Abstract
Background/objectives
Studies have reported an association between herpes zoster ophthalmicus (HZO) and stroke. We sought to validate this association with rigorous controls for both medical comorbidities and social factors using a nationwide U.S. administrative medical claims database.
Subjects/methods
A two-step approach was taken: first a retrospective case-control study was performed, followed by a self-controlled case series (SCCS). For the case control study, cox proportional hazard regression with inverse proportional treatment weighting assessed the hazard for stroke. In the SCCS, incidence of stroke was compared prior to and after the diagnosis of HZO.
Results
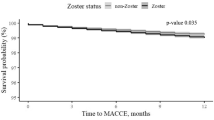
For the case–control study, 25,720 cases and 75,924 controls met our eligibility criteria. 1712 (6.7%) and 4544 (6.0%) strokes occurred in the case and control groups respectively, conferring an 18% increased risk of stroke in the observed 1-year post-HZO period (HR = 1.18, 95% CI: 1.12–1.25, p < 0.001). SCCS analysis showed the risk for stroke was highest in the month immediately after HZO episode compared to any other time range (1–30 days after, relative risk 1.58, p < 0.001) and even higher when assessing time more distal time points prior to the HZO diagnosis (days 1–30 after HZO diagnosis had RR = 1.69 (95% CI: 1.38–2.07) and RR = 1.93 (95% CI: 1.55–2.39) compared with days −120 to −91 and −150 to −121 prior to index, respectively (p < 0.001).
Conclusions
After accounting for stroke risk factors, our analysis confirms the association between HZO and stroke, with highest risk in the immediate month after an episode.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 18 print issues and online access
$259.00 per year
only $14.39 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The source data for this study were licensed by Optum, and hence we are not allowed to share the licensed data publicly.
References
Liesegang T. Herpes zoster ophthalmicus: natural history, risk factors, clinical presentation, and morbidity. Ophthalmology. 2008;115:S3–12. https://doi.org/10.1016/j.ophtha.2007.10.009.
Puri LR, Shrestha GB, Shah DN, Chaudhary M, Thakur A. Ocular manifestations in herpes zoster ophthalmicus. Nepal J Ophthalmol. 2011;3:165–71. https://doi.org/10.3126/nepjoph.v3i2.5271.
Sundström K, Weibull CE, Söderberg-Löfdal K, Bergström T, Sparén P, Arnheim-Dahlström L. Incidence of herpes zoster and associated events including stroke—a population-based cohort study. BMC Infect Dis. 2015;15:488. https://doi.org/10.1186/s12879-015-1170-y.
Kim M-C, Yun S-C, Lee H-B, Lee PH, Lee S-W, Choi S-H, et al. Herpes zoster increases the risk of stroke and myocardial infarction. J Am College Cardiol. 2017;70:295–6. https://doi.org/10.1016/j.jacc.2017.05.015.
Schink T, Behr S, Thöne K, Bricout H, Garbe E. Risk of stroke after herpes zoster—evidence from a german self-controlled case-series study. PLoS One. 2016;11:e0166554. https://doi.org/10.1371/journal.pone.0166554.
Yawn BP, Wollan PC, Nagel MA, Gilden D. Risk of stroke and myocardial infarction after herpes zoster in older adults in a US community population. Mayo Clin Proc. 2016;91:33–44. https://doi.org/10.1016/j.mayocp.2015.09.015.
Patterson BJ, Rausch DA, Irwin DE, Liang M, Yan S, Yawn BP. Analysis of vascular event risk after herpes zoster from 2007 to 2014 US insurance claims data. Mayo Clin Proc. 2019;94:763–75. https://doi.org/10.1016/j.mayocp.2018.12.025.
Lin H-C, Chien C-W, Ho J-D. Herpes zoster ophthalmicus and the risk of stroke: a population-based follow-up study. Neurology. 2010;74:792–7. https://doi.org/10.1212/WNL.0b013e3181d31e5c.
Kang J-H, Ho J-D, Chen Y-H, Lin H-C. Increased risk of stroke after a herpes zoster attack: a population-based follow-up study. Stroke. 2009;40:3443–8. https://doi.org/10.1161/STROKEAHA.109.562017.
Erskine N, Tran H, Levin L, Ulbricht C, Fingeroth J, Kiefe C, et al. A systematic review and meta-analysis on herpes zoster and the risk of cardiac and cerebrovascular events. PLoS One. 2017;12:e0181565. https://doi.org/10.1371/journal.pone.0181565.
Breuer J, Pacou M, Gauthier A, Brown MM. Herpes zoster as a risk factor for stroke and TIA: a retrospective cohort study in the UK. Neurology. 2014;82:206–12. https://doi.org/10.1212/WNL.0000000000000038.
