Abstract
Background
X-linked retinitis pigmentosa (XLRP) is the most severe form of retinitis pigmentosa (RP) and accounts for 15–20% of all RP cases. In this study, we investigated the progression of visual acuity loss across age groups in female carriers and compared it to affected males.
Methods
A PubMed literature search was conducted, and RP2 cases were included based on specific inclusion criteria. Visual acuity (VA), refractive error spherical equivalent (SE), and retinal findings were recorded. Cross-sectional analyses investigated the relationship between VA and age in carrier females and affected males. Genotype-phenotype VA correlations were studied using t-tests.
Results
35 carrier females and 28 affected males with confirmed RP2 mutations were collected from 13 studies. The mean age and logMAR VA of carrier females were 44.2 ± 17.4 years, and 0.5 ± 0.5, respectively. 78.8% of carrier females showed abnormal XLRP-related fundus findings and had significantly reduced VA compared to those with normal fundi (0.6 ± 0.5 vs. 0.1 ± 0.1; p = 0.03). Compared to affected males, no statistical correlation was found between logMAR VA and advancing age in carrier females (p = 0.75). Statistically significant linear correlations were found between logMAR VA and SE in each of carrier females (p = 0.01). There were no observed differences in logMAR VA based on mutation type (p = 0.97) or mutation location (p = 0.83). Anisometropia was observed in 38% of carrier females and 68% of affected males; these prevalence numbers are statistically significant between the two groups (1.7 ± 0.3 vs. 3.9 ± 10.9 dioptres; p = 0.03).
Conclusions
RP2 carrier females generally maintain good VA throughout their lifetime, as opposed to affected males, whose vision progressively declines. Our study provides important VA prognostic data that is crucial for patient counseling.
Similar content being viewed by others
Introduction
Retinitis Pigmentosa (RP) comprises a heterogeneous group of genetic diseases that can be inherited in an autosomal dominant, autosomal recessive or X-linked manner [1]. To date, 63 genes are reported to cause autosomal recessive RP, 30 genes cause autosomal dominant RP, and only 3 are reported to cause X-linked RP (XLRP) [2]. XLRP accounts for 15–20% of all RP cases [3, 4] and is associated with the most severe disease course compared to other genetic forms. RPGR and RP2 genes together account for over 80% of XLRP [5]. Mutations in RP2 are reported to cause 10–20% of XLRP [6], with Arg120stop being the most common mutation [7].
Male patients with XLRP show a more severe phenotype than carrier females. Typical features include night blindness, visual field constriction and reduced visual acuity (VA) [8]. In general, males with RP2-related XLRP have been shown to have more severely reduced VA compared to those with RPGR [9], likely due to earlier macular involvement [10]. Interestingly, within affected families, RP2 affected males have a clinical disease onset approximately 30 years before their carrier female relatives have any symptoms [11]. Furthermore, XLRP carrier females present with a wide clinical spectrum that ranges from being asymptomatic to having severe symptoms similar to those of male patients [10, 12, 13].
Currently, there is a large body of data regarding ophthalmic clinical features and visual prognosis in affected males with RP2. [5,6,7, 9, 10] There is a paucity of clinical data specifically pertaining to RP2 female carriers, as most studies reported on either RPGR carriers or RPGR and RP2 carriers together without distinguishing between these two genes [3, 13]. Few studies have, however, characterized the clinical phenotypes and visual clinical course in RP2 carrier females [12, 13]. In this study, we conducted a cross-sectional meta-analysis of RP2 carrier females cases collected from the literature to characterize the visual acuity spectrum across age, and to provide key clinical features comparing them to affected males.
Materials and methods
Literature search
A PubMed literature search was conducted using the following key word combinations: “RP2 protein, human”, “RP2 protein, human AND Visual Acuity”, “RP2 protein, human AND Heterozygote”, “RP2 protein, human AND Genes, Recessive”, “RP2 protein, human AND Carrier”, “RPGR protein, human AND RP2 protein, human”, “Retinitis Pigmentosa 2”, and “Retinitis Pigmentosa 2 AND Visual Acuity”.
