Abstract
Vision impairment (VI) is an important contributor to the global burden of disability and is associated with decreased well-being. Recent research has attempted to devise a conceptual framework to explain the health consequences of VI. One proposed mechanism by which VI leads to declines in well-being and other adverse health and disability outcomes is through limitations in social participation (SP). SP is an integral component of overall functioning, optimal aging, and well-being, and reductions in SP are associated with lower health-related quality of life. The purpose of this systematic review was to appraise the existing literature on the relationship between VI and SP. The protocol for this review was registered on PROSPERO (CRD42018102767) and adhered to PRISMA guidelines. A comprehensive search of five databases (MEDLINE, EMBASE, PsycINFO, Scopus, Sociology Database) yielded 881 unique studies, of which 19 met inclusion criteria. Among the 19 included studies, 18 concluded that VI was associated with reduced SP and one reported mixed results. Bias was assessed using the Effective Public Health Practice Project Quality Assessment. In the quality assessment, four studies were rated “moderate” and fifteen were rated “weak.” There was wide variation in study populations and measurement of VI and SP. In conclusion, there is consensus that VI is associated with reduced SP. However, more rigorous study design and better standardization in the assessment of VI and SP could facilitate valid comparisons across populations, diseases, and levels of VI. Attempts to provide vision rehabilitation and mitigate the effects of VI on overall health and well-being might consider strategies to improve SP.
摘要
视力损伤 (VI) 是造成全球残疾负担的重要因素并且与人的幸福感降低有关。近期的一项研究设计了一个概念框架来说明VI对健康的影响。其中一个可能的机制是, VI导致幸福感降低的机制之一是参与社会活动受限。社会参与度是组成整体功能, 最佳老龄状态和幸福感的一部分, 社会参与度减少与健康的生活质量下降有关。本篇系统回顾旨在评价已发表的关于VI与社会参与度相关性的文章。本篇系统综述的实施方案登记在PROSPERO (CRD42018102767), 并且遵照PRISMA指南。对五个数据库(MEDLINE, EMBASE, PsycINFO, Scopus, Sociology Database)进行系统文献检索, 共涵盖881个不同的研究, 其中19篇符合入选标准。在这19篇入选文章中, 18篇的结论是VI与社会参与度下降有关, 1篇文章的结论不明确。是否存在偏倚采用EPHPPQA方法进行评估。在文章质量评估中, 4篇文章被评为“可信度中等”, 15篇文章被评为“可信度低”。这些文章在VI和社会参与度的调查人群和研究方法上都存在较大差异。总体而言, VI与社会参与度下降具有相关性已达成共识。然而, 在评估AI与社会参与度的相关性时, 更严格的实验设计, 更好的评价标准可以促进研究在不同的人群, 疾病和VI分级中做有效的比较。尝试提供视力康复并减轻VI对幸福感的影响, 可以考虑改善SP的策略。
Similar content being viewed by others
Introduction
Worldwide, vision impairment (VI) and blindness affect more than 250 million people [1]. Prior research has shown that VI is associated with decreased health-related quality of life, an increased risk of falls, depression, cognitive decline, and loss of independence [2]. A number of studies have also suggested that vision loss may have a negative impact on social functioning. This is notable since participation in valued social activities can have important health benefits, including increased well-being, decreased anxiety and depression, and even lower rates of dementia and mortality [3].
Social participation (SP) has been studied using a variety of different conceptual frameworks, including the World Health Organization International Classification of Functioning, Disability, and Health (ICF) [4]. The ICF is a broad model that aims to describe the diverse contributors to overall health and well-being, including health conditions, the body, environmental factors, and participation. However, some contend that SP is not adequately characterized in the ICF since it does not distinguish fully between limitations in activities (e.g., hobbies) and social engagement [5,6,7]. Consequently, others have adopted more nuanced models such as the National Health and Aging Trends Study Disability Framework [8] and Levasseur et al.’s Taxonomy of Social Activities [5] to conceptualize SP and its relationship to health and well-being.
Since there is no consensus definition of SP, it can be challenging for vision researchers and medical providers to discern the association between VI and SP. However, assessing this relationship may be important for promoting overall health, well-being, and vision-related quality of life through comprehensive vision rehabilitation. In order to develop targeted vision rehabilitation strategies that include the promotion of SP for those with poor vision, it is vital to understand more fully the association between VI and SP [9]. Accordingly, in this systematic review, we summarize the current understanding of the association between VI and SP in community-dwelling adults. The objective of this systematic review is to help researchers and clinicians to address gaps in the current understanding of the relationship between VI and SP and to design interventions that promote social functioning in visually impaired adults.
