Abstract
Purpose
Carney complex (CNC), is an autosomal dominant multiple neoplasia and lentiginosis syndrome. We aimed to identify risk factors associated with the occurrence and recurrence of cardiac myxomas, the predominant cause of death in CNC patients.
Methods
Patients with CNC were monitored prospectively between 1995 and 2020 for the development of cardiac myxomas.
Results
Of the 319 patients studied, 136 (42.6%) developed myxomas. The mean age at diagnosis was 28.7 ± 16.6 years in females and 25.0 ± 16.4 years in males. By age 30, 35% of females and 45% of males had at least one myxoma. The CNC-related lesions, lentigines, cutaneous, mucosal, or breast myxomas, thyroid nodules, pituitary adenoma, and schwannoma were significantly more frequent (all p < 0.05) among patients with myxomas. Forty-four percent of patients had recurrences; nearly all within the first 8 and 16 years for males and females, respectively. Recurrences were more common in females.
Conclusion
This is the largest study to date and provides the first-time risk estimates by age and gender for cardiac myxomas in CNC patients. Cardiac myxomas are common by age 30 and often recur, especially in women, but the risk drops in 10 to 20 years. These findings may guide patient counseling, screening intervals, and surgical approaches.
Clinical Trial Registration
Clinical Trial Registration: Defining the Genetic Basis for the Development of Primary Pigmented Nodular Adrenocortical Disease and the Carney complex, Registration number: NCT00001452 URL: https://clinicaltrials.gov/ct2/show/NCT00001452.
Similar content being viewed by others
INTRODUCTION
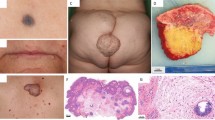
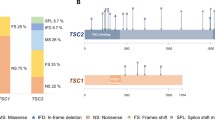
Carney complex (CNC) (OMIM 160980) is a rare multiple neoplasia and lentiginosis syndrome. It was initially described by Dr. J. Aidan Carney in 19851 as a “complex of myxomas, spotty skin pigmentation and endocrine overactivity,” and in 1986, it was named Carney complex.2 It is characterized by multiple endocrine and nonendocrine tumors, abnormal skin pigmentation and myxomas of the heart, breast, bone, skin, and mucosae, melanotic schwannoma, and a predisposition to various cancers, such as those developing in the thyroid, ovaries, pancreas, and liver.3 About 70% of CNC cases are familial, inherited in an autosomal dominant manner. Inactivating variants of the regulatory subunit type 1A of the cAMP–dependent protein kinase (PRKAR1A) gene at 17q22-24 (CNC 1 locus) are found in more than 70% of patients with CNC with almost 100% penetrance.3,4,5 A second locus has been mapped by genetic linkage analysis on the short arm of chromosome 2 (2p16) (CNC 2 locus).6,7 Finally, a copy-number gain of the short arm of chromosome 1 including the PRKACB gene was reported in a single case of a CNC patient who presented with skin pigmentation, acromegaly, and myxomas.8
Cardiac myxomas are rare in the general population, with an estimated incidence of 0.5–1 per million population per year,9,10 but common in patients with CNC. They are found in 20–40% of CNC patients.11 CNC-associated cardiac myxomas constitute the predominant cause of death among these patients; they tend to be multiple and may occur as early as at birth.4 Among patients with CNC, recurrence of myxomas has been associated with excess of growth hormone secretion.12
We reviewed data from the largest cohort of its kind with a worldwide collection of records of CNC patients with and without cardiac myxoma. Our objective was to identify risk factors that could predispose to the occurrence and recurrence of cardiac myxomas and provide evidence-based recommendations regarding the follow-up of CNC patients.
MATERIALS AND METHODS
Ethics statement
The research protocol was approved by the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD) (1995–2011) and the National institute of Diabetes and Digestive and Kidney Diseases (NIDDK) Institutional Review Boards (2012–2020). Patients who were diagnosed with CNC and participated in the clinical protocol 95-CH-0059 were included in the analysis. Patients were enrolled and screened in this study from 19953,6 to 2020. For genetic testing and for all CNC-related research, patients and their parents gave written informed consent; younger patients signed assent when appropriate.
Clinical studies
The study population consisted of two main groups of CNC patients: (1) patients who have been diagnosed, treated, and followed up at the National Institutes of Health (NIH) and (2) patients who were referred to NIH from around the world. Clinical information for all patients, including detailed hospital records, echocardiograms, cardiac magnetic resonance imaging (MRI) reports, and family history, were collected and reviewed. All patients that met the criteria for CNC (Table 1) were identified and reviewed. Of them, 319 patients fulfilled the criteria and were included in the study. All patients that were included in the study underwent echocardiography and a subset of them (n = 35) had cardiovascular magnetic resonance imaging (MRI) as part of the initial assessment and/or routine follow-up.