Data collection
The following inclusion criteria were used to narrow the selection process: (1) reports with confirmed RP2 cases with data on VA, spherical equivalent (SE), and family history; (2) reports with data on RP2 carrier females and at least one affected male relative; (3) only cross-sectional and/or the earliest set of longitudinal data from each reported RP2 case was collected and used in the analysis; (4) previously published papers, cases series and case reports were specifically selected (abstracts and presentations were excluded); (5) language was restricted to English only; and, (6) timeline between 1992 and 2019 was used to chronologically frame the literature search.
Carrier female status of RP2 was defined as a female patient carrying a RP2 mutation and either having an affected biological son or father with the same mutation, or having a biological mother or brother with the same mutation.
The following data was extracted from the selected articles when available: patient’s age at the ophthalmic exam, gender, genetic mutation, VA, refractive error, and retinal findings. Note was made of affected males from the same family, their VA and refractive errors.
Data analysis
For statistical analysis purposes, Snellen VA data was converted to logMAR equivalents. VA recorded as counting fingers, hand movement, light perception, and no light perception, were replaced by the following values: 2.6, 2.7, 2.8 and 2.9, respectively, as per Roberts at al. [14]. Similarly, the refractive error was converted to SE in dioptres.
To standardize the data collection process, we grouped the patients into “normal” and “abnormal” groups based on their reported fundus findings. Abnormal was defined as having a retinopathy with findings strictly related to XLRP. These included “pericentral atrophy”, “peripheral atrophy”, “peripheral granularity”, “macular atrophy”, “temporal atrophy”, “peripheral pigmentation”, “bone-spicule-like pigmentation”, and “abnormal RPE pigment” (Supplementary Table 1).
To investigate differences in VA severity between affected males and carrier females, we used the logMAR VA threshold of 1.0 (Snellen: 20/200) defined as “severe visual impairment” by the World Health Organization (WHO) [15], and then categorized affected males into two groups: those with logMAR VA less than 1.0 (defined as group 1), and those with logMAR VA equal to or greater than 1.0 (defined as group 2). We then categorized carrier females according to their affected male relative’s status into groups 1 and 2. We compared the VA of these groups using t-tests. We also carried out mutation type and mutation location-based VA and SE comparisons using t-tests to identify any possible genotype-phenotype correlations. Statistical significance was reached when the p-value was less than 5%.
Results
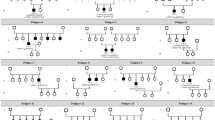
The initial PUBMED literature search yielded 133 articles. After duplicate records removal, the number was reduced to 92. Title and abstract screening resulted in the exclusion of an additional 37 records due to data not pertinent to our study’s purpose. 55 full-text papers were then screened based on inclusion/exclusion criteria and 42 full texts were excluded. The final number of studies included in this meta-analysis was 13 (Supplementary Fig. 1 and Table 1). Among these, 2 were case reports, and 11 cases with at least 2 families and/or patients. The PRISMA literature search flow diagram is shown in Supplementary Fig. 1. The period of 1992 to 2019 was chosen because, to our knowledge, the first report documenting phenotypic findings of RP2 female carriers was published in 1992 [16].
Thirty-five carrier females and 28 affected males that met inclusion criteria were included. Table 1 summarizes the demographic and ophthalmic data of the studied patients. In the carrier females’ group, the mean age was 44.2 (median: 46.5, range: 8 to 81), the mean logMAR VA was 0.5 (Snellen equivalent: ~20/60, median: 0.2, range: 0 to 1.9), and the mean SE of both eyes was −3.50 dioptres (median: −1.70, range: +4.30 to −24.00). In the affected males’ group, the mean age was 22.6 years (median: 24, range: 5 to 43), the mean logMAR VA was 1.1 (Snellen equivalent: ~20/280, median: 1.2, range: 0.1 to 2.7), and the mean SE was −6.20 dioptres (median: −5.60, range +2.80 to −13.90). Compared to affected males, carrier females were significantly older (p < 0.01), had a significantly better logMAR VA (p < 0.01), and were less myopic (although the difference was not statistically significant, p = 0.16). While there was no statistically significant linear relationship between the mean logMAR VA and age of carrier females (Fig. 1, p = 0.75), there was a statistically significant linear correlation in the affected males group (Fig. 1, p = 0.03).
