Abstract
Purpose
Few studies of vision screening in school-aged children were reported in Tibetan Plateau. We herein summarize the results of a mandatory vision screening conducted in young children in the Tibetan Plateau of Southwest China.
Methods
The Lhasa Childhood vision Screening (LCVS) performed uncorrected distant visual acuity (UCVA) test on primary school students in urban Lhasa from July to September 2019. Pin-hole corrected VA (PCVA) was obtained for individuals with the UCVA less than 20/25. Decreased VA was defined for UCVA based on the American Academy of Pediatrics guidelines 2016 (UCVA < 20/32 for over 60 months). Visual impairment (VI), Mild VI, and moderate VI to blindness, defined as a PCVA less than 20/40, less than 20/40 to 20/63 and less than 20/63 in the better eye, respectively.
Results
Overall, 34,848 children aged 9.03 ± 1.87 years fulfilled the screening with a response rate of 98.5%. 18,412 (52.8%) of the participants were males, and 30,531(87.6%) were Tibetan. The prevalence of decreased VA, VI, Mild VI, and moderate VI to blindness was 35.6%, 4.4%, 3.5%, and 1.0%, respectively. The prevalence of decreased VA in grade 1–6 students was 28.8%, 20.8%, 26.9%, 40.7%, 50.8%, 59.5%, respectively. The prevalence of VI in grade 1 to 6 students was 1.5%, 1.4%, 2.4%, 5.6%, 7.7% and 9.9%, respectively.
Conclusion
This study documented a relatively low prevalence of decreased VA and VI in Tibetan primary school students than other urban populations in China. An increasing trend of poor vision with grades was found.
Similar content being viewed by others
Introduction
Poor vision is one of the most common problems affecting primary school students [1]. It is estimated that more than 19 million children are blind or vision impaired globally [2]. The majority of visual impairments (VI) are preventable or treatable. Varma R et al. reported that almost 25% of school-aged children in the United States have vision abnormalities [3]. According to the India census of 2001, 48% of all disability was vision disorder among children aged 5–9 years [3]. Evaluation of VI in school-aged children demonstrated that nearly half of all childhood disabilities in China were poor vision [4].
Vision screening in children is essential and may prevent permanent VI and blindness. Early diagnosis and treatment may promote a better visual outcome. But if vision abnormalities in young children were left untreated, permanent loss of vision, problems at school, bullying, reduced function and quality of life, depression, anxiety, and injuries would present [5].
Tibetan Plateau is different due to its unique characteristics such as geographical location with high altitude, intense ultraviolet radiation, different time zone, and ethnic composition compared to the central part of China. These features may affect visual development in children [6]. To our knowledge, there is currently a lack of large-scale vision screening of school-aged children in the plateau area in China. Given this, the Lhasa Childhood vision Screening (LCVS) was mandated and funded. The objective of LCVS was to determine the vision status of children in Lhasa, to support the early diagnosis and treatment for children with eye disorders, and evaluate the potential eye care needs of these regions. The present study recruits the largest sample of Tibetan children who were not well studied before.
Methods
This cross-sectional study was approved by the Institutional Review Board of Beijing Tongren Hospital, Capital Medical University (TRECKY2019-146) and conducted according to the Declaration of Helsinki. No individual-participant data were used. As school principals were children’s legal guardians in China and the study involved no intervention beyond screening, the LCVS did not require parental consent.
Study area and design
Vision screening was carried out among urban primary school children in Lhasa, Tibet Autonomous Region, China. Lhasa is located in the middle of the Tibetan plateau. Lhasa has three districts and five counties with an average altitude of 3650 m. There are approximately 40,000 primary school students, mainly Tibetan children, from 28 elementary schools in the three urban districts of Lhasa selected for LCVS. The enrolment rate of primary-school-age children there is 99.7%. Primary education in Lhasa lasts for six years, including grades 1–6.