Materials and methods
Protocol and registration
This systematic review was registered on the PROSPERO International prospective register of systematic reviews (CRD42018102767; www.crd.york.ac.uk/prospero) and followed the guidelines for conducting systematic reviews from the Preferred Reporting Items for Systematic Review and Meta-analysis (PRISMA) checklist (Supplementary Table) [10].
Inclusion and exclusion criteria
This review included all studies that quantitatively evaluated the association between VI and SP in community-dwelling adults. Papers were included if they met all of the following criteria: (1) studies of community-dwelling adults age 18 and older; (2) studies that included objective (e.g., visual acuity, visual field, contrast sensitivity, and stereopsis) or subjective (e.g., self-reported) vision assessments; (3) studies that provided quantitative measures of SP; (4) studies that reported a measure of the association between VI and SP; and (5) publications in English, including conference papers and abstracts published from January 1988 to June 2018. We included retrospective or prospective studies, including but not limited to cross-sectional, cohort, case-control, and clinical trial study designs. We also included studies examining dual sensory loss if they reported the independent association between VI and SP.
Studies were excluded from our review if they met any of the following conditions: (1) studies conducted with a focus on a narrow population (e.g., pregnant women, cognitively impaired individuals, students, etc.); (2) studies that only reported the combined impact of dual sensory loss on SP; (3) studies with an explicit focus on other conditions (e.g., multiple sclerosis, cerebral palsy, Parkinson disease, Alzheimer dementia, congestive heart failure, etc.) that could have confounded the association between VI and SP; and (4) studies that measured SP as part of a multidimensional scale with a single summary score, since in these cases it was not possible to discern the association of VI with SP specifically.
Search and selection
A comprehensive search of five databases (MEDLINE, EMBASE, PsycINFO, Scopus, and Sociology Database) was conducted using the following search terms: (“VI” OR “vision loss” OR “poor vision” OR “low vision” OR “visual impairment” OR “visually impaired” OR “loss of vision” OR “blindness”) AND (“SP” OR “social involvement” OR “social engagement” OR “community participation” OR “community involvement” OR “community engagement”). Reference lists of published articles were hand searched and study authors were contacted for additional information when necessary. Studies were included if they were published between January 1988 and June 2018 in English and met the stated inclusion and exclusion criteria.
One author (KS) collected all studies found in the initial search and imported these into Systematic Review Accelerator (CREBP, Bond University, Queensland, Australia) to perform de-duplication. Two authors (KS and CRF) performed initial screening to exclude studies that did not meet the review criteria. The same two authors (KS and CRF) applied inclusion and exclusion criteria independently to remaining studies and the senior author (JRE) arbitrated any disagreements and made the final decision to include or exclude studies. Data were collected based on a modified version of the Cochrane Data Extraction and Assessment Template and collated using Microsoft Excel (Microsoft Corporation, Redmond, Washington, USA) [11].
Social participation (SP)
In order to distinguish between activity and participation restrictions, we adopted Levasseur et al.’s Taxonomy of Social Activities [5], which describes SP using a six-level hierarchy. In this hierarchy, the lowest three levels include activities such as being with others but not interacting, whereas the highest three levels include a “person’s involvement in activities that provide interaction with others in society or the community.” Therefore, for the purpose of this review, we defined SP as belonging to levels 4–6 of the Taxonomy of Social Activities. The ability to distinguish between activity and participation restrictions in this review was important since prior research has demonstrated that activity and participation restrictions represent distinct constructs [7].
Data extraction
Data were collated from included publications and entered into an Excel spreadsheet (Microsoft, Redmond, WA). Criteria that were abstracted from each study included: (1) study author and year of publication; (2) type of study (e.g., cross-sectional, case-control, etc.); (3) location where the study was conducted; (4) ocular condition(s) of study participants; (5) method of VI assessment (e.g., VA, VF, self-report); (6) outcomes measured in addition to SP (e.g., activities of daily living, mental health, etc.); (7) recruitment strategy; (8) sample size; (9) mean age of the study sample; (10) whether the study had a control group; (11) conclusions of the study; and (12) risk of bias.
