Learning Objectives
Upon completion of this activity, participants will:
-
1.
Describe DALYs caused by paediatric vision impairment in different age groups by socioeconomic indicators and other factors in 2017, according to a retrospective analysis of GBD data.
-
2.
Determine the trend from 1990 to 2017 in DALYs caused by paediatric vision impairment in different age groups, according to a retrospective analysis of GBD data.
-
3.
Identify clinical and public health implications of findings regarding DALYs caused by paediatric vision impairment in different age groups, according to a retrospective analysis of GBD data.
Continuing Medical Education
In support of improving patient care, this activity has been planned and implemented by Medscape, LLC and Springer Nature. Medscape, LLC is jointly accredited by the Accreditation Council for Continuing Medical Education (ACCME), the Accreditation Council for Pharmacy Education (ACPE), and the American Nurses Credentialing Center (ANCC), to provide continuing education for the healthcare team.
Medscape, LLC designates this Journal-based CME activity for a maximum of 1.0 AMA PRA Category 1 Credit(s)™. Physicians should claim only the credit commensurate with the extent of their participation in the activity.
Successful completion of this CME activity, which includes participation in the evaluation component, enables the participant to earn up to 1.0 MOC points in the American Board of Internal Medicine’s (ABIM) Maintenance of Certification (MOC) program. Participants will earn MOC points equivalent to the amount of CME credits claimed for the activity. It is the CME activity provider’s responsibility to submit participant completion information to ACCME for the purpose of granting ABIM MOC credit.
Credit hours
1.0
Expiration date:
Release date:
Post-test link: https://medscape.org/eye/posttest949866
Authors/Editors disclosure information
Sobha Sivaprasad, MD, has disclosed the following relevant financial relationships: Served as an advisor or consultant for: Allergan, Inc.; Apellis Pharmaceuticals; Bayer AG; Boehringer Ingelheim Pharmaceuticals, Inc.; Heidelberg Pharma GmbH; Novartis Pharmaceuticals Corporation; Oculis; Optos; Oxurion NV; Roche. Served as a speaker or a member of a speakers bureau for: Allergan, Inc.; Bayer AG; Novartis Pharmaceuticals Corporation; Optos. Received grants for clinical research from: Allergan, Inc.; Bayer AG; Boehringer Ingelheim Pharmaceuticals, Inc.; Novartis Pharmaceuticals Corporation; Optos. Parya Abdolalizadeh, MD, MPH, disclosed has no relevant financial relationships. Samira Chaibakhsh, PhD, disclosed has no relevant financial relationships. Khalil Ghasemi Falavarjani, MD, disclosed has no relevant financial relationships.
Abstract
Objective
To assess the trend of paediatric visual impairment and its disparities by year, sex, age and national socioeconomic levels using disability-adjusted life years (DALYs).
Methods
It is a retrospective analysis of data from the Global Burden of Disease (GBD) 2017. Global and national DALY numbers and rates of vision impairment in three paediatric age groups of 1–4 (preschool children), 5–9 (school children) and 10–14 years (teenagers) years were obtained from the GBD 2017 database. The socioeconomic indices for 195 countries were derived from international open databases. Main outcome measures were comparison of DALYs due to paediatric vision impairment in different age groups by socioeconomic indicators in 2017 and analysis of the trend from 1990.
Results
The global prevalence of distance and/or near vision impairment for 1–14 years was 2.8% (95% uncertainty interval (UI): 2.5–3.1) in 2017. The highest DALYs for distance and/or near vision impairment [number=589.93 thousands (95%UI: 367.71–933.29), rate = 92.72 (95%UI: 57.79–146.68)] were observed in teenagers. DALY rate of distance and/or near vision impairment was not associated with socioeconomic indicators, however, DALY rate of refractive disorders had positive correlation with national socioeconomic development. The global trends of DALY numbers in distance and/or near vision impairment as well as refractive and other causes remained stable from 1990 to 2015 (0.128 ≤ P ≤ 0.738), however, DALY rates had a statistically significant trend of reduction in all paediatric age groups (0.003 ≤ P ≤ 0.024).
Conclusion
The global health burden of paediatric vision impairment decreased from 1990. Refractive, near vision impairment and other causes were associated with socioeconomic development.