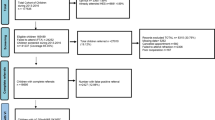
LCVS was led by the Lhasa municipal government. The screening protocol was designed by the Strabismus and Pediatric Ophthalmology Department of Beijing Tongren Hospital and conducted by trained volunteers with the permission of all the principals of the participating children. The screening was conducted from July 1 to September 20, 2019. The procedure of the LCVS was shown in Fig. 1. Uncorrected distant visual acuity (UCVA) was examined monocularly for all the participants. Students with UCVA of equal to or more than 20/25 in both eyes passed the screening. For students with UCVA of less than 20/25 in either eye, a retest of pin-hole corrected distant visual acuity (PCVA) was obtained.
UCVA uncorrected distant visual acuity, PCVA corrected visual acuity with pin-hole. UCVA was examined monocularly for all the participants. Students with UCVA of equal to or more than 20/25 in both eyes passed the screening. For students who failed the screening (with UCVA of less than 20/25 in either eye), a retest of PCVA was obtained. 41.6% with UDVA of less than 20/25 were retested with corrected VA by pin-hole. 12.7% of the participants with a corrected VA of equal to or more than 20/25 in both eyes were suggested to referral to optometrists, while 28.9% of the students with a corrected VA of less than 20/25 in either eye were suggested to referral to optometrists or ophthalmologists for further examinations.
Recruitment strategies
Before the program, we obtained a list of all primary school students from grade 1 to grade 6 in urban Lhasa from the education bureau. The local government held a coordination meeting before the recruitment. Parents’ meetings were held to explain the details and acquire the oral consent of this mandatory vision screening. Teachers in charge would arrange for the children to participate in the screening in-class-unit in the examination rooms of LCVS prepared in their schools at an appointed date and time.
Inclusion and exclusion criteria for participants
All the primary school students in urban Lhasa were encouraged to participate in the screening except the principals or the parents of the students who refused and addressed the reasons to the local government. Students with mental illness or other medical conditions that are unable to cooperate with the test were excluded.
Training for the examiners
Volunteers and school teachers familiar with the languages of Chinese and Tibetan underwent a one-day training program implemented by the optometrists and ophthalmologists from Beijing Tongren Eye Center. The training program included students’ pre-screening training at class for teachers, communication with students while testing, the arrangement of the examination room, the standard operation procedure of VA test, and the record of VA results. Screening groups consisted of teachers and volunteers were arranged to conduct the screening by the school at an appointed date and time.
Visual acuity assessment
UCVA was examined through E Standard Logarithm Eyesight Table at a distance of 5 m. The threshold VA testing was used in LCVS. Monocularly VA was assessed with the right eye tested first. The children were asked by the examiner to start at the top of the eye chart and continue reading down each line until they distinguished the smallest line of optotypes discernible. VA was noted as the finest line, where over half of the optotypes were recognized. Values of VA were converted to logarithm of minimal angle of resolution (logMAR) units. PCVA was obtained for students with UCVA less than 20/25 (logMAR vision 0.1) in either eye.
Definition of decreased visual acuity for UCVA
Decreased VA was defined for UCVA based on the current American Academy of Pediatrics (AAP) guidelines updated in 2016 (UCVA < 20/50 for 36–47 months, UCVA < 20/40 for 48–59 months, and UCVA < 20/32 for over 60 months) [7]. All children in the current study aged over 60 months.
Definitions of visual impairment for corrected VA
We used a category of VA suggested by recent studies and for comparison with other surveys. The survey used the corrected VA by pinhole as an alternative method to identify VI. VI was defined as follows (according to the corrected VA in the better eye): Anyone with a corrected VA less than 20/40 was classified as visually impaired. Mild VI was defined as a corrected VA of less than 20/40 to 20/63, moderate VI to blindness was defined as a corrected VA of less than 20/63, moderate VI was defined as a corrected VA of less than 20/63 to 20/200, severe VI was defined as a corrected VA of less than 20/200 to 10/200. Blindness was a corrected VA of less than 20/400.
