Abstract
Background/Objectives
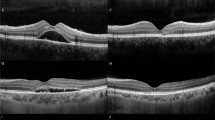
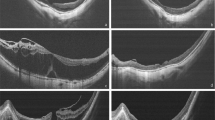
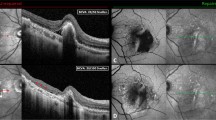
To analyse short-term changes of mean photoreceptor thickness (PRT) on the ETDRS-grid after vitrectomy and membrane peeling in patients with epiretinal membrane (ERM).
Subjects/Methods
Forty-eight patients with idiopathic ERM were included in this prospective study. Study examinations comprised best-corrected visual acuity (BCVA) and optical coherence tomography (OCT) before surgery, 1 week (W1), 1 month (M1) and 3 months (M3) after surgery. Mean PRT was assessed using an automated algorithm and correlated with BCVA and central retinal thickness (CRT).
Results
Regarding PRT changes of the study eye in comparison to baseline values, a significant decrease at W1 in the 1 mm, 3 mm and 6 mm area (all p-values < 0.001), at M1 (p = 0.009) and M3 (p = 0.019) in the central 1 mm area, a significant increase at M3 in the 6 mm area (p < 0.001), but no significant change at M1 in the 3 mm and 6 mm area and M3 in the 3 mm area (all p-values > 0.05) were observed. BCVA increased significantly from baseline to M3 (0.3LogMAR-0.15LogMAR, Snellen equivalent = 20/40-20/28 respectively; p < 0.001). There was no correlation between baseline PRT and BCVA at any visit after surgery, nor between PRT and BCVA at any visit (all p-values > 0.05). Decrease in PRT in the 1 mm (p < 0.001), 3 mm (p = 0.013) and 6 mm (p = 0.034) area after one week correlated with the increase in CRT (449.9 µm–462.2 µm).
Conclusions
Although the photoreceptor layer is morphologically affected by ERMs and after their surgical removal, it is not correlated to BCVA. Thus, patients with photoreceptor layer alterations due to ERM may still benefit from surgery and achieve good functional rehabilitation thereafter.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
Data are available from the authors upon reasonable request.
References
Bu SC, Kuijer R, Li XR, Hooymans JMM, Los LI. Idiopathic epiretinal membrane. In: Retina. 8th ed. Elsevier; 2014. p. 2317–35.
Scheerlinck LME, Van Der Valk R, Van Leeuwen R. Predictive factors for postoperative visual acuity in idiopathic epiretinal membrane: a systematic review. Acta Ophthalmol. 2015;93:203–12.
Mylonas G, Schranz M, Georgopoulos M, Sacu S, Deak G, Reumueller A, et al. Are there funduscopic and optical coherence tomography preoperative characteristics to predict surgical difficulty of epiretinal membrane removal? Curr Eye Res [Internet]. 8th ed. 2020;00:1–5. Available from: https://doi.org/10.1080/02713683.2020.1712425.
Govetto A, Virgili G, Rodriguez FJ, Figueroa MS, Sarraf D, Hubschman JP. Functional and anatomical significance of the ectopic inner foveal layers in eyes with idiopathic epiretinal membranes: surgical results at 12 months. In: Retina (Philadelphia, Pa). 8th ed. Elsevier; 2019. p. 347–57.
Datlinger F, Georgopoulos M, Aliyeva L, Meyer EL, Abela-Formanek C, Pollreisz A, et al. Postoperative movement of the fovea after successful surgery in patients with idiopathic epiretinal membranes. Retina 2021;41:510–5. https://doi.org/10.1097/IAE.0000000000002896.
Inoue M, Morita S, Watanabe Y, Kaneko T, Yamane S, Kobayashi S, et al. Inner segment/outer segment junction assessed by spectral-domain optical coherence tomography in patients with idiopathic epiretinal membrane. In: American Journal of Ophthalmology [Internet]. 8th ed. Elsevier; 2010. p. 834–9. Available from: https://www.sciencedirect.com/science/article/pii/S0002939410004307.
