Abstract
Introduction
Retinopathy of prematurity (ROP) is a vision-threatening disease of premature infants. Practice guidelines recommend that all infants screened for ROP receive follow-up eye examinations to screen for ophthalmic complications.1 The purpose of this study was to identify risk factors for the development of strabismus, amblyopia, high refractive error, and cataracts among ROP-screened, non-treated infants.
Methods
Retrospective single-centre study of ROP-screened, non-treated premature infants with ophthalmic follow-up. Clinical variables were screened for association with ocular findings at follow-up. Multivariable logistic regression was used to determine the risk factors associated with ocular findings.
Results
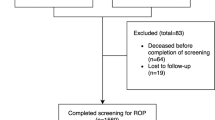
309 patients were seen for follow-up at 0.97 (0.69) [mean (SD)] years after neonatal intensive care unit (NICU) discharge. Strabismus was predicted by occipitofrontal circumference (OFC) z-score at NICU discharge (OR 0.61; 95% CI [0.42, 0.88]; p = 0.008), intraventricular haemorrhage (IVH) grade III or IV (OR 3.18; 95% CI [1.18, 8.54]; p = 0.02), and exclusive formula feeding at NICU discharge (OR 2.20; 95% CI [1.07, 4.53]; p = 0.03). Significant predictors of amblyopia were OFC z-score at discharge (OR 0.55; 95% CI [0.31, 0.96]; p = 0.03) and necrotising enterocolitis (NEC) (OR 6.94; 95% CI [1.38, 35.00]; p = 0.02). NEC was a significant risk factor for high refractive error (OR 7.27; 95% CI [1.39, 37.94]; p = 0.02).
Conclusions
Among premature infants screened but not treated for ROP, severe IVH, NEC, low OFC z-score, and exclusive formula feeding at NICU discharge were risk factors for ocular morbidity. These findings affirm the value of ophthalmic follow-up for all ROP-screened infants, particularly those with the identified risk factors.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Fierson WM.American Academy Of Pediatrics Section On Ophthalmology, American Academy Of Ophthalmology. et al. Screening examination of premature infants for retinopathy of prematurity. Pediatrics. 2018;142:e20183061 10.1542/peds.2018-3061.
Holmström GE, Källen K, Hellström A, Jakobsson PG, Serenius F, Stjernqvist K. et al. Ophthalmologic outcome at 30 months’ corrected age of a prospective Swedish cohort of children born before 27 weeks of gestation: the extremely preterm infants in Sweden study. JAMA Ophthalmol. 2014;132:182–9.https://doi.org/10.1001/jamaophthalmol.2013.5812.
Gulati S, Andrews CA, Apkarian AO, Musch DC, Lee PP, Stein JD. The impact of gestational age and birth weight on the risk of strabismus among premature infants. JAMA Pediatr. 2014;168:850–6. https://doi.org/10.1001/jamapediatrics.2014.946
Tolia VN, Ahmad KA, Jacob J, Kelleher AS, McLane N, Arnold RW. et al. Two-year outcomes of infants with stage 2 or higher retinopathy of prematurity: results from a large multicenter registry. Am J Perinatol. 2020;37:196–203.https://doi.org/10.1055/s-0039-1694983.
Kemper AR, Freedman SF, Wallace DK. Retinopathy of prematurity care: patterns of care and workforce analysis. J AAPOS. 2008;12:344–8. https://doi.org/10.1016/j.jaapos.2008.02.012
Jacob J, Matrix Z, Skopec D, Ticho B, Arnold RW. Factors associated with retinopathy of prematurity ophthalmology workload. J Perinatol. 2018;38:1588–93. https://doi.org/10.1038/s41372-018-0212-x
Kemper AR, Wallace DK. Neonatologists’ practice and experience in arranging retinopathy of prematurity screening services. Pediatrics. 2007;120:527–31. https://doi.org/10.1542/peds.2007-0378
Wade KC, Ying G, Baumritter A, Gong A, Kemper AR, Quinn GE. Factors in premature infants associated with low risk of developing retinopathy of prematurity. JAMA Ophthalmol. 2019;137:160–6. https://doi.org/10.1001/jamaophthalmol.2018.5520
Löfqvist C, Engström E, Sigurdsson J, Hård AL, Niklasson A, Ewald U. et al. Postnatal head growth deficit among premature infants parallels retinopathy of prematurity and insulin-like growth factor-1 deficit. Pediatrics. 2006;117:1930–8. https://doi.org/10.1542/peds.2005-1926.
Binenbaum G, Ying G, Quinn GE, Huang J, Dreiseitl S, Antigua J. et al. The CHOP postnatal weight gain, birth weight, and gestational age retinopathy of prematurity risk model. Arch Ophthalmol. 2012;130:1560–5. https://doi.org/10.1001/archophthalmol.2012.2524.