Similar content being viewed by others
Introduction
The global population with vision impairment was 252 million in 2015, among them 216 million people had low vision (3/60≤ visual acuity <6/18 in the better eye) and 16 million were blind (visual acuity <3/60 in the better eye) [1]. It has been estimated that the number of people with vision impairment will rise to 275 million by 2020, worldwide [1]. The Global Burden of Disease (GBD) study showed that vision impairment was the third-ranked disability in terms of disability-adjusted life years (DALY) after anaemia and hearing loss worldwide, from 1990 to 2017 [2]. Childhood blindness and visual impairment are important public health issues worldwide[3]. The WHO estimated 1.4 million blind children (under 18 years) globally in 2000 [3]. According to the global estimation in 2010, 19 million children with ages less than 14 years had vision impairment [3].
In addition to the prevalence data, knowledge of the burden of paediatric vision impairment enables comparisons of epidemiologic patterns over time and across countries which is valuable for health policy making and resource allocations. The health burden of disease can be measured by DALY which compares the current status with an ideal condition in which people live up to the age of standard life expectancy in perfect health. The years lived with disability (YLD) part of DALY reflects both the age of onset and severity of the disability; more severe disability at younger age, the higher YLD. Therefore, health burden of paediatric vision impairment can be more devastating due to lower age of onset and the potential lifespan of children.
The health burden of common ocular diseases in adult age groups, including uncorrected refractive disorders, cataract, glaucoma and age-related macular degeneration has been already reported [4,5,6,7,8]. However, limited studies have focused on health burden of vision impairment in paediatric age groups notably considering the prevalence, not the DALY [9, 10]. Global estimations in 1999, reported an overall prevalence of 0.1 to 1.1 per 1000 children, with higher prevalence in low income countries [9]. The aim of this study was to evaluate the global health burden of paediatric visual impairment across countries with different national levels of socioeconomic development and its time trends using the DALY data available from the GBD 2017.
Methods
This study used the GBD 2017 data obtained from Global Health Data Exchange (GHDx) supported by the Institute for Health Metrics and Evaluation (IHME). GHDx provides a resource for prevalence and health burden of 359 diseases and injuries including some eye diseases across 195 countries/territories from 1990 to 2017 [11].
GHDx defines vision impairment and blindness as visual acuity (VA) < 6/12 and VA < 3/60 respectively [11]. Near vision impairment was also defined as a near visual acuity less than N6 at 40 centimetres [12]. Refractive disorders, near vision loss, cataract, glaucoma, macular degeneration, and other causes are subgroups of vision impairment in GHDx, however, cataract, glaucoma and macular degeneration are not considered in paediatric age groups (≤14 years) [13]. Therefore, we used data of distance and/or near vision impairment and blindness due to eye disease, and subgroups of refractive disorders, near vision impairment, and other causes of vision impairment in three paediatric age groups in this study adopting ‘cause’ option under ‘context’ tag in searching strategies of GBD. The age groups were defined in accordance with the GHDx categories: 1–4 (preschool children), 5–9 (school children), and 10–14 (teenagers) years old.
DALY is a comprehensive indicator of disease burden that is calculated by summing the healthy years of life lost due to disability (years lived with disability, YLD) or premature death (years of life lost, YLL). The human development index (HDI) has been developed to compare the socioeconomic level across countries by considering years of school education, expected years of school education, life expectancy, and gross national income. The result of HDI is reported in a range of 0 to 1, with higher values showing more socioeconomic development. Moreover, the countries have been divided into four socioeconomic subgroups: low (0-0.549), medium (0.550–0.699), high (0.700–0.799), and very high (0.800–1.000) HDI. The Inequality-adjusted HDI adjusts the HDI for inequality in the distribution of each dimension in that population. Gross domestic product (GDP) per capita of individual countries is another common indicator for national wealth and economic progress as calculated by purchasing power parity (constant 2011 international US dollar). The Socio-demographic index (SDI) is a composite indicator of income per capita, average educational attainment in the population over 15 years, and the total fertility rates, ranging from 0 to 1, with higher numbers imply higher educational attainment, higher income per capita, and lower fertility rate [13].