Quality assessment and data analysis
Two authors (KS and CRF) independently assessed the risk of bias in each study using the Effective Public Health Practice Project Quality Assessment Tool (EPHPP) [12]. This instrument was developed for use in public health and provides a standardized method to assess study quality and develop recommendations for study findings. Studies have demonstrated that EPHPP is a valid and reliable instrument for assessing study bias [13,14,15], and it has been used widely in prior systematic reviews. The EPHPP assesses: (1) selection bias; (2) study design; (3) confounders; (4) blinding; (5) data collection methods; (6) withdrawals and dropouts; (7) intervention integrity; and (8) analysis. Selection bias was graded on the likelihood and extent to which study participants were representative of the target population. Confounders were assessed to determine the degree to which studies controlled for variables that were associated with both the exposure and outcome. Data collection methods and analysis depended on the validity and reliability of measurement tools and on the appropriateness of statistical methods. Three other domains including “blinding,” “intervention integrity,” and “withdrawals and dropouts” were not applicable since no study was classified as a clinical trial. Following the validated EPHPP assessment strategy [12], for each included study the five relevant domains were ranked on a three-point Likert scale with three representing a low risk of bias (“strong”), two a possible risk of bias (“moderate”), and one a high risk of bias (“weak”). An overall rating was derived following the EPHPP methodology. A study consisting of at least one “weak” rating was not able to receive an overall rating higher than “moderate,” while those with two or more “weak” ratings were automatically classified as “weak” overall based on the EPHPP assessment.
A narrative synthesis was constructed from the findings of each included study. The synthesis was structured around the type of study, target population characteristics, and measures of VI and SP. When available, maximally adjusted odds ratios, relative risks and/or 95% CIs were abstracted to illustrate the magnitude of the association between VI and SP. Three researchers were primarily involved in the review, with two summarizing and grading the quality of the evidence (KS and CRF) from each study and a third (JRE) adjudicating any discrepancies.
The University of Michigan institutional review board deemed this study exempt because data were collected and synthesized from previously published studies in which informed consent has already been obtained by the investigators. The study followed the tenets of the Declaration of Helsinki.
Results
There were 881 studies that met search criteria. Of these, 817 were excluded based on review of the titles and abstracts. Among the remaining 64 studies that underwent full-text review, 19 met all inclusion criteria and were qualitatively analyzed. Full details of the systematic review process are illustrated in the PRISMA flow diagram in Fig. 1.
Association between VI and SP
Table 1 presents data summarizing key features of each of the included studies. Eighteen studies (95%) were cross-sectional and one was a longitudinal cohort study. Studies included participants from 18 different countries on four continents, including one study that was multi-national with data from 11 European countries. Sixteen of the studies did not focus on participants with a specific eye disease, while one focused on age-related macular degeneration, one on diabetic retinopathy, and one on glaucoma.
Eighteen studies (95%) concluded that VI was associated with reduced SP. One study reported mixed results that showed participants with VI perceived more restrictions in socializing with others, but not in brief interpersonal interactions and relationships.
Vision and SP measures
Visual acuity was the most commonly used metric to assess visual function (n = 12, 63%). Visual acuity cutoffs to define VI ranged from <20/40 to <20/70. Self-reported measures of visual function were used to define VI in 11 studies (58%). These measures varied, with some asking respondents to rate their vision on a Likert scale, while others asked about difficulty with various daily activities, and others asked participants if they had trouble seeing. Seven studies (37%) used visual field criteria to define VI, and one study used contrast sensitivity.
Measures of SP also varied across studies. Four studies (21%) used the ICF framework as a basis for assessing SP. Ten studies (53%) used different formal validated questionnaires for assessing SP, and the remaining five (26%) used informal or non-validated survey questions.
Quality assessment
Most studies recruited participants from a convenience sample (n = 11, 58%) and were cross-sectional (n = 18, 95%). For each study, Table 2 divides the bias assessment based on the five applicable domains of the EPHPP, in addition to an overall study rating. The risk of confounding was influenced by study design, as more than half the studies (53%) received a ranking of “weak” in the confounders domain due to lack of appropriate data and/or inadequate adjusting, matching, or stratifying.
