for which typical triangular heat maps with LD indices will not work. Disentangler also applies expectation-maximization algorithms to estimate the haplotype frequencies between adjacent markers, and it uses then this information to determine the order of the alleles for each marker and the number of crossing lines between adjacent markers40,41. We created separate population-specific maps for cases and controls, using the whole collection for Asians and a randomized set of 5,000 cases and 5,000 controls for Europeans.
Unravelling candidate functional variants
Using the independently associated HLA alleles and/or haplotypes, their significant amino acids and SNPs, we searched for the best overall HLA model. First, we used a forward selection stepwise regression of significant amino acids within the independently associated regions. For each gene or region we looked for the set of significant amino acid positions and we defined the classical alleles with consistent residues at those positions. We also included as covariates in these risk models the independent markers previously identified. The aim was to find the best set of amino acids and/or HLA alleles that were independently associated with lung cancer as judged by the lowest AIC (Akaike Information Criterion) and BIC (Bayesian Information Criterion)42,43.
Ribbon representations of the associated HLA molecules were constructed with the UCSF Chimera software44 to locate significant amino acids in the tri-dimensional structure of the protein (http://www.cgl.ucsf.edu/chimera/). We also used the online tool HaploReg v4.138 to confirm location of each SNP in relation to annotated protein-coding genes and non-coding regulatory elements (http://archive.broadinstitute.org/mammals/haploreg/haploreg.php).
Data availability
Genotype data for the lung cancer OncoArray study have been deposited at the database of Genotypes and Phenotypes (dbGaP) under accession phs001273.v1.p1. The Asian replication dataset was downloaded from dbGaP under accession phs000716.v1.p1.
References
Sun, S., Schiller, J. H. & Gazdar, A. F. Lung cancer in never smokers—a different disease. Nat. Rev. Cancer 7, 778–790 (2007).
Brennan, P., Hainaut, P. & Boffetta, P. Genetics of lung-cancer susceptibility. Lancet Oncol. 12, 399–408 (2011).
Timofeeva, M. N. et al. Influence of common genetic variation on lung cancer risk: meta-analysis of 14900 cases and 29485 controls. Hum. Mol. Genet 21, 4980–4995 (2012).
McKay, J. D. et al. Large-scale association analysis identifies new lung cancer susceptibility loci and heterogeneity in genetic susceptibility across histological subtypes. Nat. Genet. 49, 1126–1132 (2017).
Lan, Q. et al. Genome-wide association analysis identifies new lung cancer susceptibility loci in never-smoking women in Asia. Nat. Genet. 44, 1330–1335 (2012).
de Bakker, P. I. W. et al. A high-resolution HLA and SNP haplotype map for disease association studies in the extended human MHC. Nat. Genet. 38, 1166–1172 (2006).
Sanchez-Mazas, A., Buhler, S. & Nunes, J. M. A new HLA map of Europe: regional genetic variation and its implication for peopling history, disease-association studies and tissue transplantation. Hum. Hered. 76, 162–177 (2013).
Buhler, S. & Sanchez-Mazas, A. HLA DNA sequence variation among human populations: molecular signatures of demographic and selective events. PLoS ONE 6, e14643 (2011).
Leslie, S., Donnelly, P. & McVean, G. A statistical method for predicting classical HLA alleles from SNP data. Am. J. Hum. Genet. 82, 48–56 (2008).
de Bakker, P. I. W. & Raychaudhuri, S. Interrogating the major histocompatibility complex with high-throughput genomics. Hum. Mol. Genet. 21, R29–R36 (2012).
Neefjes, J., Jongsma, M. L. M., Paul, P. & Bakke, O. Towards a systems understanding of MHC class I and MHC class II antigen presentation. Nat. Rev. Immunol. 11, 823 (2011).
Beatty, G. L. & Gladney, W. L. Immune escape mechanisms as a guide for cancer immunotherapy. Clin. Cancer Res. 21, 687–692 (2015).
Schreiber, R. D., Old, L. J. & Smyth, M. J. Cancer immunoediting: integrating immunity’s roles in cancer suppression and promotion. Science 331, 1565–1570 (2011).