The calculation method of DALY has been previously reported in the methodological reports of GBD study [2]. Briefly, the DALY number shows the total DALY due to paediatric eye disease in a country. The DALY rate reflects the health burden is calculated by accounting population size (DALY per 100,000 populations). The age-standardized DALY rate was not calculated for this study because we assessed the DALY of vision impairment in each paediatric age group separately. Therefore, the global DALY numbers and crude rates of three paediatric age groups in 5-year intervals (1990, 1995, 2000, 2005, 2010 and 2015) as well as the DALY numbers and crude rates in individual countries in 2017 were retrieved for statistical analysis.
The national level of HDI, Inequality-adjusted HDI and the number of medical doctors per 10000 people in 2017 were extracted from the Human Development Report (http://hdr.undp.org/en/data), which was released by United Nations Development Program (UNDP). Gross domestic product (GDP) was obtained from the World Bank open database in 2017 (http://data.worldbank.org/). The country-level SDI in 2017 was available in the open database of the GHDx (http://ghdx.healthdata.og/). Global maps were generated using the data visualization tool of the GHDx (https://vizhub.healthdata.org/gbd-compare/).
Trend analysis of DALY numbers and DALY rates in each age-subgroup during study years were performed using regression model with auto-correlated errors by R 3.6.3 software (R Development Core Team, New Zealand). Other Statistical analyses were performed using SPSS software version 24 (SPSS, Inc, Chicago, IL, USA). Analysis of variance test was used to compare the mean DALY rate across countries of different HDI subclasses. Levene test was utilized for assessing homogeneity of variances. The correlation between five socioeconomic indicators and DALY rates were evaluated by Pearson correlation test. Comparison of national DALY numbers and rates between sex categories was performed by the independent Student’s t-tests in each age group. Results were considered statistically significant at P < 0.05.
Results
Global overview of the prevalence and health burden of visual impairment in 2017
In 2017, the prevalence of distance and/or near vision impairment in children aged 1–14 years was 2.8% (95% Uncertainty Interval (UI): 2.5–3.1) worldwide. About 3% of teenagers [3.5% (95% UI: 2.9–4.3)] suffered from distance and/or near vision impairment who had the highest prevalence among paediatric age groups followed by school children [3.0% (95% UI: 2.4–3.8)] and preschool children [2.0% (95% UI: 1.6–2.5)]. Table 1 shows the global DALY numbers and rates for paediatric age groups in GBD 2017. The DALY number and rate of teenagers were higher than preschool and school children (Table 1). India and China had the highest DALY numbers of distance and/or near vision impairment in all three paediatric age groups. The lowest DALY number was observed for Dominica. Israel was placed in the top rank in terms of DALY rate after adjustment for population size while Barbados and Sweden had the lowest DALY rates (Supplementary Tables 1–3).
Prevalence and DALY of refractive disorders
The prevalence of children aged 1–14 years with refractive disorders was 1.8% (95% UI: 1.5–2.1). The prevalence was 2.1% (95% UI: 1.5–2.8) in school children, 2% (95% UI: 1.4–2.7) in teenagers and 1.6% (95% UI: 1.2–2) in preschool children which were close to each other. The DALY number was the highest in school children while DALY rate was similar between school children and teenagers (Table 1). India and China were the top two countries with highest DALY numbers in all paediatric age groups in 2017. The highest DALY rate was observed in Israel, Papua New Guinea and Myanmar. The lowest DALY number and rate were observed in Dominica and Barbados, respectively (Supplementary Tables 1–3).
Prevalence and DALY of near vision impairment
About 0.7% (95% UI: 2.5–3.1) of children between 1 and 14 years had near vision impairment in 2017. The highest prevalence was observed in teenagers [1.4% (95% UI: 1.3–1.6)] followed by school children [0.9% (95% UI: 0.8–1.0)] and preschool children [0.4% (95% UI: 0.3–0.4)]. Similar ranking was found in DALY number and rate (Table 1). The DALY number of paediatric near vision impairment was highest in India and China. However, paediatric near vision impairment showed different global pattern regarding to DALY rates (per 100,000), being the greatest in Mauritania, central Africa and democratic republic of Congo in 3 paediatric age groups. The lowest DALY number and rate was observed in Andorra and Denmark, respectively (Supplementary Tables 1–3).