Oster SF, Mojana F, Brar M, Yuson RMS, Cheng L, Freeman WR. Disruption of the photoreceptor inner segment/outer segment layer on spectral domain-optical coherence tomography is a predictor of poor visual acuity in patients with epiretinal membranes. In: Retina. 8th ed. Elsevier; 2010. p. 713–8.
Michalewski J, Michalewska Z, Cisiecki S, Nawrocki J. Morphologically functional correlations of macular pathology connected with epiretinal membrane formation in spectral optical coherence tomography (SOCT). In: Graefe’s Archive for Clinical and Experimental Ophthalmology [Internet]. 8th ed. Elsevier; 2007. p. 1623–31. Available from: http://link.springer.com/10.1007/s00417-007-0579-4.
Suh MH, Seo JM, Park KH, Yu HG. Associations between macular findings by optical coherence tomography and visual outcomes after epiretinal membrane removal. In: American Journal of Ophthalmology [Internet]. 8th ed. Elsevier; 2009. p. 473–480.e3. Available from: https://www.sciencedirect.com/science/article/pii/S0002939408007472.
Mitamura Y, Hirano K, Baba T, Yamamoto S. Correlation of visual recovery with presence of photoreceptor inner/outer segment junction in optical coherence images after epiretinal membrane surgery. Br J Ophthalmol [Internet]. 8th ed. 2009;93:171–5. Available from: http://www.ncbi.nlm.nih.gov/pubmed/18971234.
Ozdek S, Ozdemir Zeydanli E, Karabas L, Teke MY, Yilmaz G, Citirik M, et al. Relation of anatomy with function following the surgical treatment of idiopathic epiretinal membrane: a multicenter retrospective study. Graefe’s Arch Clin Exp Ophthalmol. 2021;259:891–904.
Shiono A, Kogo J, Klose G, Takeda H, Ueno H, Tokuda N, et al. Photoreceptor outer segment length: a prognostic factor for idiopathic epiretinal membrane surgery. In: Ophthalmology [Internet]. 8th ed. Elsevier; 2013. p. 788–94. Available from: https://doi.org/10.1016/j.ophtha.2012.09.044.
Kuriyan AE, DeBuc DC, Smiddy WE. Reflectance and thickness analysis of retinal layers in patients with epiretinal membranes using spectral-domain OCT before and after vitrectomy with membrane peeling. In: Ophthalmology Retina. 8th ed. Elsevier; 2019. p. 371–8.
Orlando JI, Seebock P, Bogunovic H, Klimscha S, Grechenig C, Waldstein S, et al. U2-net: a Bayesian u-net model with epistemic uncertainty feedback for photoreceptor layer segmentation in pathological oct scans. In: Proceedings - International Symposium on Biomedical Imaging [Internet]. 8th ed. Elsevier; 2019. p. 1441–5. Available from: http://arxiv.org/abs/1901.07929.
Orlando JI, Gerendas BS, Riedl S, Grechenig C, Breger A, Ehler M, et al. Automated quantification of photoreceptor alteration in macular disease using optical coherence tomography and deep learning. Sci Rep. 2020;10:1–12.
Spaide RF, Curcio CA. Anatomical correlates to the bands seen in the outer retina by optical coherence tomography: literature review and model. Retina. 2011;31:1609–19.
Staurenghi G, Sadda S, Chakravarthy U, Spaide RF. Proposed lexicon for anatomic landmarks in normal posterior segment spectral-domain optical coherence tomography: The IN•OCT consensus. Ophthalmology [Internet]. 2014;121:1572–8. Available from: https://doi.org/10.1016/j.ophtha.2014.02.023.
Pollreisz A, Reiter GS, Bogunovic H, Baumann L, Jakob A, Schlanitz FG, et al. Topographic distribution and progression of soft drusen volume in age-related macular degeneration implicate neurobiology of fovea. Investig Ophthalmol Vis Sci. 2021;62:26.
Kuznetsova A, Brockhoff PB, Christensen RHB. lmerTest Package: tests in linear mixed effects models. J Stat Softw, Artic [Internet]. 2017;82:1–26. https://www.jstatsoft.org/v082/i13.
