Abstract
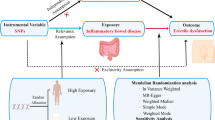
Considering that vascular endothelial cell dysfunction is the pathological basis of erectile dysfunction (ED), and recognizing the beneficial effects of 25-hydroxyvitamin D (25(OH)D) on vascular endothelial cell protection, the researchers diligently investigated the causal relationship between serum 25(OH)D levels and ED. However, inconsistent clinical evidence has left the association between serum 25(OH)D levels and ED unclear. The objective of this work was to employ Mendelian randomization (MR) analysis to ascertain the potential causal relationship between serum 25(OH)D levels and ED. We conducted a two-sample MR analysis utilizing data from publicly available genome-wide association studies (GWASs). The primary analysis method for the MR analysis was the inverse-variance weighted (IVW) method, supplemented by the MR-Egger and weighted median methods. In addition, we evaluated heterogeneity with Cochran’s Q test, assessed pleiotropy using the MR-Egger intercept test, and performed a leave-one-out analysis to identify single-nucleotide polymorphisms (SNPs) with potential effects. Outliers were detected using MR-pleiotropy residual sum and outlier (MR-PRESSO). Genetically predicted serum 25(OH)D levels were not found to be causally associated with ED in IVW method (OR = 1.028, 95% CI = 0.845–1.250, P = 0.785), MR-Egger method (OR = 1.057, 95% CI = 0.782–1.430, P = 0.720), and weighted median method (OR = 1.225, 95% CI = 0.920–1.633, P = 0.165). The results of sensitivity analyses reinforced our conclusion, indicating no evidence of heterogeneity or directional pleiotropy. In summary, our findings do not substantiate a genetic-level causal link between serum 25(OH)D levels and the prevalence of ED. Nonetheless, future research, including larger MR studies, clinical trials, and additional observational studies, is essential to validate and reinforce the outcomes of our present study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
71 SNPs included in this MR analysis were included in supplemental material Table S1.
Code availability
The reader can reasonably request the MR analysis code from the corresponding authors.
References
NIH Consensus Conference. Impotence. NIH Consensus Development Panel on Impotence. JAMA. 1993;270:83–90.
Kupelian V, Link CL, Rosen RC, McKinlay JB. Socioeconomic status, not race/ethnicity, contributes to variation in the prevalence of erectile dysfunction: results from the Boston Area Community Health (BACH) Survey. J Sex Med. 2008;5:1325–33.
Ng EM, Cheng JY. Prevalence and biopsychosocial correlates of erectile dysfunction in Hong Kong: a population-based study. Urology. 2007;70:131–6.
Chew KK, Stuckey B, Bremner A, Earle C, Jamrozik K. Male erectile dysfunction: its prevalence in Western australia and associated sociodemographic factors. J Sex Med. 2008;5:60–9.
Ayta IA, McKinlay JB, Krane RJ. The likely worldwide increase in erectile dysfunction between 1995 and 2025 and some possible policy consequences. BJU Int. 1999;84:50–6.
Papagiannopoulos D, Khare N, Nehra A. Evaluation of young men with organic erectile dysfunction. Asian J Androl. 2015;17:11–6.
Caskurlu T, Tasci AI, Resim S, Sahinkanat T, Ergenekon E. The etiology of erectile dysfunction and contributing factors in different age groups in Turkey. Int J Urol. 2004;11:525–9.
Karadeniz T, Topsakal M, Aydogmus A, Basak D. Erectile dysfunction under age 40: etiology and role of contributing factors. ScientificWorldJournal. 2004;4:171–4.
Donatucci CF, Lue TF. Erectile dysfunction in men under 40: etiology and treatment choice. Int J Impot Res. 1993;5:97–103.
Dean RC, Lue TF. Physiology of penile erection and pathophysiology of erectile dysfunction. Urol Clin North Am. 2005;32:379.
Guay AT. ED2: erectile dysfunction = endothelial dysfunction. Endocrinol Metab Clin North Am. 2007;36:453–63.