Quality control procedures
Quality control procedures were implemented throughout the entire study. All examinations were required to be performed according to the standard operating procedure. Five ophthalmologists were arranged at the field site to check out the arrangement of the examination rooms, the screening procedures, and the result records during the screening. For clinical record forms with problems (missing data, misdata, and logic errors), re-tests were performed at the end of the screening day. Database using Epidata software 3.1 was set up before the screening (The Epidata Association, Odense, Denmark). Double entry of all the data was carried out by two trained individuals.
Statistical analysis
Statistical analysis was performed using SAS software (version 9.4, SAS Inc, Cary, NC, USA). Characteristics of the participants were summarized with Means ± standard deviation (SD), frequencies, and percentages. The independent t-test was used to compare the difference of visual acuity (LogMAR) between two groups (e.g. boys and girls). The one-way ANOVA analysis was used to compare the difference among three or more groups, and multiple comparisons would be performed with Bonferonni post hoc test when a significant difference was detected. The Chi-square test was used for the comparison of proportions between groups. The χ2 test for trend was used to test the overall trends across grades. A double-sided p value of less than 0.05 was considered statistically significant.
Results
Study Population and recruitment
The response rate of LCVS was 98.5% (34,848/35,364). Reasons for not attending the screening were addressed in detail in Fig. 1. PCVA of 24,485 eyes (12,390 right, 12,095 left) from 14,501 participants (41.6%) with UCVA of less than 20/25was obtained. 4418 (12.7%) participants were suggested to referral to optometrists, while 10,083 (28.9%) participants were suggested to referral to optometrists or ophthalmologists for further examinations.
Characteristics of participants in LCVS
Characteristics of the participants are shown in Table 1. The mean age of the participants was 9.03 ± 1.87 years, 52.8% (18,412/34,848) were males. 87.6% (30,531/34,848) of the participants were Tibetan. No age differences between boys and girls were found in the participants (9.03 ± 1.84 vs 9.02 ± 1.64 totally, p = 0.52; 6.63 ± 0.56 vs 6.61 ± 0.58 in grade 1, p = 0.165; 7.65 ± 0.77 vs 7.62 ± 0.72 in grade 2, p = 0.105; 8.67 ± 0.78 vs 8.64 ± 0.75 in grade 3, p = 0.128; 9.75 ± 0.79 vs 9.71 ± 0.87 in grade 4, p = 0.06; 10.77 ± 0.71 vs 10.75 ± 0.71 in grade 5, p = 0.312; 11.75 ± 0.77 vs 11.71 ± 0.74 in grade 6, p = 0.119.
Visual acuity status of different grades
The visual acuity status of different grades is shown in Table 2. The average UCVA of the left eyes was better than that of the right eyes (LogMAR vision 0.16 ± 0.25 vs 0.17 ± 0.26, p < 0.001). Male subjects had better UCVA than female subjects (LogMAR vision 0.20 ± 0.27 vs 0.15 ± 0.25, p < 0.001).
As a significant correlation was found between the right and the left eyes (R = 0.82, p < 0.001), we used the results of the right eyes for further analysis. Significant differences were found between grades (p < 0.001) except grade 1 vs grade 2 (p = 0.106) in UCVA, and in corrected VA except grade 1 vs grade 3 (p = 0.118). A decreasing trend with grade was found in both UCVA and corrected VA.
Categories of visual acuity
The prevalence of decreased VA and VI in different grades are shown in Table 3. Girls showed a higher prevalence of decreased VA (38.6% vs 32.8%, p < 0.001, analysed by the right eyes) and VI (5.2% vs 3.8%) than boys. The prevalences of decreased VA and VI were increased with grades (p < 0.001).
