Abstract
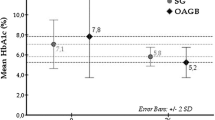
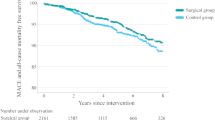
This study aimed to assess the remission and relapse of hypertension (HTN) in hypertensive individuals who underwent sleeve gastrectomy (SG) and one-anastomosis gastric bypass (OAGB) and identify the predictors of HTN remission and relapse following bariatric surgery. A prospective cohort study with a follow-up of 3 years was conducted on severely obese patients between 2013 and 2018. Hypertension remission was defined as the normalization of blood pressure (BP) with the discontinuation of medical treatment, and HTN relapse was defined as the need for the onset of antihypertensive drugs or the occurrence of BP impairment. A total of 787 hypertensive patients were included in this study. The cumulative incidence of HTN remission and relapse were 83.9% (95% CI: 81.6–86.5) and 31.4% (95% CI: 25.6–38.2), respectively. Remission and relapse were not significantly different among the patients undergoing either surgery (SG or OAGB). A higher remission rate was linked to a younger age and the use of fewer antihypertensive medications pre-operation. However, failure to successfully lose weight during the first year postoperative and weight regain predicted a higher risk of HTN relapse after 3 years. Following bariatric surgery, BP drops initially but then gradually rises. These alterations are responsible for about 31% relapse after 3 years in those who initially achieve remission. Patients who are younger and use less antihypertensive medications before surgery may benefit the most from bariatric surgery in terms of HTN. First-year successful weight loss and control of weight regain may prevent HTN relapse in the following years.

This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The datasets used and analyzed in the current study are available from the corresponding author on reasonable request.
References
Stevens G, Mascarenhas M, Mathers C. Global health risks: progress and challenges. Bull World Health Organ. 2009;87:646.
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J. Global burden of hypertension: analysis of worldwide data. Lancet. 2005;365:217–23.
Sarki AM, Nduka CU, Stranges S, Kandala NB, Uthman OA. Prevalence of hypertension in low- and middle-income countries: a systematic review and meta-analysis. Medicine. 2015;94:e1959.
Yusufali AM, Khatib R, Islam S, Alhabib KF, Bahonar A, Swidan HM, et al. Prevalence, awareness, treatment and control of hypertension in four Middle East countries. J Hypertens. 2017;35:1457–64.
Afsargharehbagh R, Rezaie-Keikhaie K, Rafiemanesh H, Balouchi A, Bouya S, Dehghan B. Hypertension and pre-hypertension among Iranian adults population: a meta-analysis of prevalence, awareness, treatment, and control. Curr Hypertens Rep. 2019;21:27.
Garrison RJ, Kannel WB, Stokes J 3rd, Castelli WP. Incidence and precursors of hypertension in young adults: the Framingham Offspring Study. Prev Med. 1987;16:235–51.
Hall ME, do Carmo JM, da Silva AA, Juncos LA, Wang Z, Hall JE. Obesity, hypertension, and chronic kidney disease. Int J Nephrol Renov Dis. 2014;7:75–88.
Cohen JB. Hypertension in obesity and the impact of weight loss. Curr Cardiol Rep. 2017;19:98.
Hall JE, do Carmo JM, da Silva AA, Wang Z, Hall ME. Obesity, kidney dysfunction and hypertension: mechanistic links. Nat Rev Nephrol. 2019;15:367–85.
Severin R, Sabbahi A, Mahmoud AM, Arena R, Phillips SA. Precision medicine in weight loss and healthy living. Prog Cardiovasc Dis. 2019;62:15–20.
English WJ, Williams DB. Metabolic and bariatric surgery: an effective treatment option for obesity and cardiovascular disease. Prog Cardiovasc Dis. 2018;61:253–69.
Wiggins T, Guidozzi N, Welbourn R, Ahmed AR, Markar SR. Association of bariatric surgery with all-cause mortality and incidence of obesity-related disease at a population level: a systematic review and meta-analysis. PLoS Med. 2020;17:e1003206.
Angrisani L, Santonicola A, Iovino P, Vitiello A, Higa K, Himpens J, et al. IFSO Worldwide Survey 2016: primary, endoluminal, and revisional procedures. Obes Surg. 2018;28:3783–94.
Climent E, Goday A, Pedro-Botet J, Solà I, Oliveras A, Ramón JM, et al. Laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for 5-year hypertension remission in obese patients: a systematic review and meta-analysis. J Hypertens. 2020;38:185–95.
Vest AR, Heneghan HM, Agarwal S, Schauer PR, Young JB. Bariatric surgery and cardiovascular outcomes: a systematic review. Heart. 2012;98:1763–77.