Statistical analysis
Data were described using frequency distributions for categorical variables and mean ± SD were calculated for continuous variables. The presence of other stigmata of the syndrome in patients with and without cardiac myxoma was assessed using logistic regression models for repeated binary outcome to account for dependence between family members. The distribution of age at first diagnosis of myxoma, as well as the distribution of time to recurrence of myxoma, were assessed using Kaplan–Meier survival curves. We calculated the Kaplan–Meier curve for age at first observed myxoma by randomly selecting one individual from each family cluster in the sample (to have an independent sample of individuals): each family was represented with either the first observed myxoma or a randomly selected myxoma free family member. The association between gender of the patients with their time to first occurrence of myxoma, as well as time to recurrence of myxoma, was assessed using Cox’s proportional hazards regression model with frailty to account for dependence between family members. Hazard ratios less than 1 indicate reduced risk and greater than 1 indicate increased risks for myxoma. Statistical significance was set at p < 0.05. Data analysis was performed by SAS 9.4 and R 3.6.
RESULTS
Over the study period, 136 of the 319 CNC (42.6%) patients developed at least one cardiac myxoma. A total of 78 patients with cardiac myxomas (57.3%) were females. The patients who had a PRKAR1A variant (n = 289) were not significantly more likely to have a myxoma compared with those without a PRKAR1A variant (n = 21) (p = 0.183). We also had nine patients with unknown genetics, because they had not been tested. The summary of all additional findings of CNC in these patients are shown in Table 2.
In 42 (30.8%) of 136 patients the initial location was uncertain. In 11 of them, the initial evaluation revealed myxomas in multiple locations. In those cases in which the location was known, a total of 104 tumors, 86 (82.7%) were found in the atrium, 55 (64%) in the left atrium (LA), 14 in the right atrium (RA), and 17 in the atrium not otherwise specified. In the ventricle, 18 tumors were identified: 10 in the left ventricle (LV), 7 in the right ventricle (RV), and 1 not otherwise specified.
The mean age at the detection of a patient’s initial cardiac myxoma was 28.7 years (SD = ±14.65) for females and 25.0 years (SD = ±16.42) for males (Table 3). The first event occurred at a later age in women compared with men (frailty Cox model, p < 0.0001) (Fig. 1); as a sensitivity analysis, the Kaplan–Meier curve for Fig. 1 was recalculated multiple times with repeat sampling and similar curves were observed (results not shown). However, first recurrences occurred sooner in women compared with men (frailty Cox model, p = 0.013) (Fig. 2). In addition, women were 65% less likely to get a myxoma for the first time (frailty Cox model, p < 0.0001, 95% confidence interval [CI]: 0.226, 0.564), but 2.5 times more likely to get a recurrence compared with men (frailty Cox model, p = 0.013, 95% CI: 1.21, 5.31).
At least one recurrent event happened in 60 patients (44%) and of them, 44 (73.3%) were females. In 35 patients, the recurrent cardiac myxoma was in the same location as in the initial tumor (22 of which were in LA), in 13 it was in a new location (6 of which were in LA), and in 12 the exact location was uncertain. The mean number of years to first recurrence in all chambers was 4.2 years (SD = ±3.5 years). A second recurrence took place in 21 patients, a third recurrence in 8 patients, and a fourth recurrence in 4 patients. Data from 35 cardiac MRIs revealed the most common location to be at the interatrial septum (16/35 cases) followed by posterior/lateral free wall in 8 cases and the intraventricular septum in 5 cases.
In addition, we looked at various other manifestations of CNC to see if they might be useful to predict the presence of a myxoma and we found the following lesions to be significantly more frequent (all p values < 0.05) in those with myxomas than in those without myxomas: skin or mucosal lentigines, cutaneous or mucosal myxomas, breast myxomatosis, thyroid lesions, pituitary adenomas, and psammomatous melanotic schwannomas (Table 2). No significant differences were found in the presence of other features of CNC. Between patients that had only once cardiac myxoma and those with at least one recurrence, no significant statistical differences were found in the presence of the previous features (Table 2); however, the numbers were small. These numbers are likely to underestimate the true incidence of these manifestations because, for example, not every skin lesion in every patient was biopsied and MRI of the breast was not performed in all women.
DISCUSSION
This study is one of the largest of its kind to date. First, a recurrence of the myxoma occurred in 44% of our patients, a number much higher than reported before; the incidence of a recurrence ranged between 10% and 22% in previous studies.13,14 In addition, our study reports the incidence of a cardiac myxoma in CNC patients, as well as its first recurrence based on their gender. The overall risk of developing the tumor by the age of 30 years was shown to be up to 35% for females and 45% for males, with an increasing risk over time (i.e., by the age of 45, 65% of females and 70% of males had at least one tumor [p < 0.0001]) (Fig. 1).