Discussion
Living at altitudes above 3000 m is known to have biological effects on humans [8]. The particular geographical location, unique plateau environment, ethnic composition, and Tibetan cultural characteristics of Lhasa might affect the vision of people there, especially the vision development of young children [9]. Bali et al. found that the adult subjects from high altitude had wider inter–outer canthal distance and interpupillary distance, narrower palpebral fissure length in the vertical dimension, and lower intraocular pressure than their counterparts living at lower altitudes. At the same time, the axial length, lens thickness, and anterior chamber depth were comparable in the two groups [9]. Research on ocular parameter differences between children in high/ lower altitudes was a hitherto unexplored area in the literature. Whether the geographical features account for the differences between the current findings and other studies needs further studies. To the best of our knowledge, this is the first study to provide large-scale data on vision screening of primary school children in urban Lhasa in the Tibetan Plateau of Southwest China. The response rate was 98.5%. 87.6% of the participants were Tibetan. This study documents a relatively high prevalence of decreased VA and VI in Tibetan primary school students as expected due to its lower economic and educational level. A statistically significant increasing trend of poor vision with grade is found.
Vision screenings are important for the eye care of childhood. In a joint position statement, vision screening was recommended for school-aged children every 1–2 years [10]. We here used the definition of decreased VA defined for UCVA based on the AAP guidelines updated in 2016 [7]. Few studies reported a decrease VA using the AAP definition, especially in China. We had translated and published it in influential Chinese journals to promote the usage of the evaluation approach. The total prevalence of decreased VA found in Lhasa (35.6%, grade 1–6, 2019) was higher than that reported in American (15–20%, grade kindergarten to grade 5, 2015) using the comparable VA threshold (UCVA < 20/40 for kindergarten or first grade and UCVA < 20/30 for grade 2–5) [11]. The prevalence of vision loss (UCVA less than 20/25) found in Lhasa (41.5%) was lower than other urban populations in China (55–64.2%) [12, 13]. This might be due to the combined effects of the unique environmental factors and economic backwardness in Lhasa. The age difference of the participants and the time of the study performed might also account for the results. The prevalence of VI reported in many epidemiology studies raged from 0.32–19.4% in children [14]. The difference might result from the usage of VI definition, the age of participants, economic development status, and so on [4, 15, 16]. The Chinese government has paid special attention to children’s eye care in recent years. Children’s vision health has been made the theme of the Chinese Eye Care Day for the latest seven years. That is the reason why many local governments conducted mandatory vision screening. Education on students and parents about the importance of timely vision screening and early treatment for vision loss was also emphasized.
Pinhole correction indicated of undercorrected refractive error in the participants. In the present study, more than 80% of the participants with UCVA less than 20/40 passed the definition line of 20/40 corrected by pin-hole. This was evident in many epidemiology studies, where uncorrected refractive error especially myopia accounted for about 47%-92.7% of the reduced vision in school-age children [14]. The present vision screening study could not collect the suggested referral information for the large sample size. We carried out a cluster randomly selected five-year follow-up cohort study named Lhasa Childhood Eye Study (LCES) in grade 1 students of Lhasa right after the screening. Examinations of standardized ocular, systematic examinations, and questionnaires were performed in the cohort study. The prevalence of hyperopia, emmetropia, myopia, and high myopia reported in the baseline of LCES was 6.91%, 89.22%, 3.86%, and 0.16%, respectively [17]. The top two causes of VI in grade one students were amblyopia and congenital cataract [18, 19]. More results of ophthalmic conditions in children of Lhasa would be reported with the carrying on of LCES.
