Abstract
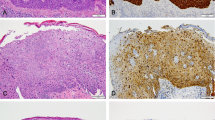
Penile intra-epithelial neoplasia (PeIN) is a known precursor for penile cancer. It may be undifferentiated or differentiated. The former is related to high-risk Human Papilloma Virus (HPV) and associated with p16 over-expression. Patients may present with red patches or lesions on the penis which on occasion may affect sexual activity.This study will assess associations between p16 status, patient parameters, treatment choice and outcomes. Data were collected on patients diagnosed with PeIN, who were referred to a single European Network, between 2008 and 2018. The following parameters were collected utilising patient records: demographics, smoking status, performance status, comorbidities, HPV/p16 status, lichen sclerosus (LS) status, treatment and clinical response. Log rank, Kaplan–Meier, Pearson Chi-Squared and Fishers Exact test were utilised to determine significance. One hundred thirty-seven patients were identified with PeIN and no invasive cancer. Staining for p16 was available in 91 patients and 74 patients were p16+. There were no significant differences in disease-free survival (DFS) for smoking status, performance status, comorbidities and lichen sclerosus, although patients with lichen sclerosus tended to recur sooner. Overall, p16+ patients showed significantly better DFS over p16− patients (n = 67; 10.4 vs 7.4 months; p = 0.023). In p16+ patients receiving treatment with imiquimod alone or with surgery, response rates were 100% vs 54% without imiquimod (n = 56; p = 0.017). In p16− patients receiving treatment with imiquimod alone or with surgery, response rates were 100% vs 56% without imiquimod (n = 17; p = 0.99). Overall 13.6% of patients progressed to cancer. The results indicate treatment combinations with immunotherapy tend to provide better responses despite p16 status. Patients with p16+ disease have a longer disease-free survival. Approximately 14% of patients progress to invasive disease. However, given the limitations in this study, further research is required to confirm these findings.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Gao W, Song LB, Yang J, et al. Risk factors and negative consequences of patient’s delay for penile carcinoma. World J Surg Oncol. 2016;14:124.
Arya M, Kalsi J, Kelly J, Muneer A. Malignant and premalignant lesions of the penis. BMJ. 2013;346:f1149.
Kidd LC, Chaing S, Chipollini J, Giuliano AR, Spiess PE, Sharma P. Relationship between human papillomavirus and penile cancer-implications for prevention and treatment. Transl Androl Urol. 2017;6:791–802.
Montes Cardona CE, García-Perdomo HA Incidence of penile cancer worldwide: systematic review and meta-analysis. Rev Panam Salud Publica. 2017; 41:e117.
Maddineni SB, Lau MM, Sangar VK. Identifying the needs of penile cancer sufferers: a systematic review of the quality of life, psychosexual and psychosocial literature in penile cancer. BMC Urol. 2009;2009:8.
Arya M, Li R, Pegler K, Sangar V, Kelly JD, Minhas S, et al. Long-term trends in incidence, survival and mortality of primary penile cancer in England. Cancer Causes Control. 2013;24:2169–76.
Maden C, Sherman KJ, Beckmann AM, et al. History of circumcision, medical conditions, and sexual activity and the risk of penile cancer. J Natl Cancer Inst. 1993;85:19–24.
Korenromp EL, Wi T, Resch S, Stover J, Broutet N. Costing of National STI Program Implementation for the Global STI Control Strategy for the Health Sector, 2016–2021. PLoS ONE. 2017;12.
Ventimiglia E, Horenblas S, Muneer A, Salonia A. Human papillomavirus infection and vaccination in males. Eur Urol Focus. 2016;2:355-62.
von Krogh G, Horenblas S. Diagnosis and clinical presentation of premalignant lesions of the penis. Scand J Urol Nephrol Suppl. 2000;205:201–14.
Hakenberg OW, Compérat EM, Minhas S, Necchi A, Protzel CWN. EAU guidelines on penile cancer: 2014 update. Eur Urol. 2015;67:142.
