Abstract
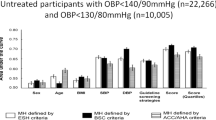
Masked hypertension is defined by office blood pressure (BP) in the controlled-BP range while out-of-office BP measured by ambulatory BP monitoring (ABPM) and home BP monitoring (HBPM) is in the uncontrolled range. However, diagnosis of masked hypertension may differ if assessed by different out-of-office BP indices. This study aims to investigate the diagnostic agreement of masked uncontrolled hypertension (MUHT) detected by ABPM indices (ABPM-MUHT) and HBPM indices (HBPM-MUHT) using the same all-in-one device (TM2441; A&D Company). The present study enrolled a total of 2322 treated hypertensive patients (males 53.2%, average age 69.2 ± 11.5 years) from the Home-Activity ICT-based Japan Ambulatory Blood Pressure Monitoring Prospective (HI-JAMP) Study, who consecutively underwent office BP monitoring, 24-h ABPM (at 30-min intervals), and 5-day HBPM (twice each morning and evening) using the same device. When out-of-office BP control status was assessed only by 24-h average SBP or by the average of morning and evening SBP, the diagnostic agreement of MUHT detected by ABPM and HBPM was 29.7% among the 445 patients with any type of MUHT. When out-of-office BP indices in each time-window were simultaneously assessed, the diagnostic agreement increased to 40–45.7%. Our results indicated the importance of assessing BPs at various times of day, especially morning hours, for perfect hypertension management. Diagnosis of masked hypertension only by an averaged BP index, without considering specific time-windows, might underestimate cardiovascular risk.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Whelton PK, Carey RM, Aronow WS, Casey DE Jr, Collins KJ, Dennison Himmelfarb C, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2018;71:e127–e248.
Williams B, Mancia G, Spiering W, Agabiti Rosei E, Azizi M, Burnier M, et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur Heart J. 2018;39:3021–104.
Umemura S, Arima H, Arima S, Asayama K, Dohi Y, Hirooka Y, et al. The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2019). Hypertens Res. 2019;42:1235–481.
Stergiou GS, Palatini P, Parati G, O’Brien E, Januszewicz A, Lurbe E, et al. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. J Hypertens. 2021;39:1293–302.
Kario K, Tomitani N, Morimoto T, Kanegae H, Lacy P, Williams B. Relationship between blood pressure repeatedly measured by a wrist-cuff oscillometric wearable blood pressure monitoring device and left ventricular mass index in working hypertensive patients. Hypertens Res. 2022;45:87–96.
Sega R, Facchetti R, Bombelli M, Cesana G, Corrao G, Grassi G, et al. Prognostic value of ambulatory and home blood pressures compared with office blood pressure in the general population: follow-up results from the Pressioni Arteriose Monitorate e Loro Associazioni (PAMELA) study. Circulation 2005;111:1777–83.
Kang YY, Li Y, Huang QF, Song J, Shan XL, Dou Y, et al. Accuracy of home versus ambulatory blood pressure monitoring in the diagnosis of white-coat and masked hypertension. J Hypertens. 2015;33:1580–7.
Anstey DE, Muntner P, Bello NA, Pugliese DN, Yano Y, Kronish IM, et al. Diagnosing masked hypertension using ambulatory blood pressure monitoring, home blood pressure monitoring, or both? Hypertension 2018;72:1200–7.
Ntineri A, Niiranen TJ, McManus RJ, Lindroos A, Jula A, Schwartz C, et al. Ambulatory versus home blood pressure monitoring: frequency and determinants of blood pressure difference and diagnostic disagreement. J Hypertens. 2019;37:1974–81.
Kario K, Hoshide S, Saito K, Sato K, Hamasaki H, Suwa H, et al. Validation of the TM-2441 ambulatory blood pressure measurement device according to the ISO 81060-2: 2013 standard. Blood Press Monit. 2019;24:38–41.
Kario K, Tomitani N, Nishizawa M, Harada N, Kanegae H, Hoshide S Concept, study design, and baseline blood pressure control status of the nation-wide prospective HI–JAMP study using multisensor ABPM. Hypertens Res. 2022; in press.
Group JCSJW. Guidelines for the clinical use of 24h ambulatory blood pressure monitoring (ABPM) (JCS 2010): - digest version. Circ J. 2012;76:508–19.
Kario KWJ, Chia YC, Wang TD, Li Y, Siddique S, Shin J, et al. The HOPE Asia Network 2022 Up-date Consensus Statement on morning hypertension management J Clin Hypertens. 2022; in press.
Yang WY, Thijs L, Zhang ZY, Asayama K, Boggia J, Hansen TW, et al. Evidence-based proposal for the number of ambulatory readings required for assessing blood pressure level in research settings: an analysis of the IDACO database. Blood Press. 2018;27:341–50.
Kario K. Global Impact of 2017 American Heart Association/American College of Cardiology Hypertension Guidelines: A Perspective From Japan. Circulation 2018;137:543–5.
Asayama K, Thijs L, Li Y, Gu YM, Hara A, Liu YP, et al. Setting thresholds to varying blood pressure monitoring intervals differentially affects risk estimates associated with white-coat and masked hypertension in the population. Hypertension 2014;64:935–42.
Hoshide S, Yano Y, Haimoto H, Yamagiwa K, Uchiba K, Nagasaka S, et al. Morning and evening home blood pressure and risks of incident stroke and coronary artery disease in the Japanese general practice population: The Japan Morning Surge-Home Blood Pressure Study. Hypertension 2016;68:54–61.
