Abstract
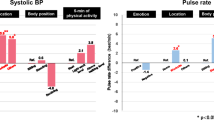
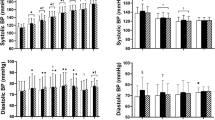
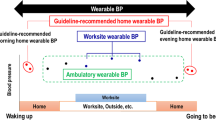
This study investigated psychological stress-induced blood pressure (BP) elevation according to self-measured data obtained by a wearable watch-type oscillometric device for multiple days in 50 working hypertension patients (mean ± SD age: 60.5 ± 8.9 years; 92.0% men; 96% treated for hypertension). Participants were asked to self-measure their BPs at five predetermined times as well as at any additional time points at their own discretion under ambulatory conditions for a maximum of 7 days. At the time of each BP measurement, participants self-reported their location, emotion, and degree of stress. A total of 1220 BP readings with self-reported situational information were obtained from 50 participants over 5.5 ± 1.2 days. Systolic BP (SBP) and diastolic BP (DBP) measured during moments of self-reported negative emotions (i.e., anger, tension, anxiety, or sadness) were significantly higher (5.0 ± 1.3 and 2.0 ± 0.8 mmHg, both p < 0.05) than those during moments of self-reported positive emotions (i.e., happiness or calm). SBP/DBP were significantly increased under a moderate or high degree of stress by [4.5 ± 1.1]/[2.5 ± 0.7] and [10.2 ± 3.0]/[4.7 ± 1.8] mmHg, respectively. As a result, it was estimated that SBP/DBP increased 15.2/8.5 mmHg in the presence of highly stressful negative emotions. In conclusion, self-measurement of BP monitoring with a wearable device for multiple days is a feasible method to detect daily stress-induced BP elevation in working adults.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Munakata M. Clinical significance of stress-related increase in blood pressure: current evidence in office and out-of-office settings. Hypertens Res. 2018;41:553–69.
Mukkamala R, Yavarimanesh M, Natarajan K, Hahn JO, Kyriakoulis KG, Avolio AP, et al. Evaluation of the accuracy of cuffless blood pressure measurement devices: challenges and proposals. Hypertension. 2021;78:1161–7.
Kario K. Management of hypertension in the digital era: small wearable monitoring devices for remote blood pressure monitoring. Hypertension. 2020;76:640–50.
Kuwabara M, Harada K, Hishiki Y, Kario K. Validation of two watch-type wearable blood pressure monitors according to the ANSI/AAMI/ISO81060-2:2013 guidelines: Omron HEM-6410T-ZM and HEM-6410T-ZL. J Clin Hypertens (Greenwich). 2019;21:853–8.
Kario K, Shimbo D, Tomitani N, Kanegae H, Schwartz JE, Williams B. The first study comparing a wearable watch-type blood pressure monitor with a conventional ambulatory blood pressure monitor on in-office and out-of-office settings. J Clin Hypertens (Greenwich). 2020;22:135–41.
Tomitani N, Hoshide S, Kario K. Self-measured worksite blood pressure and its association with organ damage in working adults: Japan Morning Surge Home Blood Pressure (J-HOP) worksite study. J Clin Hypertens (Greenwich). 2021;23:53–60.
Tomitani N, Kanegae H, Suzuki Y, Kuwabara M, Kario K. Stress-induced blood pressure elevation self-measured by a wearable watch-type device. Am J Hypertens. 2021;34:377–82.
Kario K, Tomitani N, Morimoto T, Kanegae H, Lacy P, Williams B. Relationship between blood pressure repeatedly measured by a wrist-cuff oscillometric wearable blood pressure monitoring device and left ventricular mass index in working hypertensive patients. Hypertens Res. 2022;45:87–96.
Vaessen T, Rintala A, Otsabryk N, Viechtbauer W, Wampers M, Claes S, et al. The association between self-reported stress and cardiovascular measures in daily life: a systematic review. PLoS One. 2021;16:e0259557.
Kario K, Schwartz JE, Gerin W, Robayo N, Maceo E, Pickering TG. Psychological and physical stress-induced cardiovascular reactivity and diurnal blood pressure variation in women with different work shifts. Hypertens Res. 2002;25:543–51.
Campbell J, Ehlert U. Acute psychosocial stress: does the emotional stress response correspond with physiological responses? Psychoneuroendocrinology. 2012;37:1111–34.
El Sayed K, Macefield VG, Hissen SL, Joyner MJ, Taylor CE. Rate of rise in diastolic blood pressure influences vascular sympathetic response to mental stress. J Physiol. 2016;594:7465–82.
Gordon AM, Mendes WB. A large-scale study of stress, emotions, and blood pressure in daily life using a digital platform. Proc Natl Acad Sci USA. 2021;118:e2105573118.
Kamarck TW, Li X, Wright AGC, Muldoon MF, Manuck SB. Ambulatory blood pressure reactivity as a moderator in the association between daily life psychosocial stress and carotid artery atherosclerosis. Psychosom Med. 2018;80:774–82.
Birk JL, Cornelius T, Edmondson D, Schwartz JE. Duration of perseverative thinking as related to perceived stress and blood pressure: an ambulatory monitoring study. Psychosom Med. 2019;81:603–11.
Coccina F, Pierdomenico AM, Pizzicannella J, Ianni U, Bufano G, Madonna R, et al. Prognostic value of daytime and nighttime blood pressure in treated hypertensive patients according to age and sex. J Clin Hypertens (Greenwich) 2020;22:2014–21.
Triantafyllidi H, Benas D, Schoinas A, Birmpa D, Trivilou P, Varytimiadi E, et al. Hypertension-mediated organ damage regression associates with blood pressure variability improvement three years after successful treatment initiation in essential hypertension. J Clin Hypertens (Greenwich). 2021;23:1150–8.
Kario K. Evidence and perspectives on the 24-hour management of hypertension: hemodynamic biomarker-initiated ‘anticipation medicine’ for zero cardiovascular event. Prog Cardiovasc Dis. 2016;59:262–81.
Acknowledgements
The HeartGuide device was supplied by Omron Healthcare Co., Ltd., which also provided funding for the study. However, the collection and analysis of data in this study were conducted entirely independently of Omron Healthcare Co., Ltd.
Funding
This study was financially supported by Omron Healthcare. However, Omron Healthcare had no role in the data collection or analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KK has received research grants from Omron Healthcare, A&D, and Fukuda Denshi. NT was the recipient of a JSPS KAKENHI grant (no. 20K17127).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Tomitani, N., Kanegae, H. & Kario, K. Self-monitoring of psychological stress-induced blood pressure in daily life using a wearable watch-type oscillometric device in working individuals with hypertension. Hypertens Res 45, 1531–1537 (2022). https://doi.org/10.1038/s41440-022-00946-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-00946-9
Keywords
This article is cited by
-
History and evolution of blood pressure measurement
Clinical Hypertension (2024)
-
Could wristwatch-type wearable oscillometric blood pressure monitoring be a third option for out-of-office blood pressure monitoring?
Hypertension Research (2024)
-
How do we tackle nighttime blood pressure?
Hypertension Research (2023)
-
The effect of psychological stress and physical activity on ambulatory blood pressure variability detected by a multisensor ambulatory blood pressure monitoring device
Hypertension Research (2023)
-
Evidence for the surge blood pressure resonance hypothesis as a trigger for cardiovascular disease events
Hypertension Research (2023)