Overall, four studies (21%) were categorized as “moderate” (e.g., possible risk of bias) and fifteen (79%) were categorized as “weak” (e.g., high risk of bias). No study received an overall rating of “strong” because all had a “weak” rating for study design; in all but one case this was due to studies being cross-sectional, a design that is considered “weak” in the risk of bias assessment.
Discussion
Understanding the relationship between poor vision and SP is an important step toward promoting health and well-being in visually impaired adults. This systematic review found that there is strong agreement in the scientific literature that VI is associated with reduced SP. However, there was also a moderate to high risk of bias in all studies. This systematic review makes several important contributions. First, it highlights the importance of adopting standard definitions and assessment tools for research on complex health-related constructs like SP. In addition, the consistent association between poor vision and restricted SP points to an unmet opportunity to develop, evaluate, and implement models of vision rehabilitation that promote SP, which could ultimately improve health, well-being and vision-related quality of life.
Quality of evidence
Our systematic review evaluated bias among the 19 included studies utilizing the validated EPHPP [12]. Most included studies were cross-sectional and used convenience sampling to select participants who were seeking vision services. Consequently, these studies were susceptible to selection bias and may have yielded estimates that do not reflect true associations in the target population. Ten of the eleven studies that utilized convenience sampling reported that VI was associated with reduced SP, while one study found that VI was associated with reduction in socializing with others but was not associated with restrictions in brief interpersonal interactions and relationships. Studies that used convenience samples may have underestimated the true association between VI and SP, since those seeking eye care or vision rehabilitative services may be more likely to have access to supportive care, an opportunity to interact with those providing care, and/or a chance to meet others facing similar challenges. Of the remaining 8 studies that used a systematic sampling strategy, 2 had a “weak” rating in just a single domain, and all reported that VI was associated with reduced SP.
A secondary finding was heterogeneity in the measurement and reporting of SP. Studies measured SP using a variety of instruments. Similarly, VI was assessed by self-report in some studies and by several different objective measures of visual function in others. The parameters used to define SP and VI may have impacted results across and within studies. For example, Jones et al. found that restricted SP had a stronger association with self-reported blindness (adjusted OR = 2.85 [95% CI 2.04–3.97]) than with self-reported VI (defined as “trouble seeing, even with glasses or contact lenses,” but not blind; [adjusted OR 2.19, 95% CI 2.00–2.41]) [16]. This finding suggests that severity of VI could be associated with the likelihood of SP restrictions. However, when another study used the same definition of SP, but defined VI based on having received a referral for low vision services, the investigators failed to detect a difference in SP between the study sample and controls [17].
In future studies, a more standardized approach to measurement of VI and SP could be implemented. This would facilitate comparisons across different studies, performance of meta-analyses, and an even more in-depth understanding of the relationship between VI and SP across different populations. Items measuring SP should only reflect participation restriction, which must be assessed separately from activity restriction, an important but distinct construct [7]. Ultimately, research in this area would benefit substantially from the adoption of single valid, reliable, and unidimensional consensus instrument to measure SP.
Association between VI and SP
This systematic review found that there is strong consensus in the literature that VI is associated with reduced SP. However, since nearly all of the studies in this review were cross-sectional, causality cannot be determined. Findings suggest that higher order activities in Levasseur’s Taxonomy of Social Activities (levels 4–6) [5], such as collaborating with and helping others, and contributing to society, may be more sensitive to changes in vision than lower order activities like “being around” others (level 2). For example, Alma et al. reported a positive association between VI and reduced involvement in clubs/associations and sports participation, but not with assisting others or engaging in brief interpersonal interactions [17]. Similarly, Zimdars et al. found that VI was more strongly associated with membership in an organization and participation in cultural activities than it was with the quality of relationships with friends and family [18]. These results imply that those social activities that may be likely to provide the greatest benefit—for example, interacting with people and communities—may also be the most challenging for those with poor vision.
There are numerous hypotheses that could explain the association between VI and SP. Intuitively, VI may cause a reduction in SP directly since VI can make it challenging for people to leave their homes and enter spaces where social activities normally occur [17, 19]. Poor vision may affect other factors, such as activity limitations, that in turn lead to reduced SP. In addition, VI and reduced SP are both associated with depression [20,21,22,23], though it is not known whether depression is a confounder, mediator, or result of the association between VI and SP. It is also plausible that reduced SP could lead to an increased incidence of VI, if those who are less socially engaged are also less likely to get eye exams, as some prior studies have suggested [24]. Future studies should explicitly investigate the directionality and causal pathways between VI and SP in order to test the aforementioned hypotheses.