Prevalence and DALY of other causes
The global prevalence of paediatric vision impairment due to other causes was 0.1% (95% UI: 0.1–0.2). The prevalence in each separate age group was the same [0.1% (95% UI: 0.1–0.2)]. The DALY numbers and DALY rates had the highest values in teenagers among all paediatric age groups (Table 1). China and India remained the top countries for the DALY numbers in all paediatric age groups for other causes of vision impairment, while the highest rates of DALY (per 100,000) were observed in Israel and Oman. The lowest DALY number was in Dominica. Bhutan had the lowest DALY rate in school children and teenagers and Barbados had lowest DALY rate in preschool children (Supplementary Tables 1–3).
Global health burden of paediatric vision impairment in 2017 by gender
The mean DALY numbers of distance and/or near vision impairment in female vs. males were 837.02 ± 3124.56 vs. 884.57 ± 3216.09 in preschool children (P = 0.87), 1506.76 ± 5751.83 vs. 1540.34 ± 5556.59 in school children (P = 0.96) and, 1606.60 ± 6327.34 vs. 1578.05 ± 5705.58 in teenagers (P = 0.97). The mean DALY rate of distance and/or near vision impairment was not statistically significantly different between males and females in preschool children (57.46 ± 20.47 vs. 57.14 ± 20.37, respectively, P = 0.88), school children (81.67 ± 26.86, 82.86 ± 25.76, respectively, P = 0.66) and teenagers (87.81 ± 28.36, 91.00 ± 27.40, respectively, P = 0.27) in 2017.
Association of global health burden of paediatric vision impairment in 2017 with socioeconomic factors
DALY rate of distance and/or near vision impairment
The DALY rate of total visual impairment did not have any correlation with five socioeconomic factors in three age groups (Table 2) except a weak correlation between HDI and DALY rate (r = 0.17, P = 0.02) as well as inequality-adjusted HDI and DALY rate (r = 0.21, P = 0.01) in preschool children. Furthermore, the mean DALY rates were similar among countries with various HDI levels (P for preschool children = 0.11, P for school children = 0.62, P for teenagers = 0.87).
DALY rate of refractive disorders
The health burden of refractive disorders correlated significantly with HDI, inequality-adjusted HDI, SDI and number of physicians in three age groups although the strength of correlation was weak (Table 2). The DALY rate of refractive disorders was statistically significantly different among countries with different levels of HDI in preschool children (P = 0.004), school children (P = 0.007) and teenagers (P = 0.02).
DALY rate of near vision impairment
The DALY rate of near vision impairment was significantly associated with five socioeconomic indictors. The DALY rate increased with reduction of HDI, inequality-adjusted HDI, SDI, GDP and number of physicians (Table 2). In addition, 4 HDI subgroups had different mean DALY rates in terms of near vision impairment in children (P < 0.001 for all age groups).
DALY rate of other causes of vision impairment
The HDI, inequality-adjusted HDI, SDI and number of physicians were inversely correlated with DALY rate of other causes of vision impairment in school children and teenagers (Table 2). Statistically significant difference in DALY rates was found between countries with different levels of HDI in school children (P = 0.04) and teenagers (P = 0.002) except for preschool children (P = 0.68).
Trend of DALY from 1990 to 2015
The prevalence of distance and/or near vision impairment in the paediatric age group was 2.9% (95% UI: 2.5–3.3) in 1990 that was changed to 2.8% (95% UI: 2.6–3.0) in 2015. Table 3 shows the DALY numbers and DALY rates in 1990 and 2015 as well as their trends between 1990 and 2015 in three paediatric age groups.
DALY of distance and/or near vision impairment
No statistically significant trend for DALY numbers was detected in all paediatric age groups between 1990 and 2015 (Fig. 1A). There was a statistically significant decrease in DALY rates in three age groups during the same period (Fig. 2A, Table 3). Trend analysis showed −0.25 (SE = 0.05, P = 0.007) decrease of DALY rate in preschool children (1–4 years old), −0.33 (SE = 0.09, P = 0.02) in school children (5–9 years old) and −0.35 (SE = 0.10, P = 0.02) in teenagers per year.
DALY of refractive disorders
The DALY rates decreased significantly in three paediatric age groups, however, no significant trend was observed for DALY numbers from 1990 to 2015 (Table 3, Figs. 1B and 2B). The decrease of DALY rate per year in three age groups followed the same trend; −0.22 (SE = 0.05, P = 0.009) in preschool children, −0.31 (SE = 0.09, P = 0.02) in school children and, −0.33 (SE = 0.09, P = 0.02) in teenagers.