Lesseur, C. et al. Genome-wide association analyses identify new susceptibility loci for oral cavity and pharyngeal cancer. Nat. Genet. 48, 1544–1550 (2016).
Chen, D. et al. Genome-wide association study of susceptibility loci for cervical cancer. J. Natl Cancer Inst. 105, 624–633 (2013).
Coulie, P. G., Van den Eynde, B. J., van der Bruggen, P. & Boon, T. Tumour antigens recognized by T lymphocytes: at the core of cancer immunotherapy. Nat. Rev. Cancer 14, 135–146 (2014).
Kachuri, L. et al. Fine mapping of chromosome 5p15.33 based on a targeted deep sequencing and high density genotyping identifies novel lung cancer susceptibility loci. Carcinogenesis 37, 96–105 (2016).
Zheng, X. et al. HIBAG—HLA genotype imputation with attribute bagging. Pharm. J. 14, 192–200 (2014).
Price, P. et al. The genetic basis for the association of the 8.1 ancestral haplotype (A1, B8, DR3) with multiple immunopathological diseases. Immunol. Rev. 167, 257–274 (1999).
Candore, G., Lio, D., Colonna Romano, G. & Caruso, C. Pathogenesis of autoimmune diseases associated with 8.1 ancestral haplotype: effect of multiple gene interactions. Autoimmun. Rev. 1, 29–35 (2002).
Miller, F. W. et al. Genome-wide association study identifies HLA 8.1 ancestral haplotype alleles as major genetic risk factors for myositis phenotypes. Genes Immun. 16, 470–480 (2015).
Trowsdale, J. The MHC, disease and selection. Immunol. Lett. 137, 1–8 (2011).
Sharon, E. et al. Genetic variation in MHC proteins is associated with T cell receptor expression biases. Nat. Genet. 48, 995–1002 (2016).
Trowsdale, J. & Knight, J. C. Major histocompatibility complex genomics and human disease. Annu. Rev. Genom. Hum. Genet. 14, 301–323 (2013).
Thibodeau, J., Bourgeois-Daigneault, M.-C. & Lapointe, R. Targeting the MHC Class II antigen presentation pathway in cancer immunotherapy. Oncoimmunology 1, 908–916 (2012).
Comber, J. D. & Philip, R. MHC class I antigen presentation and implications for developing a new generation of therapeutic vaccines. Ther. Adv. Vaccin. 2, 77–89 (2014).
Amos, C. I. et al. The OncoArray Consortium: a network for understanding the genetic architecture of common cancers. Cancer Epidemiol. Biomark. Prev. 26, 126–135 (2017).
Price, A. L. et al. Principal components analysis corrects for stratification in genome-wide association studies. Nat. Genet. 38, 904–909 (2006).
Brown, W. M. et al. Overview of the MHC fine mapping data. Diabetes Obes. Metab. 11, 2–7 (2009).
Pillai, N. E. et al. Predicting HLA alleles from high-resolution SNP data in three Southeast Asian populations. Hum. Mol. Genet. 23, 4443–4451 (2014).
Okada, Y. et al. Risk for ACPA-positive rheumatoid arthritis is driven by shared HLA amino acid polymorphisms in Asian and European populations. Hum. Mol. Genet. 1–11 (2014). https://doi.org/10.1093/hmg/ddu387
Jia, X. et al. Imputing amino acid polymorphisms in human leukocyte antigens. PLoS ONE 8, e64683 (2013).
Browning, B. L. & Browning, S. R. A unified approach to genotype imputation and haplotype-phase inference for large data sets of trios and unrelated individuals. Am. J. Hum. Genet. 84, 210–223 (2009).
Mcmahon, G., Ring, S. M., Davey-Smith, G. & Timpson, N. J. Genome-wide association study identifies SNPs in the MHC class II loci that are associated with self-reported history of whooping cough. Hum. Mol. Genet. 24, 5930–5939 (2015).
Jeanmougin, M., Noirel, J., Coulonges, C. & Zagury, J.-F. HLA-check: evaluating HLA data from SNP information. BMC Bioinf. 18, 334 (2017).
Karnes, J. H. et al. Comparison of HLA allelic imputation programs. PLoS ONE 12, e0172444 (2017).