Wright KW, Edelman PM, Walonker F, Yiu S. Reliability of fixation preference testing in diagnosing amblyopia. Arch Ophthalmol. 1986;104:549–53. https://doi.org/10.1001/archopht.1986.01050160105023
Wallace DK, Morse CL, Melia M, Sprunger DT, Repka MX, Lee KA. et al. Pediatric eye evaluations preferred practice pattern®. Ophthalmology. 2018;125:P184–P227. https://doi.org/10.1016/j.ophtha.2017.09.032.
Fenton TR, Kim JH. A systematic review and meta-analysis to revise the Fenton growth chart for preterm infants. BMC Pediatrics. 2013;13:59 https://doi.org/10.1186/1471-2431-13-59
Benjamini Y, Hochberg Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc Ser B (Methodol).1995;57:289–300.
Bae SP, Kim EK, Yun J, Yoon YM, Shin SH, Park SY. Retinopathy of prematurity requiring treatment is closely related to head growth during neonatal intensive care unit hospitalization in very low birth weight infants. Neonatology. 2022;119:176–83. https://doi.org/10.1159/000519714
Gale CR. Critical periods of brain growth and cognitive function in children. Brain. 2004;127:321–9. https://doi.org/10.1093/brain/awh034
Phillips J, Christiansen SP, Ware G, Landers S, Kirby RS. Ocular morbidity in very low birth-weight infants with intraventricular hemorrhage. Am J Ophthalmol. 1997;123:218–23. https://doi.org/10.1016/S00029394(14)71039-6
O’Keefe M, Kafil-Hussain N, Flitcroft I, Lanigan B. Ocular significance of intraventricular haemorrhage in premature infants. Br J Ophthalmol. 2001;85:357–9. https://doi.org/10.1136/bjo.85.3.357
Khanna S, Sharma A, Ghasia F, Tychsen L. Prevalence of the infantile strabismus complex in premature children with and without periventricular leukomalacia. Am J Ophthalmol. 2022;240:342–51.https://doi.org/10.1016/j.ajo.2022.03.028
Fundora JB, Binenbaum G, Tomlinson L, Yu Y, Ying GS, Maheshwari A. et al. Association of surgical necrotizing enterocolitis and its timing with retinopathy of prematurity. Am J Perinatol. 2023;11:1178–84. 10.1055/s-0041-1733785.
Goldstein GP, Leonard SA, Kan P, Koo EB, Lee HC, Carmichael SL. Prenatal and postnatal inflammation-related risk factors for retinopathy of prematurity. J Perinatol. 2019;39:964–73.https://doi.org/10.1038/s41372-019-0357-2
Fang JL, Sorita A, Carey WA, Colby CE, Murad MH, Alahdab F. Interventions to prevent retinopathy of prematurity: a meta-analysis. Pediatrics. 2016;137:e20153387. https://doi.org/10.1542/peds.2015-3387
Yang Z, Lu Z, Shen Y, Chu T, Pan X, Wang C. et al. Prevalence of and factors associated with astigmatism in preschool children in Wuxi City, China. BMC Ophthalmol. 2022;22:146. https://doi.org/10.1186/s12886-022-02358-2.
Fieß A, Kölb-Keerl R, Schuster AK, Knuf M, Kirchhof B, Muether PS. et al. Prevalence and associated factors of strabismus in former preterm and fullterm infants between 4 and 10 Years of age. BMC Ophthalmol. 2017;17:228. https://doi.org/10.1186/s12886-017-0605-1.
Altobelli E, Angeletti PM, Verrotti A, Petrocelli R. The impact of human milk on necrotizing enterocolitis: a systematic review and meta-analysis. Nutrients. 2020;12:1322. https://doi.org/10.3390/nu12051322
Hong EH, Shin YU, Bae GH, Choi YJ, Ahn SJ, Kim I. et al. Ophthalmic complications in retinopathy of prematurity in the first decade of life in Korea using the national health insurance database. Sci Rep. 2022;12:911. https://doi.org/10.1038/s41598-021-04616-7.
Acknowledgements
We thank members of Department of Paediatrics and the Department of Ophthalmology and Visual Science for their collaboration on this project. Thank you to Gina Myers, RN, for her assistance in data collection and to Hongjie Gu for advice on statistical analysis.
Funding
This project was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health under Award Number TL1TR002344, the Doris Duke Charitable Foundation Fund to Retain Clinical Scientists under Grant 2020144, and an Unrestricted Grant from Research to Prevent Blindness. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
JIS contributed to designing the study, conducting the chart review, extracting and analysing data, interpreting results, and writing the manuscript. RR contributed to designing the study, interpreting results, and writing the manuscript. SM contributed to designing the study, conducting the chart review, extracting and analysing data. GL contributed to designing the study and writing the manuscript. AL contributed to designing the study and writing the manuscript. MMR contributed to designing the study, extracting and analysing data, interpreting results, and writing the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Strelnikov, J.I., Rao, R., Majidi, S. et al. Retinopathy of prematurity screening: prevalence and risk factors of ophthalmic complications in non-treated preterm infants. Eye (2024). https://doi.org/10.1038/s41433-023-02921-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41433-023-02921-1