Hothorn T, Bretz F, Westfall P. Simultaneous inference in general parametric models. Biom J. 2008;50:346–63.
Semeraro F, Morescalchi F, Duse S, Gambicorti E, Russo A, Costagliola C. Current trends about inner limiting membrane peeling in surgery for epiretinal membranes. J Ophthalmol. 2015;2015:671905.
Spaide RF. Closure of an outer lamellar macular hole by vitrectomy: hypothesis for one mechanism of macular hole formation. Retina [Internet]. 2000;20:1–14. https://journals.lww.com/retinajournal/Fulltext/2000/06000/Closure_of_an_Outer_Lamellar_Macular_Hole_by.1.aspx.
Yamada E. Some structural features of the fovea centralis in the human retina. Arch Ophthalmol. 1969;82:151–9.
Gass JD. Müller cell cone, an overlooked part of the anatomy of the fovea centralis: hypotheses concerning its role in the pathogenesis of macular hole and foveomacualr retinoschisis. Arch Ophthalmol (Chic, Ill 1960). 1999;117:821–3.
Woon WH, Greig D, Savage MD, Wilson MCT, Grant CA, Mokete B, et al. Movement of the inner retina complex during the development of primary full-thickness macular holes: implications for hypotheses of pathogenesis. Graefe’s Arch Clin Exp Ophthalmol. 2015;253:2103–9.
Bringmann A, Unterlauft JD, Barth T, Wiedemann R, Rehak M, Wiedemann P. Foveal configurations with disappearance of the foveal pit in eyes with macular pucker: presumed role of Müller cells in the formation of foveal herniation. Exp Eye Res [Internet]. 2021;207:108604 https://doi.org/10.1016/j.exer.2021.108604.
Govetto A, Bhavsar KV, Virgili G, Gerber MJ, Freund KB, Curcio CA, et al. Tractional abnormalities of the central foveal bouquet in epiretinal membranes: clinical spectrum and pathophysiological perspectives. Am J Ophthalmol [Internet]. 2017;184:167–80. https://doi.org/10.1016/j.ajo.2017.10.011.
Lindqvist N, Liu Q, Zajadacz J, Franze K, Reichenbach A. Retinal Glial (Müller) cells: sensing and responding to tissue stretch. Investig Ophthalmol Vis Sci. 2010;51:1683–90.
Miyamoto N, Ishida K, Kurimoto Y. Restoration of photoreceptor outer segments up to 24 months after pars plana vitrectomy in patients with diabetic macular edema. Ophthalmol Retin [Internet]. 2017;1:389–94. https://doi.org/10.1016/j.oret.2017.01.017.
Ruberto G, Parisi V, Vandelli G, Falcione A, Manzoni F, Riva I, et al. Surgery for idiopathic epimacular membrane: morpho-functional outcomes based on the preoperative macular integrity of the photoreceptoral junction. A prospective pilot study. Adv Ther [Internet]. 2020;37:566–77. https://doi.org/10.1007/s12325-019-01165-4.
Treumer F, Wacker N, Junge O, Hedderich J, Roider J, Hillenkamp J. Foveal structure and thickness of retinal layers long-term after surgical peeling of idiopathic epiretinal membrane. Investig Ophthalmol Vis Sci. 2011;52:744–50.
Zou J, Tan W, Huang W, Liu K, Li F, Xu H. Association between individual retinal layer thickness and visual acuity in patients with epiretinal membrane: a pilot study. PeerJ. 2020;2020:1–16.
Arichika S, Hangai M, Yoshimura N. Correlation between thickening of the inner and outer retina and visual acuity in patients with epiretinal membrane. Retina. 2010;30:503–8.
Ooto S, Hangai M, Takayama K, Sakamoto A, Tsujikawa A, Oshima S, et al. High-resolution imaging of the photoreceptor layer in epiretinal membrane using adaptive optics scanning laser ophthalmoscopy. Ophthalmol [Internet]. 2011;118:873–81. https://doi.org/10.1016/j.ophtha.2010.08.032.