DALY of near vision impairment
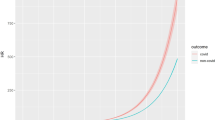
The DALY number and rate increased from 1990 to 2015 however, the trend of changes was statistically significant for DALY numbers of all age groups and DALY rate of teenagers (Table 3, Figs. 1C and 2C). The teenagers had the highest increase of DALY number per year [631.57 (SE = 145.42, P = 0.01)] followed by school children [257.42 (SE = 17.52, P < 0.001)] and preschool children [75.24 (SE = 7.55, P = 0.001)]. The increase in DALY rate of near vision impairment in teenagers was 0.04 (SE = 0.01, P = 0.005) per year.
DALYs of other causes
A statistically significant decrease in DALY rates was observed between 1990 and 2015 in all age groups (Figs. 1D and 2D, Table 3). The DALY rate decreased −0.03 (SE = 0.01, P = 0.003) in preschool children, −0.04 (SE = 0.01, P = 0.005) in school children and −0.06 (SE = 0.01, P = 0.003) in teenagers per year.
DALY of distance and/or near vision impairment trend analysis in sex subgroups revealed that DALY rates were decreased statistically significantly from 1990 to 2015 for both genders. The change of DALY rate for males was −0.24 (SE = 0.05, P = 0.009) in preschool children, −0.33 (SE = 0.10, P = 0.03) in school children and, −0.38 (SE = 0.10, P = 0.02) in teenagers per year. The change was −0.26 (SE = 0.05, P = 0.006), −0.32 (SE = 0.08, P = 0.02), and −0.32 (SE = 0.09, P = 0.03) per year for the preschool, school and teenage females, respectively, during the same period.
Discussion
In this study, the DALY rate of total visual impairment in three paediatric age groups decreased significantly from 1990 to 2015, while the crude DALY numbers remained stable. The same pattern was observed in refractive disorders and other causes of vision impairment. These findings suggest an improving trend in global eye health in children that may be attributed to the advances in screening, diagnosis and treatment of paediatric vision impairment [10, 14]. Paediatric vision impairment is either avoidable or treatable in majority of cases [9, 10, 15]. National and international programs such as VISION 2020 (The Right to Sight) have emphasized the control of childhood vision impairment through developing and implementing screening programs and cost-effective interventions [10, 14, 15]. VISION 2020 has been launched in 2000 to reduce the global prevalence of avoidable childhood blindness from 0.75 to 0.4 per 1000 children by the year 2020 [14]. This program has focused on screening of refractive disorders and retinopathy of prematurity (ROP) as well as eliminating the ocular morbidities with infectious or malnutrition aetiologies [13]. Improvements in DALY rates may reflect an improvement in interventions in this age group. However, constant amount of crude DALY numbers between 1990 and 2015 implies either growth of paediatric population (population aged 0–14 years old increased from 1.73 billion at 1990 to 1.92 billion at 2015) [16], longer life expectancies (increased from 65.43 years at 1990 to 71.95 at 2015) [16] and/or increasing incidence of paediatric visual impairment.
The significant cause of inequality in eye health has been attributed to socioeconomic disparities influencing the number of ophthalmologists per million people, with more concentration in regions with higher GDP per capita and HDI [17,18,19]. Furthermore, the HDI is directly related to the level of education which affects the annual use of eye services and affordability of the costs [20, 21]. Higher age-standardized DALY rates of common ocular diseases in adults have been reported to be associated with lower socioeconomic levels [4,5,6,7]. It was also demonstrated that low income increases the incidence of sight-threatening conditions and limits the delivery of treatments in adults [8]. We found no significant correlation except positive weak correlation between DALY rate of preschool children with these socioeconomic indicators. Similar results between DALY and all socioeconomic indices indicate the robustness and reliability of our findings. The DALY rate did not differ between low, medium, high and very high income countries, implying that the health burden of distance and/or near vision impairment in children is equally distributed in recent years. However, it does not mean similar prevalence of different causes of vision impairment in countries with different socioeconomic levels.