Benaiges D, Sagué M, Flores-Le Roux JA, Pedro-Botet J, Ramón JM, Villatoro M, et al. Predictors of hypertension remission and recurrence after bariatric surgery. Am J Hypertens. 2016;29:653–9.
Nudotor RD, Canner JK, Haut ER, Prokopowicz GP, Steele KE. Comparing remission and recurrence of hypertension after bariatric surgery: vertical sleeve gastrectomy versus Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2021;17:308–18.
Reynolds K, Barton LJ, Basu A, Fischer H, Arterburn DE, Barthold D, et al. Comparative effectiveness of gastric bypass and vertical sleeve gastrectomy for hypertension remission and relapse: the ENGAGE CVD Study. Hypertension. 2021;78:1116–25.
Stenberg E, Marsk R. Remission, relapse, and risk of major cardiovascular events after metabolic surgery in persons with hypertension: a Swedish nationwide registry-based cohort study. PLoS Med. 2021;18:e1003817.
Barzin M, Hosseinpanah F, Motamedi MA, Shapoori P, Arian P, Daneshpour MA, et al. Bariatric surgery for morbid obesity: Tehran Obesity Treatment Study (TOTS) rationale and study design. JMIR Res Protoc. 2016;5:e8.
de Onis M, Habicht JP. Anthropometric reference data for international use: recommendations from a World Health Organization Expert Committee. Am J Clin Nutr. 1996;64:650–8.
Brethauer SA, Kim J, el Chaar M, Papasavas P, Eisenberg D, Rogers A, et al. Standardized outcomes reporting in metabolic and bariatric surgery. Surgery for obesity and related diseases: official journal of the American Society for Bariatric. Surgery. 2015;11:489–506.
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2018;138:e426–83.
Livhits M, Mercado C, Yermilov I, Parikh JA, Dutson E, Mehran A, et al. Preoperative predictors of weight loss following bariatric surgery: systematic review. Obes Surg. 2012;22:70–89.
King WC, Hinerman AS, Courcoulas AP. Weight regain after bariatric surgery: a systematic literature review and comparison across studies using a large reference sample. Surg Obes Relat Dis. 2020;16:1133–44.
Arterburn DE, Telem DA, Kushner RF, Courcoulas AP. Benefits and risks of bariatric surgery in adults: a review. JAMA. 2020;324:879–87.
Ebadinejad A, Barzin M, Abiri B, Mahdavi M, Khalaj A, Ebrahimi D, et al. The effect of bariatric surgery in comparison with the control group on the prevention of comorbidities in people with severe obesity: a prospective cohort study. BMC Surg. 2022;22:290.
Khalaj A, Tasdighi E, Hosseinpanah F, Mahdavi M, Valizadeh M, Farahmand E, et al. Two-year outcomes of sleeve gastrectomy versus gastric bypass: first report based on Tehran obesity treatment study (TOTS). BMC Surg. 2020;20:160.
Wu C, Bai R, Yan W, Yan M, Song M. Clinical outcomes of one anastomosis gastric bypass versus sleeve gastrectomy for morbid obesity. Obes Surg. 2020;30:1021–31.
Schiavon CA, Bhatt DL, Ikeoka D, Santucci EV, Santos RN, Damiani LP, et al. Three-year outcomes of bariatric surgery in patients with obesity and hypertension: a randomized clinical trial. Ann Intern Med. 2020;173:685–93.
Climent E, Oliveras A, Pedro-Botet J, Goday A, Benaiges D. Bariatric surgery and hypertension. J Clin Med. 2021;10:4049.
Moriconi D, Manca ML, Anselmino M, Rebelos E, Bellini R, Taddei S, et al. Predictors of type 2 diabetes relapse after Roux-en-Y gastric bypass: a ten-year follow-up study. Diabetes Metab. 2022;48:101282.
Rebelos E, Moriconi D, Scalese M, Denoth F, Molinaro S, Siciliano V, et al. Impact of postprandial hypoglycemia on weight loss after bariatric surgery. Obes Surg. 2020;30:2266–73.
Rezaei S, Mahmoudi Z, Sheidaei A, Aryan Z, Mahmoudi N, Gohari K, et al. Salt intake among Iranian population: the first national report on salt intake in Iran. J Hypertens. 2018;36:2380–9.
Hall ME, Cohen JB, Ard JD, Egan BM, Hall JE, Lavie CJ, et al. Weight-loss strategies for prevention and treatment of hypertension: a scientific statement from the American Heart Association. Hypertension. 2021;78:e38–50.