Colakoglu A, Akar SB. Potential role of Müller cells in the pathogenesis of macropsia associated with epiretinal membrane: a hypothesis revisited. Int J Ophthalmol. 2017;10:1759–67.
Hikichi T, Matsumoto N, Ohtsuka H, Higuchi M, Matsushita T, Ariga H, et al. Comparison of one-year outcomes between 23- and 20-gauge Vitrectomy for preretinal membrane. Am J Ophthalmol [Internet]. 2009;147:639–643.e1. https://doi.org/10.1016/j.ajo.2008.10.009.
Markatia Z, Hudson J, Leung EH, Sajjad A, Gibbons A. The Postvitrectomy Cataract. Int Ophthalmol Clin. 2022;62:79–91. https://doi.org/10.1097/IIO.0000000000000440.
Xu H, Chen M, Forrester JV, Lois N. Cataract surgery induces retinal pro-inflammatory gene expression and protein secretion. Investig Ophthalmol Vis Sci. 2011;52:249–55.
Barth H, Crafoord S, Arnér K, Ghosh F. Inflammatory responses after vitrectomy with vitreous substitutes in a rabbit model. Graefe’s Arch Clin Exp Ophthalmol. 2019;257:769–83.
Zobor G, Sacu S, Hollaus M, Aliyeva L, Schmalek A-S, Schmidt-Erfurth U, et al. The postoperative course of choroidal and central retinal thickness in epiretinal membranes with respect to membrane severity. Ophthalmic Res. 2021;64:1020–8.
Casini G, Loiudice P, Lazzeri S, Pellegrini M, Ripandelli G, Figus M, et al. Analysis of choroidal thickness change after 25-gauge vitrectomy for idiopathic epiretinal membrane with or without phacoemulsification and intraocular lens implantation. Ophthalmologica. 2017;237:78–84.
Jonnal RS, Kocaoglu OP, Zawadzki RJ, Lee SH, Werner JS, Miller DT. The cellular origins of the outer retinal bands in optical coherence tomography images. Investig Ophthalmol Vis Sci. 2014;55:7904–18.
Jonnal RS, Gorczynska I, Migacz JV, Azimipour M, Zawadzki RJ, Werner JS. The properties of outer retinal band three investigated with adaptive-optics optical coherence tomography. Investig Ophthalmol Vis Sci. 2017;58:4559–68.
Srinivasan VJ, Kho AM, Chauhan P. Visible light optical coherence tomography reveals the relationship of the myoid and ellipsoid to band 2 in humans. Transl Vis Sci Technol. 2022;11:1–14.
Acknowledgements
We thank the team of the Vienna Clinical Trial Center (VTC) for their contribution.
Author information
Authors and Affiliations
Contributions
MH acquired and analysed patient data and wrote the original manuscript. MG provided input for the study design, performed surgery and interpreted patient data. JI acquired and analysed patient data. JB performed statistical analyses and contributed to writing the article. OL analysed and interpreted patient data. HB analysed patient data and provided his experience and knowledge for patient data interpretation. USE provided their input for the study design, reviewed and edited the manuscript. SS, the corresponding author of this article, designed the study, performed surgery, overviewed the conduction of the study, interpreted patient data, reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
HB received research grants from Heidelberg Engineering and Apellis and speaker fees from Bayer, Roche, and Apellis. Stefan Sacu received funds from Bayer, Roche, Novartis, Iveric and Ionis. USE is a scientific consultant for Apellis, received grant support from Kodiak, Novartis, Apellis and RetInSight and received Patents/Royalty from RetInSight. JI, MH, MG, OL and JB report no conflicts of interest. The authors alone are responsible for the content and writing of the paper.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hollaus, M., Georgopoulos, M., Iby, J. et al. Analysing early changes of photoreceptor layer thickness following surgery in eyes with epiretinal membranes. Eye 38, 863–870 (2024). https://doi.org/10.1038/s41433-023-02793-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02793-5