Implications
Poor vision and restricted SP are both associated with decreased health, well-being and health-related quality of life [9]. An improved understanding of the relationship between VI and SP is crucial for informing future work to develop and evaluate interventions that promote SP and well-being for visually impaired adults. Some studies suggest that incorporating a problem-solving approach into low vision occupational therapy could improve SP [25, 26]. A team-based vision rehabilitation approach that included ophthalmic nursing, ophthalmology, optometry, social work, occupational therapy, and rehabilitation counseling also had a positive effect on SP [25]. However, therapeutic approaches that included cognitive restructuring and education/functional training did not appear to have a positive effect [26]. In stroke survivors, exercise has proven to be an important component of rehabilitation strategies that improve SP [27]. The benefits of exercise included improved physical ability to leave the home and elevated mood. A similar approach could be valuable for promoting SP in those with VI. The role of co-occurring cognitive and mental health conditions as well as physical disorders should also be explored since VI rarely occurs in isolation. Targeting each of these may maximize the effect of comprehensive rehabilitation.
Strengths and limitations
There were several limitations to this study. Since measures of SP and VI were heterogeneous, it was difficult to compare results across studies and it was therefore not feasible to perform a meta-analysis. We only included studies published in English, though several included studies were from non-English speaking countries. In addition, a majority of studies had an overall “weak” rating on the bias assessment, leaving open the possibility that conclusions from these studies were biased. In the bias assessment, cross-sectional observational studies received a “weak” rating on the study design domain, and any study with a “weak” rating in one or more domains cannot receive an overall “strong” bias assessment. Because no studies included in this systematic review were interventional, three of the eight bias assessment domains were inapplicable. Strengths of this study include a comprehensive search through five databases; adherence with the PRISMA methodology for conducting a systematic review [10] and the EPHPP for assessing study bias [12]; and a focus on SP, an emerging topic in vision science that to date has not been systematically appraised but is highly relevant to a holistic and patient-centered approach to optimizing vision-related quality of life.
Conclusions
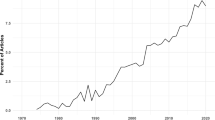
There is strong consensus in the literature that VI is associated with reduced SP in community-dwelling adults [28]. The number of adults with VI in the United States is expected to more than double over the next 30 years. Consequently, these findings have important implications as researchers, medical providers, and caregivers attempt to maximize overall health and well-being in adults with poor vision. In future work, investigators should develop and employ a standardized measure of SP. Additional research is also needed to evaluate longitudinally the association between VI and SP in order to determine causality, the factors that mediate this pathway, and the accommodations that are useful for decreasing social limitations in this population. Understanding the relationship between VI and SP is vital to the development of future interventions to promote SP and, ultimately, to improve health and well-being in visually impaired adults.
References
Flaxman SR, Bourne RRA, Resnikoff S, Ackland P, Braithwaite T, Cicinelli MV, et al. Global causes of blindness and distance vision impairment 1990–2020: a systematic review and meta-analysis. Lancet Glob Health. 2017;5:e1221–e34.
National Academies of Sciences, Engineering, and Medicine. Making eye health a population health imperative: Vision for tomorrow. Washington DC: National Academies Press; 2016.
Cherry KE, Walker EJ, Brown JS, Volaufova J, LaMotte LR, Welsh DA, et al. Social engagement and health in younger, older, and oldest-old adults in the Louisiana Healthy Aging Study. J Appl Gerontol. 2013;32:51–75.
The World Health Organization. International classification of functioning, disability, and health (ICF). Geneva: The World Health Organization; 2001.
Levasseur M, Richard L, Gauvin L, Raymond E. Inventory and analysis of definitions of social participation found in the aging literature: proposed taxonomy of social activities. Soc Sci Med. 2010;71:2141–9.
Piskur B, Daniels R, Jongmans MJ, Ketelaar M, Smeets RJ, Norton M, et al. Participation and social participation: are they distinct concepts? Clin Rehabil. 2014;28:211–20.
Jette AM, Tao W, Haley SM. Blending activity and participation sub-domains of the ICF. Disabil Rehabil. 2007;29:1742–50.