A striking finding of our study is that the first event occurred significantly later in women compared with men; however, over the observed duration of follow-up, nearly all recurrences occurred earlier in women compared with men (Fig. 2). In addition, a recurrent event rarely happened more than 8 years after the initial occurrence in men and 17 years in women. These findings have significant clinical implications for the follow-up of patients with CNC; i.e., in men, follow-up may be needed more frequently for the first 8 years after the initial event.
Cardiac myxomas in patients with CNC are of great concern because they can cause intracardiac obstruction, strokes due to the formation of emboli, and sudden death.12,15 When cardiac myxomas recur frequently, they may require heart transplantation in a number of patients.16 They are the leading cause of death in patients with CNC.3,17,18 In our population, 42.6% of the patients with CNC developed a cardiac tumor, which is a higher number than what has previously been reported.3,4,19
In our study, in accordance with previous data,12 gender did not seem to play a role in the initial appearance of a cardiac myxoma in CNC patients. This is in contrast to other smaller studies that showed a higher prevalence of myxomas in male patients with CNC.20 On the other hand, 73.3% of the cases that experienced a recurrence were females, pointing to a much higher probability of recurrence for women than men.
Thyroid involvement in CNC patients has been described before4,6,19,21,22 as a feature of the syndrome, ranging from benign lesions (i.e., follicular/nodular hyperplasia) to carcinoma.21,22 What is interesting in our findings is that thyroid gland manifestations occurred in 8.1% of CNC patients without cardiac myxoma versus 25.7% of CNC patients with cardiac myxoma (p = 0.001). In addition, breast myxomatosis was present in 9.7% versus 34.6% of CNC patients, without and with cardiac myxoma respectively (p = 0.008). Other interesting associations are shown in Table 2. In other words, it is more likely that a person will develop a cardiac myxoma if they had thyroid lesions or breast myxomas.
In terms of age, the highest incidence of a new tumor was in the second and third decade of life, in agreement with previous studies.3,10 However, our study also showed tumors presenting as early as at 4 years and as late as at 80 years of age. Regarding the location of the myxoma, atrial involvement was significantly higher than other sites; the atrial septum was the most frequent point of origin for the tumor, a finding that has been reported before.23
In conclusion, our study provides risk estimates by age and gender for cardiac myxomas in patients with CNC. The data are useful for clinicians, patients, and their families. Early diagnosis is vital and currently cardiac ultrasound is recommended annually or biannually (if prior myxoma history is present) for early detection of primary or recurrent tumor.15 Screening should begin in infancy with biannual echocardiograms. This may go until young adulthood. If there is prior history of cardiac myxoma, echocardiograms should be performed biannually for 20 years after the initial myxoma for both men and women at any age; after that time, surveillance may be performed every 12 months until the end of life. Although recurrences are rarer in older age as this study demonstrates, an annual echocardiogram for all patients with CNC for the rest of their lives is a small price to pay for preventing the dire consequences of a tumor that could have been excised.
References
Carney JA, Gordon H, Carpenter PC, Shenoy BV, Go VL. The complex of myxomas, spotty pigmentation, and endocrine overactivity. Medicine (Baltimore). 1985;64:270–283.
Bain J. “Carney’s complex”. Mayo Clin Proc. 1986;61:508.
Stratakis CA, Kirschner LS, Carney JA. Clinical and molecular features of the Carney complex: diagnostic criteria and recommendations for patient evaluation. J Clin Endocrinol Metab. 2001;86:4041–4046.
Bertherat J, Horvath A, Groussin L, et al. Mutations in regulatory subunit type 1A of cyclic adenosine 5’-monophosphate-dependent protein kinase (PRKAR1A): phenotype analysis in 353 patients and 80 different genotypes. J Clin Endocrinol Metab. 2009;94:2085–2091.
Stratakis CA. Mutations of the gene encoding the protein kinase A type I-alpha regulatory subunit (PRKAR1A) in patients with the “complex of spotty skin pigmentation, myxomas, endocrine overactivity, and schwannomas” (Carney complex). Ann N Y Acad Sci. 2002;968:3–21.
Stratakis CA, Carney JA, Lin JP, et al. Carney complex, a familial multiple neoplasia and lentiginosis syndrome. Analysis of 11 kindreds and linkage to the short arm of chromosome 2. J Clin Invest. 1996;97:699–705.
Matyakhina L, Pack S, Kirschner LS, et al. Chromosome 2 (2p16) abnormalities in Carney complex tumours. J Med Genet. 2003;40:268–277.
Forlino A, Vetro A, Garavelli L, et al. PRKACB and Carney complex. N Engl J Med. 2014;370:1065–1067.