Foy CG, Newman JC, Berlowitz DR, Russell LP, Kimmel PL, Wadley VG, et al. Blood Pressure, Sexual Activity, and Erectile Function in Hypertensive Men: Baseline Findings from the Systolic Blood Pressure Intervention Trial (SPRINT). J Sex Med. 2019;16:235–47.
Batty GD, Li Q, Czernichow S, Neal B, Zoungas S, Huxley R, et al. Erectile dysfunction and later cardiovascular disease in men with type 2 diabetes: prospective cohort study based on the ADVANCE (Action in Diabetes and Vascular Disease: Preterax and Diamicron Modified-Release Controlled Evaluation) trial. J Am Coll Cardiol. 2010;56:1908–13.
Roumeguère T, Wespes E, Carpentier Y, Hoffmann P, Schulman CC. Erectile dysfunction is associated with a high prevalence of hyperlipidemia and coronary heart disease risk. Eur Urol. 2003;44:355–9.
Gades NM, Nehra A, Jacobson DJ, McGree ME, Girman CJ, Rhodes T, et al. Association between smoking and erectile dysfunction: a population-based study. Am J Epidemiol. 2005;161:346–51.
Srichomchey P, Sukprasert S, Khulasittijinda N, Voravud N, Sahakitrungruang C, Lumjiaktase P. Vitamin D3 Supplementation Promotes Regulatory T-Cells to Maintain Immune Homeostasis After Surgery for Early Stages of Colorectal Cancer. Vivo. 2023;37:286–93.
Hiremath VP, Rao CB, Naik V, Prasad KV. Anti-inflammatory effect of vitamin D on gingivitis: a dose-response randomised control trial. Oral Health Prev Dent. 2013;11:61–9.
Cojic M, Kocic R, Klisic A, Kocic G. The Effects of Vitamin D Supplementation on Metabolic and Oxidative Stress Markers in Patients With Type 2 Diabetes: A 6-Month Follow Up Randomized Controlled Study. Front Endocrinol. 2021;12:610893.
Tian Y, Lv G, Yang Y, Zhang Y, Yu R, Zhu J, et al. Effects of vitamin D on renal fibrosis in diabetic nephropathy model rats. Int J Clin Exp Pathol. 2014;7:3028–37.
Weinstein SJ, Purdue MP, Smith-Warner SA, Mondul AM, Black A, Ahn J, et al. Serum 25-hydroxyvitamin D, vitamin D binding protein and risk of colorectal cancer in the Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial. Int J Cancer. 2015;136:E654–64.
Sabico S, Wani K, Grant WB, Al-Daghri NM. Improved HDL Cholesterol through Vitamin D Status Correction Substantially Lowers 10-Year Atherosclerotic Cardiovascular Disease Risk Score in Vitamin D-Deficient Arab Adults. Nutrients. 2023;15:551.
Lim S, Kim MJ, Choi SH, Shin CS, Park KS, Jang HC, et al. Association of vitamin D deficiency with incidence of type 2 diabetes in high-risk Asian subjects. Am J Clin Nutr. 2013;97:524–30.
Hoogendijk WJ, Lips P, Dik MG, Deeg DJ, Beekman AT, Penninx BW. Depression is associated with decreased 25-hydroxyvitamin D and increased parathyroid hormone levels in older adults. Arch Gen Psychiatry. 2008;65:508–12.
Kim DH, Meza CA, Clarke H, Kim JS, Hickner RC. Vitamin D and Endothelial Function. Nutrients. 2020;12:575.
Andrukhova O, Slavic S, Zeitz U, Riesen SC, Heppelmann MS, Ambrisko TD, et al. Vitamin D is a regulator of endothelial nitric oxide synthase and arterial stiffness in mice. Mol Endocrinol. 2014;28:53–64.
Kono K, Fujii H, Nakai K, Goto S, Kitazawa R, Kitazawa S, et al. Anti-oxidative effect of vitamin D analog on incipient vascular lesion in non-obese type 2 diabetic rats. Am J Nephrol. 2013;37:167–74.
Zhou W, Yuan G, Wang Q. Vitamin D attenuates lipopolysaccharide-induced inflammatory response in endothelial cells through inhibition of PI3K/Akt/NF-κB signaling pathway. Pharmazie. 2019;74:412–7.