Each point represents the mean visual acuity (VA) of both eyes for each patient with respect to age in years. The gray circles represent carrier females and the black squares represent the affected male relatives. The dashed lines represent the linear regression line fitted between the VA and age for carrier females (gray, y = 0.002x + 0.39, p = 0.75) and affected males (black, y = 0.03x + 0.40, p = 0.03), respectively.
Retinopathy, defined as XLRP-related abnormal fundus findings, was reported in 78.8% (26/33) of carrier females, with a mean age of 40.6 years and mean logMAR VA of 0.6 (Table 1). 91.7% (22/24) of affected males were reported to have XLRP-related retinopathy with a mean age of 21.4 years and mean logMAR of 1.0 (Table 1).
Anisometropia greater than or equal to 1.0 dioptre of SE between both eyes was observed in 38% (8/21) of carrier females, and 68% (12/19) of affected males. There was a statistically significant difference between the degree of anisometropia in affected males and carrier females (1.7 ± 0.3 vs. 3.9 ± 10.9 dioptres; p = 0.03).
Severity of VA loss
This analysis was conducted after separating affected males into two groups based on the WHO severe visual impairment threshold. In affected males’ group 1 (logMAR VA less than 1.0), the mean age was 18.0 years (median: 17.5, range: 5 to 32) and the mean age logMAR VA 0.5 (median: 0.5, range: 0.1 to 1.0). In affected males group 2 (logMAR VA equal to or greater than 1.0), the mean age was 25.7 years (median: 25.5, range: 13 to 43) and the mean logMAR VA was 1.7 (median: 1.5, range: 1.2 to 2.7). After categorizing the carrier females based on their affected male relative’s status into groups 1 or 2, those in group 1 had a mean age 43.9 (median: 44.5, range: 17 to 81) and a mean logMAR VA of 0.4 (median: 0.2, range: 0 to 1.8). Carrier females in group 2 had a mean age of 44.6 (median: 52.5, range: 8 to 68) and a mean logMAR VA of 0.6 (median: 0.5, range: 0 to 1.9).
There was no statistically significant linear correlation between the logMAR VA and age of affected males in either group 1 (p = 0.59) or group 2 (p = 0.09) (Fig. 2A). Similarly, no statistically significant linear correlations were found between logMAR VA and age of carrier females in groups 1 (p = 0.52) and 2 (p = 0.82) (Fig. 2B). Interestingly, while a clear separation in the VA data of affected males exists with respect to the 1.0 logMAR severe visual impairment threshold (Fig. 2A), no clear separation was observed among the carrier females whose VA showed a random scattering with respect to the same threshold (Fig. 2B). Additionally, there was no statistically significant difference between carrier females logMAR VA in groups 1 and 2 (0.4 ± 0.5 vs. 0.6 ± 0.5; p = 0.20). This further confirms the absence of correlation between VA severity among the carrier females.
Affected males were categorized into two groups with respect to logMAR visual acuity (VA) of 1.0 threshold: group 1 (logMAR VA less than 1.0), and group 2 (logMAR VA equal to or greater than 1.0). Carrier females were then categorized into group 1 or 2 depending on their intrafamilial affected males corresponding grouping. A Linear regressions of mean VA vs. age in affected males’ groups. The empty and solid black squares represent affected males in group 1 and 2, respectively. The dotted and dashed black lines represent the linear regression line fitted between the logMAR VA and age for affected males in group 1 (y = −0.007x + 0.62, p = 0.65) and in group 2 (y = 0.03x + 0.81, p = 0.04), respectively. B Linear regressions of mean VA vs. age in carrier females’ groups. The empty and solid gray circles represent affected males in group 1 and 2, respectively. The dotted and dashed gray lines represent the linear regression line fitted between the logMAR VA and age for carrier females in group 1 (y = −0.0003x + 0.34, p = 0.97) and group 2 (y = 0.001x + 0.60, p = 0.93), respectively. The black solid line in both figures represents the logMAR VA threshold of 1.0.