Raychaudhuri, S. et al. Five amino acids in three HLA proteins explain most of the association between MHC and seropositive rheumatoid arthritis. Nat. Genet. 44, 291–296 (2012).
Ward, L. D. & Kellis, M. HaploReg: a resource for exploring chromatin states, conservation, and regulatory motif alterations within sets of genetically linked variants. Nucleic Acids Res. 40, D930–D934 (2012).
Mägi, R. & Morris, A. P. GWAMA: software for genome-wide association meta-analysis. BMC Bioinf. 11, 288 (2010).
Okada, Y. et al. HLA-Cw*1202-B*5201-DRB1*1502 haplotype increases risk for ulcerative colitis but reduces risk for Crohn’s disease. Gastroenterology 141, 864–871.e5 (2011).
Okada, Y. et al. Construction of a population-specific HLA imputation reference panel and its application to Graves’ disease risk in Japanese. Nat. Genet. 47, 798–802 (2015).
Burnham, K. P., Anderson, D. R. & Burnham, K. P. Model Selection and Multimodel Inference: A Practical Information-theoretic Approach. Ch.6 (Springer, 2002).
Morris, D. L. et al. Unraveling Multiple MHC Gene Associations with systemic lupus erythematosus: model choice indicates a role for HLA alleles and non-HLA genes in Europeans. Am. J. Hum. Genet. 91, 778–793 (2012).
Pettersen, E. F. et al. UCSF Chimera? A visualization system for exploratory research and analysis. J. Comput. Chem. 25, 1605–1612 (2004).
Acknowledgements
Transdisciplinary Research for Cancer in Lung (TRICL) research team of the International Lung Cancer Consortium (ILCCO) was supported by (U19-CA148127 and CA148127S1). The ILCCO data harmonization is supported by Cancer Care Ontario Research Chair of Population Studies to R. H. and Lunenfeld-Tanenbaum Research Institute, Sinai Health System. TRICL-ILCCO Oncoarray was supported by in-kind genotyping Centre for Inherited Disease Research (26820120008i-0-26800068-1). CAPUA study was supported by FIS-FEDER/Spain grant numbers FIS-01/310, FIS-PI03-0365, and FIS-07-BI060604, FICYT/Asturias grant numbers FICYT PB02-67 and FICYT IB09-133, and the University Institute of Oncology (IUOPA), of the University of Oviedo and the Ciber de Epidemiología y Salud Pública. CIBERESP, SPAIN. The work performed in the CARET study was supported by the The National Institute of Health/National Cancer Institute: UM1 CA167462 (PI: Goodman), National Institute of Health UO1‐CA6367307 (PIs Omen, Goodman); National Institute of Health R01 CA111703 (PI Chen), National Institute of Health 5R01 CA15198901A1(PI Doherty). Norway study was supported by Norwegian Cancer Society, Norwegian Research Council The NELCS study: Grant Number P20RR018787 from the National Center for Research Resources (NCRR), a component of the National Institutes of Health (NIH). The Liverpool Lung project is supported by the Roy Castle Lung Cancer Foundation. The Harvard Lung Cancer Study was supported by the NIH (National Cancer Institute) grants CA092824, CA090578, CA074386. The Multiethnic Cohort Study was partially supported by NIH Grants CA164973, CA033619, CA63464 and CA148127. The work performed in MSH-PMH study was supported by The Canadian Cancer Society Research Institute (020214), Ontario Institute of Cancer and Cancer Care Ontario Chair Award to RJH and GL and the Alan Brown Chair and Lusi Wong Programs at the Princess Margaret Hospital Foundation. NJLCS work was funded by the State Key Program of National Natural Science of China (81230067), the National Key Basic Research Program Grant (2011CB503805), the Major Program of the National Natural Science Foundation of China (81390543). Tampa Lung Cancer Study (Tampa) was supported by National Institutes of Health: R01 DE013158, PO1 CA68384 and R01 ES025460. The Shanghai Cohort Study (SCS) was supported by National Institutes of Health R01 CA144034 (PI: Yuan) and UM1 CA182876 (PI: Yuan). The Singapore Chinese Health Study (SCHS) was supported by National Institutes of Health R01 CA144034 (PI: Yuan) and UM1 CA182876 (PI: Yuan). TCL work has been supported in part the James & Esther King Biomedical Research Program (09KN-15), National Institutes of Health