Wu X, Zhang Y, Zhang W, Liu G, Jiang H, Huang H, et al. The relationship between serum 25-hydroxy vitamin D and arteriogenic erectile dysfunction. Andrologia. 2022;54:e14568.
Dumbraveanu I, Banov P, Arian I, Ceban E. The Correlations of Clinical and Biochemical Indices of Vitamin D with Erectile Dysfunction. J Med Life. 2020;13:144–50.
Farag YMK, Guallar E, Zhao D, Kalyani RR, Blaha MJ, Feldman DI, et al. Vitamin D deficiency is independently associated with greater prevalence of erectile dysfunction: The National Health and Nutrition Examination Survey (NHANES) 2001–2004. Atherosclerosis. 2016;252:61–7.
Zhang JH, Li W, Wang CY, Zhang AN, Jia BZ, Li YW, et al. Correlation analysis of carotid artery intima-media thickness, serum 25(OH)D and men with erectile dysfunction. Front Endocrinol. 2022;13:1027430.
Sudarević B, Begić I, Šimunović D, Kuveždić H, Šerić V, Zibar L. Vitamin D Status in Renal Transplant recipients is not Associated with Erectile Dysfunction. Acta Clin Croat. 2017;56:195–202.
Smith GD, Ebrahim S. Mendelian randomization’: can genetic epidemiology contribute to understanding environmental determinants of disease? Int J Epidemiol. 2003;32:1–22.
Sekula P, Del Greco MF, Pattaro C, Köttgen A. Mendelian Randomization as an Approach to Assess Causality Using Observational Data. J Am Soc Nephrol. 2016;27:3253–65.
Lawlor DA, Harbord RM, Sterne JA, Timpson N, Davey Smith G. Mendelian randomization: using genes as instruments for making causal inferences in epidemiology. Stat Med. 2008;27:1133–63.
Skrivankova VW, Richmond RC, Woolf BAR, Yarmolinsky J, Davies NM, Swanson SA, et al. Strengthening the Reporting of Observational Studies in Epidemiology Using Mendelian Randomization: The STROBE-MR Statement. JAMA. 2021;326:1614–21.
Revez JA, Lin T, Qiao Z, Xue A, Holtz Y, Zhu Z, et al. Genome-wide association study identifies 143 loci associated with 25 hydroxyvitamin D concentration. Nat Commun. 2020;11:1647.
Bovijn J, Jackson L, Censin J, Chen CY, Laisk T, Laber S, et al. GWAS Identifies Risk Locus for Erectile Dysfunction and Implicates Hypothalamic Neurobiology and Diabetes in Etiology. Am J Hum Genet. 2019;104:157–63.
Collins A. Allelic association: linkage disequilibrium structure and gene mapping. Mol Biotechnol. 2009;41:83–89.
Burgess S, Thompson SG, CRP CHD Genetics Collaboration. Avoiding bias from weak instruments in Mendelian randomization studies. Int J Epidemiol. 2011;40:755–64.
Pierce BL, Ahsan H, Vanderweele TJ. Power and instrument strength requirements for Mendelian randomization studies using multiple genetic variants. Int J Epidemiol. 2011;40:740–52.
Fang SC, Rosen RC, Vita JA, Ganz P, Kupelian V. Changes in erectile dysfunction over time in relation to Framingham cardiovascular risk in the Boston Area Community Health (BACH) Survey. J Sex Med. 2015;12:100–8.
Keller J, Chen YK, Lin HC. Hyperthyroidism and erectile dysfunction: a population-based case-control study. Int J Impot Res. 2012;24:242–6.
Xiao Y, Xie T, Peng J, Zhou X, Long J, Yang M, et al. Factors associated with anxiety and depression in patients with erectile dysfunction: a cross-sectional study. BMC Psychol. 2023;11:36.
Esposito K, Giugliano F, Di Palo C, Giugliano G, Marfella R, D’Andrea F, et al. Effect of lifestyle changes on erectile dysfunction in obese men: a randomized controlled trial. JAMA. 2004;291:2978–84.