The LCVS showed that the burden of reduced VA and VI had increased dramatically among primary school children from grade 1 to grade 6 in Urban Lhasa. It was consistent with many previous studies showing that VI was associated with older age [12, 15]. It was reported that the increasing prevalence of vision loss among different generations was mainly due to intensive schooling [20]. The Chinese government had introduced policies to lighten the load on the students and encourage more time spent outdoors. As the PCVA roughly reflects the corrected VA, the increasing prevalence of VI (based on PCVA in the present study) with age may partly reflect the high prevalence of eye problems secondary to the long-standing uncorrected myopia or hyperopia, such as strabismus and amblyopia, as well as congenital cataract. Our study found statistically significant differences between grades in UCVA except grade 1 vs. grade 2 and corrected VA except grade 1 vs. grade 3. The vision of grade 1 students showed a worse result than expected. One explanation might be the younger average age which was 6.62 ± 0.53. Vision function in Children of that age might still be in the developing stage [21]. Another reason might be poor cooperation resulting from the difficulty in understanding the visual acuity test procedure. The other explanation might be examination fatigue resulting from a younger age. It is reported that examination fatigue among younger children might play a role in vision assessment inaccuracy [10, 21]. Further studies were needed to provide evidence to support the assumptions. We found that girls were more susceptible than boys to having reduced VA. The result was consistent with many epidemiology studies that myopia occurred more often in girls than in boys, especially in older children [14,15,16]. It was hypothesized that the reasons for sex differences might be determined by genetic factors, dietary factors, and amount of close work, as well as were connected with puberty [22].
This study was the first time Lhasa conducted vision screening in school-aged children. We set the cut-off limit at 20/25 for a referral, which may be accurate and sufficient to identify children with refractive errors [1]. More evidence-based and economic studies are needed to determine a proper cut-off limit. The development status of the screening region should be considered as well.
A large representative sample size of school students from all grades in primary school was conducted in the current study, helping to evaluate the association between visual status and categories with age and grade. Nevertheless, the limitation of our study should be mentioned. As the blind schools in Lhasa were not included in the present study, this sample of schoolchildren could only represent urban children in regular schools in urban Lhasa. Best corrected VA (BCVA) was not performed in the LCVS. Given that the link between pin-hole corrected VA and BCVA is not simple, using pin-hole corrected VA as a proxy measure for VI may not be accurate. However, it is a great challenge to perform BCVA in an extensive sample screening program in China, especially in the Tibetan plateau of China.
In conclusion, these summary vision screening data indicate the burden of decreased VA and VI among children in Lhasa. These data help design strategies for eye care and health services in the Tibetan Plateau of Southwest China, which may also have public health implications for other developing countries. Continued vision screening is needed considering the rising incidence of myopia during school years.
Summary
What was known before
-
Few research vision screening in school-aged children were reported in Tibetan Plateau.
What this study adds
-
34,848 children in Lhasa aged 9.03 ± 1.87 years fulfilled the screening with a response rate of 98.5%. This study documented a relatively high prevalence of decreased VA and VI in Tibetan primary school students in Lhasa. An increasing trend of poor vision with grade was found.
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Jin J. Vision screening in children. JAMA. 2017;318:878.
Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. Br J Ophthalmol. 2012;96:614–8.
Varma R, Tarczy-Hornoch K, Jiang X. Visual impairment in preschool children in the United States. JAMA Ophthalmol. 2017;135:610.
Jan C, Xu R, Luo D, Xiong X, Song Y, Ma J, et al. Association of visual impairment with economic development among Chinese schoolchildren. JAMA Pediatr. 2019;173:e190914.
Good WV. Vision screening in very young children—making sense of an inexorable diagnostic process. JAMA Pediatr. 2017;171:1046–7.
Qian X, Liu B, Wang J, Wei N, Qi X, Li X, et al. Prevalence of refractive errors in Tibetan adolescents. BMC Ophthalmol. 2018;18:118.
Donahue SP, Baker CN. Procedures for the evaluation of the visual system by pediatricians. Pediatrics. 2016;137:1–9.
Jha KN. High altitude and the eye. Asia Pac J Ophthalmol (Philos). 2012;1:166–9.
Bali J, Chaudhary KP, Thakur R. High altitude and the eye: a case controlled study in clinical ocular anthropometry of changes in the eye. High Alt Med Biol. 2005;6:327–38.
Jonas DE, Amick HR, Wallace IF, Feltner C, Vander Schaaf EB, Brown CL, et al. Vision screening in children aged 6 months to 5 years. JAMA. 2017;318:845.