Refractive error analysis
The mean SE of both eyes was −3.5 dioptres (median: −1.7, range: +4.3 to −24.0) for carrier females and −6.2 dioptres (median: −5.6, range: +2.8 to −13.9) for affected males. There was a statistically significant linear correlation between logMAR VA and SE in carrier females (p = 0.01, Fig. 3), and in affected males (p = 0.01, Fig. 3).
Each point represents the mean visual acuity (VA) of both eyes for each patient with respect to its corresponding spherical equivalent in dioptres (SE). The gray circles represent carrier females and the black squares represent the affected male relatives. The dashed lines represent the linear regression of logMAR VA vs. SE for carrier females (gray, y = −0.039x + 0.37, p = 0.01) and affected males (black, y = −0.06x + 0.70, p = 0.007) respectively.
Gene mutation analysis
Genetic mutation type was available for 66% (23) of carrier females and 86% (24) of affected males, and mutation location was available for 66% (23) of carrier females and 86% (24) of affected males (Table 2). The most common mutations in carrier females were nonsense mutations (48%). Nearly half (48%) of the mutations occurred on Exon 2 (Supplementary Table 2).
Table 2 compares the VA by mutation type in carrier females and affected males. When comparing affected males to carrier females with missense mutations in RP2, statistically significant differences were found in their logMAR VA (1.4 ± 0.6 vs. 0.4 ± 0.3; p = 0.001) but not in their SE (−6.5 ± 2.4 vs. −4.4 ± 6.1 vs.; p = 0.38). Similarly, when comparing affected males to carrier females with nonsense mutations in RP2, statistically significant differences were found in their logMAR VA (1.2 ± 0.8 vs. 0.4 ± 0.6; p = 0.02) but not in their SE (−1.8 ± 3.1 vs. −4.5 ± 4.8; p = 0.28). In the affected males’ group when data was categorized by missense vs. nonsense mutations, no significant differences were found in the logMAR VA (1.4 ± 0.6 vs. 1.2 ± 0.8; p = 0.54), however, significant differences were found in SE (−6.5 ± 2.4 vs. −1.8 ± 3.1; p = 0.01).
In the carrier females’ group, when data was categorized by missense vs. nonsense mutations, no statistically significant differences were found in either the one-way ANOVA of the logMAR VA (0.4 ± 0.3 vs. 0.4 ± 0.6; p = 0.97, Supplementary Table 2) or the SE (−4.4 ± 6.1 vs. −4.5 ± 4.8; p = 0.98, Supplementary Table 2). When data was categorized based on mutation location (Exon 1 vs. Exon 2 vs. Intron 3), no statistically significant differences were found in the one-way ANOVA of the logMAR VA (p = 0.83) or the SE (p = 0.59). There were also no statistically significant differences in the logMAR VA, when t-testing exon 1 vs. exon 2 (0.4 ± 0.2 vs. 0.5 ± 0.6; p = 0.87, Supplementary Table 2), exon 2 vs. intron 3 (0.5 ± 0.6 vs. 0.3 ± 0.3, p = 0.57, Supplementary Table 2), or exon 1 vs. intron 3 (0.4 ± 0.2 vs. 0.3 ± 0.3; p = 0.55, Supplementary Table 2).
Discussion
The present comparative meta-analysis is, to our knowledge, the largest study profiling the visual acuity in RP2 carrier females and affected males. The carrier female group exhibited variability in the severity of vision loss that ranged from normal visual acuity (VA) to severe reduction of vision. While there was a clear relationship between decreasing VA and increasing age in affected males, no such relationship was found in carrier females. Affected males had also significantly worse VA than carrier females as well as a higher mean myopic refractive error. We found no significant differences in the logMAR VA of carrier females when categorized according to the severity of vision loss in their affected male relatives.
Ophthalmoscopic findings in XLRP carrier females can range from a tapetal-like reflex and isolated regions of peripheral pigment atrophy and clumping to extensive retinal degeneration that includes diffuse bone spicule-like pigmentation and attenuated vessels [8, 12, 17]. The wide spectrum of phenotypes among carrier females is likely attributed to X chromosome inactivation during embryogenesis, a physiological phenomenon referred to as lyonization [18]. This random inactivation persists in daughter cells, resulting in a mosaic distribution where either the maternal or paternal X-chromosome is active [19].