Zhang W, Zhang Y, Liu G, Wu X, Huang H, Jiang H, et al. An objective correlation of specific haematological parameters with ED severity. Andrologia. 2022;54:e14448.
Macdonald EJ, Gaines JM, Kim JI, Paduch DA. Exploring the relationship between socioeconomic status and erectile dysfunction: an analysis of the National Health and Nutrition Examination Survey. Int J Impot Res. 2023;35:478–83.
Yannas D, Zago E, Cavallini E, Todisco T, Vignozzi L, Corona G, et al. Education degree predicts cardiovascular outcomes in men suffering from erectile dysfunction. Andrology. 2023;11:1086–95.
Selvin E, Burnett AL, Platz EA. Prevalence and risk factors for erectile dysfunction in the US. Am J Med. 2007;120:151–7.
Burgess S, Davey Smith G, Davies NM, Dudbridge F, Gill D, Glymour MM, et al. Guidelines for performing Mendelian randomization investigations: update for summer 2023. Wellcome Open Res. 2023;4:186.
Burgess S, Butterworth A, Thompson SG. Mendelian randomization analysis with multiple genetic variants using summarized data. Genet Epidemiol. 2013;37:658–65.
Bowden J, Davey Smith G, Burgess S. Mendelian randomization with invalid instruments: effect estimation and bias detection through Egger regression. Int J Epidemiol. 2015;44:512–25.
Bowden J, Davey Smith G, Haycock PC, Burgess S. Consistent Estimation in Mendelian Randomization with Some Invalid Instruments Using a Weighted Median Estimator. Genet Epidemiol. 2016;40:304–14.
Bowden J, Del Greco MF, Minelli C, Davey Smith G, Sheehan N, Thompson J. A framework for the investigation of pleiotropy in two-sample summary data Mendelian randomization. Stat Med. 2017;36:1783–802.
Verbanck M, Chen CY, Neale B, Do R. Detection of widespread horizontal pleiotropy in causal relationships inferred from Mendelian randomization between complex traits and diseases. [published correction appears in Nat Genet. 2018 Aug50(8):1196]. Nat Genet. 2018;50:693–8.
Barassi A, Pezzilli R, Colpi GM, Corsi Romanelli MM, Melzi d’Eril GV. Vitamin D and erectile dysfunction. J Sex Med. 2014;11:2792–800.
El-Bahnasawy MS, El-Assmy A, Dawood A, Abobieh E, Dein BA, El-Din AB, et al. Effect of the use of internal iliac artery for renal transplantation on penile vascularity and erectile function: a prospective study. J Urol. 2004;172:2335–9.
Gontero P, Oderda M, Filippini C, Fontana F, Lazzarich E, Stratta P, et al. Does kidney transplantation onto the external iliac artery affect the haemodynamic parameters of the cavernosal arteries? Asian J Androl. 2012;14:621–5.
Wei Y, Chen P, Chen Q, Zhu H. Serum vitamin D levels and erectile dysfunction: A systematic review and meta-analysis. Andrologia. 2019;51:e13211.
Crafa A, Cannarella R, Condorelli RA, La Vignera S, Calogero AE. Is There an Association Between Vitamin D Deficiency and Erectile Dysfunction? A Systematic Review and Meta-Analysis. Nutrients. 2020;12:1411.
MacLaughlin J, Holick MF. Aging decreases the capacity of human skin to produce vitamin D3. J Clin Invest. 1985;76:1536–8.
Author information
Authors and Affiliations
Contributions
Dawei Gao, Cheng Chen, and Ziliang Wu contributed equally to this work. Dawei Gao was responsible for writing and revising the manuscript. Cheng Chen and Ziliang Wu were responsible for data collection and analysis. Huakang Li was responsible for verifying the data. Cheng Xie provided methodological guidance and suggestions for revisions to the manuscript. Bo Tang provided the research direction. All authors contributed to the article and approved the submitted version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gao, D., Chen, C., Wu, Z. et al. The association between serum 25-hydroxyvitamin D levels and erectile dysfunction: a two-sample Mendelian randomization analysis. Int J Impot Res (2024). https://doi.org/10.1038/s41443-024-00862-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41443-024-00862-1