Abstract
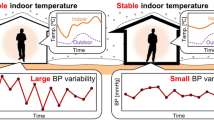
The association of blood pressure and temperature is well known in seasonal observation, and low temperature in the winter season is often considered a cause of high blood pressure. The current evidence for short-term studies of temperature and blood pressure is based on the daily observation, however continuous monitoring with wearable devices will allow us to evaluate the rapid effect of cold temperature exposure on blood pressure. In a Japanese, prospective intervention study from 2014 to 2019 (the Smart Wellness Housing survey), approximately 90% of Japanese lived in cold houses (indoor temperature less than 18 °C). Importantly, the indoor temperature was associated with the increase of morning systolic blood pressure. We recently addressed the sympathetic nervous activation of individuals in both their houses and a highly insulated and airtight model house in the winter season using portable electrocardiography equipment. A few subjects showed a morning surge in sympathetic activity, which was more intense at their cold houses, which suggests the importance of the indoor environment in the management of early morning hypertension. In near future, real-time monitoring with wearable devices will provide important information for a better life-environment, leading to risk reduction of morning surge and cardiovascular events.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
The Eurowinter Group. Cold exposure and winter mortality from ischaemic heart disease, cerebrovascular disease, respiratory disease, and all causes in warm and cold regions of Europe. Lancet. 1997;349:1341–6.
Modesti PA, Rapi S, Rogolino A, Tosi B, Galanti G. Seasonal blood pressure variation: implications for cardiovascular risk stratification. Hypertens Res. 2018;41:475–82.
Brennan PJ, Greenberg G, Miall WE, Thompson SG. Seasonal variation in arterial blood pressure. Brit Med J. 1982;285:919–23.
Modesti PA, Morabito M, Massetti L, Rapi S, Orlandini S, Mancia G, et al. Seasonal blood pressure changes: a n independent relationship with temperature and daylight hours. Hypertens. 2013;61:908–14.
Hong YC, Kim H, Lim YH, Yoon HJ, Kwon YM, Park M. Identification of RAS genotypes that modulate blood pressure change by outdoor temperature. Hypertens Res. 2013;36:540–5.
Kario K, Pickering TG, Hoshide S, Eguchi K, Ishikawa J, Morinari M, et al. Morning blood pressure surge and hypertensive cerebrovascular disease: role of the alpha adrenergic sympathetic nervous system. Am J Hypertens. 2004;17:668–75.
Saad WA, Guarda IF, Camargo LA, Santos TA. Nitric oxide and L-type calcium channel influences the changes in arterial blood pressure and heart rate induced by central angiotesin II. Behav Brain Funct. 2008;24:4–22.
Hu J, He G, Luo J, Xu Y, Xu X, Song X, et al. Temperature adjusted hypertension prevalence and control rate: a series of cross-sectional studies in Guangdong Province, China. J Hypertens. 2021;39:911–18.
Hozawa A, Kuriyama S, Shimazu T, Ohmori-Matsuda K, Tsuji I. Seasonal variation in home blood pressure measurements and relation to outside temperature in Japan. Clin Exp Hypertens. 2011;33:153–8.
Zhao H, Jivraj S, Moody A. My blood pressure is low today, do you have the heating on?’ The association between indoor temperature and blood pressure. J Hypertens. 2019;37:504–12.
Tikhonoff V, Casiglia E. Body, indoor, outdoor temperature - and arterial blood pressure. J Hypertens. 2021;39:861–3.
Housing Bureau, Ministry of Land, Infrastructure, Transport and Tourism. The first session of the committee on energy saving measures for houses and buildings for a decarbonized society (in Japanese). 2021. https://www.mlit.go.jp/jutakukentiku/house/content/001400905.pdf. Accessed 7 Jul 2022.
Umishio W, Ikaga T, Kario K, Fujino Y, Hoshi T, Ando S, et al. Cross-sectional analysis of the relationship between home blood pressure and indoor temperature in winter: a nationwide smart wellness housing survey in Japan. Hypertension. 2019;74:756–66.
Tochihara Y, Hamaguchi N, Yadoguchi I, Kaji Y, Shoyama S. Effects of room temperature on physiological and subjective responses to bathing in the elderly. J Hum Environ Syst. 2012;15:13–9.