Fishman and colleagues [17] initially reported the classic fundus finding of a tapetal-like reflex in XLRP carriers. Interestingly, a case series of 27 XLRP carriers found that carriers with macular pigmentary changes had a poorer visual prognosis than carriers with normal fundi [13]. In the present study, 78.8% of carrier females with reported abnormal XLRP-related fundus findings had a significantly more reduced VA compared to those with normal fundi (Table 1). Moreover, none of the patients with a normal fundus or with only a tapetal-like reflex had any significant change in VA or visual field over time [13].
XLRP is distinct from other forms of RP in which central visual acuity is generally conserved due to foveal sparing [20]. While RPGR- [8] and RP2-associated XLRP have variable phenotypes [5, 21,22,23], some studies have found that the latter is characterized by a higher prevalence of early onset, progressive myopia and early impaired central vision, while the former is characterized by late-onset night blindness [5]. Other authors have reported no clear clinical difference between RPGR-related and RP2-related phenotypes [11, 24,25,26].
In XLRP, relatively early VA loss is likely due to earlier cone and foveal involvement [8]. Sharon et al. [9] reported a mean logMAR VA in affected RP2-related XLRP males of 1.0 (Snellen equivalent: ~20/210) and of 0.6 (Snellen equivalent: ~20/82) in those with RPGR-related disease. In this study, we computed a VA mean logMAR of 1.1 ± 0.7 (Snellen equivalent: ~20/250) at a mean age of 22.6 ± 8.9 years in RP2-related affected males, which is comparable to that in the current literature. As expected, carrier females showed a significantly better logMAR VA (0.5 ± 0.5) at a mean older age of 44.2 ± 17.4 years when compared to affected males. Furthermore, there was no statistical linear relationship between the mean logMAR VA and age of carrier females while those two variables were statistically correlated in affected males (Fig. 1). Additionally, we found no statistically significant differences in the logMAR VA of carrier females when categorized according to the severity of vision loss in their affected male relatives (Fig. 2). All these observations are not surprising as the phenotypic manifestation of XLRP in carrier females depends mainly on the protective effect of X-inactivation.
Comander et al. [12] reported that the majority of carrier females had a normal logMAR VA averaging 0.1 (Snellen equivalent: ~20/27), while a minority (2.5%) showed severe visual impairment due to an underlying maculopathy, presumed to be associated with high myopia [21]. Our findings support this observation as we found a significant linear correlation between the severity of myopia and the logMAR VA worsening in both RP2-related carrier females and affected males (Fig. 3).
The association between myopia and RP2-related XLRP has been previously documented [12, 27], and our analysis supports this fact. In the current study, the mean SE in carrier females was −3.5 dioptres, which was about 3 dioptres less myopic than affected males. Previous studies reported a median SE of −0.3 (+1.75 to −11.0) dioptres in carrier females and −5.8 (+1.0 to −10.0) dioptres in affected males [21]. Of note, we also found anisometropia greater than or equal to 1.0 dioptre of SE between the right and left eyes in 38% of carrier females compared to 68% of affected males (~1.8 folds difference). Li et al. [28] reported that carrier females with high myopic anisometropia could be attributed to the skewed X inactivation leading to dissimilar growth between the eyes.
We explored the effects of different RP2 mutations on the RP phenotype. The location and type of RP2 mutations can provide insight into phenotypic expression [29]. In the present study, 52% of mutations occurred in exon 2 of the RP2 gene. Mutations at this site can affect the evolutionary conserved protein by substituting charged hydrophilic residues with uncharged ones, likely impairing the RP2 protein function [29]. Generally, missense mutations (or in-frame mutations) can result in proteins with a reduced function, while truncating mutations (frameshift or splice) cause severe phenotypes due to nonfunctional protein [10]. Splice mutations can result in severe phenotypes, especially when they occur early in the gene resulting in premature truncation [10]. We found no correlation between severity of VA loss and the type of mutation or its location in both affected males and carrier females (Table 2). Additionally, we could not confirm previously reported genotype-phenotype correlations [29] likely due to the relatively small sample size in this study.
