Abstract
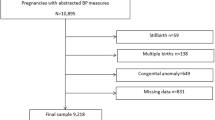
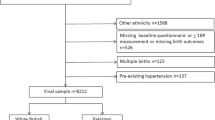
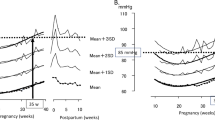
To investigate the potential associations between visit-to-visit blood pressure variability (VVV) and adverse birth outcomes in pregnancies, 48,209 pregnant women without proteinuria or chronic hypertension before 20 weeks of gestation who delivered live singletons between January 2014 and November 2019 in Taizhou or Taicang cities were recruited. VVV was estimated as the standard deviation and coefficient of variation of blood pressure [i.e., systolic blood pressure (SBP), diastolic blood pressure (DBP) and mean arterial pressure (MAP)] measured from 20 weeks of gestation onwards. Pregnant women were classified into four groups according to the corresponding quartiles for each VVV index. It was found that VVV was significantly higher in women with small for gestational age (SGA) or low birth weight (LBW) infants than in their counterparts. Graded associations between VVV categories and poor birth outcomes were observed. In particular, when comparing the women with the highest to the lowest quartiles of standard deviation and coefficient variation of DBP, the odds ratios (95% confidence interval) for SGA was 1.15 (1.06–1.26) and 1.14 (1.05–1.25), respectively. Interestingly, the addition of DBP-VVV to established risk factors improved risk prediction of SGA; DBP-VVV demonstrated modestly superior predictive performance to VVV obtained from SBP or MAP. Similar results were found even among normotensive pregnancies. Our findings indicated that VVV during pregnancy, especially DBP-VVV, was independently associated with poor birth outcomes of pregnancies in East China. The inclusion of DBP-VVV with established risk factors may help in identifying pregnancies at high risk of SGA. Validations are needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Lees C, Marlow N, Arabin B, Bilardo CM, Brezinka C, Derks JB, et al. Perinatal morbidity and mortality in early-onset fetal growth restriction: cohort outcomes of the trial of randomized umbilical and fetal flow in Europe (TRUFFLE). Ultrasound Obstet Gynecol. 2013;42:400–8.
Crispi F, Bijnens B, Figueras F, Bartrons J, Eixarch E, Noble FL, et al. Fetal growth restriction results in remodeled and less efficient hearts in children. Circulation. 2010;121:2427–36.
Ohkuchi A, Hirashima C, Arai R, Takahashi K, Suzuki H, Ogoyama M, et al. Temporary hypertension and white coat hypertension in the first trimester as risk factors for preeclampsia. Hypertens Res. 2019;42:2002–12.
Magee LA, Pels A, Helewa M, Rey E, von Dadelszen P. Diagnosis, evaluation, and management of the hypertensive disorders of pregnancy: executive summary. J Obstet Gynaecol Can. 2014;36:416–41.
Bramham K, Parnell B, Nelson-Piercy C, Seed P, Poston L, Chappell L. Chronic hypertension and pregnancy outcomes: systematic review and meta-analysis. BMJ (Clin Res ed). 2014;348:g2301.
Zhu B, Huang K, Bao W, Yan S, Hao J, Zhu P, et al. Dose-response relationship between maternal blood pressure in pregnancy and risk of adverse birth outcomes: Ma’anshan birth cohort study. Pregnancy Hypertens. 2019;15:16–22.
Roberts L, Chaemsaithong P, Sahota DS, Nicolaides KH, Poon LCY. Protocol for measurement of mean arterial pressure at 10-40weeks’ gestation. Pregnancy Hypertens. 2017;10:155–60.
Wright A, Wright D, Ispas CA, Poon LC, Nicolaides KH. Mean arterial pressure in the three trimesters of pregnancy: effects of maternal characteristics and medical history. Ultrasound Obstet Gynecol. 2015;45:698–706.
Bakalis S, Stoilov B, Akolekar R, Poon LC, Nicolaides KH. Prediction of small-for-gestational-age neonates: screening by uterine artery Doppler and mean arterial pressure at 30-34 weeks. Ultrasound Obstet Gynecol. 2015;45:707–14.
Tan EK, Tan EL. Alterations in physiology and anatomy during pregnancy. Best Pract Res Clin Obstet Gynaecol. 2013;27:791–802.
Hermida R, Ayala D, Iglesias M. Predictable blood pressure variability in healthy and complicated pregnancies. Hypertension. 2001;38:736–41.
Melchiorre K, Sharma R, Khalil A, Thilaganathan B. Maternal cardiovascular function in normal pregnancy: evidence of maladaptation to chronic volume overload. Hypertension. 2016;67:754–62.