Kario K, Saito I, Kushiro T, Teramukai S, Ishikawa Y, Mori Y, et al. Home blood pressure and cardiovascular outcomes in patients during antihypertensive therapy: primary results of HONEST, a large-scale prospective, real-world observational study. Hypertension. 2014;64:989–96.
Ohkubo T, Imai Y, Tsuji I, Nagai K, Kato J, Kikuchi N, et al. Home blood pressure measurement has a stronger predictive power for mortality than does screening blood pressure measurement: a population-based observation in Ohasama, Japan. J Hypertens. 1998;16:971–5.
Kario K, Iwashita M, Okuda Y, Sugiyama M, Saito I, Kushiro T, et al. Morning home blood pressure and cardiovascular events in Japanese hypertensive patients. Hypertension 2018;72:854–61.
Narita K, Hoshide S, Kario K. Seasonal variation in day-by-day home blood pressure variability and effect on cardiovascular disease incidence. Hypertension. 2022;79:2062–70.
Nakagami H, Akiyama H, Otsuka H, Iwamae A, Yamada H. Blood pressure fluctuations and the indoor environment in a highly insulated and airtight model house during the cold winter season. Hypertens Res. 2022;45:1217–9.
Nakagami H, Akiyama H, Otsuka H, Takahashi SA, Sawada K, Kobayashi N, et al. Morning surge in sympathetic nervous activity in the indoor environment during the cold winter season. Hypertens Res. 2023;46:231–5.
Akselrod S, Gordon D, Ubel FA, Shannon DC, Berger AC, Cohen RJ. Power spectrum analysis of heart rate fluctuation: a quantitative probe of beat-to-beat cardiovascular control. Science. 1981;213:220–2.
Task force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology. Heart rate variability: standards of measurement, physiological interpretation and clinical use. Circulation. 1996;93:1043–65.
Public Health England. Minimum Home Temperature Thresholds for Health in Winter: A Systematic Literature Review. 2014. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/468196/Min_temp_threshold_for_homes_in_winter.pdf.
World Health Organization. Housing and Health Guidelines. 2018. https://www.who.int/sustainable-development/publications/housing-health-guidelines/en/.
Building Research Establishment. Energy Follow-Up Survey 2011: Report 2: Mean household temperatures; BRE report number 283078, Dec 2013. https://assets.publishing.service.gov.uk/government/uploads/system/uploa….
Quinn A, Shaman J. Indoor temperature and humidity in New York city apartments during winter. Sci Total Environ. 2017;583:29–35.
Kario K, Harada N, Okura A. State-of-the-art rapid review of the current landscape of digital hypertension. Conn Health. 2022;1:46–58.
Nakagami H. New wave of digital hypertension management for clinical applications. Hypertens Res. 2022;45:1549–51.
Kario K. Management of hypertension in the digital era: small wearable monitoring devices for remote blood pressure monitoring. Hypertension. 2020;76:640–50.
Tomitani N, Kanegae H, Kario K. Self-monitoring of psychological stress-induced blood pressure in daily life with a wearable watch-type oscillometric device in working hypertensives. Hypertens Res. 2022;45:1531–7.
Tomitani N, Kanegae H, Suzuki Y, Kuwabara M, Kario K. Stress-induced blood pressure elevation self-measured by a wearable watch-type device. Am J Hypertens. 2021;34:377–82.
Funding
This study was partially supported by a collaboration research fund from the Asahi Kasei Construction Materials Corporation.
Author information
Authors and Affiliations
Contributions
HN wrote the paper. HO and HA: Data collection and support for analysis. All authors drafted the paper and approved the final version for submission.
Corresponding author
Ethics declarations
Conflict of interest
The Department of Health Development and Medicine is an endowed department supported by Anges, Daicel, and FunPep. Hiroshi Akiyama and Hiroki Otsuka are employees of the Asahi Kasei Construction Materials Corporation.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nakagami, H., Otsuka, H. & Akiyama, H. Monitoring with wearable devices will clarify the association between indoor temperature and blood pressure. Hypertens Res 46, 1450–1455 (2023). https://doi.org/10.1038/s41440-023-01261-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-023-01261-7