Limitations of the current study include the small sample size and lack of primary data. The mutation analysis of the RP2 gene was not standardized across the 13 studies. Additionally, some studies did not provide wide-field color and fundus auto-fluorescence imaging of carrier females, potentially missing tapetal-like or other clinical findings. Nonetheless, we believe that the current study adds significantly to the understanding of visual acuity spectrum in RP2-associated XLRP patients and provides important tools for counseling carrier females regarding visual prognosis and their potential affected male progeny.
What was known before
-
Ophthalmic clinical features and visual prognosis in affected males with RP2 and RPGR. Ophthalmic clinical features in female carriers of RPGR.
What this study adds
-
Cross-sectional meta-analysis of RP2 carrier female cases collected from the literature to characterize the visual acuity spectrum across age.
-
Characterization of clinical phenotypes, including the clinical course of vision change, and anisometropia in RP2 carrier females: although no statistical correlation was found between logMAR visual acuity and advancing age in carrier females, there was, however, significant linear correlations between logMAR visual acuity and spherical equivalent. There were also statistically significant differences in anisometropia between carrier females and affected males.
References
Daiger SP, Bowne SJ, Sullivan LS. Perspective on genes and mutations causing retinitis pigmentosa. Arch Ophthalmol. 2007;125:151–8.
RetNet: Disease Table. Accessed 3 March 2021. https://sph.uth.edu/retnet/disease.htm#23.115d
Fishman GA. Retinitis pigmentosa. Genetic percentages. Arch Ophthalmol. 1978;96:822–6.
Boughman JA, Conneally PM, Nance WE. Population genetic studies of retinitis pigmentosa. Am J Hum Genet. 1980;32:223–35.
Pelletier V, Jambou M, Delphin N, Zinovieva E, Stum M, Gigarel N, et al. Comprehensive survey of mutations in RP2 and RPGR in patients affected with distinct retinal dystrophies: genotype-phenotype correlations and impact on genetic counseling. Hum Mutat. 2007;28:81–91.
Hardcastle AJ, Thiselton DL, Van Maldergem L, Saha BK, Jay M, Plant C, et al. Mutations in the RP2 gene cause disease in 10% of families with familial X-linked retinitis pigmentosa assessed in this study. Am J Hum Genet. 1994;64:1210–5.
Vorster AA, Rebello MT, Coutts N, Ehrenreich L, Gama AD, Roberts LJ, et al. Arg120stop nonsense mutation in the RP2 gene: mutational hotspot and germ line mosaicism? Clin Genet. 2004;65:7–10.
De Silva SR, Arno G, Robson AG, Fakin A, Pontikos N, Mohamed MD, et al. The X-linked retinopathies: physiological insights, pathogenic mechanisms, phenotypic features and novel therapies. Prog Retin Eye Res. 2021;82:100898.
Sharon D, Sandberg MA, Rabe VW, Stillberger M, Dryja TP, Berson EL. RP2 and RPGR mutations and clinical correlations in patients with X-linked retinitis pigmentosa. Am J Hum Genet. 2003;73:1131–46.
Jayasundera T, Branham KE, Othman M, Rhoades WR, Karoukis AJ, Khanna H, et al. The RP2 phenotype and pathogenetic correlations in X-linked retinitis pigmentosa. Arch Ophthalmol. 2010;128:915–23.
Rosenberg T, Schwahn U, Feil S, Berger W. Genotype-phenotype correlation in X-linked retinitis pigmentosa 2 (RP2). Ophthalmic Genet. 1999;20:161–72.
Comander J, Weigel-DiFranco C, Sandberg MA, Berson EL. Visual function in carriers of X-linked retinitis pigmentosa. Ophthalmology 2015;122:1899–906.
Grover S, Fishman GA, Anderson RJ, Lindeman M. A longitudinal study of visual function in carriers of X-linked recessive retinitis pigmentosa. Ophthalmology 2000;107:386–96.