Boehme AK, Esenwa C, Elkind MSV. Stroke risk factors, genetics, and prevention. Circ Res. 2017;120:472–95. https://doi.org/10.1161/CIRCRESAHA.116.308398.
Gillum RF, Ingram DD. Relation between residence in the southeast region of the United States and stroke incidence: the NHANES I epidemiologic follow up study. Am J Epidemiol. 1996;144:665–73. https://doi.org/10.1093/oxfordjournals.aje.a008979.
Ahacic K, Trygged S, Kåreholt I. Income and education as predictors of stroke mortality after the survival of a first stroke. Stroke Res Treat. 2012;2012:983145. https://doi.org/10.1155/2012/983145.
CDC. Stroke Facts. Centers for Disease Control and Prevention n.d. https://www.cdc.gov/stroke/facts.htm.
Parameswaran GI, Wattengel BA, Chua HC, Swiderek J, Fuchs T, Carter MT, et al. Increased stroke risk following herpes zoster infection and protection with zoster vaccine. Clin Infect Dis. 2022:ciac549. https://doi.org/10.1093/cid/ciac549.
Sreenivasan N, Basit S, Wohlfahrt J, Pasternak B, Munch TN, Nielsen LP, et al. The short- and long-term risk of stroke after herpes zoster—a nationwide population-based cohort study. PLoS ONE. 2013;8:e69156. https://doi.org/10.1371/journal.pone.0069156.
Langan SM, Minassian C, Smeeth L, Thomas SL. Risk of stroke following herpes zoster: a self-controlled case-series study. Clin Infect Dis. 2014;58:1497–503. https://doi.org/10.1093/cid/ciu098.
Meyer JJ, Liu K, Danesh-Meyer HV, Niederer RL. Prompt antiviral therapy is associated with lower risk of cerebrovascular accident following herpes zoster ophthalmicus. Am J Ophthalmol. 2022;242:215–20. https://doi.org/10.1016/j.ajo.2022.06.020.
Terlizzi E, Black L. Shingles vaccination among adults aged 60 and over: United States, 2018. NCHS Data Brief. No 370 National Center for Health Statistics 2020 1–8.
Young L. Zoster vaccine live for the prevention of shingles in the elderly patient. CIA. 2008;3:241–50. https://doi.org/10.2147/CIA.S1225.
Minassian C, Thomas SL, Smeeth L, Douglas I, Brauer R, Langan SM. Acute cardiovascular events after herpes zoster: a self-controlled case series analysis in vaccinated and unvaccinated older residents of the United States. PLoS Med. 2015;12:e1001919. https://doi.org/10.1371/journal.pmed.1001919.
Xu J, Lupu F, Esmon CT. Inflammation, innate immunity and blood coagulation. Hamostaseologie. 2010;30:8–9.
Nagel MA, Mahalingam R, Cohrs RJ, Gilden D. Virus vasculopathy and stroke: an under-recognized cause and treatment target. Infect Disord Drug Targets. 2010;10:105–11. https://doi.org/10.2174/187152610790963537.
Nagel MA, Cohrs RJ, Mahalingam R, Wellish MC, Forghani B, Schiller A, et al. The varicella zoster virus vasculopathies: clinical, CSF, imaging, and virologic features. Neurology. 2008;70:853–60. https://doi.org/10.1212/01.wnl.0000304747.38502.e8.
Grose C. Heightened risk of ischemic stroke after recent herpes zoster ophthalmicus: GROSE. J Med Virol. 2018;90:1283–4. https://doi.org/10.1002/jmv.25201.
Sawyer AR, Williams G. Misdiagnosis of burns: herpes zoster ophthalmicus. J Burn Care Res. 2006;27:914–6. https://doi.org/10.1097/01.BCR.0000245647.13372.5B.
Acknowledgements
Meeting presentation: Results to be presented at the ARVO annual meeting, New Orleans, LA, April 25th, 2023.
Funding
National Institutes of Health University of Pennsylvania Core Grant for Vision Research (2P30EYEY001583). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. Additional funding was provided by Research to Prevent Blindness and the Paul and Evanina Mackall Foundation. Funding from each of the above sources was received in the form of block research grants to the Scheie Eye Institute. None of the funding organizations had any role in the design or conduction of the study.
Author information
Authors and Affiliations
Contributions
ASG, BVB, and SEO designed the study. YY responsible for data analysis and statistics. ASG, TP, and BVB wrote up the report. YY and SEO provided edits to the written report.
Corresponding author
Ethics declarations
Competing interests
ASG, TP, YY have no financial disclosures. BVB has no relevant financial disclosures and has consulted for EyePoint Pharmaceuticals. SEO is a consultant for Abbvie.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gupta, A.S., Pradeep, T., Yu, Y. et al. The association of stroke with herpes zoster ophthalmicus. Eye 38, 488–493 (2024). https://doi.org/10.1038/s41433-023-02708-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-023-02708-4