Samson R, Ayinapudi K, Le Jemtel TH, Oparil S. Obesity, hypertension, and bariatric surgery. Curr Hypertens Rep. 2020;22:46.
le Roux CW, Welbourn R, Werling M, Osborne A, Kokkinos A, Laurenius A, et al. Gut hormones as mediators of appetite and weight loss after Roux-en-Y gastric bypass. Ann Surg. 2007;246:780–5.
Sandoval DA, D’Alessio DA. Physiology of proglucagon peptides: role of glucagon and GLP-1 in health and disease. Physiol Rev. 2015;95:513–48.
Bonfils PK, Taskiran M, Damgaard M, Goetze JP, Floyd AK, Funch-Jensen P, et al. Roux-en-Y gastric bypass alleviates hypertension and is associated with an increase in mid-regional pro-atrial natriuretic peptide in morbid obese patients. J Hypertens. 2015;33:1215–25.
Landsberg L, Aronne LJ, Beilin LJ, Burke V, Igel LI, Lloyd-Jones D, et al. Obesity-related hypertension: pathogenesis, cardiovascular risk, and treatment—a position paper of the The Obesity Society and The American Society of Hypertension. Obesity. 2013;21:8–24.
Petersen KS, Blanch N, Keogh JB, Clifton PM. Effect of weight loss on pulse wave velocity: systematic review and meta-analysis. Arterioscler Thromb Vasc Biol. 2015;35:243–52.
Moritz E, Dadson P, Saukko E, Honka MJ, Koskensalo K, Seppälä K, et al. Renal sinus fat is expanded in patients with obesity and/or hypertension and reduced by bariatric surgery associated with hypertension remission. Metabolites. 2022;12:617.
Agha R, Abdall-Razak A, Crossley E, Dowlut N, Iosifidis C, Mathew G. STROCSS 2019 guideline: strengthening the reporting of cohort studies in surgery. Int J Surg. 2019;72:156–65.
Sjöström CD, Peltonen M, Wedel H, Sjöström L. Differentiated long-term effects of intentional weight loss on diabetes and hypertension. Hypertension. 2000;36:20–5.
O’Brien E, Parati G, Stergiou G, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension position paper on ambulatory blood pressure monitoring. J Hypertens. 2013;31:1731–68.
Kotsis V, Stabouli S, Bouldin M, Low A, Toumanidis S, Zakopoulos N. Impact of obesity on 24-hour ambulatory blood pressure and hypertension. Hypertension. 2005;45:602–7.
Oliveras A, Goday A, Sans L, Arias CE, Vazquez S, Benaiges D, et al. Changes in central 24-h ambulatory blood pressure and hemodynamics 12 months after bariatric surgery: the BARIHTA study. Obes Surg. 2020;30:195–205.
Vidal J, Nicolau J, Romero F, Casamitjana R, Momblan D, Conget I, et al. Long-term effects of Roux-en-Y gastric bypass surgery on plasma glucagon-like peptide-1 and islet function in morbidly obese subjects. J Clin Endocrinol Metab. 2009;94:884–91.
Acknowledgements
The authors would like to thank the hospital staff, assistants, and coordinators who took part in this research. Also, special thanks to Mohammadreza Golsibi for his assistance and support in working with the electronic patient data system.
Author information
Authors and Affiliations
Contributions
AE: study design, data collection, coordination of patients’ issues, manuscript preparation, and final approval of the manuscript. MS: data collection, literature review, and manuscript preparation. FH: data collection, literature review, and manuscript preparation. AK: study design, performing surgical operations, and final approval of the manuscript. MM: data analysis, data interpretation, and manuscript preparation. FG: data collection, literature review, and manuscript preparation. MV: final approval of the manuscript. MB: study design, revising the manuscript, and final approval of the manuscript. All authors reviewed and approved the final draft of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All the procedures performed in the study were approved by the Research Ethics Committee of the Research Institute for Endocrine Sciences of Shahid Beheshti University of Medical Sciences and were in accordance with the ethical standards of the institutional Human Research Review Committee (IR.SBMU.ENDOCRINE.REC.1400.096) and the 1964 Helsinki declaration and its later amendments. Informed written consent was obtained from all participants.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ebadinejad, A., Shahshahani, M., Hosseinpanah, F. et al. Comparison of hypertension remission and relapse after sleeve gastrectomy and one-anastomosis gastric bypass: a prospective cohort study. Hypertens Res 46, 1287–1296 (2023). https://doi.org/10.1038/s41440-023-01180-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-023-01180-7
Keywords
This article is cited by
-
Bariatric surgery to treat hypertension
Hypertension Research (2023)