Oken MM, Creech RH, Tormey DC, et al. Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5:649–55.
Micali G, Nasca MR, Tedeschi A. Topical treatment of intraepithelial penile carcinoma with imiquimod. Clin Exp Dermatol. 2003;28:s4–6.
Porter WM, Francis N, Hawkins D, Dinneen M, Bunker CB. Penile intraepithelial neoplasia: clinical spectrum and treatment of 35 cases. Br J Dermatol. 2002;147:1159–65.
Kizer WS, Prarie T, Morey AF. Balanitis xerotica obliterans: epidemiologic distribution in an equal access health care system. South Med J. 2003;96:9–11.
Lee A, Bradford J, Fischer G. Long-term management of adult vulvar lichen sclerosus: a prospective cohort study of 507 women. JAMA Dermatol. 2015;151:1061–67.
Pietrzak P, Hadway P, Corbishley CM, Watkin NA. Is the association between balanitis xerotica obliterans and penile carcinoma underestimated? BJU Int. 2006;98:74–6.
Barbagli G, Palminteri E, Mirri F, Guazzoni G, Turini D, Lazzeri M. Penile carcinoma in patients with genital lichen sclerosus: a multicenter survey. J Urol. 2006;175:1359–63.
Mannweiler S, Sygulla S, Winter E, Regauer S. Two major pathways of penile carcinogenesis: HPV-induced penile cancers overexpress p16INK4a, HPV-negative cancers associated with dermatoses express p53, but Lack p16INK4a overexpression. J Am Acad Dermatol. 2013;69:73–81.
Albieri V, Kjaer SK, Olesen TB, Sand FL, Rasmussen CL, Albieri V, et al. Prevalence of human papillomavirus DNA and p16INK4a in penile cancer and penile intraepithelial neoplasia: a systematic review and meta-analysis. Lancet Oncol. 2019;20:145–58.
Lont AP, Kroon BK, Horenblas S, Gallee MPW, Berkhof J, Meijer CJLM, et al. Presence of high-risk human papillomavirus DNA in penile carcinoma predicts favorable outcome in survival. Int J Cancer. 2006;119:1078–81.
Gunia S, Erbersdobler A, Hakenberg OW, Koch S, May M. p16 INK4a is a marker of good prognosis for primary invasive penile squamous cell carcinoma: a multi-institutional study. J Urol. 2012;187:899–907.
Heideman DAM, Bleeker MCG, Ahmed HU, Arya M, Horenblas S, Snijders PJF et al. In: Muneer A, Arya MHS, editors. Molecular biology of penile cancer: textbook of penile cancer. London: Springer; 2012. p. 13–25.
Sujenthiran A, Yan S, Ager M, Corbishley C, Ayres B, Watkin N. Oncological outcomes of 100 glans resurfacing procedures for superficial invasive penile cancer. Eur Urol Suppl. 2018;17:e50.
Giuliano AR, Palefsky JM, Goldstone S, Moreira ED, Penny ME, Aranda C, et al. Efficacy of quadrivalent HPV vaccine against HPV infection and disease in males. N Engl J Med. 2011;364:401–11.
Ingles DJ, Pierce Campbell CM, Messina JA, Stoler MH, Lin H-Y, Fulp WJ, et al. Human papillomavirus virus (HPV) genotype- and age-specific analyses of external genital lesions among men in the HPV infection in men (HIM) study. J Infect Dis. 2015;211:1060–7.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ashley, S., Shanks, J.H., Oliveira, P. et al. Human Papilloma Virus (HPV) status may impact treatment outcomes in patients with pre-cancerous penile lesions (an eUROGEN Study). Int J Impot Res 33, 620–626 (2021). https://doi.org/10.1038/s41443-020-0327-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-020-0327-4
This article is cited by
-
Surgical technique and outcomes following coronal-sparing glans resurfacing for benign and malignant penile lesions
International Journal of Impotence Research (2022)
-
Penile cancer
Nature Reviews Disease Primers (2021)