Kario K, Saito I, Kushiro T, Teramukai S, Ishikawa Y, Mori Y, et al. Home blood pressure and cardiovascular outcomes in patients during antihypertensive therapy: primary results of HONEST, a large-scale prospective, real-world observational study. Hypertension 2014;64:989–96.
Kario K, Ishikawa J, Pickering TG, Hoshide S, Eguchi K, Morinari M, et al. Morning hypertension: the strongest independent risk factor for stroke in elderly hypertensive patients. Hypertens Res. 2006;29:581–7.
Booth JN 3rd, Jaeger BC, Huang L, Abdalla M, Sims M, Butler M, et al. Morning blood pressure surge and cardiovascular disease events and all-cause mortality in blacks: The Jackson Heart Study. Hypertension 2020;75:835–43.
Kario K, Pickering TG, Umeda Y, Hoshide S, Hoshide Y, Morinari M, et al. Morning surge in blood pressure as a predictor of silent and clinical cerebrovascular disease in elderly hypertensives: a prospective study. Circulation 2003;107:1401–6.
Kario K. Systemic hemodynamic atherothrombotic syndrome: a blind spot in the current management of hypertension. J Clin Hypertens. 2015;17:328–31.
Mokwatsi GG, Hoshide S, Kanegae H, Fujiwara T, Negishi K, Schutte AE, et al. Direct comparison of home versus ambulatory defined nocturnal hypertension for predicting cardiovascular events: The Japan Morning Surge-Home Blood Pressure (J-HOP) Study. Hypertension 2020;76:554–61.
Kallem RR, Meyers KE, Sawinski DL, Townsend RR. A comparison of two ambulatory blood pressure monitors worn at the same time. J Clin Hypertens. 2013;15:321–5.
Stergiou GS, Kyriakoulis KG, McManus RJ, Andreadis EA, Jula A, Kollias A, et al. Phenotypes of masked hypertension: Isolated ambulatory, isolated home and dual masked hypertension. J Hypertens. 2020;38:218–23.
Shin J, Kario K, Chia YC, Turana Y, Chen CH, Buranakitjaroen P, et al. Current status of ambulatory blood pressure monitoring in Asian countries: A report from the HOPE Asia Network. J Clin Hypertens. 2020;22:384–90.
Mancia G, Facchetti R, Vanoli J, Dolfini V, Grassi G, Reproducibility of blood pressure phenotypes identified by office and ambulatory blood pressure in treated hypertensive patients. Data from the PHYLLIS study. Hypertens Res. 2022 (e-pub ahead of print 2022/08/09; https://doi.org/10.1038/s41440-022-00982-5).
Gkaliagkousi E, Protogerou AD, Argyris AA, Koletsos N, Triantafyllou A, Anyfanti P, et al. Contribution of single office aortic systolic blood pressure measurements to the detection of masked hypertension: data from two separate cohorts. Hypertens Res. 2021;44:215–24.
Kario K, Hoshide S, Tomitani N, Nishizawa M, Yoshida T, Kabutoya T, et al. Inconsistent control status of office, home, and ambulatory blood pressure all taken using the same device: The HI–JAMP study baseline data. Am J Hypertens. 2022; in press.
Hoshide S, Kario K, de la Sierra A, Bilo G, Schillaci G, Banegas JR, et al. Ethnic differences in the degree of morning blood pressure surge and in its determinants between Japanese and European hypertensive subjects: data from the ARTEMIS study. Hypertension 2015;66:750–6.
Tomitani N, Wanthong S, Roubsanthisuk W, Buranakitjaroen P, Hoshide S, Kario K. Differences in ambulatory blood pressure profiles between Japanese and Thai patients with hypertension /suspected hypertension. J Clin Hypertens. 2021;23:614–20.
Acknowledgements
The authors thank all nurses and physicians of the participating centers for their excellent cooperation and help. The authors also thank Ms. Noriko Harada, Ms. Tomoko Shiga, and Ms. Tomoko Morimoto for their assistance with study coordination and data management, and Mr. Nobuhiko Yasui and Mr. Toshiyuki Kiuchi for their valuable advice.
Funding
This study was financially supported in part by A&D Co., Ltd., by Otsuka Medical Devices Co., Ltd., and by a grant from the Foundation for the Development of the Community (Tochigi).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
KK has received research grants from Omron Healthcare Co., Ltd., A&D Co., Ltd., and Fukuda Denshi Co., Ltd. M. The other authors report no conflicts.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tomitani, N., Hoshide, S., Kario, K. et al. Diagnostic agreement of masked uncontrolled hypertension detected by ambulatory blood pressure and home blood pressure measured by an all-in-one BP monitoring device: The HI–JAMP study. Hypertens Res 46, 157–164 (2023). https://doi.org/10.1038/s41440-022-01073-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-01073-1
Keywords
This article is cited by
-
The role of wearable home blood pressure monitoring in detecting out-of-office control status
Hypertension Research (2024)
-
2023 update and perspectives
Hypertension Research (2024)
-
Masked hypertension: how not to miss an even more silent killer
Hypertension Research (2023)
-
Preface—this month’s Asian perspectives
Hypertension Research (2023)
-
Effective out-of-office BP monitoring to detect masked hypertension: perspectives for wearable BP monitoring
Hypertension Research (2023)