A recent meta-analysis in 2020 showed higher prevalence of refractive disease in school children in Asia and Europe comparing to the Africa and South America with lower socioeconomic levels [22]. Our results are in agreement with global trends and showed that health burden of refractive disorders had uneven distribution across countries in all paediatric age groups; higher socioeconomic levels in terms of HDI, inequality-adjusted HDI, SDI, and number of physician were associated with higher DALY rates (Table 2). The main proposed hypothesis is lifestyle change and environmental factors including incremental near work tasks, excessive use of near electronic devices and decreased outdoor activities which usually occur in children of wealthy countries [22]. On the other hand, this pattern contradicted to the relationship of socioeconomic levels with near vision impairment and other causes of vision impairment (Table 2). Therefore, the effect of refractive disorders on burden of distance and/near (total) vision impairment may be dampened by the effects of near vision impairment and other causes of vision impairment. Additionally, factors, other than affordability [23, 24], affect the DALYs of refractive errors in paediatrics comparing to the adults age group. Although paediatric refractive errors can be corrected by the spectacles as a non-invasive, inexpensive and cost-effective method, the compliance rate of children is less than half [25]. The suboptimal compliance with spectacle is higher in upper-middle-income countries [26] which may also contribute the high burden of paediatric refractive errors in countries with high socioeconomic levels despite of the availability of treatment. Another barrier of treatment in paediatric refractive error is true diagnosis that is under-detected even in developed countries due to particular difficulties in paediatric vision assessment and ocular examination [27, 28].
In GBD, near vision impairment has been considered as difficulty with near vision tasks at a reading distance. Some factors including distance visual acuity, accommodation capability, and near vision correction affect the near visual acuity [29]. The frequency of accommodative insufficiency ranges between 0.2 and 39 percent in paediatrics which decreases the near-distance performance [30, 31] On the other hand, some paediatric ocular disease such as congenital cataract, retinopathy of prematurity corneal disorders and, etc. contributes to simultaneous distance and near vision impairment. Low vision in children especially at near distance can be improved by low vision aids [26]. Our results revealed a disproportionate distribution of the burden of near vision impairment in children. Poor African countries, such as Mauritania, Central Africa and democratic republic of Congo, with lower socioeconomics have the highest DALY rates in all paediatric age groups. Strong correlation between five socioeconomic indices and DALY rates also supported the results. Beyond the poor health services to treat the underlying ocular disease, it may be due to the expense of low vision aids especially non-optical and electronic devices as well as poor social and educational cares [10, 32, 33].
The category of ‘other causes’ of vision impairment in GDHx database includes a total of 57 eye conditions including congenital cataract, congenital glaucoma, acquired infectious disease, corneal opacities, and ROP [34]. Wide international variations were reported for the causes of paediatric blindness and severe vision loss in 2000 [9, 10, 13, 35]. The level of regional socioeconomic development and eye health services have been proposed as the main causes of the disparity [10, 35]. Our study showed a weak correlation between the health burden of the ‘other causes’ of vision loss and socioeconomic level of countries. However, we cannot conclude equal distribution of the other causes worldwide because this category of GBD is a heterogenic group of different ocular conditions. More investigations are needed to explore the global health burden of each disease in relation to the development and socioeconomic conditions.
This study has some limitations. First, data were unavailable in some subcategories for few countries. Second, data for some potential confounders, such as environmental and genetic factors, was not included in GBD [36]. Similarly, correlations between DALYs and SDIs should not be considered as causal. In addition, some causes of vision loss among children, such as ROP, hereditary anomalies, congenital cataract and congenital glaucoma, have not been separately investigated in the GHDx database, probably because of the rarity of the conditions and limited reliable population-based data. This may result in underestimating the magnitude of these condition [10, 37]. The results of this study is likely to underestimate the vision impairment burden of children because we focused on children younger than 14 years old. Despite these shortcomings, GHDx is the most precise and standard database to evaluate the global health burdens owing to the paediatric ocular disease across time and places. To be comparable to the previous studies, the trends of the DALYs were reported in 5-year intervals [4,5,6,7]. However, we further analysed and reported the trends of changes per year. The trend analysis of DALYs in more recent years (2015–2020) needs additional studies. On the other hand, the use of DALYs in paediatric epidemiology has the limits of age-weighting regarding to childhood onset impairment with lifelong impact. It does not consider whether every year of life is ‘equal’ or whether disabled years in early versus late childhood confer differential burden. Additionally, the life expectancy as a component of DALY, differs significantly across health care settings and it should be noticed when attempting comparisons between countries.