Freedman VA. Adopting the ICF language for studying late-life disability: a field of dreams? J Gerontology Ser A, Biol Sci Med Sci. 2009;64:1172–4. discussion 5–6
Lamoureux EL, Hassell JB, Keeffe JE. The determinants of participation in activities of daily living in people with impaired vision. Am J Ophthalmol. 2004;137:265–70.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JP, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ (Clin Res Ed). 2009;339:b2700.
Cochrane Public Health. Review Authors. https://ph.cochrane.org/review-authors., Acessed 26 November 2019.
Effective Public Health Practice Project. Quality assessment tool for quantitative studies. Hamilton, ON: Effective Public Health Practice Project; 1998. https://merst.ca/ephpp/. Accessed 26 November 2019
Thomas BH, Ciliska D, Dobbins M, Micucci S. A process for systematically reviewing the literature: providing the research evidence for public health nursing interventions. Worldviews Evid Based Nurs. 2004;1:176–84.
Armijo-Olivo S, Stiles CR, Hagen NA, Biondo PD, Cummings GG. Assessment of study quality for systematic reviews: a comparison of the cochrane collaboration risk of bias tool and the effective public health practice project quality assessment tool: methodological research. J Eval Clin Pract. 2012;18:12–8.
da Silva AT, Hauschild DB, de Almeida Oliveira LD, de Fragas Hinnig P, Franco Moreno YM, Wazlawik E. Association of hyperhydration evaluated by bioelectrical impedance analysis and mortality in patients with different medical conditions: systematic review and meta-analyses. Clin Nutr ESPEN. 2018;28:12–20.
Jones GC, Crews JE, Danielson ML.Health risk profile for older adults with blindness: an application of the international classification of functioning, disability, and health framework.Ophthalmic Epidemiol.2010;17:400–10.
Cimarolli VR, Boerner K, Brennan-Ing M, Reinhardt JP, Horowitz A. Challenges faced by older adults with vision loss: a qualitative study with implications for rehabilitation. Clin Rehabil. 2012;26:748–57.
Zimdars A, Nazroo J, Gjonça E. The circumstances of older people in England with self-reported visual impairment: a secondary analysis of the English Longitudinal Study of Ageing (ELSA). Br J Vis Impair. 2012;30:22–30.
Laliberte Rudman D, Gold D, McGrath C, Zuvela B, Spafford MM, Renwick R. “Why would I want to go out?”: age-related vision loss and social participation. Can J Aging. 2016;35:465–78.
Crews JE, Chou CF, Sekar S, Saaddine JB. The prevalence of chronic conditions and poor health among people with and without vision impairment, aged ≥65 Years, 2010–2014. Am J Ophthalmol. 2017;182:18–30.
Zhang X, Bullard KM, Cotch MF, Wilson MR, Rovner BW, McGwin G Jr., et al. Association between depression and functional vision loss in persons 20 years of age or older in the United States, NHANES 2005–2008. JAMA Ophthalmol. 2013;131:573–81.
Croezen S, Avendano M, Burdorf A, van Lenthe FJ. Social participation and depression in old age: a fixed-effects analysis in 10 European countries. Am J Epidemiol. 2015;182:168–76.
Frank CR, Xiang X, Stagg BC, Ehrlich JR. Longitudinal associations of self-reported vision impairment with symptoms of anxiety and depression among older adults in the United States. JAMA Ophthalmol. 2019;137:793–800.
Ehrlich JR, Stagg BC, Andrews C, Kumagai A, Musch DC. Vision Impairment and receipt of eye care among older adults in Low- and Middle-Income Countries. JAMA Ophthalmol. 2018;137:146–58.
Berger S, McAteer J, Schreier K, Kaldenberg J. Occupational therapy interventions to improve leisure and social participation for older adults with low vision: a systematic review. Am J Occup Therapy. 2013;67:303–11.
Roets-Merken LM, Draskovic I, Zuidema SU, van Erp WS, Graff MJ, Kempen GI, et al. Effectiveness of rehabilitation interventions in improving emotional and functional status in hearing or visually impaired older adults: a systematic review with meta-analyses. Clin Rehabil. 2015;29:107–19.
Obembe AO, Eng JJ. Rehabilitation interventions for improving social participation after stroke: a systematic review and meta-analysis. Neurorehabilit Neural Repair. 2016;30:384–92.