Hark LA, Mayro EL, Tran J, Pond M, Schneider R, Torosian J. et al. Improving access to vision screening in urban Philadelphia elementary schools. J AAPOS. 2016;20:439–443.
Sun HP, Li A, Xu Y, Pan CW. Secular trends of reduced visual acuity from 1985 to 2010 and disease burden projection for 2020 and 2030 among primary and secondary school students in China. JAMA Ophthalmol. 2015;133:262–8.
Wang J, Ying GS, Fu X, Zhang R, Meng J, Gu F, et al. Prevalence of myopia and vision impairment in school students in Eastern China. BMC Ophthalmol. 2020;20:2.
Atowa UC, Hansraj R, Wajuihian SO. Visual problems: a review of prevalence studies on visual impairment in school-age children. Int J Ophthalmol. 2019;12:1037–43.
Zhao L, Stinnett SS, Prakalapakorn SG. Visual acuity assessment and vision screening using a novel smartphone application. The. J Pediatrics. 2019;213:203–10.
Burnett AM, Yashadhana A, Lee L, Serova N, Brain D, Naidoo K. Interventions to improve school-based eye-care services in low- and middle-income countries: a systematic review. B World Health Organ. 2018;96:682–94.
Chen W, Fu J, Meng Z, Li L, Su H, Dai W, et al. Lhasa childhood eye study: the rationale, methodology, and baseline data of a 5 year follow-up of school-based cohort study in the Tibetan plateau region of Southwest China. BMC Ophthalmol. 2020;20:250.
Meng Z, Fu J, Chen W, Li L, Su H, Dai W, et al. Prevalence of amblyopia and associated risk factors in Tibetan grade one children. Ophthalmic Res. 2021;64:280–9.
Li L, Fu J, Chen W, Meng Z, Sun Y, Su H, et al. Difference of refractive status before and after cycloplegic refraction: the Lhasa childhood eye study. JPN J Ophthalmol. 2021;65:526–36.
Pan CW, Zheng YF, Wong TY, Lavanya R, Wu RY, Gazzard G, et al. Variation in prevalence of myopia between generations of migrant indians living in Singapore. Am J Ophthalmol. 2012;154:376–81.
Becker R, Hubsch S, Graf MH, Kaufmann H. Examination of young children with Lea symbols. Br J Ophthalmol. 2002;86:513–6.
Czepita M, Czepita D, Safranow K. Role of gender in the prevalence of myopia among Polish schoolchildren. J Ophthalmol. 2019;2019:9748576.
Acknowledgements
The authors are grateful for the support from the Lhasa local government for helping organize the survey.
Funding
The research was supported by Open Research Fund from Beijing Advanced Innovation Center for Big Data-Based Precision Medicine, Beijing Tongren Hospital, Beihang University & Capital Medical University (BHTR-KFJJ-202013); Capital Health Development Special Fund of China -Major Project(SF-2018-1-2051); Capital Health Development Special Fund of China -Youth Project (2018-4-1083); High Level Health Technical Talent Training Program of Beijing Municipal Health Bureau (2015-3-023); Beijing Municipal Science & Technology Commission (Z171100001017066). The sponsor or funding organization had no role in the design or conduct of this research. No conflicting relationship exists for any author.
Author information
Authors and Affiliations
Contributions
All authors have read and approved the manuscript. WWC and JF designed the study. WWC, JF, AS, LL, YYS and ZJM joined the data collection. AS and ZJM were involved in data cleaning and verification. LL analysed the data. WWC drafted the manuscript. JF contributed to the interpretation of the results and critical revision of the manuscript for important intellectual content and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, W., Fu, J., Sun, A. et al. Paediatric vision screening in Urban Lhasa from the Tibetan Plateau of Southwest China. Eye 37, 1336–1341 (2023). https://doi.org/10.1038/s41433-022-02126-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-02126-y