Specialized Programs of Research Excellence (SPORE) Grant (P50 CA119997), and by a Cancer Center Support Grant (CCSG) at the H. Lee Moffitt Cancer Center and Research Institute, an NCI designated Comprehensive Cancer Center (grant number P30-CA76292). The Vanderbilt Lung Cancer Study – BioVU dataset used for the analyses described was obtained from Vanderbilt University Medical Center’s BioVU, which is supported by institutional funding, the 1S10RR025141-01 instrumentation award, and by the Vanderbilt CTSA grant UL1TR000445 from NCATS/NIH. Dr. Aldrich was supported by NIH/National Cancer Institute K07CA172294 (PI: Aldrich) and Dr. Bush was supported by NHGRI/NIH U01HG004798 (PI: Crawford). The L2 study. Lung cancer cases and controls were recruited through a multicentric case-control study coordinated by the International Agency for Research on Cancer in Russia, Poland, Serbia, Czech Republic, and Romania from 2005 to 2013. Cases were incident cancer patients collected from general hospitals. Controls were recruited from individuals visiting general hospitals and out-patient clinics for disorders unrelated to lung cancer and/or its associated risk factors, or from the general population. Information on lifestyle risk factors, medical and family history was collected from subjects by interview using a standard questionnaire. All study participants provided written informed consent. The current study included 1,133 lung cancer cases and 1,117 controls genotyped on the Oncoarray. The study in Lodz center was partially funded by Nofer Institute of Occupational Medicine, under task NIOM 10.13: Predictors of mortality from non-small cell lung cancer - field study.
Author information
Authors and Affiliations
Contributions
A.F.-I. contributed to data harmonization, HLA imputation, HLA quality control, formal analysis, writing original draft. C.L. contributed to data harmonization and HLA imputation. X.X., Y.L., D.C.Q., J.B., Y.H., A.K., D.Z., X.J. contributed to genotype calling and primary quality control filters. J.M., D.A., S.L., M.-S.T., A.T., A.F.-S., G.F.-T., C.C., J.D., G.G., S.E.B., M.T.L., M.J., J.K.F., M.D., H.B., H.-E.W., A.R., A.R., D.C., G.R., S.A., S.S., X.W., O.M., H.B., L.L.M., X.Z., G.L., A.A., E.D., L.A.K., E.H.F.M.H., H.S., J.D., A.H., S.Z., M.J., K.G., N.C., P.W., M.T., G.S., D.Z., A.M., M.K., S.O., J.L., M.S., B.S., V.J., I.H., C.B., M.S., M.O., Y.-C.H., J.-M.Y., P.L., M.B.S., M.C.A. contributed to data collection. R.J.H. coordinated the Lung Cancer OncoArray, is responsible for phenotype data harmonization across OncoArray studies and contributed to data collection. C.I.A. designed and coordinated the Lung Cancer OncoArray, and contributed to data collection. P.B. contributed to conceptualization, contributed to data collection, supervision, project administration, funding acquisition, and provided overall supervision and management. All authors contributed to reviewing and editing original draft.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ferreiro-Iglesias, A., Lesseur, C., McKay, J. et al. Fine mapping of MHC region in lung cancer highlights independent susceptibility loci by ethnicity. Nat Commun 9, 3927 (2018). https://doi.org/10.1038/s41467-018-05890-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-018-05890-2
This article is cited by
-
Context-aware single-cell multiomics approach identifies cell-type-specific lung cancer susceptibility genes
Nature Communications (2024)
-
HLA imputation and its application to genetic and molecular fine-mapping of the MHC region in autoimmune diseases
Seminars in Immunopathology (2022)
-
Interstitial lung abnormalities in patients with stage I non-small cell lung cancer are associated with shorter overall survival: the Boston lung cancer study
Cancer Imaging (2021)
-
A novel regQTL-SNP and the risk of lung cancer: a multi-dimensional study
Archives of Toxicology (2021)
-
The landscape of host genetic factors involved in immune response to common viral infections
Genome Medicine (2020)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.