Roberts MF, Fishman GA, Roberts DK, Heckenlively JR, Weleber RG, Anderson RJ, et al. Retrospective, longitudinal, and cross sectional study of visual acuity impairment in choroideraemia. Br J Ophthalmol. 2002;86:658–62.
World Health Organization. Consultation on development of standards for characterization of vision loss and visual functioning: Geneva, 4-5 September 2003. Published online 2003. Accessed 13 March 2021. https://apps.who.int/iris/handle/10665/68601
Friedrich U, Warburg M, Kruse TA, Andréasson S. X-linked retinitis pigmentosa: new map studies of XLRP2, and a possible human centromere effect. Hum Genet. 1992;88:683–7.
Fishman GA, Weinberg AB, McMahon TT. X-linked recessive retinitis pigmentosa. Clinical characteristics of carriers. Arch Ophthalmol. 1986;104:1329–35.
Lyon MF. Gene action in the X-chromosome of the mouse (Mus musculus L.). Nature. 1961;190:372–3.
Wu H, Luo J, Yu H, Rattner A, Mo A, Wang Y, et al. Cellular resolution maps of X chromosome inactivation: implications for neural development, function, and disease. Neuron 2014;81:103–19.
Bax NM, Valkenburg D, Lambertus S, Klevering BJ, Boon CJF, Holz FG, et al. Foveal sparing in central retinal dystrophies. Invest Ophthalmol Vis Sci. 2019;60:3456–67.
Neidhardt J, Glaus E, Lorenz B, Netzer C, Li Y, Schambeck M, et al. Identification of novel mutations in X-linked retinitis pigmentosa families and implications for diagnostic testing. Mol Vis. 2008;14:1081–93.
Jin Z-B, Liu X-Q, Hayakawa M, Murakami A, Nao-i N. Mutational analysis of RPGR and RP2 genes in Japanese patients with retinitis pigmentosa: identification of four mutations. Mol Vis. 2006;12:1167–74.
Prokisch H, Hartig M, Hellinger R, Meitinger T, Rosenberg T. A population-based epidemiological and genetic study of X-linked retinitis pigmentosa. Invest Ophthalmol Vis Sci. 2007;48:4012–8.
Kurata K, Hosono K, Hayashi T, Mizobuchi K, Katagiri S, Miyamichi D, et al. X-linked retinitis pigmentosa in Japan: clinical and genetic findings in male patients and female carriers. Int J Mol Sci. 2019;20:1518.
Ji Y, Wang J, Xiao X, Li S, Guo X, Zhang Q. Mutations in RPGR and RP2 of Chinese patients with X-linked retinitis pigmentosa. Curr Eye Res. 2010;35:73–79.
Flaxel C, Jay M, Thiselton D, Nayudu M, Hardcastle A, Wright A, et al. Difference between RP2 and RP3 phenotypes in X linked retinitis pigmentosa. Br J Ophthalmol. 1999;83:1144–8.
Kühnel K, Veltel S, Schlichting I, Wittinghofer A. Crystal structure of the human retinitis pigmentosa 2 protein and its interaction with Arl3. Structure 2006;14:367–78.
Li H-P, Yuan S-Q, Wang X-G, Sheng X-L, Li X-R. Myopia with X-linked retinitis pigmentosa results from a novel gross deletion of RPGR gene. Int J Ophthalmol. 2020;13:1306–11.
Miano MG, Testa F, Filippini F, Trujillo M, Conte I, Lanzara C, et al. Identification of novel RP2 mutations in a subset of X-linked retinitis pigmentosa families and prediction of new domains. Hum Mutat. 2001;18:109–19.
Acknowledgements
None.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
OBS, and RGC, participated in study design, data collection, data analysis, manuscript writing, as well as manuscript review and editing. EIT participated in study design, data analysis, manuscript writing, as well as manuscript review editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Saeed, O.B., Traboulsi, E.I. & Coussa, R.G. Profiling of visual acuity and genotype correlations in RP2 patients: a cross-sectional comparative meta-analysis between carrier females and affected males. Eye 37, 350–355 (2023). https://doi.org/10.1038/s41433-022-01954-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-022-01954-2