Chan T, Friedman DS, Bradley C, Massof R. Estimates of incidence and prevalence of visual impairment, low vision, and blindness in the United States. JAMA Ophthalmol. 2018;136:12–9.
Alma MA, van der Mei SF, Melis-Dankers BJ, van Tilburg TG, Groothoff JW, Suurmeijer TP. Participation of the elderly after vision loss. Disabil Rehabil. 2011;33:63–72.
Alma MA, Van der Mei SF, Groothoff JW, Suurmeijer TP. Determinants of social participation of visually impaired older adults. Qual Res. 2012;21:87–97.
Bachar E, Shanan J. Long lasting blindness, availability of resources, and early aging. Percept Mot Skills. 1997;84:675–88.
Cimarolli VR, Boerner K, Reinhardt JP, Horowitz A, Wahl HW, Schilling O, et al. A population study of correlates of social participation in older adults with age-related vision loss. Clin Rehabil. 2017;31:115–25.
Crews JE, Campbell VA. Vision impairment and hearing loss among community-dwelling older Americans: implications for health and functioning. Am J Public Health. 2004;94:823–9.
Desrosiers J, Wanet-Defalque MC, Temisjian K, Gresset J, Dubois MF, Renaud J, et al. Participation in daily activities and social roles of older adults with visual impairment. Disabil Rehabil. 2009;31:1227–34.
Gallagher P, Mulvany F. Levels of ability and functioning: using the WHODAS II in an Irish context. Disabil Rehabil. 2004;26:506–17.
Jaarsma EA, Dekker R, Koopmans SA, Dijkstra PU, Geertzen JH. Barriers to and facilitators of sports participation in people with visual impairments. Adapted Phys Activity Q. 2014;31:240–64.
Lamoureux EL, Hassell JB, Keeffe JE. The impact of diabetic retinopathy on participation in daily living. Arch Ophthalmol. 2004;122:84–8.
Latorre-Arteaga S, Gil-Gonzalez D, Vives-Cases C, La Parra Casado D. Vision and hearing health inequities in the Roma population: a national cross-sectional study in Spain. J Immigr Minor Health. 2017;19:1304–14.
Matthews K, Nazroo J, Whillans J. The consequences of self-reported vision change in later-life: evidence from the English Longitudinal Study of ageing. Public Health. 2017;142:7–14.
Mick P, Parfyonov M, Wittich W, Phillips N, Kathleen Pichora-Fuller M. Associations between sensory loss and social networks, participation, support, and loneliness: analysis of the Canadian Longitudinal Study on Aging. Can Fam Physician. 2018;64:e33–e41.
Nael V, Peres K, Carriere I, Daien V, Scherlen AC, Arleo A, et al. Visual impairment, undercorrected refractive errors, and activity limitations in older adults: findings from the three-city alienor study. Invest Ophthalmol Vis Sci. 2017;58:2359–65.
Pongsachareonnont P, Uramphorn N, Hounnaklang N. Association between visual status and mental health status in Thai rural elderly: a community-based study. Int J Ophthalmol. 2018;11:852–7.
Viljanen A, Tormakangas T, Vestergaard S, Andersen-Ranberg K. Dual sensory loss and social participation in older Europeans. Eur J Ageing. 2014;11:155–67.
Yang Y, Trope GE, Buys YM, Badley EM, Gignac MA, Shen C, et al. Glaucoma severity and participation in diverse social roles: does visual field loss matter? J Glaucoma. 2016;25:e697–703.
Funding
This work was supported by grants from the National Eye Institute (K23 EY027848) to JRE; a pilot grant from the Michigan Center on the Demography of Aging at the University of Michigan funded through a National Institute on Aging core grant (P30 AG012846); an unrestricted grant from Research to Prevent Blindness to the Department of Ophthalmology and Visual Sciences at the University of Michigan; and the Lighthouse Guild.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Shah, K., Frank, C.R. & Ehrlich, J.R. The association between vision impairment and social participation in community-dwelling adults: a systematic review. Eye 34, 290–298 (2020). https://doi.org/10.1038/s41433-019-0712-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41433-019-0712-8
This article is cited by
-
The burden of vision loss in the Middle East and North Africa region, 1990–2019
Archives of Public Health (2023)