In conclusion, to the best of our knowledge, this is the first report of the health burden of paediatric vision loss in the context of international socioeconomic conditions. Our findings emphasize on investment to maintain and extend paediatric eye health programs to screen, diagnose and manage the refractive disorders with the largest and growing DALY number in all socioeconomic levels. However, facilities, skilled personnel and preventive measures need to be continued for other causes of paediatric vision impairment all over the world. The rehabilitation centres and therapeutic strategies for near vision impairment should be considered particularly to the countries with low socioeconomics, where a higher health burden in children was detected.
Summery
What was known before?
-
According to the global estimation in 2010, 19 million children with ages less than 14 years had vision impairment.
-
The DALY of most common adult eye disease including cataract, glaucoma and age-related macular degeneration have been correlated with socioeconomic levels of countries.
What this study adds?
-
The prevalence of paediatric vision impairment was 2.8% in 2017.
-
The DALY rates of visual impairment in paediatric age groups decreased nearly 0.3 per year over 25 years.
-
Refractive, near vision impairment and other causes of vision impairment in paediatrics were associated with socioeconomic development.
References
Flaxman SR, Bourne RRA, Resnikoff S, Ackland P, Braithwaite T, Cicinelli MV, et al. Vision loss expert group of the Global Burden of Disease Study. Global causes of blindness and distance vision impairment 1990-2020: a systematic review and meta-analysis. Lancet Glob Health. 2017;5:e1221–e1234.
GBD. DALYs and HALE Collaborators. Global, regional, and national disability-adjusted life-years (DALYs) for 359 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392:1859–922. 2017
Pascolini D, Mariotti SP. Global estimates of visual impairment: 2010. Br J Ophthalmol. 2012;96:614–8.
Wang W, He M, Li Z, Huang W. Epidemiological variations and trends in health burden of glaucoma worldwide. Acta Ophthalmol. 2019;97:e349–e355.
He M, Wang W, Huang W. Variations and trends in health burden of visual impairment due to cataract: a global analysis. Invest Ophthalmol Vis Sci. 2017;58:4299–306.
Wang D, Jiang Y, He M, Scheetz J, Wang W. Disparities in the global burden of age-related macular degeneration: an analysis of trends from 1990 to 2015. Curr Eye Res. 2019;44:657–63.
Lou L, Yao C, Jin Y, Perez V, Ye J. Global patterns in health burden of uncorrected refractive error. Invest Ophthalmol Vis Sci. 2016;57:6271–7.
Lane M, Lane V, Abbott J, Braithwaite T, Shah P, Denniston AK. Multiple deprivation, vision loss, and ophthalmic disease in adults: Global perspectives. Surv Ophthalmol. 2018;63:406–36.
Gilbert CE, Anderton L, Dandona L, Foster A. Prevalence of visual impairment in children: a review of available data. Ophthalmic Epidemiol. 1999;6:73–82.
Gilbert C, Foster A. Childhood blindness in the context of VISION 2020 the right to sight. Bull World Health Organ. 2001;79:227–32.
Global Health Data Exchange. GBD Data Tool. Available at: http://ghdx.healthdata.org/gbd- results-tool. Accessed February 25, 2020.
WHO World report on vision Available at: https://www.who.int/publications/i/item/world-report-on-vision. Accessed March 6, 2021.
Measuring the health-related Sustainable Development Goals in 188 countries: a baseline analysis from the Global Burden of Disease Study 2015. GBD 2015 SDG Collaborators. Lancet. 2016;388:1813-50.
World Health Organization. Preventing blindness in children, Report of a WHO/ IAPB scientific meeting. Geneva:WHO. 2000. (WHO/PBL/00.77).
Action plan for the prevention of avoidable blindness and visual impairment 2014–2019: towards universal eye health: a global action plan 2014–2019. Available at: http://www.who.int/blindness/actionplan/en/index.html. Accessed March 7, 2020.
https://data.worldbank.org/indicator/. Accessed October 30, 2020.
Hong H, Mujica OJ, Anaya J, Lansingh VC, Lopez E, Silva JC. The challenge of universal eye health in Latin America: distributive inequality of ophthalmologists in 14 countries. BMJ Open. 2016;6:e12819.
Resnikoff S, Felch W, Gauthier TM, Spivey B. The number of ophthalmologists in practice and training worldwide: a growing gap despite more than 200,000 practitioners. Br J Ophthalmol. 2012;96:783–7.