Grindheim G, Estensen M, Langesaeter E, Rosseland L, Toska K. Changes in blood pressure during healthy pregnancy: a longitudinal cohort study. J Hypertension. 2012;30:342–50.
Y Y, JP R, CE L, S S, MJ P, K B-D, et al. Association of blood pressure patterns in young adulthood with cardiovascular disease and mortality in middle age. JAMA Cardiol. 2020; https://doi.org/10.1001/jamacardio.2019.5682.
Nwabuo CC, Yano Y, Moreira HT, Appiah D, Vasconcellos HD, Aghaji QN, et al. Association between visit-to-visit blood pressure variability in early adulthood and myocardial structure and function in later life. JAMA Cardiol. 2020; https://doi.org/10.1001/jamacardio.2020.0799.
Kasim HH, Masri MA, Noh NA, Mokhtar A, Mokhtar RH. Clinical implications of blood pressure variability (BPV) in pregnancies: a review. Horm Mol Biol Clin Investig. 2019;39:1–13.
Hermida RC, Ayala DE. Prognostic value of ambulatory blood pressure measurements for the diagnosis of hypertension in pregnancy. Expert Rev Cardiovasc Ther. 2004;2:375–91.
Faber R, Baumert M, Stepan H, Wessel N, Voss A, Walther T. Baroreflex sensitivity, heart rate, and blood pressure variability in hypertensive pregnancy disorders. J Hum Hypertens. 2004;18:707–12.
Flood P, McKinley P, Monk C, Muntner P, Colantonio LD, Goetzl L, et al. Beat-to-beat heart rate and blood pressure variability and hypertensive disease in pregnancy. Am J Perinatol. 2015;32:1050–8.
Jieyu L, Yingying C, Tian G, Jiaxiang W, Jiawen L, Yingjie G, et al. Visit-to-visit blood pressure variability is associated with gestational hypertension and pre-eclampsia. Pregnancy Hypertens. 2019;18:126–31.
Magee L, Singer J, Lee T, McManus R, Lay-Flurrie S, Rey E, et al. Are blood pressure level and variability related to pregnancy outcome? Analysis of control of hypertension in pregnancy study data. Pregnancy Hypertens. 2020;19:87–93.
Kim S, Lee J, Park J. Differences in visit-to-visit blood pressure variability between normotensive and hypertensive pregnant women. Hypertens Res. 2019;42:67–74.
H SC, R PM. Reproducibility of measures of visit-to-visit variability in blood pressure after transient ischaemic attack or minor stroke. Cerebrovasc Dis. 2009;28:331–40.
Ohkuma T, Woodward M, Jun M, Muntner P, Hata J, Colagiuri S, et al. Prognostic value of variability in systolic blood pressure related to vascular events and premature death in type 2 diabetes mellitus: the ADVANCE-ON study. Hypertension. 2017;70:461–8.
Liu J, Tao L, Cao Y, Teng H, Wang J, Wang M, et al. Stage 1 hypertension defined by the 2017 American College of Cardiology/American Heart Association guideline and risk of adverse birth outcomes in Eastern China. J Hypertens. 2020;38:1090–102.
Brown M, Buddle M, Farrell T, Davis G, Jones M. Randomised trial of management of hypertensive pregnancies by Korotkoff phase IV or phase V. Lancet. 1998;352:777–81.
Australia. NHFo. Hypertension management guide for doctors 2004. 2004; http://www.heartfoundation.org.au.
American college of Obstetricians and Gyneocologists. Hypertension in Pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. Obstet Gynecol. 2013;122:1122–31.
American Diabetes Association. Standards of medical care in diabetes-2013. Diabetes Care. 2013;36:S11–66.
WHO. Haemoglobin concentrations for the diagnosis of anaemia and assessment of severity. Edited by World Health Organization. 2011; http://apps.who.int/iris/bitstream/10665/85839/3/WHONMHNHD_MNM_11.1_eng.pdf.
Stagnaro-Green A, Abalovich M, Alexander E, Azizi F, Mestman J, Negro R, et al. Guidelines of the American Thyroid Association for the diagnosis and management of thyroid disease during pregnancy and postpartum. Thyroid. 2011;21:1081–125.
Spong C. Defining “term” pregnancy: recommendations from the Defining “Term” Pregnancy Workgroup. JAMA. 2013;309:2445–6.
ACoOa G. ACOG Committee Opinion No 579: definition of term pregnancy. Obstet Gynecol. 2013;122:1139–40.
Mikolajczyk R, Zhang J, Betran A, Souza J, Mori R, Gülmezoglu A, et al. A global reference for fetal-weight and birthweight percentiles. Lancet. 2011;377:1855–61.