Sarjeant JM, Butany J, Cusimano RJ. Cancer of the heart: epidemiology and management of primary tumors and metastases. Am J Cardiovasc Drugs. 2003;3:407–421.
Briassoulis G, Kuburovic V, Xekouki P, et al. Recurrent left atrial myxomas in Carney complex: a genetic cause of multiple strokes that can be prevented. J Stroke Cerebrovasc Dis. 2012;21:914 e911–918.
Espiard S, Bertherat J. Carney complex. Front Horm Res. 2013;41:50–62.
Bandettini WP, Karageorgiadis AS, Sinaii N, et al. Growth hormone and risk for cardiac tumors in Carney complex. Endocr Relat Cancer. 2016;23:739–746.
Kwon OY, Kim GJ, Jang WS, Lee YO, Cho JY, Lee JT. Fourth recurrence of cardiac myxoma in a patient with the Carney complex. Korean J Thorac Cardiovasc Surg. 2016;49:119–121.
Mahilmaran A, Seshadri M, Nayar PG, Sudarsana G, Abraham KA. Familial cardiac myxoma: Carney’s complex. Tex Heart Inst J. 2003;30:80–82.
Stratakis CA, Raygada M. Carney complex. In: Adam MP, Ardinger HH, Pagon RA, et al., editors. GeneReviews. Seattle: University of Washington; 1993.
Gammie JS, Abrishamchian AR, Griffith BP. Cardiac autotransplantation and radical bi-atrial resection for recurrent atrial myxoma. Ann Thorac Surg. 2007;83:1545–1547.
Roselli EE. Reoperative cardiac surgery: challenges and outcomes. Tex Heart Inst J. 2011;38:669–671.
Russell JL, LeBlanc JG, Sett SS, Potts JE. Risks of repeat sternotomy in pediatric cardiac operations. Ann Thorac Surg. 1998;66:1575–1578.
Espiard S, Vantyghem MC, Assie G, et al. Frequency and Incidence of Carney complex manifestations: a prospective multicenter study with a three-year follow-up. J Clin Endocrinol Metab. 2020;105:dgaa002.
Carney JA. Differences between nonfamilial and familial cardiac myxoma. Am J Surg Pathol. 1985;9:53–55.
Stratakis CA, Courcoutsakis NA, Abati A, et al. Thyroid gland abnormalities in patients with the syndrome of spotty skin pigmentation, myxomas, endocrine overactivity, and schwannomas (Carney complex). J Clin Endocrinol Metab. 1997;82:2037–2043.
Carney JA, Lyssikatos C, Seethala RR, et al. The spectrum of thyroid gland pathology in Carney complex: the importance of follicular carcinoma. Am J Surg Pathol. 2018;42:587–594.
Wang H, Li Q, Xue M, Zhao P, Cui J. Cardiac myxoma: a rare case series of 3 patients and a literature review. J Ultrasound Med. 2017;36:2361–2366.
Kamilaris CDC, Faucz FR, Voutetakis A, Stratakis CA. Carney complex. Exp Clin Endocrinol Diabetes. 2019;127:156–164.
Acknowledgements
We would like to thank all of the Carney complex patients and their families for participating in this study. This work was supported by the research project Z01-HD008920 (principal investigator: C.A.S.) of the Intramural Research Program of the Eunice Kennedy Shriver National Institute of Child Health & Human Development (NICHD), National Institutes of Health (NIH) (Bethesda, MD, USA). The funding source had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; or preparation, review, or approval of the manuscript.
Disclosure
C.A.S. holds patents on technologies involving PRKAR1A and related genes; his laboratory has also received research funding support by Pfizer Inc. for work unrelated to this subject investigation. The other authors declare no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pitsava, G., Zhu, C., Sundaram, R. et al. Predicting the risk of cardiac myxoma in Carney complex. Genet Med 23, 80–85 (2021). https://doi.org/10.1038/s41436-020-00956-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41436-020-00956-3
Keywords
This article is cited by
-
Cardiac myxomas: causes, presentations, diagnosis, and management
Irish Journal of Medical Science (1971 -) (2024)
-
A polo ball in the right atrium, importance of echocardiographic characteristics of intracardiac myxomas: a case report
Journal of Medical Case Reports (2023)
-
The benign nature and rare occurrence of cardiac myxoma as a possible consequence of the limited cardiac proliferative/ regenerative potential: a systematic review
BMC Cancer (2023)
-
Carney complex- why thorough medical history taking is so important - report of three cases and review of the literature
Endocrine (2022)
-
The need for tumor surveillance of children and adolescents with cancer predisposition syndromes: a retrospective cohort study in a tertiary-care children’s hospital
European Journal of Pediatrics (2022)