Trimmel J. Inequality and inequity in eye health. Community Eye Health. 2016;29:1–3.
Wagner LD, Rein DB. Attributes associated with eye care use in the United States: a meta-analysis. Ophthalmology. 2013;120:1497–501.
Holden BA, Fricke TR, Wilson DA, Jong M, Naidoo KS, Sankaridurg P, et al. Global prevalence of myopia and high myopia and temporal trends from 2000 through 2050. Ophthalmology. 2016;123:1036–42.
Grzybowski A, Kanclerz P, Tsubota K, Lanca C, Saw SM. A review on the epidemiology of myopia in school children worldwide. BMC Ophthalmol. 2020;20:27.
Thompson S, Naidoo K, Gonzalez-Alvarez C, Harris G, Chinanayi F, Loughman J. Barriers to use of refractive services in Mozambique. Optom Vis Sci. 2015;92:59–69.
Marmamula S, Keeffe JE, Raman U, Rao GN. Population-based cross-sectional study of barriers to utilisation of refraction services in South India: Rapid Assessment of Refractive Errors (RARE) Study. BMJ Open. 2011;1:e000172.
Dhirar N, Dudeja S, Duggal M, Gupta PC, Jaiswal N, Singh M, et al. Compliance to spectacle use in children with refractive errors- a systematic review and meta-analysis. BMC Ophthalmol. 2020;20:71.
Labib TA, El Sada MA, Mohamed B, Sabra NM, Abdel Aleem HM. Assessment and management of children with visual impairment. Middle East Afr J Ophthalmol. 2009;16:64–8.
O’Donoghue L, Rudnicka AR, McClelland JF, Logan NS, Saunders KJ. Visual acuity measures do not reliably detect childhood refractive error-an epidemiological study. PLoS ONE. 2012;7:e34441.
Qiu M, Wang SY, Singh K, Lin SC. Racial disparities in uncorrected and undercorrected refractive error in the United States. Invest Ophthalmol Vis Sci. 2014;55:6996–7005.
Vos JJ, Padmos P, Boogaard J. Occupational testing of near vision. Ophthalmic Physiol Opt. 1994;14:413–8.
Hashemi H, Khabazkhoob M, Nabovati P, Shahraki FA, Ostadimoghaddam H, Faghihi M, et al. Accommodative insufficiency in a student population in Iran. J Optom. 2019;12:161–7.
Sterner B, Gellerstedt M, Sjöström A. Accommodation and therelationship to subjective symptoms with near work for youngschool children. Ophthalmic Physiol Opt. 2006;26:148–55.
Lee SMY, Cho JCW. Low vision devices for children. Commun Eye Health. 2007;20:28–29.
Dijk KV. Providing care for children with low vision. Commun Eye Health. 2007;20:24–25.
Boyers LN, Karimkhani C, Hilton J, Richheimer W, Dellavalle RP. Global burden of eye and vision disease as reflected in the Cochrane Database of Systematic Reviews. JAMA Ophthalmol. 2015;133:25–31.
Courtright P, Hutchinson AK, Lewallen S. Visual impairment in children in middle- and lower-income countries. Arch Dis Child. 2011;96:1129–34.
Adhikari S, Shrestha MK, Adhikari K, Maharjan N, Shrestha UD. Factors associated with childhood ocular morbidity and blindness in 3 ecological regions of Nepal: Nepal pediatric ocular disease study. BMC Ophthalmol. 2014;14:125.
Stevens GA, White RA, Flaxman SR, Price H, Jonas JB, Keeffe J, et al. Vision loss expert group. global prevalence of vision impairment and blindness: magnitude and temporal trends, 1990-2010. Ophthalmology. 2013;120:2377–84.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
PA was responsible for the designing of the work, data extraction, interpretation of the results, drafting the work, and approve of the final version to be published. SC was responsible for the analysis and approval of the final version to be published. KGF had substantial contributions to the conception or design of the work, revise the draft critically for important intellectual content, and approve of the final version to be published.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Abdolalizadeh, P., Chaibakhsh, S. & Falavarjani, K.G. Global burden of paediatric vision impairment: a trend analysis from 1990 to 2017. Eye 35, 2136–2145 (2021). https://doi.org/10.1038/s41433-021-01598-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-021-01598-8