Hughes M, Black R, Katz J. 2500-g low birth weight cutoff: history and implications for future research and policy. Matern Child Health J. 2017;21:283–9.
Pencina M, D’Agostino R, D’Agostino R, Vasan R. Evaluating the added predictive ability of a new marker: from area under the ROC curve to reclassification and beyond. Stat Med. 2008;27:157–72. discussion 207-112.
DeLong E, DeLong D, Clarke-Pearson D. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics. 1988;44:837–45.
Shimbo D, Shea S, McClelland RL, Viera AJ, Mann D, Newman J, et al. Associations of aortic distensibility and arterial elasticity with long-term visit-to-visit blood pressure variability: the Multi-Ethnic Study of Atherosclerosis (MESA). Am J Hypertens. 2013;26:896–902.
Song H, Wei F, Liu Z, Zhao Y, Ye L, Lu F, et al. Visit-to-visit variability in systolic blood pressure: correlated with the changes of arterial stiffness and myocardial perfusion in on-treated hypertensive patients. Clin Exp Hypertens. 2015;37:63–9.
Diaz KM, Veerabhadrappa P, Kashem MA, Feairheller DL, Sturgeon KM, Williamson ST, et al. Relationship of visit-to-visit and ambulatory blood pressure variability to vascular function in African Americans. Hypertens Res. 2012;35:55–61.
Rothwell P, Howard S, Dolan E, O’Brien E, Dobson J, Dahlöf B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet. 2010;375:895–905.
Shah D, Khalil R. Bioactive factors in uteroplacental and systemic circulation link placental ischemia to generalized vascular dysfunction in hypertensive pregnancy and preeclampsia. Biochemical Pharmacol. 2015;95:211–26.
Spinillo A, Gardella B, Adamo L, Muscettola G, Fiandrino G, Cesari S. Pathologic placental lesions in early and late fetal growth restriction. Acta Obstet Gynecol Scand. 2019;98:1585–94.
Gunnarsdottir J, Akhter T, Högberg U, Cnattingius S, Wikström A. Elevated diastolic blood pressure until mid-gestation is associated with preeclampsia and small-for-gestational-age birth: a population-based register study. BMC Pregnancy Childbirth. 2019;19:186.
Nobles CJ, Mendola P, Mumford SL, Naimi AI, Yeung EH, Kim K, et al. Preconception blood pressure levels and reproductive outcomes in a prospective cohort of women attempting pregnancy. Hypertension. 2018;71:904–10.
Nørgaard S, Vestgaard M, Jørgensen I, Ásbjörnsdóttir B, Ringholm L, McIntyre H, et al. Diastolic blood pressure is a potentially modifiable risk factor for preeclampsia in women with pre-existing diabetes. Diabetes Res Clin Pract. 2018;138:229–37.
Li Y, Wei FF, Wang S, Cheng YB, Wang JG. Cardiovascular risks associated with diastolic blood pressure and isolated diastolic hypertension. Curr Hypertens Rep. 2014;16:489.
Duvekot JJ, Cheriex EC, Pieters FA, Peeters LL. Severely impaired fetal growth is preceded by maternal hemodynamic maladaptation in very early pregnancy. Acta Obstet Gynecol Scand. 1995;74:693–7.
Ayala DE, Hermida RC, Mojón A, Fernández JR, Silva I, Ucieda R, et al. Blood pressure variability during gestation in healthy and complicated pregnancies. Hypertension. 1997;30:611–8.
Funding
This work is supported by a grant from the Jiangsu Commission of Health (Grant number: H2019010) and a grant from the Natural Science Foundation of the Jiangsu Higher Education Institutions of China and a Project of the Priority Academic Program Development of Jiangsu Higher Education Institutions (PAPD).
Author information
Authors and Affiliations
Contributions
JY contributed to the design and concept of the manuscript; JL and HT drafted the manuscript; LY, YC, LT, BZ, and FW helped in acquisition of the data; JW contributed to analysis and interpretation of the data; ZW and BH contributed to the revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Liu, J., Yang, L., Teng, H. et al. Visit-to-visit blood pressure variability and risk of adverse birth outcomes in pregnancies in East China. Hypertens Res 44, 239–249 (2021). https://doi.org/10.1038/s41440-020-00544-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-00544-7
Keywords
This article is cited by
-
Blood pressure variability correlates with right ventricular strain in women with gestational hypertension and preeclampsia
Journal of Human Hypertension (2022)
-
Annual reports on hypertension research 2020
Hypertension Research (2022)
-
Blood-pressure variability is associated with left-ventricular mechanics in patients with gestational hypertension and preeclampsia
Hypertension Research (2021)